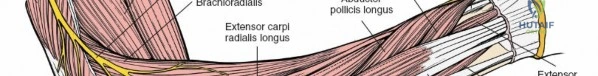
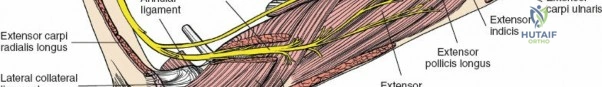
As an academic orthopedic surgeon and medical educator, understanding the intricate applied anatomy of the posterior forearm is paramount for safe and effective surgical intervention on the radius. This guide provides an exhaustive review of the posterior approach to the radius, emphasizing nerve supply, muscle compartmentalization, and critical surgical pearls for residents, fellows, and practicing orthopedic surgeons.
Introduction and Epidemiology
The posterior approach to the radius is a versatile and effective surgical corridor for addressing various pathologies affecting the proximal and middle thirds of the radial shaft. While the volar Henry approach is more commonly employed for distal and mid-shaft diaphyseal fractures due to its consistent anatomy and lower reported rates of nerve injury, the posterior approach offers direct access to the dorsal aspect of the radius, particularly advantageous for certain fracture patterns, non-unions, or specific tumor resections. Mastering this approach necessitates an in-depth understanding of the dorsal forearm musculature and, critically, the course and innervation pattern of the posterior interosseous nerve (PIN).
Fractures of the radial shaft constitute a significant proportion of upper extremity trauma. Isolated radial shaft fractures are less common than combined radius and ulna fractures (both bone forearm fractures), but both can necessitate surgical stabilization. The epidemiology often shows a bimodal distribution, affecting younger, active individuals due to high-energy trauma, and older, osteoporotic patients from low-energy falls. While stable, minimally displaced fractures may be managed non-operatively, displaced or unstable fractures, open fractures, and those associated with neurovascular compromise frequently require open reduction and internal fixation (ORIF). The selection of a surgical approach is often dictated by the fracture location, pattern, and surgeon familiarity, with the posterior approach offering a distinct advantage for dorsal comminution, specific malunions requiring dorsal corrective osteotomies, or when prior volar plating precludes a second volar exposure. Minimizing iatrogenic injury, particularly to the PIN, is the guiding principle for a successful outcome.
Surgical Anatomy and Biomechanics
A thorough understanding of the topographical and functional anatomy of the dorsal forearm is foundational for safely navigating the posterior approach to the radius. The twelve muscles of the dorsal forearm are traditionally divided into three functional groups, each with distinct origins, insertions, and innervation patterns.
Dorsal Forearm Muscle Compartments
-
The Mobile Wad of Three:
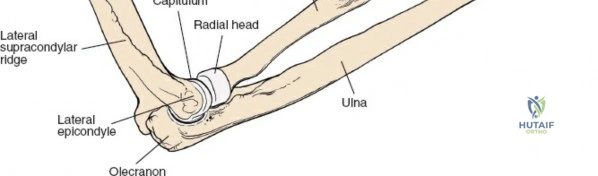
These three muscles form the lateral bulk of the forearm. They originate from a continuous line spanning the lateral supracondylar ridge and the lateral epicondyle of the humerus.- Brachioradialis (BR): Originates from the upper two-thirds of the lateral supracondylar ridge and inserts into the radial styloid. It primarily flexes the elbow, especially in a neutral forearm position, and assists in pronation/supination to a neutral position. Innervated by the radial nerve (proximal to PIN branching).
- Extensor Carpi Radialis Longus (ECRL): Originates from the lower one-third of the lateral supracondylar ridge and inserts into the base of the second metacarpal. It extends and radially deviates the wrist. Innervated by the radial nerve (proximal to PIN branching).
- Extensor Carpi Radialis Brevis (ECRB): Originates from the lateral epicondyle via the common extensor origin and inserts into the base of the third metacarpal. It extends and radially deviates the wrist. Crucially, the ECRB receives its nerve supply from the posterior interosseous nerve (PIN) proximal to the supinator muscle, making its proximal portion a safe plane for dissection as its nerve branches are well proximal to the typical operative field for mid-shaft radius exposures.

-
The Superficial Extensor Muscles:
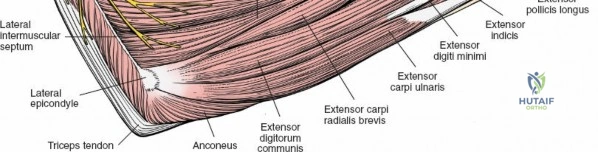
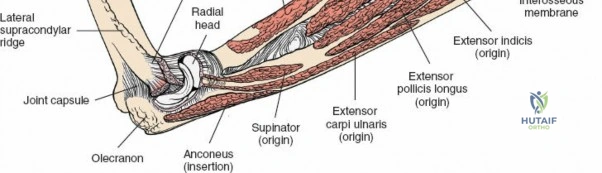
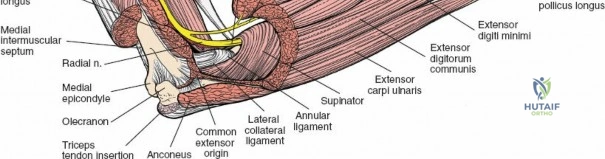
These muscles fan out from the lateral epicondyle of the humerus, forming the bulk of the superficial dorsal forearm. From ulnar to radial, these include:- Anconeus: A small, triangular muscle originating from the lateral epicondyle and inserting onto the olecranon and posterior ulna. It assists in elbow extension and stabilizes the ulna during pronation/supination. Innervated by the radial nerve (branch to anconeus often arises proximal to PIN).
- Extensor Carpi Ulnaris (ECU): Originates from the lateral epicondyle and posterior ulna, inserting into the base of the fifth metacarpal. It extends and ulnarly deviates the wrist. Innervated by the posterior interosseous nerve (PIN).
- Extensor Digiti Minimi (EDM): Originates from the lateral epicondyle and inserts into the extensor expansion of the little finger. It extends the little finger. Innervated by the posterior interosseous nerve (PIN).
- Extensor Digitorum Communis (EDC): Originates from the lateral epicondyle and inserts into the extensor expansions of the medial four fingers. It extends the medial four fingers at the metacarpophalangeal (MCP) joints and assists in interphalangeal (IP) joint extension. Innervated by the posterior interosseous nerve (PIN) in the forearm.
One important internervous plane in this superficial layer is between the Extensor Carpi Ulnaris (supplied by PIN) and the Flexor Carpi Ulnaris (supplied by the ulnar nerve) on the ulnar side. However, for the posterior approach to the radius, the critical plane is between the ECRB and the EDC. This plane is safe because the ECRB receives its nerve supply well proximal to the distal extent of the common extensor origin, leaving the distal portion of its belly amenable to retraction without denervation.
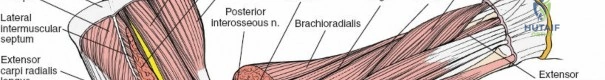
-
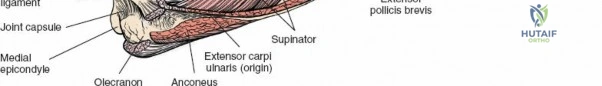
The Five Deep Muscles:
These muscles are positioned deep to the superficial extensors and are intimately associated with the radius and interosseous membrane. All five are innervated by the PIN.- Supinator: Originates from the lateral epicondyle, radial collateral ligament, annular ligament, and supinator crest of the ulna, inserting onto the dorsal, lateral, and anterior surfaces of the proximal third of the radius. Its primary function is supination of the forearm. The Posterior Interosseous Nerve (PIN) passes through its two heads.
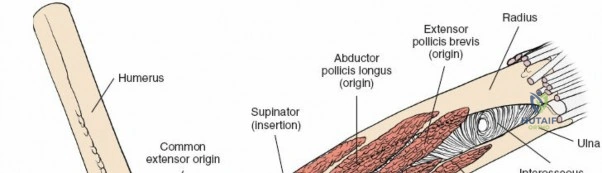
- Abductor Pollicis Longus (APL): Originates from the posterior surfaces of the ulna and radius (distal to supinator) and the interosseous membrane, inserting into the base of the first metacarpal. It abducts and extends the thumb.
- Extensor Pollicis Brevis (EPB): Originates from the posterior surface of the radius (distal to APL) and interosseous membrane, inserting into the base of the proximal phalanx of the thumb. It extends the metacarpophalangeal (MCP) joint of the thumb.
- Extensor Pollicis Longus (EPL): Originates from the posterior surface of the ulna and interosseous membrane, inserting into the base of the distal phalanx of the thumb. It extends the interphalangeal (IP) joint of the thumb and adducts/radially deviates the wrist.
- Extensor Indicis (EI): Originates from the posterior surface of the ulna and interosseous membrane, inserting into the extensor expansion of the index finger. It extends the index finger independently.
The APL, EPB, and EPL cross the forearm obliquely from ulnar to radial, forming the boundaries of the anatomical snuffbox.

Posterior Interosseous Nerve (PIN) Anatomy and Vulnerability
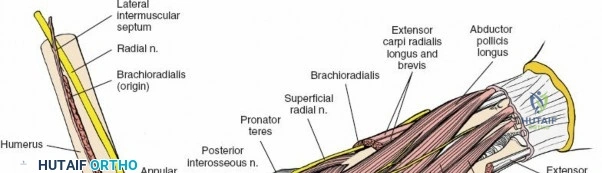
The PIN is a purely motor branch of the radial nerve. It arises from the radial nerve anterior to the lateral epicondyle, typically at the level of the radiohumeral joint. It then courses distally, entering the supinator muscle through the Arcade of Frohse (a fibrous arch in the superficial head of the supinator). This arcade is a critical point of potential compression or iatrogenic injury.
Within the supinator muscle, the PIN winds around the radial neck and then exits the supinator on its posterior aspect, emerging into the deep posterior compartment of the forearm. Distal to its exit from the supinator, the PIN innervates all the muscles of the deep posterior compartment (supinator, APL, EPB, EPL, EI) and the superficial extensors (ECU, EDM, EDC). Notably, it supplies the ECRB proximal to the supinator.
The PIN is particularly vulnerable during the posterior approach in the proximal forearm, especially when exposing the radial neck or proximal radial shaft. Aggressive retraction of the supinator can lead to neuropraxia or, less commonly, transection. Awareness of its entry point into the supinator (approximately 3-4 cm distal to the lateral epicondyle) and its deep course is crucial.
Vascular Supply
The dorsal forearm receives its primary vascular supply from the posterior interosseous artery (PIA), which arises from the common interosseous artery, a branch of the ulnar artery. The PIA courses between the superficial and deep extensor muscles, often alongside the PIN. Proximally, perforators from the radial recurrent artery also contribute. Care should be taken to preserve this vascularity, especially during extensive subperiosteal dissection, as it contributes to bone healing.
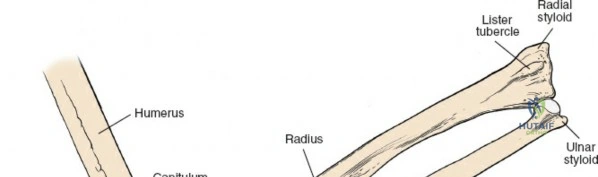
Biomechanics of the Radius and Forearm
The radius, along with the ulna, forms a functional unit crucial for forearm rotation (pronation and supination). The curvature of the radial shaft is critical for maintaining this rotational integrity. Disruption of this curvature (e.g., malunion) can significantly impair forearm rotation. The posterior approach is typically chosen when direct access to the dorsal aspect of the radial shaft is required, especially for complex fracture patterns or deformity corrections where restoring the dorsal contour is key. The stability of fixation must withstand the powerful forces of pronation and supination, which are generated by the numerous muscles acting on the forearm.
Indications and Contraindications
The selection of a surgical approach to the radius is guided by a precise assessment of the fracture pattern, patient factors, and anticipated surgical needs. The posterior approach offers distinct advantages in specific scenarios but also carries inherent risks.
Indications for the Posterior Approach to the Radius
- Proximal and Mid-Shaft Radial Fractures: Especially those with significant dorsal comminution, displacement, or angular deformity that requires direct visualization for reduction and dorsal plate application.
- Radial Non-Unions or Malunions: When a dorsal corrective osteotomy is necessary to restore radial bow and forearm rotation.
- Tumors or Lesions: Requiring excision from the dorsal aspect of the radial diaphysis.
- Osteomyelitis: Of the radial shaft requiring debridement and external fixation or plate coverage.
- Revision Surgery: In cases where a prior volar plate is present or when extensive scarring from a previous volar approach makes re-entry hazardous.
- Specific Fracture Patterns: Such as proximal radius fractures involving the metaphysis that may be better stabilized with a dorsal plate for biomechanical reasons or to avoid disruption of the volar musculature.
Contraindications for the Posterior Approach to the Radius
- Active Local Infection: At the proposed surgical site.
- Severe Soft Tissue Compromise: Including extensive burns, crush injuries, or necrotic tissue that precludes safe wound closure.
- Pathology Best Addressed by Other Approaches: For instance, distal radius fractures are typically approached volarly, and radial head fractures may necessitate a posterolateral approach (Kaplan's or Kocher's) rather than a true posterior diaphyseal approach.
- Significant Volar Commensuration or Instability: Where a volar plate is deemed biomechanically superior for stabilization.
- Known Allergy to Implant Materials: (General contraindication for ORIF).
Summary of Operative versus Non-Operative Indications
| Indication Type | Operative Management | Non-Operative Management |
|--------------------|------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------ |
| Primary Indication | Displaced or unstable midshaft radial fractures requiring direct visualization and reduction for stable fixation. This includes:
- Complex displaced fractures (ee.g., highly comminuted, spiral).
- Open fractures (requiring debridement and stable fixation).
- Fractures with neurovascular compromise (after initial reduction attempts).
- Non-unions or malunions (especially those with dorsal angulation or significant loss of radial bow).
- Pathologic fractures (tumor excision, stable fixation).
- Revision surgery where prior volar approach or implant compromises access. | Non-displaced or minimally displaced fractures without significant instability or functional impairment. This typically includes:
- Stable, closed, simple fracture patterns.
- Stress fractures without significant displacement.
- Pediatric radial shaft fractures with good remodeling potential.
- Patients with severe comorbidities precluding surgery.
- Acceptable alignment after closed reduction (e.g., in children). |
Pre Operative Planning and Patient Positioning
Meticulous preoperative planning is a cornerstone of safe and effective surgical management.
Preoperative Assessment
A comprehensive patient history and physical examination are essential. Evaluate the patient's overall health, comorbidities, medication use, and functional demands. Neurovascular status of the extremity, particularly sensation and motor function, must be thoroughly documented preoperatively to identify any pre-existing deficits and for comparison postoperatively. Assess the soft tissue envelope for any injury, swelling, or open wounds that might complicate the approach.
Radiographic evaluation typically includes orthogonal views (AP and lateral) of the forearm, including the elbow and wrist joints to rule out associated injuries (e.g., Monteggia fracture-dislocation). A computed tomography (CT) scan with 3D reconstructions can be invaluable for complex comminuted fractures, articular involvement, or in planning corrective osteotomies for malunions, providing precise details of fracture morphology and displacement.
Anesthesia
Regional anesthesia (e.g., brachial plexus block) combined with general anesthesia is often preferred, as it provides excellent intraoperative muscle relaxation and prolonged postoperative analgesia, facilitating early rehabilitation. Local anesthetic infiltration at the incision site can also supplement pain control.
Patient Positioning and Surgical Preparation
The patient is typically positioned supine on the operating table. The affected arm is placed on a dedicated hand table, allowing full access to the dorsal forearm. The elbow should be flexed to 90 degrees, and the forearm pronated. This pronated position moves the mobile wad radially and positions the PIN more anteriorly, away from the direct line of incision and initial dissection, theoretically offering some protection. However, extreme pronation can tighten the supinator, potentially making PIN identification or careful retraction more challenging. A neutral or slightly pronated position is usually adequate.
A tourniquet is applied to the upper arm to provide a bloodless field, which is critical for identifying delicate structures and maintaining clear surgical planes. The arm is then meticulously prepped and draped in a sterile fashion, ensuring adequate exposure from the elbow to the wrist. The image intensifier (fluoroscopy) should be readily available and positioned to allow unobstructed AP and lateral views of the radius throughout the procedure.
Incision Planning
The skin incision is typically a straight longitudinal incision centered over the dorsal aspect of the radial shaft, extending proximally from the level of the radial head/neck to just proximal to the dorsal wrist crease, as dictated by the extent of the pathology. For mid-shaft fractures, a 10-15 cm incision is usually sufficient. Proximally, it should be curved slightly laterally to avoid crossing the elbow flexion crease at a right angle, which can lead to scar contracture. Palpate the radial head and the dorsal aspect of the radial shaft to guide the incision.
Detailed Surgical Approach and Technique
The posterior approach to the radius requires a systematic, layered dissection to protect vital neurovascular structures, particularly the PIN.
Skin Incision and Superficial Dissection
-
Skin Incision: A straight longitudinal incision is made over the dorsal radial shaft, as planned. The incision should be generous enough to allow adequate exposure without excessive retraction.

-
Subcutaneous Tissue: The incision is deepened through the subcutaneous fat. Identify and ligate or coagulate any superficial veins (e.g., branches of the cephalic vein). Superficial nerves, such as the lateral antebrachial cutaneous nerve, may be encountered more proximally and radially; these should be identified and protected, typically retracted radially.
-
Deep Fascia: Incise the deep forearm fascia longitudinally. This exposes the underlying muscle belly of the mobile wad radially and the superficial extensors ulnarly.

Identification of Internervous Plane and Deep Dissection
The key to the posterior approach lies in identifying and utilizing the safe internervous plane between the extensor carpi radialis brevis (ECRB) and the extensor digitorum communis (EDC).
-
Identify the Mobile Wad: Visually identify the brachioradialis (BR) muscle, which forms the radial border of the mobile wad. Deep and ulnar to the BR, identify the ECRL and ECRB. The ECRB is typically the most superficial of the two.

-
Identify the Superficial Extensors: Ulnar to the mobile wad, identify the extensor digitorum communis (EDC) and, further ulnar, the extensor carpi ulnaris (ECU).
-
Locate the Internervous Plane: The surgical plane is found between the ECRB (radially) and the EDC (ulnarly). This plane is exploited because, as previously discussed, the ECRB receives its PIN innervation well proximal to the supinator, making its distal muscle belly safe for retraction. Both ECRB and EDC are innervated by the PIN, but their nerve entry points allow for safe separation.
Carefully dissect along this plane using blunt and sharp dissection. Retract the ECRB and ECRL radially. Retract the EDC and other superficial extensors (EDM, ECU) ulnarly. This exposes the deep layer of muscles, including the supinator and, more distally, the deep thumb extensors (APL, EPB, EPL).
-
Protecting the Posterior Interosseous Nerve (PIN): This is the most critical step. The PIN penetrates the supinator muscle, usually 3-4 cm distal to the lateral epicondyle.
- Proximal Radius Exposure: For fractures involving the radial neck or very proximal shaft, a direct attempt to visualize and protect the PIN is often recommended. This involves careful blunt dissection along the supinator muscle. The PIN can be identified winding through the supinator. The supinator muscle can be split longitudinally or partially released from its ulnar origin to expose the proximal radius. When splitting the supinator, perform it along its fibers, identifying the PIN as it emerges from deep within its substance. Retract the PIN, typically with a vessel loop, to protect it throughout the procedure.
- Mid-Shaft Radius Exposure: For fractures confined to the mid-shaft, the PIN is typically deep within the supinator and posterior to the radial shaft, or has already exited the supinator to innervate the deep extensors. By retracting the ECRB/ECRL radially and EDC/other superficial extensors ulnarly, the supinator muscle becomes visible. The muscle bellies of the APL and EPB may be visible more distally. Avoid aggressive subperiosteal dissection on the posterior aspect of the radius, particularly in the proximal third, to prevent stripping the PIN branches or causing traction injury. If the fracture is more distal in the mid-shaft, the APL and EPB may need to be carefully elevated from the posterior radius.

Exposure of the Radius and Fracture Management
-
Subperiosteal Exposure: Once the PIN is identified and protected, or its anatomical course is respected, the periosteum over the dorsal aspect of the radial shaft is incised longitudinally. Subperiosteal elevation is then performed using an elevator to expose the fracture site. Avoid extensive stripping to preserve soft tissue attachments and vascularity.
-
Fracture Reduction: The fracture fragments are reduced using direct manipulation, traction, or bone clamps. Care is taken to restore the anatomical length, rotation, and radial bow. Provisional fixation is achieved with K-wires or reduction clamps. Intraoperative fluoroscopy confirms satisfactory reduction.

-
Internal Fixation: A contoured dorsal plating system (e.g., a low-profile Locking Compression Plate) is typically applied to the dorsal surface of the radius. The plate should be centered over the dorsal aspect of the radial shaft. Ensure sufficient screws are placed proximal and distal to the fracture site, respecting the working length principle. Screw length selection is critical to achieve bicortical purchase without violating the volar cortex or impinging on the interosseous membrane. Fluoroscopy is again used to confirm plate position and screw placement.

Wound Closure
-
Irrigation and Hemostasis: Thoroughly irrigate the wound with sterile saline. Achieve meticulous hemostasis.
-
Muscle and Fascia Closure: The deep muscles (supinator or APL/EPB) are allowed to fall back into their natural position. The deep fascia is then loosely approximated over the muscle bellies to minimize dead space.
-
Subcutaneous and Skin Closure: The subcutaneous layer is closed with absorbable sutures. The skin is closed with staples or non-absorbable sutures. A sterile dressing is applied.
Complications and Management
Despite meticulous technique, complications can arise following the posterior approach to the radius. Early recognition and appropriate management are critical for optimizing patient outcomes.
Common Complications
| Complication | Incidence (Approx.) | Salvage Strategies and Management |
| Radial Shaft Fractures | Displaced or comminuted diaphyseal fractures. | Non-displaced, stable patterns that maintain acceptable radial bow and length. |
| * |
*Specific Conditions Requiring the Approach:
- Distal Radius Fractures with Dorsal Displacement/Comminution: If a volar approach is inadequate for reduction or stabilization of dorsal pathology, a supplementary or primary posterior approach may be considered (though less common).
- Revision Surgery for Implant Related Issues: If a previous volar plate needs removal or adjustment and a dorsal approach offers safer access to the hardware or the bony defect. | |
| Other Conditions | Non-healing wounds or osteomyelitis requiring direct debridement of the radial bone. | Non-critical soft tissue injuries or infections without bone involvement. |
| Previous Surgery | Extensive scarring or failure of previous approaches. | Well-healed previous incisions and successful outcomes from other approaches. |
Management of Complications
- PIN Injury: Initially, conservative management with splinting and close observation is typically employed, as many traumatic neuropathies will spontaneously recover. If recovery does not occur within an expected timeframe (e.g., 3-6 months) or if there is evidence of complete nerve transection, surgical exploration, neurolysis, direct repair, or nerve grafting may be considered. In cases of irreparable injury, tendon transfers (e.g., pronator teres to ECRB/EDC, FCR to EDC) can restore lost motor function.
- Infection: Superficial infections may be managed with oral antibiotics. Deep infections require aggressive surgical debridement, intravenous antibiotics, and potentially implant removal. If the fracture is not healed, a two-stage procedure may be necessary, with initial debridement and external fixation, followed by definitive internal fixation after infection eradication.
- Non-Union/Malunion: Non-unions necessitate revision surgery, often involving plate removal, debridement of fibrous tissue, potentiation of bone healing (e.g., reaming and bone grafting – autograft or allograft), and rigid internal fixation. Malunions with significant functional impairment require corrective osteotomy, often with removal of previous hardware, precise osteotomy, and new internal fixation.
- Implant Failure: Plate breakage or screw pullout generally mandates revision surgery with removal of failed hardware, reassessment of fracture healing, and application of new, more robust fixation (e.g., longer plate, larger screws, supplementary bone graft).
- Compartment Syndrome: Although rare in forearm fractures, vigilance is essential. Clinical signs include severe pain out of proportion to injury, pain on passive stretch of fingers, paresthesia, pallor, and paralysis. Emergent fasciotomy of all forearm compartments is the definitive treatment.
- Complex Regional Pain Syndrome (CRPS): A challenging complication characterized by disproportionate pain, swelling, stiffness, and autonomic dysfunction. Early diagnosis and a multidisciplinary approach involving pain management specialists, physical therapists, and psychological support are crucial. Treatment includes physical therapy, neuropathic pain medications, sympathetic blocks, and sometimes neuromodulation.
Post Operative Rehabilitation Protocols
Postoperative rehabilitation is critical for maximizing functional recovery and minimizing long-term disability. Protocols must be individualized based on the fracture stability, quality of fixation, patient's comorbidities, and surgeon preference.
Early Phase (0-2 Weeks)
- Pain and Edema Control: Initiate multimodal analgesia. Elevate the extremity to reduce swelling.
- Wound Care: Daily wound checks, dressing changes, and monitoring for signs of infection. Suture/staple removal typically at 10-14 days.
- Early Motion (Protected):
- Wrist: Immediate active and passive range of motion (ROM) of the wrist (flexion/extension, radial/ulnar deviation) is encouraged, provided the fixation is stable and does not involve the wrist joint.
- Fingers and Thumb: Aggressive active ROM of all digits, including thumb circumduction, to prevent stiffness.
- Elbow and Shoulder: Active ROM for the elbow and shoulder to prevent stiffness in adjacent joints.
- Immobilization: Depending on surgeon preference and fracture stability, a removable splint or brace may be used for comfort and protection, especially during sleep or high-risk activities. However, static immobilization is generally minimized to prevent stiffness.
Intermediate Phase (2-6 Weeks)
- Gradual Increase in ROM: Progress active and passive ROM of the forearm and wrist. Gentle pronation and supination exercises are initiated, carefully monitoring for pain and resistance. The amount of rotation permitted is often guided by radiographic evidence of early callus formation.
- Light Strengthening: Begin with isometric exercises for wrist extensors and flexors. Progress to light resistance exercises using therapy putty or resistance bands.
- Scar Management: Initiate scar massage and desensitization techniques once the wound is well-healed to prevent adhesions and minimize hypersensitivity.
Advanced Phase (6 Weeks and Beyond)
- Progressive Strengthening: Increase the intensity and range of strengthening exercises for the wrist, forearm, and hand. Focus on grip strength, pinch strength, and functional movements.
- Functional Activities: Incorporate activities of daily living (ADLs) and work-specific tasks.
- Return to Activity: Gradually allow return to recreational activities, sports, and heavy labor as bone healing progresses and strength improves. This phase is guided by radiographic union and clinical assessment of strength and pain. Typically, return to full activity is allowed once radiographic union is evident and there is no pain with provocative testing.
- Monitoring: Continue to monitor for late complications such as non-union, malunion, implant-related issues, or CRPS.
Throughout the rehabilitation process, close collaboration between the surgeon and a hand therapist is essential to tailor the protocol to individual patient needs and progress.
Summary of Key Literature and Guidelines
The posterior approach to the radius, while less frequently utilized than the volar Henry approach for diaphyseal fractures, remains an indispensable tool for orthopedic surgeons. Landmark anatomical descriptions, such as those by Thompson, provide the historical foundation for understanding the dorsal forearm planes. The identification and protection of the posterior interosseous nerve (PIN) are consistently highlighted as the most critical aspects of this approach across the orthopedic literature.
Current AO (Arbeitsgemeinschaft für Osteosynthesefragen) principles emphasize stable internal fixation for radial shaft fractures, advocating for anatomical reduction and restoration of radial bow and length. While the AO-recommended approach for diaphyseal forearm fractures is typically volar, the posterior approach is recognized for specific indications, especially in the proximal and mid-radial diaphysis, or when dealing with dorsal bone loss or comminution.
Research comparing volar versus dorsal plating for radial shaft fractures suggests generally similar outcomes in terms of union rates, though specific fracture patterns may favor one approach over the other. Studies on PIN palsy following dorsal approaches report a variable incidence, typically ranging from 0.5% to 5%, underscoring the necessity for meticulous surgical technique and anatomical awareness. Modern, low-profile locking plates have improved outcomes by providing enhanced biomechanical stability, allowing for earlier mobilization.
Guidelines generally recommend:
* Preoperative imaging, including CT for complex cases.
* Careful patient positioning to optimize exposure and minimize nerve stretch.
* Utilizing the internervous plane between ECRB and EDC.
* Direct visualization and protection of the PIN, particularly during proximal radial exposure.
* Anatomical reduction and stable internal fixation to restore radial geometry.
* Early, protected range of motion to prevent stiffness, guided by fixation stability.
The literature continues to evolve, with ongoing refinements in implant design and surgical techniques. However, the fundamental principles of anatomical understanding, meticulous dissection, and neurovascular protection remain timeless and paramount for safe and successful outcomes when employing the posterior approach to the radius.
Clinical & Radiographic Imaging