Comprehensive Management of Transverse Plus Posterior Wall Acetabular Fractures: A Case Study
Key Takeaway
A Transverse plus Posterior Wall Acetabular Fracture, often from high-energy trauma, involves a fracture line traversing the acetabulum (transverse component) and a significant posterior wall fragment. Diagnosis relies on detailed clinical examination, orthogonal radiographs, and crucial CT scans with 3D reconstructions to characterize fracture displacement, articular involvement, and guide pre-operative planning, especially after hip dislocation reduction.
Welcome to this Grand Rounds presentation. Today, we will conduct an exhaustive review of a complex pelvic trauma scenario, focusing on the evaluation, classification, and operative management of a transverse plus posterior wall acetabular fracture. This fracture pattern represents a highly challenging intra-articular injury that demands a meticulous understanding of pelvic osteology, precise radiographic interpretation, and advanced surgical techniques to restore joint congruity and optimize patient outcomes.
Patient Presentation and History
A 42-year-old male, previously fit and active with no significant past medical history, presented to the emergency department following a high-energy motor vehicle accident. He was an unrestrained front-seat passenger involved in a head-on collision, resulting in a direct impact of his right knee against the dashboard. Initial pre-hospital assessment revealed a Glasgow Coma Scale of 15, stable vital signs, and isolated right hip pain. There was no loss of consciousness or other obvious major trauma.
Upon arrival at the trauma bay, the patient complained of severe, incapacitating pain in his right hip and an absolute inability to bear weight. He denied paresthesia or weakness distally. His past medical history was unremarkable, with no known allergies and no regular medications. He was a non-smoker and consumed alcohol socially. Pre-injury functional status was independent ambulation without aids, engaging in regular recreational sports.
Mechanism of Injury Biomechanics
The mechanism of injury is a classic "dashboard injury," which involves an axial load transmitted longitudinally through the femoral shaft to the hip joint. The specific fracture pattern generated by this vector depends critically on the position of the hip at the exact moment of impact. In this presentation, the hip was likely in a position of flexion and neutral to slight adduction.
When the hip is flexed and adducted, the femoral head is driven posteriorly, frequently resulting in a posterior hip dislocation combined with a posterior wall fracture. The addition of the transverse component indicates that the force vector also possessed a significant central or medial trajectory, driving the femoral head into the depth of the acetabulum and shearing across both the anterior and posterior columns. The energy required to propagate a fracture line transversely across the innominate bone while simultaneously avulsing the posterior wall is substantial, correlating with the high-velocity nature of the head-on collision.
Advanced Trauma Life Support Protocol
Management commenced strictly according to Advanced Trauma Life Support protocols. The primary survey confirmed a patent airway, bilateral equal breath sounds, and hemodynamic stability with a blood pressure of 135/85 mmHg and a heart rate of 88 beats per minute. A pelvic binder was not initially applied as the mechanism and clinical presentation strongly suggested an isolated acetabular injury rather than a mechanically unstable pelvic ring disruption, which was subsequently confirmed clinically and radiographically. The secondary survey was isolated to the right lower extremity and pelvic region.
Clinical Examination Findings
Upon initial assessment, the patient was alert and oriented. General systemic examination revealed stable hemodynamics. Inspection of the right lower limb demonstrated a visibly shortened, internally rotated, and adducted posture of the right hip, classically consistent with a posterior hip dislocation. Significant swelling and ecchymosis were noted around the greater trochanter and posterior buttock.
Soft Tissue Envelope Assessment
Meticulous inspection of the soft tissue envelope is paramount in high-energy pelvic trauma. No open wounds or skin tenting were present. However, the presence of substantial posterior ecchymosis prompted a thorough evaluation for a Morel-Lavallée lesion—a closed degloving injury where the subcutaneous tissue is sheared from the underlying fascia, creating a potential space filled with blood, lymph, and necrotic fat. Palpation revealed a localized area of fluctuance over the posterior greater trochanter, raising suspicion for an early Morel-Lavallée effusion, which requires careful monitoring as it significantly increases the risk of post-operative surgical site infection if incised through during the surgical approach.
Osteological and Articular Evaluation
Palpation elicited exquisite tenderness globally around the right hip joint, particularly over the greater trochanter, posterior aspect of the iliac wing, and ischial tuberosity. The pelvis was stable to anterior-posterior compression and lateral distraction, confirming the integrity of the pelvic ring and isolating the pathology to the acetabulum.
Active and passive range of motion of the right hip was severely restricted and painful. Attempted flexion, abduction, and external rotation were met with intense guarding and discomfort. Given the obvious clinical deformity and high suspicion for dislocation, further range of motion testing was deferred until radiographic confirmation and subsequent closed reduction under conscious sedation.
Neurological and Vascular Assessment
A comprehensive neurological and vascular examination was performed. Distal pulses including the femoral, popliteal, dorsalis pedis, and posterior tibial arteries were all palpable, strong, and symmetrical with the contralateral limb. Capillary refill was brisk, and the Ankle-Brachial Index was symmetric, ruling out gross vascular compromise.
Sensory examination revealed intact sensation to light touch and pinprick throughout the dermatomes of the right lower extremity. Motor examination demonstrated full strength in ankle dorsiflexion, plantarflexion, toe extension, and knee extension.
Specific testing for sciatic nerve integrity is a critical requirement in posterior hip dislocations and posterior wall fractures. The sciatic nerve lies in close proximity to the posterior column and is frequently tethered or compressed by displaced fracture fragments or the dislocated femoral head. Assessment of both the tibial division (plantarflexion, toe flexion, sensation over the plantar foot) and the peroneal division (dorsiflexion, extensor hallucis longus function, sensation over the first dorsal web space) was meticulously performed and found to be intact. The peroneal division is particularly susceptible to injury due to its lateral position and relative tethering at the fibular head and sciatic notch.
Imaging and Diagnostics
Initial imaging in the emergency department commenced with standard orthogonal radiographs, which are the cornerstone of acute acetabular fracture evaluation.
Standard Radiographic Evaluation
-
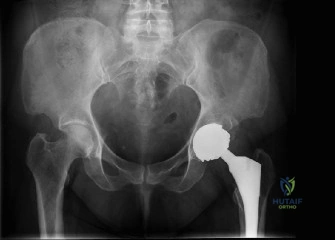
Anteroposterior Pelvis Radiograph: Demonstrated a right posterior hip dislocation with an associated acetabular fracture. The femoral head appeared congruent in the dislocated position, but a large posterior wall fragment was evident, and there was suspicion of involvement of the posterior column. The fracture lines extended superiorly into the posterior aspect of the ilium. The tear-drop sign was disrupted, and the ilioischial line was involved.

Pre-operative AP pelvis radiograph demonstrating a right posterior hip dislocation with an associated acetabular fracture involving the posterior wall and column, with superior extension into the posterior ilium. -
Judet Views:
- Iliac Oblique View: Confirmed disruption of the posterior column and posterior wall. It provided better visualization of the anterior column, which appeared intact in its entirety, and the anterior wall. The iliac wing component of the fracture was also better delineated.
- Obturator Oblique View: Clearly demonstrated the extent of the anterior column and the anterior half of the pelvic ring. In this specific case, the obturator oblique view revealed a disruption of the anterior column line (iliopectineal line), which, when combined with the posterior column disruption seen on the iliac oblique, confirmed the presence of a transverse fracture component. The spur sign, classically associated with associated both-column fractures, was absent, helping to differentiate the transverse pattern.
Advanced Cross Sectional Imaging
Following emergent closed reduction of the posterior hip dislocation in the emergency department under procedural sedation, a post-reduction AP pelvis radiograph confirmed concentric reduction of the femoral head. Subsequently, a fine-cut Computed Tomography scan of the pelvis with 2D multiplanar reformats and 3D surface rendering was obtained.
The CT scan is mandatory for comprehensive pre-operative planning. In this patient, the axial cuts delineated the precise size and comminution of the posterior wall fragment. More importantly, the CT revealed a critical finding: marginal impaction of the articular cartilage along the posterior rim. Marginal impaction occurs when the cancellous bone of the acetabular dome is crushed by the dense cortical bone of the femoral head during the dislocation event. Failure to recognize and surgically elevate this impacted segment leads to a non-congruent joint, rapid cartilage wear, and inevitable early post-traumatic osteoarthritis.
Furthermore, the sagittal and coronal reformats allowed for exact mapping of the transverse fracture line. The transverse component was noted to be juxtatectal (crossing exactly at the level of the superior acetabular dome), dividing the innominate bone into an intact upper iliac segment and a lower ischiopubic segment. Intra-articular loose bodies, consisting of osteochondral shear fragments from the femoral head and acetabular wall, were also identified within the dependent portion of the joint space.
Pre Operative Templating
Digital pre-operative templating was performed using the 3D CT reconstructions. The templating process involved virtual reduction of the transverse component followed by the posterior wall. Implant selection was mapped, anticipating the need for an interfragmentary lag screw for the transverse component (placed either antegrade down the posterior column or retrograde from the ischium), combined with a contoured reconstruction plate to buttress the posterior wall and neutralize the posterior column.
Differential Diagnosis
Accurate classification of acetabular fractures using the Judet and Letournel system is essential for determining the surgical approach and predicting outcomes. The differential diagnosis for a fracture involving the posterior wall and a column disruption includes several distinct patterns.
| Fracture Pattern Classification | Radiographic Hallmarks | Mechanism of Injury | Preferred Surgical Approach |
|---|---|---|---|
| Transverse + Posterior Wall | Disrupted iliopectineal & ilioischial lines; large posterior wall fragment; intact obturator ring. | Dashboard injury; axial load on flexed, neutral/adducted hip. | Kocher-Langenbeck (if transverse is reducible posteriorly) or Dual Approach. |
| T-Type + Posterior Wall | Disrupted iliopectineal & ilioischial lines; vertical fracture line through obturator ring; posterior wall fragment. | Axial load on flexed hip with hyper-abduction. | Combined approaches (e.g., Kocher-Langenbeck + Ilioinguinal/Stoppa). |
| Posterior Column + Posterior Wall | Disrupted ilioischial line; intact iliopectineal line; posterior wall fragment; inferior extension to ischium. | Axial load on flexed hip with internal rotation. | Kocher-Langenbeck. |
| Associated Both Column | All primary radiographic lines disrupted; "Spur sign" present on obturator oblique; dissociation of articular surface from axial skeleton. | Lateral compression or complex high-energy axial loading. | Ilioinguinal, Modified Stoppa, or Pararectus (often without posterior approach). |
In this case, the presence of a fracture line crossing both the anterior and posterior columns (disrupting both the iliopectineal and ilioischial lines) without involving the obturator foramen rules out a T-type fracture and an isolated posterior column fracture. The absence of the spur sign and the fact that a portion of the articular surface (the intact superior ilium) remains attached to the axial skeleton rules out an associated both-column fracture. Thus, the diagnosis is definitively a Transverse plus Posterior Wall fracture.
Surgical Decision Making and Classification
The Letournel classification system divides acetabular fractures into five elementary types and five associated types. The Transverse plus Posterior Wall fracture is one of the five associated patterns. It combines a transverse fracture, which divides the innominate bone horizontally, with a posterior wall fracture, which compromises posterior joint stability.
Indications for Operative Intervention
Non-operative management of acetabular fractures is strictly reserved for minimally displaced fractures (less than 2mm of step-off), fractures that do not involve the weight-bearing dome (roof arc measurements greater than 45 degrees), and fractures that exhibit dynamic stability on fluoroscopic stress views.
In this patient, operative intervention was absolutely indicated due to several factors:
1. Posterior Instability: The posterior wall fragment was large, involving more than 40% of the posterior articular surface. A defect of this size renders the hip joint biomechanically unstable, predisposing the patient to recurrent posterior dislocations even with routine activities.
2. Intra Articular Incongruity: The juxtatectal transverse component created a significant step-off in the weight-bearing dome. Articular step-offs greater than 2mm rapidly alter joint contact pressures, leading to accelerated cartilage destruction.
3. Marginal Impaction: The CT scan identified osteochondral impaction of the posterior rim. This requires direct surgical elevation and bone grafting to restore the native radius of curvature of the acetabulum.
4. Intra Articular Loose Bodies: The presence of osteochondral fragments within the joint space necessitates arthrotomy and debridement to prevent mechanical locking and third-body wear.
Surgical Approach Selection
The selection of the surgical approach is arguably the most critical decision in acetabular fracture surgery. For a Transverse plus Posterior Wall fracture, the Kocher-Langenbeck approach is the workhorse.
The rationale for utilizing an isolated posterior approach (Kocher-Langenbeck) in this specific case is based on the ability to directly visualize and reduce the posterior wall, while indirectly or directly reducing the transverse component. The transverse fracture can often be manipulated through the greater sciatic notch using specialized reduction tools. If the anterior aspect of the transverse fracture (the anterior column component) is highly displaced and cannot be reduced from the posterior side, a combined approach (adding an anterior Ilioinguinal or modified Stoppa approach) might be necessary. However, pre-operative CT templating suggested that the transverse component was amenable to reduction via the posterior approach using a Jungbluth clamp applied across the posterior column.
Timing of the surgery was determined by the patient's physiologic status and the local soft tissue envelope. The initial hip dislocation was reduced emergently to restore blood supply to the femoral head and minimize the risk of avascular necrosis. Definitive fixation was scheduled for post-injury day four, allowing for optimization of the patient, resolution of the initial soft tissue swelling, and careful monitoring of the posterior Morel-Lavallée lesion, which fortunately remained stable and did not require separate debridement.
Surgical Technique and Intervention
The goal of surgical intervention is anatomic reduction of the articular surface and rigid internal fixation to allow for early mobilization.
Patient Positioning and Preparation
The patient was placed under general endotracheal anesthesia. A Foley catheter was inserted to decompress the bladder and monitor intra-operative fluid balance. The patient was positioned in the prone position on a radiolucent Jackson table. The prone position is highly advantageous for the Kocher-Langenbeck approach as it allows the hip to be extended and the knee flexed, significantly relaxing the tension on the sciatic nerve.
The entire right lower extremity, hemipelvis, and lower abdomen were prepped and draped in a standard sterile fashion, allowing for free manipulation of the limb during the procedure. Intra-operative fluoroscopy was positioned to ensure unobstructed access for AP and Judet views.
The Kocher Langenbeck Approach
A standard Kocher-Langenbeck incision was utilized. The incision began slightly distal and posterior to the posterior superior iliac spine, extending distally to the tip of the greater trochanter, and then continued longitudinally down the axis of the femoral shaft.
The subcutaneous tissues were dissected, taking care to achieve meticulous hemostasis. The fascia lata was incised in line with the skin incision, and the gluteus maximus was split along the direction of its muscle fibers. The superior gluteal neurovascular bundle, exiting the greater sciatic notch superior to the piriformis, was identified and carefully protected.
The sciatic nerve was immediately identified as it emerged from the greater sciatic notch, deep to the gluteus maximus and superficial to the short external rotators. A vessel loop was loosely placed around the nerve for continuous identification, but no traction was applied. The nerve was mobilized gently to allow visualization of the underlying structures.
The short external rotators (piriformis, superior gemellus, obturator internus, and inferior gemellus) were identified. The piriformis tendon was tagged and tenotomized near its insertion on the greater trochanter. The obturator internus and gemelli were similarly tagged and released. The reflection of the obturator internus muscle belly was used as a soft tissue cushion to protect the sciatic nerve during retraction. The quadratus femoris was left intact to preserve the ascending branch of the medial femoral circumflex artery, which provides the critical blood supply to the femoral head.
Joint Debridement and Marginal Impaction Elevation
Upon reflecting the short external rotators, the large posterior wall fracture fragment was identified and carefully mobilized, preserving its soft tissue attachments to the joint capsule to maintain its vascularity. The hip joint was distracted manually, and the intra-articular hematoma and loose osteochondral bodies were thoroughly irrigated and removed.
Direct visualization of the articular surface confirmed the presence of marginal impaction. Using a curved osteotome, the impacted articular cartilage and its underlying subchondral bone were carefully elevated back to their native anatomical position, matching the contour of the femoral head. This created a cavitary defect in the underlying cancellous bone of the posterior column. This defect was immediately packed with cancellous allograft to structurally support the elevated articular segment.
Reduction of the Transverse Component
With the joint cleared and the marginal impaction addressed, attention was turned to the transverse fracture component. The transverse fracture line was identified crossing the posterior column.
Reduction of the transverse component required addressing both the displacement and the rotation. A Schanz pin was inserted into the ischial tuberosity to act as a joystick, allowing for manipulation of the distal ischiopubic segment. A Jungbluth pelvic reduction clamp was then applied. One tine of the clamp was placed in a drill hole superior to the fracture line on the intact ilium, and the other tine was placed in a drill hole inferior to the fracture line on the ischium.
By manipulating the ischial Schanz pin and carefully tightening the Jungbluth clamp, the transverse component was anatomically reduced. The reduction was confirmed visually along the retroacetabular surface and digitally by palpating the quadrilateral surface through the greater sciatic notch. Fluoroscopic AP and Judet views were obtained to confirm the reduction of the anterior column component of the transverse fracture.
Once anatomic reduction was achieved, provisional fixation of the transverse component was obtained using smooth Kirschner wires. Definitive fixation was then accomplished by placing a 3.5mm fully threaded cortical lag screw in an antegrade fashion from the posterior column, crossing the transverse fracture line perpendicular to its plane, and achieving purchase in the dense bone of the ischium.
Fixation of the Posterior Wall
Following stabilization of the transverse component, the posterior wall fragment was reduced anatomically against the reconstructed marginal impaction and the intact superior dome. Provisional fixation was achieved with ball-spiked pushers and K-wires.
Definitive fixation of the posterior wall utilized a combination of spring plates and a buttress plate. Two under-contoured 3.5mm one-third tubular plates (spring plates) were applied directly over the posterior wall fragment to provide localized compression and resist shear forces.
A 3.5mm pelvic reconstruction plate was then meticulously templated and contoured to match the complex anatomy of the posterior column. The plate spanned from the dense bone of the superior ilium, across the posterior wall fragment and the transverse fracture line, down to the ischial tuberosity. The plate was secured with alternating cortical and cancellous screws. Care was taken to ensure that screws placed in the peri-articular region were extra-articular.
Intra Operative Imaging and Closure
Final intra-operative fluoroscopy, including AP, Iliac Oblique, and Obturator Oblique views, confirmed anatomic reduction of both the transverse and posterior wall components. The teardrop was restored, the iliopectineal and ilioischial lines were re-established, and the joint space was symmetric.
To definitively rule out intra-articular hardware penetration, the hip was taken through a full range of motion under live fluoroscopy. The absence of crepitus or mechanical block, combined with clear radiographic joint spaces throughout the arc of motion, confirmed extra-articular screw placement.
The wound was irrigated copiously with sterile saline. A subfascial closed suction drain was placed. The short external rotators were repaired back to their trochanteric insertions to provide a soft tissue barrier over the hardware and protect the sciatic nerve. The split in the gluteus maximus was loosely approximated, the fascia lata was closed tightly with interrupted heavy absorbable sutures, and the subcutaneous tissue and skin were closed in layers.
Post Operative Protocol and Rehabilitation
The post-operative management of acetabular fractures is as critical as the surgical execution. The rehabilitation protocol is designed to protect the fixation construct while promoting early mobility to prevent systemic complications.
Weight Bearing Status and Mobilization
The patient was restricted to toe-touch weight-bearing (approximately 10-15% of body weight) on the operative right lower extremity for a period of 8 to 10 weeks. This restriction is necessary to prevent shear forces across the posterior wall and axial loading across the transverse component while primary bone healing occurs.
Physical therapy was initiated on post-operative day one. Early interventions focused on isometric quadriceps and hamstring strengthening, ankle pumps to promote venous return, and gentle passive and active-assisted range of motion of the hip within a pain-free arc. Flexion was limited to 90 degrees to prevent excessive stress on the posterior wall repair.
Deep Vein Thrombosis Prophylaxis
Pelvic trauma and major orthopedic surgery place the patient at an exceptionally high risk for deep vein thrombosis and subsequent pulmonary embolism. Mechanical prophylaxis with sequential compression devices was utilized bilaterally while the patient was in bed. Chemical prophylaxis was initiated 12 hours post-operatively, utilizing low-molecular-weight heparin (Enoxaparin 40mg subcutaneously daily), which was continued for a total of 35 days post-injury, in accordance with current orthopedic trauma guidelines.
Heterotopic Ossification Prophylaxis
The Kocher-Langenbeck approach involves significant dissection of the gluteal musculature, carrying a high risk of heterotopic ossification (HO)—the abnormal formation of mature lamellar bone within the soft tissues. Severe HO can severely restrict hip range of motion and compromise functional outcomes.
Prophylaxis against HO can be achieved via localized external beam radiation or non-steroidal anti-inflammatory drugs. In this patient, chemical prophylaxis was chosen. Indomethacin 75mg sustained-release was prescribed daily for a duration of 3 to 6 weeks. Concomitant use of a proton pump inhibitor was initiated to mitigate the risk of gastrointestinal ulceration associated with prolonged NSAID use.
Long Term Follow Up
The patient was discharged to a specialized rehabilitation facility on post-operative day five. Routine clinical and radiographic follow-up was scheduled at 2 weeks, 6 weeks, 12 weeks, 6 months, and 1 year.
At the 12-week mark, radiographs demonstrated progressive fracture consolidation with maintenance of anatomic alignment and no evidence of hardware failure or avascular necrosis of the femoral head. The patient was subsequently transitioned to a progressive weight-bearing protocol and advanced strengthening exercises, with the ultimate goal of returning to his pre-injury level of occupational and recreational activity.
Clinical Pearls and Pitfalls
The management of transverse plus posterior wall acetabular fractures is fraught with potential complications. Mastery of this injury pattern requires an awareness of several critical pearls and pitfalls.
Sciatic Nerve Protection
Pitfall: Iatrogenic sciatic nerve palsy is the most devastating intra-operative complication associated with the Kocher-Langenbeck approach. It most commonly results from excessive or prolonged traction on the nerve during exposure of the posterior column.
Pearl: Maintain the hip in extension and the knee in at least 60 degrees of flexion throughout the procedure to minimize tension on the nerve. Avoid placing retractors directly on the nerve. Utilize the reflected obturator internus muscle belly as a physical barrier between the retractors and the sciatic nerve. Regularly inspect the nerve throughout the case to ensure it is not under undue tension.
Addressing Marginal Impaction
Pitfall: Failure to recognize and elevate marginal impaction on pre-operative CT or intra-operatively leads to a non-congruent joint. If the posterior wall is simply fixed over the impacted segment, the femoral head will subluxate into the defect, leading to rapid, catastrophic post-traumatic arthritis.
Pearl: Always scrutinize the axial and coronal CT cuts for impacted articular fragments. Intra-operatively, before reducing the main posterior wall fragment, meticulously inspect the articular margin. Elevate the impacted segment anatomically and support it robustly with structural bone graft (autograft from the greater trochanter or allograft) before applying the definitive fixation plate.
Avoiding Intra Articular Hardware
Pitfall: The complex, multi-planar geometry of the acetabulum makes screw placement challenging. Screws placed in the danger zones (particularly the superior and anterior-superior quadrants from a posterior approach) can easily penetrate the articular surface, leading to mechanical cartilage destruction.
Pearl: Utilize the concept of the "safe zone" for screw placement. Always confirm screw trajectory with multiple fluoroscopic views. The most reliable method to rule out intra-articular penetration is the dynamic fluoroscopic stress test: take the hip through a full, continuous arc of motion under live fluoroscopy. If a screw is intra-articular, it will bridge the joint space and cause the joint space to widen or demonstrate mechanical catching during motion. Listen for crepitus.
Monitoring for Avascular Necrosis
Pitfall: Avascular necrosis of the femoral head is a late complication, often presenting months to years after the initial injury. It is directly related to the initial trauma (disruption of the ligamentum teres and retinacular vessels during dislocation) and the timing of the initial reduction.
Pearl: Emergent closed reduction of the dislocated hip within 6 hours of injury is the single most important modifiable factor in reducing the risk of AVN. During the surgical approach, meticulously preserve the quadratus femoris muscle and the ascending branch of the medial femoral circumflex artery. Counsel the patient extensively on the signs of AVN and maintain long-term radiographic surveillance.
