ABOS Part I & OITE Orthopedic Review: AC Joint & Sarcoma MCQs | Part 22152
Key Takeaway
This module offers a comprehensive review for ABOS Part I and AAOS OITE exams. It features 20 advanced MCQs on high-yield orthopedic topics, including acromioclavicular joint separations (Rockwood classification, surgical management) and dedifferentiated liposarcoma (diagnosis, staging, treatment, surgical margins). This content is designed to enhance knowledge for orthopedic board exam preparation.
ABOS Part I & OITE Orthopedic Review: AC Joint & Sarcoma MCQs | Part 22152
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 25-year-old male presents to the emergency department after a direct fall onto the superior aspect of his right shoulder during a rugby match. He reports immediate severe pain and inability to lift his arm. On examination, there is marked superior displacement of the distal clavicle, significant tenting of the skin, and a palpable gap between the clavicle and acromion. The deltoid and trapezius muscles appear extensively stripped from the distal clavicle. A clinical image is shown below.
Based on the clinical presentation and the provided image, which Rockwood classification best describes this injury?

Explanation
Correct Answer: E
The patient's presentation, including a direct fall, marked superior displacement of the distal clavicle, significant skin tenting, and extensive stripping of the deltoid and trapezius muscles, is characteristic of a Rockwood Type V AC joint separation. The clinical image further supports the severe superior displacement and soft tissue disruption.
- Type I: Involves a sprain of the AC ligaments without significant disruption or instability.
- Type II: Characterized by a complete tear of the AC ligaments, but intact coracoclavicular (CC) ligaments, leading to partial superior subluxation (typically less than 25% of clavicular height).
- Type III: Involves complete tears of both AC and CC ligaments, with the clavicle displaced superiorly by 25% to 100% of its height, but generally remaining within the sagittal contour of the acromion. Deltoid and trapezius attachments may be intact or minimally disrupted.
- Type IV: Distinguished by complete tears of AC and CC ligaments with posterior displacement of the clavicle into or through the trapezius muscle.
- Type V: Represents a severe injury with complete tears of AC and CC ligaments, marked superior displacement of the clavicle (typically >100% of its height), and extensive stripping of the deltoid and trapezius from the distal clavicle. This matches the clinical vignette and image.
Question 2
A 30-year-old construction worker sustains a Rockwood Type III AC joint separation. Understanding the biomechanics of the AC joint is crucial for treatment planning. Which of the following statements accurately describes the primary role of the coracoclavicular (CC) ligaments in AC joint stability?
Explanation
Correct Answer: B
The coracoclavicular (CC) ligaments (conoid and trapezoid) are the primary vertical stabilizers of the AC joint. They provide approximately 70-80% of the vertical stability, resisting superior translation of the clavicle relative to the acromion. Their disruption, as seen in Type III and higher injuries, leads to significant vertical instability.
- Option A: The AC ligaments (superior, inferior, anterior, posterior) primarily resist anterior and posterior shear forces and contribute to horizontal stability.
- Option C: The AC ligaments contribute the majority of horizontal stability, while the CC ligaments primarily provide vertical stability.
- Option D: The conoid ligament primarily resists superior translation and posterior rotation, while the trapezoid ligament primarily resists superior translation and posterior displacement, and limits horizontal movement. Their roles are more complex than simply anterior/posterior displacement resistance.
- Option E: The coracoacromial ligament forms part of the coracoacromial arch, which prevents superior humeral head migration, but the CC ligaments are distinct and primarily stabilize the AC joint itself.
Question 3
A 40-year-old male presents with a painful right shoulder after falling directly onto his acromion. Radiographs reveal complete tears of both the acromioclavicular (AC) and coracoclavicular (CC) ligaments. The distal clavicle is superiorly displaced by approximately 75% of its height relative to the acromion, but an axillary lateral view confirms it remains within the sagittal contour of the acromion. The deltoid and trapezius muscle attachments appear largely intact. Which Rockwood classification best describes this injury?
Explanation
Correct Answer: B
The description of complete tears of both AC and CC ligaments, with the clavicle superiorly displaced by 25% to 100% of its height and remaining within the sagittal contour of the acromion, is the classic definition of a Rockwood Type III AC joint separation. The largely intact deltoid and trapezius attachments further support this classification.
- Type II: Involves a complete tear of the AC ligaments but intact CC ligaments, with partial superior subluxation (less than 25% displacement).
- Type IV: Characterized by complete tears of AC and CC ligaments, but with posterior displacement of the clavicle into or through the trapezius muscle, which is not described here.
- Type V: Involves complete tears of AC and CC ligaments with marked superior displacement (>100% of clavicular height) and extensive stripping of the deltoid and trapezius muscles, which is more severe than described.
- Type VI: A rare injury involving inferior dislocation of the clavicle beneath the coracoid process or acromion.
Question 4
A 32-year-old professional overhead baseball pitcher sustains a Rockwood Type III AC joint separation in his dominant throwing arm. He is highly motivated to return to elite-level competition as quickly and safely as possible. Given the controversy surrounding Type III management, what is the most appropriate initial treatment recommendation for this patient, according to the provided case material?
Explanation
Correct Answer: B
The case material explicitly states that for Rockwood Type III injuries, operative indications include 'Acute injuries in young, high-demand individuals (e.g., overhead athletes, manual laborers) where functional demands are high and an earlier return to full activity is desired.' A professional overhead baseball pitcher with a dominant arm injury perfectly fits this description, making immediate surgical reconstruction the most appropriate initial recommendation.
- Option A: While non-operative management is an option for Type III injuries, it is generally reserved for sedentary individuals, those with low functional demands, or elderly patients with comorbidities. It is less suitable for a high-demand athlete aiming for a quick return to sport.
- Option C: A trial of non-operative management is a valid approach for some Type III patients, but for a professional athlete, delaying surgical intervention could prolong recovery and potentially compromise their career. The case suggests immediate surgery for this specific profile.
- Option D: Distal clavicle excision (Mumford procedure) is typically performed for symptomatic AC joint arthrosis, often a long-term complication, or sometimes concurrently with reconstruction in chronic cases, not as an initial treatment for an acute Type III separation.
- Option E: While a hook plate is a surgical option, modern literature (as summarized in the case) favors suture-button systems due to lower hardware-related complications and the need for a second surgery for removal of hook plates. More importantly, the question asks for the most appropriate initial treatment recommendation, which is surgery, not a specific hardware choice.
Question 5
During an open reduction and internal fixation of a Rockwood Type V AC joint separation, the surgeon is carefully dissecting to expose the coracoid process for coracoclavicular ligament reconstruction. The anatomical illustration below highlights the relevant structures.
Which critical neurovascular structure is at the highest risk of iatrogenic injury if dissection is not meticulously performed, particularly when drilling tunnels through the base of the coracoid?
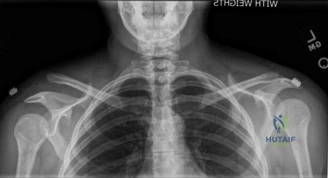
Explanation
Correct Answer: C
The case explicitly states that 'The brachial plexus and subclavian vessels lie inferior and medial to the coracoid process. Extreme caution is required during surgical dissection and drilling around the coracoid to avoid iatrogenic injury.' These structures are immediately adjacent to the coracoid base, making them highly vulnerable during tunnel drilling or aggressive dissection.
- Option A: The axillary nerve is typically located more inferiorly and posteriorly, wrapping around the surgical neck of the humerus, and is less directly at risk during coracoid exposure for AC joint reconstruction.
- Option B: The suprascapular nerve passes through the suprascapular notch and is at risk during procedures involving the scapular neck or glenoid, but not typically during coracoid exposure.
- Option D: The cephalic vein is located more laterally in the deltopectoral groove and, while needing protection, is generally less critical than the major neurovascular bundle medial to the coracoid.
- Option E: The long thoracic nerve runs along the medial border of the scapula and is at risk during procedures involving the chest wall or scapular dissection, not typically during coracoid exposure.
Question 6
A surgeon is performing an AC joint reconstruction using a suture-button system for coracoclavicular ligament reconstruction, as shown in the intraoperative image below. After achieving anatomical reduction of the clavicle, the sutures are tensioned and secured. What is the primary biomechanical principle by which this suture-button construct provides vertical stability to the AC joint?

Explanation
Correct Answer: D
The suture-button system for coracoclavicular (CC) ligament reconstruction works by passing strong suture tapes through tunnels drilled in the clavicle and coracoid. When tensioned, these sutures pull the clavicle inferiorly towards the coracoid process, thereby approximating the two structures and functionally replacing the torn CC ligaments. This restores vertical stability to the AC joint.
- Option A: While AC joint capsular repair may be performed concurrently, the suture-button construct itself is primarily for CC ligament reconstruction and vertical stability, not direct AC ligament repair.
- Option B: Suture-button systems provide dynamic stability, allowing for some micromotion, rather than rigid bony fixation between the clavicle and acromion. Rigid fixation between the clavicle and acromion alone has largely been abandoned due to high failure rates.
- Option C: The goal is to restore the normal anatomical relationship and stability, not to compress the articular surfaces for fusion. Fusion is not a desired outcome for acute AC joint reconstruction.
- Option E: While some historical techniques (e.g., Weaver-Dunn) involved coracoacromial ligament transfer, the suture-button system is a distinct method for CC ligament reconstruction and does not primarily act as a scaffold for other ligament transfers.
Question 7
A 35-year-old male underwent surgical repair for a Rockwood Type V AC joint separation. A post-operative radiograph is provided below.
Based on the radiograph, which of the following statements best describes the primary fixation method used and its main purpose?

Explanation
Correct Answer: C
The post-operative radiograph clearly shows a suture-button construct, characterized by small cortical buttons on the superior aspect of the clavicle and inferior aspect of the coracoid, connected by suture material (not directly visible but implied by the buttons). As detailed in the case, suture-button systems are increasingly popular for coracoclavicular (CC) ligament reconstruction, providing dynamic vertical stability by approximating the clavicle to the coracoid.
- Option A: A clavicle hook plate would appear as a plate with a hook extending under the acromion, which is not seen here. While it provides some stability, it's associated with higher irritation rates.
- Option B: K-wires would appear as thin metallic pins crossing the joint, which are absent in this image. K-wires are generally associated with high rates of migration and infection.
- Option D: An AC joint plate would be positioned directly over the AC joint, typically with screws into both the clavicle and acromion, which is not the primary construct shown.
- Option E: Tension band wiring is typically used for fractures, not primary ligamentous reconstruction of the AC joint in this manner.
Question 8
A 48-year-old male undergoes surgical reconstruction for a Rockwood Type IV AC joint separation using a suture-button system. Six months post-operatively, he presents with persistent pain, instability, and a noticeable superior prominence of the distal clavicle. Radiographs confirm a loss of reduction with significant superior displacement of the clavicle. Which of the following is the most appropriate initial salvage strategy?
Explanation
Correct Answer: C
The patient presents with a clear loss of reduction and persistent instability after initial surgery. The case material explicitly lists 'Loss of Reduction / Re-dislocation' as a common complication (5-20%) and states the salvage strategy is 'Revision surgery with stronger fixation (e.g., additional suture-buttons, allograft augmentation, AC plate). Address technical errors (e.g., inadequate tensioning, improper tunnel placement, premature mobilization). For chronic cases, more robust reconstruction with graft.'
- Option A: While rehabilitation is crucial, it cannot correct a structural loss of reduction. Aggressive therapy without addressing the underlying instability would likely be ineffective and potentially harmful.
- Option B: Observation and NSAIDs are insufficient for a symptomatic loss of reduction, which indicates mechanical failure of the initial repair.
- Option D: Distal clavicle excision (Mumford procedure) is typically reserved for symptomatic AC joint arthrosis or osteolysis, not for acute or subacute loss of reduction of a Type IV injury, which requires restoration of stability.
- Option E: A corticosteroid injection might temporarily mask pain but does not address the mechanical instability caused by the loss of reduction.
Question 9
A 29-year-old patient is 4 weeks post-operative from an AC joint reconstruction with a suture-button system. They are currently in Phase I (Protection & Early Motion) of their rehabilitation protocol. Which of the following activities is strictly contraindicated at this stage to protect the healing repair?
Explanation
Correct Answer: D
Phase I of rehabilitation (4-6 weeks post-op) is focused on protecting the healing repair and maintaining passive range of motion. The guidelines explicitly state to 'avoid cross-body adduction or AC joint compression' and 'No lifting, pushing, pulling, or active shoulder movements against resistance.' Active cross-body adduction directly stresses the AC joint and could jeopardize the repair.
- Option A: Gentle pendulum exercises are initiated around 1-2 weeks post-op and are appropriate for Phase I.
- Option B: Active range of motion exercises for the elbow, wrist, and hand should begin immediately post-op to prevent stiffness.
- Option C: Gentle passive shoulder flexion (0-90 degrees) may be initiated around 2-3 weeks under therapist guidance, making it an appropriate activity for Phase I.
- Option E: Gentle scapular retraction and protraction exercises (non-weight bearing) are encouraged to maintain scapulothoracic mobility.
Question 10
A 55-year-old sedentary patient, 3 years after non-operative management of a Rockwood Type III AC joint separation, presents with chronic, localized pain and crepitus over the AC joint, particularly with overhead activities and reaching across the body. Physical examination reveals tenderness and pain with cross-body adduction. Radiographs demonstrate significant degenerative changes and osteophytes at the AC joint. What is the most appropriate surgical intervention for this patient's current symptoms?
Explanation
Correct Answer: C
The patient's presentation of chronic, localized pain, crepitus, and radiographic evidence of degenerative changes (arthrosis/osteophytes) at the AC joint, 3 years after injury, is characteristic of symptomatic AC joint arthrosis. The case material states that 'Distal clavicle excision (Mumford procedure) may also be performed concurrently if significant AC joint arthritis is present' and 'Distal Clavicle Osteolysis... If refractory symptoms, consider Mumford procedure (distal clavicle excision).' For symptomatic AC joint arthrosis, the Mumford procedure is the definitive surgical treatment.
- Option A: Revision CC ligament reconstruction is indicated for chronic instability or loss of reduction, but the primary issue here is symptomatic arthrosis, not necessarily instability requiring reconstruction.
- Option B: Open reduction and internal fixation with a hook plate is for acute AC joint separations or chronic instability, not for degenerative arthritis of the joint itself.
- Option D: Arthroscopic subacromial decompression addresses impingement in the subacromial space, which is distinct from AC joint arthrosis, although they can coexist. The primary pathology described is AC joint degeneration.
- Option E: While physical therapy is always part of conservative management, for chronic, symptomatic degenerative changes refractory to non-operative care, surgical intervention is often required.
Question 11
A 62-year-old male presents with a slowly enlarging, painless mass in his right posterior thigh, first noticed 18 months prior, with rapid growth in the last 6 months. Physical examination reveals a deep-seated, firm-to-rubbery, 10x8 cm mass with severely limited mobility. Distal neurovascular status is intact. Given these initial findings, which of the following characteristics is the *most* concerning for a soft tissue sarcoma?
Explanation
Correct Answer: D
The most concerning characteristic for a soft tissue sarcoma in this presentation is the deep subfascial location and recent rapid growth. The case explicitly states, 'The presentation of a deep, painless, enlarging soft tissue mass greater than 5 centimeters in an adult must be considered a soft tissue sarcoma until proven otherwise. The historical details, specifically the deep subfascial location and the recent acceleration in growth, raise immediate suspicion for a malignant process.' Deep location, size greater than 5 cm, and rapid growth are classic 'red flags' for malignancy.
Option A (The patient's age of 62 years): While soft tissue sarcomas are more common in older adults, age alone is not the most concerning feature compared to tumor characteristics. Sarcomas can occur at any age.
Option B (The mass being painless): Painless masses are often dismissed, but many sarcomas are indeed painless, especially in their early stages. Pain is a late symptom, often indicating nerve involvement or rapid expansion, but its absence does not rule out malignancy.
Option C (The insidious onset 18 months prior): The insidious onset is common for many soft tissue masses, both benign and malignant. The change in growth pattern (rapid acceleration) is more concerning than the initial slow growth.
Option E (Intact distal neurovascular status): Intact neurovascular status is a reassuring sign regarding limb function but does not diminish the suspicion of malignancy. Sarcomas can grow to a large size by displacing neurovascular structures before causing deficits.
Question 12
Following initial evaluation, an MRI of the right thigh was performed. The image below shows an axial T1-weighted view of the mass. Based on the provided image and the detailed MRI description in the case, which of the following is the most accurate interpretation of the findings?
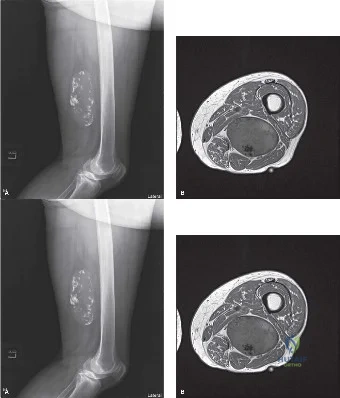
Explanation
Correct Answer: C
The case explicitly describes the MRI findings: 'The majority of the tumor exhibited high signal intensity on T1-weighted images that suppressed on STIR sequences, confirming the presence of macroscopic adipose tissue. However, unlike a simple benign lipoma, the mass demonstrated significant heterogeneity. There were thickened, irregular internal septations (>2 mm) and distinct nodular areas of non-fatty tissue that were isointense to muscle on T1, hyperintense on T2, and demonstrated avid, heterogeneous enhancement following gadolinium administration.' This biphasic appearance, with both fatty and solid enhancing components, is the classic radiological hallmark of an atypical lipomatous tumor or a dedifferentiated liposarcoma.
Option A (A homogeneous mass with low signal intensity on T1, consistent with a myxoid liposarcoma): Myxoid liposarcomas typically lack macroscopic fat on T1 and show very high signal on T2 due to the myxoid matrix, often appearing cyst-like. This does not match the description of high T1 signal from fat.
Option B (A predominantly fatty mass with thin septations (<2mm) and no enhancing non-fatty components, typical of a simple lipoma): While the mass is predominantly fatty, the description of 'thickened, irregular internal septations (>2 mm) and distinct nodular areas of non-fatty tissue that... demonstrated avid, heterogeneous enhancement' rules out a simple lipoma, which would have thin septations and no significant enhancing non-fatty components.
Option D (A highly heterogeneous mass with significant necrosis and hemorrhage, lacking macroscopic fat, characteristic of a pleomorphic liposarcoma): Pleomorphic liposarcomas are typically high-grade, highly heterogeneous, and often lack visible macroscopic fat on MRI. While the mass is heterogeneous, the presence of significant macroscopic fat on T1 makes pleomorphic liposarcoma less likely as the primary radiological diagnosis.
Option E (A mass with serpiginous vascular channels and phleboliths, suggestive of an intramuscular hemangioma): The MRI description does not mention serpiginous vascular channels or phleboliths (signal voids), which are characteristic of hemangiomas. Plain films also did not identify phleboliths.
Question 13
Given the high suspicion for a malignant soft tissue sarcoma based on the MRI findings, an image-guided core needle biopsy was planned. Which of the following is the *most* critical aspect of the biopsy strategy for this patient?
Explanation
Correct Answer: C
The most critical aspect of the biopsy strategy is targeting the solid, enhancing, non-fatty nodular components identified on MRI. The case states: 'Multiple cores were obtained using a 14-gauge coaxial system, specifically targeting the solid, enhancing, non-fatty nodular components identified on the MRI, as these areas harbor the highest grade of malignancy and dictate the overall prognosis and treatment strategy. Biopsying only the fatty components could lead to a false-negative diagnosis of a simple lipoma or under-grading the lesion as merely an atypical lipomatous tumor.'
Option A (Obtaining only fatty tissue samples to confirm the lipomatous nature of the lesion): This is incorrect and dangerous. As explained in the case, biopsying only fatty components risks missing the high-grade dedifferentiated component, leading to under-diagnosis and inappropriate treatment.
Option B (Performing an open incisional biopsy to ensure adequate tissue volume): While incisional biopsies provide more tissue, a well-planned core needle biopsy is generally preferred for extremity sarcomas due to lower morbidity and less risk of tumor seeding, provided it is performed by an experienced musculoskeletal radiologist. The case specifically mentions a percutaneous, ultrasound-guided core needle biopsy.
Option D (Ensuring the biopsy tract is placed perpendicular to the long axis of the limb): The biopsy tract should be placed longitudinally, in line with the planned surgical incision, to ensure it can be completely excised en bloc with the tumor. A perpendicular tract would be difficult to excise completely.
Option E (Avoiding any muscle penetration to minimize post-biopsy hematoma): While minimizing hematoma is important, avoiding any muscle penetration is often impossible for deep intramuscular lesions. The key is to ensure the biopsy tract traverses only the muscle immediately adjacent to the tumor and falls entirely within the planned future surgical excision ellipse, even if it means traversing muscle.
Question 14
Based on the clinical presentation, physical examination, and the MRI findings (including the image provided), which of the following diagnoses is most consistent with Mr. J.A.'s tumor?
Explanation
Correct Answer: C
The clinical and radiological findings are most consistent with a Dedifferentiated Liposarcoma. The case explicitly states: 'The presence of a predominantly fatty tumor with thick septations and nodular, enhancing, non-lipomatous components is the classic radiological hallmark of an atypical lipomatous tumor or a dedifferentiated liposarcoma.' The table in the case further reinforces this, describing DDLPS as having a 'Biphasic appearance. Fatty regions adjacent to prominent, solid, non-fatty, avidly enhancing nodular components.'
Option A (Simple Lipoma): A simple lipoma would be homogeneously fatty with thin septations (<2mm) and no nodular enhancement. This contradicts the MRI findings of thickened septations and enhancing non-fatty nodules.
Option B (Myxoid Liposarcoma): Myxoid liposarcomas typically lack macroscopic fat on T1 and show very high T2 signal due to the myxoid matrix. The MRI here clearly shows macroscopic fat (high T1 signal).
Option D (Intramuscular Hemangioma): Hemangiomas can be heterogeneous but are characterized by serpiginous vascular channels and often phleboliths (signal voids), which were not described in this case's MRI or plain films.
Option E (Pleomorphic Liposarcoma): Pleomorphic liposarcomas are high-grade and typically lack visible macroscopic fat on MRI, presenting as highly heterogeneous, necrotic, and hemorrhagic masses. While this tumor has high-grade features, the prominent macroscopic fat on T1 makes pleomorphic liposarcoma less likely than dedifferentiated liposarcoma, which specifically arises from a fatty precursor.
Question 15
The core needle biopsy revealed a biphasic tumor with areas consistent with Well-Differentiated Liposarcoma and an abrupt transition to a high-grade, pleomorphic spindle cell proliferation. To definitively confirm the diagnosis and distinguish it from other high-grade sarcomas, which molecular finding is the diagnostic hallmark for this tumor?
Explanation
Correct Answer: C
The diagnostic hallmark for the ALT/WDLPS and Dedifferentiated Liposarcoma spectrum is MDM2 and CDK4 gene amplification. The case explicitly states: 'To definitively confirm the diagnosis, molecular profiling utilizing Fluorescence In Situ Hybridization was performed. The tumor cells demonstrated high-level amplification of the MDM2 (Murine Double Minute 2) and CDK4 (Cyclin-Dependent Kinase 4) genes located on chromosome 12q13-15. This molecular signature is the diagnostic hallmark of the ALT/WDLPS and Dedifferentiated Liposarcoma spectrum, distinguishing it definitively from pleomorphic liposarcoma or undifferentiated pleomorphic sarcoma.'
Option A (FUS-DDIT3 translocation (t(12;16))): This translocation is characteristic of Myxoid Liposarcoma.
Option B (EWSR1 rearrangement): This is the defining molecular alteration in Ewing Sarcoma and some other round cell sarcomas.
Option D (INI1 (SMARCB1) deletion): This is characteristic of epithelioid sarcoma and malignant rhabdoid tumors.
Option E (SS18-SSX fusion gene): This fusion gene is the diagnostic hallmark of Synovial Sarcoma.
Question 16
Based on the final histopathological diagnosis of Dedifferentiated Liposarcoma (FNCLCC Grade 2) and the following staging parameters: Tumor (T): >10 cm, deep to superficial fascia (T3); Node (N): No regional lymph node involvement (N0); Metastasis (M): No distant metastasis (M0). What is the correct AJCC stage for this patient's soft tissue sarcoma?
Explanation
Correct Answer: E
The patient's AJCC stage is Stage IIIB. According to the AJCC staging system for Soft Tissue Sarcoma of the Trunk and Extremities (which is detailed in the case):
- T3: Tumor greater than 10 cm and deep to the superficial fascia.
- N0: No regional lymph node involvement.
- M0: No distant metastasis.
- G2: FNCLCC Grade 2 (Intermediate-to-High Grade).
Combining these factors:
- T3 (large, deep)
- N0 (no nodal spread)
- M0 (no distant mets)
- G2 (intermediate/high grade)
A T3, N0, M0, Grade 2 tumor corresponds to Stage IIIB. Stage IIIB indicates a large, deep, intermediate-to-high-grade tumor with a significant risk of both local recurrence and distant hematogenous metastasis.
The other options represent lower stages that do not match the combination of a large (T3) and intermediate-to-high grade (G2) tumor.
Question 17
The multidisciplinary tumor board recommended neoadjuvant external beam radiation therapy followed by wide surgical resection. Which of the following is a primary oncologic advantage of neoadjuvant (preoperative) radiation therapy for this patient's large, deep, high-grade dedifferentiated liposarcoma?
Explanation
Correct Answer: C
A primary oncologic advantage of neoadjuvant radiation therapy is that it treats a smaller target volume and potentially sterilizes the reactive pseudocapsule, making surgical resection easier. The case states: 'Neoadjuvant radiation therapy (typically 50 Gy in 25 fractions) offers several distinct oncologic advantages: it treats a smaller target volume, potentially sterilizes the reactive pseudocapsule, thickens the tumor pseudocapsule making surgical resection easier, and requires a lower total dose, thereby reducing long-term tissue fibrosis and joint stiffness.'
Option A (Significantly lower risk of acute postoperative wound complications compared to adjuvant radiation): This is incorrect. The case explicitly mentions: 'However, as demonstrated by the landmark O'Sullivan trial, neoadjuvant radiation carries a significantly higher risk of major acute postoperative wound complications (up to 35%) compared to adjuvant radiation.'
Option B (Requires a higher total radiation dose, leading to better tumor kill): This is incorrect. Neoadjuvant radiation typically uses a lower total dose (e.g., 50 Gy) compared to adjuvant radiation (e.g., 60-66 Gy) because the tumor is still in situ, allowing for a smaller, more focused field. The goal is to downstage and sterilize, not necessarily to deliver a higher total dose.
Option D (Allows for immediate surgical resection without delay): This is incorrect. Neoadjuvant radiation delays surgery by several weeks (typically 5-6 weeks for treatment plus a recovery period), which is a known drawback.
Option E (It is the only effective method to preserve the sciatic nerve in such cases): While neoadjuvant radiation can help with local control and potentially facilitate nerve-sparing surgery, it is not the only effective method. Surgical technique (epimesial dissection) is also crucial, and nerve preservation depends on the extent of tumor invasion, not solely on radiation.
Question 18
During the surgical resection, the tumor pseudocapsule was found to be densely adherent to the epineurium of the sciatic nerve. The orthopedic oncologist performed an epimesial dissection, sharply peeling the epineurium away from the intact sciatic nerve fascicles, leaving the epineurium attached to the tumor specimen. What type of surgical margin does this technique represent at the interface with the sciatic nerve?
Explanation
Correct Answer: B
An epimesial dissection, where the outermost layer of the nerve sheath (epineurium) is left attached to the tumor specimen, constitutes a Marginal (R1) margin at that specific anatomical location. The case states: 'This constitutes a planned marginal (R1) resection at this specific anatomical location. The rationale is that the combination of this marginal resection and the neoadjuvant radiation therapy provides excellent local control rates while preserving limb function, avoiding the devastating morbidity of a complete sciatic nerve resection.'
- A. Wide (R0) margin: This implies a resection with a cuff of uninvolved healthy tissue (typically >1 cm) around the entire tumor, with no microscopic tumor at the margin. While the overall goal is R0, at the nerve interface, this was not achieved due to adherence.
- C. Intralesional (R2) margin: This means gross tumor was left behind, or the tumor was cut through. This is not the case here, as the nerve fascicles were preserved, and the epineurium was removed with the tumor.
- D. Amputation margin: This refers to the margin of an amputation, which was avoided in this limb-sparing procedure.
- E. Contaminated margin: This term is not a standard oncologic margin classification in the same way as R0, R1, R2. It might refer to a situation where tumor cells are spilled, but the epimesial dissection is a controlled, planned technique.
Question 19
Following the wide surgical resection and epimesial dissection of the sciatic nerve, the patient underwent postoperative management. Given the history of neoadjuvant radiation therapy, which of the following is the *most* critical aspect of acute postoperative wound management?
Explanation
Correct Answer: C
The most critical aspect of acute postoperative wound management, especially after neoadjuvant radiation, is meticulous drain management, leaving drains in until output is consistently low, to prevent seroma and wound dehiscence. The case highlights this: 'Drain management is critical. The closed-suction drains were left in place until the output decreased to less than 30 cc per 24-hour period for two consecutive days. In irradiated fields, lymphatic leakage can be prolonged, and premature drain removal frequently leads to seroma formation and subsequent wound dehiscence.'
Option A (Early aggressive range of motion exercises to prevent stiffness): While rehabilitation is important, early aggressive range of motion could jeopardize wound healing, especially in an irradiated field prone to dehiscence. Rehabilitation is phased and carefully progressed.
Option B (Immediate removal of surgical drains within 24 hours to reduce infection risk): This is incorrect. Premature drain removal in irradiated fields is a major cause of seroma and wound complications, as lymphatic leakage can be prolonged. Drains are kept in longer than usual.
Option D (High-dose systemic corticosteroids to reduce inflammation and promote wound healing): Corticosteroids can impair wound healing and increase infection risk, especially in the context of surgery and radiation. They are generally not used routinely for this purpose.
Option E (Strict bed rest for the first week to minimize stress on the wound): While activity is restricted, strict bed rest is generally avoided due to the risk of DVT and other complications. Early mobilization within safe limits is encouraged, along with DVT prophylaxis.
Question 20
A 45-year-old male presents with a deep, painless thigh mass. MRI shows a predominantly fatty lesion with thin septations (<2mm) and no enhancing non-fatty components. A biopsy confirms mature adipocytes with no atypia. In contrast, Mr. J.A.'s tumor was a Dedifferentiated Liposarcoma. Which of the following features *most* reliably distinguishes Mr. J.A.'s tumor from the 45-year-old male's lesion?
Explanation
Correct Answer: D
The features that most reliably distinguish Mr. J.A.'s Dedifferentiated Liposarcoma from the 45-year-old male's lesion (which sounds like a simple lipoma or possibly an atypical lipomatous tumor without dedifferentiation) are the identification of thickened, irregular septations and enhancing non-fatty nodules on MRI, along with MDM2/CDK4 amplification. The case explicitly states that these MRI findings are the 'classic radiological hallmark' of ALT/WDLPS/DDLPS, and MDM2/CDK4 amplification is the 'diagnostic hallmark' distinguishing it from other sarcomas and benign lesions.
Option A (The presence of a deep-seated mass): Both simple lipomas and liposarcomas can be deep-seated (intramuscular). This alone does not distinguish them.
Option B (The absence of pain): Both benign lipomas and many liposarcomas (including Mr. J.A.'s) can be painless. Pain is not a reliable distinguishing factor.
Option C (The presence of macroscopic fat on MRI): Both simple lipomas and well-differentiated/dedifferentiated liposarcomas contain macroscopic fat and would show high signal on T1-weighted images. This feature alone does not differentiate them.
Option E (The patient's age at presentation): While liposarcomas are more common in older adults, and the 45-year-old is younger than Mr. J.A. (62), age is not a definitive diagnostic criterion. Both benign and malignant lesions can occur across a wide age range.
Question 21
During surgical reconstruction of a chronic Type V AC joint separation, the surgeon aims to restore normal clavicular translation. The conoid ligament is primarily responsible for resisting which of the following forces?
Explanation
Question 22
A 14-year-old boy is diagnosed with high-grade osteosarcoma of the distal femur. He undergoes 10 weeks of neoadjuvant chemotherapy. According to the Huvos grading system, a 'good response' to chemotherapy is defined as what percentage of tumor necrosis on the resection specimen?
Explanation
Question 23
A 28-year-old male competitive weightlifter complains of an aching right shoulder pain, exacerbated by bench pressing and cross-body adduction. Radiographs show subchondral cystic changes and widening of the AC joint. If conservative management fails, which of the following is the most appropriate surgical step?
Explanation
Question 24
A 25-year-old female presents with a slow-growing, deep soft tissue mass in her popliteal fossa. Biopsy reveals a biphasic tumor with both epithelial and spindle cell components. Which of the following chromosomal translocations is most characteristic of this tumor?
Explanation
Question 25
A 35-year-old mountain biker falls off his bike and sustains a shoulder injury. Examination reveals a painful, non-reducible distal clavicle that is impaled posteriorly into the trapezius fascia. According to the Rockwood classification, what type of injury is this?
Explanation
Question 26
A 32-year-old female presents with a painless mass behind her knee. Radiographs reveal a densely ossified mass attached to the posterior cortex of the distal femur by a broad stalk. A 'string sign' is faintly visible. What is the most common histologic grade and typical management for this lesion?
Explanation
Question 27
A 29-year-old male undergoes a free tendon graft reconstruction of the coracoclavicular ligaments. Six weeks postoperatively, he reports a sudden pop after lifting a heavy box. Radiographs show recurrent superior clavicular displacement and an avulsion fracture of the coracoid base. What is the most likely technical cause of this complication?
Explanation
Question 28
A 10-year-old boy presents with a diaphyseal femur lesion showing a permeative, 'onion-skin' periosteal reaction. Biopsy reveals sheets of small round blue cells. The diagnostic translocation for this tumor primarily involves the fusion of the EWS gene with which of the following?
Explanation
Question 29
When performing an anatomic reconstruction of the coracoclavicular ligaments, accurate tunnel placement is crucial. The normal footprint of the conoid ligament on the clavicle is located approximately how far medial to the AC joint line?
Explanation
Question 30
A 55-year-old man has a biopsy-proven Grade 2 (intermediate) chondrosarcoma of the proximal humerus. There is endosteal scalloping of >2/3 of the cortical thickness and soft tissue extension on MRI. What is the standard definitive treatment?
Explanation
Question 31
A 28-year-old professional baseball pitcher sustains a Rockwood Type III AC joint separation of his throwing arm. After 3 months of nonoperative management, he still experiences severe pain and subjective weakness during throwing motions, with prominent scapular dyskinesia. What is the most appropriate next step in management?
Explanation
Question 32
A 16-year-old boy presents with knee pain. Radiographs show a purely lytic, expansile lesion in the distal femoral metaphysis with a pathologic fracture. MRI reveals multiple fluid-fluid levels. Biopsy demonstrates high-grade malignant cells producing osteoid. What is the most appropriate initial treatment?
Explanation
Question 33
A 40-year-old male sustains a severe shoulder trauma in a high-speed collision. Clinical examination shows a flattened shoulder contour, and radiographs demonstrate the distal clavicle is positioned inferior to the coracoid process, posterior to the conjoined tendon. Which Rockwood classification type is this injury?
Explanation
Question 34
A 42-year-old male complains of chronic hip pain. Radiographs reveal an epiphyseal lytic lesion in the proximal femur with central calcifications. Histology demonstrates cells with abundant clear cytoplasm and distinct boundaries. What is the most likely diagnosis?
Explanation
Question 35
A patient presents with an indeterminate AC joint injury. Routine AP and scapular Y views are inconclusive. Which of the following radiographic views is most useful to specifically evaluate posterior displacement of the clavicle relative to the acromion (Rockwood Type IV)?
Explanation
Question 36
A 20-year-old female presents with a mass on the anterior tibial diaphysis. Imaging reveals a predominately cartilaginous matrix tumor resting on the cortex surface, with 'hair-on-end' spicules but no medullary involvement. What is the typical histologic grade of this tumor?
Explanation
Question 37
In a biomechanical study evaluating AC joint stability, sequential sectioning of ligaments is performed. Sectioning of the superior AC ligament primarily increases which of the following translations of the distal clavicle?
Explanation
Question 38
A 60-year-old female treated for breast cancer with radiation 12 years ago presents with a rapidly enlarging mass in her ipsilateral scapula. Biopsy confirms high-grade osteosarcoma. Which of the following statements regarding radiation-induced sarcomas is true?
Explanation
Question 39
The classic Weaver-Dunn procedure for chronic AC joint instability involves resection of the distal clavicle and transfer of which ligament to the distal clavicle?
Explanation
Question 40
A 65-year-old male presents with a destructive, osteolytic lesion in his proximal humerus. A core needle biopsy is obtained. Immunohistochemistry is strongly positive for cytokeratin and negative for vimentin. What is the most likely diagnosis?
Explanation
Question 41
A 28-year-old professional hockey player undergoes coracoclavicular (CC) ligament reconstruction for a chronic Type V acromioclavicular (AC) joint separation. To anatomically recreate the CC ligaments, the surgeon must place drill holes in the clavicle. Which of the following best describes the anatomic location of the conoid and trapezoid ligaments?
Explanation
Question 42
A 14-year-old boy presents with right thigh pain and a low-grade fever. Radiographs reveal a permeative diaphyseal lesion with an 'onion-skin' periosteal reaction. A biopsy confirms small round blue cells. Which of the following chromosomal translocations is most characteristic of this tumor?
Explanation
Question 43
A 35-year-old male falls on the point of his shoulder. Clinical examination suggests an AC joint injury, but standard AP views of the shoulder show overlapping structures. Which radiographic view is most appropriate to isolate and evaluate the AC joint without scapular spine superimposition?
Explanation
Question 44
A 24-year-old female presents with a slowly enlarging, painless mass about her knee. MRI reveals a deep soft tissue mass adjacent to the joint. Histology demonstrates a biphasic pattern of spindle cells and epithelial cells. This specific sarcoma has an unusually high propensity for metastasis to which of the following locations?
Explanation
Question 45
A 45-year-old male falls directly on his shoulder and presents with intense pain. The axillary lateral radiograph reveals that the distal clavicle is displaced posteriorly into the trapezius muscle. Which Rockwood classification type is this injury?
Explanation
Question 46
When planning a biopsy for a suspected extremity soft tissue sarcoma, which of the following principles is most critical for preserving limb-salvage surgical options?
Explanation
Question 47
During a distal clavicle excision (Mumford procedure) for AC joint osteoarthritis, the surgeon must be careful not to resect too much bone. Resecting more than what length of the distal clavicle significantly increases the risk of anterior-posterior instability?
Explanation
Question 48
A 55-year-old male presents with a large, destructive lesion in his right ilium with stippled 'popcorn' calcifications on plain film. Biopsy confirms a grade II conventional chondrosarcoma. Which of the following is the most appropriate primary treatment?
Explanation
Question 49
A surgeon is repairing an acute AC joint separation using a suspensory cortical button construct placed through the clavicle and coracoid. Postoperatively, the patient experiences a sudden loss of reduction and anterior shoulder pain. Which of the following is the most common hardware-related mode of failure for this specific technique?
Explanation
Question 50
A 35-year-old patient undergoes resection of a myxoid liposarcoma of the thigh. In addition to the standard staging CT of the chest, which of the following imaging modalities is highly recommended for staging this specific subtype of soft tissue sarcoma?
Explanation
Question 51
While testing the stability of the acromioclavicular joint, you note significant anterior-posterior (A-P) translation but normal superior-inferior stability. Which ligamentous structure is primarily injured?
Explanation
Question 52
A 15-year-old male is diagnosed with high-grade osteosarcoma of the distal femur. He undergoes neoadjuvant chemotherapy. Which of the following histologic findings in the resected tumor specimen is the strongest predictor of long-term overall survival?
Explanation
Question 53
A 22-year-old competitive weightlifter presents with insidious onset of right shoulder pain, exacerbated by the bench press and cross-body adduction. Radiographs show subchondral cysts, osteopenia, and microfractures of the distal clavicle. What is the initial treatment of choice for this condition?
Explanation
Question 54
A 42-year-old male presents with a painful lytic lesion in the epiphysis of the proximal humerus. Biopsy demonstrates malignant cells with abundant clear cytoplasm and distinct cell membranes, mixed with areas of chondroid matrix. This entity is most likely to be confused radiographically with which of the following benign lesions?
Explanation
Question 55
When performing an anatomic coracoclavicular ligament reconstruction using a tendon graft, restoring the functional biomechanics of the joint requires routing the graft properly. Which of the following best describes the structural restraint roles of the native CC ligaments?
Explanation
Question 56
A 20-year-old presents with a rapidly enlarging mass of the proximal tibia. Radiographs show a lytic, expansile lesion. MRI demonstrates multiple fluid-fluid levels, highly suggestive of an aneurysmal bone cyst (ABC). However, core biopsy reveals high-grade malignant cells producing a lacy, osteoid matrix. What is the diagnosis?
Explanation
Question 57
A 30-year-old male sustains a severe AC joint injury after a high-velocity motorcycle crash. On examination, his shoulder is flattened, and the acromion is prominent. Radiographs reveal a Rockwood Type VI separation. Which concomitant clinical finding must the examiner have a high index of suspicion for?
Explanation
Question 58
Which of the following describes the most common soft tissue sarcoma occurring in patients older than 50 years, which historically presented as a diagnosis of exclusion and consists of a storiform, pleomorphic cellular pattern?
Explanation
Question 59
A 33-year-old laborer undergoes delayed surgical reconstruction of a Rockwood Type V AC joint injury that occurred 4 months ago. Why is a biologic graft (e.g., semitendinosus allograft) favored over isolated non-absorbable suture fixation for this chronic injury?
Explanation
Question 60
A 65-year-old breast cancer survivor, who underwent lumpectomy and radiation therapy 10 years ago, presents with a new, rapidly growing, painful mass in the irradiated scapula. Biopsy demonstrates high-grade osteosarcoma. Which of the following features is most typical of radiation-induced sarcomas?
Explanation
Question 61
In evaluating the stability of the acromioclavicular (AC) joint, which of the following structures serves as the primary restraint to anterior-posterior translation of the distal clavicle?
Explanation
Question 62
A 24-year-old male presents with a slowly enlarging, painless mass about his left knee. Biopsy reveals a biphasic tumor containing both spindle and epithelial cells. Which of the following chromosomal translocations is highly characteristic of this lesion?
Explanation
Question 63
A 28-year-old cyclist falls directly onto his shoulder. Clinical examination reveals a prominent distal clavicle. To accurately diagnose a Rockwood type IV acromioclavicular joint injury, which radiographic view is most critical?
Explanation
Question 64
A 15-year-old boy with high-grade osteosarcoma of the distal femur completes neoadjuvant chemotherapy and undergoes surgical resection. What percentage of tumor necrosis is the standard threshold to classify the tumor as having a 'good response' to chemotherapy?
Explanation
Question 65
During a coracoclavicular ligament reconstruction, anatomic placement of the grafts is essential. Which of the following accurately describes the anatomic insertion of the conoid ligament on the clavicle relative to the trapezoid ligament?
Explanation
Question 66
A 12-year-old girl presents with a destructive diaphyseal lesion of the fibula with a periosteal 'onion-skin' reaction. Immunohistochemistry is strongly positive for CD99. What is the most likely fusion gene associated with this malignancy?
Explanation
Question 67
A 34-year-old competitive weightlifter complains of a 6-month history of localized right acromioclavicular joint pain, worsened by bench presses. Radiographs reveal widening of the AC joint and subchondral cysts in the distal clavicle. If conservative management fails, what is the most appropriate surgical intervention?
Explanation
Question 68
A 45-year-old man undergoes excision of a deep intramuscular thigh mass. Histology demonstrates a 'chicken-wire' capillary network and lipoblasts. Which of the following genetic alterations is diagnostic for this tumor?
Explanation
Question 69
A 25-year-old office worker sustains a Rockwood Type III acromioclavicular joint separation. Compared to acute operative repair, nonoperative management of this injury is most consistently associated with which of the following outcomes?
Explanation
Question 70
The coracoclavicular (CC) ligaments are the primary restraints to superior translation of the distal clavicle. Regarding their anatomy and biomechanics, which of the following statements is true?
Explanation
Question 71
A 14-year-old boy presents with a painful mass in his distal femur. Radiographs reveal a sunburst periosteal reaction and Codman's triangle. A biopsy is planned. Which of the following principles is critical when performing a biopsy for a suspected musculoskeletal sarcoma?
Explanation
Question 72
A 32-year-old cyclist falls directly on his right shoulder and is diagnosed with a Rockwood Type IV acromioclavicular (AC) joint injury. Which of the following best describes the anatomical displacement characteristic of this injury?
Explanation
Question 73
A 16-year-old girl with high-grade conventional osteosarcoma of the proximal tibia undergoes neoadjuvant chemotherapy followed by limb-salvage surgery. Which of the following factors is the most important predictor of her overall survival?
Explanation
Question 74
During surgical reconstruction of a chronic acromioclavicular joint dislocation, a surgeon plans to drill tunnels in the clavicle to recreate the coracoclavicular (CC) ligaments. To accurately reproduce the native anatomy, the medial tunnel (for the conoid) and lateral tunnel (for the trapezoid) should be placed at what respective distances from the distal end of the clavicle?
Explanation
Question 75
A 10-year-old boy presents with thigh pain and fever. Radiographs show a permeative, diaphyseal lesion in the femur with an onion-skin periosteal reaction. A biopsy confirms small round blue cells. Which of the following genetic translocations is most characteristic of this tumor?
Explanation
Question 76
A 28-year-old female presents with a slowly enlarging, painful mass on the dorsal aspect of her foot. Radiographs reveal soft tissue calcifications. Biopsy demonstrates a biphasic tumor with both epithelial and spindle cells. What is the most common route of metastasis for this specific sarcoma, and to which organ?
Explanation
Question 77
A patient undergoes a Weaver-Dunn procedure for a chronic Type V acromioclavicular (AC) joint separation. This procedure involves detaching a ligament from its native insertion and transferring it to the distal clavicle. Which ligament is transferred, and how does its biomechanical strength compare to the intact native coracoclavicular (CC) ligaments?
Explanation
Question 78
A 55-year-old male presents with a large, painful, destructive lesion in his proximal humerus. Biopsy confirms a high-grade conventional chondrosarcoma. Which of the following is the most appropriate definitive management?
Explanation
Question 79
When obtaining a Zanca view to radiographically evaluate an acute acromioclavicular (AC) joint injury, what is the proper positioning of the X-ray beam?
Explanation
None
