Paget Disease of the Hand: Pathophysiology, Diagnosis, and Surgical Management
Key Takeaway
Paget disease of the hand is an exceedingly rare manifestation of osteitis deformans characterized by disorganized bone remodeling. It presents with sclerotic, fusiform enlargement of the metacarpals or phalanges. While primarily managed medically, surgical intervention is indicated for pathologic fractures, severe functional deformity, or malignant transformation. This guide details the biomechanical challenges, diagnostic differentiation from fibrous dysplasia, and specialized surgical techniques required for managing pagetic bone.
INTRODUCTION TO PAGET DISEASE IN THE UPPER EXTREMITY
Paget disease of bone (osteitis deformans) is a chronic, focal skeletal disorder characterized by aberrant and excessive bone remodeling. While it frequently affects the axial skeleton, pelvis, femur, and skull, its manifestation in the long bones of the hand and upper extremity is exceedingly rare. When it does occur in the hand, it presents unique diagnostic and surgical challenges due to the intricate biomechanics of the digits and the profound structural alterations of the affected bone.
The incidence of Paget disease in the hand is statistically negligible compared to its prevalence in the general population. However, orthopedic surgeons must be adept at recognizing its pathognomonic signs—specifically, the sclerotic, fusiform enlargement of the metacarpals or phalanges—to differentiate it from other tumorous conditions such as fibrous dysplasia, enchondromatosis, or metastatic disease.
Clinical Pearl: The presence of an isolated, enlarged, and sclerotic metacarpal in an elderly patient should immediately raise the clinical suspicion of Paget disease, prompting a systemic evaluation for polyostotic involvement.
PATHOPHYSIOLOGY AND BIOMECHANICS
The pathophysiology of Paget disease is divided into three distinct, albeit overlapping, phases that directly dictate the biomechanical properties of the bone and influence surgical decision-making:
- The Initial Osteolytic Phase: Characterized by aggressive, localized bone resorption mediated by giant, multinucleated osteoclasts. In the hand, this may present as an advancing wedge of osteolysis (blade-of-grass sign), though this is rarely captured before progressing.
- The Mixed Osteoblastic-Osteolytic Phase: A compensatory, disorganized surge in osteoblastic activity occurs. The newly formed bone is woven rather than lamellar. The bone becomes highly vascularized, leading to localized warmth and potential high-output states.
- The Sclerotic (Osteosclerotic) Phase: Bone turnover decreases, leaving behind a dense, enlarged, and structurally chaotic mass of woven bone. This bone exhibits a "mosaic" or "jigsaw puzzle" pattern of cement lines on histology.
Biomechanical Implications for the Hand Surgeon
Despite its dense, sclerotic appearance on radiographs, pagetic bone is biomechanically inferior. The disorganized woven bone lacks the tensile and compressive strength of normal lamellar bone. It is highly brittle and prone to transverse, "chalk-stick" pathologic fractures. Furthermore, the loss of normal corticomedullary differentiation makes intramedullary fixation techniques nearly impossible, while the extreme hardness of the sclerotic phase can lead to drill bit breakage and hardware failure during open reduction and internal fixation (ORIF).
CLINICAL PRESENTATION
Patients with Paget disease of the hand typically present in their sixth to eighth decade of life. The clinical presentation may include:
* Insidious Pain: Often described as a deep, dull ache that occurs at rest and at night, distinguishing it from mechanical osteoarthritis.
* Visible Deformity: Fusiform swelling and bowing of the affected digit or metacarpal.
* Hyperthermia: The skin overlying the active pagetic lesion may be warm to the touch due to profound local hypervascularity.
* Secondary Arthrosis: Enlargement of the periarticular bone can alter joint kinematics, leading to secondary osteoarthritis of the metacarpophalangeal (MCP) or interphalangeal (IP) joints.
DIAGNOSTIC IMAGING AND WORKUP
Radiographic Evaluation
Standard posteroanterior (PA), lateral, and oblique radiographs of the hand are the cornerstone of diagnosis. Radiographs reveal a pathognomonic sclerotic, fusiform enlargement of the long bones. There is a distinct loss of the normal corticomedullary junction, cortical thickening, and a coarse, trabecular "cotton-wool" appearance.
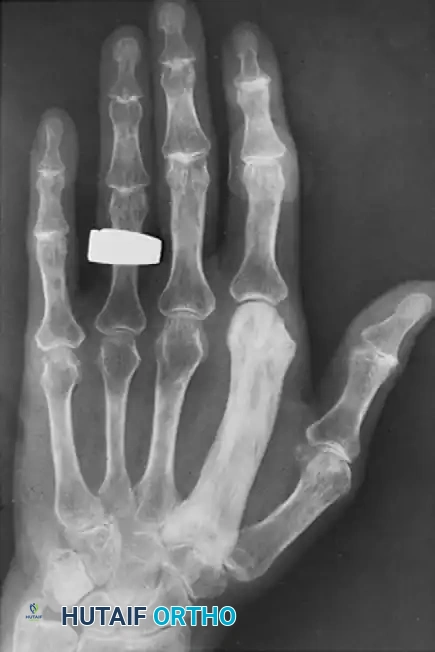
Figure: Paget disease of the second metacarpal. Note the profound sclerotic fusiform enlargement, cortical thickening, and complete obliteration of the medullary canal compared to the adjacent normal metacarpals.
Advanced Imaging and Laboratory Workup
- Bone Scintigraphy (Technetium-99m): Highly sensitive for identifying the extent of polyostotic disease. Pagetic lesions demonstrate intense, uniform radiotracer uptake.
- Computed Tomography (CT): Useful for preoperative planning, particularly to assess the exact degree of sclerosis and to rule out subtle pathologic fractures.
- Magnetic Resonance Imaging (MRI): Indicated if there is suspicion of malignant transformation (e.g., cortical destruction, soft tissue mass).
- Laboratory Markers: Serum alkaline phosphatase (ALP) is typically elevated, reflecting increased osteoblastic activity. Procollagen type I N-terminal propeptide (PINP) is a highly sensitive marker for monitoring disease activity.
DIFFERENTIAL DIAGNOSIS
Paget disease in the hand must be meticulously differentiated from other osseous lesions:
* Fibrous Dysplasia: Often presents with a "ground-glass" appearance rather than the coarse, sclerotic trabeculation of Paget disease. Fibrous dysplasia typically lacks the extreme cortical thickening seen in the sclerotic phase of Paget's.
* Enchondroma: The most common benign bone tumor of the hand. Presents as a well-circumscribed, central lytic lesion with stippled calcifications, not as a diffuse fusiform enlargement.
* Metastatic Disease: May present as destructive lytic or blastic lesions. A history of primary malignancy (e.g., prostate, breast, lung) is usually present.
* Osteosarcoma: While primary osteosarcoma of the hand is rare, secondary osteosarcoma can arise within pagetic bone (Pagetoid sarcoma).
SURGICAL INDICATIONS
While the primary management of Paget disease is medical (utilizing bisphosphonates such as zoledronic acid to inhibit osteoclast activity), surgical intervention in the hand is indicated under specific circumstances:
- Pathologic Fractures: Transverse "chalk-stick" fractures that are unstable or displaced.
- Severe Functional Deformity: Bowing or enlargement that mechanically impedes adjacent digit function or causes severe secondary joint contractures.
- Malignant Transformation: The development of Pagetoid osteosarcoma, fibrosarcoma, or chondrosarcoma, necessitating limb salvage surgery or amputation.
- Nerve Compression: Extremely rare in the hand, but massive enlargement of carpal bones (if involved) could theoretically precipitate carpal tunnel syndrome.
Surgical Warning: Surgery on active pagetic bone is associated with massive intraoperative hemorrhage due to hypervascularity. Preoperative medical optimization with bisphosphonates or calcitonin is strongly recommended to reduce disease activity and vascularity prior to elective procedures.
PREOPERATIVE PLANNING AND POSITIONING
- Anesthesia: Regional anesthesia (brachial plexus block) is preferred to provide excellent intraoperative conditions and postoperative analgesia.
- Positioning: The patient is positioned supine with the operative arm extended on a radiolucent hand table.
- Tourniquet: A pneumatic upper arm tourniquet is essential. Exsanguination should be performed carefully. In cases of suspected malignant transformation, exsanguination with an Esmarch bandage is contraindicated; instead, the arm should be elevated for 3 minutes prior to tourniquet inflation to prevent tumor embolization.
- Instrumentation: Standard hand trays must be supplemented with high-speed burrs, sharp drill bits (multiple spares, as sclerotic bone dulls bits rapidly), and robust fixation systems (locking plates).
SURGICAL APPROACHES AND TECHNIQUES
Technique 1: Open Reduction and Internal Fixation (ORIF) of a Pagetic Metacarpal Fracture
Fractures in pagetic bone are notoriously difficult to fix due to the brittle nature of the bone and the obliterated medullary canal.
Step 1: Surgical Approach
* Make a longitudinal dorsal incision centered over the fractured metacarpal.
* Dissect through the subcutaneous tissue, taking care to protect the dorsal sensory branches of the radial or ulnar nerves.
* Incise the extensor paratenon longitudinally. Retract the extensor tendon laterally or medially, depending on the fracture geometry.
* Incise the periosteum longitudinally. Note: Periosteal stripping should be kept to an absolute minimum to preserve the already compromised blood supply to the pagetic bone.
Step 2: Fracture Reduction
* Pagetic fractures are often transverse. Use pointed reduction forceps to achieve anatomic alignment.
* Due to the sclerotic nature of the bone, standard reduction techniques relying on cortical elasticity will fail. The bone will not "flex" into place; it must be perfectly aligned.
Step 3: Hardware Selection and Application
* Plate Selection: A low-profile locking compression plate (LCP) is highly recommended. Standard non-locking screws rely on friction against the bone, which can easily strip in the disorganized pagetic cortex. Locking screws provide a fixed-angle construct.
* Drilling: This is the most critical step. The sclerotic bone is exceptionally hard.
* Use sharp, new drill bits.
* Drill at a slow speed with continuous saline irrigation to prevent thermal necrosis of the bone. Thermal necrosis will inevitably lead to aseptic loosening and non-union.
* Clear the drill flutes frequently.
* Tapping: The bone must be tapped before screw insertion. Attempting to insert self-tapping screws into sclerotic pagetic bone will result in screw head stripping or shaft breakage.
* Fixation: Apply the plate dorsally. Ensure at least three bicortical locking screws are placed proximal and distal to the fracture site.
Step 4: Closure
* Repair the periosteum if possible.
* Allow the extensor tendon to fall back into its anatomic position.
* Close the skin with non-absorbable sutures.
Technique 2: Corrective Osteotomy for Severe Fusiform Deformity
In cases where the fusiform enlargement and bowing of the metacarpal severely restrict the motion of adjacent digits, a corrective osteotomy may be indicated.
Step 1: Approach and Exposure
* Utilize the same dorsal approach as described above.
* Expose the apex of the deformity.
Step 2: The Osteotomy
* Do not use an osteotome, as the brittle pagetic bone will shatter, propagating uncontrolled fracture lines.
* Use an oscillating saw with continuous saline irrigation to perform a closing wedge osteotomy at the apex of the deformity.
* Remove the wedge of sclerotic bone.
Step 3: Fixation and Grafting
* Reduce the osteotomy to correct the bowing.
* Fixate the osteotomy using a dorsal locking plate, adhering strictly to the slow-drilling and tapping principles outlined above.
* Because pagetic bone has poor healing potential, autologous cancellous bone graft (harvested from the distal radius) should be packed into the osteotomy site to stimulate union.
Technique 3: Management of Malignant Transformation (Pagetoid Sarcoma)
Malignant degeneration occurs in approximately 1% of patients with Paget disease, most commonly osteosarcoma. In the hand, this presents as rapid swelling, intractable pain, and cortical destruction.
Step 1: Biopsy
* A core needle biopsy or incisional biopsy must be performed first to confirm the histologic diagnosis. The biopsy tract must be placed in line with the planned definitive resection.
Step 2: Resection (Ray Amputation vs. Limb Salvage)
* Ray Amputation: For aggressive sarcomas of the metacarpals or phalanges, a radical ray amputation (removal of the digit and its corresponding metacarpal) is often the most oncologically sound procedure, providing wide margins.
* Limb Salvage: As described by Leit and Tomaino, limb salvage in the upper extremity requires meticulous preoperative staging (MRI, chest CT). If the tumor is localized to a single metacarpal without neurovascular encasement, a wide en bloc resection can be performed.
* Reconstruction: Following wide resection, the skeletal defect can be reconstructed using a free vascularized bone transfer (e.g., fibula or medial femoral condyle), as detailed by Murray. Vascularized grafts are superior to non-vascularized allografts in this setting due to the poor healing environment of the surrounding pagetic tissue and the potential need for adjuvant radiation or chemotherapy.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The postoperative management of the pagetic hand requires a delicate balance between protecting the fragile fixation and preventing stiffness.
- Immobilization: The hand is placed in a bulky Jones dressing with a volar intrinsic-plus splint (wrist at 30 degrees extension, MCP joints at 70-90 degrees flexion, IP joints fully extended) for the first 10-14 days.
- Wound Care: Sutures are removed at 2 weeks.
- Rehabilitation: Once the soft tissues have healed, active range of motion (AROM) of the digits is initiated under the guidance of a certified hand therapist. Passive range of motion (PROM) and dynamic splinting should be delayed until radiographic evidence of early union is observed, typically at 6-8 weeks.
- Medical Management: Postoperative continuation of bisphosphonate therapy is crucial. Collaboration with an endocrinologist or rheumatologist ensures optimal suppression of aberrant bone turnover, which aids in hardware integration and reduces the risk of hardware failure.
COMPLICATIONS AND PITFALLS
Surgeons operating on pagetic bone in the upper extremity must be prepared for a higher complication rate compared to normal bone:
- Delayed Union and Non-union: The disorganized architecture of pagetic bone inherently impairs the normal fracture healing cascade. Prolonged immobilization or the addition of bone stimulators may be required.
- Hardware Failure: Screw pull-out or plate breakage is common if locking technology is not utilized or if thermal necrosis occurs during drilling.
- Intraoperative Hemorrhage: Operating during the active mixed phase can result in significant blood loss. Preoperative medical suppression is the best preventative strategy.
- Infection: The bulky nature of the enlarged bone can lead to tight skin closures, increasing the risk of wound dehiscence and subsequent deep space infection.
- Missed Malignancy: A sudden change in pain quality or rapid expansion of a previously stable pagetic lesion must be treated as a sarcoma until proven otherwise. Failure to biopsy a suspicious lesion can lead to catastrophic oncologic outcomes.
CONCLUSION
Paget disease of the hand is a rare clinical entity that demands a high index of suspicion for accurate diagnosis. While the classic sclerotic, fusiform enlargement on radiographs is diagnostic, the orthopedic surgeon must remain vigilant for complications such as pathologic fractures and malignant transformation. When surgical intervention is required, meticulous preoperative planning, respect for the compromised biomechanics of pagetic bone, and the use of modern locking fixation techniques are paramount to achieving successful outcomes and preserving hand function.
You Might Also Like
