Pediatric Lateral Condyle Fracture: The Critical Role of Internal Oblique Radiographs
Key Takeaway
The internal oblique radiograph is crucial for diagnosing pediatric lateral condyle fractures because standard AP/lateral views often obscure subtle displacement or articular involvement due to developing ossification centers. This specialized view clearly delineates the fracture line, extent of displacement, rotation, and articular surface involvement, enabling accurate Salter-Harris classification and guiding optimal management decisions.
Introduction and Epidemiology
A 7-year-old male presented to the emergency department following a fall from a monkey bar apparatus at school. He reports falling directly onto his outstretched right hand with his elbow in extension. The patient immediately experienced acute pain, swelling, and refusal to move the right elbow. There was no reported loss of consciousness or associated head, neck, or other limb injuries. His parents reported no significant past medical history, no known allergies, and he was up-to-date on immunizations. No history of bleeding disorders or bone fragility was noted. He is right-hand dominant.
Upon initial assessment, the patient was alert, cooperative, and in moderate distress due to pain.
- Inspection: Marked diffuse swelling was evident over the right elbow, predominantly on the lateral aspect, with subtle ecchymosis. There was no obvious gross deformity, skin tenting, or open wounds. The elbow was held in a position of slight flexion (approximately 30 degrees).
- Palpation: Significant tenderness was elicited over the lateral epicondyle and supracondylar region of the distal humerus. Palpation of the radial head and olecranon was also painful but less localized. No crepitus was appreciated without causing undue discomfort.
- Range of Motion (ROM): Active ROM was severely restricted and painful. Passive ROM was attempted gently, revealing an arc of flexion from approximately 30 degrees to 80 degrees, with significant pain at the end ranges. Supination and pronation were similarly painful and limited.
- Neurological Assessment: A thorough neurological examination revealed intact motor and sensory function in the radial, ulnar, and median nerve distributions. Specifically, the patient could extend the wrist and fingers (radial nerve), abduct and adduct the fingers (ulnar nerve), and oppose the thumb and flex the wrist/fingers (median nerve). No paresthesias or dysesthesias were reported.
- Vascular Assessment: The radial and ulnar pulses were bilaterally palpable, strong, and symmetrical. Capillary refill was brisk (<2 seconds) in all digits of the right hand. The limb was warm and well-perfused. No compartment syndrome signs were present.
Initial radiographic evaluation of the right elbow consisted of standard anterior-posterior (AP) and lateral views.
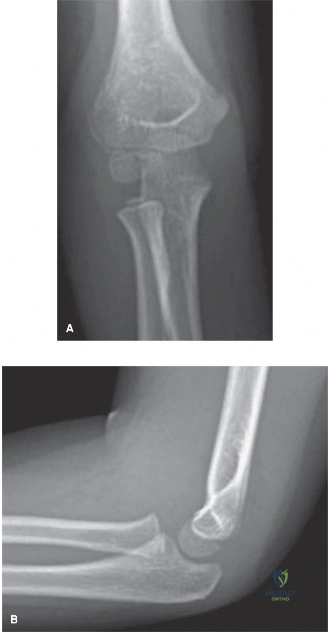
- AP View: The AP radiograph demonstrated diffuse soft tissue swelling and a subtle lucency suggesting a fracture line originating from the lateral metaphysis of the distal humerus. However, the extent of displacement and articular involvement, particularly the physeal extension, was not clearly delineated due to superimposition of the distal humeral epiphysis and the developing ossification centers. The lucency appeared to extend towards the capitellum.
- Lateral View: The lateral view revealed an anterior fat pad sign, indicating an intra-articular effusion. The fracture line was difficult to discern precisely on this view, but the capitellum and lateral condyle appeared to be slightly displaced posteriorly relative to the humeral shaft. However, the true degree of displacement, rotation, and articular fragment size remained equivocal.
Given the clinical suspicion of a lateral condyle fracture and the ambiguous findings on standard views, an internal oblique radiograph of the elbow was obtained. This view is crucial in pediatric elbow trauma, particularly for assessing lateral condyle fractures, as it projects the capitellum and trochlea more clearly, revealing the true extent of the fracture line and any subtle displacement or rotation that might be missed on standard projections.
Internal Oblique View: The internal oblique view unequivocally demonstrated a Salter-Harris Type IV fracture of the lateral condyle of the humerus. The fracture line was clearly visible, extending from the lateral metaphysis, through the physis, and into the articular surface, confirming a displaced intra-articular fracture requiring surgical intervention.
This clinical vignette perfectly illustrates the diagnostic nuances of pediatric lateral condyle fractures. Representing approximately 15 to 20 percent of all pediatric elbow fractures, lateral condyle fractures are the second most common elbow fracture in children, surpassed only by supracondylar humerus fractures. The peak incidence occurs between 6 and 10 years of age. Unlike supracondylar fractures, which are typically extra-articular, lateral condyle fractures are inherently intra-articular and involve the physis. This anatomical reality dictates a highly vigilant approach to diagnosis and management, as missed or inadequately treated fractures carry a high risk of nonunion, malunion, progressive cubitus valgus, and subsequent tardy ulnar nerve palsy.
Surgical Anatomy and Biomechanics
A profound understanding of the developing pediatric elbow is mandatory for the orthopedic surgeon managing lateral condyle fractures. The distal humerus develops from four distinct secondary ossification centers, which appear in a predictable sequence often remembered by the mnemonic CRITOE (Capitellum, Radial head, Internal epicondyle, Trochlea, Olecranon, External epicondyle). The capitellum is the first to ossify, typically between 1 and 2 years of age, while the external (lateral) epicondyle is the last, appearing between 10 and 12 years.
Ossification Sequence and Vascularity
At the typical age of injury (6 to 10 years), the lateral condyle is largely cartilaginous. The fracture fragment invariably includes the lateral metaphysis, the entire capitellum, and a variable portion of the lateral trochlear ridge. Because the majority of the fragment is radiolucent cartilage, standard radiographs consistently underestimate the true size of the fractured segment.
The vascular anatomy of the lateral condyle is critical to surgical decision-making. The capitellum receives its primary blood supply from posterior end-arteries that enter the non-articular posterior aspect of the lateral condyle. There is no significant collateral circulation. Consequently, aggressive posterior soft tissue dissection during open reduction risks devascularizing the fragment, leading to avascular necrosis (AVN) of the capitellum, often manifesting radiographically as a "fishtail" deformity.
Fracture Mechanics and Classification
Two primary mechanisms of injury have been proposed. The "pull-off" theory suggests that a varus force applied to an extended elbow causes the lateral collateral ligament complex and the common extensor origin to avulse the lateral condyle. The "push-off" theory posits that a fall on an outstretched hand transmits an axial load through the radius, driving the radial head directly into the capitellum and shearing it off.
Fractures are historically categorized using the Milch classification, which is based on the location of the fracture line relative to the trochlear groove.
* Milch Type I: The fracture line courses lateral to the trochlear groove (Salter-Harris IV). The lateral trochlear ridge remains attached to the intact medial humerus, preserving elbow stability.
* Milch Type II: The fracture line extends into the apex of the trochlear groove (Salter-Harris II or IV). This destabilizes the radius and ulna relative to the humerus, allowing lateral translation of the forearm. Milch Type II fractures are significantly more common.
More clinically relevant for treatment algorithms is the Jakob classification, which evaluates the degree of displacement and the integrity of the cartilaginous articular hinge.
* Jakob Stage 1: Nondisplaced fracture (<2 mm) with an intact articular surface.
* Jakob Stage 2: Displaced fracture (>2 mm) with an intact articular hinge, but the metaphyseal fragment is displaced laterally.
* Jakob Stage 3: Completely displaced and rotated fracture. The articular hinge is torn, and the pull of the common extensor musculature rotates the fragment in multiple planes (typically laterally, proximally, and posteriorly).
Indications and Contraindications
The management of pediatric lateral condyle fractures hinges entirely on the precise measurement of displacement and the assessment of articular congruity. Because the fracture is intra-articular and bathed in synovial fluid, and because the common extensor muscles exert continuous deforming forces, nonoperative management is reserved strictly for truly nondisplaced fractures.
| Parameter | Operative Management | Non Operative Management |
|---|---|---|
| Displacement | > 2 mm of displacement on any radiographic view | < 2 mm of displacement on all views |
| Articular Hinge | Disrupted or questionable integrity | Intact cartilaginous hinge |
| Joint Congruity | Step-off present or fragment rotated | Perfectly congruent joint surface |
| Fracture Age | Acute or subacute (< 3 weeks) | Acute fractures meeting criteria above |
| Late Presentations | Symptomatic nonunion, progressive valgus | Asymptomatic established nonunion (relative) |
Operative intervention is strongly indicated for any fracture demonstrating greater than 2 mm of displacement. Even in fractures with exactly 2 mm of displacement, many surgeons favor closed reduction and percutaneous pinning (CRPP) or open reduction and internal fixation (ORIF) due to the high rate of late displacement in cast immobilization.
Contraindications to immediate surgical intervention include active local soft tissue infection, severe soft tissue compromise (such as massive blistering where surgical incisions would traverse compromised skin), or a medically unstable polytrauma patient. In cases of delayed presentation (greater than 3 to 4 weeks) where the fracture has begun to consolidate in a malunited position, aggressive open reduction is relatively contraindicated due to the exceedingly high risk of avascular necrosis resulting from the extensive soft tissue stripping required to mobilize the fragment.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning requires high-quality orthogonal imaging. The standard AP and lateral views are often insufficient due to the complex three-dimensional anatomy of the developing elbow and the superimposition of the radial head over the capitellum on the lateral view.
Advanced Imaging and the Internal Oblique Radiograph

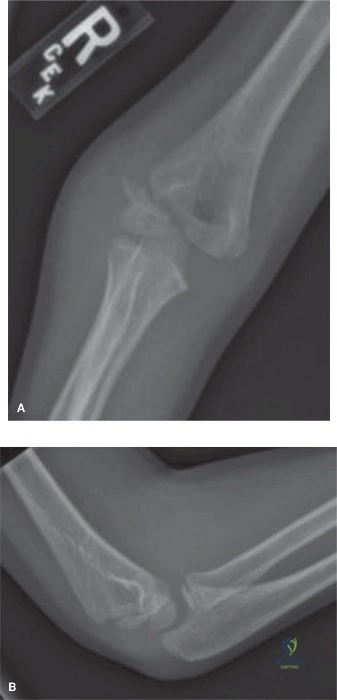
The internal oblique radiograph is the definitive imaging modality for assessing the true displacement of a lateral condyle fracture. The view is obtained by internally rotating the arm 45 degrees. This specific projection places the lateral condyle in profile and removes the superimposition of the ulna and radial head.
The internal oblique view is highly sensitive for detecting gap formation at the posterior aspect of the lateral metaphysis, which is often the first sign of displacement. If the fracture gap measures greater than 2 mm on the internal oblique view, the articular hinge is likely compromised, and surgical fixation is warranted. In rare cases where radiographs remain equivocal, magnetic resonance imaging (MRI) or an arthrogram can be utilized to directly visualize the cartilaginous articular surface, though these are rarely necessary if high-quality internal oblique views are obtained.
Operating Room Setup
The patient is positioned supine on the operating table. The affected upper extremity is placed on a radiolucent hand table. A sterile tourniquet is applied high on the arm to ensure a bloodless surgical field, which is critical for identifying the cartilaginous articular surfaces. The C-arm fluoroscopy unit should be positioned to enter from the head of the table or parallel to the hand table, allowing for unencumbered AP, lateral, and oblique imaging throughout the procedure.
Detailed Surgical Approach and Technique
While closed reduction and percutaneous pinning can be attempted for Jakob Stage 2 fractures (2-4 mm displacement with an intact hinge), open reduction and internal fixation (ORIF) is the gold standard for any fracture with a disrupted articular hinge or rotation (Jakob Stage 3).
The Lateral Approach
The surgical approach utilizes a direct lateral incision, exploiting the internervous plane between the anconeus (innervated by the radial nerve) and the extensor carpi ulnaris (innervated by the posterior interosseous nerve).
- Incision: A 3 to 5 cm longitudinal incision is made centered over the lateral epicondyle, extending proximally along the supracondylar ridge and distally toward the radial head.
- Superficial Dissection: Subcutaneous tissues are divided. The deep fascia is incised in line with the skin incision.
- Identifying the Interval: The Kocher interval is identified. The common extensor origin (extensor carpi radialis brevis and extensor digitorum communis) is retracted anteriorly, while the anconeus and triceps are retracted posteriorly.
- Joint Arthrotomy: The joint capsule is incised anteriorly. It is imperative to direct the dissection anteriorly to expose the radiocapitellar joint. The posterior aspect of the lateral condyle must not be stripped of its soft tissue attachments, as this houses the critical blood supply to the capitellum.
Fracture Reduction and Fixation
Once the joint is exposed, the fracture hematoma is irrigated and meticulously cleared using a curette or freer elevator. The metaphyseal fracture edges are identified. The articular surface is inspected directly.
Reduction is achieved by manipulating the metaphyseal fragment. A dental pick or a small single-prong skin hook can be utilized to gently maneuver the fragment into position. The reduction is assessed directly by visualizing the articular surface anteriorly to ensure a perfect cartilaginous step-free joint.
Once anatomic reduction is achieved, it is provisionally held with a smooth Kirschner wire (K-wire). Definitive fixation is typically achieved using two or three smooth K-wires (1.6 mm or 2.0 mm, depending on patient age).
* Pin Configuration: The most biomechanically stable configuration utilizes divergent pins. The first pin is directed from the lateral condyle, across the fracture site, engaging the medial cortex of the distal humerus. The second pin is directed more proximally up the lateral column. Parallel pins are also acceptable provided they achieve bicortical purchase.
* Alternative Fixation: In older children or adolescents approaching skeletal maturity, cannulated screw fixation (typically 3.5 mm or 4.0 mm) may be utilized to provide interfragmentary compression. However, screws must not cross an open physis to avoid premature growth arrest.
After fixation, the tourniquet is deflated, and hemostasis is achieved. The capsule and extensor aponeurosis are repaired meticulously with absorbable sutures to prevent late lateral soft tissue prominence. The pins are typically bent and left protruding through the skin to facilitate removal in the clinic, though some surgeons prefer to bury them to reduce infection risk.
Complications and Management
Pediatric lateral condyle fractures are notorious for their complication profile, primarily due to the complex anatomy and the unforgiving nature of intra-articular physeal injuries.
| Complication | Estimated Incidence | Etiology and Management Strategy |
|---|---|---|
| Lateral Spurring (Overgrowth) | 50% - 70% | Caused by periosteal stripping and hyperemic response. Usually asymptomatic. Reassure parents; excision rarely indicated unless cosmetically unacceptable or symptomatic. |
| Delayed Union / Nonunion | 1% - 5% | Due to inadequate fixation, missed >2mm displacement, or synovial fluid bathing the fracture. Management depends on symptoms. In situ fixation vs. open reduction with bone grafting. Late open reduction carries high AVN risk. |
| Cubitus Valgus | 5% - 10% | Secondary to nonunion or premature physeal closure of the lateral condyle. May lead to tardy ulnar nerve palsy. Managed with corrective supracondylar osteotomy and ulnar nerve transposition if symptomatic. |
| Avascular Necrosis (Fishtail Deformity) | < 2% | Iatrogenic disruption of posterior vascular supply during open reduction. Leads to central capitellar collapse. Difficult to salvage; may require complex joint reconstruction or osteochondral grafting. |
| Pin Tract Infection | 5% - 10% | Superficial infection of percutaneous pins. Managed with oral antibiotics and local pin care. Rarely requires premature pin removal unless deep infection is suspected. |
The management of established nonunion is one of the most controversial topics in pediatric orthopedics. If a nonunion is identified late (e.g., months or years after the injury) but the patient is completely asymptomatic with good range of motion, many surgeons advocate for benign neglect. Attempting to achieve union late requires extensive soft tissue stripping, which carries an unacceptably high risk of devascularizing the fragment and causing AVN. If the nonunion is symptomatic or associated with progressive valgus deformity, in situ fixation with bone grafting, often accompanied by an ulnar nerve transposition, is the preferred salvage strategy.
Post Operative Rehabilitation Protocols
Postoperative management is designed to protect the surgical fixation while the fracture consolidates.
Immediately postoperatively, the patient is placed in a well-padded long arm splint or bivalved cast with the elbow in 90 degrees of flexion and the forearm in neutral to slight pronation. Pronation helps relax the common extensor musculature, reducing the distracting forces on the lateral condyle fragment.
The patient is evaluated in the clinic at 1 week for wound inspection and radiographic assessment to ensure maintenance of reduction. Immobilization is typically continued for a total of 3 to 4 weeks. At the 3 to 4 week mark, radiographs are obtained out of the cast. If sufficient callus formation is evident and the fracture line is bridging, percutaneous pins are removed in the clinic setting.
Following pin removal, the patient may begin active range of motion exercises. It is critical to emphasize active motion only. Passive stretching or aggressive physical therapy is strictly contraindicated in the pediatric elbow, as it increases the risk of joint stiffness, heterotopic ossification, and myositis ossificans. Parents should be counseled that achieving full extension may take up to 6 to 12 months, and a mild residual extension deficit (5 to 10 degrees) is common but rarely functionally limiting. Return to contact sports and high-impact activities (such as monkey bars) is generally restricted for 10 to 12 weeks post-injury to allow for complete bony remodeling.
Summary of Key Literature and Guidelines
The academic foundation for managing lateral condyle fractures is built upon several seminal papers and evolving societal guidelines.
The necessity of the internal oblique radiograph, as highlighted in the opening clinical vignette, was definitively established by Song et al., who demonstrated that standard AP and lateral views miss critical posterior displacement in a significant percentage of cases. Their work validated the internal oblique view as the most sensitive imaging modality for determining the integrity of the articular hinge.
The Jakob classification remains the most clinically useful paradigm for surgical decision-making. Validation studies have consistently shown that Jakob Stage 1 fractures can be safely managed in a cast with close radiographic follow-up, while Stage 2 and Stage 3 fractures require stabilization. The debate between CRPP and ORIF for Stage 2 fractures continues, but recent literature leans heavily toward ORIF if there is any doubt regarding articular congruity, as the morbidity of a small lateral incision is vastly outweighed by the consequences of a malreduced joint.
Recent guidelines from the Pediatric Orthopaedic Society of North America (POSNA) emphasize the absolute necessity of anatomic reduction. While K-wire fixation remains the standard of care for the vast majority of these fractures, biomechanical studies have shown that divergent pin placement offers superior torsional stability compared to parallel pins. Furthermore, literature regarding the late management of nonunions continues to caution against aggressive late open reduction, reinforcing the principle that the best treatment for a lateral condyle nonunion is its prevention through accurate initial diagnosis and meticulous surgical execution.
