Arthroscopic Meniscoplasty for Discoid Lateral Meniscus: A Masterclass
Key Takeaway
Join us in the OR for an immersive masterclass on arthroscopic meniscoplasty for discoid lateral meniscus. We'll meticulously detail patient positioning, portal placement, precise saucerization techniques, and stabilization strategies for unstable variants. Learn to manage critical anatomy, avoid pitfalls, and optimize patient outcomes, ensuring a comprehensive understanding of this challenging pediatric procedure.
Comprehensive Introduction and Patho-Epidemiology
The discoid lateral meniscus represents a fascinating and often challenging intra-articular pathology that demands a precise, nuanced approach from the orthopedic surgeon. Unlike the standard meniscal tear encountered in routine sports medicine practice, the discoid meniscus is a morphological anomaly characterized by an abnormal thickening and an extended footprint over the lateral tibial plateau. Instead of the typical, biomechanically efficient crescent shape that facilitates optimal load distribution and joint congruence, it presents as a dense, disc-like structure. This anomalous morphology fundamentally alters the kinematics of the lateral compartment, predisposing the tissue to intrasubstance degeneration, complex tear patterns, and subsequent mechanical symptoms. Understanding its unique characteristics is paramount before one even considers making a portal incision.
Epidemiologically, the discoid meniscus is an anomaly predominantly affecting the lateral compartment, with over 99% of documented cases occurring on the lateral side of the knee. The overall incidence reported in the literature varies widely, ranging from 1% to 15% within the general population, with higher prevalences frequently noted in Asian demographics. A critical clinical pearl to retain is the high rate of bilaterality; approximately 10% to 20% of children and adolescents diagnosed with a symptomatic discoid meniscus will present with or eventually develop bilateral involvement. Therefore, a comprehensive diagnostic workup must always include a thorough clinical evaluation of the contralateral knee, even in the absence of overt presenting symptoms.
The pathogenesis of the discoid meniscus has been a subject of historical debate, primarily divided between congenital and developmental theories. Historically, Smillie proposed that the discoid shape was a result of a failure of normal central resorption during embryological development. However, subsequent anatomical studies have failed to identify discoid menisci in fetal deaths or stillborns at various stages of gestation, heavily suggesting that it is not simply a failure of regression. Modern consensus leans toward an abnormal developmental process, potentially driven by altered mechanical forces or hypermobility (as proposed by Kaplan), which leads to the progressive hypertrophy and morphological alteration of the meniscus during early childhood weight-bearing.
The natural history of a discoid meniscus is highly variable. While discoid menisci have been found incidentally as asymptomatic variants in elderly individuals, clinical symptoms typically manifest in the late first or early second decade of life. The classic presentation involves a pediatric or adolescent patient reporting a distinct, often audible, catch or "clunk" on the lateral aspect of the knee during flexion-extension arcs. This is frequently termed "snapping knee syndrome." Symptoms may progress from painless snapping to painful mechanical locking, where the hypermobile and thickened meniscus becomes incarcerated within the joint space, requiring physical manipulation for reduction. Chronic impingement and recurrent microtrauma inevitably lead to intrasubstance tearing, precipitating effusions and a painful loss of terminal extension.
Detailed Surgical Anatomy and Biomechanics
To master the surgical management of this condition, one must possess an exhaustive understanding of both normal and anomalous meniscal anatomy. A normal meniscus is composed primarily of Type I collagen, with fibers arranged in a highly organized circumferential pattern to resist hoop stresses, interspersed with radial tie fibers that prevent longitudinal splitting. In a discoid meniscus, this microstructural architecture is profoundly disorganized. Histological analyses reveal a chaotic arrangement of collagen fibers, decreased vascularity, and widespread areas of mucoid degeneration. This intrinsic structural inferiority renders the discoid meniscus highly susceptible to horizontal cleavage tears and complex, multi-planar failure under normal physiologic loads.
The morphological variations of the discoid meniscus are universally categorized using the Watanabe Classification system, which describes three primary types. The Complete type is characterized by a massive meniscal body that covers the entirety of the lateral tibial plateau, extending from the lateral capsule to the intercondylar eminence. The Incomplete variant is smaller, covering a partial aspect of the lateral compartment, but still exhibiting abnormal thickness and a wider-than-normal footprint compared to a standard crescentic meniscus. Both complete and incomplete types generally possess normal peripheral capsular attachments, making them relatively stable unless a superimposed tear occurs.
The third variant, the Wrisberg Type, is anatomically and clinically the most critical. It can present with either complete or incomplete compartment coverage, but its defining, pathological characteristic is the absolute absence of normal posterior peripheral attachments. Specifically, the posterior meniscotibial (coronary) ligaments are congenitally absent. The posterior horn of the meniscus is tethered solely by the meniscofemoral ligament of Wrisberg, which attaches to the medial femoral condyle. This inherent lack of stable peripheral fixation makes the Wrisberg type intrinsically hypermobile. During knee flexion, the medial femoral condyle pulls the unanchored posterior horn anteriorly and medially into the intercondylar notch, resulting in the classic, dramatic "clunk" and severe mechanical locking symptoms.
Biomechanically, the lateral compartment of the knee relies heavily on the meniscus for load transmission, shock absorption, and secondary stabilization. The convex-on-convex articulation of the lateral femoral condyle and lateral tibial plateau dictates that the lateral meniscus carries up to 70% of the compartment's load. A discoid meniscus disrupts this delicate equilibrium. Its abnormal thickness and disorganized collagen matrix fail to effectively dissipate hoop stresses. Furthermore, the hypermobility inherent in the Wrisberg variant, or secondary to tears in complete/incomplete variants, leads to abnormal shear forces across the articular cartilage. Over time, this altered kinematic profile accelerates chondral wear, predisposing the young patient to early-onset osteoarthritis if left unaddressed or if managed with overly aggressive total meniscectomy.
Exhaustive Indications and Contraindications
The paradigm for treating discoid lateral menisci has shifted dramatically over the past few decades. Historically, the standard of care was a total meniscectomy, which predictably led to devastating, rapid-onset lateral compartment osteoarthritis in young patients. Today, the fundamental philosophy is tissue preservation. The overarching goal is to relieve mechanical symptoms and prevent further cartilage degradation while retaining a stable, functional peripheral meniscal rim. It is a cardinal rule of pediatric orthopedics that an asymptomatic discoid meniscus, discovered incidentally on MRI for an unrelated issue, should be left strictly alone. Prophylactic saucerization is not indicated and carries unnecessary surgical risks.
Surgical intervention is explicitly indicated when a patient presents with a symptomatic discoid meniscus that has failed a diligent course of nonoperative management. Nonoperative modalities include activity modification, targeted physical therapy focusing on quadriceps and hamstring strengthening, and judicious use of NSAIDs for symptomatic relief. If the patient experiences recurrent mechanical locking, persistent loss of range of motion (particularly an extension deficit), intractable joint line pain, or recurrent effusions, surgical meniscoplasty is warranted. Furthermore, the presence of a highly unstable Wrisberg variant, characterized by severe "snapping" and functional disability, is a strong indication for prompt surgical stabilization and reshaping to prevent catastrophic tearing of the anomalous tissue.
Contraindications to arthroscopic meniscoplasty must be carefully weighed. Absolute contraindications are rare but include active intra-articular or periarticular infections, which must be eradicated prior to any elective joint surgery. Relative contraindications require nuanced clinical judgment. In older adult patients who present with a symptomatic discoid meniscus but also exhibit advanced, bone-on-bone lateral compartment osteoarthritis (Kellgren-Lawrence Grade 3 or 4), a simple meniscoplasty is unlikely to provide durable symptom relief. In such cases, the primary pain generator is osteoarthritic, and the patient may require realignment osteotomy or arthroplasty, depending on age and activity level.
| Category | Indications for Arthroscopic Meniscoplasty | Contraindications for Arthroscopic Meniscoplasty |
|---|---|---|
| Clinical Symptoms | Recurrent mechanical locking or catching; "Snapping knee" | Asymptomatic incidental finding |
| Pain & Function | Intractable lateral joint line pain; Persistent loss of motion | Mild, intermittent pain manageable with NSAIDs |
| Pathology | MRI-confirmed symptomatic tear in a discoid meniscus | Advanced lateral compartment osteoarthritis (Relative) |
| Stability | Unstable Wrisberg variant with functional impairment | Active intra-articular or local skin infection (Absolute) |
| Conservative Tx | Failure of a 6-12 week non-operative rehabilitation program | Patient non-compliance with post-operative restrictions |
Before committing to surgical intervention, the surgeon must exhaustively rule out other pathologies within the differential diagnosis. A meniscal cyst, often associated with horizontal cleavage tears, can present with a palpable lateral mass and joint line pain. A standard tear in a non-discoid meniscus must be differentiated via MRI. Anterior cruciate ligament (ACL) tears can cause giving-way episodes mimicking meniscal instability. Osteochondritis dissecans (OCD) of the lateral femoral condyle can cause effusions and mechanical symptoms. Finally, patellofemoral instability or subluxation, highly prevalent in the pediatric and adolescent population, can easily be misdiagnosed as lateral compartment snapping if a meticulous physical examination is not performed.
Pre-Operative Planning, Templating, and Patient Positioning
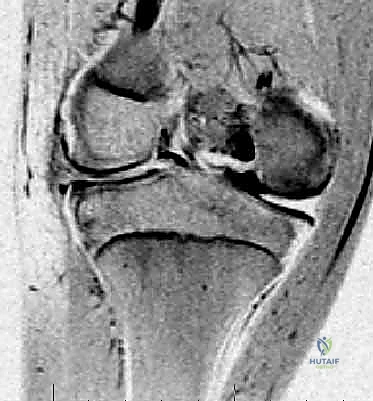
Meticulous preoperative planning is the absolute cornerstone of a successful outcome in discoid meniscus surgery. This begins with a rigorous clinical and radiographic evaluation. On physical examination, the surgeon must assess for a hypermobile lateral meniscus, noting any palpable, audible, or visually apparent snapping during the flexion-extension arc. The McMurray test is invaluable; a positive test reproduces pain and a distinct clunk, while an equivocal test may produce a clunk without pain, which is common in un-torn but hypermobile discoid menisci. Standard weight-bearing radiographs (AP, lateral, Rosenberg, and Merchant views) should be scrutinized for indirect signs of a discoid meniscus, such as widening of the lateral joint space, squaring of the lateral femoral condyle, and cupping of the lateral tibial plateau.
Magnetic Resonance Imaging (MRI) is the gold standard for definitive preoperative templating. The surgeon must personally review the sequences, not merely rely on the radiological report. On sagittal views, a normal meniscus is seen as a "bowtie" on two consecutive 3-mm slices. A discoid meniscus is diagnosed when the bowtie sign persists on three or more consecutive slices. On coronal views, a meniscal width exceeding 14 to 15 mm, or extending into the intercondylar notch, confirms the diagnosis. Crucially, the MRI must be evaluated for intrasubstance signal changes indicating mucoid degeneration or frank tearing, and the posterior capsular attachments must be scrutinized to anticipate a Wrisberg variant.
Once the patient is transported to the operating theater and anesthetized, a comprehensive examination under anesthesia (EUA) is mandatory. Without the confounding variables of patient guarding, apprehension, or pain, the surgeon can accurately assess the true extent of lateral meniscal instability and passive range of motion. A definitive McMurray test under anesthesia often reveals profound hypermobility that was masked in the clinic. This EUA sets the baseline for the intraoperative decision-making process, particularly regarding the necessity of peripheral stabilization in addition to saucerization.
Patient positioning must be executed flawlessly to ensure optimal visualization and instrument maneuverability. The patient is placed supine on the operating table. A pneumatic tourniquet is meticulously applied to the proximal thigh of the operative leg over adequate padding. A standard rigid leg holder is positioned over the tourniquet to secure the thigh. Crucially, the foot of the operating table is dropped or flexed 90 degrees. This allows both legs to hang freely, enabling the operative knee to be manipulated into deep flexion. The contralateral leg is well-padded and secured out of the surgical field. This setup allows the surgeon to easily place the operative leg into the "figure-4" position, applying a varus force and internal rotation to open the lateral compartment, which is absolutely critical for accessing the posterior horn of the discoid meniscus.
Step-by-Step Surgical Approach and Fixation Technique
The intraoperative execution of an arthroscopic meniscoplasty requires patience, superior spatial awareness, and a mastery of arthroscopic instrumentation. We begin by establishing standard arthroscopic portals using a No. 11 blade. The inferolateral parapatellar portal is established first, serving as the primary viewing portal. The inferomedial parapatellar portal is then created under direct intra-articular visualization using a spinal needle to ensure the optimal trajectory, serving as the primary working portal. A lateral suprapatellar pouch portal is highly recommended for dedicated outflow, which maintains a clear visual field by constantly flushing debris and blood while regulating intra-articular hydrostatic pressure.
Once portals are established, a systematic diagnostic arthroscopy is performed, sweeping through the patellofemoral joint, medial compartment, and intercondylar notch before focusing on the lateral compartment. The knee is placed in the figure-4 position to maximize lateral joint space opening. Using a calibrated arthroscopic probe, the discoid meniscus is meticulously evaluated. The surgeon must probe sequentially over and under the posterior horn, gently pulling it anteriorly. If the posterior horn displaces more than 40% to 50% anteriorly into the joint space, a Wrisberg variant or severe peripheral detachment is confirmed, mandating peripheral suture fixation in addition to the saucerization.
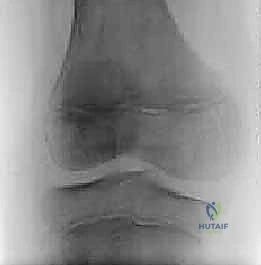
As seen in the intraoperative image above, a complete discoid lateral meniscus can be clearly visualized extending deep into the intercondylar notch. The central portion often exhibits fibrillations or complex tearing due to chronic mechanical impingement. The goal of saucerization is to reshape this massive structure into a functional, crescentic meniscus, preserving a peripheral rim of approximately 6 to 8 mm. Resection begins at the free edge of the meniscus within the notch.

Initiation of the saucerization process, demonstrated here, requires precise instrumentation. I prefer to use a straight or slightly angled arthroscopic basket punch to make the initial coronal incision, working from the notch laterally toward the body of the meniscus. This establishes the new "free edge." The resection is then carried out in a piecemeal fashion. A combination of specialized baskets—including up-biters, back-biters, and 90-degree rotary punches—are utilized to resect the excess anterior and posterior horn tissue. The surgeon must constantly reference the popliteal hiatus and the lateral capsule to ensure the resection does not inadvertently violate the peripheral rim.

Throughout the resection, the surgeon must periodically probe the remaining tissue and adjacent structures, as shown above, assessing the depth of any associated tears and ensuring the ACL and articular cartilage remain pristine. Once the desired crescent shape is achieved, attention turns to the thickness of the remnant. A discoid meniscus is pathologically thick; leaving a thick, blocky remnant will result in continued impingement and symptom recurrence.
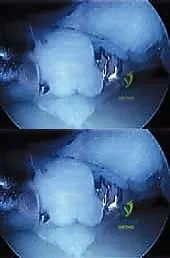
The remnant must be carefully thinned to approximate normal meniscal anatomy. This is accomplished using an aggressive oscillating shaver or a motorized burr, carefully contouring the superior and inferior surfaces of the meniscal rim. The surgeon must exercise extreme caution to avoid iatrogenic damage to the underlying lateral tibial plateau cartilage during this step.

Finally, if a Wrisberg variant was identified, or if the saucerization process has unmasked peripheral instability, the remnant must be stabilized. This is achieved using all-inside meniscal repair devices or traditional inside-out suturing techniques. Vertical mattress sutures are placed sequentially along the posterior and middle thirds of the meniscus, firmly anchoring the reshaped rim to the posterior capsule. The final construct, as visualized above, should resemble a stable, contoured, crescentic meniscus that translates physiologically with knee motion without snapping or locking.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, arthroscopic meniscoplasty for discoid meniscus carries inherent risks and potential complications. Intraoperative complications are primarily related to iatrogenic injury. The most common is scuffing or gouging of the lateral femoral condyle or tibial plateau articular cartilage, which can occur when maneuvering rigid basket punches or shavers within a tight lateral compartment. Over-resection is another critical error; aggressively removing too much tissue effectively results in a subtotal or total meniscectomy, destroying the load-bearing capacity of the lateral compartment and guaranteeing early osteoarthritic progression. Furthermore, if an inside-out repair technique is utilized for stabilization, the common peroneal nerve is at risk and must be protected via a meticulous lateral approach and retractor placement.
Postoperative complications largely center around recurrent symptoms and tissue failure. Because the retained meniscal rim of a discoid meniscus remains histologically abnormal (mucoid degeneration, disorganized collagen), it is inherently weaker than a normal meniscus. Consequently, the incidence of re-tearing the saucerized remnant is notable, reported in the literature to be between 10% and 20% within the first five years post-surgery. Patients may present with recurrent effusions, joint line pain, or new mechanical symptoms. Additionally, failure to recognize and stabilize a Wrisberg variant during the index procedure will inevitably lead to continued snapping and rapid failure of the saucerized rim.
Management of these complications requires a tiered approach. Minor recurrent effusions or mild pain can often be managed with a return to conservative modalities, including intra-articular corticosteroid injections and physical therapy. However, a symptomatic re-tear of the meniscal remnant typically necessitates a revision arthroscopy. During revision, the surgeon must carefully assess the remaining tissue; if a repairable tear is present, revision repair is attempted. If the tissue is irreparably macerated, further resection may be required.
| Complication | Estimated Incidence | Prevention Strategy | Salvage / Management Strategy |
|---|---|---|---|
| Iatrogenic Cartilage Injury | 2% - 5% | Use figure-4 position; Avoid levering instruments; Use smaller diameter scopes if necessary. | Chondroplasty; Microfracture for full-thickness defects. |
| Remnant Re-tear | 10% - 20% | Preserve adequate rim width (6-8mm); Avoid over-thinning; Strict adherence to rehab protocol. | Revision arthroscopy: partial resection or revision repair. |
| Persistent Instability | 5% - 10% | Rigorous intraoperative probing; Always repair Wrisberg variants or detached peripheral rims. | Revision arthroscopy with peripheral suture stabilization. |
| Early Osteoarthritis | 15% - 30% (Long-term) | Avoid total meniscectomy; Maximize tissue preservation; Correct coronal alignment if needed. | Conservative management; Meniscal Allograft Transplant (MAT); Osteotomy. |
| Peroneal Nerve Injury | < 1% | Meticulous dissection and retractor placement during inside-out meniscal repair. | Observation (often neuropraxia); Neurolysis if persistent. |
In the most severe salvage scenarios—where a young patient has undergone a functional total meniscectomy due to massive, irreparable tearing of a discoid meniscus and subsequently develops debilitating lateral compartment pain and early chondral wear—Meniscal Allograft Transplantation (MAT) becomes the treatment of choice. MAT aims to restore the biomechanical function of the lateral compartment, alleviate pain, and potentially delay the progression of osteoarthritis. However, MAT is a technically demanding procedure with its own set of strict indications, requiring normal coronal alignment and stable ligamentous structures to be successful.
Phased Post-Operative Rehabilitation Protocols
The postoperative rehabilitation protocol following a discoid meniscoplasty is heavily dictated by the exact nature of the surgical intervention. If a simple saucerization was performed without any peripheral repair, the rehabilitation can be relatively accelerated. However, if peripheral suture stabilization (repair) was required, the protocol must be strictly conservative to protect the healing meniscal capsular junction. The following outlines a comprehensive, phased approach for a patient who has undergone saucerization with concurrent peripheral stabilization, representing the most cautious and protective pathway.
Phase I: Maximum Protection Phase (Weeks 0-4)
The primary goals of this initial phase are to protect the surgical repair, control post-operative inflammation and effusion, and re-establish voluntary quadriceps control. The patient is typically placed in a hinged knee brace locked in full extension for weight-bearing. Weight-bearing status is restricted to toe-touch (TTWB) or partial weight-bearing (PWB) with crutches to minimize compressive and shear forces on the healing meniscus. Range of motion (ROM) is initiated immediately but is strictly limited to 0 to 90 degrees of flexion. Flexion past 90 degrees places excessive stress on the posterior horn repair. Therapeutic exercises focus on isometric quadriceps sets, straight leg raises (in the brace), and patellar mobilizations to prevent arthrofibrosis.
Phase II: Moderate Protection and ROM Restoration (Weeks 4-8)
During this phase, the focus shifts to restoring full, painless range of motion and normalizing the gait pattern. The hinged knee brace is progressively unlocked, and the patient is transitioned to full weight-bearing (FWB) as tolerated, weaning off crutches. ROM exercises are advanced beyond 90 degrees, aiming for full, symmetrical flexion by week 8. Closed kinetic chain exercises are introduced, including mini-squats (limited to 60 degrees of flexion), leg presses, and stationary cycling. Proprioceptive training and balance exercises are also initiated to restore neuromuscular control of the lower extremity.
Phase III: Strengthening and Endurance Phase (Weeks 8-12)
With full ROM achieved and the repair biologically stable, the rehabilitation program intensifies to rebuild muscular strength and endurance. The brace is discontinued. Isotonic and isokinetic strengthening of the quadriceps, hamstrings, and hip musculature is aggressively pursued. Advanced closed kinetic chain exercises, such as lunges and step-ups, are incorporated. Cardiovascular endurance training is expanded to include elliptical machines and swimming (straight-leg kicking only; breaststroke whip kicks are strictly prohibited as they generate massive meniscal shear forces).
Phase IV: Return to Sport and Advanced Activity (Months 3-6+)
The final phase bridges the gap between clinical rehabilitation and a safe return to athletic competition or heavy physical labor. Progression into Phase IV requires an effusion-free knee, full ROM, and isokinetic strength testing demonstrating at least 85% to 90% symmetry compared to the contralateral limb. Agility drills, plyometrics, and sport-specific functional training are progressively integrated. The patient is cleared for full, unrestricted activity only when they can confidently perform cutting, pivoting, and explosive movements without pain, apprehension, or biomechanical compensation. Long-term follow-up is essential, as these patients remain at a higher lifetime risk for lateral compartment degenerative changes.
Summary of Landmark Literature and Clinical Guidelines
The evolution of surgical management for the discoid lateral meniscus is deeply rooted in historical literature and continuous clinical refinement. The foundational understanding of this pathology dates back to the mid-20th century. Smillie’s seminal work in 1948 detailed the morphological variations and hypothesized the embryological failure of central resorption, a theory that dominated orthopedic thought for decades. Subsequently, Kaplan’s anatomical studies in 1957 challenged this, identifying the absence of the posterior meniscotibial ligaments and the presence of the meniscofemoral ligament as the primary drivers of hypermobility and subsequent hypertrophy, laying the groundwork for understanding the Wrisberg variant.
The definitive classification system universally utilized today was published by Watanabe in 1979. His categorization into Complete, Incomplete, and Wrisberg types remains the gold standard for preoperative templating and intraoperative decision-making. Watanabe’s work was instrumental in standardizing the nomenclature, allowing for accurate comparison of outcomes across different surgical cohorts.
Modern clinical guidelines and outcome studies have unequivocally driven the paradigm shift from total meniscectomy to tissue-preserving saucerization. Landmark studies by Ahn et al. and Kocher et al. in the early 2000s demonstrated that arthroscopic saucerization yields good to excellent short- to mid-term clinical outcomes, with significant reductions in pain and mechanical symptoms. Crucially, these studies emphasized that failure to recognize and concurrently repair peripheral instability (the Wrisberg variant) during saucerization is the primary cause of early surgical failure and persistent snapping.
Current literature focuses heavily on long-term chondroprotective efficacy. While saucerization is vastly superior to total meniscectomy, long-term follow-up studies (10 to 15 years post-operatively) indicate that the retained discoid remnant does not function identically to a normal meniscus. Mild to moderate radiographic progression of lateral compartment osteoarthritis is still observed in a significant subset of patients. Therefore, contemporary clinical guidelines stress the importance of conservative resection—leaving an 8mm rim whenever possible—and meticulous peripheral stabilization. Future directions in the field are actively exploring the role of biological augmentation (such as PRP or bone marrow aspirate concentrate) during meniscoplasty to enhance the healing potential of the abnormal meniscal tissue, aiming to further improve the long-term survivorship of the lateral compartment.
