Hand And Wrist: And Emq Questio Review | Dr H...
00:00
Start Quiz
Question 1High Yield
A 46-year-old man has incomplete paraplegia after being involved in a motor vehicle accident. The CT scan shown in Figure 5 reveals marked canal compromise. What is the most appropriate management to improve neurologic status?
Explanation
According to a study by the Scoliosis Research Society, the use of anterior decompression is most predictable for improving neurologic status. This is particularly true of bowel and bladder functional loss. Laminectomy is contraindicated because it further destabilizes the spine. Posterior instrumentation and indirect reduction through distraction and ligamentotaxis only incompletely decompress the compromised canal and are successful only if performed within 48 hours of injury. While some improvement may occur with closed management, the amount of recovery is less than that achieved with surgical decompression. A posterior approach and instrumentation may be added to the anterior decompression based on the characteristics of associated injuries to the posterior element.
REFERENCES: Gertzbein SD: Scoliosis Research Society multicenter spine fracture study. Spine 1992;17:528-540.
Garfin SR, Vaccaro AR (eds): Orthopaedic Knowledge Update: Spine. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1997, pp 197-215.
Cammisa FP Jr, Eismont FJ, Green BA: Dural laceration occurring with burst fractures and associated laminar fractures. J Bone Joint Surg Am 1989;71:1044-1052.
REFERENCES: Gertzbein SD: Scoliosis Research Society multicenter spine fracture study. Spine 1992;17:528-540.
Garfin SR, Vaccaro AR (eds): Orthopaedic Knowledge Update: Spine. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1997, pp 197-215.
Cammisa FP Jr, Eismont FJ, Green BA: Dural laceration occurring with burst fractures and associated laminar fractures. J Bone Joint Surg Am 1989;71:1044-1052.
Question 2High Yield
-A 63-year-old woman with osteopenia is struck by a motor vehicle and sustains a Schatzker 2 (AO/OTA Type B) fracture of the lateral tibial plateau. She has
1.5 cm of joint depression and 7 mm of condylar widening. What is the most appropriate surgical fixation for this injury?
1.5 cm of joint depression and 7 mm of condylar widening. What is the most appropriate surgical fixation for this injury?
Explanation
_**RESPONSES FOR QUESTIONS 101 THROUGH 104**_
1. Open reduction and internal fixation with absolute stability
2. Open reduction and internal fixation with relative stability
3. Closed reduction with casting
4. Reamed locked intramedullary nailing
5. External fixation
_For each of the following fractures choose the best method for definitive fixation._
1. Open reduction and internal fixation with absolute stability
2. Open reduction and internal fixation with relative stability
3. Closed reduction with casting
4. Reamed locked intramedullary nailing
5. External fixation
_For each of the following fractures choose the best method for definitive fixation._
Question 3High Yield
A 26-year-old man underwent excision of a ganglion cyst of the tibiofibular joint 1 year ago. It has now recurred and is extremely symptomatic. Nonsurgical management has failed to provide relief. What type of surgery provides the most predictable results for this patient?
Explanation
DISCUSSION: Recurrence of a ganglion cyst of the tibiofibular joint is most successfully treated by proximal tibiofibular joint fusion. A repeat excision will most likely result in recurrence of the cyst. Total or partial excision may lead to instability of the posterolateral structures of the knee. Interpositional arthroplasty has not been proven to be effective for the treatment of recurrent ganglion cysts of the proximal tibiofibular joint.
REFERENCES: Miskovsky S, Kaeding C, Weis L: Proximal tibiofibular joint ganglion cysts: Excision, recurrence, and joint arthrodesis. Am J Sports Med 2004;32:1022-1028.
Vatansever A, Bal E, Okcu G: Ganglion cysts of the proximal tibiofibular joint review of literature with three case reports. Arch Orthop Trauma Surg 2006;126:637-640.
REFERENCES: Miskovsky S, Kaeding C, Weis L: Proximal tibiofibular joint ganglion cysts: Excision, recurrence, and joint arthrodesis. Am J Sports Med 2004;32:1022-1028.
Vatansever A, Bal E, Okcu G: Ganglion cysts of the proximal tibiofibular joint review of literature with three case reports. Arch Orthop Trauma Surg 2006;126:637-640.
Question 4High Yield
Figures 1 through 3 are the radiographs of a 12-year-old female soccer player, who presents with insidious onset of right knee swelling and pain with activity, including walking, over the last month. She has been placed on crutches by the urgent care for comfort. Examination reveals intraarticular effusion, tenderness over the lateral anterior knee, and some discomfort with motion limited by swelling.
Ligamentous examination is stable. What is the best next step in evaluation and/or management?
Ligamentous examination is stable. What is the best next step in evaluation and/or management?

Explanation
■
The images demonstrate osteochondritis dissecans. The history of pain with even mild activity such as walking, presence of effusion, and limited range of motion raise concern for an unstable lesion. MRI is the best modality to detect this and would be the next indicated step in evaluation.
CT is better for delineating bony anatomy, not the stability of the lesion. Arthroscopy is not indicated before MRI. Patients with stable lesions and open physes can heal their lesions without surgery. Physical therapy would not be appropriate without first determining the stability of the lesion.
■
The images demonstrate osteochondritis dissecans. The history of pain with even mild activity such as walking, presence of effusion, and limited range of motion raise concern for an unstable lesion. MRI is the best modality to detect this and would be the next indicated step in evaluation.
CT is better for delineating bony anatomy, not the stability of the lesion. Arthroscopy is not indicated before MRI. Patients with stable lesions and open physes can heal their lesions without surgery. Physical therapy would not be appropriate without first determining the stability of the lesion.
Question 5High Yield
A 55-year-old patient is seeking a surgical consultation for a painful flatfoot deformity that has failed to respond to nonsteroidal anti-inflammatory drugs, shoe and activity modifications, and orthoses. The patient is of medium build, a nonsmoker, and has no history of diabetes mellitus. Radiographs are shown in Figures 43a through 43c. Based on these findings, treatment should consist of
Explanation
The patient has a degenerative collapse of the midfoot through the tarsometatarsal joints with significant forefoot abduction; therefore, a midfoot arthrodesis is required to address the arthritic joints and deformity at the tarsometatarsal articulation. All of the other procedures correct hindfoot deformities and therefore would not be appropriate treatment.
REFERENCES: Brage M: Degenerative joint disease of the midfoot. Foot Ankle Clin 1999;4:355-367.
Mann RA, Prieskorn D, Sobel M: Mid-tarsal and tarsometatarsal arthrodesis for primary degenerative osteoarthrosis or osteoarthrosis after trauma. J Bone Joint Surg Am
1996;78:1376-1385.
REFERENCES: Brage M: Degenerative joint disease of the midfoot. Foot Ankle Clin 1999;4:355-367.
Mann RA, Prieskorn D, Sobel M: Mid-tarsal and tarsometatarsal arthrodesis for primary degenerative osteoarthrosis or osteoarthrosis after trauma. J Bone Joint Surg Am
1996;78:1376-1385.
Question 6High Yield
A 73-year-old man who underwent repair of the left rotator cuff 6 years ago reports good pain relief but notes residual weakness of the left shoulder, especially with overhead tasks. He denies having pain at night and has minimal discomfort with activities of daily living but is dissatisfied with his shoulder strength. Radiographs show an acromiohumeral interval of 2 mm. Appropriate management should consist of
Explanation
An exercise program to strengthen the deltoid and remaining rotator cuff will most likely offer the best results. Revision rotator cuff surgery yields better results in decreasing pain than improving strength and function, and this patient has only minimal pain. Tendon transfers, involving the use of the latissimus dorsi or teres major, have been used when the rotator cuff is deemed irreparable but are not indicated in elderly patients with minimal symptoms.
REFERENCES: Bigliani LU, Cordasco FA, McIlveen SJ, Musso ES: Operative treatment of failed repairs of the rotator cuff. J Bone Joint Surg Am 1992;74:1505-1515.
DeOrio JK, Cofield RH: Results of a second attempt at surgical repair of a failed initial rotator-cuff repair. J Bone Joint Surg Am 1984;66:563-567.
Gerber C, Vinh TS, Hertel R, Hess CW: Latissimus dorsi transfer for the treatment of massive tears of the rotator cuff: A preliminary report. Clin Orthop 1988;232:51-61.
REFERENCES: Bigliani LU, Cordasco FA, McIlveen SJ, Musso ES: Operative treatment of failed repairs of the rotator cuff. J Bone Joint Surg Am 1992;74:1505-1515.
DeOrio JK, Cofield RH: Results of a second attempt at surgical repair of a failed initial rotator-cuff repair. J Bone Joint Surg Am 1984;66:563-567.
Gerber C, Vinh TS, Hertel R, Hess CW: Latissimus dorsi transfer for the treatment of massive tears of the rotator cuff: A preliminary report. Clin Orthop 1988;232:51-61.
Question 7High Yield
Which subtype of Ehlers-Danlos syndrome (EDS) is caused by lysyl hydroxylase deficiency:
Explanation
Many of the mutations responsible for the differing subtypes of Ehlers-Danlos syndrome (EDS) have not been identified (EDS types I, II, and III). Lysyl hydroxylase deficiency has been identified as the cause of type IV. A mutation in type I collagen has been identified as the cause of EDS VII.
Question 8High Yield
Which of the angles depicted in Figure 60 has been found to most closely correlate with a patient’s lumbar lordosis, thoracic kyphosis, and overall sagittal alignment?
Explanation
Angle A represents pelvic incidence (PI), a constant anatomic relationship between the pelvis and sacrum. Angle B represents pelvic tilt, and angle C represents sacral slope. Pelvic tilt and sacral slope can change depending on the rotation of the pelvis. Pelvic incidence has been found directly correlate with the magnitude of lumbar lordosis and thoracic kyphosis because it determines the angle at the base
of the spine (the lumbosacral junction). To obtain sagittal balance, the remainder of the spine compensates, resulting in the degree of lumbar lordosis and thoracic kyphosis to maintain an upright posture. Thus, PI must be considered in the evaluation of sagittal balance and potential reconstructive procedures. Angle D represents the T1 angle.
of the spine (the lumbosacral junction). To obtain sagittal balance, the remainder of the spine compensates, resulting in the degree of lumbar lordosis and thoracic kyphosis to maintain an upright posture. Thus, PI must be considered in the evaluation of sagittal balance and potential reconstructive procedures. Angle D represents the T1 angle.
Question 9High Yield
A 14-year-old boy is seen for back pain. Radiographic evaluation reveals a grade III isthmic spondylolisthesis. What measurement is most useful in predicting the likelihood of progression?

Explanation
DISCUSSION: Slip angle has been shown to be highly predictive of the risk for increased slippage in patients with spondylolisthesis. None of the other radiographic parameters listed has been shown to be predictive of the risk for increased slippage.
REFERENCES: Huang RP, Bohlman HH, Thompson GH, et al: Predictive value of pelvic incidence in progression of spondylolisthesis. Spine 2003;28:2381-2385.
Mac-Thiong JM, Wang Z, de Guise JA, et al: Postural model of sagittal spino-pelvic alignment and its relevance for lumbosacral developmental spondylolisthesis. Spine 2008;33:2316-2325.
**2010 Pediatric Orthopaedic Examination Answer Book • 23**
Figure 22a Figure 22b
REFERENCES: Huang RP, Bohlman HH, Thompson GH, et al: Predictive value of pelvic incidence in progression of spondylolisthesis. Spine 2003;28:2381-2385.
Mac-Thiong JM, Wang Z, de Guise JA, et al: Postural model of sagittal spino-pelvic alignment and its relevance for lumbosacral developmental spondylolisthesis. Spine 2008;33:2316-2325.
**2010 Pediatric Orthopaedic Examination Answer Book • 23**
Figure 22a Figure 22b
Question 10High Yield
A 2-week-old, otherwise healthy neonate presents at the emergency department with a 1-day history of fever, pain with diaper changes, and poor feeding. The complete blood count, erythrocyte sedimentation rate, and white blood cell count are all elevated. On examination, the baby holds the leg flexed, abducted, and externally rotated and has pain with any attempts at ranging the hip. Plain radiographs are negative, but hip ultrasonography shows a large hip joint effusion. The patient is taken to the operating room and undergoes a hip aspirate and irrigation and debridement of this septic hip. What is the most likely organism causing the infection?
Explanation
■
Although Staphylococcus aureus is the most common infecting organism in children with septic arthritis, in an otherwise healthy newborn, Streptococcus occurs more commonly. Kingella kingae is becoming a more commonly seen infecting organism, but it is more often seen in the toddler age range. Newborns in the neonatal intensive care unit are at risk for infections with Gram-negative organisms as well. With the introduction of a vaccine against Haemophilus influenzae, this organism is now rarely seen as a causative agent in septic arthritis.
Although Staphylococcus aureus is the most common infecting organism in children with septic arthritis, in an otherwise healthy newborn, Streptococcus occurs more commonly. Kingella kingae is becoming a more commonly seen infecting organism, but it is more often seen in the toddler age range. Newborns in the neonatal intensive care unit are at risk for infections with Gram-negative organisms as well. With the introduction of a vaccine against Haemophilus influenzae, this organism is now rarely seen as a causative agent in septic arthritis.
Question 11High Yield
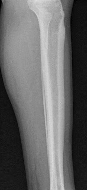
A 19-year old Division 1 offensive lineman sustains an ankle injury during a game. He has pain with weight-bearing and is unable to return to the game. Figures 1 through 5 are his radiographs taken the next day. What is the best next step?
---
---
---
---
---
---
---
---
---
---
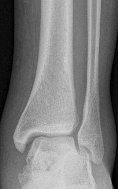
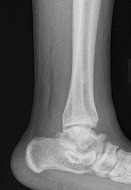
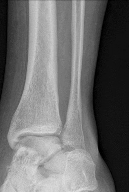
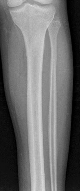
Explanation
The radiographs reveal medial clear space widening and an oblique proximal fibula fracture (best seen on the lateral view overlapping the tibia). This is consistent with an unstable syndesmotic injury. Operative repair of the syndesmosis with reduction and fixation is warranted. Immobilization is the best option for a stable syndesmotic injury. Physical therapy and MRI are not warranted given the findings on the _radiographs._
Question 12High Yield
Which of the following activities can improve posterior capsular contractures?
Explanation
Posterior capsule stretching is performed in the cross-chest and behind the back positions. Stretching in internal rotation in the abducted shoulder will further stretch the posterior capsule. Wide grip stretch, and anterior capsule and strengthening exercises will not necessarily stretch the capsule.
REFERENCES: Ellenbacher TS: Shoulder internal and external rotation strength and range of motion of highly-skilled junior tennis players. Isokinetic Exercise Sci 1992;2:1-8.
Kibler WB, McMullen J, Uhl J: Shoulder rehabilitation strategies, guidelines, and practice. Op Tech Sports Med 2000;8:258-267.
REFERENCES: Ellenbacher TS: Shoulder internal and external rotation strength and range of motion of highly-skilled junior tennis players. Isokinetic Exercise Sci 1992;2:1-8.
Kibler WB, McMullen J, Uhl J: Shoulder rehabilitation strategies, guidelines, and practice. Op Tech Sports Med 2000;8:258-267.
Question 13High Yield
An 8-year-old basketball player jumped up and felt a pop in his knee. He has diffuse anterior swelling and pain, and he is unable to perform a straight-leg raise. A small fleck of bone is seen distal to the patella on his radiograph.
Explanation
- Patellar sleeve fracture
Question 14High Yield
A 32-year-old football coach has had a 4-month history of increasing right wrist pain, particularly during blocking exercises, and he reports significant pain with range of motion and gripping activities. He denies any history of trauma. Examination reveals dorsal wrist tenderness and boggy fullness over the dorsum of the wrist. No erythema is noted. Grip strength is 60% compared with the opposite side. Radiographs are shown in Figures 5a and 5b. What is the most likely diagnosis?
Explanation
The patient has Kienbock’s disease (osteonecrosis of the lunate), which presents with boggy synovitis of the wrist, decreased range of motion, and often normal radiographs. The patient’s radiographs reveal small fragments from the lunate, with increased density in the lunate body. While a traumatic event may precede the patient’s pain, often an insidious increase in pain is found. Repetitive trauma has been suggested as a possible cause. This disease process is classically associated with an ulnar-negative variant. An MRI scan, revealing a low-intensity signal in the lunate, is the best diagnostic tool for early Kienbock’s disease.
REFERENCES: Green DP, Hotchkiss RN, Pederson WC: Green’s Operative Hand Surgery, ed 4. Philadelphia, PA, Churchill Livingstone, 1999, pp 837-848.
Gerwin M, Weiland AJ: Avascular necrosis of the carpals. Hand Clin 1993, p 761.
REFERENCES: Green DP, Hotchkiss RN, Pederson WC: Green’s Operative Hand Surgery, ed 4. Philadelphia, PA, Churchill Livingstone, 1999, pp 837-848.
Gerwin M, Weiland AJ: Avascular necrosis of the carpals. Hand Clin 1993, p 761.
Question 15High Yield
A 2-year-old child is brought to your office for evaluation of a "big hand." Upon examination, you notice that the child has mildly enlarged ring and small fingers. There is full range of motion without instability. After examination of the patient, you discuss the diagnosis of macrodactyly with the parents. The parents feel assured after your discussion of the disease process and your review of the radiographs. You should next see the patient:
Explanation
Patients with macrodactyly should be followed up yearly. Although the parents may be difficult, this is not a reason to stop seeing a patient. The other answers choices are incorrect because treatment would be too late.
Question 16High Yield
A 20-year-old collegiate running back lowers his head to absorb a hit and is tackled to the ground. He is able to get up immediately and return to the sidelines on his own power but reports to the medical staff that he felt a burning sensation in his left shoulder, arm, and hand for 15 seconds following the hit. The feeling has since resolved. This is the first time this sensation has occurred. Examination on the sidelines reveals full and painless neck range of motion and normal and symmetric strength throughout the upper and lower extremity. What is the best next course of action?
Explanation
This player has experienced a “stinger” or “burner”, which results from a transient stretch or compression of the nerves emanating from the brachial plexus. This player experienced complete resolution of symptoms quickly and had a normal physical examination immediately after the injury. As this was the player’s first stinger, he may return to the game without restriction. Multiple stingers would warrant further neurologic work-up. With a normal physical examination, cervical immobilization is not necessary.
60
60
Question 17High Yield
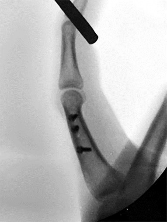
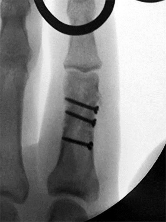
Figures 1 through 3 are the clinical photograph and radiographs of a 25-year-old, left-hand-dominant man who injured his left index finger. Which treatment option will most effectively allow satisfactory fracture alignment and maximize motion?
---
---
---
---
---
---
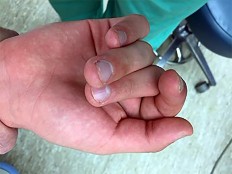
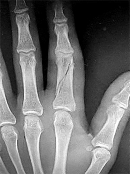
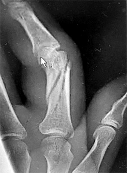
Explanation
This patient has an oblique index proximal phalanx fracture with malrotation. Buddy-taping and digital splinting would not predictably maintain fracture reduction and would result in a malunion with rotational deformity and possible shortening. Closed reduction and spanning external fixation in extension would result in significant digital stiffness. ORIF (Figures 4 and 5) followed by an early ROM program would allow anatomic fracture alignment and give this patient the best chance to regain the majority of motion in the shortest amount of time.
---
---
---
---
Question 18High Yield
A 14-year-old boy sustains a twisting injury to his right shoulder and recalls feeling a snap during a wrestling match. Examination shows hesitancy to raise the arm away from the side, diffuse tenderness and swelling of the upper arm, and no evidence of neurovascular compromise. Figures 6a and 6b show an AP radiograph and MRI scan. What is the most likely diagnosis?
Explanation
While difficult to appreciate on the AP radiograph of the shoulder, the increased physeal signal demonstrated on the axial MRI scan is consistent with a nondisplaced growth plate fracture. A comparison radiograph of the left shoulder also could be considered and the injured shoulder evaluated for physeal widening.
Proximal humeral fractures in children are somewhat unusual, representing less than 1% of all fractures seen in children and only 3% to 6% of all epiphyseal fractures. Physeal injuries are classified according to the Salter-Harris classification scheme. Salter-Harris type I fractures represent approximately 25% of physeal injuries to the proximal humerus in adolescents.
The proximal humeral physis is responsible for 80% of the longitudinal growth of the humerus; therefore, there is tremendous potential for remodeling of fractures in this region. Management for nondisplaced Salter-Harris type I fractures is limited to a short period of immobilization followed by a gradual return to activities as clinical symptoms resolve.
REFERENCES: Curtis RJ, Rockwood CA Jr: Fractures and dislocations of the shoulder in children, in Rockwood CA Jr, Matsen FA III (eds): The Shoulder. Philadelphia, PA, WB Saunders, 1990, pp 991-1007.
Salter RB, Harris WR: Injuries involving the epiphyseal plate. J Bone Joint Surg Am 1963;45:587-622.
Proximal humeral fractures in children are somewhat unusual, representing less than 1% of all fractures seen in children and only 3% to 6% of all epiphyseal fractures. Physeal injuries are classified according to the Salter-Harris classification scheme. Salter-Harris type I fractures represent approximately 25% of physeal injuries to the proximal humerus in adolescents.
The proximal humeral physis is responsible for 80% of the longitudinal growth of the humerus; therefore, there is tremendous potential for remodeling of fractures in this region. Management for nondisplaced Salter-Harris type I fractures is limited to a short period of immobilization followed by a gradual return to activities as clinical symptoms resolve.
REFERENCES: Curtis RJ, Rockwood CA Jr: Fractures and dislocations of the shoulder in children, in Rockwood CA Jr, Matsen FA III (eds): The Shoulder. Philadelphia, PA, WB Saunders, 1990, pp 991-1007.
Salter RB, Harris WR: Injuries involving the epiphyseal plate. J Bone Joint Surg Am 1963;45:587-622.
Question 19High Yield
**FOR ALL MCQS CLICK THE LINK ORTHO****MCQ BANK**
Intermediate doses (650 mg to 4 g/day) inhibit COX-1 and COX-2, blocking prostaglandin (PG) production, and have analgesic and antipyretic effects. Illustration A shows the mechanism of action of aspirin.
InCORRECT Answers: 1,2,4,5: Aspirin does not have any of these mechanisms of action.
725. A study is proposed in which 2 groups of patients are randomized to treatment with bisphosphonates or placebo. This is an example of what study type?
Intermediate doses (650 mg to 4 g/day) inhibit COX-1 and COX-2, blocking prostaglandin (PG) production, and have analgesic and antipyretic effects. Illustration A shows the mechanism of action of aspirin.
InCORRECT Answers: 1,2,4,5: Aspirin does not have any of these mechanisms of action.
725. A study is proposed in which 2 groups of patients are randomized to treatment with bisphosphonates or placebo. This is an example of what study type?


























Explanation
In a parallel design trial, participants are randomized to 2 or more groups, each of which receives a different treatment or intervention. For example, Group A receives the drug and Group B receives the placebo. This type of
design allows for comparison between groups. In a crossover design clinical trial, both groups receive both interventions over a defined time period. For example, Groups A and B both receive the drug as well as the placebo. This allows for within-participant comparisons. In a cohort study, patient groups are followed over time on the basis of having or not having received an exposure. Cohort studies are not randomized. In a case series, patients often receive a particular treatment and the outcomes are then examined.
726. An otherwise healthy 50-year-old man who is a smoker undergoes a posterior spine fusion with instrumentation for spondylolisthesis. What can the patient do to minimize his risk for pseudarthrosis?
1. Increase calcium and vitamin D intake
2. Avoid all nonsteroidal anti-inflammatory drugs (NSAIDs)
3. Maintain smoking cessation
4. Engage in early physical therapy to strengthen the trunk musculature
**CORRECT answer: 3**
Smoking is the biggest risk factor for nonunion and should be strictly avoided. NSAIDs interfere with bone healing, but not as strongly as smoking. Early mobilization would potentially stress the construct, inducing movement that leads to nonunion. Without history of calcium and vitamin D deficiency, increasing intake would not decrease the risk of nonunion.
727. When making a comparison to autograft incorporation, the inflammatory process in allograft tissue anterior cruciate ligament (ACL) reconstruction
1. occurs earlier.
2. occurs later.
3. is prolonged.
4. is shortened.
**CORRECT answer: 3**
Compared to similar autograft, allograft tissue demonstrates a prolonged inflammatory response, slower rate of biological incorporation and remodeling, and a higher proportion of large-diameter collagen fibrils. Native ACL inserts
into bone through a transition of 4 distinct zones: tendon, unmineralized fibrocartilage, mineralized fibrocartilage, and bone. This transition is not reproduced with tendon grafts, which instead heal with interposed fibrovascular scar at the graft-tunnel interface. The scar rapidly remodels to form perpendicular fibers resembling Sharpey fibers and, eventually, mature bone growth into the outer portion of the graft. The intra- articular portion of allograft undergoes an initial phase of necrosis followed by repopulation by host synovial cells into the acellular collagen scaffold.
Revascularization and maturation complete the ligamentization of graft tissue.
728. A researcher decides she wants to look at the current total number of patients who have methicillin-resistant** _Staphylococcus aureus_**(MRSA) infections in a hospital on 1 particular day. What is the researcher measuring?
1. Correlation coefficient of MRSA
2. Prevalence of MRSA
3. Incidence of MRSA
4. Relative risk of MRSA
**CORRECT answer: 2**
The prevalence of a disease is a measure of the number of cases of a disease at or during a specific time point or time period. In this case, the researcher wants to know the prevalence of disease on a given day. Incidence measures new cases of a disease or event per unit of time. Correlation coefficient is a measure of how 2 things correlate with one another, while relative risk is a statistical outcome that is often used in case-control or cohort studies to provide a measure of the risk of a particular disease occurring when a certain exposure has already occurred.
729. A 48-year-old man who is scheduled to undergo total knee replacement has an X-linked clotting disorder that leads to abnormal bleeding and recurrent, spontaneous hemarthrosis. Before undergoing surgery, he should have replacement therapy of
1. protein C and S.
2. vitamin K.
3. von Willebrand factor.
4. factor VIII.
**CORRECT answer: 4**
Hemophilia A is an X-linked recessive deficiency of factor VIII that can lead to significant bleeding problems including recurrent spontaneous hemarthroses that can lead to synovitis and joint destruction. von Willebrand disease is a lack of von Willebrand factor that leads to decreased platelet aggregation; more commonly patients have mucosal bleeding and not hemarthroses. Vitamin K deficiency is not hereditary; it is typically attributable to inadequate dietary intake, malabsorption, and loss of storage sites from hepatocellular disease. Protein C and S deficiencies are autosomal-dominant diseases that lead to thrombosis, not bleeding, as protein C and S shut off thrombin formation.
730. What is the recommended optimal timing of presurgical antibiotic administration to prevent infection in patients undergoing total joint replacement surgery?
1. Within 1 hour before incision
2. Within 2 hours before incision
3. Immediately after incision
4. Within 1 hour after incision
**CORRECT answer: 1**
The current recommendation for antibiotic prophylaxis for major orthopaedic surgical procedures is to administer intravenous antibiotics within 1 hour of surgical incision. Redosing of antibiotics should occur 3 to 4 hours after the initial dose for procedures that extend beyond 3 to 4 hours. Little evidence supports postsurgical antibiotic use beyond 24 hours. As you move beyond 1 hour from time of administration of antibiotics, risk for infection increases and rates of bacterial cell death decline. It is not acceptable to
administer presurgical antibiotics after incision.
731. **Bacterial resistance to antibiotics in biofilm is an example of**
1. avoidance.
2. decreased susceptibility.
3. inactivation.
4. mutation. **CORRECT answer: 1**
Three basic mechanisms of antibiotic resistance have been identified: avoidance, decreased susceptibility, and inactivation. Biofilm formation is a classic example of avoidance, whereby the biofilm creates a physical barrier to the antibiotic. Bacteria can decrease their susceptibility to antibiotics by mutating the antibiotic target or generating a mechanism to inactivate the antibiotic. Biofilm formation develops when a sufficient mass of bacteria forms on a surface. The cell-to-cell signaling becomes sufficient to activate transcription of genes needed for biofilm formation in a process known as quorum sensing. Once the bacteria produce a mature biofilm, they enter a greatly reduced or stationary phase of growth. Lastly, high-shear
environments seem to stimulate biofilm production.
732. A patient with Paget disease who is intolerant of bisphosphonates is given calcitonin. What is the mechanism of action of calcitonin?
1. Promotes reabsorption of phosphate in the renal tubules
2. Interferes with osteoclast maturation
3. Interferes with intestinal absorption of calcium
4. Upregulates osteoblast formation
**CORRECT answer: 2**
Calcitonin is a hormone that reduces serum calcium concentration by directly interfering with osteoclast maturation via receptors. Calcitonin inhibits phosphate reabsorption and decreases calcium reabsorption in the kidneys. By attenuating cartilage breakdown and stimulating cartilage formation via inhibitory pathways of matrix metalloproteinases, calcitonin also has a
chondro-protective effect on articular cartilage. Calcitonin has no major effects on intestinal absorption of calcium, but may aid in small-bowel secretion of sodium, potassium, chloride, and water. Calcitonin also has no receptor effect on osteoblasts.
733. **A cartilage water content increase is the hallmark of which**
**osteoarthritis stage?**
1. Prearthritis
2. Early
3. Late
4. Terminal
**CORRECT answer: 2**
The first stage of osteoarthritis is marked by an increase in water content secondary to disruption of the matrix framework. This is followed by an increase in chondrocyte anabolic and catabolic activity in response to tissue damage. Wnt-induced signal protein 1 increases chondrocyte protease expression. Failure to restore tissue balance ultimately leads to continued destruction and osteoarthritis. One hallmark of osteoarthritic cartilage is a reduced repair mechanism attributable to decreased chondrocyte response to growth factor stimulation (transforming growth factor-alpha and insulin-like growth factor-1).
Mitochondrial dysfunction and increased production of reactive oxygen species may promote cell senescence, a progressive slowing of cellular activity. Microscopic evidence of cartilage degeneration begins with fibrillation of the superficial and transition zones, followed by disruption of the tidemark by subchondral blood vessels and eventual subchondral bone remodeling. This process ultimately leads to cartilage degradation with decreased water content in the late and terminal phases of osteoarthritis.
734. **What is the plasma half-life of warfarin?**
1. 1 to 2 hours
2. 4 to 6 hours
3. 12 to 18 hours
4. 36 to 42 hours
**CORRECT answer: 4**
Warfarin, which is dosed daily, can take 72 to 96 hours to reach therapeutic levels. It has a plasma half-life of 36 to 42 hours. Low-molecular heparins have a plasma half-life of 4 to 5 hours, and fondaparinux has a half-life of 17 to 21 hours. Warfarin will not affect the International Normalized Ratio (INR) until 2 to 3 days after it is given. Patients on chronic warfarin therapy should
have treatment stopped 3 to 5 days before elective surgery to allow the INR to normalize.
735. A 70-year-old woman with a body mass index (BMI) of 34 and a history of hypercholesterolemia has elected to undergo total hip arthroplasty. Her son recently learned he has Factor V Leiden following an episode of pulmonary embolism. What are this patient's risk factors for thromboembolic disease?
1. Type of surgery, age, and BMI
2. Type of surgery, hypercholesterolemia, and age
3. Age, BMI, and hypercholesterolemia
4. BMI, type of surgery, and hypercholesterolemia
**CORRECT answer: 1**
Risk stratification is one of the most critical clinical evaluations before undergoing total joint arthroplasty. Many factors have been identified to increase risk for venous thromboembolism (VTE). The major factors include previous VTE, obesity, type of surgery (such as total joint arthroplasty), hypercoagulable states, myocardial infarction, congestive heart failure, family history of VTE, and hormonal replacement therapy.
Hypercholesterolemia is not a risk factor for thromboembolic disease.
736. **DNA replication occurs during which phase of the cell cycle?**
1. M
2. S
3. R
4. G1
5. G2
**CORRECT answer: 2**
The cell cycle consists of four distinct phases: initial growth (G1), DNA replication/synthesis (S), a gap (G2), and mitosis (M) (see illustration).
The G1 and G2 phases of the cell cycle represent the “gaps” or growth phases in the cell cycle that occur between DNA synthesis and mitosis. G0 cells are in a stable state and have not entered the cell cycle. During the S phase, the DNA is synthesized and replicated. During the M phase or mitosis, all genetic material divides into two daughter cells.
The cells are diploid (2N) in the G0 and G1 phases. The cells become tetraploid (4N) at the end of S and for the entire G2 phases. There is no R phase in the cell cycle.
737. **What antithrombotic agent is a selective factor I0a inhibitor?**
1. Warfarin
2. Low-molecular-weight heparin
3. Rivaroxaban
4. Aspirin
**CORRECT answer: 3**
Rivaroxaban is a selective factor I0a inhibitor. Aspirin is a cyclooxygenase inhibitor. Low-molecular-weight heparin is a nonspecific anticoagulant. Warfarin is a vitamin K antagonist and reduces production of clotting factors II, VII, IX, and X.
738. A 68-year-old woman had advanced right knee arthritis and total knee replacement was planned. She learned she had primary biliary cirrhosis at age 41 and now has advancing liver failure. Preoperative coagulation tests show a baseline International Normalized Ratio (INR) of 1.36. Appropriate methods to prevent thromboembolic
**disease as recommended by the 2011 AAOS Clinical Practice Guideline,**_Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee_
**_Arthroplasty_****, include**
1. use of mechanical prophylaxis (eg, pneumatic calf compressors) while in the hospital.
2. oral warfarin with a goal INR between 2.0 and 3.0.
3. low-dose warfarin for 3 weeks postsurgically beginning 48 hours after surgery.
4. no prophylaxis because this patient already is partially anticoagulated secondary to her liver disease.
**CORRECT answer: 1**
The 2011 AAOS Clinical Practice Guideline, _Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee Arthroplasty_ , recommends the use of mechanical prophylaxis for patients at increased risk
for bleeding (including those with liver disease or hemophilia). This recommendation is the consensus of the workgroup that established these guidelines because there was insufficient evidence to justify a stronger recommendation in this clinical scenario. The other responses use no prophylaxis or pharmacological prophylaxis. Pharmacological prophylaxis is not recommended in patients who are at increased risk for bleeding.
739. The pharmacokinetics of which deep venous thrombosis (DVT) prophylactic agent are affected by liver function and dietary intake?
1. Dalteparin
2. Warfarin
3. Fondaparinux
4. Enoxaparin
**CORRECT answer: 2**
Warfarin is an oral vitamin K antagonist that is rapidly absorbed from the gastrointestinal tract. It accumulates in the liver, where it is metabolized and excreted. The pharmacokinetics of warfarin can be affected by certain drugs or disease states that influence liver function. Fondaparinux is a synthetic factor Xa inhibitor that is eliminated through the kidneys. Both Dalteparin and Enoxaparin are low-molecular-weight heparins that activate antithrombin and inhibit factors Xa and IIa. Like Fondaparinux, they are eliminated through the kidneys and should be used with caution in patients with kidney disease.
740. What infection-control measure has been shown to have the most notable impact in reducing surgical-site infections?
1. Intravenous antibiotic administration within 1 hour of surgical incision
2. Screening and decolonization of patients colonized with methicillin-resistant
Staphylococcus aureus
3. Horizontal laminar flow
4. Use of enclosed body exhaust suits
**CORRECT answer: 1**
Timely administration of prophylactic antibiotics is the most important factor shown to decrease surgical-site infections. The use of horizontal laminar flow and body exhaust suits has not been shown to significantly affect infection rates.
741. The resistance to pullout of a screw in osteoporotic bone is increased by all of the following EXCEPT?
1. Placement parallel to the trabecular pattern
2. Purchase in cortical bone
3. Use of a fixed angle (locking screw construct)
4. Tapping prior to screw placement
5. Augmentation with polymethylmethacrylate
**CORRECT answer: 4**
Of the options listed, tapping prior to screw placement is the only variable that does not increase the pullout strength of a screw in osteoporotic bone.
Cornell reviews internal fixation in osteoporotic bone. According to this article, the quality of the bone is the primary determinant of the holding power of an individual screw. Other factors that increase the pullout strength include fixation in cortical bone (cortical bone has greater mineral density and, therefore, greater resistance to screw pullout than trabecular bone), screws placed parallel to the trabecular pattern, and screw fixation augmented with PMMA. The addition of a locking plate will also increase the resistance to failure by creating a fixed angle construct. Tapping prior to placement of the screw has not been shown to increase resistance to pullout, on the contrary studies have shown
this decreases resistance to pullout.
Turner et al examined the holding strength of small and large diameter screws in healthy bovine and diseased human bone. They found the screw diameter, trabecular orientation of the bone, and mineral content of the bone all affect the holding strength. A larger diameter screw, parallel placement to the trabecular pattern, and purchase in bone with a higher density all increase the holding strength.
742. Gigantism affects which region of the growth plate labeled in Figure A?
1. A
2. B
3. C
4. D
5. E
**CORRECT answer: 3**
Gigantism, like achondroplasia, affects the proliferative zone (Region C of Figure A) of the growth plate. In Figure A, Region A is the epiphysis, Region B is the resting zone, Region D is the hypertrophic zone, and Region E is the metaphysis. Illustration A is another depiction of the physis which is labeled. Gigantism is typically caused by a pituitary adenoma which over secretes growth hormone. Its effect on the proliferative zone results in bone overgrowth and excessive height and limb length. Acromegaly may also be
caused by a pituitary adenoma that over secretes growth hormone, but has its effect once the physis has closed.
743. Plain radiographs do not provide an accurate assessment of bone mineral density (BMD) until what percentage of mineral has been lost?
1/. 5%
2/. 20%
3/. 40%
4/. 90%
**CORRECT answer: 3**
Radiographic evidence of BMD loss is not apparent until 40% reduction. Osteopenia should not be ruled out based on an apparently normal mineralized bone.
744. Figure 85 is the radiograph of a 3-year-old boy whose chief issue is knocked knees. His mother notes that she has a similar condition and required multiple surgeries as a child. She states that her son walks with an unsteady gait and is small for his age. He does not currently take any medications and is not under medical care for any disorders. What is the most appropriate next treatment step?
1. Recommend bilateral valgus-producing proximal femoral osteotomies to CORRECT coxa vara
2. Recommend bilateral medial distal femoral and proximal tibial hemiepiphyseal arrests to CORRECT genu valgum using guided growth
3. Obtain serum calcium, phosphorus, alkaline phosphatase, and vitamin D
studies and refer the patient to an endocrinologist for evaluation
4. Refer the patient to a geneticist to evaluate him for skeletal dysplasia
**CORRECT answer: 3**
The radiograph shows a patient with osteopenia; marked limb deformity, including bilateral coxa vara and bilateral genu valgum; and extreme physeal widening, which is pathonomonic for rickets. Although surgery to CORRECT the limb deformities may be appropriate, a definitive diagnosis first needs to be established, and, if possible, the patient needs to be treated medically. In cases in which limb realignment surgery has been performed without proper medial correction of the metabolic bone disease, the recurrence rate is high. Serum calcium, phosphorus, alkaline phosphatase, and vitamin D are appropriate screening studies for diagnosis of metabolic bone disease, and treatment is most commonly performed by an endocrinologist. A geneticist may play a role in establishing the cause of the disease, especially if there is a hereditary component, but this step should not delay the consultation with endocrinology.
745. A 45-year-old man is placed on indomethacin for heterotopic ossification prophylaxis following surgery for an acetabular fracture. What is the most likely side effect of this medication?
1. Renal failure
2. Hepatitis
3. Peripheral neuropathy
4. Deep vein thrombosis
5. Gastrointestinal ulceration
**CORRECT answer: 5**
Indomethacin, commonly used to prevent heterotopic ossification, is associated with a high rate of gastrointestinal toxicity.
Berger, in a case-based review of nonsteroidal anti-inflammatory use in Orthopaedics, notes that NSAIDs block the protective effect of prostaglandins on the gastrointestinal mucosa, in addition to causing variable rates of platelet dysfunction. Elderly patients using NSAIDS are estimated to have a 4 to 5 times increased relative risk of death due to gastrointestinal hemorrhage compared with matched cohorts. Indomethacin, in particular, has a high rate
of gastrointestinal complications when compared with other NSAIDs.
746. **What region of the physis does collagen type X play a prominent role?**
1. resting zone
2. proliferative zone
3. zone of hypertrophy
4. metaphysis
5. diaphysis
**CORRECT answer: 3**
Type X collagen is important for bone mineralization and is produced by hypertrophic chondrocytes in the zone of hypertrophy.
There are 4 zones of the physis. The first is the RESTING ZONE, which is characterized by widely dispersed chondrocytes, abundant matrix, and is relatively inactive in cell or matrix turnover. The second zone is the PROLIFERATIVE ZONE. It characterized by longitudinal columns of flattened cells, significant endoplasmic reticulum, high ionized calcium. The third zone is the HYPERTROPHIC zone. It is characterized by enlargement of cells,
persistent metabolic activity, accumulate and calcium, synthesize alkaline phosphatase and type X collagen, aiding in mineralization. The final zone, in the METAPHYSIS, comprises the primary and secondary spongiosa layers. These layers are characterized by vascular invasion and bone remodeling, respectively.
Illustration A shows a histological view of the phyeal zones. Zone C is the proliferative zone, Zone D is the hypertrophic zone, and Zone E is the metaphysis.
InCORRECT Answers:
Answers 1,2,3,5: collagen type X play the greatest role in the zone of hypertrophy.
747. Which of the following modalities has been shown to have a positive effect when treating early stages of complex regional pain syndrome?
1. Casting of the involved extremity
2. Plyometric exercises
3. Ultrasound therapy
4. Acupuncture
5. Gentle physiotherapy
**CORRECT answer: 5**
Complex regional pain syndrome type I (reflex sympathetic dystrophy) is defined as a disease that develops after an initial noxious or painful event which causes the development of pain and dysfunction out of proportion to the event. It sometimes cannot be linked to a specific physiologic process. Hyperesthesias, edema, and/or blood flow changes are prevalent. Type II (synonym for causalgia) has a known identifiable nerve injury. Hypotheses include increased sympathetic tone causes feedback loop, activation of nociceptors to neurons in spinal cord, continued ischemia, re-activation of pain receptors, and possibly unregulated sensitivity of alpha adrenergic receptors.
For treatment, early gentle physiotherapy is recommended for this condition. Aggressive passive range of motion is contraindicated in the early phases because it will provoke pain and inflammation. The primary goal of therapy is to decrease pain and prevent stiffness. Contrast baths can help desensitize
and improve blood flow, and TENS (transcutaneous electrical nerve stimulator) has been shown to have a positive outcome on CRPS type II only (those with identifiable nerve lesions). Illustration A shows the basic pathology of this
condition.
748. **The force generated by a muscle is most highly dependent on its**
1. cross-sectional area.
2. fiber type.
3. length.
4. morphology.
5. level of conditioning.
**CORRECT answer: 1**
The cross-sectional area of a muscle determines to a great extent the force generated by the muscle. The force of a muscle contraction is controlled by the amount of myofibrils that contract; the greater the amount of contracting myofibrils, the greater the force of contraction. Fiber types have less to do
with the force of contraction and more to do with the duration and speed of contraction. Muscle length affects contraction force through the Blix curve. The morphology of a muscle can affect the cross-sectional area by varying the angle of the fibers in relation to the force vector. Conditioning mostly affects duration and fatigability.
749. Arachidonic acid is directly metabolized by which of the following substances?
1. Carbonic anhydrase
2. HMG-CoA reductase
3. 1-lipoxygenase
4. Cyclooxygenase
5. Thromboxane synthetase
**CORRECT answer: 4**
Arachidonic acid is the common substrate that is directly metabolized by cyclooxygenase into the prostanoids including prostaglandins, prostacyclin and thromboxane.
Cyclooxygenase 1 enzyme, or COX-1, results in prostaglandins responsible for maintenance and protection of the GI tract. Cyclooxygenase-II enzyme, or COX-2, results in prostaglandins responsible for inflammation and pain. Leukotrienes are synthesized from arachidonic acid by 5-Lipoxygenase, not 1-Lipoxygenase. Mevalonate is involved in the HMG-CoA reductase pathway – the metabolic pathway that produces cholesterol (site of action of the statins). A diagram of arachidonic acid metabolism is provided in Illustration A.
750. A 50-year-old male sustains a closed head injury and closed femur fracture after falling off of a ladder. His GCS is currently 15, and he only speaks Spanish; he has several family members in the waiting room of the hospital. Which of the following is true regarding informed consent for fixation of his femur fracture?
1. Patient must be able to read the consent form
2. Patient must be able to sign the consent form
3. Patient does not need to be able to communicate in any manner to give his or her own informed consent
4. Patient must not be on any antidepressant medication prior to verbal or written informed consent
5. Patient should give verbal informed consent prior to narcotic administration
**CORRECT answer: 5**
The patient should give verbal informed consent by understanding the important risks and benefits (not necessarily every potential complication that could possibly occur), as well as the indications for and alternatives to a procedure. This should be performed prior to administration of narcotic medication. However, narcotic administration should not be delayed for patients in pain secondary to lack of availability of a written consent form, if the verbal conversation has occurred, as documentation of the consent process can still be performed prior to surgical intervention.
Wenger et al developed a survey of 102 orthopaedic surgeons who correctly answered a mean of nineteen (73%) of the 26 questions. The respondents appropriately handled questions involving economic aspects, truth-telling, confidentiality, and an incompetent colleague. However, there was less understanding of proper ethical conduct with regard to informed consent
(58%), the physician-patient relationship (72%), and end-of-life decision- making (78%). There was also an analysis of the inCORRECT responses by the surgeons in the survey: Nineteen percent of the 102 respondents thought that a patient must be able to read the consent form, 39% thought that the patient must understand all of the risks of the procedure, 12% did not think that the patient needed to be able to communicate in some fashion to give their own consent, and 29% indicated that the patient must not be taking any
medication with psychoactive effects.
The CORRECT answers include; discussing the important (not necessarily all) risks and benefits as well as the indications for and alternatives to a procedure, ability to communicate with a patient that will give their own
consent, and the use of antidepressant medications are not a preclusion to the informed consent process.
751. Which of the following factors is most critical to the success of a meniscal allograft transplantation?
1. Accurate graft size
2. Donor cell viability
3. Reestablishment of the central meniscal blood supply
4. Suppression of the immune response
5. Cryopreservation of the donor graft
**CORRECT answer: 1**
Success of a meniscal allograft transplantation is strongly dependent on accurate graft sizing, typically within 5% of the native meniscus. Previous studies have established that donor cell viability is not mandatory for the survival of these grafts since they are replaced by the recipient’s cells (at least peripherally) within several weeks. Thus, cryopreservation of the graft to ensure cell viability is not necessary. There is a limited immune response to musculoskeletal allografts; therefore, immunosuppression, as is required for visceral organ transplantation, is not indicated.
752. A 21-year-old collegiate scholarship football player has an episode of transient quadriplegia. An MRI scan of the cervical spine reveals cord edema and severe congenital spinal stenosis. The athlete has aspirations of playing on a professional level and demands that he
be allowed to play. The team physician should give what recommendation to the college?
1. Do not allow the athlete to return to football.
2. Allow the athlete to participate.
3. Allow the athlete to play only if he signs a waiver.
4. Suggest that the college and atahlete enter binding arbitration.
5. Allow the athlete to play with special equipment.
**CORRECT answer: 1**
Federal courts have ruled that a student-athlete does not have a constitutional right to participate in athletics against medical advice. As long as the student retains his scholarship, the college is under no legal or ethical obligation to allow the student to participate in sports. A waiver would not hold up in court and would not indemnify the college or the team physician against suit. No equipment has been shown to be effective
in preventing transient quadriplegia.
753. **All of the following substances inhibit osteoclast activity, EXCEPT?**
1. Tumor necrosis factor-alpha (TNF-a)
2. Osteoprotegerin
3. Calcitonin
4. Bisphosphonates
5. Denosumab
**CORRECT answer: 1**
Osteoclasts have been identified as a key cellular target in the treatment of many diseases including osteoporosis, particle-induced osteolysis in total joint arthroplasty, and tumor-induced osteolysis. As such, anti-osteoclastic agents are a hot topic of orthopaedic research.
Calcitonin and Osteoprotegerin are naturally occuring cytokines which act either on cell surface receptors (calcitonin receptor) or bind soluable mediators
(RANK-L) to inhibit osteoclasts. While two forms of bisphosphonates exist, both function to induce osteoclast apoptosis (programmed cell death). Denosumab is a monoclonal antibody to RANK-L which when given subcutaneously, binds and sequesters RANK-L, preventing it from stimulating RANK, a pro-osteoclastic receptor.
Schoppet et al wrote a comprehensive review of osteoprotegerin or OPG, a cytokine produced by many cells including osteoblasts and marrow stromal cells. It is a vital component in regulating bone resorption as it inhibits both osteoclast activation and differentiation by acting as a decoy receptor for RANK-L. The mechanism of RANK-L is seen in Illustration A.
754. A player on a professional football team sustains a knee injury and is diagnosed with an anterior cruciate ligament rupture. When employed as the team physician, your ethical obligation is to inform
1. the player but not the team.
2. the team but not the player.
3. neither the team nor the player.
4. both the team and the player.
5. the team, the player, and the media
**CORRECT answer: 4**
When you are employed as a team physician, you are obligated to inform the players and the team organization of all athletically relevant medical issues. This differs significantly from the normal rule of patient confidentiality. If the player came to see you and you were not the team physician, you may not inform the team unless the player so desires. As the team physician, you are not obligated to inform the media.
755. Protamine functions to reverse the pharmacologic effects of which of the following anti-coagulants?
1. Aspirin
2. Clopidogrel (e.g. plavix)
3. Low molecular weight heparin
4. Warfarin
5. Hirudin
**CORRECT answer: 3**
Protamine functions to partially reverse the pharmacologic effects of low molecular weight heparin (LMWH). Protamine may help to stop bleeding related to LWMH, although anti- factor Xa activity is not fully normalized by protamine. Vitamin K reverses the pharmacologic effect of warfarin. As aspirin
and clopidogrel function directly at the level of the platelet, there is no medical method to "reverse" these effects. Hirudin is a naturally occuring enzyme with anti-coagulant property in the salivary glands of leeches.
756. Storage of musculoskeletal allografts by cryopreservation is achieved by
1. replacing water in the tissue with alcohol to a moisture level of 5% and then using a vacuum process to remove the alcohol from the tissue.
2. maintaining maximum cellular viability of fresh tissue without long-term storage.
3. using chemicals to remove cellular water and controlled rate freezing to prevent
ice crystal formation.
4. freezing the graft twice and packaging the tissue without solution at minus 80 degrees C.
5. freezing the graft in water without an antibiotic solution soak during quarantine, with final storage in liquid nitrogen.
**CORRECT answer: 3**
Cryopreservation uses chemicals to remove cellular water and controlled rate freezing to prevent ice crystal formation. The tissue is procured, cooled to wet ice temperature for quarantine, and then stored in a container with cryoprotectant solution of dimethyl sulfoxide or glycerol which displaces the cellular water. The controlled rate freezing is then done to prevent ice crystal formation. Fresh allografts are not frozen in order to maintain maximum cellular viability, and this process limits the shelf life of osteochondral allografts. Freeze-drying involves replacement of water in the tissue with
alcohol to a moisture level of 5% and then uses a vacuum process to remove the alcohol from the tissue. Preparation of fresh frozen grafts involves freezing the graft twice and packaging the tissue without solution at minus 80 degrees C.
757. A new scientific study is completed investigating the use of a new technique for lumbar decompression. The prospective cohort study enrolled 400 total patients into two groups (laminectomy versus interspinous spacer) based on 80% power and beta value of 0.2. Patients were not randomized in the study. Results showed a greater improvement in pre to post operative Oswestry Disability Index (ODI) in the interspinous spacer group (38.4) versus laminectomy group (34.1). ODI scores can range from 0 (no disability) to 100 (maximum disability). P value was 0.002.
**Interpretation of these results suggests which of the following?**
1. The number needed to treat (NNT) is high
2. The study was underpowered due to use of a high beta value
3. Due to lack of randomization, the study is subject to the Hawthorne effect
4. The difference in the primary outcome was stastically significant but likely did not reach the minimum clinically important difference
5. The control group was improperly selected given their improvement in ODI scores
**CORRECT answer: 4**
While most outcome measures do not have a well-established minimal clinically important difference (MCID), a 4.3 point difference in ODI is well below any reported MCID. The results suggest that the difference in primary endpoint was statistically significant but likely did not reach the MCID.
Interpretation of clinical studies requires a basic understanding of statistical and clinical principles. While the traditionally reported p values can comment on the statistical significance of a comparison in a data set, it does not give any information regarding the clinical relevance of the result. The MCID for several clinical outcomes has been studied, but consensus does not exist on this value for most outcome measurements.
Nevertheless, the clinical relevance of a study finding is much stronger when it reaches
MCID and is statistically significant.
Vaccaro et al. prospectively investigated the management of type II dens fracture in geriatric patients. They found improved outcomes in patients
undergoing surgical management of these injuries based on the Neck Disability Index (NDI).
Young et al. evaluated the reliability and validity of the NDI in a prospective randomized study. They found an MCID of 7.5 and a minimum detectable change (MDC) of 10.2. Their findings suggest that 10 points should be used as MCID for the NDI.
Gatchel et al. comment on both the importance and difficulty of establishing MCID for outcome measures. They stress the importance of interpreting statistically significant results in the context of MCID.
InCORRECT Answers:
Answer 1: NNT is a measure used in studies assessing relative risk of certain disease states. It does not apply to this study.
Answer 2: The beta value and power used in this study are standard for most studies. Answer 3: Lack of randomization can lead to confounding. The Hawthorne effect refers to change in patient behavior when they know they are part of a study.
Answer 5: The study was comparing one surgical intervention to another. The control group was appropriately selected.
758. Which of the following is most likely to decrease surgical mortality and inpatient morbidity while simultaneously increasing surgical team adherence to life-saving steps in operating room crisis situations?
1. An intra-operative surgical team leader
2. A surgical checklist
3. The presence of a senior surgeon
4. Magnet certification of nursing staff
5. Exclusion of surgical residents from the operating room team
**CORRECT answer: 2**
The utilization of a surgical safety checklist has demonstrated substantial reductions in surgical morbidity and mortality. Checklist use has also demonstrated efficacy in increasing team adherence to life-saving care plans in operating room crises.
The World Health Organization concept of a surgical safety checklist concept was validated in 2009 as a way of improving surgical outcomes. Successful implementation of a surgical checklist relies upon surgeon leadership to educate staff on its rationale and the practical components of implementation in the operating room.
Haynes et al. evaluated a 19-item surgical safety checklist and evaluated its ability to reduce complications and deaths associated with surgery in a global population. Across 8 diverse hospitals in 8 cities around the world, their study demonstrated that implementation of a pre-surgical checklist resulted in a
50% reduction in mortality (1.5% to 0.8%) and a 37% reduction in inpatient complications (11% to 7%). The patients in the study were over the age of 16 and undergoing non- cardiac surgery.
Conley et al. evaluated the effectiveness of implementation of surgical safety checklists in five hospitals using a series of interviews conducted with surgeons. Analysis of the survey results demonstrated that effective implementation relied upon surgeon leadership to explain the necessity of the checklist and how to effectively implement its use. When surgeon leadership failed in these functions, hospital staff failed to comprehend the utility of the checklist and were not able to appropriately use it. These failures eventually led to institutional abandonment of the safety checklist.
Arriaga et al. evaluated the utility of checklists to guide the surgical team through intraoperative crisis situations (e.g., massive hemorrhage, cardiac arrest). Their study of 17 surgical teams undergoing 106 simulated surgical- crises demonstrated that use of a crisis checklist led to greater adherence to life-saving steps of a care plan. 97% of participants agreed that they desired a checklist to be present if a crisis were to occur while they themselves were undergoing surgery.
InCORRECT answers:
Answers 1, 3-5: None of these have consistently demonstrated substantive improvement in surgical morbidity and mortality.
759. Which of the following is true regarding the sequence of motor unit recruitment during muscle contracture?
1. The sequence is: slow twitch, fatigue-resistant units (1st); fast-twitch, easily fatigable units (2nd); fast-twitch, fatigue-resistant units (3rd)
2. The sequence is: slow twitch, fatigue-resistant units (1st); fast-twitch, fatigue-resistant units (2nd); fast-twitch, easily fatigable units (3rd)
3. The sequence is: slow twitch, fatigue-resistant units (1st); slow-twitch, easily fatigable units (2nd); fast-twitch, easily fatigable units (3rd)
4. The sequence is: fast-twitch, fatigue-resistant units (1st); fast-twitch, easily fatigable units (2nd); slow twitch, fatigue-resistant units (1st);
5. The sequence is: fast-twitch, easily fatigable units (1st); fast-twitch, fatigue- resistant units (2nd); slow twitch, fatigue-resistant units (1st);
**CORRECT answer: 2**
The order of muscle recruitment starts with Type I fibers (slow twitch, fatigue- resistant units), followed by Type II units that first includes Type IIa (fast- twitch, fatigue-resistant) and ends with Type IIb (fast-twitch, easily fatigable)
Motor units are recruited in order of size, starting with small sized units that generate low
force, progressing to larger units with increasing strength of muscle contraction. Type I slow oxidative motor units have a lower threshold for activation, activate under lower force requirements, and generate less force. Type II units have a higher threshold and activate during activities that require significant force. Type IIa fibers are fast oxidative/glycolytic and Type IIb fibers are fast glycolytic. The terms "slow" and "fast" refer to the speed that myosin ATPases split ATP. The easy fatigability of type IIb fibers occurs because (1) they rely on anaerobic glycolysis to produce ATP, resulting in accumulation of lactic acid, which brings about muscular fatigue and (2) their low capillary density.
Staron reviewed human muscle fiber types. They state that children (2-5y) have a higher percentage of type I fibers than newborns and adults. Aging causes loss of function from sarcopenia (loss of muscle mass, loss of motor units, particularly type II) and reduced maximum oxygen consumption begining at 25y. Regarding sex differences, females have muscles 40% smaller than men because of smaller fibers and fewer total numbers of fibers diameter cross-sectional area.
Illustration A shows the distribution of muscle fiber types. Illustrations B and C show the progression in muscle fiber activation.
InCORRECT Answers:
Answer 1: Type IIb units (fast-twitch, easily fatigable) are the last to be activated. Answer 3: There are no slow twitch, easily fatigable units (only slow twitch, fatigue- resistant units).
Answers 4 and 5: Fast-twitch units (Type II) are not activated initially. Untrained individuals cannot voluntarily activate all higher threshold type II motor units
760. Which of the following conditions exhibit the inheritance pattern shown in Figure A, assuming no new mutations?
1. Duchenne muscular dystrophy
2. Hunter's syndrome
3. Hemophilia
4. Spondyloepiphyseal dysplasia (SED) tarda
5. Diastrophic dysplasia
**CORRECT answer: 5**
The pedigree chart (males are squares and females are circles) shown in Figure A demonstrates an autosomal recessive trait.
Diastrophic dysplasia is the only autosomal recessive condition with all of the other options being X-linked recessive disorders. Along with Becker's MD these are the main orthopaedic X-linked recessive disorders.
There are many more autosomal recessive orthopaedic disorders. Autosomal recessive pedigrees often appear in both sexes with equal frequency, tend to skip generations, and affected offspring are usually born to unaffected parents. When both parents are heterozygote, approximately 1/4 of the progeny will be affected.
X-linked and autosomal dominant disorders will not skip generations.
X-linked recessive disorders will always have affected sons if the mother has the disease (this does not occur in the 3rd cross of Figure A on the far right).
761. Which of the following is NOT a component of the WHO surgical safety checklist?
1. Whether team members have introduced themselves
2. Whether antibiotics have been given within the last 60 minutes
3. Whether essential imaging is displayed
4. Whether the CORRECT implants are in the room and if the product representative needs to be present
5. Whether there is a risk of blood loss
**CORRECT answer: 4**
The WHO surgical safety checklist concerns all surgical specialties. Whether CORRECT implants are in the room and if the representative needs to be present is not a component of this checklist.
The WHO checklist has 3 phases: the sign in (before induction), the time out (before skin incision), and the sign out (before the patient leaves the room). According to the WHO checklist, the steps that must occur prior to induction of anesthesia include checking the patient’s identity, procedure, consent, and signed surgical site are confirmed; an anesthesia safety check that includes evaluation for a difficult airway and aspiration risk is performed; and determination of risk for excessive blood loss is completed. Other features of this checklist are found in Illustration A.
Haynes et al. reviewed outcomes at 8 hospitals in 8 cities before and after introduction of the WHO surgical safety checklist. They found that the death rates were 1.5% and 0.8% and complication rates were 11.0% and 7.0% before and after introduction, respectively (p<0.05 for both).
Illustration A shows the WHO surgical safety checklist InCORRECT Answers:
Answers 1,2,3,5: These are all components of the WHO surgical safety checklist.
See Illustration A.
762. A 25-year-old female falls off her bike around 10:30 PM and sustains the closed injury seen in figures A and B. On exam, she is neurovascularly intact, but reports severe pain with finger flexion or extension. The chief resident calls the attending who reports he is at a benefit event and has had a few drinks, but feels fine and can operate on the patient in 1 hour and demands that the case be scheduled. When the attending arrives, he seems more jovial than normal. After the time out is complete, he reports he is feeling tired and is going to take a nap in the lounge, but he is confident the chief resident can complete the case. What should the resident do next?
1. Start the case and wake the surgeon up if any problems arise
2. Perform a closed reduction, apply a sugar tong splint, and schedule the case electively
3. Complete the case if she is confident she can do it
4. Express concern to the attending about his impairment
5. Wait for the surgeon to regain sobriety
**CORRECT answer: 4**
The surgeon in this case is likely impaired. It is the duty of the resident to confront the attending regarding his potential impairment, and if the surgeon insists on proceeding, to report the attending to another attending or department chief before the patient is put in a more dangerous situation.
The AAOS Code of Ethics and Professionalism for Orthopaedic Surgeons states surgeons "should be attuned to evolving mental or physical impairment, both in themselves and in their colleagues, and take or encourage necessary measures to ensure patient safety." The AMA code of medical ethics reports that physicians have an obligation to intervene to prevent their impaired colleagues from harming a patient. By reporting the impaired physician one might be saving him/her from medicolegal troubles down the road.
Oreskovich et al. conducted a nationwide survey of physicians across all medical specialties (26.7% response rate) and found that 12.9% of male physicians and 21.4% of female physicians met criteria for alcohol abuse/dependence. Younger physicians and depressed physicians were more likely to abuse alcohol. Dermatologists and orthopaedic surgeons were the medical specialties most likely to abuse alcohol while pediatrics and neurology were the least likely.
Dyrbye et al. conducted a cross-sectional survey of medical students (35% response rate) to assess how burnout and depression may affect students' willingness to report impaired colleagues. They determined that students with evidence of burnout or depression were significantly less likely to feel they should report colleagues impaired by mental health issues or substance abuse. The authors concluded that not only is more explicit training regarding professional responsibilities needed, but maintaining wellness is critical in the individual's willingness to fulfill their professional roles.
Figures A and B show displaced radius and ulna shaft fractures. InCORRECT Answers:
Answer 1 & 3: Even if the chief resident is capable of completing the case independently, it is inappropriate for a resident to operate without adequate supervision.
Answer 2: Closed reduction, splinting, and elective management would be inappropriate in this patient as she may have an evolving compartment syndrome Answer 5: It is inappropriate to keep a patient under anesthesia for a prolonged time due to physician impairment. Additionally, the patient may have an evolving compartment syndrome that should be addressed emergently
763. What is the first class of antibody to appear in serum after exposure to a foreign antigen?
1. IgA
2. IgD
3. IgE
4. IgG
5. IgM
**CORRECT answer: 5**
IgM is the first class of antibody to appear in our serum after exposure to an antigen. IgG is the most abundant immunoglobulin in our body. IgA is the major class of antibody in external secretions such as intestinal mucus, bronchial mucus, saliva, and tears. IgE is important in conferring protection against parasites and is also increased in allergic reactions. The role of IgD is not known.
764. A 67-year-old female falls off of a step ladder while changing a lightbulb in her kitchen and sustains the injury shown in Figures A and B. During fixation, the surgeon elects to use an osteoconductive bone graft substitute. Which of the following has been shown to have highest early compressive strength?
1. Coralline hydroxyapatite
2. Collagen-based matrices
3. Calcium phosphate
4. Calcium sulfate
5. Tricalcium phosphate
**CORRECT answer: 3**
Of the above bone graft substitutes, calcium phosphate demonstrates the highest early compressive strength.
Calcium phosphate is an injectable compound comprised of inorganic calcium and phosphate that hardens in situ and cures by a crystallization reaction to form dahllite, a carbonated apatite similar to that found in the mineral phase of bone. Reduction and placement of internal fixation must be performed prior to application of the calcium phosphate. Compared to cancellous bone grafts and other bone graft substitutes, calcium phosphate, when hardened, has a much higher compressive strength (4 to 10 times greater than cancellous
bone) and may be useful in preventing subsequent displacement or depression of reduced articular fragments.
Russell et al. prospectively compared autologous bone graft to calcium phosphate cement in a randomized controlled trial of 119 patients. The baseline demographics including the height, weight, age, sex, and injury pattern were comparable. The authors found a significantly higher rate of articular subsidence in the three to twelve month
post-operative period with the bone graft group. They concluded that calcium phosphate was associated with greater compressive strength and less subsidence.
Welch et al. directly compared calcium phosphate and autologous bone graft used to fill subchondral defects created in an animal model. The authors found that the prevalence and degree of fracture subsidence was significantly reduced at all time-points, from 24 hours to 18 months, in the defects treated with calcium phosphate cement compared with those filled with autograft (p <
0.05).
Figures A and B are AP and lateral radiographs of a right knee demonstrating a Schatzker II split-depression tibial plateau fracture.
Illustrations A shows, on the left, a photomicrograph of a subchondral defect treated with calcium phosphate demonstrating no subsidence and, on the right, a specimen treated with autologous bone graft showing subsidence.
InCORRECT Answers:
Answer 1: The compressive strength of coralline hydroxyapatite is only slightly greater than cancellous bone, but less than that of calcium phosphate.
Answer 2: Collagen-based matrices have compressive strength less than cancellous bone.
Answer 4: The compressive strength of calcium sulfate is similar to cancellous bone, but less than that of calcium phosphate.
Answer 5: The compressive strength of tricalcium phosphate is equal to or slightly less than cancellous bone.
765. In which of the following clinical scenarios would an urgent ophthalmology consultation be warranted to mitigate potential irreversible complications of the primary pathology?
1. A 4-year old male with proportionate dwarfism secondary to an autosomal recessive mutation resulting in L-alpha iduronidase deficiency.
2. A 5-year old male with proportionate dwarfism secondary to an X-linked recessive
mutation resulting in sulpho-iduronate-sulphatase deficiency
3. A 6-year old female with 2 months of persistent left knee swelling and associated stiffness, intermittent fever, and elevated ESR.
4. A 7-year old male with developmental delay, dolichostenomelia, and positive urine nitroprusside test secondary to a cystathionine b-synthase deficiency.
5. A 10-year old developmentally normal male with dolichostenomelia, generalized ligamentous laxity, and pecrus carinatum.
**CORRECT answer: 3**
Urgent ophthalmology consultation for slit lamp examination is warranted for the 6-year- old patient with juvenile idiopathic arthritis (JIA) in order to rule
out anterior uveitis. Ocular involvement in the disease process may lead to rapid and irreversible vision loss if not caught and appropriately treated early.
JIA is characterized by persistent arthritis in any individual joint for ≥6 weeks. The diagnosis of JIA is one of exclusion and requires onset of symptoms by age 16. The most common subtype of JIA is oligoarticular JIA, which typically
presents in females between 1-3 years of age, most often as morning stiffness and a relatively painless limp. The knee is most often affected. Uveitis is a common systemic manifestation of the disease process, and is most often asymptomatic, with up to 30% of patients experiencing loss of vision. This can be mitigated by early detection via slit lamp examination and subsequent ophthalmologic intervention.
Punaro reviews the presentation and orthoapedic manifestations of JIA. The authors note that while the diagnosis may be difficult due to the nonspecific presentation, early ophthalmologic evaluation is important for detection and treatment of ocular manifestations of the disease.
The Sherry article provides an overview of new treatment methods including intraarticular joint injections of methotrexate and etanercept, which have produced giant leaps in the treatment of the associated joint inflammation and resultant destruction.
InCORRECT answers:
Answer 1: This patient presents with Hurler syndrome, and while corneal clouding is characteristic, the process is due to glycosaminoglycan infiltration of the cornea and cannot be mitigated by ophthalmologic intervention.
Answer 2: This patient presents with Hunter syndrome, which may sometimes present with mild corneal clouding similar to Hurler syndrome, but is more often associated with clear corneas.
Answer 4: This patient presents with homocysteinuria. Although inferior lens dislocation is common, this is not an urgent diagnosis and does not result in irreversible blindness. Ophthalmologic intervention cannot prevent but is required to treat this complication.
Answer 5: This patient presents with Marfan's syndrome. Superior lens dislocation is common with this pathology, but similar to homocysteinuria, this is not an urgent diagnosis and cannot be prevented by early ophthalmologic evaluation.
766. A 42-year-old healthy woman presents to the emergency department with the injury shown in figures A and B. She undergoes the procedure shown in figures C and D. Which of the following is true regarding this procedure?
1. Fracture fragments must be cleaned and aligned anatomically
2. It relies on endochondral bone formation through chondrocyte proliferation and hypertrophy
3. It relies on endochondral bone formation through development of cutting cones
4. It relies on intramembranous bone formation through chondrycyte proliferation and hypertrophy
5. It relies on intramembranous bone formation though development of cutting cones
**CORRECT answer: 2**
The patient presents with an extra-articular distal tibia fracture and undergoes bridge plating. This method of fixation relies on endochondral bone formation through chondrocyte activity (secondary bone healing).
Fracture healing relies on complex interplay of biochemical and mechanical factors and can occur through intramembranous (primary bone healing)and endochondral bone formation (secondary bone healing). Primary bone healing relies on anatomic reduction, compression, and very little strain at the fracture site to allow for Haversian remodeling (development of cutting cones).
Absolute stability constructs lead to primary bone healing. Alternatively, secondary bone healing occurs in the periosteum and soft tissues in slightly higher strain environments. Relative stability constructs, such as intramedullary nails, external fixators, and bridge plates are examples of fixation that rely on secondary bone healing.
Perren reviews the biological and mechanical properties of bone remodeling and the complex interplay of patient, injury and surgical factors that influence healing. The use of relative stability fixation techniques allows bone to overcome the initial excess strain at a
fracture site and build a scaffold that brings the strain to more reasonable levels. The author stresses the importance of understanding bone biology to select optimal implant and methods of surgical fixation.
Figures A and B are AP and lateral radiographs, respectively, showing a comminuted distal tibia fracture. Figures C and D are post-operative radiographs after use of a bridge plating technique.
InCORRECT Answers:
Answer 1: This is usually required for primary bone healing
Answer 3: Cutting cones are seen in Haversian remodeling during primary bone healing
Answer 4, 5: Intramembranous bone formation occurs during primary bone healing and would not be present in this case.
767. A 61-year-old female smoker has a dual-energy x-ray absorptiometry scan at the femoral neck with a T-score of -1.5. She has a seizure disorder and takes phenytoin. According to the World Health Organization Fracture Risk Assessment Tool (FRAX), she has a ten year probability of sustaining a hip fracture of 4.8% and a ten- year probablity of sustaining a major osteoporotic fracture of 8%. In addition to a smoking cessation program, what is the most appropriate next step in treatment?
1. Initiate 1200 mg of calcium and repeat scan in 6 months
2. Initiate 800 units of Vitamin D and repeat scan in 6 months
3. Initiate 1200 mg of calcium, 800 units of Vitamin D, and repeat scan in 1 year
4. Initiate 1200 mg of calcium, 800 units of Vitamin D, begin bisphosphonate therapy, refer to neurologist to replace/discontinue phenytoin, and repeat scan in 1 year
5. Initiate 1200 mg of calcium, 800 units of Vitamin D, refer to neurologist to replace/discontinue phenytoin, and repeat scan in 1 year
**CORRECT answer: 4**
This patient has osteopenia and the FRAX assessment shows a ten-year probability of sustaining a hip fracture of >3%, which necessitates pharmacologic treatment and repeat scan in 1 year.
Osteoporosis is a systemic skeletal disorder that is characterized by the loss of bone tissue, disruption of bone architecture, and bone fragility, leading to an increased risk of fractures. Bone loss and low bone mass are asymptomatic until fractures occur.
Osteopenia is defined as a T score of -1 to -2.5 and osteoporosis is defined by a T score of < -2.5. Risk factors for osteoporosis are found in illustration A.
Unnanuntana et al. report that due to the limitations to DEXA, the FRAX was developed. The aim of FRAX is to provide an assessment tool for the prediction of fractures in men and women with use of clinical risk factors with or without femoral neck bone mineral
density. When reviewing the FRAX results, they recommend initiating treatment when there is a ten-year risk of hip fracture
>3% or a ten-year risk of a major osteoporosis-related fracture >20%.
Cosman et al. review the the 2008 National Osteoporosis Foundation
guidelines and report that pharmacologic treatment for osteoporosis should be considered if patients are postmenopausal women or men > 50 AND meet one of the following criteria: have a prior hip or vertebral fracture, a T score -2.5
or less at the femoral neck or spine, a T score between -1.0 and -2.5 at the femoral neck or spine AND a 10-year risk of hip fracture greater than 3% or
10-year risk of major osteoporosis-related fracture greater than 20%. DEXA scans should be repeated every 1-2 years if patients are on pharmacologic treatment.
Illustration A is a table listing the risk factors for osteoporosis. InCORRECT Answers:
Answers 1, 2, 3, and 5 do not include the CORRECT treatment which is 1200 mg
of calcium, 800 units of Vitamin D, bisphosphonate therapy, addressing the phenytoin side effects, and repeat scan in 1 year.
768. Which of the following statements about Familial Hypophosphatemic Rickets (Vitamin D resistant Rickets) is TRUE?
1. It is the second most common form of heritable rickets behind Type I Hereditary Vitamin D-Dependent Rickets
2. It is caused by inability of renal tubules to absorb phosphate
3. Leads to decreased vertical physeal width
4. There is a associated hyperphosphatemia
5. Early treatment with calcitriol results in completely normal bone mineralization
**CORRECT answer: 2**
Familial Hypophosphatemic Rickets results from a genetic defect of the PHEX gene that ultimately leads to renal phosphate wasting due to the inability of the renal tubules to absorb phosphate.
Familial Hypophosphatemic Rickets, also known as X-linked hypophosphatemic rickets, has been linked to mutations in the phosphate-regulating endopeptidase homolog X-linked (PHEX) gene that result in increased
fibroblast growth factor 23 (FGF-23) levels and, in turn, renal phosphate wasting. Laboratory analysis will demonstrate hypophosphatemia and a slightly elevated alkaline phosphatase with otherwise normal vitamin D and
calcium levels. Patients usually present with genu varum, medial tibial torsion, and short stature. The mainstay of treatment involves vitamin D supplementation with surgical treatment indicated for patients with
progressive bone deformities despite adequate medical therapy.
Hunziker et al. performed a histological analysis quantifying chondrocyte growth of the proximal tibial physis in rats. The authors found that chondrocytes remained in a fixed location at the physis and in the late hypertrophic zone increased in cellular height by four- fold and cellular volume by ten-fold. During the vascular invasion of the primary spongiosa, they showed that approximately one chondrocyte was eliminated every three hours. The authors concluded that quantifying normal growth plate anatomy can help understand pathologies affecting the physis.
Sharkey et al. reviewed the medical and surgical management of X-linked hypophosphatemic rickets. Per the literature included, the authors recommended medical treatment consisting of calcitriol 20 to 30 ng/kg split into two to three doses per day as well as 20 to 40 mg/kg of elemental phosphorus split between three to five doses per day, to ensure a steady serum level. They recommended that treatment be followed with serial radiographs of the knee, height measurements, and serum labs to ensure an appropriate response to therapy and avoidance of treatment complications. The authors concluded that the mainstay of treatment is calcitriol and phosphate replacement, with surgery indicated for patients with progressive bone deformities.
Illustration A depicts an AP bilateral knee radiograph of a patient with X-linked Hypophosphatemic rickets demonstrating increased physeal vertical width. Illustration B is a table depicting serum marker findings in X-linked
Hypophosphatemic Rickets compared to other bone metabolic disorders.
InCORRECT Answers:
Answer 1: Familial Hypophosphatemic Rickets (Vitamin D resistant Rickets) is the most common form of heritable rickets.
Answer 3: Radiographs of patients with X-linked Hypophosphatemic Rickets will demonstrate increased physeal vertical width due to disrupted mineralization within the zone of provisional calcification as well as vascular invasion of the primary spongiosa. Answer 4: X-linked Hypophosphatemic Rickets patients will have hypophosphatemia and elevated alkaline phosphatase with normal calcium and vitamin D levels.
Answer 5: Treatment with calcitriol supplementation improves outcomes, reduces the risk of deformity recurrence following surgery, and improves height. However, there is still abnormal bone mineralization even with adequate calcitriol supplementation.
769. All of the following have been associated with increased postoperative bleeding due to their direct effect on platelet function EXCEPT:
1. St John’s Wort
2. Aged Garlic Extracts
3. Aspirin
4. Ginseng
5. Ginkgo biloba
**CORRECT answer: 1**
All of the following listed have been associated with increased postoperative bleeding due to their direct effect on platelet function EXCEPT St John’s wort, which exerts its effects on the CNS by inhibiting serotonin, norepinephrine, and dopamine reuptake by neurons.
Ginkgo biloba, ginseng, and garlic are all herbal remedies that have been associated with increased postoperative bleeding and related complications. All three are known to act directly on platelet function. Physicians should be
aware not only of prescribed medications but also alternative nutraceuticals, herbal medications, and dietary supplements that are used by the patient.
Ang-Lee et al. review common herbal medications and their physiologic effects. They emphasize during the preoperative evaluation, physicians should
explicitly elicit and document a history of herbal medication use. Physicians should be familiar with the potential perioperative effects of the commonly used herbal medications to prevent, recognize, and treat potentially serious problems associated with their use and discontinuation.
Bebbington et al. reported on persistent postoperative bleeding after total hip arthroplasty secondary to ginkgo biloba usage. They found the postoperative bleeding stopped 6 weeks after the ginkgo biloba usage was discontinued.
Illustration A shows the mechanism of aspirin, which targets cyclooxygenase
1, and thus inhibits the conversion of Arachiodonic acid to Prostaglandin. This leads to a decrease in platelet activation and aggregation.
InCORRECT Answers:
Answer 2: Aged garlic extracts inhibits platelet aggregation by increasing cyclic nucleotides and inhibiting fibrinogen binding and platelet shape change.
Answer 3: ASA inhibits coagulation by inhibiting the production of prostaglandins and thromboxanes through irreversible inactivation of the cyclooxygenase enzyme.
Answer 4: Ginseng works through antiplatelet activity of panaxynol, a constituent of ginseng.
Answer 5: Ginkgo biloba is a popular nutraceutical for patients who have early dementia, intermittent claudication secondary to peripheral vascular disease, vertigo, and tinnitus. It
is reported to improve mental alertness and cognitive deficiency. It has antiplatelet properties as a result of one of its components, ginkgolide B, which displaces platelet- activating factor from its receptor binding sight.
770. As a diaphyseal fracture heals, peripheral callus forms about the shaft axis, creating a structure with a substantially larger diameter than the original diaphyseal shaft. What biomechanical properties does this callus impart to the healing fracture site?
1. Callus decreases torsional stability and stiffness at the fracture site
2. Callus formation is random and unstructured and does not affect the local biomechanical properties
3. The callus decreases peak torque to failure with time
4. The callus increases the moment of inertia, resulting in less strain at the fracture site
5. The callus decreases the moment of inertia, increasing stress at the fracture site
**CORRECT answer: 4**
Callus formation is biomechanically beneficial because it increases the outer diameter of the bone, leading to an increase in stiffness, torsional strength, moment of inertia, and decreases resultant interfragmentary strain at the fracture site.
The biomechanical role of the peripheral callus is to provide initial stability to the fracture and to act as a scaffold for gradual mineralization. Because the bending stiffness of a structure is proportional to the 4th power of the diameter, a peripherally located callus provides substantial stability to the
fracture, despite the relatively low stiffness and strength of callus. For example, doubling the diameter of the callus increases the resistance to bending by a factor of 16. As mineralization progresses, the bending stiffness and strength of the healed fracture eventually may be substantially greater than that of the original, intact bone.
Augat et al. review the mechanical and biological aspects of fracture healing. They report that increased diameter of periosteal callus formation benefits healing by enlarging the cross-sectional area of area of the bridging tissue and reducing interfragmentary motion. Patients with osteoporosis are known to have decreased callus mineralization and biomechanical properties.
Illustration A demonstrates how diaphyseal fracture callus expands its diameter to increase stiffness, increase the moment of inertia, and decrease strain at the fracture site.
InCORRECT Answers:
Answer 1: Callus will increase torsional stability and stiffness, not decrease Answer 2: While callus formation may be randomly arranged initially, it quickly becomes orderly as the fracture heals and remodels according to Wolff's law. As stated above, callus formation influences the local biomechanical
properties.
Answer 3: Callus formation increases peak torque to failure
Answer 5: Callus will actually increase the moment of inertia and distribute stress at the fracture site.
771. A 55-year-old male has severe knee pain and swelling for 2 days. He denies nausea, vomiting, fevers, or chills. On exam, the patient has an erythematous knee with a large effusion. He has pain with
attempted range of motion. Radiographs are unremarkable. WBC, CRP, and ESR are within normal limits. The knee was aspirated and the
**WBC count was 20,000. A specimen from the aspirate is seen in Figure**
1. **What is the next best step in treatment?**
1. Begin empiric antibiotics
2. Begin oral NSAIDs
3. Begin treatment with allopurinol
4. Emergent irrigation and debridement of the knee
5. Obtain serum uric acid level
**CORRECT answer: 2**
This patient has an acute gouty attack. The best treatment at this time is the initiation of an oral NSAID such as indomethacin.
It is clinically difficult to differentiate gout from an acute septic joint. Arthrocentesis and joint fluid analysis are used to diagnose both conditions. Crystals found in the fluid are suggestive of gout, though they may also cause an elevation of the synovial WBC count. Patients with an acute gouty flare may not have elevated serum uric acid levels. The treatment of acute gout is generally with indomethacin or colchicine for those who cannot tolerate NSAIDs. Chronic gout is treated usually with allopurinol. A similar scenario
may be encountered with pseudogout. The treatment approach is similar with the addition of a corticosteroid injection acutely.
Shah et al. performed a retrospective study to determine the incidence of septic arthritis in the presence of joint crystals. They report that the presence of crystals cannot exclude septic arthritis with certainty. They found that only
1.5% of patients had synovial fluid samples with crystal disease and concomitant bacterial growth. They conclude that the incidence increases to
11% if the synovial WBC count is > 50,000 and 22% if the synovial WBC count is > 100,000.
Choi et al. performed a review to determine the links between dietary and other factors and the incidence of gout. They report that red meats, seafood, beer, and liquor increase the risk of gout while total protein, wine, and purine rich vegetables did not. They also note that dairy products may be protective. They conclude that adiposity, weight gain, hypertension, and diuretics were all independent risk factors for gout while weight loss is protective.
Figure A demonstrates monosodium urate crystals that are negatively birefringent crystals seen in gout.
InCORRECT Answers:
Answer 1: There is no indication to begin antibiotic therapy as all inflammatory markers are within normal limits and the synovial WBC is below 50,000. Answer 3: Allopurinol would be the long-term treatment for gout and is not indicated in an acute attack.
Answer 4: There is no indication for irrigation and debridement of a joint with an acute gouty attack.
Answer 5: Serum uric acid levels may be normal in those with an acute gouty attack. The diagnosis was made with aspiration.
772. In 2012, the American College of Chest Physicians (ACCP) brought forth changes to their guidelines on postoperative pharmacologic venous thromboembolism prophylaxis (VTEP) after total joint arthroplasty in order to converge with the American Academy of Orthopaedic Surgeons (AAOS).
Which of the following describes the change in surgeon practice patterns following the convergence of these guidelines?
1. An increase in the prescribing of ASA (aspirin) monotherapy
2. An increase in the prescribing of coumadin at INR goals of 2-3
3. An increase in the prescribing of low-molecular-weight heparin monotherapy
4. An increase in the use of elastic compressive stockings as monotherapy
5. An increase in the prescribing of fish oil as monotherapy
**CORRECT answer: 1**
In 2012, the ACCP supported ASA monotherapy compared with no prophylaxis. This brought about a convergence of ACCP and AAOS recommendations and led to a subsequent increase in the prescribing of ASA
monotherapy among orthopedic surgeons following total knee arthroplasty.
Following elective total hip or knee arthroplasty, post-operative VTE prophylaxis has been shown to significantly lower the risk of deep venous thrombosis compared to rates of 60% without chemoprophylaxis. The 2012
ACCP guidelines on VTE prophylaxis include ASA, low molecular weight heparin (LMWH), fondaparinux, apixaban, dabigatran, rivaroxaban, low-dose unfractionated heparin (LDUH), or adjusted-dose vitamin K antagonist (VKA) for a minimum of 10-14 days following elective joint arthroplasty surgery. The guidelines also recommend dual therapy of mechanical and chemoprophylaxis while inpatient.
Shah et al. looked at venous thromboembolism prophylaxis (VTEP) practice patterns before and after the ACCP guidelines in 2012 regarding the use of ASA monotherapy. They found a roughly 40% increase in the prescribing of ASA monotherapy on POD#1 and at discharge. They concluded that ASA was readily and rapidly incorporated into clinical practice and highlights how guidelines affect practice patterns.
Freedman et al. in a 2000 meta-analysis of randomized, controlled trials looked at postoperative VTE prophylaxis in patients following elective total hip arthroplasty. They found warfarin had the lowest risk of proximal deep vein thrombosis and no significant differences among agents with regard to the risk of fatal pulmonary embolism or of mortality with any cause. They concluded that the best prophylactic agent in terms of both efficacy and safety was warfarin.
InCORRECT Answers:
Answers 2, 3, 4, and 5: Following the ACCP and AAOS convergence regarding ASA monotherapy, prescribing patterns in ASA were found to increase.
773. SOX-9 is a key transcription factor involved in the differentiation of which of the following cell lineages?
1. Osteoclasts
2. Osteoblasts
3. Chondrocytes
4. Fibroblasts
5. SOX-9 is not a transcription factor, it is a transmembrane tyrosine kinase receptor
**CORRECT answer: 3**
SOX-9 is considered a “master switch” for the differentiation of cells of chondrocytic lineage.
As described in the review by Hoffman et al, SOX-9 binds to a critical consensus sequence in the collagen 2 (Col2) promoter to activate its transcription. Formation of the cartilage template involves a multi-step process in which prechondrogenic mesenchymal cells form condensations prior to differentiating into matrix-producing chondroblasts.
Retinoids, particularly retinoic acid, are among the numerous signaling molecules that have been implicated in this process. Efforts aimed at understanding the mechanisms by which expression of retinoic acid receptor attenuates chondroblast differentiation led to the discovery of the transcriptional activity of SOX-9.
774. Which of the following is NOT included in the best management of a elderly female newly diagnosed with a fragility fracture?
1. Hip and spine densitometry
2. Laboratory analysis for secondary causes of osteoporosis
3. Administration of calcium 1,500 mg/day
4. Administration of Vitamin D 400 to 800 IU/day
5. Low protein diet
**CORRECT answer: 5**
The management of fragility fractures includes both treatment of the diagnosed fracture and optimization of patient health to help prevent future fractures. Appropriate management includes densitometry, laboratory analysis for secondary causes of osteoporosis, and metabolic optimization to heal the current fracture with appropriate calcium, vitamin D, and a protein enriched diet. The referenced manuscript suggests bone mineral density testing to all women age 65 and older and men age 70 and older as well as appropriate levels of calcium and vitamin D to allow for fracture healing.
775. Which of the following chromosomal translocations is associated with osteosarcoma?
1. SYT-SSX1
2. CHOP-TLS
3. EWS-FLI1
4. FKHR-PAX3
5. no translocation associated
**CORRECT answer: 5**
Osteosarcoma has no associated chromosomal translocation, but often has a mutation in Rb gene (retinoblastoma gene).
Answer 1: Synovial cell sarcoma is characterized by translocation t(X;18) (p11;q11) in more than 90% of cases which causes the fusion gene is called the SYT-SSX1, SYT- SSX2, or SYT-SSX4. Answer 2: The consistent cytogenetic abnormality in myxoid liposarcoma is translocation t(12;16)(q13;p11.2). This involves fusion of the transcription factor gene CHOP, which is essential for adipocytic differentiation, to the translocated in liposarcoma (TLS) gene on chromosome 16. Answer 3: Translocation t(11;22) is one of a series of related translocations occurs in more than 95% of the Ewing sarcoma family of tumors. This translocation joins the Ewing sarcoma gene EWS on chromosome
22 to a gene of the ETS family, friend leukemia insertion (FLI1) on chromosome 11, creating an aberrant activating transcriptional factor. Answer
4: The alveolar subtype of rhabdomyosarcoma accounts for 31% of rhabdo cases and involves a unique translocation occurs between the FKHR gene on chromosome 13 and either the PAX3 gene on chromosome 2 (70%) or the PAX7 gene on chromosome 1 (30%).
776. Which of the following terms best describes failure to exercise the degree of diligence and care that a reasonable and prudent person would exercise under similar conditions?
1. Intent
2. Causation
3. Standard of care
4. Breach of duty
5. Damages
**CORRECT answer: 4**
Malpractice is defined as negligence by a healthcare provider that results in injury to a patient. Medical negligence comprises four elements: duty, breach of duty, causation, and damages.
The duty of the physician is to provide care equal to the same standard of care ordinarily executed by surgeons in the same medical specialty. Breach of duty occurs when action or failure to act deviates from the standard of care.
InCORRECT answers:
1: Intent is something that is intended; an aim or purpose.
2: Causation is present when it is demonstrated that failure to meet the standard of care was the direct cause of the patient’s injuries.
3: Standard of care is the level and type of treatment that would be expected in similar situations by treating physicians.
5: Damages are monies awarded as compensation for injuries sustained as the result of medical negligence.
777. Which of the following laboratory values would be consistent with nutritional rickets?
1. increased calcium level
2. increased phosphate level
3. decreased alkaline phosphatase level
4. increased vitamin D level
5. increased parathyroid hormone level
**CORRECT answer: 5**
With decreased vitamin D intake, intestinal calcium and phosphate absorption are reduced leading to hypocalcemia. Decreased serum calcium stimulates increased PTH (secondary hyperparathyroidism) that leads to bone resorption resulting in low to normal levels of serum calcium. Overall laboratory studies show low to normal calcium, low phosphate (excreted because of effect of PTH), increased PTH, low levels of vitamin D and increased alkaline phosphatase levels.
778. Ligaments are viscoelastic, meaning that their tensile strength is affected by:
1. Torsion and tension only
2. Orientation of applied strain
3. Rate of applied load
4. Compression only
5. Tension only
**CORRECT answer: 3**
Ligaments are viscoelastic material which means their stress-strain curve patterns are time/rate dependent (as a result of the internal friction).
The inital portion of the stress-strain curve, called the toe region, exhibits a high deformation/low force characteristic due to the uncrimping of collagen fibers and the elasticity of elastin. Next is the linear region where slippage within and then between collagen fibrils occurs. In this stage, ligaments gets stiffer (increased tensile strength) at higher strain rates.
Illustration A shows the different regions of the stress-strain curve.
779. Which of the following groups correctly identifies serologic tests that are required by the American Association of Tissue Banks (AATB) for musculoskeletal tissue allografts?
1. Cytomegalovirus, Hepatitis A, Hepatitis B, Hepatitis C, HIV, Syphillis
2. Cytomegalovirus, Hepatitis A, Hepatitis B, Hepatitis C, HIV
3. Hepatitis A, Hepatitis B, Hepatitis C, HIV, Syphillis
4. Hepatitis B, Hepatitis C, HIV, Syphillis
5. Hepatitis B, Hepatitis C, HIV
**CORRECT answer: 4**
The American Association of Tissue Banks performs screening testing on all allografts in addition to screening patients medical history. Specific tests include: HIV, HBV, HCV,
HTLV-I/II, and Syphilis (see [_www.aatb.or_ g for more](http://www.aatb.org/) info on screening process). Neither Cytomegalovirus (CMV) nor Hepatitis A is routinely tested for in the American Association of Tissue Banks for musculoskeletal tissue.
780. Which of the following is most often implicated as an etiology for a hypertrophic nonunion?
1. Malreduction with open plating
2. Smoking
3. Inadequate mechanical stability
4. Open injury with significant soft tissue stripping
5. Infection
**CORRECT answer: 3**
Hypertrophic nonunions are caused by inadequate stability, with callus formation by an appropriate biological response. Lack of biology leads to an atrophic nonunion.
Hypertrophic nonunions should be treated with a fixation construct that lends appropriate stability without creating a poor biological environment.
781. **Ca10(P04)6(OH)2 is the chemical formula of**
1. Calcium hydroxyapatite
2. Osteocalcium phosphate
3. Calcium pyrophosphate
4. Osteocalcin
5. Polymethylmethacrylate
**CORRECT answer: 1**
The chemical structure of hydroxyapatite is Ca10(PO4)6(OH)2. Hydroxyapatite is a naturally occurring mineral form of calcium apatite with the formula Ca5(PO4)3(OH), but is usually written Ca10(PO4)6(OH)2 to denote that the crystal unit cell comprises two entities. Up to 50% of bone by weight is made up of a modified form of hydroxyapatite. It is one of few materials that will support bone ingrowth and osseointegration when used in orthopaedic, dental and maxillofacial applications.
782. Which of the following best describes the benefits of implementing diversity and cultural competency in orthopaedic training programs?
1. Incorporating foreign languages in the residency curriculum to improve communication with members of diverse backgrounds.
2. Teaching the social stereotypes of diverse cultures to improve the delivery of healthcare.
3. Establishing racial and gender enrolment quotas in residency programs to better serve all members of the community.
4. Enhancing trainees knowledge of diverse cultures to improve patient- physician relationships, optimize patient access to orthopaedic care, and enhance the quality and delivery of care.
5. Promoting orthopaedic trainees to travel to other countries to obtain surgical experience in different cultures.
**CORRECT answer: 4**
The goals of diversity and cultural competency in orthopaedic training is to enhance the knowledge of patient-physician relationships in diverse cultural groups so to improve access and quality of orthopaedic care.
There is increasing cultural diversity within our populations. The ability to better serve a heterogenous population relies on the ability to enhance the knowledge of patient- physican relationships so that people of all backgrounds can better access and benefit from the healthcare system.
White et al. examined the need for diversity in orthopaedics. For example, African- Americans have higher infant mortality rates, shorter life expectancies, fewer joint replacements, and more amputations than caucasians. It was concluded that cultural competency in orthopaedics is good for patients and for the country.
Illustration A shows a 2008 NSF census of the USA population. InCORRECT Answers:
Answer 1: Incorporating languages into an orthopaedic curriculum would only benefit a small sub-population of patients and isolate many others.
Answer 2: Teaching social stereotypes of diverse cultures can be viewed as discriminatory towards those groups.
Answer 3: While healthcare facilities with diverse staff are more likely to influence and successfully treat a nations diverse population, quotas of racial and gender backgrounds in orthopaedic residency will not entirely address the complete cultural competency that is required of every orthopaedic surgeon.
Answer 5: Traveling to isolated countries will not give residents a complete understanding of cultural diversity.
783. A clinical study for lateral epicondylitis allocates 1 group to receive physical therapy for 4 weeks and another group a new oral medication for 4 weeks. Then the 2 groups immediately switch therapies with one another for the next 4 weeks. The half-life of the medication used in the study is 2 weeks. Which of the following best describes the bias that is present in this study design?
1. Recall bias
2. Verification bias
3. Washout period bias
4. Detection bias
5. Incorporation bias
**CORRECT answer: 3**
In a crossover study design, the washout period is the time between therapies, receiving no therapy, so that the effect of the first therapy is allowed to wear off. In this scenario, the medication's long half-life may continue to have effects after the first group (receiving the medication) has switched to the physical therapy treatment.
Verification bias occurs when results of a diagnostic test influence whether patients are assigned to a
treatment group. Incorporation bias occurs when someone studies a diagnostic test that includes features of the target outcome. Recall bias occurs when
patients who experience an adverse outcome have a different likelihood of recalling an exposure than others that don't have an adverse outcome. Detection bias occurs when one looks more carefully for an outcome in one specific group more than the other group(s). The review article by Kocher et al describes the basics of biostatistics for clinicians.
784. A 62-year-old man undergoes an uncomplicated total shoulder replacement 9 months ago. What is an appropriate choice of prophylactic antibiotics to be taken prior to dental work if he has no allergies?
1. Daptomycin 600 milligrams intravenous 2 hours prior to procedure
2. Cephalexin 2 grams oral 1 hour prior to procedure
3. Levaquin 500 milligrams oral 1 hour prior to procedure
4. Trimethoprim-sulfamethoxazole 2 tablets double-strength oral 1 hour prior to procedure
5. No antibiotics are necessary
**CORRECT answer: 5**
Antibiotics are not necessary for this uncomplicated shoulder arthroplasty situation.
785. Disruption of which of the following interrupts the major source of nutrients to the growth plate?
1. Diaphyseal artery
2. Metaphyseal artery
3. Perichondrial artery
4. Synovial fluid
5. Synovial blood vessels
**CORRECT answer: 3**
Blood supply to the growth plate is supplied both via the perichondrial artery, which is the main source of nutrients, and the epiphyseal artery, which supplies the proliferative zone of the growth plate.
In a parallel design trial, participants are randomized to 2 or more groups, each of which receives a different treatment or intervention. For example, Group A receives the drug and Group B receives the placebo. This type of
design allows for comparison between groups. In a crossover design clinical trial, both groups receive both interventions over a defined time period. For example, Groups A and B both receive the drug as well as the placebo. This allows for within-participant comparisons. In a cohort study, patient groups are followed over time on the basis of having or not having received an exposure. Cohort studies are not randomized. In a case series, patients often receive a particular treatment and the outcomes are then examined.
726. An otherwise healthy 50-year-old man who is a smoker undergoes a posterior spine fusion with instrumentation for spondylolisthesis. What can the patient do to minimize his risk for pseudarthrosis?
1. Increase calcium and vitamin D intake
2. Avoid all nonsteroidal anti-inflammatory drugs (NSAIDs)
3. Maintain smoking cessation
4. Engage in early physical therapy to strengthen the trunk musculature
**CORRECT answer: 3**
Smoking is the biggest risk factor for nonunion and should be strictly avoided. NSAIDs interfere with bone healing, but not as strongly as smoking. Early mobilization would potentially stress the construct, inducing movement that leads to nonunion. Without history of calcium and vitamin D deficiency, increasing intake would not decrease the risk of nonunion.
727. When making a comparison to autograft incorporation, the inflammatory process in allograft tissue anterior cruciate ligament (ACL) reconstruction
1. occurs earlier.
2. occurs later.
3. is prolonged.
4. is shortened.
**CORRECT answer: 3**
Compared to similar autograft, allograft tissue demonstrates a prolonged inflammatory response, slower rate of biological incorporation and remodeling, and a higher proportion of large-diameter collagen fibrils. Native ACL inserts
into bone through a transition of 4 distinct zones: tendon, unmineralized fibrocartilage, mineralized fibrocartilage, and bone. This transition is not reproduced with tendon grafts, which instead heal with interposed fibrovascular scar at the graft-tunnel interface. The scar rapidly remodels to form perpendicular fibers resembling Sharpey fibers and, eventually, mature bone growth into the outer portion of the graft. The intra- articular portion of allograft undergoes an initial phase of necrosis followed by repopulation by host synovial cells into the acellular collagen scaffold.
Revascularization and maturation complete the ligamentization of graft tissue.
728. A researcher decides she wants to look at the current total number of patients who have methicillin-resistant** _Staphylococcus aureus_**(MRSA) infections in a hospital on 1 particular day. What is the researcher measuring?
1. Correlation coefficient of MRSA
2. Prevalence of MRSA
3. Incidence of MRSA
4. Relative risk of MRSA
**CORRECT answer: 2**
The prevalence of a disease is a measure of the number of cases of a disease at or during a specific time point or time period. In this case, the researcher wants to know the prevalence of disease on a given day. Incidence measures new cases of a disease or event per unit of time. Correlation coefficient is a measure of how 2 things correlate with one another, while relative risk is a statistical outcome that is often used in case-control or cohort studies to provide a measure of the risk of a particular disease occurring when a certain exposure has already occurred.
729. A 48-year-old man who is scheduled to undergo total knee replacement has an X-linked clotting disorder that leads to abnormal bleeding and recurrent, spontaneous hemarthrosis. Before undergoing surgery, he should have replacement therapy of
1. protein C and S.
2. vitamin K.
3. von Willebrand factor.
4. factor VIII.
**CORRECT answer: 4**
Hemophilia A is an X-linked recessive deficiency of factor VIII that can lead to significant bleeding problems including recurrent spontaneous hemarthroses that can lead to synovitis and joint destruction. von Willebrand disease is a lack of von Willebrand factor that leads to decreased platelet aggregation; more commonly patients have mucosal bleeding and not hemarthroses. Vitamin K deficiency is not hereditary; it is typically attributable to inadequate dietary intake, malabsorption, and loss of storage sites from hepatocellular disease. Protein C and S deficiencies are autosomal-dominant diseases that lead to thrombosis, not bleeding, as protein C and S shut off thrombin formation.
730. What is the recommended optimal timing of presurgical antibiotic administration to prevent infection in patients undergoing total joint replacement surgery?
1. Within 1 hour before incision
2. Within 2 hours before incision
3. Immediately after incision
4. Within 1 hour after incision
**CORRECT answer: 1**
The current recommendation for antibiotic prophylaxis for major orthopaedic surgical procedures is to administer intravenous antibiotics within 1 hour of surgical incision. Redosing of antibiotics should occur 3 to 4 hours after the initial dose for procedures that extend beyond 3 to 4 hours. Little evidence supports postsurgical antibiotic use beyond 24 hours. As you move beyond 1 hour from time of administration of antibiotics, risk for infection increases and rates of bacterial cell death decline. It is not acceptable to
administer presurgical antibiotics after incision.
731. **Bacterial resistance to antibiotics in biofilm is an example of**
1. avoidance.
2. decreased susceptibility.
3. inactivation.
4. mutation. **CORRECT answer: 1**
Three basic mechanisms of antibiotic resistance have been identified: avoidance, decreased susceptibility, and inactivation. Biofilm formation is a classic example of avoidance, whereby the biofilm creates a physical barrier to the antibiotic. Bacteria can decrease their susceptibility to antibiotics by mutating the antibiotic target or generating a mechanism to inactivate the antibiotic. Biofilm formation develops when a sufficient mass of bacteria forms on a surface. The cell-to-cell signaling becomes sufficient to activate transcription of genes needed for biofilm formation in a process known as quorum sensing. Once the bacteria produce a mature biofilm, they enter a greatly reduced or stationary phase of growth. Lastly, high-shear
environments seem to stimulate biofilm production.
732. A patient with Paget disease who is intolerant of bisphosphonates is given calcitonin. What is the mechanism of action of calcitonin?
1. Promotes reabsorption of phosphate in the renal tubules
2. Interferes with osteoclast maturation
3. Interferes with intestinal absorption of calcium
4. Upregulates osteoblast formation
**CORRECT answer: 2**
Calcitonin is a hormone that reduces serum calcium concentration by directly interfering with osteoclast maturation via receptors. Calcitonin inhibits phosphate reabsorption and decreases calcium reabsorption in the kidneys. By attenuating cartilage breakdown and stimulating cartilage formation via inhibitory pathways of matrix metalloproteinases, calcitonin also has a
chondro-protective effect on articular cartilage. Calcitonin has no major effects on intestinal absorption of calcium, but may aid in small-bowel secretion of sodium, potassium, chloride, and water. Calcitonin also has no receptor effect on osteoblasts.
733. **A cartilage water content increase is the hallmark of which**
**osteoarthritis stage?**
1. Prearthritis
2. Early
3. Late
4. Terminal
**CORRECT answer: 2**
The first stage of osteoarthritis is marked by an increase in water content secondary to disruption of the matrix framework. This is followed by an increase in chondrocyte anabolic and catabolic activity in response to tissue damage. Wnt-induced signal protein 1 increases chondrocyte protease expression. Failure to restore tissue balance ultimately leads to continued destruction and osteoarthritis. One hallmark of osteoarthritic cartilage is a reduced repair mechanism attributable to decreased chondrocyte response to growth factor stimulation (transforming growth factor-alpha and insulin-like growth factor-1).
Mitochondrial dysfunction and increased production of reactive oxygen species may promote cell senescence, a progressive slowing of cellular activity. Microscopic evidence of cartilage degeneration begins with fibrillation of the superficial and transition zones, followed by disruption of the tidemark by subchondral blood vessels and eventual subchondral bone remodeling. This process ultimately leads to cartilage degradation with decreased water content in the late and terminal phases of osteoarthritis.
734. **What is the plasma half-life of warfarin?**
1. 1 to 2 hours
2. 4 to 6 hours
3. 12 to 18 hours
4. 36 to 42 hours
**CORRECT answer: 4**
Warfarin, which is dosed daily, can take 72 to 96 hours to reach therapeutic levels. It has a plasma half-life of 36 to 42 hours. Low-molecular heparins have a plasma half-life of 4 to 5 hours, and fondaparinux has a half-life of 17 to 21 hours. Warfarin will not affect the International Normalized Ratio (INR) until 2 to 3 days after it is given. Patients on chronic warfarin therapy should
have treatment stopped 3 to 5 days before elective surgery to allow the INR to normalize.
735. A 70-year-old woman with a body mass index (BMI) of 34 and a history of hypercholesterolemia has elected to undergo total hip arthroplasty. Her son recently learned he has Factor V Leiden following an episode of pulmonary embolism. What are this patient's risk factors for thromboembolic disease?
1. Type of surgery, age, and BMI
2. Type of surgery, hypercholesterolemia, and age
3. Age, BMI, and hypercholesterolemia
4. BMI, type of surgery, and hypercholesterolemia
**CORRECT answer: 1**
Risk stratification is one of the most critical clinical evaluations before undergoing total joint arthroplasty. Many factors have been identified to increase risk for venous thromboembolism (VTE). The major factors include previous VTE, obesity, type of surgery (such as total joint arthroplasty), hypercoagulable states, myocardial infarction, congestive heart failure, family history of VTE, and hormonal replacement therapy.
Hypercholesterolemia is not a risk factor for thromboembolic disease.
736. **DNA replication occurs during which phase of the cell cycle?**
1. M
2. S
3. R
4. G1
5. G2
**CORRECT answer: 2**
The cell cycle consists of four distinct phases: initial growth (G1), DNA replication/synthesis (S), a gap (G2), and mitosis (M) (see illustration).
The G1 and G2 phases of the cell cycle represent the “gaps” or growth phases in the cell cycle that occur between DNA synthesis and mitosis. G0 cells are in a stable state and have not entered the cell cycle. During the S phase, the DNA is synthesized and replicated. During the M phase or mitosis, all genetic material divides into two daughter cells.
The cells are diploid (2N) in the G0 and G1 phases. The cells become tetraploid (4N) at the end of S and for the entire G2 phases. There is no R phase in the cell cycle.
737. **What antithrombotic agent is a selective factor I0a inhibitor?**
1. Warfarin
2. Low-molecular-weight heparin
3. Rivaroxaban
4. Aspirin
**CORRECT answer: 3**
Rivaroxaban is a selective factor I0a inhibitor. Aspirin is a cyclooxygenase inhibitor. Low-molecular-weight heparin is a nonspecific anticoagulant. Warfarin is a vitamin K antagonist and reduces production of clotting factors II, VII, IX, and X.
738. A 68-year-old woman had advanced right knee arthritis and total knee replacement was planned. She learned she had primary biliary cirrhosis at age 41 and now has advancing liver failure. Preoperative coagulation tests show a baseline International Normalized Ratio (INR) of 1.36. Appropriate methods to prevent thromboembolic
**disease as recommended by the 2011 AAOS Clinical Practice Guideline,**_Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee_
**_Arthroplasty_****, include**
1. use of mechanical prophylaxis (eg, pneumatic calf compressors) while in the hospital.
2. oral warfarin with a goal INR between 2.0 and 3.0.
3. low-dose warfarin for 3 weeks postsurgically beginning 48 hours after surgery.
4. no prophylaxis because this patient already is partially anticoagulated secondary to her liver disease.
**CORRECT answer: 1**
The 2011 AAOS Clinical Practice Guideline, _Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee Arthroplasty_ , recommends the use of mechanical prophylaxis for patients at increased risk
for bleeding (including those with liver disease or hemophilia). This recommendation is the consensus of the workgroup that established these guidelines because there was insufficient evidence to justify a stronger recommendation in this clinical scenario. The other responses use no prophylaxis or pharmacological prophylaxis. Pharmacological prophylaxis is not recommended in patients who are at increased risk for bleeding.
739. The pharmacokinetics of which deep venous thrombosis (DVT) prophylactic agent are affected by liver function and dietary intake?
1. Dalteparin
2. Warfarin
3. Fondaparinux
4. Enoxaparin
**CORRECT answer: 2**
Warfarin is an oral vitamin K antagonist that is rapidly absorbed from the gastrointestinal tract. It accumulates in the liver, where it is metabolized and excreted. The pharmacokinetics of warfarin can be affected by certain drugs or disease states that influence liver function. Fondaparinux is a synthetic factor Xa inhibitor that is eliminated through the kidneys. Both Dalteparin and Enoxaparin are low-molecular-weight heparins that activate antithrombin and inhibit factors Xa and IIa. Like Fondaparinux, they are eliminated through the kidneys and should be used with caution in patients with kidney disease.
740. What infection-control measure has been shown to have the most notable impact in reducing surgical-site infections?
1. Intravenous antibiotic administration within 1 hour of surgical incision
2. Screening and decolonization of patients colonized with methicillin-resistant
Staphylococcus aureus
3. Horizontal laminar flow
4. Use of enclosed body exhaust suits
**CORRECT answer: 1**
Timely administration of prophylactic antibiotics is the most important factor shown to decrease surgical-site infections. The use of horizontal laminar flow and body exhaust suits has not been shown to significantly affect infection rates.
741. The resistance to pullout of a screw in osteoporotic bone is increased by all of the following EXCEPT?
1. Placement parallel to the trabecular pattern
2. Purchase in cortical bone
3. Use of a fixed angle (locking screw construct)
4. Tapping prior to screw placement
5. Augmentation with polymethylmethacrylate
**CORRECT answer: 4**
Of the options listed, tapping prior to screw placement is the only variable that does not increase the pullout strength of a screw in osteoporotic bone.
Cornell reviews internal fixation in osteoporotic bone. According to this article, the quality of the bone is the primary determinant of the holding power of an individual screw. Other factors that increase the pullout strength include fixation in cortical bone (cortical bone has greater mineral density and, therefore, greater resistance to screw pullout than trabecular bone), screws placed parallel to the trabecular pattern, and screw fixation augmented with PMMA. The addition of a locking plate will also increase the resistance to failure by creating a fixed angle construct. Tapping prior to placement of the screw has not been shown to increase resistance to pullout, on the contrary studies have shown
this decreases resistance to pullout.
Turner et al examined the holding strength of small and large diameter screws in healthy bovine and diseased human bone. They found the screw diameter, trabecular orientation of the bone, and mineral content of the bone all affect the holding strength. A larger diameter screw, parallel placement to the trabecular pattern, and purchase in bone with a higher density all increase the holding strength.
742. Gigantism affects which region of the growth plate labeled in Figure A?
1. A
2. B
3. C
4. D
5. E
**CORRECT answer: 3**
Gigantism, like achondroplasia, affects the proliferative zone (Region C of Figure A) of the growth plate. In Figure A, Region A is the epiphysis, Region B is the resting zone, Region D is the hypertrophic zone, and Region E is the metaphysis. Illustration A is another depiction of the physis which is labeled. Gigantism is typically caused by a pituitary adenoma which over secretes growth hormone. Its effect on the proliferative zone results in bone overgrowth and excessive height and limb length. Acromegaly may also be
caused by a pituitary adenoma that over secretes growth hormone, but has its effect once the physis has closed.
743. Plain radiographs do not provide an accurate assessment of bone mineral density (BMD) until what percentage of mineral has been lost?
1/. 5%
2/. 20%
3/. 40%
4/. 90%
**CORRECT answer: 3**
Radiographic evidence of BMD loss is not apparent until 40% reduction. Osteopenia should not be ruled out based on an apparently normal mineralized bone.
744. Figure 85 is the radiograph of a 3-year-old boy whose chief issue is knocked knees. His mother notes that she has a similar condition and required multiple surgeries as a child. She states that her son walks with an unsteady gait and is small for his age. He does not currently take any medications and is not under medical care for any disorders. What is the most appropriate next treatment step?
1. Recommend bilateral valgus-producing proximal femoral osteotomies to CORRECT coxa vara
2. Recommend bilateral medial distal femoral and proximal tibial hemiepiphyseal arrests to CORRECT genu valgum using guided growth
3. Obtain serum calcium, phosphorus, alkaline phosphatase, and vitamin D
studies and refer the patient to an endocrinologist for evaluation
4. Refer the patient to a geneticist to evaluate him for skeletal dysplasia
**CORRECT answer: 3**
The radiograph shows a patient with osteopenia; marked limb deformity, including bilateral coxa vara and bilateral genu valgum; and extreme physeal widening, which is pathonomonic for rickets. Although surgery to CORRECT the limb deformities may be appropriate, a definitive diagnosis first needs to be established, and, if possible, the patient needs to be treated medically. In cases in which limb realignment surgery has been performed without proper medial correction of the metabolic bone disease, the recurrence rate is high. Serum calcium, phosphorus, alkaline phosphatase, and vitamin D are appropriate screening studies for diagnosis of metabolic bone disease, and treatment is most commonly performed by an endocrinologist. A geneticist may play a role in establishing the cause of the disease, especially if there is a hereditary component, but this step should not delay the consultation with endocrinology.
745. A 45-year-old man is placed on indomethacin for heterotopic ossification prophylaxis following surgery for an acetabular fracture. What is the most likely side effect of this medication?
1. Renal failure
2. Hepatitis
3. Peripheral neuropathy
4. Deep vein thrombosis
5. Gastrointestinal ulceration
**CORRECT answer: 5**
Indomethacin, commonly used to prevent heterotopic ossification, is associated with a high rate of gastrointestinal toxicity.
Berger, in a case-based review of nonsteroidal anti-inflammatory use in Orthopaedics, notes that NSAIDs block the protective effect of prostaglandins on the gastrointestinal mucosa, in addition to causing variable rates of platelet dysfunction. Elderly patients using NSAIDS are estimated to have a 4 to 5 times increased relative risk of death due to gastrointestinal hemorrhage compared with matched cohorts. Indomethacin, in particular, has a high rate
of gastrointestinal complications when compared with other NSAIDs.
746. **What region of the physis does collagen type X play a prominent role?**
1. resting zone
2. proliferative zone
3. zone of hypertrophy
4. metaphysis
5. diaphysis
**CORRECT answer: 3**
Type X collagen is important for bone mineralization and is produced by hypertrophic chondrocytes in the zone of hypertrophy.
There are 4 zones of the physis. The first is the RESTING ZONE, which is characterized by widely dispersed chondrocytes, abundant matrix, and is relatively inactive in cell or matrix turnover. The second zone is the PROLIFERATIVE ZONE. It characterized by longitudinal columns of flattened cells, significant endoplasmic reticulum, high ionized calcium. The third zone is the HYPERTROPHIC zone. It is characterized by enlargement of cells,
persistent metabolic activity, accumulate and calcium, synthesize alkaline phosphatase and type X collagen, aiding in mineralization. The final zone, in the METAPHYSIS, comprises the primary and secondary spongiosa layers. These layers are characterized by vascular invasion and bone remodeling, respectively.
Illustration A shows a histological view of the phyeal zones. Zone C is the proliferative zone, Zone D is the hypertrophic zone, and Zone E is the metaphysis.
InCORRECT Answers:
Answers 1,2,3,5: collagen type X play the greatest role in the zone of hypertrophy.
747. Which of the following modalities has been shown to have a positive effect when treating early stages of complex regional pain syndrome?
1. Casting of the involved extremity
2. Plyometric exercises
3. Ultrasound therapy
4. Acupuncture
5. Gentle physiotherapy
**CORRECT answer: 5**
Complex regional pain syndrome type I (reflex sympathetic dystrophy) is defined as a disease that develops after an initial noxious or painful event which causes the development of pain and dysfunction out of proportion to the event. It sometimes cannot be linked to a specific physiologic process. Hyperesthesias, edema, and/or blood flow changes are prevalent. Type II (synonym for causalgia) has a known identifiable nerve injury. Hypotheses include increased sympathetic tone causes feedback loop, activation of nociceptors to neurons in spinal cord, continued ischemia, re-activation of pain receptors, and possibly unregulated sensitivity of alpha adrenergic receptors.
For treatment, early gentle physiotherapy is recommended for this condition. Aggressive passive range of motion is contraindicated in the early phases because it will provoke pain and inflammation. The primary goal of therapy is to decrease pain and prevent stiffness. Contrast baths can help desensitize
and improve blood flow, and TENS (transcutaneous electrical nerve stimulator) has been shown to have a positive outcome on CRPS type II only (those with identifiable nerve lesions). Illustration A shows the basic pathology of this
condition.
748. **The force generated by a muscle is most highly dependent on its**
1. cross-sectional area.
2. fiber type.
3. length.
4. morphology.
5. level of conditioning.
**CORRECT answer: 1**
The cross-sectional area of a muscle determines to a great extent the force generated by the muscle. The force of a muscle contraction is controlled by the amount of myofibrils that contract; the greater the amount of contracting myofibrils, the greater the force of contraction. Fiber types have less to do
with the force of contraction and more to do with the duration and speed of contraction. Muscle length affects contraction force through the Blix curve. The morphology of a muscle can affect the cross-sectional area by varying the angle of the fibers in relation to the force vector. Conditioning mostly affects duration and fatigability.
749. Arachidonic acid is directly metabolized by which of the following substances?
1. Carbonic anhydrase
2. HMG-CoA reductase
3. 1-lipoxygenase
4. Cyclooxygenase
5. Thromboxane synthetase
**CORRECT answer: 4**
Arachidonic acid is the common substrate that is directly metabolized by cyclooxygenase into the prostanoids including prostaglandins, prostacyclin and thromboxane.
Cyclooxygenase 1 enzyme, or COX-1, results in prostaglandins responsible for maintenance and protection of the GI tract. Cyclooxygenase-II enzyme, or COX-2, results in prostaglandins responsible for inflammation and pain. Leukotrienes are synthesized from arachidonic acid by 5-Lipoxygenase, not 1-Lipoxygenase. Mevalonate is involved in the HMG-CoA reductase pathway – the metabolic pathway that produces cholesterol (site of action of the statins). A diagram of arachidonic acid metabolism is provided in Illustration A.
750. A 50-year-old male sustains a closed head injury and closed femur fracture after falling off of a ladder. His GCS is currently 15, and he only speaks Spanish; he has several family members in the waiting room of the hospital. Which of the following is true regarding informed consent for fixation of his femur fracture?
1. Patient must be able to read the consent form
2. Patient must be able to sign the consent form
3. Patient does not need to be able to communicate in any manner to give his or her own informed consent
4. Patient must not be on any antidepressant medication prior to verbal or written informed consent
5. Patient should give verbal informed consent prior to narcotic administration
**CORRECT answer: 5**
The patient should give verbal informed consent by understanding the important risks and benefits (not necessarily every potential complication that could possibly occur), as well as the indications for and alternatives to a procedure. This should be performed prior to administration of narcotic medication. However, narcotic administration should not be delayed for patients in pain secondary to lack of availability of a written consent form, if the verbal conversation has occurred, as documentation of the consent process can still be performed prior to surgical intervention.
Wenger et al developed a survey of 102 orthopaedic surgeons who correctly answered a mean of nineteen (73%) of the 26 questions. The respondents appropriately handled questions involving economic aspects, truth-telling, confidentiality, and an incompetent colleague. However, there was less understanding of proper ethical conduct with regard to informed consent
(58%), the physician-patient relationship (72%), and end-of-life decision- making (78%). There was also an analysis of the inCORRECT responses by the surgeons in the survey: Nineteen percent of the 102 respondents thought that a patient must be able to read the consent form, 39% thought that the patient must understand all of the risks of the procedure, 12% did not think that the patient needed to be able to communicate in some fashion to give their own consent, and 29% indicated that the patient must not be taking any
medication with psychoactive effects.
The CORRECT answers include; discussing the important (not necessarily all) risks and benefits as well as the indications for and alternatives to a procedure, ability to communicate with a patient that will give their own
consent, and the use of antidepressant medications are not a preclusion to the informed consent process.
751. Which of the following factors is most critical to the success of a meniscal allograft transplantation?
1. Accurate graft size
2. Donor cell viability
3. Reestablishment of the central meniscal blood supply
4. Suppression of the immune response
5. Cryopreservation of the donor graft
**CORRECT answer: 1**
Success of a meniscal allograft transplantation is strongly dependent on accurate graft sizing, typically within 5% of the native meniscus. Previous studies have established that donor cell viability is not mandatory for the survival of these grafts since they are replaced by the recipient’s cells (at least peripherally) within several weeks. Thus, cryopreservation of the graft to ensure cell viability is not necessary. There is a limited immune response to musculoskeletal allografts; therefore, immunosuppression, as is required for visceral organ transplantation, is not indicated.
752. A 21-year-old collegiate scholarship football player has an episode of transient quadriplegia. An MRI scan of the cervical spine reveals cord edema and severe congenital spinal stenosis. The athlete has aspirations of playing on a professional level and demands that he
be allowed to play. The team physician should give what recommendation to the college?
1. Do not allow the athlete to return to football.
2. Allow the athlete to participate.
3. Allow the athlete to play only if he signs a waiver.
4. Suggest that the college and atahlete enter binding arbitration.
5. Allow the athlete to play with special equipment.
**CORRECT answer: 1**
Federal courts have ruled that a student-athlete does not have a constitutional right to participate in athletics against medical advice. As long as the student retains his scholarship, the college is under no legal or ethical obligation to allow the student to participate in sports. A waiver would not hold up in court and would not indemnify the college or the team physician against suit. No equipment has been shown to be effective
in preventing transient quadriplegia.
753. **All of the following substances inhibit osteoclast activity, EXCEPT?**
1. Tumor necrosis factor-alpha (TNF-a)
2. Osteoprotegerin
3. Calcitonin
4. Bisphosphonates
5. Denosumab
**CORRECT answer: 1**
Osteoclasts have been identified as a key cellular target in the treatment of many diseases including osteoporosis, particle-induced osteolysis in total joint arthroplasty, and tumor-induced osteolysis. As such, anti-osteoclastic agents are a hot topic of orthopaedic research.
Calcitonin and Osteoprotegerin are naturally occuring cytokines which act either on cell surface receptors (calcitonin receptor) or bind soluable mediators
(RANK-L) to inhibit osteoclasts. While two forms of bisphosphonates exist, both function to induce osteoclast apoptosis (programmed cell death). Denosumab is a monoclonal antibody to RANK-L which when given subcutaneously, binds and sequesters RANK-L, preventing it from stimulating RANK, a pro-osteoclastic receptor.
Schoppet et al wrote a comprehensive review of osteoprotegerin or OPG, a cytokine produced by many cells including osteoblasts and marrow stromal cells. It is a vital component in regulating bone resorption as it inhibits both osteoclast activation and differentiation by acting as a decoy receptor for RANK-L. The mechanism of RANK-L is seen in Illustration A.
754. A player on a professional football team sustains a knee injury and is diagnosed with an anterior cruciate ligament rupture. When employed as the team physician, your ethical obligation is to inform
1. the player but not the team.
2. the team but not the player.
3. neither the team nor the player.
4. both the team and the player.
5. the team, the player, and the media
**CORRECT answer: 4**
When you are employed as a team physician, you are obligated to inform the players and the team organization of all athletically relevant medical issues. This differs significantly from the normal rule of patient confidentiality. If the player came to see you and you were not the team physician, you may not inform the team unless the player so desires. As the team physician, you are not obligated to inform the media.
755. Protamine functions to reverse the pharmacologic effects of which of the following anti-coagulants?
1. Aspirin
2. Clopidogrel (e.g. plavix)
3. Low molecular weight heparin
4. Warfarin
5. Hirudin
**CORRECT answer: 3**
Protamine functions to partially reverse the pharmacologic effects of low molecular weight heparin (LMWH). Protamine may help to stop bleeding related to LWMH, although anti- factor Xa activity is not fully normalized by protamine. Vitamin K reverses the pharmacologic effect of warfarin. As aspirin
and clopidogrel function directly at the level of the platelet, there is no medical method to "reverse" these effects. Hirudin is a naturally occuring enzyme with anti-coagulant property in the salivary glands of leeches.
756. Storage of musculoskeletal allografts by cryopreservation is achieved by
1. replacing water in the tissue with alcohol to a moisture level of 5% and then using a vacuum process to remove the alcohol from the tissue.
2. maintaining maximum cellular viability of fresh tissue without long-term storage.
3. using chemicals to remove cellular water and controlled rate freezing to prevent
ice crystal formation.
4. freezing the graft twice and packaging the tissue without solution at minus 80 degrees C.
5. freezing the graft in water without an antibiotic solution soak during quarantine, with final storage in liquid nitrogen.
**CORRECT answer: 3**
Cryopreservation uses chemicals to remove cellular water and controlled rate freezing to prevent ice crystal formation. The tissue is procured, cooled to wet ice temperature for quarantine, and then stored in a container with cryoprotectant solution of dimethyl sulfoxide or glycerol which displaces the cellular water. The controlled rate freezing is then done to prevent ice crystal formation. Fresh allografts are not frozen in order to maintain maximum cellular viability, and this process limits the shelf life of osteochondral allografts. Freeze-drying involves replacement of water in the tissue with
alcohol to a moisture level of 5% and then uses a vacuum process to remove the alcohol from the tissue. Preparation of fresh frozen grafts involves freezing the graft twice and packaging the tissue without solution at minus 80 degrees C.
757. A new scientific study is completed investigating the use of a new technique for lumbar decompression. The prospective cohort study enrolled 400 total patients into two groups (laminectomy versus interspinous spacer) based on 80% power and beta value of 0.2. Patients were not randomized in the study. Results showed a greater improvement in pre to post operative Oswestry Disability Index (ODI) in the interspinous spacer group (38.4) versus laminectomy group (34.1). ODI scores can range from 0 (no disability) to 100 (maximum disability). P value was 0.002.
**Interpretation of these results suggests which of the following?**
1. The number needed to treat (NNT) is high
2. The study was underpowered due to use of a high beta value
3. Due to lack of randomization, the study is subject to the Hawthorne effect
4. The difference in the primary outcome was stastically significant but likely did not reach the minimum clinically important difference
5. The control group was improperly selected given their improvement in ODI scores
**CORRECT answer: 4**
While most outcome measures do not have a well-established minimal clinically important difference (MCID), a 4.3 point difference in ODI is well below any reported MCID. The results suggest that the difference in primary endpoint was statistically significant but likely did not reach the MCID.
Interpretation of clinical studies requires a basic understanding of statistical and clinical principles. While the traditionally reported p values can comment on the statistical significance of a comparison in a data set, it does not give any information regarding the clinical relevance of the result. The MCID for several clinical outcomes has been studied, but consensus does not exist on this value for most outcome measurements.
Nevertheless, the clinical relevance of a study finding is much stronger when it reaches
MCID and is statistically significant.
Vaccaro et al. prospectively investigated the management of type II dens fracture in geriatric patients. They found improved outcomes in patients
undergoing surgical management of these injuries based on the Neck Disability Index (NDI).
Young et al. evaluated the reliability and validity of the NDI in a prospective randomized study. They found an MCID of 7.5 and a minimum detectable change (MDC) of 10.2. Their findings suggest that 10 points should be used as MCID for the NDI.
Gatchel et al. comment on both the importance and difficulty of establishing MCID for outcome measures. They stress the importance of interpreting statistically significant results in the context of MCID.
InCORRECT Answers:
Answer 1: NNT is a measure used in studies assessing relative risk of certain disease states. It does not apply to this study.
Answer 2: The beta value and power used in this study are standard for most studies. Answer 3: Lack of randomization can lead to confounding. The Hawthorne effect refers to change in patient behavior when they know they are part of a study.
Answer 5: The study was comparing one surgical intervention to another. The control group was appropriately selected.
758. Which of the following is most likely to decrease surgical mortality and inpatient morbidity while simultaneously increasing surgical team adherence to life-saving steps in operating room crisis situations?
1. An intra-operative surgical team leader
2. A surgical checklist
3. The presence of a senior surgeon
4. Magnet certification of nursing staff
5. Exclusion of surgical residents from the operating room team
**CORRECT answer: 2**
The utilization of a surgical safety checklist has demonstrated substantial reductions in surgical morbidity and mortality. Checklist use has also demonstrated efficacy in increasing team adherence to life-saving care plans in operating room crises.
The World Health Organization concept of a surgical safety checklist concept was validated in 2009 as a way of improving surgical outcomes. Successful implementation of a surgical checklist relies upon surgeon leadership to educate staff on its rationale and the practical components of implementation in the operating room.
Haynes et al. evaluated a 19-item surgical safety checklist and evaluated its ability to reduce complications and deaths associated with surgery in a global population. Across 8 diverse hospitals in 8 cities around the world, their study demonstrated that implementation of a pre-surgical checklist resulted in a
50% reduction in mortality (1.5% to 0.8%) and a 37% reduction in inpatient complications (11% to 7%). The patients in the study were over the age of 16 and undergoing non- cardiac surgery.
Conley et al. evaluated the effectiveness of implementation of surgical safety checklists in five hospitals using a series of interviews conducted with surgeons. Analysis of the survey results demonstrated that effective implementation relied upon surgeon leadership to explain the necessity of the checklist and how to effectively implement its use. When surgeon leadership failed in these functions, hospital staff failed to comprehend the utility of the checklist and were not able to appropriately use it. These failures eventually led to institutional abandonment of the safety checklist.
Arriaga et al. evaluated the utility of checklists to guide the surgical team through intraoperative crisis situations (e.g., massive hemorrhage, cardiac arrest). Their study of 17 surgical teams undergoing 106 simulated surgical- crises demonstrated that use of a crisis checklist led to greater adherence to life-saving steps of a care plan. 97% of participants agreed that they desired a checklist to be present if a crisis were to occur while they themselves were undergoing surgery.
InCORRECT answers:
Answers 1, 3-5: None of these have consistently demonstrated substantive improvement in surgical morbidity and mortality.
759. Which of the following is true regarding the sequence of motor unit recruitment during muscle contracture?
1. The sequence is: slow twitch, fatigue-resistant units (1st); fast-twitch, easily fatigable units (2nd); fast-twitch, fatigue-resistant units (3rd)
2. The sequence is: slow twitch, fatigue-resistant units (1st); fast-twitch, fatigue-resistant units (2nd); fast-twitch, easily fatigable units (3rd)
3. The sequence is: slow twitch, fatigue-resistant units (1st); slow-twitch, easily fatigable units (2nd); fast-twitch, easily fatigable units (3rd)
4. The sequence is: fast-twitch, fatigue-resistant units (1st); fast-twitch, easily fatigable units (2nd); slow twitch, fatigue-resistant units (1st);
5. The sequence is: fast-twitch, easily fatigable units (1st); fast-twitch, fatigue- resistant units (2nd); slow twitch, fatigue-resistant units (1st);
**CORRECT answer: 2**
The order of muscle recruitment starts with Type I fibers (slow twitch, fatigue- resistant units), followed by Type II units that first includes Type IIa (fast- twitch, fatigue-resistant) and ends with Type IIb (fast-twitch, easily fatigable)
Motor units are recruited in order of size, starting with small sized units that generate low
force, progressing to larger units with increasing strength of muscle contraction. Type I slow oxidative motor units have a lower threshold for activation, activate under lower force requirements, and generate less force. Type II units have a higher threshold and activate during activities that require significant force. Type IIa fibers are fast oxidative/glycolytic and Type IIb fibers are fast glycolytic. The terms "slow" and "fast" refer to the speed that myosin ATPases split ATP. The easy fatigability of type IIb fibers occurs because (1) they rely on anaerobic glycolysis to produce ATP, resulting in accumulation of lactic acid, which brings about muscular fatigue and (2) their low capillary density.
Staron reviewed human muscle fiber types. They state that children (2-5y) have a higher percentage of type I fibers than newborns and adults. Aging causes loss of function from sarcopenia (loss of muscle mass, loss of motor units, particularly type II) and reduced maximum oxygen consumption begining at 25y. Regarding sex differences, females have muscles 40% smaller than men because of smaller fibers and fewer total numbers of fibers diameter cross-sectional area.
Illustration A shows the distribution of muscle fiber types. Illustrations B and C show the progression in muscle fiber activation.
InCORRECT Answers:
Answer 1: Type IIb units (fast-twitch, easily fatigable) are the last to be activated. Answer 3: There are no slow twitch, easily fatigable units (only slow twitch, fatigue- resistant units).
Answers 4 and 5: Fast-twitch units (Type II) are not activated initially. Untrained individuals cannot voluntarily activate all higher threshold type II motor units
760. Which of the following conditions exhibit the inheritance pattern shown in Figure A, assuming no new mutations?
1. Duchenne muscular dystrophy
2. Hunter's syndrome
3. Hemophilia
4. Spondyloepiphyseal dysplasia (SED) tarda
5. Diastrophic dysplasia
**CORRECT answer: 5**
The pedigree chart (males are squares and females are circles) shown in Figure A demonstrates an autosomal recessive trait.
Diastrophic dysplasia is the only autosomal recessive condition with all of the other options being X-linked recessive disorders. Along with Becker's MD these are the main orthopaedic X-linked recessive disorders.
There are many more autosomal recessive orthopaedic disorders. Autosomal recessive pedigrees often appear in both sexes with equal frequency, tend to skip generations, and affected offspring are usually born to unaffected parents. When both parents are heterozygote, approximately 1/4 of the progeny will be affected.
X-linked and autosomal dominant disorders will not skip generations.
X-linked recessive disorders will always have affected sons if the mother has the disease (this does not occur in the 3rd cross of Figure A on the far right).
761. Which of the following is NOT a component of the WHO surgical safety checklist?
1. Whether team members have introduced themselves
2. Whether antibiotics have been given within the last 60 minutes
3. Whether essential imaging is displayed
4. Whether the CORRECT implants are in the room and if the product representative needs to be present
5. Whether there is a risk of blood loss
**CORRECT answer: 4**
The WHO surgical safety checklist concerns all surgical specialties. Whether CORRECT implants are in the room and if the representative needs to be present is not a component of this checklist.
The WHO checklist has 3 phases: the sign in (before induction), the time out (before skin incision), and the sign out (before the patient leaves the room). According to the WHO checklist, the steps that must occur prior to induction of anesthesia include checking the patient’s identity, procedure, consent, and signed surgical site are confirmed; an anesthesia safety check that includes evaluation for a difficult airway and aspiration risk is performed; and determination of risk for excessive blood loss is completed. Other features of this checklist are found in Illustration A.
Haynes et al. reviewed outcomes at 8 hospitals in 8 cities before and after introduction of the WHO surgical safety checklist. They found that the death rates were 1.5% and 0.8% and complication rates were 11.0% and 7.0% before and after introduction, respectively (p<0.05 for both).
Illustration A shows the WHO surgical safety checklist InCORRECT Answers:
Answers 1,2,3,5: These are all components of the WHO surgical safety checklist.
See Illustration A.
762. A 25-year-old female falls off her bike around 10:30 PM and sustains the closed injury seen in figures A and B. On exam, she is neurovascularly intact, but reports severe pain with finger flexion or extension. The chief resident calls the attending who reports he is at a benefit event and has had a few drinks, but feels fine and can operate on the patient in 1 hour and demands that the case be scheduled. When the attending arrives, he seems more jovial than normal. After the time out is complete, he reports he is feeling tired and is going to take a nap in the lounge, but he is confident the chief resident can complete the case. What should the resident do next?
1. Start the case and wake the surgeon up if any problems arise
2. Perform a closed reduction, apply a sugar tong splint, and schedule the case electively
3. Complete the case if she is confident she can do it
4. Express concern to the attending about his impairment
5. Wait for the surgeon to regain sobriety
**CORRECT answer: 4**
The surgeon in this case is likely impaired. It is the duty of the resident to confront the attending regarding his potential impairment, and if the surgeon insists on proceeding, to report the attending to another attending or department chief before the patient is put in a more dangerous situation.
The AAOS Code of Ethics and Professionalism for Orthopaedic Surgeons states surgeons "should be attuned to evolving mental or physical impairment, both in themselves and in their colleagues, and take or encourage necessary measures to ensure patient safety." The AMA code of medical ethics reports that physicians have an obligation to intervene to prevent their impaired colleagues from harming a patient. By reporting the impaired physician one might be saving him/her from medicolegal troubles down the road.
Oreskovich et al. conducted a nationwide survey of physicians across all medical specialties (26.7% response rate) and found that 12.9% of male physicians and 21.4% of female physicians met criteria for alcohol abuse/dependence. Younger physicians and depressed physicians were more likely to abuse alcohol. Dermatologists and orthopaedic surgeons were the medical specialties most likely to abuse alcohol while pediatrics and neurology were the least likely.
Dyrbye et al. conducted a cross-sectional survey of medical students (35% response rate) to assess how burnout and depression may affect students' willingness to report impaired colleagues. They determined that students with evidence of burnout or depression were significantly less likely to feel they should report colleagues impaired by mental health issues or substance abuse. The authors concluded that not only is more explicit training regarding professional responsibilities needed, but maintaining wellness is critical in the individual's willingness to fulfill their professional roles.
Figures A and B show displaced radius and ulna shaft fractures. InCORRECT Answers:
Answer 1 & 3: Even if the chief resident is capable of completing the case independently, it is inappropriate for a resident to operate without adequate supervision.
Answer 2: Closed reduction, splinting, and elective management would be inappropriate in this patient as she may have an evolving compartment syndrome Answer 5: It is inappropriate to keep a patient under anesthesia for a prolonged time due to physician impairment. Additionally, the patient may have an evolving compartment syndrome that should be addressed emergently
763. What is the first class of antibody to appear in serum after exposure to a foreign antigen?
1. IgA
2. IgD
3. IgE
4. IgG
5. IgM
**CORRECT answer: 5**
IgM is the first class of antibody to appear in our serum after exposure to an antigen. IgG is the most abundant immunoglobulin in our body. IgA is the major class of antibody in external secretions such as intestinal mucus, bronchial mucus, saliva, and tears. IgE is important in conferring protection against parasites and is also increased in allergic reactions. The role of IgD is not known.
764. A 67-year-old female falls off of a step ladder while changing a lightbulb in her kitchen and sustains the injury shown in Figures A and B. During fixation, the surgeon elects to use an osteoconductive bone graft substitute. Which of the following has been shown to have highest early compressive strength?
1. Coralline hydroxyapatite
2. Collagen-based matrices
3. Calcium phosphate
4. Calcium sulfate
5. Tricalcium phosphate
**CORRECT answer: 3**
Of the above bone graft substitutes, calcium phosphate demonstrates the highest early compressive strength.
Calcium phosphate is an injectable compound comprised of inorganic calcium and phosphate that hardens in situ and cures by a crystallization reaction to form dahllite, a carbonated apatite similar to that found in the mineral phase of bone. Reduction and placement of internal fixation must be performed prior to application of the calcium phosphate. Compared to cancellous bone grafts and other bone graft substitutes, calcium phosphate, when hardened, has a much higher compressive strength (4 to 10 times greater than cancellous
bone) and may be useful in preventing subsequent displacement or depression of reduced articular fragments.
Russell et al. prospectively compared autologous bone graft to calcium phosphate cement in a randomized controlled trial of 119 patients. The baseline demographics including the height, weight, age, sex, and injury pattern were comparable. The authors found a significantly higher rate of articular subsidence in the three to twelve month
post-operative period with the bone graft group. They concluded that calcium phosphate was associated with greater compressive strength and less subsidence.
Welch et al. directly compared calcium phosphate and autologous bone graft used to fill subchondral defects created in an animal model. The authors found that the prevalence and degree of fracture subsidence was significantly reduced at all time-points, from 24 hours to 18 months, in the defects treated with calcium phosphate cement compared with those filled with autograft (p <
0.05).
Figures A and B are AP and lateral radiographs of a right knee demonstrating a Schatzker II split-depression tibial plateau fracture.
Illustrations A shows, on the left, a photomicrograph of a subchondral defect treated with calcium phosphate demonstrating no subsidence and, on the right, a specimen treated with autologous bone graft showing subsidence.
InCORRECT Answers:
Answer 1: The compressive strength of coralline hydroxyapatite is only slightly greater than cancellous bone, but less than that of calcium phosphate.
Answer 2: Collagen-based matrices have compressive strength less than cancellous bone.
Answer 4: The compressive strength of calcium sulfate is similar to cancellous bone, but less than that of calcium phosphate.
Answer 5: The compressive strength of tricalcium phosphate is equal to or slightly less than cancellous bone.
765. In which of the following clinical scenarios would an urgent ophthalmology consultation be warranted to mitigate potential irreversible complications of the primary pathology?
1. A 4-year old male with proportionate dwarfism secondary to an autosomal recessive mutation resulting in L-alpha iduronidase deficiency.
2. A 5-year old male with proportionate dwarfism secondary to an X-linked recessive
mutation resulting in sulpho-iduronate-sulphatase deficiency
3. A 6-year old female with 2 months of persistent left knee swelling and associated stiffness, intermittent fever, and elevated ESR.
4. A 7-year old male with developmental delay, dolichostenomelia, and positive urine nitroprusside test secondary to a cystathionine b-synthase deficiency.
5. A 10-year old developmentally normal male with dolichostenomelia, generalized ligamentous laxity, and pecrus carinatum.
**CORRECT answer: 3**
Urgent ophthalmology consultation for slit lamp examination is warranted for the 6-year- old patient with juvenile idiopathic arthritis (JIA) in order to rule
out anterior uveitis. Ocular involvement in the disease process may lead to rapid and irreversible vision loss if not caught and appropriately treated early.
JIA is characterized by persistent arthritis in any individual joint for ≥6 weeks. The diagnosis of JIA is one of exclusion and requires onset of symptoms by age 16. The most common subtype of JIA is oligoarticular JIA, which typically
presents in females between 1-3 years of age, most often as morning stiffness and a relatively painless limp. The knee is most often affected. Uveitis is a common systemic manifestation of the disease process, and is most often asymptomatic, with up to 30% of patients experiencing loss of vision. This can be mitigated by early detection via slit lamp examination and subsequent ophthalmologic intervention.
Punaro reviews the presentation and orthoapedic manifestations of JIA. The authors note that while the diagnosis may be difficult due to the nonspecific presentation, early ophthalmologic evaluation is important for detection and treatment of ocular manifestations of the disease.
The Sherry article provides an overview of new treatment methods including intraarticular joint injections of methotrexate and etanercept, which have produced giant leaps in the treatment of the associated joint inflammation and resultant destruction.
InCORRECT answers:
Answer 1: This patient presents with Hurler syndrome, and while corneal clouding is characteristic, the process is due to glycosaminoglycan infiltration of the cornea and cannot be mitigated by ophthalmologic intervention.
Answer 2: This patient presents with Hunter syndrome, which may sometimes present with mild corneal clouding similar to Hurler syndrome, but is more often associated with clear corneas.
Answer 4: This patient presents with homocysteinuria. Although inferior lens dislocation is common, this is not an urgent diagnosis and does not result in irreversible blindness. Ophthalmologic intervention cannot prevent but is required to treat this complication.
Answer 5: This patient presents with Marfan's syndrome. Superior lens dislocation is common with this pathology, but similar to homocysteinuria, this is not an urgent diagnosis and cannot be prevented by early ophthalmologic evaluation.
766. A 42-year-old healthy woman presents to the emergency department with the injury shown in figures A and B. She undergoes the procedure shown in figures C and D. Which of the following is true regarding this procedure?
1. Fracture fragments must be cleaned and aligned anatomically
2. It relies on endochondral bone formation through chondrocyte proliferation and hypertrophy
3. It relies on endochondral bone formation through development of cutting cones
4. It relies on intramembranous bone formation through chondrycyte proliferation and hypertrophy
5. It relies on intramembranous bone formation though development of cutting cones
**CORRECT answer: 2**
The patient presents with an extra-articular distal tibia fracture and undergoes bridge plating. This method of fixation relies on endochondral bone formation through chondrocyte activity (secondary bone healing).
Fracture healing relies on complex interplay of biochemical and mechanical factors and can occur through intramembranous (primary bone healing)and endochondral bone formation (secondary bone healing). Primary bone healing relies on anatomic reduction, compression, and very little strain at the fracture site to allow for Haversian remodeling (development of cutting cones).
Absolute stability constructs lead to primary bone healing. Alternatively, secondary bone healing occurs in the periosteum and soft tissues in slightly higher strain environments. Relative stability constructs, such as intramedullary nails, external fixators, and bridge plates are examples of fixation that rely on secondary bone healing.
Perren reviews the biological and mechanical properties of bone remodeling and the complex interplay of patient, injury and surgical factors that influence healing. The use of relative stability fixation techniques allows bone to overcome the initial excess strain at a
fracture site and build a scaffold that brings the strain to more reasonable levels. The author stresses the importance of understanding bone biology to select optimal implant and methods of surgical fixation.
Figures A and B are AP and lateral radiographs, respectively, showing a comminuted distal tibia fracture. Figures C and D are post-operative radiographs after use of a bridge plating technique.
InCORRECT Answers:
Answer 1: This is usually required for primary bone healing
Answer 3: Cutting cones are seen in Haversian remodeling during primary bone healing
Answer 4, 5: Intramembranous bone formation occurs during primary bone healing and would not be present in this case.
767. A 61-year-old female smoker has a dual-energy x-ray absorptiometry scan at the femoral neck with a T-score of -1.5. She has a seizure disorder and takes phenytoin. According to the World Health Organization Fracture Risk Assessment Tool (FRAX), she has a ten year probability of sustaining a hip fracture of 4.8% and a ten- year probablity of sustaining a major osteoporotic fracture of 8%. In addition to a smoking cessation program, what is the most appropriate next step in treatment?
1. Initiate 1200 mg of calcium and repeat scan in 6 months
2. Initiate 800 units of Vitamin D and repeat scan in 6 months
3. Initiate 1200 mg of calcium, 800 units of Vitamin D, and repeat scan in 1 year
4. Initiate 1200 mg of calcium, 800 units of Vitamin D, begin bisphosphonate therapy, refer to neurologist to replace/discontinue phenytoin, and repeat scan in 1 year
5. Initiate 1200 mg of calcium, 800 units of Vitamin D, refer to neurologist to replace/discontinue phenytoin, and repeat scan in 1 year
**CORRECT answer: 4**
This patient has osteopenia and the FRAX assessment shows a ten-year probability of sustaining a hip fracture of >3%, which necessitates pharmacologic treatment and repeat scan in 1 year.
Osteoporosis is a systemic skeletal disorder that is characterized by the loss of bone tissue, disruption of bone architecture, and bone fragility, leading to an increased risk of fractures. Bone loss and low bone mass are asymptomatic until fractures occur.
Osteopenia is defined as a T score of -1 to -2.5 and osteoporosis is defined by a T score of < -2.5. Risk factors for osteoporosis are found in illustration A.
Unnanuntana et al. report that due to the limitations to DEXA, the FRAX was developed. The aim of FRAX is to provide an assessment tool for the prediction of fractures in men and women with use of clinical risk factors with or without femoral neck bone mineral
density. When reviewing the FRAX results, they recommend initiating treatment when there is a ten-year risk of hip fracture
>3% or a ten-year risk of a major osteoporosis-related fracture >20%.
Cosman et al. review the the 2008 National Osteoporosis Foundation
guidelines and report that pharmacologic treatment for osteoporosis should be considered if patients are postmenopausal women or men > 50 AND meet one of the following criteria: have a prior hip or vertebral fracture, a T score -2.5
or less at the femoral neck or spine, a T score between -1.0 and -2.5 at the femoral neck or spine AND a 10-year risk of hip fracture greater than 3% or
10-year risk of major osteoporosis-related fracture greater than 20%. DEXA scans should be repeated every 1-2 years if patients are on pharmacologic treatment.
Illustration A is a table listing the risk factors for osteoporosis. InCORRECT Answers:
Answers 1, 2, 3, and 5 do not include the CORRECT treatment which is 1200 mg
of calcium, 800 units of Vitamin D, bisphosphonate therapy, addressing the phenytoin side effects, and repeat scan in 1 year.
768. Which of the following statements about Familial Hypophosphatemic Rickets (Vitamin D resistant Rickets) is TRUE?
1. It is the second most common form of heritable rickets behind Type I Hereditary Vitamin D-Dependent Rickets
2. It is caused by inability of renal tubules to absorb phosphate
3. Leads to decreased vertical physeal width
4. There is a associated hyperphosphatemia
5. Early treatment with calcitriol results in completely normal bone mineralization
**CORRECT answer: 2**
Familial Hypophosphatemic Rickets results from a genetic defect of the PHEX gene that ultimately leads to renal phosphate wasting due to the inability of the renal tubules to absorb phosphate.
Familial Hypophosphatemic Rickets, also known as X-linked hypophosphatemic rickets, has been linked to mutations in the phosphate-regulating endopeptidase homolog X-linked (PHEX) gene that result in increased
fibroblast growth factor 23 (FGF-23) levels and, in turn, renal phosphate wasting. Laboratory analysis will demonstrate hypophosphatemia and a slightly elevated alkaline phosphatase with otherwise normal vitamin D and
calcium levels. Patients usually present with genu varum, medial tibial torsion, and short stature. The mainstay of treatment involves vitamin D supplementation with surgical treatment indicated for patients with
progressive bone deformities despite adequate medical therapy.
Hunziker et al. performed a histological analysis quantifying chondrocyte growth of the proximal tibial physis in rats. The authors found that chondrocytes remained in a fixed location at the physis and in the late hypertrophic zone increased in cellular height by four- fold and cellular volume by ten-fold. During the vascular invasion of the primary spongiosa, they showed that approximately one chondrocyte was eliminated every three hours. The authors concluded that quantifying normal growth plate anatomy can help understand pathologies affecting the physis.
Sharkey et al. reviewed the medical and surgical management of X-linked hypophosphatemic rickets. Per the literature included, the authors recommended medical treatment consisting of calcitriol 20 to 30 ng/kg split into two to three doses per day as well as 20 to 40 mg/kg of elemental phosphorus split between three to five doses per day, to ensure a steady serum level. They recommended that treatment be followed with serial radiographs of the knee, height measurements, and serum labs to ensure an appropriate response to therapy and avoidance of treatment complications. The authors concluded that the mainstay of treatment is calcitriol and phosphate replacement, with surgery indicated for patients with progressive bone deformities.
Illustration A depicts an AP bilateral knee radiograph of a patient with X-linked Hypophosphatemic rickets demonstrating increased physeal vertical width. Illustration B is a table depicting serum marker findings in X-linked
Hypophosphatemic Rickets compared to other bone metabolic disorders.
InCORRECT Answers:
Answer 1: Familial Hypophosphatemic Rickets (Vitamin D resistant Rickets) is the most common form of heritable rickets.
Answer 3: Radiographs of patients with X-linked Hypophosphatemic Rickets will demonstrate increased physeal vertical width due to disrupted mineralization within the zone of provisional calcification as well as vascular invasion of the primary spongiosa. Answer 4: X-linked Hypophosphatemic Rickets patients will have hypophosphatemia and elevated alkaline phosphatase with normal calcium and vitamin D levels.
Answer 5: Treatment with calcitriol supplementation improves outcomes, reduces the risk of deformity recurrence following surgery, and improves height. However, there is still abnormal bone mineralization even with adequate calcitriol supplementation.
769. All of the following have been associated with increased postoperative bleeding due to their direct effect on platelet function EXCEPT:
1. St John’s Wort
2. Aged Garlic Extracts
3. Aspirin
4. Ginseng
5. Ginkgo biloba
**CORRECT answer: 1**
All of the following listed have been associated with increased postoperative bleeding due to their direct effect on platelet function EXCEPT St John’s wort, which exerts its effects on the CNS by inhibiting serotonin, norepinephrine, and dopamine reuptake by neurons.
Ginkgo biloba, ginseng, and garlic are all herbal remedies that have been associated with increased postoperative bleeding and related complications. All three are known to act directly on platelet function. Physicians should be
aware not only of prescribed medications but also alternative nutraceuticals, herbal medications, and dietary supplements that are used by the patient.
Ang-Lee et al. review common herbal medications and their physiologic effects. They emphasize during the preoperative evaluation, physicians should
explicitly elicit and document a history of herbal medication use. Physicians should be familiar with the potential perioperative effects of the commonly used herbal medications to prevent, recognize, and treat potentially serious problems associated with their use and discontinuation.
Bebbington et al. reported on persistent postoperative bleeding after total hip arthroplasty secondary to ginkgo biloba usage. They found the postoperative bleeding stopped 6 weeks after the ginkgo biloba usage was discontinued.
Illustration A shows the mechanism of aspirin, which targets cyclooxygenase
1, and thus inhibits the conversion of Arachiodonic acid to Prostaglandin. This leads to a decrease in platelet activation and aggregation.
InCORRECT Answers:
Answer 2: Aged garlic extracts inhibits platelet aggregation by increasing cyclic nucleotides and inhibiting fibrinogen binding and platelet shape change.
Answer 3: ASA inhibits coagulation by inhibiting the production of prostaglandins and thromboxanes through irreversible inactivation of the cyclooxygenase enzyme.
Answer 4: Ginseng works through antiplatelet activity of panaxynol, a constituent of ginseng.
Answer 5: Ginkgo biloba is a popular nutraceutical for patients who have early dementia, intermittent claudication secondary to peripheral vascular disease, vertigo, and tinnitus. It
is reported to improve mental alertness and cognitive deficiency. It has antiplatelet properties as a result of one of its components, ginkgolide B, which displaces platelet- activating factor from its receptor binding sight.
770. As a diaphyseal fracture heals, peripheral callus forms about the shaft axis, creating a structure with a substantially larger diameter than the original diaphyseal shaft. What biomechanical properties does this callus impart to the healing fracture site?
1. Callus decreases torsional stability and stiffness at the fracture site
2. Callus formation is random and unstructured and does not affect the local biomechanical properties
3. The callus decreases peak torque to failure with time
4. The callus increases the moment of inertia, resulting in less strain at the fracture site
5. The callus decreases the moment of inertia, increasing stress at the fracture site
**CORRECT answer: 4**
Callus formation is biomechanically beneficial because it increases the outer diameter of the bone, leading to an increase in stiffness, torsional strength, moment of inertia, and decreases resultant interfragmentary strain at the fracture site.
The biomechanical role of the peripheral callus is to provide initial stability to the fracture and to act as a scaffold for gradual mineralization. Because the bending stiffness of a structure is proportional to the 4th power of the diameter, a peripherally located callus provides substantial stability to the
fracture, despite the relatively low stiffness and strength of callus. For example, doubling the diameter of the callus increases the resistance to bending by a factor of 16. As mineralization progresses, the bending stiffness and strength of the healed fracture eventually may be substantially greater than that of the original, intact bone.
Augat et al. review the mechanical and biological aspects of fracture healing. They report that increased diameter of periosteal callus formation benefits healing by enlarging the cross-sectional area of area of the bridging tissue and reducing interfragmentary motion. Patients with osteoporosis are known to have decreased callus mineralization and biomechanical properties.
Illustration A demonstrates how diaphyseal fracture callus expands its diameter to increase stiffness, increase the moment of inertia, and decrease strain at the fracture site.
InCORRECT Answers:
Answer 1: Callus will increase torsional stability and stiffness, not decrease Answer 2: While callus formation may be randomly arranged initially, it quickly becomes orderly as the fracture heals and remodels according to Wolff's law. As stated above, callus formation influences the local biomechanical
properties.
Answer 3: Callus formation increases peak torque to failure
Answer 5: Callus will actually increase the moment of inertia and distribute stress at the fracture site.
771. A 55-year-old male has severe knee pain and swelling for 2 days. He denies nausea, vomiting, fevers, or chills. On exam, the patient has an erythematous knee with a large effusion. He has pain with
attempted range of motion. Radiographs are unremarkable. WBC, CRP, and ESR are within normal limits. The knee was aspirated and the
**WBC count was 20,000. A specimen from the aspirate is seen in Figure**
1. **What is the next best step in treatment?**
1. Begin empiric antibiotics
2. Begin oral NSAIDs
3. Begin treatment with allopurinol
4. Emergent irrigation and debridement of the knee
5. Obtain serum uric acid level
**CORRECT answer: 2**
This patient has an acute gouty attack. The best treatment at this time is the initiation of an oral NSAID such as indomethacin.
It is clinically difficult to differentiate gout from an acute septic joint. Arthrocentesis and joint fluid analysis are used to diagnose both conditions. Crystals found in the fluid are suggestive of gout, though they may also cause an elevation of the synovial WBC count. Patients with an acute gouty flare may not have elevated serum uric acid levels. The treatment of acute gout is generally with indomethacin or colchicine for those who cannot tolerate NSAIDs. Chronic gout is treated usually with allopurinol. A similar scenario
may be encountered with pseudogout. The treatment approach is similar with the addition of a corticosteroid injection acutely.
Shah et al. performed a retrospective study to determine the incidence of septic arthritis in the presence of joint crystals. They report that the presence of crystals cannot exclude septic arthritis with certainty. They found that only
1.5% of patients had synovial fluid samples with crystal disease and concomitant bacterial growth. They conclude that the incidence increases to
11% if the synovial WBC count is > 50,000 and 22% if the synovial WBC count is > 100,000.
Choi et al. performed a review to determine the links between dietary and other factors and the incidence of gout. They report that red meats, seafood, beer, and liquor increase the risk of gout while total protein, wine, and purine rich vegetables did not. They also note that dairy products may be protective. They conclude that adiposity, weight gain, hypertension, and diuretics were all independent risk factors for gout while weight loss is protective.
Figure A demonstrates monosodium urate crystals that are negatively birefringent crystals seen in gout.
InCORRECT Answers:
Answer 1: There is no indication to begin antibiotic therapy as all inflammatory markers are within normal limits and the synovial WBC is below 50,000. Answer 3: Allopurinol would be the long-term treatment for gout and is not indicated in an acute attack.
Answer 4: There is no indication for irrigation and debridement of a joint with an acute gouty attack.
Answer 5: Serum uric acid levels may be normal in those with an acute gouty attack. The diagnosis was made with aspiration.
772. In 2012, the American College of Chest Physicians (ACCP) brought forth changes to their guidelines on postoperative pharmacologic venous thromboembolism prophylaxis (VTEP) after total joint arthroplasty in order to converge with the American Academy of Orthopaedic Surgeons (AAOS).
Which of the following describes the change in surgeon practice patterns following the convergence of these guidelines?
1. An increase in the prescribing of ASA (aspirin) monotherapy
2. An increase in the prescribing of coumadin at INR goals of 2-3
3. An increase in the prescribing of low-molecular-weight heparin monotherapy
4. An increase in the use of elastic compressive stockings as monotherapy
5. An increase in the prescribing of fish oil as monotherapy
**CORRECT answer: 1**
In 2012, the ACCP supported ASA monotherapy compared with no prophylaxis. This brought about a convergence of ACCP and AAOS recommendations and led to a subsequent increase in the prescribing of ASA
monotherapy among orthopedic surgeons following total knee arthroplasty.
Following elective total hip or knee arthroplasty, post-operative VTE prophylaxis has been shown to significantly lower the risk of deep venous thrombosis compared to rates of 60% without chemoprophylaxis. The 2012
ACCP guidelines on VTE prophylaxis include ASA, low molecular weight heparin (LMWH), fondaparinux, apixaban, dabigatran, rivaroxaban, low-dose unfractionated heparin (LDUH), or adjusted-dose vitamin K antagonist (VKA) for a minimum of 10-14 days following elective joint arthroplasty surgery. The guidelines also recommend dual therapy of mechanical and chemoprophylaxis while inpatient.
Shah et al. looked at venous thromboembolism prophylaxis (VTEP) practice patterns before and after the ACCP guidelines in 2012 regarding the use of ASA monotherapy. They found a roughly 40% increase in the prescribing of ASA monotherapy on POD#1 and at discharge. They concluded that ASA was readily and rapidly incorporated into clinical practice and highlights how guidelines affect practice patterns.
Freedman et al. in a 2000 meta-analysis of randomized, controlled trials looked at postoperative VTE prophylaxis in patients following elective total hip arthroplasty. They found warfarin had the lowest risk of proximal deep vein thrombosis and no significant differences among agents with regard to the risk of fatal pulmonary embolism or of mortality with any cause. They concluded that the best prophylactic agent in terms of both efficacy and safety was warfarin.
InCORRECT Answers:
Answers 2, 3, 4, and 5: Following the ACCP and AAOS convergence regarding ASA monotherapy, prescribing patterns in ASA were found to increase.
773. SOX-9 is a key transcription factor involved in the differentiation of which of the following cell lineages?
1. Osteoclasts
2. Osteoblasts
3. Chondrocytes
4. Fibroblasts
5. SOX-9 is not a transcription factor, it is a transmembrane tyrosine kinase receptor
**CORRECT answer: 3**
SOX-9 is considered a “master switch” for the differentiation of cells of chondrocytic lineage.
As described in the review by Hoffman et al, SOX-9 binds to a critical consensus sequence in the collagen 2 (Col2) promoter to activate its transcription. Formation of the cartilage template involves a multi-step process in which prechondrogenic mesenchymal cells form condensations prior to differentiating into matrix-producing chondroblasts.
Retinoids, particularly retinoic acid, are among the numerous signaling molecules that have been implicated in this process. Efforts aimed at understanding the mechanisms by which expression of retinoic acid receptor attenuates chondroblast differentiation led to the discovery of the transcriptional activity of SOX-9.
774. Which of the following is NOT included in the best management of a elderly female newly diagnosed with a fragility fracture?
1. Hip and spine densitometry
2. Laboratory analysis for secondary causes of osteoporosis
3. Administration of calcium 1,500 mg/day
4. Administration of Vitamin D 400 to 800 IU/day
5. Low protein diet
**CORRECT answer: 5**
The management of fragility fractures includes both treatment of the diagnosed fracture and optimization of patient health to help prevent future fractures. Appropriate management includes densitometry, laboratory analysis for secondary causes of osteoporosis, and metabolic optimization to heal the current fracture with appropriate calcium, vitamin D, and a protein enriched diet. The referenced manuscript suggests bone mineral density testing to all women age 65 and older and men age 70 and older as well as appropriate levels of calcium and vitamin D to allow for fracture healing.
775. Which of the following chromosomal translocations is associated with osteosarcoma?
1. SYT-SSX1
2. CHOP-TLS
3. EWS-FLI1
4. FKHR-PAX3
5. no translocation associated
**CORRECT answer: 5**
Osteosarcoma has no associated chromosomal translocation, but often has a mutation in Rb gene (retinoblastoma gene).
Answer 1: Synovial cell sarcoma is characterized by translocation t(X;18) (p11;q11) in more than 90% of cases which causes the fusion gene is called the SYT-SSX1, SYT- SSX2, or SYT-SSX4. Answer 2: The consistent cytogenetic abnormality in myxoid liposarcoma is translocation t(12;16)(q13;p11.2). This involves fusion of the transcription factor gene CHOP, which is essential for adipocytic differentiation, to the translocated in liposarcoma (TLS) gene on chromosome 16. Answer 3: Translocation t(11;22) is one of a series of related translocations occurs in more than 95% of the Ewing sarcoma family of tumors. This translocation joins the Ewing sarcoma gene EWS on chromosome
22 to a gene of the ETS family, friend leukemia insertion (FLI1) on chromosome 11, creating an aberrant activating transcriptional factor. Answer
4: The alveolar subtype of rhabdomyosarcoma accounts for 31% of rhabdo cases and involves a unique translocation occurs between the FKHR gene on chromosome 13 and either the PAX3 gene on chromosome 2 (70%) or the PAX7 gene on chromosome 1 (30%).
776. Which of the following terms best describes failure to exercise the degree of diligence and care that a reasonable and prudent person would exercise under similar conditions?
1. Intent
2. Causation
3. Standard of care
4. Breach of duty
5. Damages
**CORRECT answer: 4**
Malpractice is defined as negligence by a healthcare provider that results in injury to a patient. Medical negligence comprises four elements: duty, breach of duty, causation, and damages.
The duty of the physician is to provide care equal to the same standard of care ordinarily executed by surgeons in the same medical specialty. Breach of duty occurs when action or failure to act deviates from the standard of care.
InCORRECT answers:
1: Intent is something that is intended; an aim or purpose.
2: Causation is present when it is demonstrated that failure to meet the standard of care was the direct cause of the patient’s injuries.
3: Standard of care is the level and type of treatment that would be expected in similar situations by treating physicians.
5: Damages are monies awarded as compensation for injuries sustained as the result of medical negligence.
777. Which of the following laboratory values would be consistent with nutritional rickets?
1. increased calcium level
2. increased phosphate level
3. decreased alkaline phosphatase level
4. increased vitamin D level
5. increased parathyroid hormone level
**CORRECT answer: 5**
With decreased vitamin D intake, intestinal calcium and phosphate absorption are reduced leading to hypocalcemia. Decreased serum calcium stimulates increased PTH (secondary hyperparathyroidism) that leads to bone resorption resulting in low to normal levels of serum calcium. Overall laboratory studies show low to normal calcium, low phosphate (excreted because of effect of PTH), increased PTH, low levels of vitamin D and increased alkaline phosphatase levels.
778. Ligaments are viscoelastic, meaning that their tensile strength is affected by:
1. Torsion and tension only
2. Orientation of applied strain
3. Rate of applied load
4. Compression only
5. Tension only
**CORRECT answer: 3**
Ligaments are viscoelastic material which means their stress-strain curve patterns are time/rate dependent (as a result of the internal friction).
The inital portion of the stress-strain curve, called the toe region, exhibits a high deformation/low force characteristic due to the uncrimping of collagen fibers and the elasticity of elastin. Next is the linear region where slippage within and then between collagen fibrils occurs. In this stage, ligaments gets stiffer (increased tensile strength) at higher strain rates.
Illustration A shows the different regions of the stress-strain curve.
779. Which of the following groups correctly identifies serologic tests that are required by the American Association of Tissue Banks (AATB) for musculoskeletal tissue allografts?
1. Cytomegalovirus, Hepatitis A, Hepatitis B, Hepatitis C, HIV, Syphillis
2. Cytomegalovirus, Hepatitis A, Hepatitis B, Hepatitis C, HIV
3. Hepatitis A, Hepatitis B, Hepatitis C, HIV, Syphillis
4. Hepatitis B, Hepatitis C, HIV, Syphillis
5. Hepatitis B, Hepatitis C, HIV
**CORRECT answer: 4**
The American Association of Tissue Banks performs screening testing on all allografts in addition to screening patients medical history. Specific tests include: HIV, HBV, HCV,
HTLV-I/II, and Syphilis (see [_www.aatb.or_ g for more](http://www.aatb.org/) info on screening process). Neither Cytomegalovirus (CMV) nor Hepatitis A is routinely tested for in the American Association of Tissue Banks for musculoskeletal tissue.
780. Which of the following is most often implicated as an etiology for a hypertrophic nonunion?
1. Malreduction with open plating
2. Smoking
3. Inadequate mechanical stability
4. Open injury with significant soft tissue stripping
5. Infection
**CORRECT answer: 3**
Hypertrophic nonunions are caused by inadequate stability, with callus formation by an appropriate biological response. Lack of biology leads to an atrophic nonunion.
Hypertrophic nonunions should be treated with a fixation construct that lends appropriate stability without creating a poor biological environment.
781. **Ca10(P04)6(OH)2 is the chemical formula of**
1. Calcium hydroxyapatite
2. Osteocalcium phosphate
3. Calcium pyrophosphate
4. Osteocalcin
5. Polymethylmethacrylate
**CORRECT answer: 1**
The chemical structure of hydroxyapatite is Ca10(PO4)6(OH)2. Hydroxyapatite is a naturally occurring mineral form of calcium apatite with the formula Ca5(PO4)3(OH), but is usually written Ca10(PO4)6(OH)2 to denote that the crystal unit cell comprises two entities. Up to 50% of bone by weight is made up of a modified form of hydroxyapatite. It is one of few materials that will support bone ingrowth and osseointegration when used in orthopaedic, dental and maxillofacial applications.
782. Which of the following best describes the benefits of implementing diversity and cultural competency in orthopaedic training programs?
1. Incorporating foreign languages in the residency curriculum to improve communication with members of diverse backgrounds.
2. Teaching the social stereotypes of diverse cultures to improve the delivery of healthcare.
3. Establishing racial and gender enrolment quotas in residency programs to better serve all members of the community.
4. Enhancing trainees knowledge of diverse cultures to improve patient- physician relationships, optimize patient access to orthopaedic care, and enhance the quality and delivery of care.
5. Promoting orthopaedic trainees to travel to other countries to obtain surgical experience in different cultures.
**CORRECT answer: 4**
The goals of diversity and cultural competency in orthopaedic training is to enhance the knowledge of patient-physician relationships in diverse cultural groups so to improve access and quality of orthopaedic care.
There is increasing cultural diversity within our populations. The ability to better serve a heterogenous population relies on the ability to enhance the knowledge of patient- physican relationships so that people of all backgrounds can better access and benefit from the healthcare system.
White et al. examined the need for diversity in orthopaedics. For example, African- Americans have higher infant mortality rates, shorter life expectancies, fewer joint replacements, and more amputations than caucasians. It was concluded that cultural competency in orthopaedics is good for patients and for the country.
Illustration A shows a 2008 NSF census of the USA population. InCORRECT Answers:
Answer 1: Incorporating languages into an orthopaedic curriculum would only benefit a small sub-population of patients and isolate many others.
Answer 2: Teaching social stereotypes of diverse cultures can be viewed as discriminatory towards those groups.
Answer 3: While healthcare facilities with diverse staff are more likely to influence and successfully treat a nations diverse population, quotas of racial and gender backgrounds in orthopaedic residency will not entirely address the complete cultural competency that is required of every orthopaedic surgeon.
Answer 5: Traveling to isolated countries will not give residents a complete understanding of cultural diversity.
783. A clinical study for lateral epicondylitis allocates 1 group to receive physical therapy for 4 weeks and another group a new oral medication for 4 weeks. Then the 2 groups immediately switch therapies with one another for the next 4 weeks. The half-life of the medication used in the study is 2 weeks. Which of the following best describes the bias that is present in this study design?
1. Recall bias
2. Verification bias
3. Washout period bias
4. Detection bias
5. Incorporation bias
**CORRECT answer: 3**
In a crossover study design, the washout period is the time between therapies, receiving no therapy, so that the effect of the first therapy is allowed to wear off. In this scenario, the medication's long half-life may continue to have effects after the first group (receiving the medication) has switched to the physical therapy treatment.
Verification bias occurs when results of a diagnostic test influence whether patients are assigned to a
treatment group. Incorporation bias occurs when someone studies a diagnostic test that includes features of the target outcome. Recall bias occurs when
patients who experience an adverse outcome have a different likelihood of recalling an exposure than others that don't have an adverse outcome. Detection bias occurs when one looks more carefully for an outcome in one specific group more than the other group(s). The review article by Kocher et al describes the basics of biostatistics for clinicians.
784. A 62-year-old man undergoes an uncomplicated total shoulder replacement 9 months ago. What is an appropriate choice of prophylactic antibiotics to be taken prior to dental work if he has no allergies?
1. Daptomycin 600 milligrams intravenous 2 hours prior to procedure
2. Cephalexin 2 grams oral 1 hour prior to procedure
3. Levaquin 500 milligrams oral 1 hour prior to procedure
4. Trimethoprim-sulfamethoxazole 2 tablets double-strength oral 1 hour prior to procedure
5. No antibiotics are necessary
**CORRECT answer: 5**
Antibiotics are not necessary for this uncomplicated shoulder arthroplasty situation.
785. Disruption of which of the following interrupts the major source of nutrients to the growth plate?
1. Diaphyseal artery
2. Metaphyseal artery
3. Perichondrial artery
4. Synovial fluid
5. Synovial blood vessels
**CORRECT answer: 3**
Blood supply to the growth plate is supplied both via the perichondrial artery, which is the main source of nutrients, and the epiphyseal artery, which supplies the proliferative zone of the growth plate.
Question 20High Yield
Which nerve is most likely to have evidence of a deficit after shoulder arthroplasty:
Explanation
The most common nerve that has been found to have a deficit after shoulder arthroplasty is the axillary nerve. Correct Answer: Axillary nerve
Question 21High Yield
A 63-year-old man has long-standing type 2 diabetes. He has had associated ongoing neuropathy for approximately 5 years. He now reports a red, hot, swollen right foot for the past 2 days. You place him supine in your office with the foot elevated for 30 minutes. You return to see that the redness has dissipated. What is the most likely diagnosis?
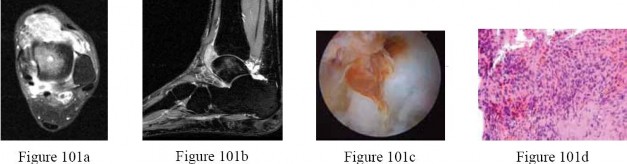
Explanation
Charcot arthropathy is a progressive condition of the musculoskeletal system that is characterized by joint dislocations, pathologic fractures, and debilitating deformities. This disorder results in progressive destruction of bone and soft tissues at weight-bearing joints; in its most severe form, it may cause significant disruption of the bony architecture. In patients with diabetes, the incidence of acute Charcot arthropathy of the foot and ankle ranges from 0.15% to 2.5%. Acute Charcot arthropathy almost always appears with signs of inflammation. Profound unilateral swelling, an increase in local skin temperature (generally, an increase of 3° to 7° above the nonaffected foot’s skin temperature), erythema,joint effusion, and bone resorption in an insensate foot are present. These characteristics, in the presence of intact skin and a loss of protective
sensation, are often pathognomonic of acute Charcot arthropathy.Cellulitis is an infection of the skin and osteomyelitis is an infection of the bone; examination of the limb would remain unchanged after 30 minutes of elevation. Reynaud and Sjogren syndromes are rheumatologic conditions that do not have these symptoms.
CLINICAL SITUATION FOR QUESTIONS 101 THROUGH 103
A 27-year-old woman has had pain in her right ankle for 2 years. Examination reveals a slightly warmjoint, without erythema. Ankle range of motion is limited by pain.
Radiographs are unremarkable.Because management consisting of immobilization, nonsteroidal anti-inflammatory drugs, and physiotherapy has failed to provide relief, MRI scans are obtained and shown in Figures 101a and 101b.An intraoperative image and the histology are shown in Figures 101c and 101d.
---
sensation, are often pathognomonic of acute Charcot arthropathy.Cellulitis is an infection of the skin and osteomyelitis is an infection of the bone; examination of the limb would remain unchanged after 30 minutes of elevation. Reynaud and Sjogren syndromes are rheumatologic conditions that do not have these symptoms.
CLINICAL SITUATION FOR QUESTIONS 101 THROUGH 103
A 27-year-old woman has had pain in her right ankle for 2 years. Examination reveals a slightly warmjoint, without erythema. Ankle range of motion is limited by pain.
Radiographs are unremarkable.Because management consisting of immobilization, nonsteroidal anti-inflammatory drugs, and physiotherapy has failed to provide relief, MRI scans are obtained and shown in Figures 101a and 101b.An intraoperative image and the histology are shown in Figures 101c and 101d.
---
Question 22High Yield
What is the main function of collagen found within articular cartilage?
Explanation
The main function of collagen in articular cartilage is to provide the tissue’s tensile strength. It also immobilizes proteoglycans within the extracellular matrix. Compressive properties are maintained by proteoglycans. Cartilage metabolism is maintained by the indwelling chondrocytes. The flow of water through the tissue promotes transport of nutrients and provides a source of lubricant for the joint.
REFERENCES: Simon SR (ed): Orthopaedic Basic Science. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1994, pp 3-44.
Mow VC, Ratcliffe A: Structure and function of articular cartilage and meniscus, in Mow VC, Hayes WC (eds): Basic Orthopaedic Biomechanics, ed 2. Philadelphia, PA, Lippincott-Raven, 1997, pp 113-177.
REFERENCES: Simon SR (ed): Orthopaedic Basic Science. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1994, pp 3-44.
Mow VC, Ratcliffe A: Structure and function of articular cartilage and meniscus, in Mow VC, Hayes WC (eds): Basic Orthopaedic Biomechanics, ed 2. Philadelphia, PA, Lippincott-Raven, 1997, pp 113-177.
Question 23High Yield
Which of the following clinical findings is most often seen with the MRI scan findings shown in Figures 19a through 19c?
Explanation
DISCUSSION: The MRI scans show a large superior labral cyst. Impingement of the cyst on the suprascapular nerve is implied by the visible atrophy of the infraspinatus muscle as seen in Figure 19c. Clinically, this is manifested by atrophy of the posterior aspect of the shoulder inferior to the scapular spine. The suprascapular nerve provides only motor function and does not provide any sensory function to the shoulder girdle; therefore, sensory deficits will not be present in this patient.
REFERENCES: Westerheide KJ, Dopirak RM, Karzel RP, et al: Suprascapular nerve palsy secondary to spinoglenoid cysts: Results of arthroscopic treatment. Arthroscopy 2006;22:721-727.
Schroder CP, Skare O, Stiris M, et al: Treatment of labral tears with associated spinoglenoid cysts without
cyst decompression. J Bone Joint Surg Am 2008;90:523-530.
Piatt BE, Hawkins RJ, Fritz RC, et al: Clinical evaluation and treatment of spinoglenoid notch ganglion cysts. J Shoulder Elbow Surg 2002; 11:600-604.
REFERENCES: Westerheide KJ, Dopirak RM, Karzel RP, et al: Suprascapular nerve palsy secondary to spinoglenoid cysts: Results of arthroscopic treatment. Arthroscopy 2006;22:721-727.
Schroder CP, Skare O, Stiris M, et al: Treatment of labral tears with associated spinoglenoid cysts without
cyst decompression. J Bone Joint Surg Am 2008;90:523-530.
Piatt BE, Hawkins RJ, Fritz RC, et al: Clinical evaluation and treatment of spinoglenoid notch ganglion cysts. J Shoulder Elbow Surg 2002; 11:600-604.
Question 24High Yield
What is the most common turf toe mechanism of injury?
Explanation
Turf toe, or capsuloligamentous injury to the first MTP joint, most commonly is caused by an axial load being applied to a fixed, dorsiflexed great toe with the heel off the ground. The external force causes further dorsiflexion of the great toe, leading to injury to the capsuloligamentous complex. A less common mechanism of turf toe is hyperplantarflexion of the great toe with valgus stress, which is seen in beach volleyball players.
RECOMMENDED READINGS
[Kadakia AR, Molloy A. Current concepts review: traumatic disorders of the first metatarsophalangeal joint and sesamoid complex. Foot Ankle Int. 2011 Aug;32(8):834-9. Review. PubMed PMID: 22049873. ](http://www.ncbi.nlm.nih.gov/pubmed/22049873)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/22049873)
Clanton TO, McGarvey W. Athletic Injuries to the soft tissues of the foot and ankle. In: Coughlin MJ, Mann RA, Saltzman CL, eds. Surgery of the Foot and Ankle. 8th ed. Philadelphia, PA: Mosby-Elsevier; 2007:1526-1535
RECOMMENDED READINGS
[Kadakia AR, Molloy A. Current concepts review: traumatic disorders of the first metatarsophalangeal joint and sesamoid complex. Foot Ankle Int. 2011 Aug;32(8):834-9. Review. PubMed PMID: 22049873. ](http://www.ncbi.nlm.nih.gov/pubmed/22049873)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/22049873)
Clanton TO, McGarvey W. Athletic Injuries to the soft tissues of the foot and ankle. In: Coughlin MJ, Mann RA, Saltzman CL, eds. Surgery of the Foot and Ankle. 8th ed. Philadelphia, PA: Mosby-Elsevier; 2007:1526-1535
Question 25High Yield
Placing the starting point for an antegrade femoral nail too anterior to the axis of the medullary canal can most commonly lead to what intraoperative complication?
Explanation
Usage of an anterior starting point that is too anterior leads to creation of significant hoop stresses in the proximal segment, potentially leading to iatrogenic fracture of the proximal segment. The referenced study by Johnson et al reviews the topic of femoral bursting and he notes that even shifting 6mm too far anteriorly can lead to proximal femoral fracture creation. He also reported that overreaming the canal by at least 0.5mm diameter is necessary to decrease hoop stresses throughout the femur, likely due to a mismatch in the radius of curvature of the femur and intramedullary nail.
Question 26High Yield
Human calcium absorption occurs in the
Explanation
Dietary calcium is absorbed in the small intestine. This absorption is stimulated by 1,25 dihydroxyvitamin D3. Correct Answer: Small intestine
Question 27High Yield
In patients with Crowe types III and IV developmental dysplasia of the hip with high hip centers, acetabular
reconstruction often requires lowering the acetabular component into the native acetabulum. In doing so, considerable risk for limb lengthening beyond 4 cm exists, making the hip difficult to reduce and raising the risk for nerve injury. Which technique is used to overcome this problem?
reconstruction often requires lowering the acetabular component into the native acetabulum. In doing so, considerable risk for limb lengthening beyond 4 cm exists, making the hip difficult to reduce and raising the risk for nerve injury. Which technique is used to overcome this problem?
Explanation
When substantial lengthening of a dysplastic hip will occur because a high dislocation is relocated into a considerably lower acetabulum, a femoral shortening may be necessary to reduce the hip and avoid a stretch injury to the sciatic nerve. No other choice specifically addresses the need for femoral shortening, and high offset stems and lateralized liners may exacerbate the problem if used alone and without femoral shortening.
Question 28High Yield
For patients who sustain their first anterior glenohumeral dislocation during sports activity, which associated injury is most commonly expected at the time of the initial dislocation?
Explanation
- Axillary nerve palsy_
Question 29High Yield
Recommendations for sports activity should include
Explanation
- avoidance of contact or collision sports.
Question 30High Yield
-A 24-year-old man is involved in a motor vehicle accident at 60 mph. He sustains multiple injuries including an intra-abdominal injury requiring a splenectomy and a closed right femoral shaft fracture.Which variable will best indicate the patient’s resuscitation status when deciding whether to proceed with definitive care of the fracture at the conclusion of the laparotomy?
Explanation
No detailed explanation provided for this question.
Question 31High Yield
What is the most common non-anesthetic-related reversible cause of sustained changes in intraoperative neurophysiologic monitoring signals during spinal surgery?
Explanation
Patient positioning that results in local nerve compression, plexus traction, or improper neck alignment is the most common non-anesthetic-related cause of changes in intraoperative neurophysiologic monitoring data during spinal surgery. Pedicle screw malpositioning, spinal cord ischemia, and retractor placement are all less common causes. Hypotension, not hypertension, can be a cause of intraoperative neurophysiologic changes.
---
---
Question 32High Yield
A 19-year-old football player who sustained three traumatic anterior shoulder dislocations underwent surgery to repair a Bankart lesion. Nine months after surgery, examination reveals stability, elevation to 150 degrees, external rotation to 0 degrees with the elbow at his side and to 50 degrees at 90 degrees of abduction, and internal rotation to T12. If his range of motion does not improve, he is at most risk for
Explanation
Loss of external rotation can lead to degenerative joint disease following an anterior stabilization procedure. A tight anterior capsule will prevent internal impingement. Risk of thoracic outlet syndrome should not be increased. Subscapularis detachment is a risk following open anterior repair; however, a gain in external rotation would be noted. In time, this patient’s shoulder may show increased posterior glenohumeral wear but should not have symptoms of recurrent subluxation unless multidirectional instability is present.
REFERENCES: Hawkins RJ, Angelo RL: Glenohumeral osteoarthrosis: A late complication of the Putti-Platt repair. J Bone Joint Surg Am 1990;72:1193-1197.
Norns TR: Complications following anterior instability repairs, in Bigliani LU (ed): Complication of Shoulder Surgery. Baltimore, MD, Williams and Wilkins, 1993, pp 98-116.
REFERENCES: Hawkins RJ, Angelo RL: Glenohumeral osteoarthrosis: A late complication of the Putti-Platt repair. J Bone Joint Surg Am 1990;72:1193-1197.
Norns TR: Complications following anterior instability repairs, in Bigliani LU (ed): Complication of Shoulder Surgery. Baltimore, MD, Williams and Wilkins, 1993, pp 98-116.
Question 33High Yield
Which of the following conditions is not associated with an increased incidence of congenital vertical talus:
Explanation
Patients with cerebral palsy do not have an increased risk of congenital vertical talus, but they may develop an acquired neuromuscular vertical talus.
Patients with myelomeningocele have approximately a 5% to 10% risk of vertical talus, far above that of the general population.
Arthrogryposis is associated with an increased risk of vertical talus.
Nail patella syndrome and Larsen syndrome are associated with an increased risk of vertical talus.
Patients with myelomeningocele have approximately a 5% to 10% risk of vertical talus, far above that of the general population.
Arthrogryposis is associated with an increased risk of vertical talus.
Nail patella syndrome and Larsen syndrome are associated with an increased risk of vertical talus.
Question 34High Yield
Which relationship is noted for the structure identified by the arrow in Figure 22b? 24
Explanation
- The anterolateral bundle is tensioned in mid flexion, and the posteromedial bundle is tensioned in both extension and high flexion.
Question 35High Yield
Figure 81 is a lateral thoracic spine radiograph of a 76-year-old man with a history of ankylosing spondylitis who falls and strikes his back. He has moderate thoracic discomfort. An initial examination does not reveal neurologic deficits. He is discharged home that day, but returns 3 days later with profound weakness in his legs. Which imaging study should have been obtained at his initial presentation?
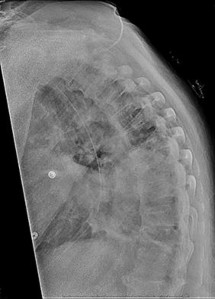
Explanation
Patients with ankylosing spondylitis are at high risk for occult vertebral fractures that are not readily detectable on radiographs. The treating surgeon must have a high suspicion for fractures in these patients and pursue further imaging of the spine with CT and (often) MRI. Even among patients who are neurologically intact, fracture displacement and neurologic deterioration can occur if fractures are not recognized early and appropriately stabilized. Fractures in patients with ankylosing spondylitis are extremely unstable and are associated with high risk for delayed neurological deterioration. Although plain film imaging of the entire spine should be considered, occult fractures can easily be missed. Imaging of the sacroiliac joints can be helpful to establish the diagnosis of ankylosing spondylitis but would not identify an occult fracture of the vertebra in this patient.
RECOMMENDED READINGS
[Finkelstein JA, Chapman JR, Mirza S. Occult vertebral fractures in ankylosing spondylitis. Spinal Cord. 1999 Jun;37(6):444-7. PubMed PMID: 10432265. ](http://www.ncbi.nlm.nih.gov/pubmed/10432265)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/10432265) [Harrop JS, Sharan A, Anderson G, Hillibrand AS, Albert TJ, Flanders A, Vaccaro AR. Failure of standard imaging to detect a cervical fracture in a patient with ankylosing spondylitis. Spine (Phila Pa 1976). 2005 Jul 15;30(14):E417-9. PubMed PMID: 16025019. ](http://www.ncbi.nlm.nih.gov/pubmed/16025019)[View Abstract at](http://www.ncbi.nlm.nih.gov/pubmed/16025019)[ ](http://www.ncbi.nlm.nih.gov/pubmed/16025019)[PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16025019)
Westerveld LA, Verlaan JJ, Oner FC. Spinal fractures in patients with ankylosing spinal disorders: a systematic review of the literature on treatment, neurological status and
[complications. Eur Spine J. 2009 Feb;18(2):145-56. doi: 10.1007/s00586-008-0764-0. Epub 2008 Sep 13. Review. PubMed PMID: 18791749. ](http://www.ncbi.nlm.nih.gov/pubmed/18791749)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/18791749)
RECOMMENDED READINGS
[Finkelstein JA, Chapman JR, Mirza S. Occult vertebral fractures in ankylosing spondylitis. Spinal Cord. 1999 Jun;37(6):444-7. PubMed PMID: 10432265. ](http://www.ncbi.nlm.nih.gov/pubmed/10432265)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/10432265) [Harrop JS, Sharan A, Anderson G, Hillibrand AS, Albert TJ, Flanders A, Vaccaro AR. Failure of standard imaging to detect a cervical fracture in a patient with ankylosing spondylitis. Spine (Phila Pa 1976). 2005 Jul 15;30(14):E417-9. PubMed PMID: 16025019. ](http://www.ncbi.nlm.nih.gov/pubmed/16025019)[View Abstract at](http://www.ncbi.nlm.nih.gov/pubmed/16025019)[ ](http://www.ncbi.nlm.nih.gov/pubmed/16025019)[PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16025019)
Westerveld LA, Verlaan JJ, Oner FC. Spinal fractures in patients with ankylosing spinal disorders: a systematic review of the literature on treatment, neurological status and
[complications. Eur Spine J. 2009 Feb;18(2):145-56. doi: 10.1007/s00586-008-0764-0. Epub 2008 Sep 13. Review. PubMed PMID: 18791749. ](http://www.ncbi.nlm.nih.gov/pubmed/18791749)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/18791749)
Question 36High Yield
Which of the following terms is used to describe complete severance of a peripheral nerve with loss of the nerve trunk continuity:
Explanation
A fifth-degree injury refers to complete disruption of the nerve trunk.
First-degree: Neuropraxia, the nerve structure is intact, full recovery is expected
Second-degree: Axonotmesis, severance of the axon leading to Wallerian degeneration, continuity of endoneurial sheath is maintained, repair is orderly, complete motor and sensory loss with denervation and fibrillation potentials
Third-degree: Injury to axons and the endoneurial tube, arrangement of individual fascicles is maintained (perineurium intact), recovery is variable
Fourth-degree: Injury to axons, endoneurial tube, fascicles with the nerve trunk being intact, Wallerian degeneration and a higher incidence of proximal nerve cell body degeneration, repair is unlikely and surgical repair of the nerve is necessary (excision and grafting)
Fifth-degree: Loss of nerve trunk continuity, neuroma formation in the proximal stump, Wallerian degeneration distally
First-degree: Neuropraxia, the nerve structure is intact, full recovery is expected
Second-degree: Axonotmesis, severance of the axon leading to Wallerian degeneration, continuity of endoneurial sheath is maintained, repair is orderly, complete motor and sensory loss with denervation and fibrillation potentials
Third-degree: Injury to axons and the endoneurial tube, arrangement of individual fascicles is maintained (perineurium intact), recovery is variable
Fourth-degree: Injury to axons, endoneurial tube, fascicles with the nerve trunk being intact, Wallerian degeneration and a higher incidence of proximal nerve cell body degeneration, repair is unlikely and surgical repair of the nerve is necessary (excision and grafting)
Fifth-degree: Loss of nerve trunk continuity, neuroma formation in the proximal stump, Wallerian degeneration distally
Question 37High Yield
A 36-year-old male is brought to the trauma center following a motor vehicle accident. Physical exam shows a deformed left lower extremity with a 1-cm open wound over the anterolateral aspect of his leg. Radiographs are provided in Figures A and


Explanation
The clinical scenario and radiographs are consistent with a Gustilo and Anderson type 3A open tibia fracture.
Melvin et al review the evidenced-based literature and make recommendations for the initial evaluation and management of open tibial shaft fractures. The time elapsed before antibiotic administration and adequate surgical debridement of all contamination are the only factors definitively shown to reduce infection and improve outcome. Traditional recommendations have suggested surgical debridement of open fractures occur within 6 hours of injury. However, there is no literature to support this time window. Certainly, open fractures should be addressed with urgency, but there is no evidence reporting a definitive time window. There is insufficient data to recommend gram negative coverage with gentamicin for all open fractures although this is a common practice. The addition of antibiotics to the irrigation solution has been shown to decrease bacterial load, but it has also demonstrated host tissue necrosis and delayed wound healing. There is not sufficient data to support its use over a castile soap solution or normal saline. Similarly, high pressure pulsatile lavage decreases bacterial load, but also seeds bacteria deeper within the soft tissues and harms host tissues. There is no evidence to support pulsatile lavage over gravity flow.
Melvin et al review the evidenced-based literature and make recommendations for the initial evaluation and management of open tibial shaft fractures. The time elapsed before antibiotic administration and adequate surgical debridement of all contamination are the only factors definitively shown to reduce infection and improve outcome. Traditional recommendations have suggested surgical debridement of open fractures occur within 6 hours of injury. However, there is no literature to support this time window. Certainly, open fractures should be addressed with urgency, but there is no evidence reporting a definitive time window. There is insufficient data to recommend gram negative coverage with gentamicin for all open fractures although this is a common practice. The addition of antibiotics to the irrigation solution has been shown to decrease bacterial load, but it has also demonstrated host tissue necrosis and delayed wound healing. There is not sufficient data to support its use over a castile soap solution or normal saline. Similarly, high pressure pulsatile lavage decreases bacterial load, but also seeds bacteria deeper within the soft tissues and harms host tissues. There is no evidence to support pulsatile lavage over gravity flow.
Question 38High Yield
A unilateral "piano key" sign, indicates
Explanation
The piano key sign is a demonstration of instability at the DRUJ, typically seen after healing from a distal radius fracture with an associated ulnar styloid fracture (as in this case) or other wrist injury. The hand is pushed down against a table top, and the distal radius translates dorsally (with the distal ulna apparently moving volarly). In fact, the distal radius is the mobile segment, while the distal ulna is fixed in space. Treatment involves repair or reconstruction of the foveal insertion of the triangular fibrocartilage complex (TFCC) and distal radioulnar ligaments. This type of instability is also common in malunions of the distal radius or distal one-third of the radial shaft (Galeazzi-type fractures). In malunions, DRUJ instability can be treated with a corrective osteotomy of the distal radius to restore the anatomic relationship between the distal ulna and the distal radius at the DRUJ. Radiocarpal and midcarpal instability do not involve the DRUJ. Disruption of the interosseous membrane (in isolation, with intact distal radioulnar ligaments and an intact TFCC) does not lead to translational instability of the DRUJ. Although hypermobility syndrome may lead to ligamentous laxity, it does not lead to unilateral DRUJ instability.
Question 39High Yield
Intraarticular fracture fragments should be removed from the joint, but if they make up a substantial portion of the joint surface, they should be incorporated in the fixation construct to obtain the goal of anatomic reduction of the joint surface
What is the most appropriate next step in management?
What is the most appropriate next step in management?
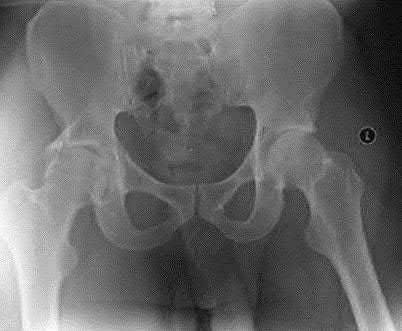
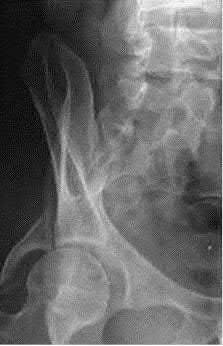
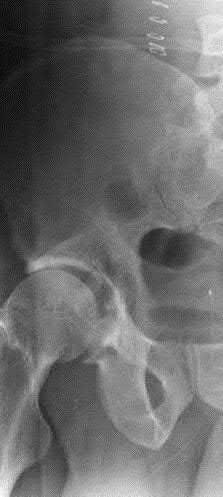
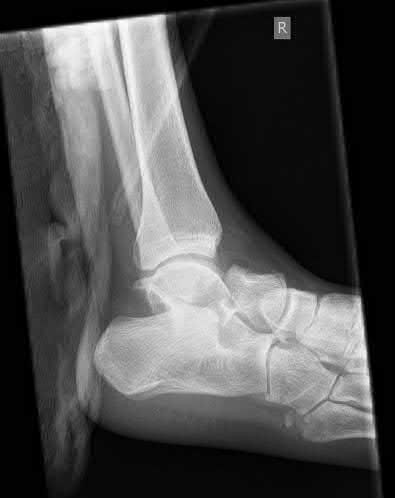
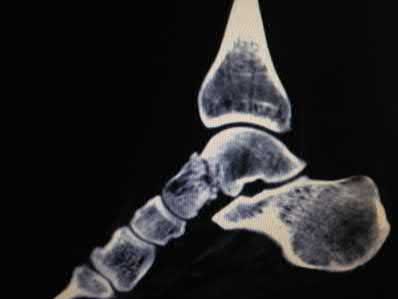
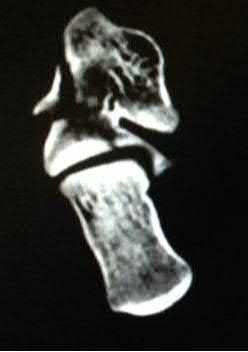
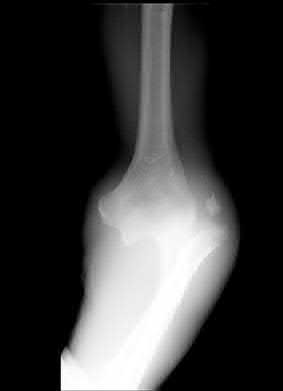
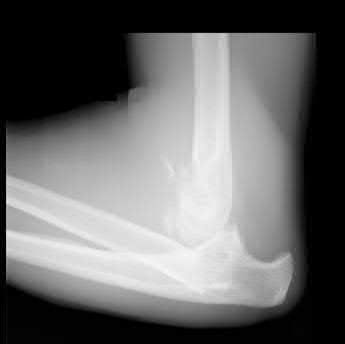
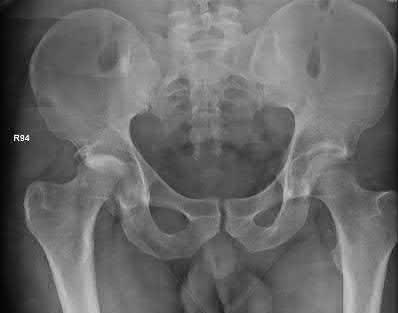
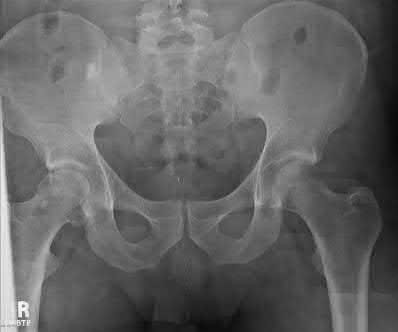
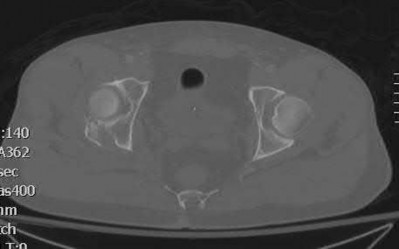
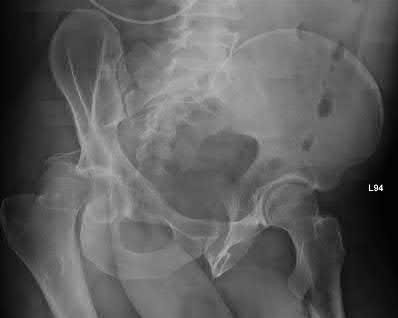
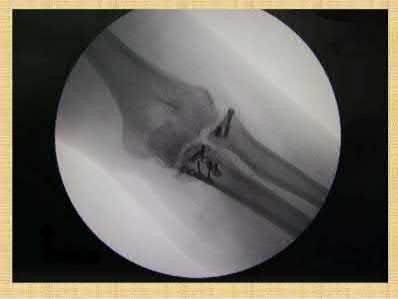
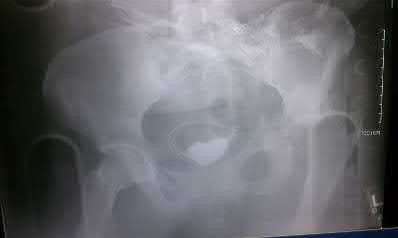
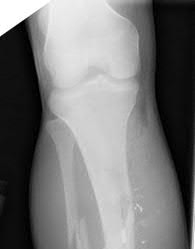
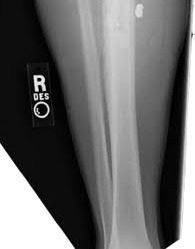
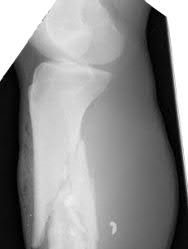
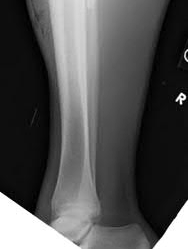




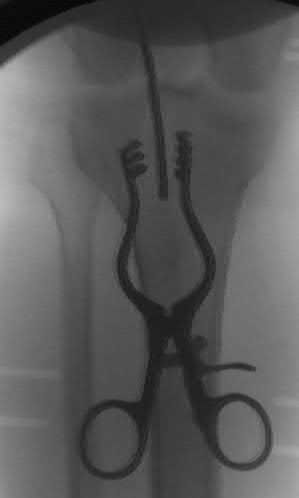
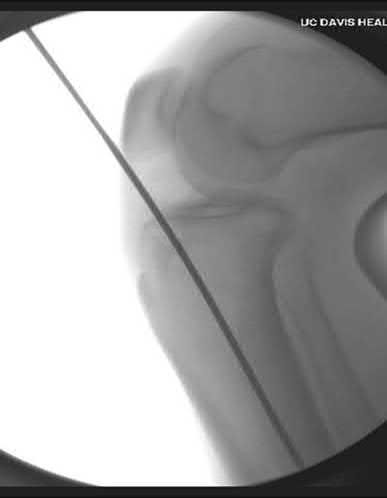
Explanation
This patient has a large posterior wall fracture of the right acetabulum with an unstable hip. The most appropriate next step in treatment is open reduction and internal fixation.
Fixation of acetabular fractures during pregnancy is not contraindicated in the setting of stable fetal heart rate and no abnormalities on pelvic ultrasound.
There is, however, an increased risk of complications for the mother and fetus. Injury severity and mechanism are most closely associated with increased rate of fetal complications. The trimester of pregnancy is not associated with increased risk of complications.
Leggon et al. reviewed 101 cases of pelvic and acetabular fractures in pregnant patients and found mechanism of injury and injury severity were associated with higher mortality for both mother and fetus. Trimester of pregnancy was not associated with increased mortality.
Flik et al. reviewed orthopaedic trauma in a pregnant patients and recommended fetal ultrasound for assessment of fetal well-being in all pregnant patients.
Desai et al. investigated orthopaedic trauma during pregnancy and reported minimal radiation risk to the fetus when obtaining x-rays. They also advocate for LMWH as one of the safest choices for anticoagulation.
Figure A is an x-ray showing a right posterior wall acetabular fracture. Figures B and C are Judet views of the pelvis focusing on the right hip. A large posterior wall fragment is visible in Figure B.
Incorrect Answers:
,3,5: ORIF is the most appropriate treatment for this posterior wall fracture. There is no contraindication to ORIF.
Answer 4: There is no indication to delay treatment as the fetal heart rate is normal and ultrasound shows no abnormalities.
Figure A is radiograph of a 50-year-old male science teacher that was involved in a motor vehicle accident. He underwent closed reduction as seen in Figure B and C. What would be the most appropriate treatment?
1) Open reduction and internal fixation with medial bridge plate and lateral screw in non-lagging mode
2) Tibiotalocalcaneal arthrodesis
3) Open reduction and internal fixation with lateral and medial screw in lagging mode
4) Closed reduction and internal fixation with medial and lateral screw in non-lagging mode
5) Closed reduction with percutaneous pins
This patient is presenting with a Hawkins II talar neck fracture with medial wall comminution. The most appropriate treatment of this patient would be open reduction internal fixation with medial plate and lateral screw in non-lagging mode.
The treatment of talar fractures is based on the severity of the fracture, soft-tissues, and patient factors. The fracture and subluxation of the subtalar joint should be reduced and stable anatomical fixation should be obtained. When there is comminution of either the superior, lateral or medial aspects of the talus, one should avoid shortening the medial wall as this will cause a varus malunion. The use of a medial or lateral plate can help to re-establish column length, which can often prevent this potential complication.
Sanders et al. showed significant complications after fixation of talar neck fractures. They showed the incidence of secondary reconstructive procedures following talar neck fractures increased from 24% +/- 5% at 1 year to 48%
+/- 10% at 10 years post-injury.
Vallier et al. retrospectively reviewed the records of 39 fractures of the talar neck treated with open reduction and internal fixation. Twenty-one (54%) of thirty-nine patients had development of posttraumatic arthritis, which was more common after comminuted fractures (p
A 28-year-old male college student sustains a severe foot injury from gunshot-related violence, and subsequently undergoes a lower-extremity amputation as shown in Figure A. At long-term follow-up, which of the following is the strongest predictor of patient satisfaction as related to his injury?
1) Age less than 30
2) Marijuana use
3) Use of negative pressure wound therapy
4) Male gender
5) Ability to return to work
The strongest factor to predict patient-reported outcomes after trauma-related lower extremity amputations is the patient's ability to return to work. This is likely due to the effect of the return to work on the physical, emotional, and financial aspects of the patient's life.
The LEAP study is a multicenter, prospective study evaluating multiple aspects of reconstruction versus amputation in the treatment of mangled extremity injuries. With regard to patient satisfaction, treatment variables such as decision for reconstruction versus amputation, or initial presence or absence of plantar sensation have little impact. In addition, demographic factors such as age, gender, socioeconomic status, and education level do not predict patient satisfaction. Instead, the most important predictors of patient satisfaction at 2 years after injury include the ability to return to work, absence of depression, faster walking speed, and decreased pain.
O'Toole et al reviewed 463 patients treated for limb-threatening lower-extremity injuries and identified factors associated with patient reported outcomes two years after surgery. They found that return to work was the most associated with outcomes, but that physical functioning, walking speed, pain levels, and presence of depression were also associated to a lesser extent with outcomes.
Bosse et al performed a multicenter, prospective study to assess outcomes of 569 patients with severe lower extremity limb injuries that resulted in either amputation or limb salvage procedures. They found that at two years postoperatively, no significant differences were seen between groups in patient-reported outcome. Worse outcomes were associated with rehospitalization for a major complication, a low educational level, nonwhite race, poverty, lack of private health insurance, poor social-support network, low self-efficacy (the patient's confidence in being able to resume life activities), and involvement in disability-compensation litigation.
Figure A shows a clinical photograph of a Pirigoff amputation at early follow-up. This amputation is an end-bearing amputation that utilizes the plantar heel pad for weightbearing, and relies on a tibiocalcaneal arthrodesis.
Incorrect Answers:
1-4: These options are not as strong of a factor of patient satisfaction in longterm follow up after trauma-induced lower extremity amputation.
A 34 year-old male falls off of motorcycle on an outstretched hand suffering the injuries shown in Figures A and B. He is brought to the operating room and undergoes radial head replacement and fixation and repair of the coronoid and the lateral collateral ligament (LCL). Prior to closing, the elbow is still unstable upon testing range of motion. What is the next best step in management?
1) Exchange radial head for larger implant
2) Complete resection of radial head
3) Cast at 90 degrees of flexion for 6-8 weeks
4) Reinforce LCL repair with non-absorbable suture
5) Repair the ulnar collateral ligament
Following complete fixation and repair of a terrible triad, a final range of motion test should be performed prior to closure. If still unstable, the next step should be to assess and repair the ulnar collateral ligament. Another option
would be to placed a hinged external fixator.
Operative reconstruction of a terrible triad injury should be performed in a systematic fashion, working from deep to superficial. Working through a lateral incision and through the radial head fracture, the coronoid should be fixed first, followed by radial head fixation or replacement and then repair/reconstruction of the LCL. If still unstable, the medial side should be addressed, or the patient placed in a hinged external fixator.
Mathew et al review the anatomic, biomechanic, and operative principles (why the above step-by-step method works) to achieving appropriate stability in order to obtain early range of motion to maximize clinical outcome.
Pugh et al. in this retrospective, multi-center study report outcomes on 36 terrible triad injuries fixed with the standard protocol described above. The authors recommend following this systematic approach to achieve the best results.
Figures A and B are AP and lateral radiographs exhibiting a terrible triad elbow fracture-dislocation.
Incorrect answers:
Answer 1. Overstuffing the radial head should be avoided.
Answer 2. Resection of the radial head is contraindicated in an unstable elbow. Answer 3. While casting the extremity may provide initial immobilization, you are unable to monitor the wound and truly assess stability, especially when swelling subsides.
Answer 4. Reinforcing the LCL will not make increase any stability not already achieved.
When treating the pathology depicted in Figures A through D, which of the following is necessary to preserve the blood supply to the femoral head?
1) Dissection of the gluteal musculature off the iliac crest
2) Ligation of the ascending branches of the lateral femoral circumflex artery
3) Greater trochanteric osteotomy
4) Identification and detachment of the piriformis tendon
5) Supine positioning
Figures A-D show a femoral head with associated acetabular fracture (Pipkin IV). Both the posterior wall fracture and the femoral head fracture can be addressed through a surgical dislocation via greater trochanteric osteotomy.
Pipkin IV femoral head fracture (with associated acetabular fractures) are somewhat problematic in that the femoral head fracture is usually anterior, while the acetabular fracture usually involves the posterior wall. A Kocher-Langenbeck approach gives good access to the posterior wall but limited access to the articular surface and femoral head avascular necrosis (AVN) is a concern. A Smith-Peterson approach provides good access to the femoral head
but not to the posterior wall. Combined approaches significantly increase the amount of surgical dissection. Surgical dislocation with trochanteric flip osteotomy provides access to the femoral head and posterior wall while preserving blood supply to the femoral head.
Solberg et al. retrospectively reviewed 12 patients with Pipkin IV injuries treated via a trochanteric flip osteotomy. All patients healed their acetabular fractures. Eleven of 12 patients healed their femoral head fractures and one patient (8.3%) developed osteonecrosis.
Henle et al. likewise treated 12 patients with Pipkin IV injuries through a trochanteric flip osteotomy. Two of 12 patients (16.7%) developed osteonecrosis. The remaining 10 patients (83.3%) had good or excellent results. Heterotopic ossification occurred in five patients, causing significant range of motion loss in four of these.
Figure A is a pre-reduction AP pelvis in which the posterior wall fracture is apparent. Figure B is a post-reduction AP pelvis in which an infra-foveal femoral head fracture is apparent (Pipkin IV). Figure C is an axial CT cut which further characterizes the posterior wall fracture. Figure D is an obturator oblique showing femoral head dislocation and posterior wall fracture. The video shows a surgical hip dislocation technique.
Incorrect Answers:
Answer 1: The extended iliofemoral approach exposes the entire innominate bone, which is not necessary to treat this injury.
Answer 2: The Smith-Peterson anterior approach provides access to the anterior femoral head but not the posterior wall of the acetabulum.
Answer 4: Detachment of the short external rotators is not necessary for surgical dislocation.
Answer 5: Surgical dislocation with greater trochanteric osteotomy is described in the lateral position. Supine positioning is not necessary.
A 42-year-old male presents to your clinic for the first time with the radiographs seen in Figure A. He sustained the injury 4 weeks ago while skiing overseas and treatment was provided by the local orthopaedic surgeon. The operative note states that he sustained an Gustilo Type I open fracture. After surgical fixation of this type of injury, what is the most common complication requiring reoperation?
1) Chronic elbow instability
2) Post-traumatic arthritis
3) Infection
4) Heterotopic ossification
5) Loss of elbow range of motion
This patient sustained a terrible triad elbow fracture-dislocation. Reduced range of motion of the elbow joint is the most common complication REQUIRING reoperation with these injuries.
Terrible triad elbow fracture-dislocations are characterized by posterolateral dislocation/lateral collateral ligament (LCL) injury, radial head fracture and coronoid fracture. Displaced fractures result in elbow instability. Acute radial head stabilization, coronoid open reduction and internal fixation, and LCL +/-medial collateral ligament (MCL) repair/reconstruction is considered the most appropriate treatment for displaced fractures. Operative complications include elbow stiffness, recurrent instability, arthritis, failure of hardware, heterotopic ossification, posterior interosseous nerve palsy and infection.
Egol et al. looked at the functional outcomes of 27 patients that underwent fixation of terrible triad injuries. At one year follow-up, the average flexion-extension arc of elbow motion was 109 degrees +/- 27 degrees, and the average pronation-supination arc was 128 degrees +/- 44 degrees. Grip strength averaged 72% of the contralateral extremity. Although operative fixation led to functional elbow stability, results were poor.
They included a reference to McKee et al. to highlight that intra-articular fractures of the elbow have high rates of stiffness. While not specific to terrible
triads, they looked at the effectiveness of the posterior elbow approach in 25 patients that underwent internal fixation of intra-articular distal humerus fractures. They showed poor outcomes at a mean follow-up of 36 months with reduced range-of-motion, decreased strength and high re-operation rates.
Figure A shows AP fluoroscopic image of a terrible triad injury that has undergone operative fixation. The radial head and coronoid have undergone open reduction internal fixation, and the MCL bony avulsion has been repaired.
Incorrect Answers:
Answer 1: Chronic elbow instability is more common following type I or II coronoid fracture when not operatively managed.
Answer 2: Post-traumatic arthritis results from chondral damage at time of injury and/or residual instability.
Answer 3: Infection is more prevalent with open fractures, however Type I injuries are usually not associated with increase in infection rates.
Answer 4: Heterotopic ossification is a common complication after fixation of these injuries. However, it does not always necessitate reoperation.
Figure A is a radiograph from a 59-year-old male that was transferred to a Level I trauma center five hours after a motor vehicle accident. Closed reduction and skeletal traction was successfully performed in the trauma bay. Which of the following factors has been shown to increase the risk of unsatisfactory clinical outcome for this patient?
1) Need for skeletal traction
2) Mechanism of injury
3) Gender
4) Age
5) Time to reduction
Age greater than 55-years-old has been found to be an independent risk factor for inferior clinical outcome in patients with combined acetabular fractures and hip dislocations.
The most important initial step in management following resuscitation involves urgent reduction of the dislocated hip. This should be followed by a preoperative CT scan and ultimately surgical fixation of the combined acetabular fracture. Hip dislocations should be reduced within 6-12 hours for optimal outcome, although different critical times have been cited, particularly for dislocations with concomitant acetabular fractures. Skeletal traction may be required to maintain hip reduction.
Moed et. al. present a Level 3 retrospective review of 100 patients who had been treated with open reduction internal fixation of an acetabular fracture. The authors found that factors associated with unsatisfactory clinical outcomes included age greater than 55, intra-articular comminution, osteonecrosis, and delay of greater than 12 hours for reduction of an associated hip dislocation.
Additionally, they showed that there was a strong association of clinical outcome and final radiographic grade.
Figure A demonstrates an acetabular fracture with concomitant hip dislocation. Incorrect Answers:
Answer 1-3, and 5: Placement and need for skeletal traction, mechanism of
injury, male gender, and time to reduction
A 37-year-old male cashier is shot in the leg. He sustains the injury shown in Figures A and B, and is subsequently taken to the operating room for intramedullary nailing. Figure C shows a radiograph of the nail starting point (*). What complication is most likely to result?
1) Varus malunion
2) Nonunion
3) Valgus malunion
4) Malrotation
5) Superficial peroneal nerve injury
This patient is presenting with a comminuted fracture of the proximal third of the tibia. He is appropriately undergoing intramedullary nail fixation, however, the start point illustrated in Figure C is too medial and often leads to a valgus malunion.
Intramedullary nail fixation is more technically demanding in proximal tibial fractures than diaphyseal fractures. The valgus deformity is due to imbalanced muscle forces on the proximal fragment, which are then accentuated by a start point that is too medial. An apex anterior (procurvatum) deformity can also occur and results from the pull of the patellar tendon or a posteriorly directed nail that deflects off the posterior tibial cortex and rotates the proximal fragment. The ideal starting point for proximal tibial fractures is slightly lateral to the medial aspect of the lateral tibial spine on a true AP x-ray and very proximal and just anterior to the anterior margin of the articular surface.
Nork et al. reported the results of intramedullary nailing of proximal tibial fractures with emphasis on techniques of reduction. Various techniques were found to be successful including attention to the proper starting point, the use of unicortical plates, and the use of a femoral distractor applied to the tibia.
Lowe et al. describe surgical techniques for complex proximal tibial fractures. They describe the extended leg position, use of a femoral distractor, temporary plate fixation, blocking (Poller) screws, and use of percutaneous clamps as means to achieve reduction during fixation.
Figure A and B show an AP and lateral radiograph of a comminuted extra-articular fracture through the proximal third of the tibia. Figure C demonstrates a start point that is too medial (represented by the asterisk) for intramedullary nail fixation. Illustration A and B show the ideal start point for intramedullary nail fixation of the tibia on AP and lateral radiographs.
Incorrect Answers:
Fixation of acetabular fractures during pregnancy is not contraindicated in the setting of stable fetal heart rate and no abnormalities on pelvic ultrasound.
There is, however, an increased risk of complications for the mother and fetus. Injury severity and mechanism are most closely associated with increased rate of fetal complications. The trimester of pregnancy is not associated with increased risk of complications.
Leggon et al. reviewed 101 cases of pelvic and acetabular fractures in pregnant patients and found mechanism of injury and injury severity were associated with higher mortality for both mother and fetus. Trimester of pregnancy was not associated with increased mortality.
Flik et al. reviewed orthopaedic trauma in a pregnant patients and recommended fetal ultrasound for assessment of fetal well-being in all pregnant patients.
Desai et al. investigated orthopaedic trauma during pregnancy and reported minimal radiation risk to the fetus when obtaining x-rays. They also advocate for LMWH as one of the safest choices for anticoagulation.
Figure A is an x-ray showing a right posterior wall acetabular fracture. Figures B and C are Judet views of the pelvis focusing on the right hip. A large posterior wall fragment is visible in Figure B.
Incorrect Answers:
,3,5: ORIF is the most appropriate treatment for this posterior wall fracture. There is no contraindication to ORIF.
Answer 4: There is no indication to delay treatment as the fetal heart rate is normal and ultrasound shows no abnormalities.
Figure A is radiograph of a 50-year-old male science teacher that was involved in a motor vehicle accident. He underwent closed reduction as seen in Figure B and C. What would be the most appropriate treatment?
1) Open reduction and internal fixation with medial bridge plate and lateral screw in non-lagging mode
2) Tibiotalocalcaneal arthrodesis
3) Open reduction and internal fixation with lateral and medial screw in lagging mode
4) Closed reduction and internal fixation with medial and lateral screw in non-lagging mode
5) Closed reduction with percutaneous pins
This patient is presenting with a Hawkins II talar neck fracture with medial wall comminution. The most appropriate treatment of this patient would be open reduction internal fixation with medial plate and lateral screw in non-lagging mode.
The treatment of talar fractures is based on the severity of the fracture, soft-tissues, and patient factors. The fracture and subluxation of the subtalar joint should be reduced and stable anatomical fixation should be obtained. When there is comminution of either the superior, lateral or medial aspects of the talus, one should avoid shortening the medial wall as this will cause a varus malunion. The use of a medial or lateral plate can help to re-establish column length, which can often prevent this potential complication.
Sanders et al. showed significant complications after fixation of talar neck fractures. They showed the incidence of secondary reconstructive procedures following talar neck fractures increased from 24% +/- 5% at 1 year to 48%
+/- 10% at 10 years post-injury.
Vallier et al. retrospectively reviewed the records of 39 fractures of the talar neck treated with open reduction and internal fixation. Twenty-one (54%) of thirty-nine patients had development of posttraumatic arthritis, which was more common after comminuted fractures (p
A 28-year-old male college student sustains a severe foot injury from gunshot-related violence, and subsequently undergoes a lower-extremity amputation as shown in Figure A. At long-term follow-up, which of the following is the strongest predictor of patient satisfaction as related to his injury?
1) Age less than 30
2) Marijuana use
3) Use of negative pressure wound therapy
4) Male gender
5) Ability to return to work
The strongest factor to predict patient-reported outcomes after trauma-related lower extremity amputations is the patient's ability to return to work. This is likely due to the effect of the return to work on the physical, emotional, and financial aspects of the patient's life.
The LEAP study is a multicenter, prospective study evaluating multiple aspects of reconstruction versus amputation in the treatment of mangled extremity injuries. With regard to patient satisfaction, treatment variables such as decision for reconstruction versus amputation, or initial presence or absence of plantar sensation have little impact. In addition, demographic factors such as age, gender, socioeconomic status, and education level do not predict patient satisfaction. Instead, the most important predictors of patient satisfaction at 2 years after injury include the ability to return to work, absence of depression, faster walking speed, and decreased pain.
O'Toole et al reviewed 463 patients treated for limb-threatening lower-extremity injuries and identified factors associated with patient reported outcomes two years after surgery. They found that return to work was the most associated with outcomes, but that physical functioning, walking speed, pain levels, and presence of depression were also associated to a lesser extent with outcomes.
Bosse et al performed a multicenter, prospective study to assess outcomes of 569 patients with severe lower extremity limb injuries that resulted in either amputation or limb salvage procedures. They found that at two years postoperatively, no significant differences were seen between groups in patient-reported outcome. Worse outcomes were associated with rehospitalization for a major complication, a low educational level, nonwhite race, poverty, lack of private health insurance, poor social-support network, low self-efficacy (the patient's confidence in being able to resume life activities), and involvement in disability-compensation litigation.
Figure A shows a clinical photograph of a Pirigoff amputation at early follow-up. This amputation is an end-bearing amputation that utilizes the plantar heel pad for weightbearing, and relies on a tibiocalcaneal arthrodesis.
Incorrect Answers:
1-4: These options are not as strong of a factor of patient satisfaction in longterm follow up after trauma-induced lower extremity amputation.
A 34 year-old male falls off of motorcycle on an outstretched hand suffering the injuries shown in Figures A and B. He is brought to the operating room and undergoes radial head replacement and fixation and repair of the coronoid and the lateral collateral ligament (LCL). Prior to closing, the elbow is still unstable upon testing range of motion. What is the next best step in management?
1) Exchange radial head for larger implant
2) Complete resection of radial head
3) Cast at 90 degrees of flexion for 6-8 weeks
4) Reinforce LCL repair with non-absorbable suture
5) Repair the ulnar collateral ligament
Following complete fixation and repair of a terrible triad, a final range of motion test should be performed prior to closure. If still unstable, the next step should be to assess and repair the ulnar collateral ligament. Another option
would be to placed a hinged external fixator.
Operative reconstruction of a terrible triad injury should be performed in a systematic fashion, working from deep to superficial. Working through a lateral incision and through the radial head fracture, the coronoid should be fixed first, followed by radial head fixation or replacement and then repair/reconstruction of the LCL. If still unstable, the medial side should be addressed, or the patient placed in a hinged external fixator.
Mathew et al review the anatomic, biomechanic, and operative principles (why the above step-by-step method works) to achieving appropriate stability in order to obtain early range of motion to maximize clinical outcome.
Pugh et al. in this retrospective, multi-center study report outcomes on 36 terrible triad injuries fixed with the standard protocol described above. The authors recommend following this systematic approach to achieve the best results.
Figures A and B are AP and lateral radiographs exhibiting a terrible triad elbow fracture-dislocation.
Incorrect answers:
Answer 1. Overstuffing the radial head should be avoided.
Answer 2. Resection of the radial head is contraindicated in an unstable elbow. Answer 3. While casting the extremity may provide initial immobilization, you are unable to monitor the wound and truly assess stability, especially when swelling subsides.
Answer 4. Reinforcing the LCL will not make increase any stability not already achieved.
When treating the pathology depicted in Figures A through D, which of the following is necessary to preserve the blood supply to the femoral head?
1) Dissection of the gluteal musculature off the iliac crest
2) Ligation of the ascending branches of the lateral femoral circumflex artery
3) Greater trochanteric osteotomy
4) Identification and detachment of the piriformis tendon
5) Supine positioning
Figures A-D show a femoral head with associated acetabular fracture (Pipkin IV). Both the posterior wall fracture and the femoral head fracture can be addressed through a surgical dislocation via greater trochanteric osteotomy.
Pipkin IV femoral head fracture (with associated acetabular fractures) are somewhat problematic in that the femoral head fracture is usually anterior, while the acetabular fracture usually involves the posterior wall. A Kocher-Langenbeck approach gives good access to the posterior wall but limited access to the articular surface and femoral head avascular necrosis (AVN) is a concern. A Smith-Peterson approach provides good access to the femoral head
but not to the posterior wall. Combined approaches significantly increase the amount of surgical dissection. Surgical dislocation with trochanteric flip osteotomy provides access to the femoral head and posterior wall while preserving blood supply to the femoral head.
Solberg et al. retrospectively reviewed 12 patients with Pipkin IV injuries treated via a trochanteric flip osteotomy. All patients healed their acetabular fractures. Eleven of 12 patients healed their femoral head fractures and one patient (8.3%) developed osteonecrosis.
Henle et al. likewise treated 12 patients with Pipkin IV injuries through a trochanteric flip osteotomy. Two of 12 patients (16.7%) developed osteonecrosis. The remaining 10 patients (83.3%) had good or excellent results. Heterotopic ossification occurred in five patients, causing significant range of motion loss in four of these.
Figure A is a pre-reduction AP pelvis in which the posterior wall fracture is apparent. Figure B is a post-reduction AP pelvis in which an infra-foveal femoral head fracture is apparent (Pipkin IV). Figure C is an axial CT cut which further characterizes the posterior wall fracture. Figure D is an obturator oblique showing femoral head dislocation and posterior wall fracture. The video shows a surgical hip dislocation technique.
Incorrect Answers:
Answer 1: The extended iliofemoral approach exposes the entire innominate bone, which is not necessary to treat this injury.
Answer 2: The Smith-Peterson anterior approach provides access to the anterior femoral head but not the posterior wall of the acetabulum.
Answer 4: Detachment of the short external rotators is not necessary for surgical dislocation.
Answer 5: Surgical dislocation with greater trochanteric osteotomy is described in the lateral position. Supine positioning is not necessary.
A 42-year-old male presents to your clinic for the first time with the radiographs seen in Figure A. He sustained the injury 4 weeks ago while skiing overseas and treatment was provided by the local orthopaedic surgeon. The operative note states that he sustained an Gustilo Type I open fracture. After surgical fixation of this type of injury, what is the most common complication requiring reoperation?
1) Chronic elbow instability
2) Post-traumatic arthritis
3) Infection
4) Heterotopic ossification
5) Loss of elbow range of motion
This patient sustained a terrible triad elbow fracture-dislocation. Reduced range of motion of the elbow joint is the most common complication REQUIRING reoperation with these injuries.
Terrible triad elbow fracture-dislocations are characterized by posterolateral dislocation/lateral collateral ligament (LCL) injury, radial head fracture and coronoid fracture. Displaced fractures result in elbow instability. Acute radial head stabilization, coronoid open reduction and internal fixation, and LCL +/-medial collateral ligament (MCL) repair/reconstruction is considered the most appropriate treatment for displaced fractures. Operative complications include elbow stiffness, recurrent instability, arthritis, failure of hardware, heterotopic ossification, posterior interosseous nerve palsy and infection.
Egol et al. looked at the functional outcomes of 27 patients that underwent fixation of terrible triad injuries. At one year follow-up, the average flexion-extension arc of elbow motion was 109 degrees +/- 27 degrees, and the average pronation-supination arc was 128 degrees +/- 44 degrees. Grip strength averaged 72% of the contralateral extremity. Although operative fixation led to functional elbow stability, results were poor.
They included a reference to McKee et al. to highlight that intra-articular fractures of the elbow have high rates of stiffness. While not specific to terrible
triads, they looked at the effectiveness of the posterior elbow approach in 25 patients that underwent internal fixation of intra-articular distal humerus fractures. They showed poor outcomes at a mean follow-up of 36 months with reduced range-of-motion, decreased strength and high re-operation rates.
Figure A shows AP fluoroscopic image of a terrible triad injury that has undergone operative fixation. The radial head and coronoid have undergone open reduction internal fixation, and the MCL bony avulsion has been repaired.
Incorrect Answers:
Answer 1: Chronic elbow instability is more common following type I or II coronoid fracture when not operatively managed.
Answer 2: Post-traumatic arthritis results from chondral damage at time of injury and/or residual instability.
Answer 3: Infection is more prevalent with open fractures, however Type I injuries are usually not associated with increase in infection rates.
Answer 4: Heterotopic ossification is a common complication after fixation of these injuries. However, it does not always necessitate reoperation.
Figure A is a radiograph from a 59-year-old male that was transferred to a Level I trauma center five hours after a motor vehicle accident. Closed reduction and skeletal traction was successfully performed in the trauma bay. Which of the following factors has been shown to increase the risk of unsatisfactory clinical outcome for this patient?
1) Need for skeletal traction
2) Mechanism of injury
3) Gender
4) Age
5) Time to reduction
Age greater than 55-years-old has been found to be an independent risk factor for inferior clinical outcome in patients with combined acetabular fractures and hip dislocations.
The most important initial step in management following resuscitation involves urgent reduction of the dislocated hip. This should be followed by a preoperative CT scan and ultimately surgical fixation of the combined acetabular fracture. Hip dislocations should be reduced within 6-12 hours for optimal outcome, although different critical times have been cited, particularly for dislocations with concomitant acetabular fractures. Skeletal traction may be required to maintain hip reduction.
Moed et. al. present a Level 3 retrospective review of 100 patients who had been treated with open reduction internal fixation of an acetabular fracture. The authors found that factors associated with unsatisfactory clinical outcomes included age greater than 55, intra-articular comminution, osteonecrosis, and delay of greater than 12 hours for reduction of an associated hip dislocation.
Additionally, they showed that there was a strong association of clinical outcome and final radiographic grade.
Figure A demonstrates an acetabular fracture with concomitant hip dislocation. Incorrect Answers:
Answer 1-3, and 5: Placement and need for skeletal traction, mechanism of
injury, male gender, and time to reduction
A 37-year-old male cashier is shot in the leg. He sustains the injury shown in Figures A and B, and is subsequently taken to the operating room for intramedullary nailing. Figure C shows a radiograph of the nail starting point (*). What complication is most likely to result?
1) Varus malunion
2) Nonunion
3) Valgus malunion
4) Malrotation
5) Superficial peroneal nerve injury
This patient is presenting with a comminuted fracture of the proximal third of the tibia. He is appropriately undergoing intramedullary nail fixation, however, the start point illustrated in Figure C is too medial and often leads to a valgus malunion.
Intramedullary nail fixation is more technically demanding in proximal tibial fractures than diaphyseal fractures. The valgus deformity is due to imbalanced muscle forces on the proximal fragment, which are then accentuated by a start point that is too medial. An apex anterior (procurvatum) deformity can also occur and results from the pull of the patellar tendon or a posteriorly directed nail that deflects off the posterior tibial cortex and rotates the proximal fragment. The ideal starting point for proximal tibial fractures is slightly lateral to the medial aspect of the lateral tibial spine on a true AP x-ray and very proximal and just anterior to the anterior margin of the articular surface.
Nork et al. reported the results of intramedullary nailing of proximal tibial fractures with emphasis on techniques of reduction. Various techniques were found to be successful including attention to the proper starting point, the use of unicortical plates, and the use of a femoral distractor applied to the tibia.
Lowe et al. describe surgical techniques for complex proximal tibial fractures. They describe the extended leg position, use of a femoral distractor, temporary plate fixation, blocking (Poller) screws, and use of percutaneous clamps as means to achieve reduction during fixation.
Figure A and B show an AP and lateral radiograph of a comminuted extra-articular fracture through the proximal third of the tibia. Figure C demonstrates a start point that is too medial (represented by the asterisk) for intramedullary nail fixation. Illustration A and B show the ideal start point for intramedullary nail fixation of the tibia on AP and lateral radiographs.
Incorrect Answers:
Question 40High Yield
In the arthroscopic photograph shown in Figure 5, the structure labeled “A” functions primarily as a restraint to translation of the humeral head in what direction?
Explanation
The superior glenohumeral ligament identified as “A” in the figure functions primarily as a restraint to inferior glenohumeral translation of the adducted arm. The middle glenohumeral ligament is highly variable and pooly defined in up to 40% of the population and functions to restrain anterior translation of the externally rotated arm in the midrange of abduction. The anterior band of the inferior glenohumeral ligament is the primary restraint to anterior/inferior translation of the head with the shoulder abducted to 90 degrees and in maximum external rotation.
REFERENCES: Ticker JB, Bigliani LU, Soslowskiy LJ, et al: Inferior glenohumeral ligament: Geometric and strain-rate dependent properties. J Shoulder Elbow Surg 1996;5:269-279.
Owen MD, Kregel KC, Wall PT, Gisolfi CV: Effects of ingesting carbohydrate beverages during exercise in the heat. Med Sci Sports Exerc 1986;18:568-575.
REFERENCES: Ticker JB, Bigliani LU, Soslowskiy LJ, et al: Inferior glenohumeral ligament: Geometric and strain-rate dependent properties. J Shoulder Elbow Surg 1996;5:269-279.
Owen MD, Kregel KC, Wall PT, Gisolfi CV: Effects of ingesting carbohydrate beverages during exercise in the heat. Med Sci Sports Exerc 1986;18:568-575.
Question 41High Yield
A 60-year-old woman has progressive neck pain, upper extremity pain, and paresthesias. A lateral cervical spine radiograph and an MRI scan are shown in Figures 52a and 52b. What is the most likely underlying diagnosis?
---
---
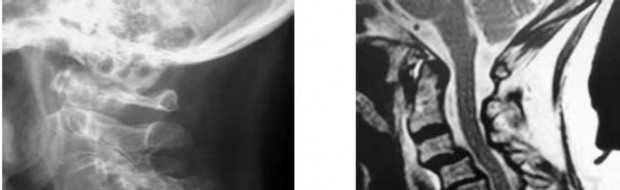
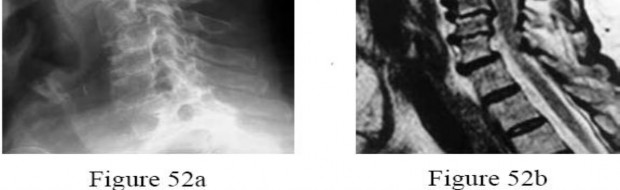
Explanation
The radiograph and sagittal T2-weighted MRI scan show multilevel degenerative changes and subaxial subluxations with anterolisthesis at C3-C4 and C4-C5 and retrolisthesis at C5-C6. In addition, there is evidence of midcervical kyphosis. Such findings are often seen in patients with rheumatoid arthritis. Patients with osteomyelitis typically show increased signal intensity in the disks and vertebral bodies. Patients with ankylosing spondylitis typically show ankylosis of the disks and vertebral
bodies. Age-related degenerative changes typically manifest as degenerative disk disease with occasional single-level spondylolisthesis, but not typically multilevel spondylolisthesis, as seen in this patient. The spinous processes are intact; these changes do not appear to be postoperative.
bodies. Age-related degenerative changes typically manifest as degenerative disk disease with occasional single-level spondylolisthesis, but not typically multilevel spondylolisthesis, as seen in this patient. The spinous processes are intact; these changes do not appear to be postoperative.
Question 42High Yield
A 55-year-old woman presents 5 years after a primary total hip arthroplasty (THA) using a cobalt alloy femoral head and a polyethylene liner. She initially did well, but now has worsening pain and weakness around the hip. She also had one episode of instability. Serum ESR and CRP were within normal limits, and serum metal ion levels demonstrated a cobalt level of 4.0 ng/mL (normal
<0.7 ng/mL) and chromium level of 2.4 ng/mL (normal <0.3 ng/mL). Her metal artifact reduction sequence (MARS) MRI scan is shown in Figure
<0.7 ng/mL) and chromium level of 2.4 ng/mL (normal <0.3 ng/mL). Her metal artifact reduction sequence (MARS) MRI scan is shown in Figure
Explanation
Trunnionosis is a recognized complication following THA and can occur with the use of a cobalt alloy femoral head on either a titanium alloy or cobalt alloy femoral stem. Patients often present with pain or swelling around the hip, but at times can present with instability.
Certain femoral stem designs have been associated with increased reports of trunnionosis. In a patient who presents with instability, swelling, and weakness around the hip with a cobalt alloy femoral head, the potential for trunnionosis and an adverse local tissue reaction should be considered. An appropriate revision option in the setting of well-fixed and well-aligned components would be conversion to a ceramic femoral head and polyethylene liner.
68
Certain femoral stem designs have been associated with increased reports of trunnionosis. In a patient who presents with instability, swelling, and weakness around the hip with a cobalt alloy femoral head, the potential for trunnionosis and an adverse local tissue reaction should be considered. An appropriate revision option in the setting of well-fixed and well-aligned components would be conversion to a ceramic femoral head and polyethylene liner.
68
Question 43High Yield
A 75-year-old woman with rheumatoid arthritis and a long history of oral corticosteroid use sustains a comminuted intra-articular distal humerus fracture. What is the best surgical option?
Explanation
TEA is the best surgical option. McKee and associates published a multicenter randomized controlled trial comparing ORIF with TEA in elderly patients. TEA resulted in better 2-year clinical functional scores and more predictable outcomes compared with ORIF. TEA was also likely to result in a lower reoperation rate; one-quarter of patients with fractures randomized to ORIF could not achieve stable fixation. Further, Frankle and associates reported a comparative study of TEA versus ORIF in 24 elderly women. TEA outcomes were again superior to ORIF at a minimum of 2 years of follow-up. TEA was especially useful in patients with comorbidities that compromise bone stock, including osteoporosis and oral corticosteroid use. Closed reduction and percutaneous pinning studies have not been published on the adult population.
25
25
Question 44High Yield
Figure 2 shows the radiograph of a 26-year-old auto mechanic who injured his right dominant elbow in a fall during a motocross race. Examination reveals pain and catching that limits his range of motion to 45 degrees of supination and 20 degrees of pronation. The interosseous space and distal radioulnar joint are stable. Management should
consist of
consist of
Explanation
The radial head is an important secondary stabilizer of the elbow, helping to resist valgus forces. There has been a movement toward open reduction and internal fixation of the radial head when technically feasible, especially in a relatively high-demand athlete or laborer. The examination and radiograph suggest that displacement of the fragment is great enough to create a mechanical block. Extended splinting would only serve to encourage arthrofibrosis. Early range of motion is appropriate if there is minimal displacement of the radial head fragement, it is stable, and there is no mechanical block to motion. Fragments larger than one third of the joint surface should be excised only if it is not possible to reduce and repair the fragment. Primary excision of the radial head should be avoided if possible. Complications after excision of the radial head include muscle weakness, wrist pain, valgus elbow instability, heterotopic ossification, and arthritis.
REFERENCES: Hotchkiss RN: Displaced fractures of the radial head: Internal fixation or excision? J Am Acad Orthop Surg 1997;5:1-10.
Esser RD, Davis S, Taavao T: Fractures of the radial head treated by internal fixation: Late results in 26 cases. J Orthop Trauma 1995;9:318-323.
REFERENCES: Hotchkiss RN: Displaced fractures of the radial head: Internal fixation or excision? J Am Acad Orthop Surg 1997;5:1-10.
Esser RD, Davis S, Taavao T: Fractures of the radial head treated by internal fixation: Late results in 26 cases. J Orthop Trauma 1995;9:318-323.
Question 45High Yield
A patient has an early stage stress fracture (grade 1) on a technetium bone scan. The magnetic resonance image findings most likely to correlate with the bone scan are:
Explanation
In 1995, Fredrickson and colleagues classified stress fractures into four grades based upon bone scans:
Grade 1Â Â Â Â Â Small ill-defined cortical area of mildly increased activity
Grade 2     Well-defined cortical area of moderately increased cortical activity
Grade 3Â Â Â Â Â Wide, cortical-medullary area of increased activity
Grade 4Â Â Â Â Â Transcortical area of intensely increased activity
In an early stress fracture (grade 1 bone scan criteria), a periosteal high signal on T2-weighted images and a normal marrow signal are present.C orrect Answer: Periosteal high signal on T2; normal marrow signal on T1- and T2-weighted images
Grade 1Â Â Â Â Â Small ill-defined cortical area of mildly increased activity
Grade 2     Well-defined cortical area of moderately increased cortical activity
Grade 3Â Â Â Â Â Wide, cortical-medullary area of increased activity
Grade 4Â Â Â Â Â Transcortical area of intensely increased activity
In an early stress fracture (grade 1 bone scan criteria), a periosteal high signal on T2-weighted images and a normal marrow signal are present.C orrect Answer: Periosteal high signal on T2; normal marrow signal on T1- and T2-weighted images
Question 46High Yield
A 26-year-old recreational athlete sustained an initial dislocation 1 year ago and was treated nonsurgically. He recently sustained a second dislocation and is scheduled for surgical repair. Plain radiographs and MR images reveal no bony defect. What is the difference in recurrence rate after open and arthroscopic repair?
Explanation
Traditionally, recurrence rates associated with open stabilization procedures have been lower than rates associated with arthroscopic repair. Recent studies show that for patients without significant bone loss, however, the recurrence rate is the same for open and arthroscopic surgeries.
RECOMMENDED READINGS
50. [Chalmers PN, Mascarenhas R, Leroux T, Sayegh ET, Verma NN, Cole BJ, Romeo AA. Do arthroscopic and open stabilization techniques restore equivalent stability to the shoulder in the setting of anterior glenohumeral instability? a systematic review of overlapping meta-analyses. Arthroscopy. 2015 Feb;31(2):355-63. doi: 10.1016/j.arthro.2014.07.008. Epub 2014 Sep 10. Review. PubMed PMID: 25217207. ](http://www.ncbi.nlm.nih.gov/pubmed/25217207)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25217207)
51. [Harris JD, Gupta AK, Mall NA, Abrams GD, McCormick FM, Cole BJ, Bach BR Jr, Romeo AA, Verma NN. Long-term outcomes after Bankart shoulder stabilization. Arthroscopy. 2013 May;29(5):920-33. doi: 10.1016/j.arthro.2012.11.010. Epub 2013 Feb 5. Review. PubMed PMID: 23395467. ](http://www.ncbi.nlm.nih.gov/pubmed/23395467)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/23395467)
CLINICAL SITUATION FOR QUESTIONS 41 THROUGH 43
Figures 41a and 41b are the radiographs of a 69-year-old, left-hand-dominant retired man with left shoulder pain. The pain has been present for several years, although he cannot pinpoint the exact time at which it started. He worked in construction but retired 3 years ago. He now reports pain interfering with activities around the house but declines recent trauma or prior shoulder surgery. He has tried different nonsteroidal anti-inflammatory drugs prescribed by his primary care physician, but these do not provide complete relief. Upon examination, he demonstrates pain and crepitus with active and passive shoulder motion. Motion is restricted, but he can actively forward flex to 100 degrees and external rotate to 30 degrees. Rotator cuff testing reveals 5/5 strength bilaterally. He has normal neurovascular examination findings.
RECOMMENDED READINGS
50. [Chalmers PN, Mascarenhas R, Leroux T, Sayegh ET, Verma NN, Cole BJ, Romeo AA. Do arthroscopic and open stabilization techniques restore equivalent stability to the shoulder in the setting of anterior glenohumeral instability? a systematic review of overlapping meta-analyses. Arthroscopy. 2015 Feb;31(2):355-63. doi: 10.1016/j.arthro.2014.07.008. Epub 2014 Sep 10. Review. PubMed PMID: 25217207. ](http://www.ncbi.nlm.nih.gov/pubmed/25217207)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25217207)
51. [Harris JD, Gupta AK, Mall NA, Abrams GD, McCormick FM, Cole BJ, Bach BR Jr, Romeo AA, Verma NN. Long-term outcomes after Bankart shoulder stabilization. Arthroscopy. 2013 May;29(5):920-33. doi: 10.1016/j.arthro.2012.11.010. Epub 2013 Feb 5. Review. PubMed PMID: 23395467. ](http://www.ncbi.nlm.nih.gov/pubmed/23395467)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/23395467)
CLINICAL SITUATION FOR QUESTIONS 41 THROUGH 43
Figures 41a and 41b are the radiographs of a 69-year-old, left-hand-dominant retired man with left shoulder pain. The pain has been present for several years, although he cannot pinpoint the exact time at which it started. He worked in construction but retired 3 years ago. He now reports pain interfering with activities around the house but declines recent trauma or prior shoulder surgery. He has tried different nonsteroidal anti-inflammatory drugs prescribed by his primary care physician, but these do not provide complete relief. Upon examination, he demonstrates pain and crepitus with active and passive shoulder motion. Motion is restricted, but he can actively forward flex to 100 degrees and external rotate to 30 degrees. Rotator cuff testing reveals 5/5 strength bilaterally. He has normal neurovascular examination findings.
Question 47High Yield
Figure 1 is the MRI from a 67-year-old man with severe neck pain 1 week following dental extraction. He has a history of poorly controlled type 2 diabetes mellitus. On examination, he is found to have grade 4 of 5 strength in the bilateral lower extremities.
He is febrile and has an elevated erythrocyte sedimentation rate and an elevated Creactive protein level. His MRI reveals an epidural abscess. What is the best next step?
He is febrile and has an elevated erythrocyte sedimentation rate and an elevated Creactive protein level. His MRI reveals an epidural abscess. What is the best next step?

Explanation
■
The patient has an epidural abscess following a dental procedure. The epidural abscess spans from C2 to the upper thoracic spine. He has severe neck pain, neurologic changes, and elevated laboratory markers. Sang and associates have demonstrated that, in patients older than 65 years with a methicillin-resistant Staphylococcus aureus infection, a history of diabetes, and neurologic deficits, nonsurgical management has a 99% chance of failure. Prompt surgical decompression to evacuate the abscess followed by antibiotic treatment is the best method of treatment for this patient.
The patient has an epidural abscess following a dental procedure. The epidural abscess spans from C2 to the upper thoracic spine. He has severe neck pain, neurologic changes, and elevated laboratory markers. Sang and associates have demonstrated that, in patients older than 65 years with a methicillin-resistant Staphylococcus aureus infection, a history of diabetes, and neurologic deficits, nonsurgical management has a 99% chance of failure. Prompt surgical decompression to evacuate the abscess followed by antibiotic treatment is the best method of treatment for this patient.
Question 48High Yield
Figures 1 and 2 are the radiograph and MRI scan of a 16-year-old boy who injured his right knee by a lateral side impact while playing football. The MRI indicates what structure was most likely injured?
---
---
---
---
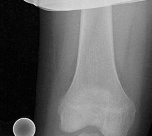
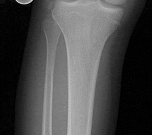
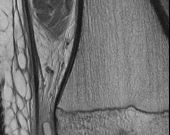
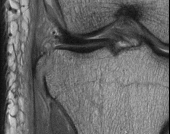
Explanation
This is a rupture of the anterolateral ligament complex and a portion of the IT band. This injury is highly correlated with a complete ACL injury. In the MRI, the curvilinear or elliptic bone fragment (Segond fracture) projected parallel to the lateral aspect of the tibial plateau, the lateral capsular sign, is seen. The lateral capsular sign is also associated with ACL tears. Thus, this is an MRI showing a complete ACL _tear._
Question 49High Yield
Second-impact syndrome following a concussion
Explanation
■
According to several consensus statements, no child or adolescent athlete with a concussion should be allowed to return to play on the same day, regardless of severity. Second-impact syndrome refers to a second traumatic head injury that occurs while an athlete is still experiencing symptoms from the first injury. Young athletes are particularly vulnerable to second-impact syndrome. The mechanism by which this syndrome occurs likely is disruption of cerebral autoregulation, which may result in cerebral vascular congestion, diffuse brain swelling, and death.
According to several consensus statements, no child or adolescent athlete with a concussion should be allowed to return to play on the same day, regardless of severity. Second-impact syndrome refers to a second traumatic head injury that occurs while an athlete is still experiencing symptoms from the first injury. Young athletes are particularly vulnerable to second-impact syndrome. The mechanism by which this syndrome occurs likely is disruption of cerebral autoregulation, which may result in cerebral vascular congestion, diffuse brain swelling, and death.
Question 50High Yield
A 29-year-old woman reports dysesthesias and burning after undergoing bunion surgery that consisted of a proximal crescentic first metatarsal osteotomy 6 months ago. Examination reveals a positive Tinel’s sign at the proximal aspect of the healed incision. What injured nerve is responsible for her continued symptoms?
Explanation
Painful incisional neuromas after bunion surgery frequently involve the dorsomedial cutaneous branch of the superficial peroneal nerve. This is the medial branch of the superficial peroneal nerve that terminates as the dorsomedial cutaneous nerve to the hallux. Branches of the deep peroneal nerve to this area are rare, and no branches to this area exist from the sural nerve. The saphenous nerve branches are generally more proximal, and the medial plantar nerve lies plantarly.
REFERENCES: Kenzora JE: Sensory nerve neuromas: Leading to failed foot surgery. Foot Ankle 1986;7:110-117.
Sarrafian SK: Anatomy of the Foot and Ankle: Descriptive, Topographic, Functional, ed 2. Philadelphia, PA, JB Lippincott, 1993.
REFERENCES: Kenzora JE: Sensory nerve neuromas: Leading to failed foot surgery. Foot Ankle 1986;7:110-117.
Sarrafian SK: Anatomy of the Foot and Ankle: Descriptive, Topographic, Functional, ed 2. Philadelphia, PA, JB Lippincott, 1993.
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding hand-and-wrist-mcq-and-emq-questions
01
Chapter 1
36 min
Hand And Wrist: Answers Emqs Review | Dr Hutaif Hand & - ...
02
Chapter 2
53 min
Advanced Hand & Wrist Orthopedic MCQs: Scaphoid Nonunion & Carpal Collapse
03
Chapter 3
99 min
Orthopedics Hand Review | Dr Hutaif Hand & Wrist Review -...
04
Chapter 4
141 min
Orthopedic Hand Review | Dr Hutaif Hand & Wrist Review - ...
05
Chapter 5
214 min
