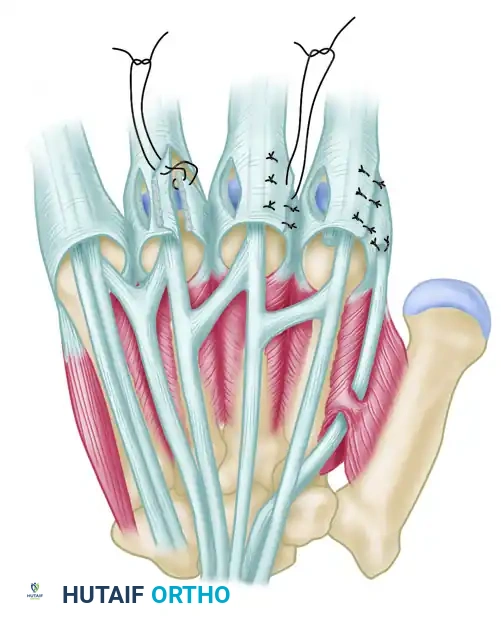
Distal Biceps Tendon Repair & Reconstruction: An Intraoperative Masterclass

Key Takeaway
Join us in the OR for an immersive masterclass on distal biceps tendon repair. We'll meticulously cover acute and chronic ruptures, detailing patient positioning, comprehensive anatomy, and step-by-step execution of single-incision (EndoButton, suture anchor) and two-incision techniques. Learn critical pearls, pitfalls, and postoperative protocols to achieve optimal patient outcomes.
Welcome, fellows, to the operating theater. Today, we're tackling a common yet challenging injury: the distal biceps tendon rupture. This is a procedure where meticulous technique and a deep understanding of the surrounding anatomy are paramount to achieving excellent functional outcomes for our patients. We'll walk through the nuances of both acute repair and chronic reconstruction, emphasizing precision every step of the way.
Understanding the Injury: Definition and Pathogenesis
A distal biceps tendon disruption signifies a tear at its insertion point on the radial tuberosity. While often thought of as a complete avulsion, it's crucial to differentiate this from more proximal injuries at the myotendinous junction or partial tears at the insertion. These distinctions guide our treatment strategy, as more proximal injuries are typically managed non-operatively.
The typical mechanism involves an eccentric muscle contraction – think of a sudden, forceful extension of the forearm from a flexed position while the biceps is actively firing. This often occurs in middle-aged men, mirroring the demographic for pectoralis major and Achilles tendon ruptures. Factors like an avascular zone just proximal to the insertion and potential impingement in the interosseous space between the radial tuberosity and proximal ulna may predispose the tendon to rupture.
Partial tears, in contrast to complete avulsions, usually lack the dramatic ecchymosis and proximal retraction. Patients often present later with persistent pain during resisted flexion and supination, and while the tendon is palpable, it's frequently tender. These partial tears can sometimes progress to complete ruptures if left untreated or if the inciting force recurs.
Clinical Presentation and Diagnostic Approach
When a patient presents with a suspected distal biceps rupture, our initial assessment is critical. A history of a rapid eccentric load on the involved extremity is almost universally present. In acute, complete ruptures, you'll typically see significant ecchymosis spreading across the antecubital fossa, distal arm, and proximal forearm. The distal biceps tendon will not be palpable in the antecubital fossa, and comparison to the contralateral, uninjured side is always helpful.
The "hook test" is a highly reliable diagnostic tool. To perform this, the patient actively supinates the forearm while you, the examiner, attempt to "hook" the distal biceps tendon from the lateral side. In a complete rupture, you won't be able to hook anything. Local edema can sometimes obscure the findings, but the hook test remains remarkably sensitive.
While MRI is generally not necessary to confirm a complete rupture, it can be invaluable in specific scenarios. If you suspect the tendon is intact but the patient has symptoms, MRI can help identify more proximal myotendinous junction injuries or subtle partial tears at the insertion, which might otherwise be missed.
Nonoperative Management: When is it an Option?
For complete distal biceps tendon ruptures, nonoperative management is an option, but it comes with a significant functional trade-off. Patients typically experience a 25% reduction in flexion strength and a substantial 40% loss of supination strength. While pain often subsides quickly, many patients report fatigue-type pain and cramping in the retracted muscle belly, especially those whose occupations demand repetitive supination (e.g., mechanics, plumbers).
If a patient's job and lifestyle are compatible with this expected strength deficit, and they are fully informed, then nonoperative management focusing on pain reduction, swelling control, and allowing use as tolerated, followed by strengthening of elbow flexion and supination, can be acceptable.
For partial tears or myotendinous junction injuries, nonoperative management is often the first line. These injuries are typically more painful than complete tears. We usually recommend a minimum of 3 to 4 months of observation and conservative treatment. Operative intervention is considered if nonoperative management fails to alleviate pain or restore function.
Preoperative Planning and Patient Positioning
Before we even make an incision, meticulous planning is key. For chronic ruptures, we must discuss the potential need for a graft with the patient. Options include semitendinosus autograft or allograft, Achilles tendon allograft (with or without a bone plug), flexor carpi radialis autograft, or fascia lata. We've seen success with primary repair out to 3 months, as the biceps brachii, like the pectoralis major, has a remarkable capacity to stretch. Beyond that, a graft becomes increasingly likely.
Now, let's get our patient positioned.
Patient Positioning:
* Supine position: The patient is placed supine on the operating table.
* Armboard: The affected extremity is positioned on a dedicated armboard, allowing full access to the antecubital fossa and forearm.
* Sterile tourniquet: A sterile tourniquet is applied to the upper arm. We'll inflate this once we're ready to proceed with the incision to ensure a bloodless field, which is critical for identifying delicate neurovascular structures.
* Fluoroscopy setup: If we're using an EndoButton technique, ensure the C-arm is draped and positioned for easy intraoperative access to confirm hardware placement.
Surgical Approaches: Single-Incision vs. Two-Incision
Historically, two-incision techniques were common but were associated with complications like heterotopic ossification and posterior interosseous nerve (PIN) palsy. This led to the development and widespread adoption of single-incision anterior approaches, which offer excellent outcomes with reduced morbidity. Today, we'll focus primarily on the single-incision anterior approach using the EndoButton, as it has demonstrated superior ultimate tensile strength and excellent clinical results. We'll also briefly touch upon suture anchor and interference screw fixation, and the two-incision technique for completeness.
Intraoperative Execution: The Single-Incision Anterior Approach (EndoButton Technique)
Alright, fellows, let's scrub in.
1. Incision and Initial Dissection
"Surgeon, let's begin with our incision. We'll make a longitudinal 4 to 5-cm anterior incision. Start precisely at the antecubital fossa and extend distally along the ulnar border of the brachioradialis muscle. This interval helps us avoid critical structures."
"As we deepen our dissection, meticulous care is required. Identify and carefully protect two key nerves: the lateral antebrachial cutaneous nerve (LABCN), which provides sensation to the radial forearm, and the superficial radial nerve (SRN). These are sensory nerves, and injury can lead to significant paresthesias or numbness. Use fine-tipped scissors and careful blunt dissection to sweep them away from our operative field."
2. Tendon Retrieval and Preparation
"Now, we need to locate and retrieve the distal biceps tendon stump. Often, it has retracted proximally, sometimes quite significantly. To facilitate retrieval, I'll ask the assistant to flex the elbow and use a retractor to gently lift the skin of the distal arm, bringing the retracted tendon into better view."
"Be prepared for some challenges here. The tendon can be quite adherent to adjacent tissues or the lacertus fibrosus, which, if intact, may have mitigated the degree of proximal retraction. If necessary, a limited tenolysis will be required to mobilize the tendon stump. Again, be extremely cautious: protect and isolate the lateral antebrachial cutaneous nerve and, critically, the brachial artery, which lies deeper and more medially. If the tendon cannot be retrieved through this anterior incision, don't hesitate. We can make a separate, smaller incision medially along the distal aspect of the arm to isolate and prepare the tendon there, then pass it into our primary distal wound."
"Once the tendon is isolated and adequately mobilized, we'll prepare its distal end for fixation. Take a no. 2 nonabsorbable suture – I prefer a strong, braided material like FiberWire. We'll weave this into the distal biceps tendon using a locking Krackow technique or another robust locking suture technique. The goal here is to create a strong, secure purchase on the tendon. Ensure your locking sutures extend approximately 4 to 5 cm proximally from the tendon end, but leave about 1 cm of the distal biceps tendon unlocked. This unlocked segment will sit flush against the radial tuberosity, maximizing bone-tendon contact."
3. EndoButton Attachment
"Now, let's attach the EndoButton. We'll take the two free ends of our no. 2 nonabsorbable suture, extending from the tendon stump, and pass them through the two central holes of the EndoButton."
"Secure the tendon to the button by tying the sutures firmly. The critical detail here is to leave absolutely no space between the end of the tendon and the EndoButton. We want a tight, direct apposition."

TECH FIG 1 • A. EndoButton attached to the distal end of the biceps tendon.
"Alternatively, if you prefer, one suture from the tendon can be passed through one central hole of the EndoButton, then back through the other central hole, and the knot tied. This places the knot between the EndoButton and the tendon stump, which some surgeons prefer for a flatter profile. Either method is acceptable as long as the tendon-button interface is secure."
"Next, we'll place our 'kite strings.' These are typically passing sutures, often a different color, placed through the other two peripheral holes of the EndoButton. These will be crucial for guiding and flipping the button."
4. Radial Tuberosity Preparation
"With our tendon prepared, we now turn our attention to the radial tuberosity. The assistant should hold the forearm in full supination throughout this step to bring the tuberosity into optimal view and prevent iatrogenic injury to the posterior interosseous nerve, which is most vulnerable in pronation. We'll use two small Bennett retractors to gently expose the radial tuberosity, carefully protecting the surrounding soft tissues."
"Using a high-speed burr, we'll create an oval cortical window in the radial tuberosity. This window should be roughly the same dimension as the distal tendon stump we've prepared. This provides a broad, cancellous bed for tendon healing. Once the cortical window is established, we'll switch to the specialized EndoButton drill. This drill is designed to create a precise bicortical hole in the far cortex, which will accommodate the EndoButton itself."
5. Passing and Securing the EndoButton
"Now for the clever part. We'll use Keith needles or a Beath needle to pass our 'kite strings' – those passing sutures from the EndoButton – through the bicortical hole we just created. Carefully guide the needles, ensuring they exit through the skin on the dorsal side of the forearm."
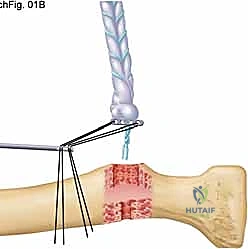
TECH FIG 1 • B. A Keith needle is placed to pass the suture.
"Once retrieved, we'll apply gentle but firm tension on one of the kite strings. This action draws the EndoButton in its vertical orientation through the hole in the far cortex of the radius. You'll feel a distinct 'pop' as it passes through."
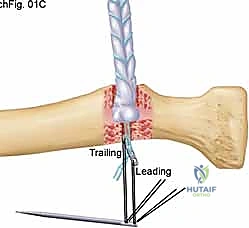
TECH FIG 1 • C. The tendon is pulled into the proximal radial hole as the EndoButton is advanced through the distal hole.
"With the EndoButton now on the far side of the radius, we'll pull the other suture – the second kite string – to flip it. You'll feel it rotate and lock into its horizontal orientation against the far cortex of the radius. This effectively creates a strong, cortical button fixation."

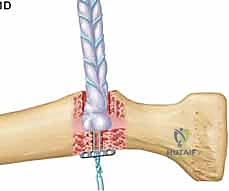
TECH FIG 1 • D. The EndoButton is flipped to secure it on the other side of the radial cortex.
"At this critical juncture, we'll bring in the fluoroscopy. We absolutely must confirm the precise placement of the button on the far side of the radial cortex. We're looking for a clear horizontal orientation, confirming it's securely seated."
"Once fluoroscopy confirms proper button placement, we'll pull one of the original no. 2 passing sutures (the ones directly attached to the tendon) independently. This action draws the prepared distal biceps tendon directly into the radial tuberosity, seating it firmly within our prepared cortical window. We want firm, anatomic tendon placement."
"Visually confirm that the tendon is seated anatomically and under appropriate tension. Once satisfied, the passing sutures (kite strings) can be completely pulled out and removed."
💡 Pearls and Pitfalls for EndoButton Technique
Pearl: Always prepare the biceps tendon with its robust Krackow stitch before you start preparing the radial tuberosity. This ensures your tendon is ready to go once the bone tunnel is complete, minimizing open time.
Pitfall: Inadequate tendon mobilization can lead to excessive tension on the repair, increasing the risk of pull-out or gapping. Don't be afraid to perform a thorough tenolysis or, if necessary, a medial incision for better access.
Pearl: Maintain full forearm supination during radial tuberosity preparation to protect the posterior interosseous nerve.
Pitfall: Failure to confirm EndoButton flip and position with fluoroscopy. A vertically oriented or malpositioned button will not provide secure fixation and is a recipe for early failure.
Salvage: If the button doesn't flip, gently manipulate the forearm and re-tension the kite strings. If it remains problematic, you may need to re-drill or switch to an alternative fixation method like suture anchors.
Alternative Single-Incision Fixation: Suture Anchor or Interference Screw
"For those who prefer other single-incision techniques, the initial anterior approach and tendon retrieval remain largely the same. However, the radial tuberosity preparation differs."
Suture Anchor Fixation:
"If you opt for suture anchors, after retrieving the tendon, we'll lightly decorticate the radial tuberosity to create a bleeding bone bed for optimal healing. Then, we'll place our suture anchors of choice. Typically, two anchors are used to provide broad fixation. We'll then pass the sutures through the prepared tendon stump and use some form of a sliding knot to advance the tendon firmly onto the bone, ensuring good apposition."
Interference Screw Fixation:
"For interference screw fixation, a precise hole is drilled into the radial tuberosity. The diameter of this hole is critical and depends entirely on the specific interference screw system and screw size you're using. The prepared tendon is then inserted into this tunnel, and the interference screw is advanced alongside it, compressing the tendon against the bone for a tight, durable fixation."
💡 Pearls and Pitfalls for Suture Anchor/Interference Screw
Pitfall: Improper tunnel sizing for interference screws can lead to either loose fixation or tendon strangulation. Always follow the manufacturer's guidelines meticulously.
Pearl: For suture anchors, ensure adequate decortication of the tuberosity to promote robust tendon-to-bone healing. Use multiple anchors for broad, secure fixation.
Salvage: If an interference screw strips, you may need to upsize the screw or switch to suture anchors. If suture anchors pull out, consider placing new anchors in a different trajectory or converting to an EndoButton if bone stock allows.
The Two-Incision Technique (Historical Context and Specifics)
"While less common now due to the advantages of single-incision approaches, it's important to understand the two-incision technique, especially for complex cases or revision scenarios."
1. Incisions and Initial Dissection
"First, a transverse anterior incision is made in the antecubital flexion crease. This incision is primarily used to locate and retrieve the distal tendon stump."
"Concurrently, a second longitudinal incision is made approximately 1 cm radial to the subcutaneous border of the ulna in the proximal forearm, at the level of the biceps tuberosity. This posterior incision provides direct access to the radial tuberosity."
2. Radial Tuberosity Preparation (Two-Incision)
"With the forearm placed in maximal pronation, we'll create an oval cavity in the biceps tuberosity using a burr. This pronated position brings the tuberosity to the most accessible position posteriorly. Once the cavity is created, we then supinate the forearm to drill our fixation holes into this cavity. Supination helps protect the posterior interosseous nerve during drilling by moving it away from the tuberosity."
3. Tendon Preparation and Passage
"A no. 2 Fiberwire suture is placed into the distal tendon stump using a Krackow technique, similar to our single-incision approach."
"Now, the critical step: we dissect through the extensor carpi ulnaris (ECU) muscle and then carefully through the supinator muscle to expose the radial tuberosity from the posterior aspect. During this dissection, fellows, take great care to avoid subperiosteal dissection on the ulna. This is a major risk factor for developing synostosis, or abnormal bone formation between the radius and ulna, which can severely limit forearm rotation."
"The sutures from the prepared tendon, still in the anterior wound, are then passed from the anterior to the posterior incision using a long hemostat. It is absolutely critical to pass these sutures through the interosseous space between the radius and ulna to avoid neurovascular structures. Once retrieved through the posterior incision, the sutures are then passed through the drill holes we made in the radial tuberosity and tied over bone with the forearm held in supination. This final supinated position helps to minimize tension on the repair during healing."
💡 Pearls and Pitfalls for Two-Incision Technique
Surgical Warning: The posterior interosseous nerve (PIN) is highly vulnerable during the two-incision approach, especially during dissection through the supinator and subperiosteal dissection on the ulna. Always identify and protect it.
Pitfall: Subperiosteal dissection on the ulna significantly increases the risk of heterotopic ossification and synostosis, leading to severe loss of forearm rotation. Stay strictly on the radial side.
Pearl: Ensure the forearm is maximally pronated for burring the tuberosity and then supinated for drilling the holes and tying the sutures. This optimizes exposure and protects the PIN.
Salvage: If a synostosis develops postoperatively, aggressive physical therapy may be initiated. If non-operative measures fail and function remains severely limited, surgical resection of the synostosis may be considered, but it's a challenging revision.
Chronic Distal Biceps Tendon Reconstructions
"For chronic distal biceps tendon ruptures – typically those presenting beyond 3 months, though we've had success with primary repair up to 3 months – a more extensive approach is often required, and a graft is usually necessary to bridge the gap."
1. Enhanced Exposure and Dissection
"We'll need more comprehensive exposure of both the biceps tendon stump and its myotendinous junction. This often necessitates a second incision at the medial aspect of the distal arm in addition to our primary anterior incision. While one could connect the two anterior incisions, this risks creating additional scarring, which we want to avoid."
"Expect significant scarring and adhesions, especially between the retracted biceps tendon and the lacertus fibrosus. A meticulous dissection is paramount here to identify and protect the lateral antebrachial cutaneous nerve and the musculocutaneous nerve, which may be entrapped in scar tissue. Some of the lacertus fibrosus can actually be incorporated into the reconstruction to add strength."
2. Graft Harvest and Preparation
"For this case, we'll use a semitendinosus autograft. The harvest is performed in a fashion similar to that used for anterior cruciate ligament reconstructions, typically from the ipsilateral leg. Once harvested, the semitendinosus graft is doubled up and folded on itself."
TECH FIG 2 • A. Hamstring tendon is doubled up and folded on itself and the free ends are passed into the distal end of the biceps tendon stump to add length.
3. Graft Integration and Fixation
"The two free ends of the doubled graft are then meticulously woven into the remaining distal biceps tendon and the myotendinous junction. The free ends of the tendon graft will exit laterally from the biceps stump."
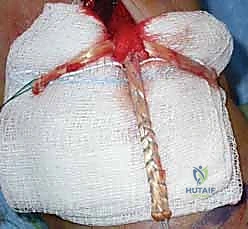
TECH FIG 2 • B. The free ends of the hamstrings tendon graft are woven into the biceps tendon stump.
"A Bunnell tendon passer is an incredibly effective tool for smoothly passing these tendon ends through the biceps stump. The goal is to create a robust graft-tendon construct that effectively lengthens the biceps unit."
"The length of the graft is chosen so that the entire reconstruction is tight at approximately 60 degrees of elbow flexion. This ensures optimal tension for functional recovery without over-tensioning. You can accomplish this by fixing the graft distally first and then performing the weave, or vice versa, depending on your preference and the specific anatomy."
"Finally, a strong nonabsorbable suture is passed through this graft-tendon construct, and this is then securely fixed to the radial tuberosity using either the EndoButton, suture anchor, or interference screw technique, as previously described for acute repairs."
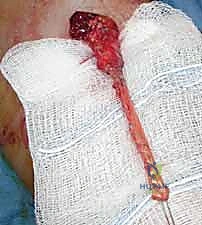
TECH FIG 2 • A B. The free ends of the hamstrings tendon graft are woven into the biceps tendon stump. A B
💡 Pearls and Pitfalls for Chronic Reconstructions
Pitfall: Underestimating the amount of scarring and retraction in chronic cases. Inadequate mobilization will lead to a high-tension repair and potential failure.
Pearl: Meticulous neurolysis of the LABCN and musculocutaneous nerve from scar tissue is crucial to prevent postoperative neuropraxia or persistent pain.
Pitfall: Incorrect graft tension. A graft that is too loose will result in persistent weakness, while a graft that is too tight can lead to flexion contracture. Aim for tight at 60 degrees of elbow flexion.
Salvage: If a graft ruptures or fails, a revision reconstruction with a larger or different type of allograft may be necessary, often requiring a more extensive exposure.
Postoperative Care and Rehabilitation
Our job isn't done when the last stitch is placed. Postoperative care is just as critical for a successful outcome.
Immediate Postoperative Period:
- Radiographs: Obtain radiographs immediately after surgery to confirm proper position of the fixation hardware (EndoButton, anchors, or screws). We'll repeat these at the first postoperative visit.
- Immobilization: For an EndoButton repair, we typically remove the splint at 2 weeks.
Rehabilitation Progression (EndoButton Repair Protocol):
- Weeks 0-2: Immobilization in a splint, typically in 90 degrees of flexion with neutral forearm rotation.
- Weeks 2-6: Splint removal. Initiate active and passive range of motion (ROM) exercises for the elbow and forearm. Crucially, no lifting greater than the weight of a cup of coffee during this period. The goal is gentle motion to prevent stiffness without stressing the repair.
- Weeks 6+: Begin progressive strengthening exercises for elbow flexion and supination. Formal physical therapy may be beneficial, though for many patients with good compliance, a home exercise program is sufficient.
Alternative Rehabilitation Approaches:
- Some authors advocate for earlier, more aggressive range-of-motion therapy, particularly with robust fixation methods.
- Conversely, a more conservative approach might limit full elbow extension until 6 to 8 weeks after surgery, especially in cases where the repair tension was high or bone quality was suboptimal.
Potential Complications and Management:
- Loss of Motion: This is a significant concern.
- Heterotopic Ossification (HO): More common with the two-incision technique but can occur with any approach. Prophylaxis with NSAIDs (e.g., indomethacin) or low-dose radiation may be considered in high-risk patients. If severe HO develops, surgical excision may be required once mature.
- Stiffness/Flexion Contracture: Aggressive but controlled ROM exercises are key. If conservative measures fail, manipulation under anesthesia or surgical release may be necessary.
- Nerve Palsy:
- Lateral Antebrachial Cutaneous Nerve (LABCN) or Superficial Radial Nerve (SRN) Neuropraxia: Often transient, causing numbness or tingling. Reassurance and observation are usually sufficient. If symptoms persist and are debilitating, nerve exploration might be considered.
- Posterior Interosseous Nerve (PIN) Palsy: A rare but devastating complication, typically associated with the two-incision approach. Can lead to wrist drop and finger extension weakness. If recognized intraoperatively, immediate decompression is critical. Postoperatively, observation and splinting are initial steps. If no recovery, nerve exploration and possible grafting may be indicated.
- Infection: Standard wound care and antibiotics. If deep infection, surgical debridement and prolonged antibiotics are required.
REFERENCES
OUTCOMES
- Patient-weighted outcome measures such as the DASH and the MEPS have been used in many studies and have demonstrated excellent results with primary repair. 1,5
-
Objective data including strength testing have also demonstrated good results with anatomic repair, especially with regard to restoring supination strength. 8
-
Chronic repairs or reconstructions have also performed well. 17
COMPLICATIONS
- Reruptures are rare in most series irrespective of the method of fixation.
-
Classic two-incision technique: Heterotopic ossification, radioulnar synostosis, and posterior interosseous nerve palsies. Heterotopic ossification and radioulnar synostosis rates have been decreased by avoiding the ulnar periosteum. 3,7
-
Single-incision technique: Lateral antebrachial cutaneous and superficial radial nerve palsies
-
Bain GI, Prem H, Heptinstall RJ, et al. Repair of distal biceps tendon rupture: a new technique using the EndoButton. J Shoulder Elbow Surg 2000;9:120–126.
-
Baker BE, Bierwagen D. Rupture of the distal tendon of the biceps brachii: operative versus non-operative treatment. J Bone Joint Surg Am 1985;67A:414–417.
-
Failla JM, Amadio PC, Morrey BF, et al. Proximal radioulnar synostosis after repair of distal biceps brachii rupture by the two-incision technique: report of four cases. Clin Orthop Relat Res 1990;253:133–136.
-
Greenberg JA, Fernandez JJ, Wang T, et al. EndoButton-assisted repair of distal biceps tendon ruptures. J Shoulder Elbow Surg 2003;12:484–490.
-
John CK, Field LD, Weiss KS, et al. Single-incision repair of acute distal biceps ruptures by use of suture anchors. J Shoulder Elbow Surg 2007;16:78–83.
-
Kaplan FT, Rokito AS, Birdzell MG, et al. Reconstruction of chronic distal biceps tendon rupture with use of fascia lata combined with a ligament augmentation device: a report of 3 cases. J Shoulder Elbow Surg 2002;11:633–636.
-
Kelly EW, Morrey BF, O’Driscoll SW. Complications of repair of the distal biceps tendon with the modified two-incision technique. J Bone Joint Surg Am 2000;82A:1575–1581.
-
Klonz A, Loitz D, Wohler P, et al. Rupture of the distal biceps brachii tendon: isokinetic power analysis and complications after anatomic reinsertion compared with fixation to the brachialis muscle. J Shoulder Elbow Surg 2003;12:607–611.
-
Levy HJ, Mashoof AA, Morgan D. Repair of chronic ruptures of the distal biceps tendon using flexor carpi radialis tendon graft. Am J Sports Med 2000;28:538–540.
-
Mazzocca AD, Burton KJ, Romeo AA, et al. Biomechanical evaluation of 4 techniques of distal biceps brachii tendon repair. Am J Sports Med 2007;35:252–258.
-
Morrey BF, Askew LJ, An KN, et al. Rupture of the distal tendon of the biceps brachii: a biomechanical study. J Bone Joint Surg Am 1985;67A:418–421.
-
O’Driscoll SW, Goncalves LB, Dietz P. The hook test for distal biceps tendon avulsion. Am J Sports Med 2007;35:1865–1869.
-
Sanchez-Sotelo J, Morrey BF, Adams RA, et al. Reconstruction of chronic ruptures of the distal biceps tendon with use of an Achilles tendon allograft. J Bone Joint Surg Am 2002;84A:999–1005.
-
Schamblin ML, Safran MR. Injury of the distal biceps at the musculotendinous junction. J Shoulder Elbow Surg 2007;16:208–212 [e-pub Dec. 13, 2006].
-
Seiler JG 3rd, Parker LM, Chamberland PD, et al. The distal biceps tendon. Two potential mechanisms involved in its rupture: arterial supply and mechanical impingement. J Shoulder Elbow Surg 1995; 4:149–156.
-
Spang JT, Weinhold PS, Karas SG. A biomechanical comparison of EndoButton versus suture anchor repair of distal biceps tendon injuries. J Shoulder Elbow Surg 2006;15:509–514.
-
Wiley WB, Noble JS, Dulaney TD, et al. Late reconstruction of chronic distal biceps tendon ruptures with a semitendinosus autograft technique. J Shoulder Elbow Surg 2006;15:440–444.
You Might Also Like