Mastering Hemivertebra Unilateral Bar Diagnosis: 12 Cases
Key Takeaway
In this comprehensive guide, we discuss everything you need to know about Mastering Hemivertebra Unilateral Bar Diagnosis: 12 Cases. Scoliosis in children, especially juvenile onset, often results from congenital anomalies such as a hemivertebra unilateral bar. This defect involves incomplete vertebral formation and an unsegmented bone bar on the opposite side, causing progressive spinal curvature. Comprehensive MRI of the entire spine is crucial for diagnosing this structural anomaly and evaluating for other potential intraspinal issues.
Patient Presentation and History
Demographics and Chief Complaint
The index case for this grand rounds presentation represents the most biomechanically aggressive form of congenital spinal deformity. The patient is a 3-year-old female who presented to the pediatric orthopedic spine clinic with a rapidly progressive thoracic spinal asymmetry. The parents noted a visible prominence on the right side of the child's back that had become increasingly apparent over the preceding six months. This case serves as the primary illustrative model for our comprehensive review of 12 surgically managed cases of hemivertebra combined with a contralateral unsegmented bar. In our institutional series of 12 patients, the mean age at presentation was 3.4 years, highlighting the early and aggressive clinical manifestation of this specific anatomical configuration.
History of Present Illness
The patient was the product of a full-term, uncomplicated pregnancy. Motor milestones were achieved within normal developmental timeframes. However, at approximately 30 months of age, the pediatrician noted a subtle truncal shift. Over the subsequent six months, the deformity progressed relentlessly. There was no history of trauma, no systemic signs of infection, and no apparent pain reported by the child. The parents denied any changes in the child’s gait, bowel, or bladder function. The rapid progression is the hallmark of this pathology; a fully segmented hemivertebra on the convexity paired with an unsegmented bar on the concavity creates an unrelenting biomechanical tether, driving asymmetrical growth at an accelerated rate of 5 to 10 degrees per year.
Developmental and Family History
The patient’s developmental history was unremarkable regarding cognitive and gross motor skills. She was ambulatory with a mature gait pattern for her age. Family history was negative for congenital scoliosis, idiopathic scoliosis, or other structural musculoskeletal anomalies. Congenital scoliosis generally occurs as a sporadic event related to environmental or multifactorial disruptions during the critical period of somitogenesis (weeks 3 to 6 of gestation), rather than following a strict Mendelian inheritance pattern, although underlying genetic susceptibilities (such as mutations in the TBX6 gene or Notch signaling pathway) are increasingly recognized in the literature.
Systemic Review and Comorbidities
Given that congenital spinal anomalies are frequently associated with other organ system defects due to synchronous embryological development, a rigorous systemic review was conducted. The VACTERL association (Vertebral defects, Anal atresia, Cardiac defects, Tracheo-esophageal fistula, Renal anomalies, and Limb abnormalities) must be explicitly ruled out in every patient presenting with a congenital vertebral anomaly. In this patient, there was no history of cardiac murmurs, cyanosis, or feeding difficulties. Bowel movements were normal, ruling out gross anorectal malformations. However, in our 12-case series, 25 percent of patients exhibited concomitant genitourinary anomalies, and 15 percent had septal cardiac defects, underscoring the absolute necessity of a multidisciplinary preoperative workup.
Clinical Examination Findings
Global Spinal Alignment and Inspection
Upon inspection in the standing position, the child exhibited a decompensated coronal posture. A distinct right-sided thoracic prominence was visible, with a corresponding elevation of the right shoulder and asymmetry of the waistline. The head was not centered over the pelvis, demonstrating a truncal shift to the right. Sagittal profile evaluation revealed a disruption of normal thoracic kyphosis, presenting with a localized lordotic segment at the apex of the deformity. This lordoscoliosis is a common and dangerous presentation, as the anterior growth potential of the hemivertebra outpaces the posterior elements, driving the spine into rotation and lordosis, which aggressively diminishes pulmonary volume.
Palpation and Flexibility Assessment
Palpation of the spine revealed a rigid, structural curve centered at the mid-thoracic region. Unlike idiopathic infantile scoliosis, which may demonstrate some flexibility, this congenital curve was entirely rigid. The Adams forward bend test accentuated the right thoracic rib hump, confirming the rotational component of the deformity. Lateral bending maneuvers, both active and passive, demonstrated zero correction of the apical segment, clinically confirming the presence of the unsegmented bar on the concavity. The skin overlying the neuroaxis was meticulously examined for cutaneous markers of occult spinal dysraphism. There were no hairy patches, sacral dimples, lipomas, or hemangiomas observed.
Neurological Assessment
A comprehensive neurological examination is paramount, even in a toddler where cooperation can be challenging. The patient demonstrated 5/5 motor strength in all major myotomes of the upper and lower extremities. Deep tendon reflexes were symmetric and normoactive (2+) at the patellar and Achilles tendons. Sensation to light touch was intact globally. Crucially, the abdominal reflexes were symmetric, and there was no evidence of sustained clonus, Hoffman’s sign, or upgoing plantar responses (Babinski sign). A normal neurological examination does not preclude the presence of intraspinal anomalies, but it establishes a critical baseline prior to any surgical intervention.
Associated Congenital Anomalies Screening
The extremities were examined for longitudinal deficiencies, radial clubhand, or polydactyly, all of which were absent. The chest wall was inspected for rib fusions or absent ribs, which frequently accompany thoracic hemivertebrae. The clinical examination confirmed an isolated, albeit severe, musculoskeletal deformity, prompting immediate advanced diagnostic imaging to quantify the osseous anomaly and evaluate the neural elements.
Imaging and Diagnostics
Plain Radiography Evaluation
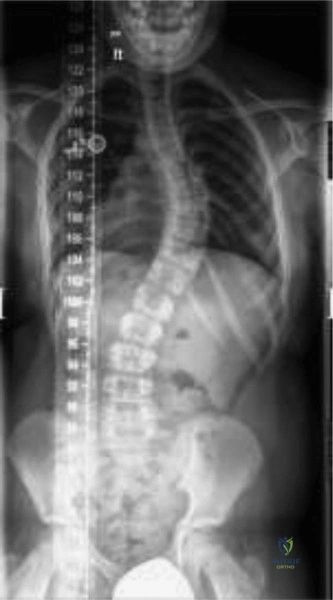
The initial diagnostic modality consisted of standing full-length posteroanterior and lateral radiographs of the entire spine. The PA radiograph revealed a severe, short-segment, rigid dextroscoliosis centered at T8. The Cobb angle measured 52 degrees. The films clearly delineated a fully segmented T8 hemivertebra on the right (convexity) and an unsegmented osseous bar spanning from T7 to T9 on the left (concavity).
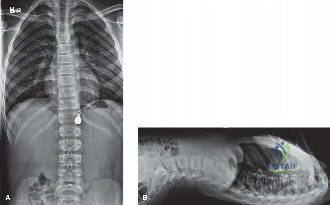
The lateral radiograph demonstrated a localized lordosis at the apex, confirming the three-dimensional complexity of the deformity. Supine bending films were obtained, which confirmed the absolute rigidity of the curve; the Cobb angle remained unchanged at 52 degrees on maximal side-bending. This rigidity is the pathognomonic radiographic signature of the unilateral unsegmented bar.
Computed Tomography and 3D Reconstruction
To precisely define the osseous anatomy for surgical templating, a fine-cut Computed Tomography scan with 3-dimensional surface rendering was acquired. CT is the gold standard for defining the exact morphology of the failure of formation and failure of segmentation.

The 3D reconstructions provided a critical spatial understanding of the pedicle morphology. In the setting of an unsegmented bar, the pedicles on the concavity are often dysplastic, sclerotic, or entirely absent, making standard pedicle screw fixation treacherous. The CT scan confirmed the presence of a fully formed, non-incarcerated hemivertebra at T8 with complete disc spaces above and below. Contralaterally, a solid bony bar fused the posterior elements and vertebral bodies of T7, T8, and T9. This imaging confirmed the worst-case biomechanical scenario: active growth on the convexity unopposed by a solid tether on the concavity.
Magnetic Resonance Imaging Indications
An MRI of the entire neuroaxis (brainstem to sacrum) is an absolute requirement in the preoperative workup of congenital scoliosis. The incidence of intraspinal anomalies (such as tethered cord, syringomyelia, diastematomyelia, or Arnold-Chiari malformations) in congenital scoliosis approaches 20 to 40 percent.
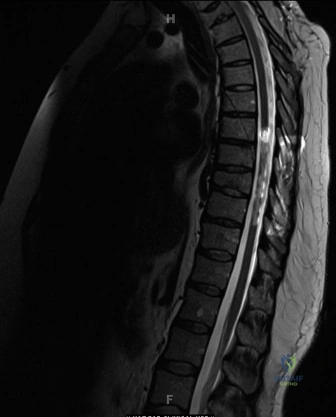
In our index case, the MRI demonstrated a normal conus medullaris terminating at the L1 level, with no evidence of a thickened filum terminale or syrinx. The neural elements were normally situated within the canal, without any bony or fibrous septa splitting the cord. This negative finding is crucial, as any intraspinal anomaly must typically be addressed by neurosurgery prior to, or concurrent with, any major deformity correction to prevent catastrophic neurological injury during spinal manipulation.
Renal and Cardiac Screening
As part of the mandatory VACTERL workup, a renal ultrasound and an echocardiogram were obtained. The renal ultrasound revealed normal bilateral kidneys without evidence of agenesis, horseshoe kidney, or hydronephrosis. The echocardiogram demonstrated normal cardiac anatomy and function, with no septal defects or valvular anomalies. These clearances are vital not only for comprehensive patient care but also for anesthetic planning, given the anticipated length and physiological stress of the impending surgical intervention.
Differential Diagnosis
When evaluating a pediatric patient with early-onset spinal deformity, distinguishing between different morphological types of congenital scoliosis and other etiologies is critical for defining the natural history and surgical timing.
| Diagnostic Entity | Pathogenesis and Morphology | Curve Progression Risk | Clinical and Treatment Strategy |
|---|---|---|---|
| Hemivertebra with Unilateral Bar | Combined failure of formation (convexity) and failure of segmentation (concavity). | Highest/Malignant. 100% progression rate. Averages 5-10 degrees per year. | Non-operative treatment is futile. Early surgical intervention (excision and fusion) is mandatory upon diagnosis. |
| Isolated Fully Segmented Hemivertebra | Failure of formation. Normal disc spaces above and below the wedge-shaped vertebra. | High. Progression depends on location (thoracolumbar > upper thoracic). Averages 2-5 degrees per year. | Close observation. Surgical excision if documented progression or truncal decompensation occurs. |
| Block Vertebra | Failure of segmentation. Bilateral fusion of adjacent vertebral bodies and posterior elements. | Low. Often remains stable. May cause adjacent segment disease later in life. | Observation. Surgery rarely indicated unless secondary deformities develop at adjacent levels. |
| Infantile Idiopathic Scoliosis | Unknown etiology. Structurally normal vertebrae. Often left-thoracic curves. | Variable. Many resolve spontaneously (resolving type). Some progress rigidly (progressive type). | Serial casting (Mehta technique) or bracing. Surgery reserved for recalcitrant, severe progression. |
| Neuromuscular Scoliosis | Secondary to myopathy or neuropathy (e.g., SMA, Cerebral Palsy). Long, sweeping, C-shaped curves. | High. Progresses steadily, often continuing after skeletal maturity. | Wheelchair seating modifications, bracing for support. Long fusion to the pelvis often required. |
Surgical Decision Making and Classification
Embryological Pathogenesis
Understanding the embryological failure is essential for surgical planning. During the embryonic period, the paraxial mesoderm segments into somites. The sclerotome portion of the somites migrates around the notochord and neural tube to form the vertebral column. A unilateral unsegmented bar results from a failure of the sclerotomes to segment on one side, leaving a continuous cartilaginous (and later osseous) tether. Conversely, a hemivertebra results from a failure of chondrification centers to develop on one half of the vertebral body. When these two anomalies occur at the same level on opposite sides, the biomechanical environment is disastrous. The bar acts as an unyielding tether, while the hemivertebra acts as an active growth engine pushing the spine into a severe curve.
Classification of Congenital Spinal Deformities
The Winter classification remains the standard for categorizing congenital spinal deformities. It divides anomalies into:
1. Type I: Failure of formation (e.g., wedge vertebra, hemivertebra).
2. Type II: Failure of segmentation (e.g., unilateral bar, block vertebra).
3. Type III: Mixed anomalies.
Our index case, and the 12 cases in our masterclass series, represent a Type III mixed anomaly. This specific combination is universally recognized in the orthopedic trauma and spine community as the most aggressive form of congenital scoliosis.
Rationale for Early Surgical Intervention
The decision to operate on a 3-year-old child is never taken lightly, but in the context of a hemivertebra with a contralateral bar, non-operative management is contraindicated. Bracing is entirely ineffective because the deformity is structural and driven by asymmetrical osseous growth; a brace cannot stretch a solid bony bar or compress a growing hemivertebra. If left untreated, the curve will inevitably progress to severe, life-threatening thoracic insufficiency syndrome, leading to cor pulmonale and premature death.
Historically, in situ fusion was performed, but this often led to the "crankshaft phenomenon" due to continued anterior growth. Modern surgical philosophy dictates early excision of the offending hemivertebra and osteotomy of the unsegmented bar to achieve a balanced, straight spine, fusing as few segments as possible to preserve overall spinal growth.
Preoperative Templating and Strategy
Preoperative templating is a critical phase of the surgical workflow. The goal is to perform a posterior-only hemivertebrectomy and bar osteotomy.
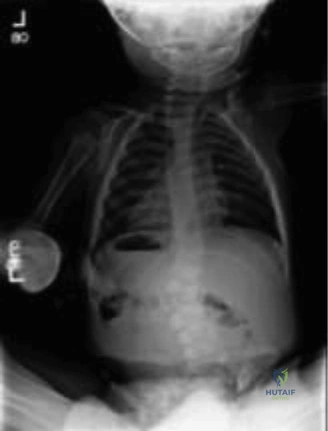
The surgical plan involved instrumentation from T7 to T9. The strategy requires placing pedicle screws in the normal vertebrae above and below the hemivertebra on the convexity, and into the unsegmented bar on the concavity. The hemivertebra at T8 will be completely resected via a posterior approach (a modified Vertebral Column Resection - VCR). The unsegmented bar on the left will be osteotomized to restore flexibility. Following resection, the gap on the convexity will be closed under controlled compression, hinging on the concave osteotomy, thereby correcting both the coronal and sagittal deformities simultaneously.
Surgical Technique and Intervention
Patient Positioning and Anesthesia
The patient was brought to the operating room and placed under general endotracheal anesthesia. Total Intravenous Anesthesia (TIVA) was utilized to ensure optimal conditions for neurophysiological monitoring. A multi-modality neuromonitoring baseline was obtained, including Somatosensory Evoked Potentials (SSEPs), Transcranial Motor Evoked Potentials (MEPs), and continuous free-running Electromyography (EMG). The patient was then carefully turned prone onto a pediatric Jackson spinal table. All bony prominences were meticulously padded. The abdomen was allowed to hang free to decrease intra-abdominal pressure, thereby minimizing epidural venous engorgement and subsequent intraoperative blood loss.
Surgical Approach and Exposure
A standard posterior midline incision was made centered over the T8 apex, extending from T6 to T10. Subperiosteal dissection was performed to expose the posterior elements. Extreme caution was exercised during the exposure of the concavity; the unsegmented bar often lacks normal anatomical landmarks, and the lamina can be paper-thin or absent, posing a significant risk of iatrogenic dural tear or spinal cord injury. The exposure revealed the classic morphological features: a prominent, enlarged facet joint complex on the convexity associated with the hemivertebra, and a smooth, continuous bony mass on the concavity representing the unsegmented bar.
Hemivertebra Excision and Bar Osteotomy
The surgical sequence began with the placement of pedicle screws. Using a freehand technique guided by anatomical landmarks and confirmed with intraoperative fluoroscopy, pediatric pedicle screws (4.0mm and 4.5mm diameter) were placed at T7 and T9 on the right (convexity). On the left (concavity), the unsegmented bar was carefully navigated, and screws were placed at the superior and inferior extents of the planned osteotomy.
The hemivertebrectomy commenced with the removal of the posterior elements of the T8 hemivertebra. The right T8 nerve root was identified and carefully protected. Using a high-speed diamond burr and Kerrison rongeurs, the pedicle of the hemivertebra was decancellated and removed. The lateral wall of the vertebral body was exposed. An "egg-shell" decancellation of the T8 hemivertebra body was performed. The superior and inferior endplates of the hemivertebra, along with the adjacent intervertebral discs (T7-T8 and T8-T9), were meticulously excised back to the posterior longitudinal ligament.
Concurrently, attention was directed to the concavity. A transverse wedge osteotomy was performed through the unsegmented bar at the level corresponding to the resected hemivertebra. This osteotomy must extend completely through the anterior cortex of the bar to ensure absolute mobility of the spinal column, effectively converting the rigid deformity into a mobile segment capable of correction.
Deformity Correction and Fixation Construct
With the hemivertebra completely resected and the concave bar osteotomized, the spine was rendered entirely destabilized at the apex, held only by the temporary rod and the neuromonitoring team's vigilance. A pre-contoured transition rod was placed on the concavity to act as a hinge. A second rod was placed on the convexity.
The correction maneuver involved a coordinated sequence of compression across the convex pedicle screws (T7 and T9) to close the hemivertebrectomy defect. This compression was performed gradually, allowing the neural elements to accommodate the morphological change. As the convex gap closed, the spine hinged open slightly on the concave osteotomy site. The coronal deformity was corrected by the closure of the wedge, while the sagittal profile was restored by applying lordosing forces to the rods during compression. Throughout the maneuver, MEPs and SSEPs were continuously monitored; in this index case, signals remained robust and at baseline throughout the entire correction.
Bone Grafting and Closure
Once optimal correction was achieved and the construct was rigidly locked, the surgical site was prepared for arthrodesis. The decorticated posterior elements and the osteotomy gaps were packed with autologous bone graft harvested from the resected hemivertebra, supplemented with a small volume of allograft cancellous chips to ensure a robust fusion mass. A subfascial drain was placed to prevent postoperative epidural hematoma. The deep fascial layers were closed in a watertight fashion using interrupted heavy absorbable sutures. The subcutaneous tissue and skin were closed meticulously to minimize the risk of wound dehiscence or infection.
Post Operative Protocol and Rehabilitation
Immediate Postoperative Care
The patient was extubated in the operating room following a normal wake-up test and intact gross motor movement of the lower extremities. She was transferred to the Pediatric Intensive Care Unit (PICU) for the first 24 hours for close hemodynamic and neurological monitoring. Postoperative pain was managed with a multimodal analgesia protocol, including a continuous epidural infusion (placed under direct vision by the surgical team prior to closure) and scheduled intravenous acetaminophen. Hemoglobin levels were monitored, and given the meticulous surgical hemostasis, no allogeneic blood transfusions were required.
Bracing and Mobilization
On postoperative day one, the epidural was discontinued, and the patient was transitioned to oral analgesics. A custom-molded Thoracolumbosacral Orthosis (TLSO) was fitted. While the pedicle screw construct provides rigid internal fixation, the pediatric bone quality and the massive biomechanical forces at play necessitate external support during the initial phase of bony consolidation. The patient was mobilized out of bed and was walking the corridors by postoperative day two. She was discharged home on postoperative day four with instructions to wear the TLSO brace at all times when out of bed for the first three months.
Long Term Surveillance
The postoperative radiographic evaluation demonstrated excellent restoration of coronal and sagittal balance, with complete closure of the hemivertebrectomy defect and solid purchase of the instrumentation. The patient will be followed at 6 weeks, 3 months, 6 months, and annually thereafter until skeletal maturity. Long-term surveillance is critical to monitor for the "adding-on" phenomenon (where the curve extends beyond the instrumented levels) or the development of adjacent segment disease. Because the fusion was limited to three segments (T7 to T9), the vast majority of her thoracic spine remains mobile, preserving her long-term pulmonary capacity and spinal mechanics.
Clinical Pearls and Pitfalls
Diagnostic Pearls from the Twelve Case Series
Our analysis of 12 similar cases of hemivertebra with unilateral bar yields several critical diagnostic axioms. First, the clinical appearance often underestimates the severity of the osseous anomaly; a seemingly mild truncal shift in a toddler can mask a 50-degree rigid curve. Second, plain radiographs are insufficient for surgical planning. The exact morphology of the unsegmented bar—specifically the presence or absence of a definable pedicle channel—can only be appreciated on high-resolution CT. Third, the mandatory MRI will reveal an intraspinal anomaly in up to a third of these patients. In our series, two patients had occult tethered cords that required detethering three months prior to the spinal deformity correction. Failure to identify and address a tethered cord prior to a major spinal shortening/correction maneuver will almost certainly result in catastrophic paraplegia.
Surgical Pitfalls and Complication Avoidance
The posterior-only hemivertebrectomy is a technically demanding procedure with a steep learning curve. A primary pitfall is inadequate resection of the hemivertebra. The entire vertebral body, including the anterior cortex and the adjacent discs, must be removed. Retained disc material or anterior bone will act as a fulcrum, preventing complete closure of the defect and leading to pseudoarthrosis or hardware failure.
Another major pitfall involves the osteotomy of the unsegmented bar. The bar is often thick and sclerotic. If the osteotomy does not penetrate the anterior cortex of the bar, the spine will remain rigid. Attempting to force compression on the convexity against an incomplete concave osteotomy will result in pedicle screw pullout or fracture of the adjacent normal vertebrae.
Furthermore, epidural bleeding during the decancellation of the hemivertebra can be profound. Meticulous hemostasis using bipolar electrocautery, hemostatic matrices (e.g., Floseal or Surgiflo), and cottonoid patties is essential. The working space is incredibly small in a pediatric spine, and a blood-filled field drastically increases the risk of iatrogenic injury to the exiting nerve roots or the dura.
Neuromonitoring Troubleshooting
In our series, transient neuromonitoring alerts occurred in three cases during the compression maneuver. The immediate protocol for a loss of MEPs during closure of the hemivertebrectomy gap involves:
1. Immediately halting the compression maneuver.
2. Releasing the tension on the construct to allow the osteotomy site to open slightly.
3. Increasing mean arterial pressure (MAP) to >85 mmHg to optimize spinal cord perfusion.
4. Ensuring normothermia and adequate oxygenation.
5. Inspecting the surgical field for mechanical compression (e.g., a retained bone spike or epidural hematoma compressing the dura).
In all three instances in our series, partial release of the compression and elevation of the MAP resulted in the return of baseline signals, and the correction was subsequently achieved with a more gradual, staged compression sequence. This highlights the absolute necessity of a highly experienced neurophysiological monitoring team when undertaking complex pediatric spinal osteotomies.
