Geriatric Complex Acetabular Fractures: A Detailed Clinical Case Study
Key Takeaway
Geriatric complex acetabular fractures, frequently from low-energy falls in osteoporotic patients, require meticulous diagnosis. This involves a thorough clinical exam followed by advanced imaging like CT with 3D reconstructions. Imaging delineates comminution, articular impaction, and column involvement, which are crucial for effective treatment planning in this challenging patient population.
Patient Presentation and History
Mechanism of Injury and Demographics
A 78-year-old female presents to the emergency department following a ground-level fall at home. The mechanism of injury involved tripping on a rug and landing directly onto her left lateral hip. She immediately experienced severe left hip pain and was unable to bear weight or mobilize her left lower extremity. She reports no loss of consciousness, head injury, or other acute injuries. This presentation is a classic representation of a fragility fracture, where low-energy trauma imparts sufficient force to compromise osteoporotic bone, a scenario increasingly prevalent in the aging population.
Medical Comorbidities and Physiological Status
Her medical history is highly relevant to both her fracture pattern and the subsequent surgical decision-making process. The patient has a documented history of osteoporosis, diagnosed five years prior, which has been managed with weekly Alendronate. This prolonged bisphosphonate use necessitates a careful evaluation of bone morphology to rule out atypical femoral fractures, although her primary injury is localized to the acetabulum.
She has a history of hypertension, which remains well-controlled on Lisinopril, and Type 2 Diabetes Mellitus, managed with Metformin, with a recently recorded HbA1c of 7.1%. The diabetic status is a critical factor regarding postoperative infection risk, wound healing, and microvascular integrity. Furthermore, she has a diagnosis of Atrial Fibrillation and is currently on Apixaban for anticoagulation. The presence of a direct oral anticoagulant (DOAC) in the setting of acute pelvic trauma introduces immediate challenges regarding hemorrhage control, timing of surgical intervention, and the potential need for reversal agents such as Andexanet alfa or prothrombin complex concentrate (PCC) depending on the timing of her last dose and renal function.
Baseline Functional Status and Cognitive Assessment
The patient exhibits mild cognitive impairment, managed primarily by her family. Despite this, she is generally independent with activities of daily living (ADLs). Her pre-injury functional baseline involved ambulation with a single-point cane, and she was capable of managing stairs and engaging in short-distance community ambulation. She resides with her daughter, which provides a reliable postoperative support system. Her history includes one previous fall in the past year that resulted in a distal radius fracture, further underscoring her high risk for recurrent fragility fractures and the systemic nature of her compromised bone mineral density.
Upon arrival in the trauma bay, the patient is alert, oriented to person and place, but visibly distressed secondary to acute pain. Vital signs remain hemodynamically stable, with a blood pressure of 135/85 mmHg, a heart rate of 88 beats per minute (irregularly irregular consistent with her atrial fibrillation), and normal oxygen saturation on room air. She is entirely unable to stand or ambulate.
Clinical Examination Findings
Inspection and Soft Tissue Assessment
Initial inspection of the left lower extremity reveals slight external rotation and apparent shortening compared to the contralateral right limb. This posturing is highly suggestive of a loss of structural integrity of the hip joint, likely secondary to medial migration of the femoral head through a fractured quadrilateral plate or an associated hip dislocation. There is moderate, progressive swelling localized over the left greater trochanter and the lateral aspect of the thigh.
A meticulous assessment of the soft tissue envelope is paramount. Acutely, there are no obvious ecchymoses, abrasions, or open wounds. The skin remains intact; however, the mechanism of a direct lateral blow necessitates high clinical suspicion for a developing Morel-Lavallée lesion. The subcutaneous tissues are palpated for fluctuance or a characteristic shear-injury fluid wave, which are currently absent but require serial monitoring.
Palpation and Structural Integrity
Palpation elicits severe, localized tenderness over the left greater trochanter, the lateral iliac crest, and the superior pubic ramus. Gentle internal and external rotation of the left lower extremity produces palpable and audible crepitus within the hip joint, confirming articular incongruity and osseous disruption. Distal palpation of the left femur, patella, and proximal tibia reveals no secondary areas of tenderness, effectively ruling out contiguous ipsilateral fractures. A gentle assessment of pelvic ring stability utilizing anterior-posterior and lateral compression forces reveals no overt rotational or vertical instability, suggesting the injury is primarily confined to the acetabulum rather than a catastrophic pelvic ring disruption.
Range of Motion and Provocative Testing
Active range of motion of the left hip is completely abolished secondary to severe pain and mechanical instability. Passive range of motion is exquisitely painful and strictly guarded by the patient. Only a few degrees of passive flexion and external rotation are achievable before profound muscle spasms of the iliopsoas, rectus femoris, and adductor complex halt any further excursion. Any attempt at passive internal rotation exacerbates the pain exponentially, a finding consistent with anterior column or quadrilateral surface displacement. The patient is entirely unable to perform an active straight leg raise, indicating a loss of the fulcrum effect of the hip joint and profound inhibition of the hip flexor mechanism. The contralateral right hip demonstrates full, pain-free active and passive range of motion.
Neurological and Vascular Assessment
A comprehensive neurovascular examination is critical, particularly given the proximity of the sciatic nerve to the posterior column and the femoral nerve to the anterior column.
* Motor Function: Gross motor strength in the right lower extremity is 5/5 across all myotomes. In the affected left lower extremity, the patient cannot lift the leg against gravity. However, isolated testing reveals flicker strength and voluntary contraction in the quadriceps (L3-L4), tibialis anterior (L4-L5), extensor hallucis longus (L5), and gastrocnemius-soleus complex (S1). While formalized strength grading is limited by pain inhibition, there is no evidence of gross foot drop or complete sciatic nerve palsy.
* Sensory Function: Sensation to light touch and pinprick is intact and symmetric across the bilateral L2 through S1 dermatomes. Proprioception at the great toe is preserved.
* Reflexes: Bilateral patellar (L3-L4) and Achilles (S1) deep tendon reflexes are symmetric and graded as 2+. No pathologic reflexes (e.g., Babinski, clonus) are elicited.
* Vascular Status: Distal arterial perfusion is robust. Femoral, popliteal, dorsalis pedis, and posterior tibial pulses are palpable, symmetric, and graded as 2+ bilaterally. Capillary refill in the left digits is brisk, occurring in less than 2 seconds. The left foot is warm and well-perfused. There are no clinical indicators of acute arterial ischemia, intimal tear, or evolving compartment syndrome of the thigh or lower leg.
Imaging and Diagnostics
Initial Radiographic Evaluation
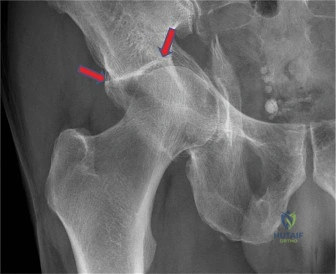
Standard trauma radiographs of the pelvis and left hip were obtained immediately upon arrival. The Anteroposterior (AP) Pelvis view demonstrates a complex, comminuted fracture involving the left acetabulum. The fracture lines clearly extend into both the anterior and posterior columns. There is significant superior dome impaction, medial displacement of the quadrilateral plate, and a classic "gull sign" indicative of severe osteopenia and superomedial articular impaction. The femoral head is medially subluxated, following the displaced quadrilateral surface into the true pelvis, creating a protrusio acetabuli deformity.
The radiographic lines of Letournel are systematically evaluated. The iliopectineal line (representing the anterior column) is disrupted. The ilioischial line (representing the posterior column) is also fractured and displaced. The radiographic teardrop is widened and medially translated. The anterior and posterior wall lines exhibit comminution, and the roof of the acetabulum shows a distinct area of subchondral impaction.
Judet Views and Pelvic Ring Assessment
To further delineate the fracture morphology, 45-degree Judet oblique radiographs were obtained.
* Obturator Oblique View: This view profiles the anterior column and the posterior wall. It confirms the severe comminution of the anterior column extending high into the ilium and reveals a non-displaced fracture line propagating through the posterior wall. The obturator ring is fractured through the superior and inferior pubic rami.
* Iliac Oblique View: This view profiles the posterior column and the anterior wall. It demonstrates a transverse-type fracture line traversing the posterior column, with the inferior segment displaced medially. The anterior wall appears relatively intact but is separated from the weight-bearing dome.
Advanced Computed Tomography Imaging
To precisely define the articular comminution, marginal impaction, and exact fracture trajectory, a fine-cut Computed Tomography (CT) scan of the pelvis with 3D reconstructions was executed.

The axial, coronal, and sagittal CT reformats provide critical surgical intelligence. The imaging confirms an Anterior Column and Posterior Hemitransverse (ACPHT) fracture pattern, a highly characteristic morphology in the geriatric population.
Key CT findings include:
1. Quadrilateral Plate Displacement: Severe comminution and medial displacement of the quadrilateral surface, resulting in loss of the medial buttress for the femoral head.
2. Marginal Impaction: A 1.5 cm area of osteochondral impaction at the superomedial weight-bearing dome (the "gull sign"). This piece is rotated and depressed into the cancellous bone of the ilium.
3. Femoral Head Status: The femoral head is medially subluxated but shows no evidence of acute fracture or impaction injury (Pipkin fracture).
4. Bone Quality: Extreme cortical thinning and severe trabecular bone loss are evident throughout the pelvis, confirming advanced osteoporosis. The sacral ala and iliac wings show significant radiolucency, which will compromise hardware purchase.
Preoperative Templating and Three Dimensional Modeling
Given the complexity of the fracture and the patient's osteoporotic bone, preoperative templating is mandatory. Digital templating software is utilized to measure the degree of medial displacement and to size the necessary fixation constructs. We template for a pre-contoured quadrilateral surface plate (infrapectineal plating) to restore the medial wall. Furthermore, because of the high likelihood of requiring an acute Total Hip Arthroplasty (THA) in the setting of severe articular impaction and osteoporotic bone, we template for a multi-hole revision acetabular shell and a fully porous-coated or cemented femoral stem. The templating process highlights the necessity for a construct that can bypass the comminution and achieve fixation in the dense bone of the sciatic buttress and the anterior ilium.
Differential Diagnosis
When evaluating a geriatric patient with a complex acetabular fracture, the Letournel classification system remains the gold standard for defining the fracture morphology. However, in osteoporotic bone, specific patterns are far more prevalent, and distinguishing between them dictates the surgical approach and fixation strategy.
| Classification Feature | Anterior Column Posterior Hemitransverse (ACPHT) | Associated Both Column Fracture | T-Type Fracture |
|---|---|---|---|
| Primary Fracture Line | High anterior column fracture extending through the pelvic brim. | Complete dissociation of all articular segments from the intact axial skeleton. | Transverse fracture line with a vertical split extending through the obturator ring. |
| Posterior Involvement | Transverse fracture line extending posteriorly, typically exiting the greater sciatic notch. | Posterior column is completely detached from the intact ilium. | Posterior column is fractured transversely, identical to the anterior column. |
| Spur Sign | Absent. The intact ilium remains connected to the posterior column above the fracture. | Present on obturator oblique view. Represents the intact iliac wing projecting above the displaced columns. | Absent. The fundamental pattern is a transverse fracture with an inferior stem. |
| Quadrilateral Plate | Frequently comminuted and medially displaced (Protrusio). | Medially displaced along with the entire acetabular construct. | May be split vertically but less commonly presents with severe isolated medial displacement. |
| Geriatric Prevalence | Highly common. The most frequent complex pattern in elderly low-energy falls. | Less common in low-energy trauma; typically requires higher energy mechanisms. | Moderate prevalence; often associated with direct lateral impact on the greater trochanter. |
| Surgical Approach | Anterior Intrapelvic (Modified Stoppa) or Ilioinguinal. | Often requires combined approaches (Anterior + Posterior) or extensive single approaches. | Kocher-Langenbeck or combined approaches depending on the level of the transverse component. |
Based on the precise radiographic and CT evaluation, the definitive diagnosis is a Left-sided Anterior Column and Posterior Hemitransverse (ACPHT) Acetabular Fracture with severe quadrilateral plate comminution, medial femoral head subluxation, and superomedial dome impaction.
Surgical Decision Making and Classification
Letournel Classification Analysis
The classification of this fracture as an ACPHT is critical. In the geriatric population, this pattern typically arises from a lateral compression force transmitted through the greater trochanter. The force vector drives the femoral head medially, resulting in the classic "blowout" of the quadrilateral plate and the anterior column, while a secondary sheer force propagates transversely across the posterior column. The presence of the "gull sign"—a pathognomonic indicator of superomedial dome impaction—signifies irreversible cartilage damage and underlying trabecular collapse.
Operative Versus Nonoperative Management
The decision between operative and nonoperative management in an elderly patient with a complex acetabular fracture is nuanced. Nonoperative management (prolonged bed rest or skeletal traction) is associated with unacceptably high rates of morbidity and mortality due to deep vein thrombosis, pulmonary embolism, decubitus ulcers, and hypostatic pneumonia. Therefore, surgical intervention is strongly indicated to mobilize the patient, relieve pain, and restore hip joint biomechanics.
The Fix and Replace Paradigm
The traditional approach to acetabular fractures involves Open Reduction and Internal Fixation (ORIF) to restore articular congruity. However, in an osteoporotic 78-year-old with severe marginal impaction and a comminuted quadrilateral plate, pure ORIF carries a high risk of failure. The osteoporotic bone often fails to hold screws, and the impacted articular cartilage inevitably leads to rapid post-traumatic osteoarthritis.
Consequently, the current gold standard for this specific demographic and fracture pattern is the "Fix and Replace" paradigm: limited ORIF to restore the structural integrity of the pelvic ring and column stability, followed immediately by an acute Total Hip Arthroplasty (THA). This approach allows for immediate full weight-bearing, which is crucial for the survival and rehabilitation of the geriatric patient.
Optimization of Medical Comorbidities
Surgical timing is dictated by the patient's anticoagulation status. The patient is on Apixaban for atrial fibrillation. Immediate surgery carries a high risk of catastrophic hemorrhage. The surgical intervention is delayed for 48 hours to allow for appropriate clearance of the DOAC, guided by anti-Xa levels and hematology consultation. During this period, the patient is placed in distal femoral skeletal traction (15 lbs) to pull the femoral head out of the pelvis, relieve pressure on the sciatic nerve, and reduce muscle spasms. Her diabetes is tightly managed with an insulin sliding scale to optimize preoperative glycemic control, targeting blood glucose levels between 140-180 mg/dL to minimize infection risk.
Surgical Technique and Intervention
Patient Positioning and Anesthesia
Following medical optimization and clearance, the patient is brought to the operating theater. General endotracheal anesthesia is induced, and a radial arterial line is placed for continuous hemodynamic monitoring. A Foley catheter is inserted to decompress the bladder, which is critical for anterior pelvic approaches.
The surgical plan involves a combined approach: an Anterior Intrapelvic (Modified Stoppa) approach for reduction and fixation of the anterior column and quadrilateral plate, followed by repositioning for a standard posterior approach to execute the Total Hip Arthroplasty.
The patient is initially placed in the supine position on a radiolucent flat Jackson table. The entire left lower extremity, hemipelvis, and abdomen are prepped and draped in a standard sterile fashion. A sterile bump is placed under the ipsilateral knee to relax the iliopsoas complex and the external iliac vessels.
Surgical Approach Selection
The Anterior Intrapelvic (Modified Stoppa) approach is selected to gain direct access to the quadrilateral surface and the pelvic brim. A Pfannenstiel incision is made 2 cm superior to the pubic symphysis. The rectus abdominis fascia is incised longitudinally along the linea alba, and the rectus bellies are retracted laterally. The transversalis fascia is carefully incised, entering the retropubic space of Retzius.
Blunt dissection is carried out laterally along the pelvic brim. The corona mortis—the anastomotic connection between the external iliac and obturator vessels—is meticulously identified, ligated with surgical clips, and divided to prevent catastrophic bleeding. The external iliac vessels and the femoral nerve are gently retracted anteriorly and laterally using a customized blunt retractor. The dissection continues posteriorly along the quadrilateral surface, identifying the obturator nerve and vessels, which are protected. The fracture lines along the pelvic brim and the comminuted quadrilateral plate are now fully visualized.
Reduction Techniques and Internal Fixation
The primary goal of the ORIF phase is to reconstruct a stable hemipelvis to support the subsequent acetabular cup. The medial displacement of the quadrilateral plate is reduced using a collinear reduction clamp and a ball-spike pusher applied directly to the quadrilateral surface. The anterior column is reduced anatomically along the pelvic brim.
Fixation is achieved using a pre-contoured pelvic brim plate (suprapectineal) combined with an infrapectineal quadrilateral surface buttress plate. The suprapectineal plate spans from the superior pubic ramus to the dense bone of the sciatic buttress near the sacroiliac joint. Cortical screws are meticulously placed, ensuring bi-cortical purchase where possible, though the osteoporotic nature of the bone requires careful torque control to prevent stripping.
The infrapectineal plate is positioned to buttress the quadrilateral surface, preventing recurrent medial migration of the femoral head. Screws are placed through the pelvic brim plate, directing them down the posterior column and into the ischium, creating a rigid construct. Intraoperative fluoroscopy (AP, Judet obliques) confirms acceptable reduction of the columns and appropriate hardware placement without intra-articular penetration.
Acute Total Hip Arthroplasty Integration
Following stable pelvic reconstruction, the anterior wound is copiously irrigated and closed in layers. The patient is then meticulously repositioned into the lateral decubitus position on a standard operating table, utilizing a peg board for rigid pelvic stabilization. The left lower extremity is re-prepped and draped.
A standard Kocher-Langenbeck (posterior) approach to the hip is utilized. The tensor fasciae latae is incised, and the gluteus maximus is split in line with its fibers. The short external rotators are tagged and released, reflecting them posteriorly to protect the sciatic nerve. A posterior capsulotomy is performed, and the hip is dislocated.
The femoral neck is osteotomized at the templated level, and the femoral head is extracted. Inspection of the acetabulum reveals the severe articular damage and the superomedial impaction (gull sign) that was identified on CT. The impacted articular fragments are elevated, and the resulting cavitary defect is grafted using morselized autograft obtained from the resected femoral head.
The acetabulum is sequentially reamed to a hemispherical shape. Because the columns have been stabilized by the anterior hardware, the reamer encounters a stable rim. A multi-hole, highly porous-coated titanium acetabular shell is impacted into place. To ensure maximum stability in the osteoporotic bone, multiple 6.5mm cancellous screws are placed through the cup into the safe zones of the ilium and the ischium, avoiding the previously placed anterior hardware. A highly cross-linked polyethylene liner is impacted into the shell.
Attention is then turned to the femur. Given the patient's age and severe osteoporosis (Dorr Type C femur), a cemented, polished, double-tapered femoral stem is selected to guarantee immediate stability and minimize the risk of periprosthetic fracture. The femoral canal is broached, a cement restrictor is placed, and third-generation cementing techniques (pulsatile lavage, retrograde cement injection, pressurization) are employed. The femoral stem is inserted, and the cement is allowed to cure.
A trial reduction is performed with a standard offset femoral head. The hip is taken through a full range of motion. The construct is highly stable, with no impingement or tendency for dislocation in flexion/internal rotation or extension/external rotation. Leg lengths and offset are restored symmetrically to the contralateral side. A permanent ceramic femoral head is impacted onto the trunnion.
Closure and Hemostasis
The hip joint is thoroughly irrigated with pulsatile lavage. A deep subfascial drain is placed to prevent hematoma formation, which is particularly important given the patient's need to resume anticoagulation. The short external rotators and the posterior capsule are meticulously repaired through transosseous drill holes in the greater trochanter to enhance posterior stability. The fascia lata, subcutaneous tissues, and skin are closed in a standard layered fashion. Sterile dressings are applied.
Post Operative Protocol and Rehabilitation
Immediate Postoperative Care and Monitoring
The patient is transferred to the Post-Anesthesia Care Unit (PACU) and subsequently to the Orthopedic Trauma Step-Down unit. Continuous hemodynamic monitoring is maintained. Postoperative laboratory studies, including a complete blood count and basic metabolic panel, are drawn at 12 and 24 hours to monitor for occult blood loss and acute kidney injury. Intravenous antibiotics (Cefazolin) are continued for 24 hours postoperatively. The subfascial drain is monitored and typically removed on postoperative day 2, provided output is less than 30 cc over an 8-hour shift.
Weight Bearing Status and Physical Therapy
The paramount advantage of the "Fix and Replace" technique is the ability to permit immediate mobilization. The patient is made Weight Bearing As Tolerated (WBAT) on the operative left lower extremity immediately on postoperative day 1. Physical and Occupational Therapy consults are initiated aggressively.
Phase I of rehabilitation focuses on bed mobility, transfers from bed to chair, and ambulation with a walker. The patient is instructed on standard posterior hip precautions (no hip flexion past 90 degrees, no internal rotation, no adduction past midline) for 6 weeks to mitigate the risk of dislocation while the posterior soft tissue envelope heals.
Venous Thromboembolism Prophylaxis
Managing Venous Thromboembolism (VTE) prophylaxis in a patient with a history of Atrial Fibrillation requires a delicate balance between preventing thromboembolic events and avoiding postoperative hematoma. Mechanical prophylaxis (sequential compression devices) is initiated immediately. Pharmacologic prophylaxis is resumed cautiously. Typically, a prophylactic dose of Low Molecular Weight Heparin (LMWH) is started 24 hours postoperatively. Once the wound is deemed dry and stable, and the drain is removed (usually around postoperative day 3), the patient is transitioned back to her home dose of Apixaban, in consultation with the cardiology and internal medicine services.
Long Term Osteoporosis Management
This fragility fracture serves as a sentinel event indicating failure of her current osteoporosis regimen (Alendronate). An inpatient endocrinology consultation is obtained. The patient will require a transition from antiresorptive therapy to an anabolic agent, such as Teriparatide or Romosozumab, to stimulate osteoblastic activity, enhance hardware integration, and prevent future contralateral hip or spinal fractures. A baseline DEXA scan is scheduled for 3 months postoperatively to establish a new baseline for monitoring therapy efficacy.
Clinical Pearls and Pitfalls
Diagnostic Pearls
- The Gull Sign: Always scrutinize the AP pelvis and CT reformats for the "gull sign." This superomedial dome impaction indicates irreversible cartilage damage and underlying trabecular collapse. In a geriatric patient, the presence of a gull sign is a strong relative indication to bypass pure ORIF and proceed directly to acute THA.
- Protrusio Acetabuli: Medial displacement of the femoral head implies catastrophic failure of the quadrilateral plate. Recognizing this dictates the need for an intrapelvic surgical approach (Stoppa) to apply a buttress plate; lateral approaches alone cannot reduce or hold the medial wall.
- Morel-Lavallée Suspicion: Even in low-energy ground-level falls, the shearing force on the lateral trochanter can create a closed degloving injury. Serial examinations of the lateral thigh for fluctuance are mandatory to prevent catastrophic deep infections.
Surgical Execution Pitfalls
- Corona Mortis Hemorrhage: During the Modified Stoppa approach, the corona mortis must be actively sought and ligated before it is inadvertently avulsed. Retraction in this area must be gentle to avoid tearing the external iliac vein.
- Inadequate Pelvic Fixation: When performing a Fix and Replace, the ORIF does not need to be anatomically perfect, but it must be biomechanically rigid enough to support the acetabular cup. Failure to adequately stabilize the anterior and posterior columns will result in early cup loosening and catastrophic construct failure.
- Cementing in Osteoporotic Femurs: Utilizing press-fit, uncemented stems in Dorr Type C osteoporotic bone carries an unacceptably high risk of intraoperative periprosthetic femur fractures. Cemented stems should be the default choice in this demographic to ensure immediate stability and allow for immediate weight-bearing.
Complication Avoidance
- Anticoagulation Rebound: Premature resumption of full-dose DOACs can lead to massive wound hematomas, leading to prolonged wound drainage and deep periprosthetic joint infection. A multidisciplinary approach with cardiology is essential for the safe bridging and resumption of Apixaban.
- Sciatic Nerve Palsy: The sciatic nerve is at risk during both the initial trauma (posterior column displacement) and the surgical intervention (retraction during the Kocher-Langenbeck approach). Keeping the knee flexed and the hip extended during posterior retraction minimizes tension on the nerve. Continuous intraoperative monitoring or frequent manual checks of retractor tension are critical.
