Comprehensive Management of Rheumatoid Thumb Deformities: Pathomechanics and Surgical Reconstruction
Key Takeaway
Rheumatoid thumb deformities present complex biomechanical challenges requiring precise surgical intervention. The Nalebuff classification categorizes these into four distinct types, with Type I (boutonnière) and Type III (swan-neck) being the most prevalent. Management depends on joint mobility and articular cartilage integrity, ranging from synovectomy and tendon reconstruction to arthrodesis. This guide details the pathomechanics, clinical evaluation, and step-by-step surgical techniques, including interphalangeal joint arthrodesis, to restore functional pinch and grip kinematics.
INTRODUCTION TO RHEUMATOID THUMB DEFORMITIES
Rheumatoid arthritis (RA) is a systemic inflammatory disease that profoundly alters the biomechanics of the hand and wrist. Because the thumb is responsible for approximately 40% to 50% of overall hand function—facilitating key pinch, tip-to-tip pinch, and power grasp—deformities in this digit result in disproportionate functional impairment. Rheumatoid thumb deformities frequently are complex and can involve the joints individually or in combination. The pathogenesis is driven by synovial proliferation (pannus) that distends joint capsules, attenuates collateral ligaments, and destroys articular cartilage, ultimately altering the moment arms of the crossing tendons.
To systematically approach these complex biomechanical failures, the classification of rheumatoid thumb deformities proposed by Nalebuff is universally utilized. This system is highly helpful in understanding the underlying pathomechanical problems and developing a stage-specific plan for surgical treatment.
PATHOMECHANICS AND THE NALEBUFF CLASSIFICATION
Nalebuff originally described four primary types of rheumatoid thumb deformities based on the initiating joint of synovial disease and the subsequent cascade of tendon imbalances. Understanding the primary epicenter of the disease is critical, as surgical correction must address the primary deforming force to prevent recurrence.
Type I: Boutonnière Deformity
Type I is the most common rheumatoid thumb deformity. It is characterized by metacarpophalangeal (MCP) joint flexion and interphalangeal (IP) joint hyperextension.
The deformity results from primary synovitis that begins at the MCP joint. The proliferating pannus bulges dorsally to stretch the joint capsule and the extensor hood. This leads to the attenuation of the extensor pollicis brevis (EPB) insertion at the base of the proximal phalanx. As the dorsal support fails, the extensor pollicis longus (EPL) tendon subluxates ulnarly and volarly, dropping below the axis of rotation of the MCP joint. Consequently, the EPL paradoxically becomes an MCP joint flexor while maintaining its extension force on the IP joint. The intrinsic muscles (abductor pollicis brevis and flexor pollicis brevis) gain a mechanical advantage, further driving the proximal phalanx into fixed flexion.
Type II: Combined Deformity
Type II deformity is rare and represents a hybrid of Type I and Type III pathomechanics. It includes MCP joint flexion and IP joint hyperextension (identical to Type I), but is complicated by concurrent trapeziometacarpal (CMC) joint subluxation or dislocation. The presence of CMC joint disease necessitates a more comprehensive surgical approach, often requiring CMC arthroplasty combined with MCP joint stabilization.
Type III: Swan-Neck Deformity
Type III is the second most common rheumatoid thumb deformity. It presents as CMC joint subluxation, MCP joint hyperextension, and IP joint flexion.
Unlike Type I, the primary epicenter of disease in Type III is the CMC joint. Synovitis at the CMC joint leads to dorsal and radial subluxation of the metacarpal base. As the metacarpal subluxates, it drifts into a fixed adduction contracture. To compensate for the narrowed first web space and to allow the patient to grasp large objects, the MCP joint is forced into hyperextension. Over time, the volar plate of the MCP joint attenuates. The hyperextended posture of the MCP joint increases tension on the flexor pollicis longus (FPL), which subsequently pulls the IP joint into flexion.
Clinical Pearl: In a Type III deformity, the MCP joint hyperextension is purely compensatory in the early stages. However, if the adduction contracture of the first web space is not released during CMC arthroplasty, the MCP joint will inevitably return to a hyperextended posture, leading to surgical failure.
Type IV: Gamekeeper’s Deformity
Type IV is unusual and results from primary ulnar collateral ligament (UCL) laxity at the MCP joint. Synovitis specifically attenuates the UCL, leading to abduction of the proximal phalanx and compensatory adduction of the first metacarpal. This mimics a chronic Gamekeeper's or Skier's thumb but is driven by inflammatory capsuloligamentous destruction rather than acute trauma.
PREOPERATIVE EVALUATION AND SURGICAL INDICATIONS
Surgical intervention is indicated when conservative measures (splinting, corticosteroid injections, disease-modifying antirheumatic drugs [DMARDs]) fail to control pain or when progressive deformity threatens hand function.
Evaluation must assess:
1. Joint Mobility: Is the deformity passively correctable or fixed?
2. Articular Cartilage: Are there radiographic signs of joint space narrowing, erosions, or subluxation?
3. Tendon Integrity: Is the EPL intact, or has it ruptured (a common complication at Lister's tubercle)?
4. Adjacent Joints: The wrist and adjacent fingers must be evaluated, as proximal instability can compromise distal reconstruction.
SURGICAL MANAGEMENT STRATEGIES
Management of Type I Deformities
- Early Stage (Correctable, preserved cartilage): Synovectomy of the MCP joint, rerouting of the EPL tendon dorsally, and shortening/reconstruction of the EPB (Harrison-Ansell procedure).
- Late Stage (Fixed deformity, destroyed cartilage): MCP joint arthrodesis is the gold standard. It provides a stable, pain-free post for pinch. The IP joint may require a volar release or concurrent arthrodesis if fixed in hyperextension.
Management of Type III Deformities
- Early Stage: CMC joint arthroplasty (e.g., ligament reconstruction and tendon interposition [LRTI] or hematoma distraction arthroplasty) combined with first web space release. The MCP joint may require volar capsulodesis or EPB transfer to prevent recurrent hyperextension.
- Late Stage: CMC arthroplasty combined with MCP joint arthrodesis.
Surgical Warning: Never fuse both the CMC and MCP joints of the thumb. At least one of these joints must remain mobile to allow for spatial positioning of the thumb during opposition.
SURGICAL TECHNIQUE: INTERPHALANGEAL AND DISTAL INTERPHALANGEAL JOINT ARTHRODESIS
Arthrodesis of the interphalangeal (IP) joint of the thumb, or the distal interphalangeal (DIP) joints of the fingers, is a highly reliable procedure for fixed, painful rheumatoid deformities. While the thumb has only one IP joint, the surgical principles, approaches, and fixation techniques are identical to those used for finger DIP joints, which are frequently addressed concurrently in the rheumatoid patient.
1. Patient Positioning and Preparation
The patient is positioned supine with the arm extended on a radiolucent hand table. A regional axillary or supraclavicular block is preferred, supplemented with a pneumatic arm tourniquet elevated to 250 mm Hg. Prophylactic intravenous antibiotics are administered prior to tourniquet inflation.
2. Surgical Approach and Incision
Exposure of the IP or DIP joint must provide adequate visualization while preserving the delicate dorsal skin flaps, which are particularly fragile in rheumatoid patients on chronic corticosteroids.
Several incisions can be utilized, including a dorsal transverse, Y-shaped, or H-shaped (step-cut) incision. The step-cut incision provides excellent exposure of the extensor mechanism and joint surfaces while minimizing the risk of longitudinal scar contracture.
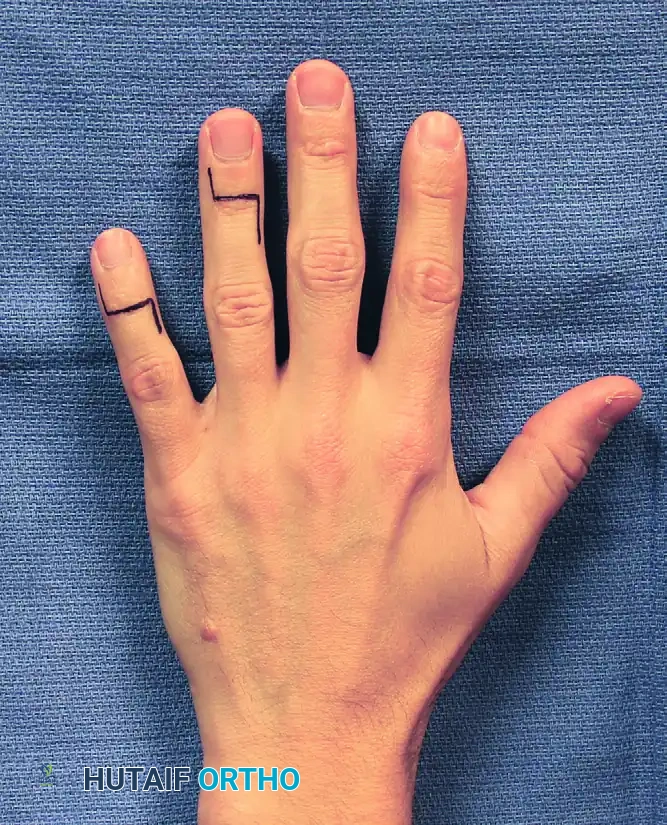
FIGURE 73-32: Incision for distal interphalangeal joint arthrodesis. Note the step-cut (H-shaped) design utilized to maximize exposure while protecting dorsal skin flap vascularity.
3. Joint Preparation
- Elevate the dorsal skin flaps meticulously, preserving the subdermal venous plexus.
- Incise the extensor tendon transversely or split it longitudinally to expose the joint capsule.
- Perform a thorough synovectomy.
- Release the collateral ligaments completely to allow the joint to be "shotgunned" (hinged open volarly), providing circumferential access to the articular surfaces.
- Using a microsaw or rongeur, resect the remaining articular cartilage down to bleeding subchondral bone.
- Technique Variation: Flat cuts can be made to shorten the digit and correct severe angulation, or a cup-and-cone reamer system can be used to preserve length and allow for fine-tuning of the fusion angle.
- For the thumb IP joint, the ideal position of fusion is 10 to 15 degrees of flexion. For finger DIP joints, fusion is typically set at 0 to 10 degrees of flexion (increasing slightly from the index to the small finger).
4. Internal Fixation
Rigid internal fixation is paramount for achieving high union rates.
* Headless Compression Screws: Currently the gold standard. A guidewire is driven antegrade through the distal phalanx, exiting the tip of the finger. The joint is reduced in the desired position, and the wire is driven retrograde into the proximal/middle phalanx. The screw is then advanced over the wire, burying the head beneath the distal phalangeal cortex to prevent nail bed irritation.
* Crossed K-wires or Tension Band: An alternative if bone stock is extremely poor or the medullary canal is too narrow for a screw.
5. Closure Techniques
Meticulous closure is required to prevent extensor lag and wound breakdown.
* Close the extensor tendon with an absorbable suture, or use a continuous pull-out suture (“roll stitch”) of nonabsorbable material.
* Close the skin with interrupted 5-0 or 6-0 nonabsorbable nylon sutures.
* Apply a sterile, non-adherent dressing and a splint, usually a dorsal splint to block extension and protect the repair.
POSTOPERATIVE CARE AND REHABILITATION
The postoperative protocol must balance the need for rigid immobilization of the arthrodesis site with the necessity of early mobilization for adjacent, non-fused joints to prevent stiffness—a critical concern in the rheumatoid hand.
- Initial Immobilization: The initial bulky dressing and dorsal splint are maintained for the first few days to control edema.
- Splint Removal and Mobilization: The splint is removed in 3 to 5 days, and active motion exercises are begun for mobile joints (e.g., the MCP and CMC joints, provided they were not surgically addressed).
- Suture Management: Skin sutures are removed in 7 to 10 days, once the wound edges are sealed and edema has subsided.
- Long-term Splinting: Additional splinting is not needed for compliant patients if rigid internal fixation (such as a headless compression screw) was achieved. If K-wires were used, a custom thermoplastic splint may be worn for 4 to 6 weeks.
- Hardware Management: Internal fixation usually is not removed unless it becomes symptomatic (e.g., a prominent screw head at the distal tuft or K-wire tract infection).
- Radiographic Follow-up: Serial radiographs are obtained at 4, 8, and 12 weeks until healing is ascertained. It is important to counsel the patient that while clinical stability may be achieved early, it may be several months before solid bone union is apparent radiographically.
COMPLICATIONS AND SALVAGE PROCEDURES
Despite meticulous technique, complications can arise, particularly in the immunocompromised rheumatoid population.
* Nonunion: Occurs in 5% to 10% of IP/DIP arthrodeses. Asymptomatic nonunions (fibrous unions) require no treatment if stable. Symptomatic nonunions require revision with bone grafting (often utilizing distal radius autograft) and upgraded fixation.
* Infection: Superficial infections are managed with oral antibiotics. Deep infections necessitate hardware removal, aggressive debridement, and temporary stabilization with external fixation or antibiotic spacers until the infection clears.
* Hardware Prominence: Screw back-out or prominent K-wires can cause skin irritation or nail bed deformities. Symptomatic hardware should be removed only after solid radiographic union is confirmed.
By adhering to the biomechanical principles outlined in the Nalebuff classification and executing precise surgical techniques, the orthopaedic surgeon can reliably restore stability, relieve pain, and significantly improve the quality of life for patients suffering from severe rheumatoid thumb deformities.
You Might Also Like
