Patient Presentation and History
We present the case of a 32-year-old professional ballet dancer, female, presenting with a 14-month history of insidious onset right posterior ankle pain. The patient reports a gradual increase in symptoms, initially presenting as a dull ache during pliés and relevés, progressing to sharp, debilitating pain with sustained pointe work and during the push-off phase of jumping. The pain is exacerbated by passive dorsiflexion of the ankle and hallux extension, as well as active hallux flexion against resistance. She describes occasional subjective "catching" or "snapping" sensation in the posterior ankle, particularly when initiating movement after a period of rest.
Her past medical history is unremarkable. She denies any specific acute traumatic event, attributing the onset to cumulative microtrauma inherent to her profession. She reports no systemic inflammatory conditions, diabetes mellitus, or other relevant comorbidities. Prior conservative management, supervised by her company's physical therapist, included activity modification, relative rest, non-steroidal anti-inflammatory drugs (NSAIDs), corticosteroid injection into the posterior ankle joint (under ultrasound guidance, approximately six months prior), and a structured rehabilitation program focusing on ankle and foot intrinsic muscle strengthening, Achilles stretching, and proprioceptive exercises. Despite these interventions, her symptoms have remained refractory, significantly impacting her ability to perform and necessitating a full work stoppage for the past three months. She expresses a strong desire to return to her elite-level performance.
The biomechanical demands of classical ballet place extraordinary stress on the posterior ankle complex. The "en pointe" and "demi-pointe" positions require extreme plantarflexion, which dramatically decreases the volume of the posterior ankle compartment. This hyperplantarflexion creates a "nutcracker" phenomenon, compressing the posterior capsular structures, the posterior process of the talus, and any accessory ossicles (such as an os trigonum) between the posterior tibial plafond and the superior surface of the calcaneus. Concurrently, the flexor hallucis longus (FHL) tendon undergoes immense tensile loading and excursion during the transition from plié (dorsiflexion) to relevé (plantarflexion), predisposing the tendon to friction, microtearing, and subsequent stenosing tenosynovitis within its fibro-osseous tunnel.
The chronicity of her symptoms, coupled with the classic mechanical presentation, strongly suggests a combined pathology of posterior ankle impingement and FHL tenosynovitis, a constellation of findings frequently termed "dancer's tendinitis" or posterior impingement syndrome. The failure of a comprehensive, six-month non-operative protocol, including image-guided corticosteroid injection, indicates a structural mechanical block and chronic fibrotic changes within the tendon sheath that are unlikely to resolve without surgical intervention.
Clinical Examination Findings
Inspection
On inspection, the patient presented with subtle, diffuse swelling localized to the posteromedial aspect of the right ankle, compared to the contralateral limb. There was no obvious erythema, warmth, or skin discoloration. Gait analysis demonstrated a cautious, shortened stance phase on the right foot, with reduced push-off and an antalgic component during ambulation. Active range of motion of the ankle revealed a painful arc during full plantarflexion and dorsiflexion, with an evident restriction in the terminal range of dorsiflexion. Active flexion of the great toe against resistance reproduced her pain and demonstrated a subtle weakness compared to the left. No specific deformities of the foot or ankle were noted, and arches were well-maintained.
Palpation
Palpation elicited exquisite tenderness along the course of the flexor hallucis longus (FHL) tendon, specifically posterior to the medial malleolus and within the fibro-osseous tunnel distal to the talar body. Pressure applied directly over the os trigonum region (if present) also reproduced her symptoms. A subtle crepitus was noted with passive motion of the great toe during palpation. The posterior aspect of the talus, in the interval between the Achilles tendon and the posterior tibial neurovascular bundle, was tender. The deltoid ligament complex and posterior tibial tendon were non-tender.
Range of Motion
- Ankle
- Dorsiflexion 10 degrees (painful at end range, contralateral 20 degrees)
- Plantarflexion 40 degrees (painful at end range, contralateral 50 degrees)
- Inversion 25 degrees (contralateral 30 degrees)
- Eversion 10 degrees (contralateral 15 degrees)
- Hallux
- Interphalangeal joint flexion Full, but painful against resistance.
- Metatarsophalangeal joint flexion Full, painful against resistance.
Provocative Testing
Specific provocative maneuvers for FHL tenosynovitis and posterior impingement were performed to isolate the precise anatomical pain generators.
- FHL Palpation with Passive Hallux Motion Significant pain and crepitus noted when the great toe was passively moved from extension to flexion while palpating the FHL tendon posterior to the medial malleolus.
- Resisted Hallux Flexion Pain sharply reproduced along the FHL tendon and posterior ankle.
- Posterior Ankle Impingement Test Forced passive plantarflexion of the ankle joint produced sharp, reproducible pain in the deep posterior ankle compartment. This pain was further exacerbated by simultaneously applying a rapid, short-amplitude overpressure at the end range of plantarflexion, confirming the mechanical entrapment of posterior structures between the tibia and calcaneus.
- FHL Stretch Test Passive forced dorsiflexion of the ankle combined with passive extension of the first metatarsophalangeal and interphalangeal joints elicited severe tension and pain along the posteromedial ankle, indicative of restricted tendon excursion within the stenotic sheath.
Neurological and Vascular Assessment
A comprehensive neurovascular examination of the lower extremity was unremarkable. Dorsalis pedis and posterior tibial pulses were palpable and symmetric bilaterally (2+). Capillary refill was brisk (less than 2 seconds) in all digits. Sensation was grossly intact to light touch and pinprick in the superficial peroneal, deep peroneal, saphenous, sural, medial plantar, and lateral plantar nerve distributions. Tinel's sign over the tarsal tunnel was negative, helping to differentiate the posteromedial pain from proximal tibial nerve entrapment. Motor function of the anterior compartment, lateral compartment, and superficial posterior compartment musculature was fully intact (5/5 strength).
Imaging and Diagnostics
The diagnostic workup for posterior ankle impingement and FHL tenosynovitis requires a multi-modality approach to evaluate both the osseous architecture and the integrity of the soft tissue structures.
Radiographic Evaluation
Standard weight-bearing radiographs of the right ankle were obtained, including anteroposterior (AP), lateral, and mortise views. The AP and mortise views demonstrated well-maintained tibiotalar joint space with no evidence of osteochondral lesions of the talar dome or arthritic changes. The lateral weight-bearing radiograph was the most revealing, demonstrating a prominent, un-united ossicle posterior to the talus, consistent with a large os trigonum. The synchondrosis between the os trigonum and the posterior talar body appeared irregular and slightly sclerotic, suggesting chronic mechanical stress and micromotion at this interface. There was no evidence of acute fracture, Haglund's deformity, or calcaneal spurring.
Advanced Imaging
Given the patient's refractory symptoms and the need for precise surgical planning, Magnetic Resonance Imaging (MRI) without contrast was indicated. The MRI protocol included T1-weighted, T2-weighted, and Short Tau Inversion Recovery (STIR) sequences in the sagittal, coronal, and axial planes.
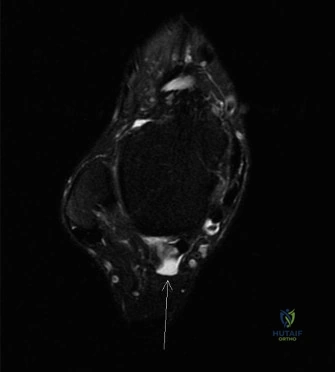
The MRI findings confirmed the clinical suspicion of a combined pathology.
- Osseous Findings The sagittal STIR images revealed significant bone marrow edema within the os trigonum and the adjacent posterior aspect of the talus, confirming active inflammation and mechanical impingement at the synchondrosis. The os trigonum measured approximately 12 mm by 8 mm. No osteochondral defects were noted in the tibiotalar or subtalar joints.
- Soft Tissue Findings Axial and sagittal T2-weighted images demonstrated a circumferential rind of hyperintense fluid surrounding the flexor hallucis longus tendon as it coursed through the fibro-osseous tunnel posterior to the talus and medial malleolus. The FHL tendon itself exhibited mild tendinosis, characterized by slight thickening and intermediate intrasubstance signal, but there was no evidence of high-grade partial or complete tearing. The FHL retinaculum appeared thickened.
- Capsuloligamentous Structures The posterior joint capsule was thickened and edematous. The posterior talofibular ligament (PTFL) and the posterior inferior tibiofibular ligament (PITFL) were intact. The Achilles tendon demonstrated normal morphology and signal intensity, ruling out insertional or midsubstance tendinopathy.
Dynamic Ultrasound
To further evaluate the subjective "snapping" reported by the patient, a dynamic ultrasound examination was performed. High-frequency linear transducer evaluation during active hallux flexion and extension revealed restricted excursion of the FHL tendon within its sheath. A distinct "triggering" phenomenon was observed as the nodular, thickened portion of the tendon attempted to pass through the proximal aspect of the fibro-osseous tunnel, correlating perfectly with the patient's symptoms. Power Doppler imaging showed increased vascularity within the tenosynovium, indicating active, chronic inflammation.
Differential Diagnosis
The differential diagnosis for posterior ankle pain in an elite dancer is broad, encompassing osseous, tendinous, capsular, and neurological etiologies. Precise localization of the pain generator is critical for appropriate surgical planning.
| Pathology | Clinical Presentation | Key Physical Exam Findings | Distinguishing Imaging Features |
|---|---|---|---|
| Posterior Ankle Impingement (Os Trigonum Syndrome) | Deep posterior ankle pain exacerbated by forced plantarflexion (en pointe). Insidious onset. | Positive posterior impingement test. Tenderness deep to the Achilles tendon. | Lateral X-ray: Os trigonum or prominent Stieda process. MRI: Bone marrow edema in os trigonum/posterior talus. |
| Flexor Hallucis Longus Tenosynovitis | Posteromedial ankle pain, pain with push-off, triggering or snapping of the great toe. | Tenderness along FHL sheath. Pain with resisted hallux flexion and passive extension. | MRI: Fluid in FHL sheath, tendon thickening. Ultrasound: Dynamic triggering, tenosynovial thickening. |
| Insertional Achilles Tendinopathy | Posterior heel pain, stiffness in the morning, pain with initial weight-bearing. | Tenderness at the Achilles insertion on the calcaneus. Palpable spur or thickening. | Lateral X-ray: Calcaneal spur (Haglund's). MRI: Thickening and increased signal at Achilles insertion, retrocalcaneal bursitis. |
| Tarsal Tunnel Syndrome | Radiating pain, numbness, and tingling into the plantar aspect of the foot and toes. | Positive Tinel's sign posterior to the medial malleolus. Sensory deficits in tibial nerve distribution. | EMG/NCS: Delayed conduction velocities of the tibial nerve. MRI: Space-occupying lesion (ganglion, lipoma) in the tarsal tunnel. |
| Posterior Tibial Tendon Dysfunction | Medial ankle pain, progressive loss of the medial longitudinal arch, weakness in inversion. | Tenderness along PTT. "Too many toes" sign. Inability to perform a single-leg heel rise. | MRI: PTT tenosynovitis, partial tearing, or complete rupture. Spring ligament attenuation. |
| Subtalar Joint Pathology (Arthritis or Coalition) | Deep hindfoot pain, difficulty walking on uneven ground, stiff hindfoot. | Restricted and painful subtalar inversion and eversion. Tenderness over the sinus tarsi. | X-ray: Joint space narrowing, osteophytes, or C-sign (coalition). CT: Definitive visualization of osseous coalition or arthritic changes. |
In this patient, the clinical presentation and imaging unequivocally point to a concomitant Posterior Ankle Impingement (secondary to an os trigonum) and FHL Tenosynovitis. The absence of neural symptoms rules out Tarsal Tunnel Syndrome, and the normal Achilles insertion rules out retrocalcaneal pathology.
Surgical Decision Making and Classification
Indications for Operative Intervention
The decision to proceed with surgical intervention in this case is driven by several compelling factors. First, the patient has failed an exhaustive, six-month course of conservative management, including physical therapy, NSAIDs, and a targeted, ultrasound-guided corticosteroid injection. In the context of stenosing tenosynovitis and mechanical osseous impingement, conservative measures often provide only temporary relief because they cannot alter the structural anatomy (the os trigonum) or the fibrotic stenosis of the FHL retinaculum.
Second, the patient is an elite, professional ballet dancer. The demands of her occupation require extreme, repetitive plantarflexion. The presence of a symptomatic os trigonum acts as a mechanical block to the necessary range of motion required for the "en pointe" position. Furthermore, the chronic triggering and tenosynovitis of the FHL severely compromise her ability to generate explosive push-off power for jumping (jetés).
Third, the MRI findings of significant bone marrow edema within the os trigonum and posterior talus indicate active, ongoing mechanical trauma. Prolonged conservative management in the presence of these findings risks further deterioration of the FHL tendon, potentially leading to longitudinal tearing or complete rupture, which would be career-ending.
Open Versus Endoscopic Approach
Historically, excision of an os trigonum and release of the FHL tendon was performed via an open posteromedial or posterolateral approach. While effective, open approaches are associated with significant morbidity, including a higher risk of wound healing complications, sural or tibial nerve injury, extensive scar tissue formation, and a prolonged rehabilitation timeline. In an elite athlete, the formation of dense postoperative scar tissue in the posterior ankle can be as debilitating as the original pathology.
The advent of hindfoot endoscopy, popularized by van Dijk, has revolutionized the management of posterior ankle pathology. The endoscopic approach utilizes two standard portals (posterolateral and posteromedial) positioned adjacent to the Achilles tendon. This technique offers several distinct advantages over open surgery
1. Superior Visualization The endoscope provides brilliant, magnified illumination of the deep posterior compartment, allowing for precise identification of the os trigonum, the FHL tendon, and the surrounding neurovascular structures.
2. Decreased Morbidity The minimally invasive nature of the portals significantly reduces soft tissue trauma, minimizing postoperative pain and wound complications.
3. Reduced Scarring Endoscopic resection minimizes the formation of posterior capsular and peritendinous scar tissue, preserving the delicate gliding mechanism of the FHL.
4. Accelerated Rehabilitation Patients can initiate early range of motion and weight-bearing, facilitating a faster return to high-level athletics.
Given this patient's profession and the need for a rapid, optimal functional recovery, a posterior endoscopic approach for excision of the os trigonum and FHL tenosynovectomy/release is the gold standard and the chosen surgical plan.
Surgical Technique and Intervention
Patient Positioning and Anesthesia
The patient was taken to the operating room and placed under general anesthesia with a supplemental regional popliteal sciatic nerve block for postoperative analgesia. She was positioned prone on a standard operating table. All bony prominences were meticulously padded. A well-padded thigh tourniquet was applied to the right lower extremity. The right foot and ankle were prepped and draped in the standard sterile fashion. The foot was allowed to hang freely over the edge of the operating table to allow for unrestricted, dynamic manipulation of the ankle and hallux during the procedure. The limb was exsanguinated with an Esmarch bandage, and the tourniquet was inflated to 250 mmHg.
Portal Placement and Approach
The success and safety of hindfoot endoscopy rely heavily on precise portal placement to avoid the sural nerve laterally and the tibial neurovascular bundle medially.
- Posterolateral Portal The posterolateral portal was established first. A vertical line was drawn parallel to the lateral border of the Achilles tendon. The portal site was marked at the level of the tip of the lateral malleolus, just anterior to the Achilles tendon. A superficial skin incision was made with a #11 blade. Subcutaneous tissues were bluntly spread with a mosquito hemostat, pointing anteriorly toward the fibula to avoid the sural nerve, which courses posterior to the fibula in this region. A 4.0 mm, 30-degree arthroscope was introduced with a blunt trocar.
- Posteromedial Portal The posteromedial portal was established under direct intra-articular visualization. A spinal needle was introduced just medial to the Achilles tendon, at the exact same horizontal level as the posterolateral portal. The needle was directed anteriorly and slightly laterally toward the arthroscope. Once the optimal trajectory was confirmed visually, a #11 blade was used to make a superficial skin incision. Blunt dissection with a hemostat was performed down to the shaft of the arthroscope. This strict adherence to blunt dissection and directing instruments toward the midline is critical to avoid injury to the medial calcaneal nerve and the tibial neurovascular bundle. A working cannula was then introduced.
Endoscopic Resection and Release
Step 1 Clearing Kager's Fat Pad
Initial visualization revealed the dense adipose tissue of Kager's fat pad obscuring the deep posterior structures. An aggressive 4.5 mm full-radius shaver was introduced through the posteromedial portal to resect the deep portion of Kager's fat pad. This debridement was carried down to the posterior aspect of the subtalar and tibiotalar joints.
Step 2 Identifying the FHL Tendon
The flexor hallucis longus tendon is the critical anatomical landmark in posterior ankle endoscopy; it serves as the "compass" for the procedure. The FHL was identified medially. Its identity was confirmed dynamically by having the assistant passively flex and extend the great toe, observing the excursion of the tendon. The FHL represents the medial limit of safe dissection; all dissection must remain lateral to the FHL to protect the tibial neurovascular bundle.
Step 3 Os Trigonum Excision
Once the FHL was identified, attention was turned laterally to the posterior process of the talus. The os trigonum was clearly visualized, bound by thick posterior capsular reflections and the posterior talofibular ligament (PTFL). The synchondrosis between the os trigonum and the talar body was identified. Using a combination of a radiofrequency wand and a shaver, the soft tissue attachments to the os trigonum were meticulously released. A small osteotome was introduced through the posteromedial portal and placed at the synchondrosis. Gentle malleting freed the ossicle from the talus. The os trigonum was then grasped with an endoscopic grasper and removed piecemeal through the enlarged posteromedial portal. The remaining posterior talar bed was smoothed with a motorized burr to ensure no residual impingement occurred during forced plantarflexion.
Step 4 FHL Retinaculum Release and Tenosynovectomy
Attention was returned to the FHL tendon. The tendon exhibited severe tenosynovitis, appearing hyperemic and thickened. The fibro-osseous tunnel (FHL retinaculum) was clearly stenotic. Using a retrograde knife, the FHL retinaculum was carefully released from proximal to distal. The release was carried out until the tendon could glide freely without any restriction. An extensive tenosynovectomy was then performed using the shaver, removing the inflammatory rind surrounding the tendon while preserving the tendon substance.
Step 5 Dynamic Intraoperative Assessment
With the os trigonum removed and the FHL released, dynamic testing was performed. The ankle was brought into maximal forced plantarflexion. Endoscopic visualization confirmed complete clearance of the posterior compartment with no residual osseous or soft tissue impingement between the tibia and calcaneus. The great toe was repeatedly flexed and extended; the FHL tendon demonstrated smooth, unrestricted excursion without triggering or catching.
Closure
The joint was thoroughly irrigated with sterile saline to remove all osseous debris. The arthroscope and instruments were removed. The portal sites were closed with simple interrupted 4-0 nylon sutures. A sterile, bulky compressive dressing was applied, and the patient was placed in a well-padded short leg controlled ankle motion (CAM) boot in a neutral position. The tourniquet was deflated, and the patient was awakened and transferred to the post-anesthesia care unit in stable condition.
Post Operative Protocol and Rehabilitation
The postoperative rehabilitation protocol for an elite ballet dancer following posterior ankle endoscopy must be meticulously phased. The goal is to balance tissue healing with the prevention of arthrofibrosis and FHL tethering, ultimately restoring the extreme ranges of motion and explosive strength required for performance.
Phase 1 Acute Healing (Weeks 0-2)
- Weight Bearing The patient is strictly non-weight-bearing (NWB) on the operative extremity, utilizing crutches.
- Immobilization The patient remains in the CAM boot at all times, except for hygiene and specific exercises.
- Range of Motion This is the most critical phase for preventing FHL tethering. The patient is instructed to perform active and passive hallux flexion and extension exercises 5-6 times per day. The FHL must glide through the surgical bed to prevent adhesions. Active ankle dorsiflexion and plantarflexion are initiated at day 3, strictly within a pain-free range.
- Wound Care Sutures are removed at the 2-week postoperative visit.
Phase 2 Early Rehabilitation (Weeks 2-6)
- Weight Bearing Transition to progressive partial weight-bearing (PWB) in the CAM boot, advancing to full weight-bearing (FWB) as tolerated by week 4. The boot is typically discontinued by week 4-5.
- Range of Motion Aggressive restoration of ankle dorsiflexion and plantarflexion. Manual therapy, including joint mobilizations (tibiotalar and subtalar) and soft tissue massage of the Achilles and posterior compartment, is initiated.
- Strengthening Introduction of isometric and early isotonic strengthening for the intrinsic foot musculature, ankle invertors/evertors, and plantarflexors. Towel scrunches and marble pickups are utilized for intrinsic strength.
- Proprioception Seated BAPS board and double-leg stance balance exercises.
Phase 3 Dance-Specific Progression (Weeks 6-12)
- Range of Motion Full, symmetric active and passive range of motion must be achieved by this phase.
- Strengthening Progression to closed-kinetic chain exercises. Eccentric loading of the Achilles and FHL complex. Single-leg heel raises are initiated and progressed.
- Ballet Integration The patient begins barre work. Initial focus is on flat-foot work and slow progressions into demi-plié and grand plié. Relevé is introduced cautiously, initially double-leg and progressing to single-leg. The transition to demi-pointe is heavily monitored for any recurrence of posterior pain.
- Cardiovascular Swimming and stationary cycling are encouraged.
Phase 4 Return to Performance (Months 3-6)
- Advanced Strengthening Explosive power development. Plyometric training (jumping and landing mechanics) is integrated.
- Pointe Work Once the patient demonstrates symmetric strength, full pain-free ROM, and excellent proprioception on demi-pointe, she is cleared to begin a graduated return to pointe work. This starts with short durations at the barre and slowly progresses to center work.
- Choreography Gradual integration into full company class and specific choreography. The timeline for full return to stage performance is highly variable but generally expected between 4 to 6 months postoperatively, depending on the dancer's strength and confidence.
Clinical Pearls and Pitfalls
Clinical Pearls
- The FHL is the Compass During posterior ankle endoscopy, the flexor hallucis longus tendon is the most critical anatomical landmark. Once identified, all dissection must remain lateral to the FHL. The tibial nerve and posterior tibial artery lie immediately medial to the FHL; respecting this boundary ensures their protection.
- Dynamic Intraoperative Testing Never conclude the procedure without performing a dynamic examination under direct endoscopic visualization. Forcefully plantarflex the ankle to ensure adequate bony resection of the os trigonum/talar process. Passively flex and extend the hallux to confirm complete release of the FHL retinaculum and smooth tendon excursion.
- Preoperative Ultrasound Utilizing dynamic ultrasound in the clinic is an invaluable adjunct to MRI. Visualizing the FHL triggering in real-time confirms the mechanical nature of the tenosynovitis and solidifies the surgical indication for retinacular release.
- Immediate Postoperative Hallux Motion Instructing the patient to begin active hallux motion in the recovery room is paramount. The posterior ankle is highly prone to scar formation. Early FHL excursion prevents the tendon from tethering to the raw bony bed of the resected os trigonum.
Surgical Pitfalls
- Sural Nerve Injury The sural nerve is at highest risk during the creation of the posterolateral portal. To mitigate this risk, the skin incision must be superficial, and deep dissection must be performed bluntly with a hemostat, directing the tips anteriorly toward the fibula and away from the nerve's expected course.
- Incomplete Resection Failing to remove the entire os trigonum or leaving a prominent posterior talar process will result in persistent impingement and surgical failure. The surgeon must meticulously clear the posterior capsular reflections to visualize the entire anatomy.
- Inadequate FHL Release The FHL retinaculum can be thick and extensive. A partial release will fail to resolve the stenosing tenosynovitis. The release must be carried far enough distally to ensure the nodular portion of the tendon can glide freely.
- Missing Concomitant Pathology Posterior impingement can occasionally mask other pathologies, such as an osteochondral lesion of the talus or subtle subtalar instability. A thorough preoperative clinical and radiographic evaluation is necessary to ensure all pain generators are addressed.
