Distal Chevron Osteotomy: A Masterclass in Hallux Valgus Correction
Key Takeaway
Join us in the OR for a detailed masterclass on the Distal Chevron Osteotomy. This guide provides an exhaustive, step-by-step breakdown of the procedure for hallux valgus correction, from essential preoperative planning and precise anatomical considerations to intraoperative execution with cannulated screw fixation. Learn critical pearls, avoid common pitfalls, and ensure excellent patient outcomes through meticulous surgical technique and comprehensive postoperative care.
Comprehensive Introduction and Patho-Epidemiology
The distal chevron osteotomy (DCO) represents a foundational pillar in the armamentarium of forefoot reconstructive surgery. Designed for the correction of mild to moderate hallux valgus, this procedure is far more than a simple osseous realignment; it is a sophisticated restoration of first ray biomechanics. Hallux valgus is a complex, progressive pathoanatomical deformity characterized by lateral deviation of the proximal phalanx, medial deviation of the first metatarsal, and a dynamic subluxation of the first metatarsophalangeal (MTP) joint. Our objective with the chevron osteotomy is to definitively address these multiplanar derangements, alleviate debilitating pain, and restore the propulsive kinematics of the forefoot.
Historically, the genesis of the distal metatarsal osteotomy can be traced back to Reverdin in 1881, who initially described a subcapital closing-wedge osteotomy. However, the modern iteration of the chevron osteotomy was definitively popularized by Austin and Leventen in 1981. Their original description championed a 60-degree V-shaped osteotomy that provided inherent multiplanar stability, theoretically obviating the need for internal fixation. As orthopedic understanding evolved and surgical techniques became more refined, surgeons such as Miller and Croce expanded the indications for this elegant procedure. Today, the contemporary DCO routinely incorporates rigid internal fixation and a meticulous lateral soft tissue release, allowing surgeons to reliably tackle moderate deformities with predictable, reproducible outcomes.
Epidemiologically, hallux valgus disproportionately affects the female population, with a widely accepted female-to-male ratio ranging from 2:1 to as high as 15:1 in operative cohorts. The etiology is multifactorial, representing a confluence of intrinsic genetic predispositions and extrinsic environmental factors. Intrinsic factors include ligamentous laxity, first ray hypermobility, pes planus, and specific metatarsal morphologies (such as a rounded metatarsal head). Extrinsic factors are dominated by constricting, narrow-toebox footwear and high heels, which force the hallux into a valgus position while simultaneously plantarflexing the first ray, thereby exacerbating the deforming forces of the extrinsic musculature.
Understanding the progressive nature of this deformity is paramount for the operating surgeon. Initially, the medial capsular structures attenuate, allowing the first metatarsal head to drift medially off the sesamoid apparatus. As the metatarsal head escapes medialward, the adductor hallucis and the lateral head of the flexor hallucis brevis (FHB) exert an unopposed lateral pull on the proximal phalanx. The extensor hallucis longus (EHL) and flexor hallucis longus (FHL) tendons subsequently bowstring laterally, transforming from stabilizing forces into primary deforming forces. The distal chevron osteotomy, when combined with appropriate soft tissue balancing, directly neutralizes this pathological cascade.
Detailed Surgical Anatomy and Biomechanics
Before initiating any surgical intervention, an exhaustive, three-dimensional understanding of the first ray anatomy is non-negotiable. The first MTP joint is an intricate diarthrodial joint, heavily reliant on its capsuloligamentous and sesamoid complexes for stability during the terminal stance phase of the gait cycle. The osseous architecture consists of the convex first metatarsal head articulating with the concave base of the proximal phalanx. The plantar aspect of the metatarsal head features two distinct, cartilage-covered longitudinal grooves separated by a central crista; these grooves serve as the articulation pathways for the medial (tibial) and lateral (fibular) sesamoids.
Osteology and Articulations
The sesamoids are not merely accessory bones; they are vital biomechanical fulcrums embedded within the tendons of the flexor hallucis brevis. Distally, they are tethered to the base of the proximal phalanx via the thick, fibrous plantar plate. Proximally, they accept the insertion of the FHB. Medially and laterally, they are suspended by the metatarso-sesamoid and sesamophalangeal ligaments. During the progression of hallux valgus, the sesamoids do not actively subluxate laterally; rather, the first metatarsal head drifts medially off the sesamoid apparatus. The crista often erodes over time due to abnormal friction, leading to intractable pain and further mechanical instability.
Ligamentous Structures and Musculature
The ligamentous and muscular anatomy dictates the deforming vectors in hallux valgus. The medial collateral ligament becomes attenuated and redundant, while the lateral collateral ligament, the deep transverse metatarsal ligament (DTML), and the adductor hallucis tendon become severely contracted. The adductor hallucis, comprising both oblique and transverse heads, inserts onto the lateral base of the proximal phalanx and the fibular sesamoid. Its release is frequently necessary to achieve a congruent MTP joint. Furthermore, the EHL and FHL tendons, which normally run centrally over the joint, bowstring laterally into the first web space, creating a vicious cycle that exacerbates the valgus drift of the hallux with every step.
Neurovascular Anatomy
The neurovascular anatomy of the first ray dictates our surgical approaches and warns against aggressive dissection. The dorsomedial digital nerve, a terminal branch of the superficial peroneal nerve, courses superficially along the medial aspect of the MTP joint and is highly vulnerable during the medial capsulotomy. The blood supply to the first metatarsal head is of paramount concern, as avascular necrosis (AVN) is a devastating complication. The primary arterial supply is derived from the first plantar metatarsal artery (a branch of the deep plantar arch), which enters the metatarsal head via a dense capsular plexus at the plantar-lateral and plantar-medial reflections. The first dorsal metatarsal artery provides supplementary flow.
Surgical Warning: The intracapsular arterial ring is heavily concentrated on the plantar aspect of the metatarsal neck. Aggressive plantar dissection, excessive lateral capsular stripping, or the use of high-heat power saws without adequate irrigation can obliterate this fragile vascular network, precipitating osteonecrosis of the capital fragment.
Exhaustive Indications and Contraindications
Patient selection is the ultimate determinant of success in forefoot reconstruction. The distal chevron osteotomy is not a panacea for all bunion deformities; its application must be strictly guided by clinical examination and precise radiographic parameters. The ideal candidate is a patient with symptomatic, painful hallux valgus that has failed conservative management (e.g., shoe modification, orthotics, NSAIDs), presenting with a mild to moderate deformity and a congruent or reducible MTP joint.
Radiographically, the DCO is indicated for a Hallux Valgus Angle (HVA) of less than 30 to 35 degrees and an Intermetatarsal Angle (IMA) of less than 15 to 16 degrees. The Distal Metatarsal Articular Angle (DMAA) must also be scrutinized. A normal DMAA is less than 10 degrees. If the DMAA is abnormally elevated (pathologic), a standard translational chevron will fail to correct the articular orientation, leading to early recurrence. In such cases, a biplanar or "reverdin-chevron" modification—incorporating a medial closing wedge into the chevron cut—is required to derotate the articular cartilage.
Contraindications must be respected to avoid catastrophic failures. Severe deformities (IMA > 16 degrees, HVA > 40 degrees) typically lack sufficient metatarsal width to allow for adequate lateral translation of the capital fragment without compromising bone-to-bone contact. First ray hypermobility, often assessed via the modified Silfverskiöld test or dynamic radiographic evaluation, is a relative contraindication; performing a distal osteotomy in the presence of severe hypermobility often leads to recurrence, making a proximal arthrodesis (Lapidus procedure) the superior choice.
| Parameter | Indications for Distal Chevron Osteotomy | Absolute Contraindications | Relative Contraindications |
|---|---|---|---|
| Hallux Valgus Angle (HVA) | 15° to 35° | > 40° (Severe Deformity) | 35° to 40° (Borderline) |
| Intermetatarsal Angle (IMA) | 10° to 15° | > 16° to 20° | Narrow 1st Metatarsal Shaft |
| MTP Joint Status | Congruent or Reducible Subluxation | Severe Osteoarthrosis (Rigidus) | Mild to Moderate Osteophytes |
| First Ray Mobility | Stable 1st Tarsometatarsal Joint | Gross Clinical Hypermobility | Mild TMT Laxity |
| Vascular Status | Intact pedal pulses, normal ABI | Peripheral Arterial Disease (PAD) | Heavy Smoker (Poor healing) |
| Neurological Status | Intact protective sensation | Charcot Neuroarthropathy | Mild Peripheral Neuropathy |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preoperative planning bridges the gap between clinical diagnosis and surgical execution. The physical examination must document the exact location of pain (e.g., medial eminence bursitis, sesamoiditis, transfer metatarsalgia), the reducible nature of the deformity, and the presence of any lesser toe deformities (such as hammertoes or crossover toes) that may require concurrent correction. Range of motion of the first MTP joint must be assessed; crepitus or severely restricted dorsiflexion suggests underlying hallux rigidus, which may necessitate an arthrodesis rather than a joint-sparing osteotomy.
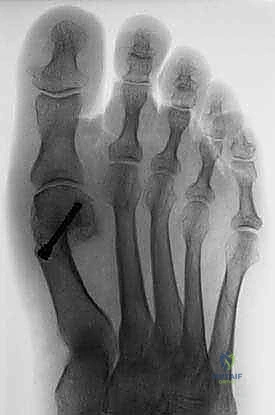
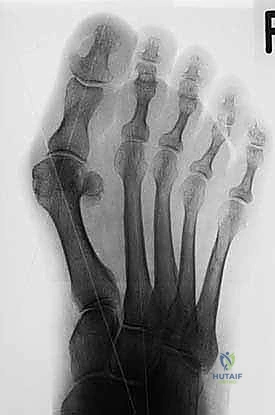
Standard weight-bearing radiographs are the cornerstone of preoperative templating. Anteroposterior (AP), lateral, and oblique views of the foot must be obtained. The AP view is utilized to measure the HVA, IMA, and DMAA, and to assess joint congruency. A sesamoid axial view is highly recommended to evaluate the degree of sesamoid subluxation and the integrity of the crista. Templating involves drawing the planned 60-degree osteotomy apex exactly in the center of the metatarsal head, anticipating a lateral translation of 4 to 6 millimeters (up to a maximum of 50% of the metatarsal shaft width).
The patient is positioned supine on the operating table with the foot positioned at the edge of the bed to allow unrestricted access to both the medial and lateral aspects of the forefoot. A bump may be placed under the ipsilateral hip to correct external rotation of the leg, ensuring the foot rests in a neutral position. A well-padded pneumatic calf or ankle tourniquet is applied to provide a bloodless surgical field, which is critical for identifying delicate neurovascular structures and assessing the adequacy of the soft tissue releases.
Anesthesia typically consists of monitored anesthesia care (MAC) supplemented by a comprehensive regional block. An ankle block, targeting the tibial, deep peroneal, superficial peroneal, saphenous, and sural nerves, provides excellent intraoperative anesthesia and prolonged postoperative analgesia. Intraoperative fluoroscopy (C-arm) must be readily available and draped into the sterile field to confirm osteotomy placement, capital fragment translation, and precise hardware positioning.
Step-by-Step Surgical Approach and Fixation Technique
The surgical execution of the distal chevron osteotomy is divided into five distinct phases: the lateral soft tissue release, the medial approach and exostectomy, the osteotomy itself, fragment translation and fixation, and finally, capsulorrhaphy.
Phase 1: Lateral Soft Tissue Release
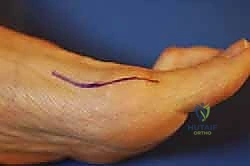
Addressing the contracted lateral structures is paramount for achieving a tension-free correction. We begin with a dorsal longitudinal incision over the first web space, approximately 3 cm in length.
Blunt dissection is utilized to protect the terminal branches of the deep peroneal nerve. A lamina spreader is placed between the first and second metatarsal heads to place the deep transverse metatarsal ligament (DTML) under tension.
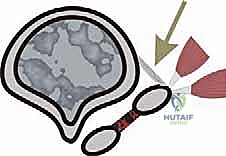
Using a #15 blade, the DTML is carefully transected. The adductor hallucis tendon is identified at its insertion on the fibular sesamoid and the base of the proximal phalanx; a tenotomy is performed if the deformity is rigid.
The lateral capsule is then fenestrated or released vertically to mobilize the fibular sesamoid. A varus stress is applied to the hallux to confirm adequate release; the toe should easily passively correct to 15-20 degrees of varus.
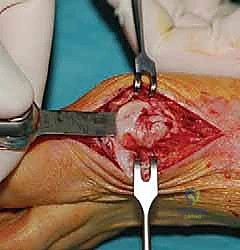
Phase 2: Medial Approach and Exostectomy
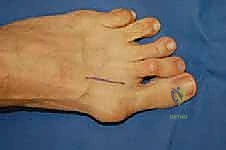
Attention is then directed to the medial aspect of the first MTP joint. A midline medial longitudinal incision is made, extending from the mid-shaft of the first metatarsal to the mid-shaft of the proximal phalanx.
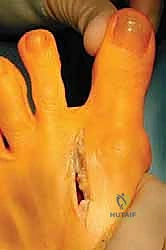
Careful subcutaneous dissection protects the dorsomedial digital nerve. An inverted L-shaped or longitudinal capsulotomy is performed, raising a full-thickness capsuloperiosteal flap to expose the medial eminence.
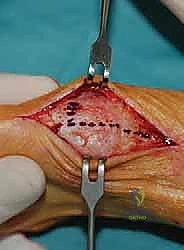
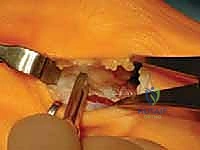
The medial eminence (bunion) is resected using a sagittal saw. It is critical to start the cut 1-2 mm medial to the sagittal sulcus to avoid violating the articular surface and to preserve the tibial sesamoid articulation.

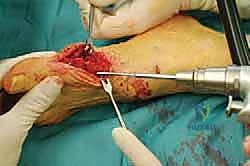
Phase 3: The Chevron Osteotomy
The apex of the osteotomy is marked with a 0.045-inch Kirschner wire, positioned exactly in the center of the metatarsal head, approximately 1 cm proximal to the articular cartilage.
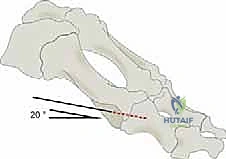
Using a micro-sagittal saw, a 60-degree V-shaped osteotomy is created. The dorsal arm exits dorsally, while the plantar arm must be kept parallel to the plantar aspect of the foot, exiting proximal to the sesamoid apparatus to avoid damaging the sesamoid articulation or the critical plantar blood supply.
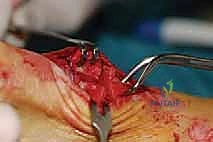
Copious cold saline irrigation is mandatory during sawing to prevent thermal necrosis of the bone.
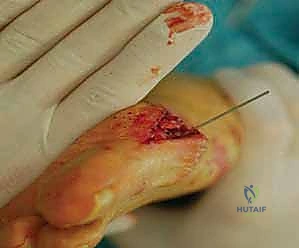
Phase 4: Translation and Fixation
Once the osteotomy is complete, the capital fragment is translated laterally. A small periosteal elevator or towel clip is used to gently shift the head laterally by 4 to 6 mm, depending on the preoperative templating (up to 50% of the shaft width).
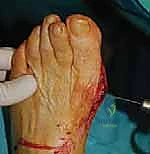
The fragment is then impacted proximally to ensure bone-to-bone apposition and inherent stability.
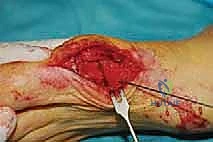
A 0.045-inch K-wire is driven obliquely from dorsal-proximal to plantar-distal to provisionally hold the osteotomy.
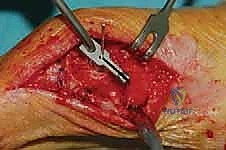
Fluoroscopy confirms the translation, restoration of the IMA, and sesamoid reduction.
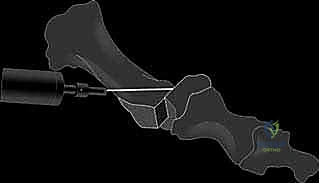
Definitive fixation is achieved utilizing a single headless compression screw or a standard cortical screw.
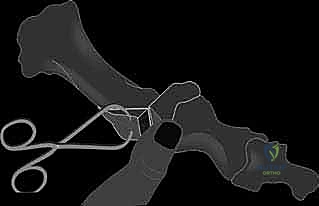
The screw is placed over the guidewire, ensuring the threads cross the osteotomy site to provide rigid interfragmentary compression.
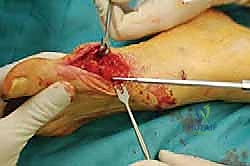
Following rigid fixation, the prominent medial overhang of the proximal metatarsal shaft is resected flush with the translated metatarsal head using the sagittal saw.
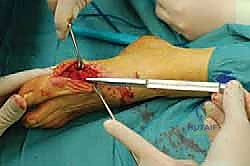
Phase 5: Capsulorrhaphy and Closure
The final, yet crucial, step is the medial capsulorrhaphy. The medial capsule is imbricated (tightened) to hold the hallux in a neutral, rectus position.
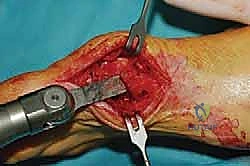
Excess capsular tissue is excised, and the capsule is closed using 2-0 or 3-0 absorbable sutures (e.g., Vicryl) in a pant-over-vest fashion.
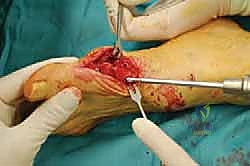
Care must be taken not to over-tighten the medial capsule, which can precipitate a devastating iatrogenic hallux varus.
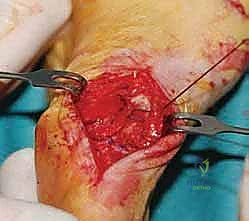
The skin is closed meticulously with 4-0 non-absorbable monofilament or subcuticular absorbable sutures. A sterile, compressive forefoot dressing is applied, utilizing a toe spica technique to splint the hallux in its newly corrected alignment.

Complications, Incidence Rates, and Salvage Management
While the distal chevron osteotomy is highly successful, it is not immune to complications. A profound understanding of potential pitfalls is essential for the operating surgeon. The most feared complication is avascular necrosis (AVN) of the first metatarsal head. Historically, incidence rates were reported as high as 20% in early non-fixated series, but modern techniques utilizing meticulous dissection and rigid fixation have reduced the incidence of clinically symptomatic AVN to less than 2-5%. AVN occurs due to disruption of the intraosseous and extraosseous blood supply, particularly the plantar metaphyseal arteries.
Recurrence of the hallux valgus deformity is another significant concern, typically occurring in 10-15% of cases. Recurrence is most commonly attributed to poor patient selection (e.g., operating on an unrecognized hypermobile first ray or an IMA > 16 degrees), inadequate lateral soft tissue release, or failure to address an elevated DMAA. Conversely, overzealous lateral release combined with aggressive medial capsular plication can result in iatrogenic hallux varus, a complication that is notoriously difficult to treat and deeply dissatisfying for the patient.
Nonunion and malunion are relatively rare (less than 2%) due to the large cancellous surface area of the metatarsal head and the inherent stability of the V-cut. However, technical errors, such as translating the capital fragment greater than 50% of the shaft width, can compromise bone-to-bone contact and lead to delayed union or hardware failure. Hardware irritation from the screw head may necessitate removal in approximately 5% of patients once clinical and radiographic union is achieved.
| Complication | Estimated Incidence | Prevention Strategy | Salvage Management |
|---|---|---|---|
| Avascular Necrosis (AVN) | < 5% (Symptomatic) | Avoid aggressive plantar dissection; use sharp saw blades with copious irrigation. | Conservative (offloading); late stage requires MTP Arthrodesis. |
| Recurrence of Deformity | 10% - 15% | Strict adherence to indications (IMA < 16°); thorough lateral release; address DMAA. | Revision osteotomy (Scarf/Lapidus) or MTP Arthrodesis. |
| Iatrogenic Hallux Varus | 2% - 5% | Avoid complete fibular sesamoidectomy; do not over-imbricate medial capsule. | Extensor hallucis brevis (EHB) transfer; reverse osteotomy; Arthrodesis. |
| Nonunion / Delayed Union | < 2% | Ensure < 50% translation; rigid internal fixation; strict post-op weight-bearing protocols. | Bone grafting and revision internal fixation. |
| Hardware Irritation | 5% - 10% | Countersink screw heads; use headless compression screws. | Hardware removal after radiographic union (typically > 3-6 months). |
Phased Post-Operative Rehabilitation Protocols
The success of the distal chevron osteotomy relies heavily on patient compliance with a structured, phased rehabilitation protocol. The immediate postoperative goal is the protection of the osteotomy site and the delicate soft tissue repairs, while simultaneously preventing debilitating MTP joint stiffness.
Phase 1: Maximum Protection (Weeks 0-2)
Immediately following surgery, the patient is placed in a rigid-soled postoperative shoe or a controlled ankle motion (CAM) boot. Weight-bearing is strictly limited to heel-touch or flat-foot weight-bearing; the patient is explicitly instructed to avoid rolling through the forefoot or pushing off the great toe. Elevation and cryotherapy are paramount to control edema, which can be significant in forefoot surgery. The initial surgical dressing, which acts as a soft tissue splint holding the hallux in rectus, remains intact until the first postoperative visit at 10-14 days.
Phase 2: Progressive Mobilization (Weeks 2-6)
At the two-week mark, sutures are removed. Radiographs are obtained to verify the maintenance of hardware position and osteotomy alignment. The patient remains in the rigid postoperative shoe but is instructed to begin active and gentle passive range of motion (ROM) exercises of the first MTP joint. Emphasizing plantarflexion is critical to prevent dorsal capsular contracture. A toe spacer may be utilized between the first and second toes to maintain the corrected alignment. Edema control via compression stockings is highly recommended.
Phase 3: Return to Function (Weeks 6-12+)
By week six, clinical and radiographic signs of bone bridging should be evident. The patient is transitioned into a wide-toebox, supportive athletic shoe. Normal heel-to-toe gait mechanics are progressively reintroduced. Physical therapy may be prescribed if MTP joint stiffness persists or if gait abnormalities are noted. High-impact activities, running, and the use of narrow or high-heeled footwear are strictly prohibited until at least 12 weeks postoperatively, and only after complete radiographic consolidation is confirmed.
Summary of Landmark Literature and Clinical Guidelines
The evolution and validation of the distal chevron osteotomy are deeply rooted in orthopedic literature. The seminal paper by Austin and Leventen (1981) remains the cornerstone text, originally reporting excellent outcomes in over 1,000 feet utilizing a non-fixated 60-degree osteotomy. Their work established the geometric stability of the V-cut, which resists dorsal displacement under weight-bearing loads.
Further refinement of the technique was documented by Meier and Kenzora in their critical analysis of the vascular anatomy of the first metatarsal head. Their cadaveric studies highlighted the profound risk of avascular necrosis associated with extensive lateral soft tissue stripping combined with a distal osteotomy, leading to the modern paradigm of performing the lateral release via a separate dorsal first web space incision rather than trans-articularly.
Long-term efficacy has been thoroughly validated. Trnka et al. published a landmark long-term follow-up study demonstrating that the clinical and radiographic corrections achieved with a fixated distal chevron osteotomy are maintained at 5 to 10 years postoperatively, provided the initial indications were strictly observed. Current clinical guidelines from the American Orthopaedic Foot & Ankle Society (AOFAS) strongly support the fixated DCO with lateral release as a gold-standard intervention for mild to moderate hallux valgus, noting its superior outcomes in terms of pain relief, joint mobility preservation, and patient satisfaction when compared to conservative measures or more aggressive proximal osteotomies in appropriately selected patients.
