Postoperative Management and Soft Tissue Closure in Replantation Surgery
Key Takeaway
Successful replantation surgery extends far beyond the microsurgical anastomosis. Meticulous wound closure, strategic postoperative splinting, and vigilant hemodynamic monitoring are paramount to graft survival. This comprehensive guide details evidence-based protocols for managing circulatory compromise, optimizing anticoagulation, and preventing vasospasm. By adhering to these rigorous postoperative pathways, microsurgeons can effectively mitigate the risks of arterial insufficiency and venous congestion, ensuring optimal functional recovery of the replanted appendage.
INTRODUCTION TO REPLANTATION WOUND MANAGEMENT
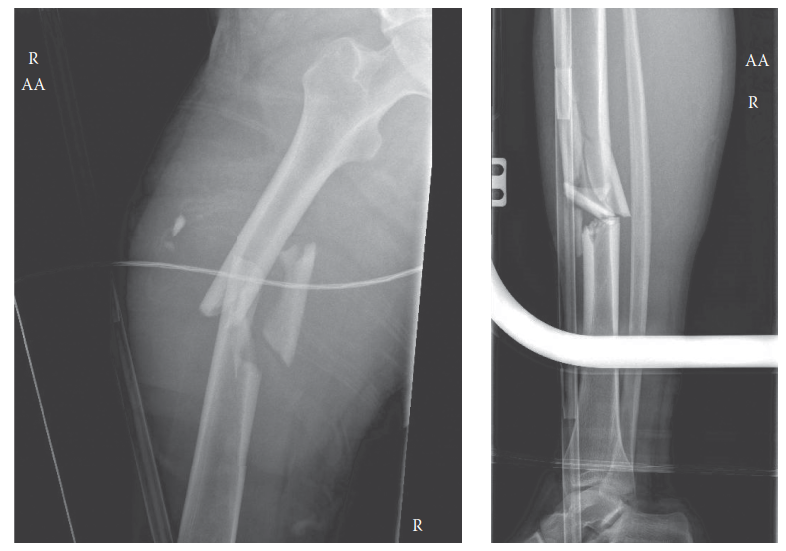
The successful replantation of an amputated digit or extremity represents a pinnacle of microsurgical achievement. However, the technical execution of vascular anastomoses and nerve repairs is only the first phase of a complex continuum of care. The postoperative period is fraught with risks, primarily vasospasm, thrombosis, and ischemia-reperfusion injury. The meticulous management of soft tissue closure, the strategic application of dressings, and the rigorous implementation of postoperative monitoring protocols are absolute prerequisites for graft survival.
This masterclass delineates the evidence-based principles of wound closure, postoperative splinting, hemodynamic monitoring, and the pharmacological management of the replanted part, providing orthopedic and plastic microsurgeons with a definitive framework for optimizing clinical outcomes.
PRINCIPLES OF WOUND CLOSURE IN REPLANTATION
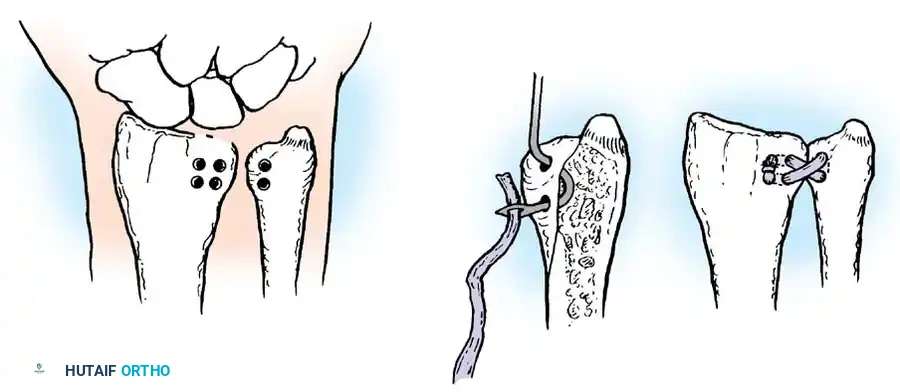
Following the definitive repair of all deep structures—including bone, tendons, nerves, and vessels—the surgeon must address the soft tissue envelope. The overriding principle of wound closure in replantation is the absolute avoidance of tension. Tension across the skin edges inevitably translates to compression of the underlying microvascular anastomoses, precipitating venous congestion and subsequent arterial thrombosis.
Primary Closure vs. Secondary Intention
Primary closure of the skin is permissible only under a strict set of criteria:
* The replantation procedure has been completed promptly, minimizing ischemic time.
* There is an absence of excessive soft tissue swelling or edema.
* The skin edges can be approximated with zero tension.
In the digits and more proximal amputation sites, the trauma associated with the injury (particularly crush or avulsion mechanisms) often results in significant edema. In these scenarios, primary closure is contraindicated. Portions of the wound must be left open to heal by secondary intention or be definitively covered with skin grafts.
Surgical Warning: Critical structures—specifically nerves, vessels, bone, articular cartilage, and tendons devoid of paratenon—must never be left exposed to desiccate. If the wound cannot be closed primarily without tension, alternative soft tissue coverage must be employed immediately to protect these vital structures.
Advanced Soft Tissue Coverage Techniques
When primary closure is not feasible, the reconstructive ladder must be utilized to achieve stable, tension-free coverage:
* Local Tissue Rearrangement: Z-plasties and local rotation flaps are highly effective for relieving circumferential tension and covering exposed neurovascular bundles.
* Skin Grafting: Split-thickness skin grafts (STSG) or full-thickness skin grafts (FTSG) are frequently utilized to cover non-critical soft tissue defects, allowing the primary wound to remain partially open to accommodate postoperative swelling.
* Complex Flap Coverage: While remote, two-stage pedicle flaps (e.g., groin flaps) and single-stage free tissue transfers (free flaps) are viable alternatives, they are rarely required in the acute setting of uncomplicated replantations.
In extensive clinical experience, a hybrid approach—combining local skin flap rotation, split-thickness skin grafting, and leaving non-critical portions of the wound open—yields the most satisfactory and reproducible results.
DRESSING APPLICATION AND BIOMECHANICS OF SPLINTING
The application of the postoperative dressing is a critical surgical step that demands the same level of precision as the microsurgical anastomosis. An improperly applied dressing can act as a tourniquet, leading to catastrophic graft loss.
The Replantation Dressing Protocol
- Contact Layer: Apply medicated petrolatum gauze directly to the skin wounds. This non-adherent layer prevents the desiccation of exposed tissues and facilitates atraumatic dressing changes.
- Absorbent Layer: Utilize a bulky dressing to cover both the dorsal and palmar surfaces. Fluffed cotton or specialized synthetic materials provide a soft, gently conforming interface.
- Moisturization: The padding must be moistened with physiological saline or lactated Ringer’s solution. This critical step serves two purposes: it allows extravasated blood to be absorbed into the bandage more readily, and it permits the bandage to conform seamlessly to the complex contours of the hand and digits.
- Avoidance of Pressure: Localized pressure must be avoided at all times. Circumferential wrapping must be applied with minimal tension.
Clinical Pearl: Dried blood within a dressing can harden and create a "cast-like" effect, acting as a circumferential constricting band. Moistening the dressing prevents this phenomenon and maintains a compliant soft tissue envelope.
Splinting and Positioning
The replanted part must be adequately padded and supported. A plaster or fiberglass splint is applied to the palmar surface to support the fingers, hand, and wrist in a safe, functional position (typically the intrinsic-plus position, unless contraindicated by specific tendon repairs).
Excessive tightness or constriction during the securing of the bandage is strictly avoided. Crucially, the fingertips and small "windows" of skin must be left exposed to allow for continuous clinical evaluation of capillary refill, turgor, and color.
POSTOPERATIVE CARE PROTOCOLS
The postoperative environment must be meticulously controlled to prevent vasospasm and optimize hemodynamics. Depending on the extent of the injury, the patient is typically maintained on strict bed rest for the first 3 to 7 days.
Environmental and Systemic Optimization
- Temperature Control: The patient's room must be maintained at a comfortably warm temperature (typically above 75°F / 24°C) to prevent cold-induced peripheral vasoconstriction.
- Strict Prohibitions: Smoking by the patient and any visitors is absolutely prohibited. Nicotine is a potent vasoconstrictor that can rapidly induce microvascular thrombosis. Abstinence from caffeine-containing beverages is also strongly advised.
- Psychological and Pain Management: Vasospasm is frequently triggered by pain, anxiety, and emotional distress. This sympathetic response must be blunted through the aggressive use of appropriate narcotic analgesics. Sedative medications, such as chlorpromazine (25 mg administered four times daily), are highly effective in reducing anxiety and providing a mild alpha-adrenergic blocking effect, which further mitigates vasospasm.
Dressing Management
During the first week, the bulky bandage is moistened with physiological solutions every 8 hours. This prevents the formation of circumferential crusts of dried blood.
Although early and frequent dressing changes might seem advantageous for assessing circulation or identifying bleeding sources, the standard policy in uncomplicated replantations is to delay the initial dressing change for at least 1 week. Premature dressing changes carry a high risk of mechanically disturbing the fragile vascular anastomoses and stimulating severe vascular spasm.
Limb Positioning and Hemodynamic Management
The baseline position for a replanted part is at heart level, provided the clinical appearance remains satisfactory. However, positioning is a dynamic tool used to manage early signs of circulatory imbalance:
* Venous Obstruction: If the replanted part appears congested, turgid, and cyanotic, venous outflow is inadequate. The limb should be elevated on several pillows to enhance gravity-assisted venous drainage.
* Arterial Insufficiency: If the part becomes pale, cool, and loses turgor, arterial inflow is compromised. Depression of the part below the level of the heart may be required to enhance arterial perfusion pressure.
MANAGEMENT OF CIRCULATORY COMPROMISE AFTER REPLANTATION
The survival of a replanted digit hinges on the early detection and rapid management of circulatory compromise. Prompt intervention can salvage a part that would otherwise progress to irreversible necrosis.
Clinical and Objective Monitoring
Mechanical monitors are invaluable adjuncts to clinical examination. Modalities such as continuous skin temperature monitoring, transcutaneous oxygen tension (TcPO2), hydrogen clearance, and fluorescein dilution are sufficiently sensitive to detect significant changes in microvascular blood flow long before clinically apparent ischemic changes manifest. A drop in surface temperature of more than 2°C or an absolute temperature below 30°C is highly indicative of vascular compromise.
Differentiating Arterial vs. Venous Insufficiency
- Arterial Insufficiency: Characterized by a cool, pale digit with a loss of tissue turgor. Capillary refill is absent, and bleeding from a pinprick is non-existent.
- Venous Obstruction: Characterized by a cyanotic (blue/purple), congested, and turgid digit. Capillary refill is excessively brisk initially, later becoming absent. Pinprick yields dark, venous blood.
Non-Operative Salvage Maneuvers
If circulatory compromise is detected, several immediate bedside measures must be instituted before considering a return to the operating room for surgical exploration:
- Optimize the Environment: Ensure the room is warm and the patient is adequately sedated and pain-free to eliminate sympathetically mediated vasospasm.
- Adjust Positioning: Elevate the limb well above the heart for venous congestion; place the limb in a dependent position for suspected arterial insufficiency.
- Release Constriction: Splints and dressings must be immediately loosened or entirely removed to ensure no external pressure is compressing the vessels. Even a single tight suture can precipitate ischemia; targeted suture removal may be necessary.
- Vascular "Milking": Using gentle digital pressure, the vessels can be lightly manipulated to clear early sludge or stasis. Arteries are lightly "milked" from proximal to distal, while veins are "milked" from distal to proximal.
Pitfall: Vascular milking must be performed with extreme caution. Aggressive manipulation can disrupt the anastomosis, induce severe intimal damage, or dislodge a stable clot, converting a salvageable situation into a catastrophic failure.
The Role of Hirudotherapy (Medicinal Leeches)
For refractory venous congestion—particularly in distal replantations where venous anastomoses were impossible or have failed—medical-grade leeches (Hirudo medicinalis) are highly effective. Leeches secrete hirudin, a potent direct thrombin inhibitor, and actively extract congested blood while promoting continued oozing from the bite site.
Warning: Hirudotherapy carries a significant risk of infection, specifically from Aeromonas hydrophila, an enteric bacterium native to the leech's gut. Prophylactic antibiotics (e.g., Ciprofloxacin or Trimethoprim-Sulfamethoxazole) are mandatory. Furthermore, leeches should never be applied to nonviable, arterial-deficient tissue.
PHARMACOLOGICAL MANAGEMENT AND REGIONAL ANESTHESIA
The pharmacological protocol following replantation is designed to maintain vasodilation, prevent thrombosis, and manage the rheological properties of the blood.
Regional Anesthesia and Sympathectomy
Nerve blocks are highly beneficial in the postoperative period for the prevention of sympathetically mediated vasospasm.
* Indwelling Catheters: In distal injuries, small Silastic catheters can be placed adjacent to the median or ulnar nerves during the primary surgery. Postoperatively, 4 to 5 mL of 0.25% bupivacaine is injected through these catheters every 6 to 8 hours to maintain a continuous regional block.
* Proximal Blocks: Stellate ganglion sympathetic blocks or axillary brachial plexus blocks utilizing bupivacaine can be performed once or twice daily in situations where severe, refractory vasospasm must be controlled.
Systemic Anticoagulation Strategies
The use of systemic anticoagulants is highly surgeon-dependent, but a combination of agents is typically employed to target different pathways of the coagulation cascade. Commonly utilized agents include Heparin, low-molecular-weight dextran, aspirin, dipyridamole, and sodium warfarin.
Heparin Therapy:
Intravenous heparin is generally reserved for replantations deemed at high risk for thrombosis. Indications for heparinization include:
* Extensive crushing or avulsing injury mechanisms.
* Poor or sluggish flow from the cut ends of vessels prior to anastomosis.
* Equivocal flow across completed anastomoses.
* Replantations performed in small children, where vessel caliber is exceptionally small.
Dextran and Aspirin Protocol:
A widely accepted and highly effective standard protocol utilizes a combination of Dextran 40 and Aspirin. Dextran acts as a volume expander, decreases blood viscosity, and alters platelet adhesiveness.
* Dextran Dosage: 500 mL administered intravenously every 24 hours (in pediatric patients, the dose is 10 mL/kg/day) for a duration of 3 days.
* Aspirin Dosage: 300 mg administered orally twice daily for 5 to 7 days to provide sustained antiplatelet activity via cyclooxygenase inhibition.
Antibiotic Prophylaxis
Given the contaminated nature of traumatic amputations and the presence of foreign materials (sutures, K-wires, plates), broad-spectrum intravenous antibiotics are administered routinely for 1 week following surgery to prevent devastating deep space infections that would compromise the replanted tissue.
CONCLUSION
The postoperative management of a replanted digit or limb is a rigorous, multidisciplinary endeavor that demands unwavering vigilance. By adhering to strict protocols regarding tension-free wound closure, meticulous dressing application, dynamic limb positioning, and targeted pharmacological intervention, the microsurgeon can successfully navigate the perilous postoperative period. Mastery of these principles ensures the highest possible rates of graft survival and sets the foundation for optimal functional rehabilitation.
You Might Also Like