Pediatric Supracondylar Humerus Fracture: A Comprehensive Clinical & Radiographic Diagnostic Case Study

Key Takeaway
Pediatric supracondylar humerus fractures are diagnosed via clinical exam (pain, swelling, deformity), thorough neurovascular assessment, and critical X-ray findings. Look for posterior displacement, disrupted anterior humeral line, abnormal Baumann's angle, and fat pad signs. Advanced imaging is usually reserved for complex cases.
Patient Presentation and History
Mechanism of Injury and Initial Presentation
A 7-year-old right-hand dominant male presented to the emergency department following a high-energy fall from playground equipment. The reported mechanism of injury was a fall onto an outstretched hand from approximately 1.5 meters in height, with the elbow locked in full extension upon impact. This mechanism is the classic generator of the extension-type supracondylar humerus fracture, which accounts for approximately 95% of all pediatric supracondylar fractures. The axial load transmitted through the extended elbow forces the olecranon process into the olecranon fossa. In the pediatric population, the ligamentous laxity allows for physiological hyperextension, converting the olecranon into a fulcrum that levers the distal humeral metaphysis anteriorly, resulting in tension failure of the anterior cortex and subsequent posterior displacement of the distal fragment.
The patient immediately experienced severe pain, profound swelling, and an absolute inability to range his left elbow. There was no reported loss of consciousness, head trauma, or other associated axial or appendicular injuries, isolating the pathology to the left upper extremity.
Demographics and Comorbidities
The patient is a healthy 7-year-old male, representing the peak epidemiological demographic for this specific injury. The incidence of supracondylar humerus fractures peaks between the ages of 5 and 7 years. This age distribution correlates directly with the physiological development of the distal humerus, where the supracondylar region undergoes significant remodeling, resulting in a decreased cross-sectional area and a relatively thin architectural profile. The presence of the olecranon and coronoid fossae further attenuates the osseous integrity in this region, creating a distinct stress riser susceptible to failure under bending moments.
The patient possesses no significant past medical history. There are no known connective tissue disorders, osteogenesis imperfecta, or neuromuscular conditions that would predispose him to pathological fractures or alter the standard treatment algorithm. Immunization status is up-to-date, including tetanus prophylaxis, which remains a critical consideration in the event of an open fracture variant. Parents deny any history of bleeding diatheses, ensuring that standard surgical hemostasis protocols will be sufficient.
Clinical Examination Findings
Inspection and Soft Tissue Assessment
Upon initial assessment in the trauma bay, the patient was alert, hemodynamically stable, but in significant distress secondary to localized pain. Gross inspection revealed profound swelling and ecchymosis circumferentially around the left elbow, extending distally into the proximal forearm. A classic S-shaped deformity of the distal arm was grossly evident, pathognomonic for a completely displaced extension-type fracture with posterior translation of the distal fragment.
Skin integrity was meticulously evaluated. The skin was intact with no open lacerations, abrasions, or punctate wounds that would suggest an open fracture (e.g., from a medially displaced proximal fragment piercing the skin). Crucially, the anterior antecubital fossa was examined for the "pucker sign." This clinical finding occurs when the sharp anteriorly displaced proximal metaphyseal spike penetrates and entraps the brachialis muscle and potentially the deep dermis. While absent in this patient, the presence of a pucker sign is a critical clinical indicator of a potentially irreducible fracture via closed means, often necessitating an open approach for extrication of the entrapped soft tissues. There were no early signs of fracture blisters, though the magnitude of swelling indicated a high risk for impending soft tissue compromise if reduction was delayed.
Palpation and Osseous Landmarks
Palpation was performed with extreme caution to avoid exacerbating pain or inducing iatrogenic neurovascular injury. Diffuse, exquisite tenderness was localized over the distal humerus, specifically at the supracondylar ridges. Gentle palpation confirmed the disruption of the normal osseous anatomy. The normal equilateral triangle formed by the medial epicondyle, lateral epicondyle, and the tip of the olecranon (in 90 degrees of flexion) was entirely distorted, though the relationship between these three specific landmarks remained intact within the displaced distal fragment itself. This distinguishes a supracondylar fracture from an elbow dislocation, where the epicondylar-olecranon relationship is inherently disrupted. Palpable crepitus was noted with minimal provocation, confirming complete osseous instability.
Range of Motion and Joint Stability
Both active and passive range of motion of the left elbow were severely restricted. The patient exhibited intense guarding. Attempts at flexion and extension were met with immediate resistance and profound pain. Pronation and supination of the forearm were similarly restricted. In the setting of an acute, clinically obvious displaced supracondylar fracture, aggressive manipulation or forced range of motion is strictly contraindicated prior to radiographic evaluation and definitive reduction, as it risks further displacement and secondary injury to the intimately associated neurovascular structures.
Comprehensive Neurological Assessment
A rigorous and documented neurological examination is paramount, given the high incidence of associated nerve injuries (10-20% in displaced extension-type fractures).
- Anterior Interosseous Nerve: The anterior interosseous nerve (AIN), a motor branch of the median nerve, is the most frequently injured nerve in extension-type supracondylar fractures, particularly those with posterolateral displacement. The AIN innervates the flexor pollicis longus, the flexor digitorum profundus to the index and middle fingers, and the pronator quadratus. Function was assessed by asking the patient to form an "OK" sign. The patient successfully demonstrated flexion at the interphalangeal joint of the thumb and the distal interphalangeal joint of the index finger, confirming intact AIN motor function.
- Median Nerve: Sensation over the palmar aspect of the index finger and thumb was intact to light touch. Motor function of the abductor pollicis brevis was confirmed by resisted palmar abduction of the thumb.
- Radial Nerve: The radial nerve is particularly vulnerable in posteromedial displacement patterns, where the nerve can be tethered or contused by the lateral spike of the proximal fragment. Sensation over the dorsal first web space was intact. Motor function was confirmed via active wrist extension and thumb extension (extensor pollicis longus).
- Ulnar Nerve: The ulnar nerve is less commonly injured in extension-type fractures but is at higher risk in flexion-type injuries or iatrogenically during medial pin placement. Sensation over the volar tip of the little finger was intact. Motor function of the dorsal and palmar interossei was confirmed by assessing finger abduction and adduction.
Vascular Assessment and Perfusion
Vascular compromise is a critical emergency in displaced supracondylar fractures, occurring in up to 1% to 20% of cases, primarily due to tethering, contusion, intimal tear, or frank transection of the brachial artery over the anteriorly displaced proximal fragment.
Bilateral radial and ulnar pulses were palpated. The left radial pulse was symmetrical in character and amplitude compared to the contralateral side. Capillary refill was brisk, measuring less than 2 seconds in all digits of the left hand. The hand was warm, pink, and well-perfused. There was no evidence of pallor, paresthesias, or paralysis that would suggest acute arterial insufficiency or acute compartment syndrome of the forearm (Volkmann's ischemia). The presence of a palpable radial pulse and normal perfusion parameters precluded the immediate need for advanced vascular imaging (e.g., CT angiography or formal arterial duplex ultrasound) at this stage.
Imaging and Diagnostics
Plain Radiography Analysis
Standard orthogonal imaging, consisting of true anteroposterior and true lateral radiographs of the left elbow, was obtained in the emergency department. Accurate radiographic interpretation is heavily reliant on understanding the pediatric ossification centers, commonly remembered by the mnemonic CRITOE (Capitellum, Radial head, Internal/Medial epicondyle, Trochlea, Olecranon, External/Lateral epicondyle), which appear sequentially at approximately 1, 3, 5, 7, 9, and 11 years of age.
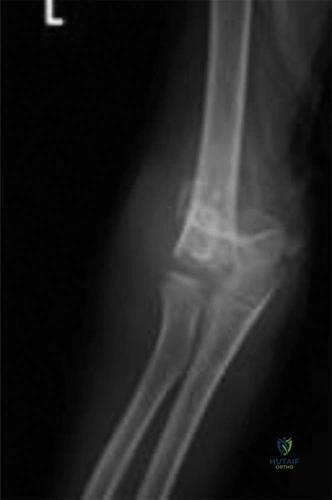
- Anteroposterior View: The AP radiograph revealed a complete, transverse fracture line propagating through the supracondylar region of the distal humeral metaphysis, proximal to the olecranon fossa. The distal fracture fragment demonstrated significant posterior and medial displacement relative to the humeral shaft. The medial displacement is a critical observation, as it dictates the required reduction maneuver (pronation) to tension the intact medial periosteal hinge.
- Baumann's Angle: This angle is formed by the intersection of a line drawn down the longitudinal axis of the humeral shaft and a line drawn along the physeal line of the lateral condyle. The normal range is typically 64 to 81 degrees, though comparison to the contralateral uninjured side is the gold standard (a difference of >5 degrees is considered abnormal). In this patient, Baumann's angle was measured at 55 degrees. This significant decrease indicates a severe varus collapse of the distal fragment. Failure to correct this angular deformity will result in a clinical cubitus varus (gunstock) deformity, which, while primarily cosmetic, can lead to late-onset posterolateral rotatory instability or tardy ulnar nerve palsy.

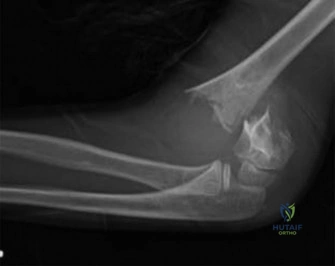
- Lateral View: The lateral radiograph is paramount for assessing sagittal plane displacement and angulation. It confirmed a complete fracture with severe posterior displacement of the distal fragment.
- Anterior Humeral Line: A line drawn down the anterior cortex of the humeral shaft should normally intersect the middle third of the capitellar ossification center. In this radiograph, the anterior humeral line passed entirely anterior to the capitellum, confirming posterior displacement and extension angulation of the distal fragment.
- Radiocapitellar Line: A line drawn through the longitudinal axis of the radius must bisect the capitellum in all radiographic views. This line remained intact, ruling out a concomitant radial head or neck dislocation (Monteggia variant).
- Teardrop Sign: The normal teardrop shape, formed by the anterior aspect of the coronoid fossa and the posterior aspect of the radial fossa, was completely disrupted, further confirming the fracture through the supracondylar region.
- Fat Pad Sign: While the fracture was grossly obvious, the presence of a large posterior fat pad sign (lifting of the joint capsule by hemarthrosis) and an elevated anterior "sail sign" were noted, indicative of a significant intra-articular effusion.
Advanced Imaging Indications
In the context of this classic, acute pediatric supracondylar humerus fracture, advanced cross-sectional imaging such as Computed Tomography or Magnetic Resonance Imaging is not indicated. CT is generally reserved for complex, comminuted intra-articular fractures (e.g., T-condylar fractures in older adolescents) or to evaluate for capitellar shear fractures (rare in this age group) when plain radiographs are equivocal. MRI has no role in the acute trauma setting for this injury pattern. Arterial duplex ultrasound is reserved for cases of a "white, pulseless hand" to localize the site of arterial occlusion or to monitor flow in a "pink, pulseless hand" following reduction.
Differential Diagnosis
The clinical presentation of a swollen, painful pediatric elbow following trauma necessitates a broad differential diagnosis. Accurate radiographic interpretation is essential to differentiate between these entities, as the surgical management and potential complications vary significantly.
| Differential Diagnosis | Pathophysiology & Mechanism | Key Radiographic Features | Clinical Differentiators |
|---|---|---|---|
| Supracondylar Humerus Fracture | Extra-articular fracture of distal humeral metaphysis. Mechanism: FOOSH with elbow extended (95%) or flexed (5%). | Disruption of anterior humeral line. Posterior/anterior displacement. Abnormal Baumann's angle. Teardrop disruption. | S-shaped deformity. High risk of AIN/vascular injury. Epicondylar-olecranon relationship intact. |
| Lateral Condyle Fracture | Intra-articular, Salter-Harris IV equivalent fracture. Mechanism: Varus stress on extended/supinated elbow, or avulsion by extensor origin. | Fracture line extending from lateral metaphysis through physis into the joint (capitellotrochlear groove). Thurston-Holland fragment. | Swelling localized laterally. High risk of nonunion and late cubitus valgus / tardy ulnar nerve palsy. |
| Transphyseal Separation | Salter-Harris I or II fracture of the entire distal humeral physis. Common in infants (<3 years) due to child abuse or birth trauma. | Posteromedial displacement of radius and ulna relative to humerus. Radiocapitellar line remains intact. | Often mistaken for elbow dislocation. Occurs in much younger demographic. High suspicion for non-accidental trauma. |
| Elbow Dislocation | Complete disruption of the ulnohumeral and radiocapitellar joints. Mechanism: FOOSH with valgus/supination stress. Rare in children <10 years. | Empty olecranon fossa. Radius and ulna displaced (usually posterolaterally) relative to the distal humerus. | Disruption of the equilateral triangle formed by medial epicondyle, lateral epicondyle, and olecranon. |
Surgical Decision Making and Classification
The Gartland Classification System
The surgical decision-making process for pediatric supracondylar humerus fractures is heavily guided by the Gartland classification system, as modified by Wilkins and later Leitch. This system categorizes fractures based on the degree of displacement and the integrity of the periosteal hinge.
- Type I: Nondisplaced or minimally displaced (<2mm). Anterior humeral line intersects the capitellum. Intact anterior and posterior periosteum.
- Type IIA: Displaced in the sagittal plane (extension angulation) but with an intact posterior cortex/periosteal hinge. No coronal plane deformity (normal Baumann's angle).
- Type IIB: Displaced in the sagittal plane with an intact posterior hinge, but accompanied by a coronal plane deformity (varus/valgus) or rotational malalignment.
- Type III: Completely displaced fracture with no cortical contact. Disruption of both anterior and posterior periosteal hinges. Highly unstable.
- Type IV (Leitch Modification): Diagnosed intraoperatively. Complete periosteal disruption circumferentially. The fracture is unstable in both flexion and extension, demonstrating multidirectional instability.
Rationale for Operative Intervention
Based on the clinical and radiographic findings, this patient presents with a Gartland Type III extension-type supracondylar humerus fracture. The distal fragment is completely displaced posteromedially, with a significant varus deformity (Baumann's angle 55 degrees).
Non-operative management (closed reduction and casting) is strictly contraindicated for Gartland Type III fractures. The complete loss of periosteal continuity renders these fractures inherently unstable. Attempting to hold a Type III fracture in a cast requires extreme hyperflexion (>110 degrees) to utilize the triceps as a tension band. In the setting of massive acute swelling, immobilizing the elbow in hyperflexion dramatically increases the intracompartmental pressure of the volar forearm, exponentially raising the risk of vascular compromise and subsequent Volkmann's ischemic contracture. Furthermore, closed management of Type III fractures carries an unacceptably high rate of loss of reduction, resulting in malunion (cubitus varus).
Therefore, the definitive indication for this patient is urgent operative intervention: Closed Reduction and Percutaneous Pinning (CRPP). The goals of surgery are to anatomically restore the anterior humeral line, correct the coronal alignment (restore Baumann's angle), correct rotational deformity, and provide rigid mechanical stability to allow for safe immobilization in a relaxed position (70-90 degrees of flexion).
Timing of Surgery
While historically considered a middle-of-the-night emergency, contemporary orthopedic literature supports that isolated, closed, neurovascularly intact Gartland III fractures can be safely treated urgently within 12 to 24 hours of injury without an increased risk of complications, open reduction rates, or compartment syndrome. However, immediate emergent intervention is mandated in the presence of:
1. Vascular compromise (white, pulseless hand).
2. Open fractures.
3. Concomitant ipsilateral forearm fractures ("floating elbow"), which increase compartment syndrome risk.
4. Massive, progressive swelling with impending skin compromise.
Given this patient's intact neurovascular status and closed injury, he was optimized for the operating room on an urgent basis.
Surgical Technique and Intervention
Patient Positioning and Preparation
The patient was taken to the operating room and placed under general anesthesia. Muscle relaxation is critical to overcome the deforming forces of the triceps and brachialis muscles. The patient was positioned supine on the operating table. The injured left upper extremity was prepped and draped in standard sterile fashion.
Two primary setups for fluoroscopy are utilized: the radiolucent arm board or using the C-arm itself as the operating table. In this case, the C-arm image intensifier was positioned parallel to the operating table, acting as the surgical surface. This allows for seamless transition between AP and lateral fluoroscopic views by simply rotating the shoulder, rather than moving the heavy C-arm, minimizing the risk of losing a tenuous reduction.
Closed Reduction Maneuvers
Reduction of a completely displaced Gartland III fracture requires a systematic, multi-step approach to manipulate the distal fragment back onto the metaphyseal shaft.
- Traction: With an assistant providing counter-traction at the axilla, longitudinal traction is applied to the forearm with the elbow in approximately 20-30 degrees of flexion. This disengages the fracture fragments and restores length.
- Medial/Lateral Translation: While maintaining traction, coronal plane translation is corrected. For this posteromedially displaced fracture, a valgus force was applied to correct the medial translation of the distal fragment.
- Correction of Rotation: The forearm is rotated to correct the rotational malalignment.
- Sagittal Reduction (Hyperflexion): The surgeon places their thumb firmly over the posterior aspect of the olecranon. While maintaining traction and coronal alignment, the elbow is smoothly hyperflexed. The thumb acts as a fulcrum, pushing the distal fragment anteriorly to close the posterior gap and restore the anterior humeral line.
- Forearm Positioning (Pronation/Supination): To lock the reduction, the intact periosteal hinge must be tensioned. For a posteromedially displaced fracture, the medial periosteal hinge is typically intact or partially intact. Pronating the forearm tightens the medial soft tissue structures, closing the lateral gap and locking the fracture in coronal alignment. (Conversely, supination is used for posterolateral displacement).
Following the reduction maneuver, the elbow was held in hyperflexion and pronation. Fluoroscopic imaging in both the AP (Jones view, shooting through the hyperflexed elbow) and true lateral projections confirmed an anatomic reduction. The anterior humeral line intersected the middle third of the capitellum, and Baumann's angle was restored to 72 degrees.
Percutaneous Pinning Construct
The choice of pin configuration—crossed pins (medial and lateral) versus divergent lateral pins—remains a topic of extensive biomechanical and clinical debate. Crossed pins offer the highest torsional stiffness and biomechanical stability. However, the placement of a medial pin carries a well-documented risk of iatrogenic injury to the ulnar nerve (up to 4%), which can subluxate anteriorly over the medial epicondyle during elbow hyperflexion. Divergent lateral pins avoid the ulnar nerve entirely but require meticulous technique to achieve adequate spread at the fracture site for sufficient stability.
Given the complete instability of this Gartland III fracture, a decision was made to utilize a divergent lateral pin construct, with a low threshold to add a medial pin if intraoperative stability was deemed insufficient.
Step-by-Step Fixation
- First Lateral Pin: A 1.6mm (0.062-inch) smooth Kirschner wire (K-wire) was driven percutaneously under power. The entry point was the center of the lateral epicondyle. The pin was directed proximally, medially, and slightly anteriorly, aiming to engage the dense cortical bone of the medial humeral metaphysis proximal to the olecranon fossa. Fluoroscopy confirmed bicortical purchase.
- Second Lateral Pin: A second 1.6mm K-wire was introduced slightly anterior and distal to the first pin, entering through the capitellum. It was directed divergently from the first pin to maximize the distance between the pins at the fracture site. Biomechanical studies indicate that maximizing pin separation at the fracture site is the most critical factor in optimizing the stability of a lateral-only construct.
- Stability Assessment: Following the placement of two lateral pins, the elbow was gently extended to 90 degrees, and rotational stability was assessed under live fluoroscopy. The fracture demonstrated absolute stability with no widening of the medial column. Therefore, a medial pin was deemed unnecessary, sparing the patient the risk of ulnar nerve injury.
- Final Imaging: Final AP, lateral, and oblique fluoroscopic images were saved, confirming anatomic reduction, restoration of all radiographic lines, and appropriate pin placement with bicortical engagement.
- Pin Management: The K-wires were bent at 90 degrees outside the skin to prevent migration, cut short, and capped. The skin entry sites were meticulously cleaned, and sterile Xeroform dressings were applied.
Post Operative Protocol and Rehabilitation
Immediate Post-Operative Immobilization
Following successful percutaneous pinning, the structural integrity of the distal humerus is restored by the hardware, eliminating the need for extreme hyperflexion. The patient was immobilized in a custom-molded, bivalved fiberglass long arm cast. Crucially, the elbow was positioned at approximately 70 to 80 degrees of flexion. Immobilizing the elbow at angles greater than 90 degrees significantly increases the risk of vascular compression and compartment syndrome, even post-operatively. The forearm was left in neutral rotation.
The patient was admitted for overnight observation to monitor neurovascular status and pain control. Elevating the affected extremity on pillows above the level of the heart is mandatory to facilitate venous return and mitigate postoperative edema.
Outpatient Management and Pin Removal
The patient was discharged on postoperative day one following confirmation of stable neurovascular status and adequate oral pain control.
- 1-Week Follow-up: The patient returned to the clinic for a wound check and radiographic evaluation. AP and lateral X-rays in the cast confirmed maintenance of reduction and stable hardware.
- 3 to 4-Week Follow-up: The standard duration for K-wire retention in pediatric supracondylar fractures is 3 to 4 weeks. At this juncture, clinical healing (absence of tenderness) and radiographic evidence of early callus formation were confirmed. The cast was removed, and the percutaneous pins were extracted in the clinic setting. Pin removal is typically well-tolerated by pediatric patients without the need for sedation, utilizing a swift, continuous pulling motion.
Rehabilitation and Range of Motion
Following pin removal, the patient was transitioned to a removable posterior splint for comfort, to be used only as needed. The cornerstone of pediatric elbow rehabilitation is active, unassisted range of motion.
Formal physical therapy is rarely indicated and can often be detrimental. Passive stretching or forceful manipulation by a therapist or parent is strictly contraindicated. Aggressive passive stretching creates microtrauma to the joint capsule and the brachialis muscle, significantly increasing the risk of heterotopic ossification (myositis ossificans) and paradoxical joint stiffness.
Parents were counseled that the return of full range of motion is a gradual process. Extension is typically the last motion to fully recover. It is common for a child to lack 10 to 15 degrees of terminal extension for several months post-injury. Complete remodeling and restoration of full, symmetrical range of motion can take up to 6 to 12 months. The patient was restricted from high-impact activities, contact sports, and playground equipment (monkey bars, trampolines) for a minimum of 8 to 12 weeks to prevent re-fracture through the remodeling metaphyseal bone.
Clinical Pearls and Pitfalls
- Pitfall - The Unrecognized Pucker Sign: Failure to identify a pucker sign in the antecubital fossa can lead to futile, repeated attempts at closed reduction. This not only damages the entrapped brachialis muscle but further contuses the median nerve and brachial artery. Early recognition warrants a low threshold for a mini-open anterior approach.
- Pearl - Managing the Pink, Pulseless Hand: A perfused but pulseless hand following a supracondylar fracture is a complex scenario. The current consensus dictates that if the hand is pink, warm, and has a capillary refill of <2 seconds, immediate closed reduction and pinning should be performed. In the vast majority of cases, anatomic reduction relieves the arterial kinking or spasm, and the pulse returns. If the hand remains pink and pulseless post-reduction, close observation is warranted; routine vascular exploration is not indicated as collateral circulation is sufficient.
- Pitfall - Iatrogenic Ulnar Nerve Injury: When utilizing a crossed-pin construct, blind percutaneous placement of the medial pin is a critical error. The ulnar nerve can subluxate anteriorly in hyperflexion. A medial pin must always be placed via a mini-open incision. The medial epicondyle is bluntly exposed, and the pin is placed under direct visualization or with a protective
