Arthroscopic Lateral Retinacular Release: An Intraoperative Masterclass
Key Takeaway
Join us in the OR for an arthroscopic lateral retinacular release. This masterclass details the procedure for excessive lateral pressure syndrome, covering crucial anatomy, patient positioning, meticulous surgical steps, and critical intraoperative decision-making. Learn to identify and manage potential complications, ensuring optimal outcomes for patients suffering from chronic patellofemoral pain and lateral patellar tilt.
Alright team, let's gather around. Today, we're tackling a common yet often misunderstood condition: Excessive Lateral Pressure Syndrome (ELPS), and we'll be performing an Arthroscopic Lateral Retinacular Release. This isn't a procedure for patellar instability, but rather for chronic anterior knee pain stemming from a pathologically tight lateral retinaculum. Understanding the nuances here is paramount to achieving excellent patient outcomes and avoiding iatrogenic complications.
Understanding the Diagnosis: ELPS
Our patient today presents with classic symptoms: insidious onset of anterior knee pain, exacerbated by activities like prolonged sitting, stair climbing, and general activity. While some may report a history of trauma, the key differentiator for ELPS is the absence of true patellar instability. This pain arises from the lateral compression of the patella against the femoral trochlea due to an unyielding lateral soft tissue restraint.
Patient History and Physical Findings
When evaluating these patients preoperatively, we're looking for a specific constellation of findings:
- Pain Characteristics: Activity-related, often worse with knee flexion activities and sustained flexion.
- Absence of Instability: Unlike true patellar instability, there's no history of the patella "giving way" or dislocating.
- Effusion: While not always present, an effusion might suggest underlying articular cartilage damage, which can be a consequence of chronic ELPS.
- Patellar Tracking (J-sign): Observe the patella as the knee flexes and extends. A "J-sign" – where the patella tracks laterally in extension and then suddenly "jumps" into the trochlear groove around 20-30 degrees of flexion – can indicate lateral tightness, though it's not pathognomonic.
- Patellar Tilt Test: This is a crucial diagnostic maneuver. With the knee fully extended, attempt to tilt the lateral facet of the patella medially. If you cannot tilt it to a neutral or slightly positive angle, the lateral retinaculum is abnormally tight. This is a primary indicator for our procedure today.
- Patellar Glide Test: Assess the lateral excursion of the patella. Up to two quadrants of lateral glide is generally considered normal. Excessive lateral translation, especially compared to the contralateral side, might suggest laxity, but in ELPS, the tightness often restricts this glide, or the patella is already sitting laterally due to the tight retinaculum.
- Patellar Apprehension Test: This test typically elicits apprehension in patients with patellar instability. In ELPS, it should be negative.
- Quadriceps Tightness: Often associated with patellofemoral pain, so assess rectus femoris and hamstring flexibility.
- Patellar Grind Test: Pain on compression of the patella into the trochlea while moving it can indicate patellofemoral arthritis, which can be a sequela of ELPS.
- Q-angle: Measure the Q-angle (quadriceps angle) to assess for bony malalignment. An increased Q-angle can predispose to lateral tracking.
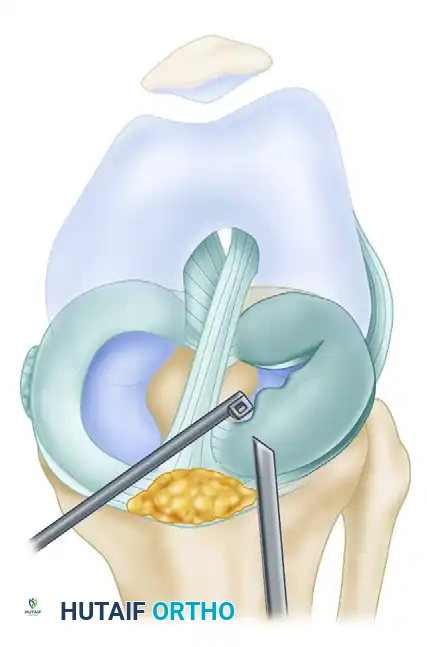
Surgical Anatomy: A Deeper Dive
Let's review the critical anatomy we'll encounter. The patellofemoral joint is a marvel of biomechanics, designed to allow the extensor mechanism to function efficiently.
- The Patella: The largest sesamoid bone, it acts as a fulcrum, increasing the lever arm of the quadriceps. Its posterior surface boasts the thickest articular cartilage in the body, a testament to the immense forces it withstands – up to 3 times body weight during stair climbing and 20 times during jumping.
- Patellar Tracking: As the knee flexes from full extension, the patella is drawn into the trochlear groove around 20 degrees. In full extension, the medial patellofemoral ligament (MPFL) is the primary static restraint against excessive lateral translation. In early flexion, the lateral trochlear ridge becomes the primary osseous restraint.
- The Lateral Retinaculum: This is our target. It's a complex fascial structure composed of several layers, including contributions from the vastus lateralis, iliotibial band, and deep transverse retinacular fibers. In ELPS, it's this structure, along with the lateral patellofemoral ligament, that becomes pathologically tight, constricting the patella laterally.
- Neurovascular Structures: This is where we must be vigilant. The superior lateral geniculate artery and vein run within the lateral retinaculum, often just superior to the lateral epicondyle. Injury to these vessels is a primary cause of hemarthrosis, the most common complication of this procedure. We'll meticulously identify and coagulate them if seen. The common peroneal nerve is more posterior and lateral, but general awareness of its course is always prudent around the knee.
Imaging and Other Diagnostic Studies
Radiographic evaluation is crucial for confirming the diagnosis and ruling out other pathologies.
- Standard Radiographs: We always obtain anteroposterior (AP), tunnel, Merchant (sunrise), and 30-degree lateral views. If arthritis is suspected, a posteroanterior (PA) flexed 45-degree view is added.
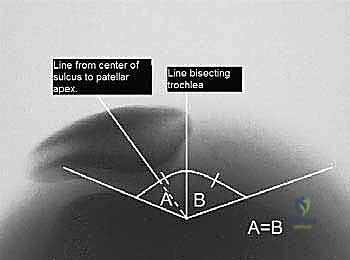
- Merchant View: This axial view is excellent for assessing lateral patellar subluxation. We measure the relationship of the patellar apex to a line bisecting the trochlear sulcus angle. If the patellar apex line is lateral to the trochlear line, the patella is subluxed laterally.

FIG 1 • A. Merchant radiograph of right knee showing measurement of lateral patellar subluxation.
* CT Scan: The gold standard for evaluating patellar tilt. An axial image is used to draw a line parallel to the posterior femoral condyles and compare it to a line along the lateral patellar facet. If these lines converge laterally, it indicates excessive lateral tilt.
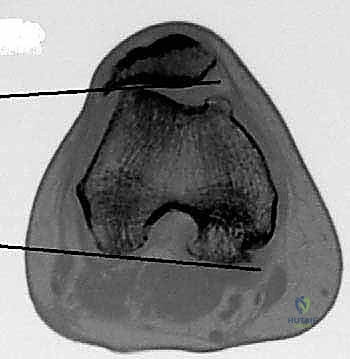
FIG 1 • B. Axial CT image of a right knee demonstrating how to measure patellar tilt.
* MRI Scan: Beneficial for assessing articular cartilage integrity, meniscal tears, and ligamentous pathology, which can often coexist. It can also demonstrate the extent of lateral retinacular thickening.
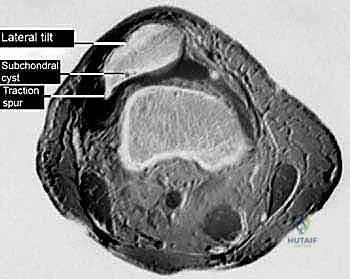
FIG 1 • C. Axial MRI scan of the right knee of a patient with excessive lateral pressure syndrome.
Preoperative Planning and Patient Positioning
Our patient has failed a comprehensive nonoperative regimen, including quadriceps stretching, strengthening, oral analgesics, and activity modification. This makes them an ideal candidate for arthroscopic lateral retinacular release.
Anesthetic Considerations
We'll use a general anesthetic for this case, often supplemented with a regional block (e.g., femoral nerve block or adductor canal block) for excellent postoperative pain control.
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Leg Support: The operative leg will be supported by a standard knee holder or a leg positioner, allowing full range of motion and easy access to all aspects of the knee joint. We want the leg free to move through flexion and extension to assess patellar tracking dynamically.
- Tourniquet Placement: A nonsterile pneumatic tourniquet is applied high on the thigh. We'll inflate this after our diagnostic arthroscopy.
- Examination Under Anesthesia (EUA): This is a critical step. Before incision, with the patient fully relaxed under anesthesia, we re-examine the knee. Assess the range of motion, patellar tilt, patellar subluxation, and ligamentous stability. Pay particular attention to patellar tracking as the knee is taken through a full ROM. Compare findings meticulously to the contralateral, non-operative knee. This confirms our diagnosis and helps us gauge the degree of tightness we need to address.
Step-by-Step Intraoperative Execution: The Operating Surgeon's Viewpoint
Alright, fellows, let's get scrubbed in. We've prepped and draped the leg in a sterile fashion.
Portal Placement
We'll establish our standard arthroscopic portals:
- Inferomedial Portal: This is our primary viewing portal. We'll make an incision approximately 1 cm medial to the patellar tendon and at the level of the inferior pole of the patella. This ensures we're well clear of the articular cartilage.
- Inferolateral Portal: This will be our working portal for the initial diagnostic arthroscopy and later for our coagulation device. It's placed approximately 1 cm lateral to the patellar tendon, again at the level of the inferior pole of the patella.
- Superolateral Inflow Portal: This portal is crucial for fluid inflow and also serves as a key landmark for the proximal extent of our release. It's established just lateral to the vastus lateralis obliquus (VLO) muscle belly, typically about 2-3 cm superior to the superolateral pole of the patella. This position ensures optimal fluid dynamics and allows clear visualization.
Diagnostic Arthroscopy
- Initial Survey: I'll insert the 30-degree arthroscope into the inferomedial portal. We'll systematically survey the entire knee joint, starting with the suprapatellar pouch, then moving to the medial and lateral gutters, the intercondylar notch, and finally, the patellofemoral joint itself.
- Concomitant Pathology: This initial diagnostic phase is absolutely critical. We're looking for any concomitant intra-articular pathology such as meniscal tears, articular cartilage lesions (especially on the patella and trochlea), and loose bodies. Any significant findings here must be addressed. Remember, a lateral release alone won't fix a large meniscal tear or a significant osteochondral defect.
- Posteromedial and Posterolateral Compartments: Using the Gillquist technique, we'll flex the knee and apply appropriate valgus or varus stress to open up these posterior compartments, allowing us to visualize the posterior horns of the menisci and the posteromedial and posterolateral capsules.
- Dynamic Patellofemoral Tracking: With the scope in the inferomedial portal, we'll cycle the knee through a range of motion, observing the patellar tracking in real-time. This helps us confirm the degree of lateral compression and how the patella engages the trochlea.
Preparing for the Release
- Exsanguination and Tourniquet Inflation: Once the diagnostic arthroscopy is complete and we've confirmed the indications for release, we'll exsanguinate the leg using an Esmarch bandage, wrapping it tightly from distal to proximal. Then, we'll inflate the tourniquet to a standard pressure, typically 250-300 mmHg, to create a bloodless field.
- Instrument Setup: Now, we'll switch our scope to the inferomedial portal. Our working instrument, a hooked electrocautery device, will be inserted through the inferolateral portal. This allows us to work directly on the lateral retinaculum under clear visualization.
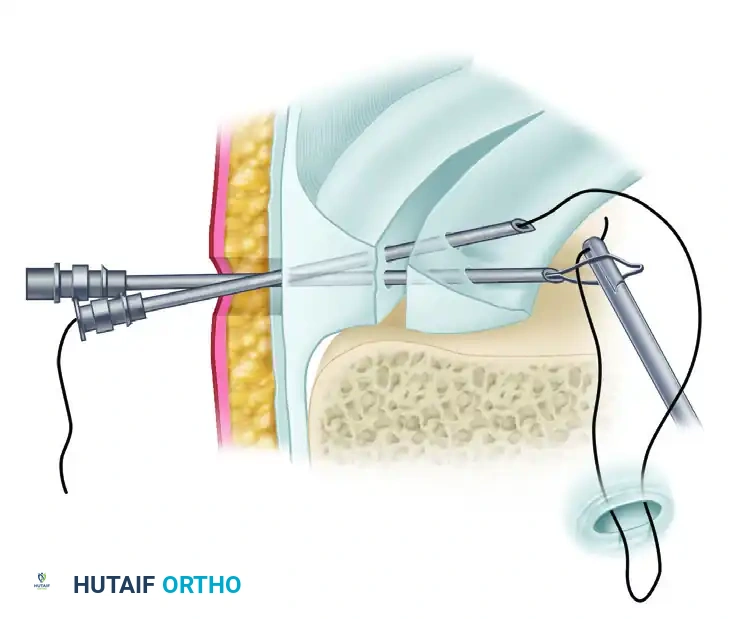
The Arthroscopic Lateral Retinacular Release
- Proximal Starting Point: We will begin the release just distal to our superolateral inflow cannula. This cannula serves as an excellent proximal landmark.
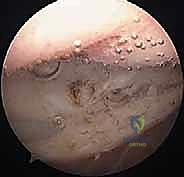
TECH FIG 1 • A. The proximal starting point for lateral retinacular release is just distal to the superolateral inflow cannula.
> **Surgical Warning:** Always maintain direct arthroscopic visualization. Never cut blindly. Your scope should always be directly visualizing the tip of your electrocautery device.
- Layered Dissection:
- Synovium: First, we'll use the electrocautery to incise the synovium overlying the lateral retinaculum. You'll see the delicate, often vascularized synovial layer part, exposing the underlying, denser retinacular tissue.
- Retinaculum: Once the synovium is cut, we'll meticulously address the underlying retinaculum. You'll feel a distinct, firm resistance as you pass the electrocautery through it. We'll make multiple passes, cutting through the tight fibers. The goal is a complete release of the restrictive bands.
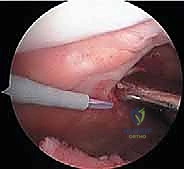
TECH FIG 1 • B. Arthroscopic view demonstrating successful release of the capsule and tight lateral retinaculum.
3. Distal Extent of Release: The release should extend distally down to the level of the inferolateral portal. This ensures adequate length of release to address the lateral compression.
> **Surgical Warning:** Exercise extreme caution to avoid cutting into the vastus lateralis muscle or its tendon. The vastus lateralis is a dynamic stabilizer of the patella, and injury can lead to weakness and potentially compromise the extensor mechanism. Stay superficial to the muscle fibers.
-
Hemostasis: As we perform the release, we'll be mindful of the superior lateral geniculate vessels. If these vessels are seen, we will aggressively coagulate them with the electrocautery to prevent postoperative bleeding and hemarthrosis.
💡 Pearls and Pitfalls: Hemostasis
- Vessel Identification: The superior lateral geniculate vessels are directly at risk. Look for them within the retinacular tissue, typically running horizontally.
- Proactive Coagulation: If you see a vessel, coagulate it thoroughly before cutting it.
- Tourniquet Deflation: A critical step for hemostasis is to gradually deflate the tourniquet before closing the portals. This allows you to identify any remaining bleeding vessels under normal perfusion and coagulate them. Don't rush this step.
- Postoperative Management: Use a cryotherapy device and a compression dressing postoperatively to further reduce the risk of hemarthrosis.
-
Assessing Adequacy of Release: Once we believe we've performed an adequate release, we'll re-assess patellar tilt. With the knee in full extension, I should now be able to tilt the patella 30 to 45 degrees medially. This is our intraoperative measure of success. If the tilt is still restricted, we may need to extend the release slightly, but always cautiously.
Surgical Warning: Avoid excessive lateral release! Overaggressive release can lead to iatrogenic medial patellar instability, a devastating complication that is often difficult to manage and can worsen symptoms. The goal is to achieve adequate tilt, not hypermobility.
-
Final Hemostasis and Closure: After confirming adequate release and meticulous hemostasis with the tourniquet deflated, we'll ensure all bleeding is controlled. We'll then close our portal sites with simple interrupted sutures or adhesive strips. A sterile compression dressing and a cryotherapy device will be applied immediately. In cases where significant bleeding was encountered, or if the patient has a coagulopathy, we may consider placing a drain, though it's not routinely necessary.
Postoperative Care and Rehabilitation
Postoperative care is as crucial as the surgery itself for a successful outcome.
- Immediate Postoperative Care:
- Compression Dressing and Cryotherapy: The compression dressing and cryotherapy device (e.g., continuous cold flow device) will remain in place for the first 24-48 hours to minimize swelling and reduce the risk of hemarthrosis.
- Weight Bearing: Patients are allowed to progress to weight-bearing as tolerated (WBAT) immediately. We encourage early mobilization.
- Crutches: Patients can discard crutches as soon as they are ambulating safely and comfortably, typically within a few days to a week.
- First Follow-up (1 Week Post-Op):
- We'll see the patient at 1 week post-surgery. At this visit, we'll assess knee motion, quadriceps function, and remove sutures.
- Physical Therapy: Formal physical therapy is often initiated at this point. The focus will be on:
- Restoring Range of Motion (ROM): Gentle flexion and extension exercises to prevent stiffness.
- Quadriceps Strengthening: Specific exercises targeting the vastus medialis obliquus (VMO) are emphasized to improve dynamic patellar stabilization. Straight leg raises, vastus medialis strengthening exercises (e.g., terminal knee extensions), and progressive resistance exercises are key.
- Patellar Mobilization: Patients are taught gentle patellar mobilization exercises to maintain mobility and prevent adhesions.
- Activity Progression: Gradual progression of activities, including low-impact exercises, leading towards a return to sport or desired activities.
- Long-Term Management:
- Patients continue with physical therapy for several weeks to months, depending on their progress.
- Return to sport typically occurs once strength and ROM are fully restored, and the patient is pain-free with activity-specific movements. This can range from 3-6 months.
Outcomes and Complications
Outcomes
Arthroscopic isolated lateral retinacular release has a reported success rate ranging from 70% to 93%, with many patients returning to their presymptomatic activity levels. It's important to remember that success rates are lower when the procedure is performed for instability alone or in the presence of advanced patellofemoral arthritis.
Complications
We must be aware of potential complications:
- Hemarthrosis: This is the most common complication. It manifests as acute swelling, pain, and restricted motion due to blood accumulating in the joint. Management typically involves aspiration of the hemarthrosis, continued compression, and cryotherapy. In severe or recurrent cases, a return to the operating room for arthroscopic washout and re-coagulation may be necessary.
- Infection: As with any surgical procedure, there's a risk of superficial or deep infection. Strict aseptic technique is paramount for prevention.
- Medial Instability from Overaggressive Release: This is perhaps the most challenging and devastating complication. If too much of the lateral retinaculum is released, the patella can become medially unstable.
- Diagnosis: Patients may report a sensation of lateral instability, but this is often a misperception. The patella sits in a medially subluxed position in early flexion and then "snaps" laterally as flexion continues. Clinically, you'll observe excessive medial patellar translation and tilt.
- Management: This is difficult. Incorrectly treating presumed lateral instability with a medial stabilization procedure (e.g., MPFL reconstruction) will worsen the symptoms. Management typically involves bracing, activity modification, and focused physical therapy to strengthen dynamic stabilizers. In severe, persistent cases, revision surgery to reconstruct the lateral restraints may be considered, but these are complex and less predictable.
- Quadriceps Tendon Rupture: A rare but severe complication, usually due to direct injury with the electrocautery or excessive tension during the procedure.
- Patella Baja: Lowering of the patella, which can result from scarring or contracture, particularly after thermal injury.
- Thermal Injury: Damage to articular cartilage or surrounding soft tissues from excessive heat generated by the electrocautery. Maintaining adequate fluid flow and avoiding direct contact with cartilage are key preventive measures.
- Arthrofibrosis: Excessive scar tissue formation within the joint, leading to stiffness and restricted range of motion. Early mobilization and physical therapy help prevent this.
💡 Pearls and Pitfalls: Landmarks Guiding Length
- Proximal Starting Point: The superolateral inflow cannula is your reliable guide for the most proximal aspect of the release. Start just distal to it.
- Distal Extent: The release should extend distally to the level of the inferolateral portal. This ensures you've addressed the entire length of the tight lateral retinaculum.
This procedure, when performed for the correct indications and with meticulous technique, can provide significant relief for patients suffering from ELPS. Always remember to prioritize careful patient selection, thorough anatomical understanding, and vigilance for potential complications. Let's proceed with caution and precision.
Additional Intraoperative Imaging & Surgical Steps
REFERENCES
-
Aderinto J, Cobb AG. Lateral release for patellofemoral arthritis. Arthroscopy 2002;18:399–403.
-
Aglietti P, Insall JN, Cerulli G. Patellar pain and incongruence. I: Measurements of incongruence. Clin Orthop Rel Res 1983;176: 217–224.
-
Aglietti P, Menchetti PPM. Biomechanics of the patellofemoral joint. In: Scuderi GR, ed. The Patella. New York: Springer-Verlag, 1995:25–48.
You Might Also Like