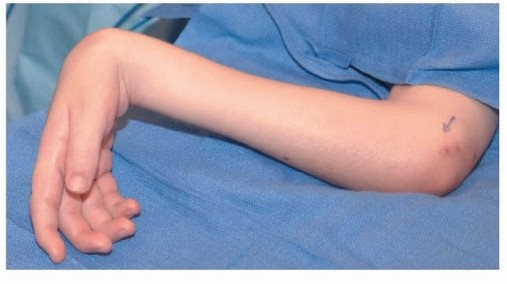
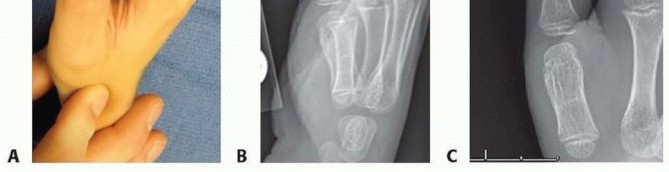
Thumb and Finger Reconstruction: Single-Stage Transfer of the Great Toe
Key Takeaway
The single-stage great toe-to-hand transfer is a highly effective microsurgical procedure for thumb reconstruction following traumatic amputation. By restoring an opposable digit with protective sensibility and up to 80% of native pinch strength, this technique significantly enhances hand function. Careful preoperative vascular mapping, meticulous two-team surgical execution, and precise donor site management are essential to minimize morbidity and optimize both aesthetic and biomechanical outcomes.
INTRODUCTION AND HISTORICAL PERSPECTIVE
The evolution of microsurgical tissue transfer has revolutionized the management of complex upper extremity amputations. In 1967, Cobbett reported the first successful single-stage toe-to-hand transfer in a human, marking a paradigm shift from the arduous, multi-staged pedicled flap techniques of the past. At a 30-year follow-up, Cobbett’s index patient remained gainfully employed as a timber checker, underscoring the exceptional durability and favorable long-term functional outcomes achievable with this procedure.
Since that pioneering milestone, continuous advancements in optical magnification, micro-instruments, and ultra-fine sutures have refined the transfer of the great toe to the hand. Today, the clinical utility of the great toe for thumb reconstruction—and the use of the second toe or combined second-third toes for multi-digit reconstruction—is universally confirmed. The great toe provides an unparalleled aesthetic and functional match for the thumb, offering glabrous skin, a robust nail complex, and a broad bony architecture that facilitates powerful pinch and grasp.
BIOMECHANICS AND CLINICAL OUTCOMES
The primary goal of thumb reconstruction is the restoration of a sensate, opposable post that can withstand the rigorous demands of daily activities.
Functional Restoration of the Hand
Following a successful great toe-to-hand transfer, patients reliably regain protective sensibility, which is paramount for preventing inadvertent injury to the reconstructed digit. Two-point discrimination often approaches 8 to 12 mm, depending on the patient's age and the quality of the neural repair. Pinch strength is typically restored to 40% to 80% of the contralateral, uninjured side. Furthermore, the psychological benefit cannot be overstated; almost all patients report high satisfaction with the aesthetic appearance of the reconstructed thumb, as the great toe closely mimics the native thumb's contour and nail plate.
Donor Site Morbidity and Foot Biomechanics
A common preoperative concern is the biomechanical impact of great toe amputation on gait and weight-bearing. Extensive biomechanical evaluations and gait analyses suggest that no significant limitation in routine ambulatory activities results from the loss of the great toe, provided the first metatarsal head is meticulously preserved. The first metatarsal head is the primary weight-bearing structure of the medial forefoot; its resection inevitably leads to transfer metatarsalgia and severe gait disturbances.
Clinical Pearl: Preservation of the first metatarsal head and the sesamoid complex is non-negotiable for maintaining normal foot biomechanics. If the thumb defect requires a longer bony segment (e.g., total first metacarpal loss), alternative reconstructive options such as pollicization or an osteocutaneous flap should be strongly considered over harvesting the first metatarsal.
Despite favorable gait outcomes, significant donor site morbidity can occur. Complications frequently include delayed healing of skin-grafted areas and residual hypertrophic scarring on the dorsum of the foot. These issues can be systematically minimized through meticulous dissection, strategic flap design, tension-free closure of the donor defect, and strict adherence to postoperative offloading protocols.
INDICATIONS AND PATIENT SELECTION
The decision to proceed with a great toe-to-hand transfer requires a comprehensive assessment of the defect, the patient's physiological status, and their functional demands.
Primary Indications
Transfer of the great toe to the hand is primarily indicated for:
* Thumb Amputations: Reconstruction of the thumb following amputations ranging from the level of the metacarpal base to the interphalangeal (IP) joint.
* Multiple Digit Amputations: This procedure is exceptionally valuable in hands with multiple injuries and amputations, as it provides a critical opposable post for any remaining digits, thereby salvaging basic hand function.
* Proximal Amputations: Toe-to-hand transfer is highly recommended for the reconstruction of a thumb lost at or near the metacarpophalangeal (MCP) joint, particularly when no adjacent, expendable digits are available for pollicization.
Relative Contraindications and Controversies
Posttraumatic thumb loss that includes the entire first metacarpal presents a reconstructive dilemma. Harvesting the first metatarsal from the foot to reconstruct the thumb metacarpal severely impairs ambulation. Therefore, total thumb loss is generally better treated by index finger pollicization, second toe transfer (which allows for metatarsal harvest with less morbidity), or a staged osteoplastic reconstruction.
Before embarking on this major reconstructive effort, the surgeon must carefully evaluate:
* Patient Age and Health: Advanced age, severe peripheral vascular disease, and active tobacco use are significant risk factors for microvascular thrombosis and flap failure.
* Motivation and Compliance: The postoperative rehabilitation process is lengthy and demands strict patient compliance.
* Occupational Demands: High-demand manual laborers may benefit more from the robust bony architecture of the great toe, whereas patients prioritizing foot aesthetics or elite athletic performance may prefer alternative donor sites.
The great toe is generally preferred over the second toe for thumb reconstruction because the lesser toes are significantly thinner and shorter, resulting in a reconstructed thumb that is functionally weaker and aesthetically mismatched.
PREOPERATIVE PLANNING AND VASCULAR MAPPING
Meticulous preoperative planning is the cornerstone of a successful microvascular transfer. As with all free tissue transfers from the lower extremity, a thorough evaluation of the vascular anatomy is mandatory.
Vascular Evaluation
- Clinical Examination: Assess pedal pulses (dorsalis pedis and posterior tibial arteries) and perform an Allen test of the foot to ensure adequate collateral perfusion to the lesser toes.
- Doppler Ultrasonography: Use a handheld Doppler probe to trace and mark the course of the dorsalis pedis artery and the first dorsal metatarsal artery (FDMA).
- Angiography: Arteriography of the foot in two planes (or high-resolution CT Angiography) is highly recommended to delineate the arterial dominance of the first web space. The FDMA exhibits significant anatomical variance (Gilbert's classification), and knowing whether the dominant supply is dorsal or plantar dictates the surgical approach.
- Hand Angiography: If there is any doubt regarding the status of the potential recipient vessels in the traumatized hand, an upper extremity angiogram should be obtained to identify suitable arterial targets (e.g., radial artery in the anatomical snuffbox) and ensure adequate venous outflow.
Templating and Soft Tissue Planning
Although the ipsilateral great toe is traditionally utilized, the contralateral great toe should be considered if the medial skin of the foot is required to resurface a specific soft tissue defect on the reconstructed thumb.
Surgical Pearl: Utilizing clay or silicone models of the toe placed in the thumb position is an invaluable technique (championed by Buncke) for determining the exact toe selection, the required angle of osteotomy, and the precise amount of skin needed.
The soft tissue requirements of the recipient hand must be satisfied either prior to the toe transfer (via traditional coverage techniques such as pedicled groin flaps) or simultaneously by incorporating a dorsal foot flap (dorsalis pedis flap) with the great toe transfer. Generally, it is preferable to plan for split-thickness skin grafting on the recipient hand rather than the donor foot, as skin grafts on the dorsum of the foot yield unpredictable results and are prone to breakdown from footwear friction.
SURGICAL TECHNIQUE: THE BUNCKE MODIFIED APPROACH
The single-stage transfer is a complex, choreographed procedure requiring two skilled microsurgical teams operating simultaneously to minimize ischemia time.
Preparation and Setup
- Physiological Monitoring: Monitor urinary output with an indwelling urinary catheter. Maintain core body temperature using a heating and cooling blanket, monitored via esophageal or rectal temperature probes. Hypothermia induces vasospasm and must be strictly avoided.
- Two-Team Approach: One team prepares the recipient hand, isolating the recipient vessels, nerves, and tendons, while the second team harvests the great toe.
- Marking: Using skin-marking pencils, outline the incisions on both the hand and foot, ensuring adequate soft tissue coverage for the anastomoses and osteosynthesis sites.
Foot Dissection: Venous and Arterial Isolation
- Venous Mapping: Allow the veins to fill by holding the foot in a dependent position over the edge of the operating table. The large superficial veins on the dorsum of the foot, particularly the tributaries to the greater saphenous system located on the medial side of the first metatarsal, should be easily visualized and marked prior to exsanguination.
- Tourniquet Control: Exsanguinate the limb by elevation or careful wrapping, and inflate the pneumatic tourniquet.
- Dorsal Incisions: Utilize straight, curved, or zigzag dorsal incisions to identify and preserve the dorsal venous network. Dissect the veins proximally to develop a long venous pedicle.
- Arterial Dissection (Dorsal Dominance): Identify the dorsalis pedis artery and its distal continuation, the FDMA. If preoperative imaging confirms a dorsal FDMA, proceed with dissection from proximal to distal, carefully protecting the artery and ligating or clipping any side branches.
- Arterial Dissection (Plantar Dominance): If the dominant artery is plantar, alter the approach. Dissect from the first web space proximally, extending a longitudinal plantar incision just lateral to the weight-bearing area of the plantar surface over the first metatarsal head. Dissect proximally to obtain sufficient arterial length. It is often necessary to divide the transverse metatarsal ligament to fully mobilize a plantar metatarsal artery.
- The "In Doubt" Approach: If the location of the dominant vessel remains ambiguous intraoperatively, begin the dissection in the first web space and dissect proximally. Ligate the arterial branch to the second toe and mobilize the first metatarsal artery proximally until its dorsal or plantar origin is definitively determined.
Surgical Warning: Never transect the proximal vascular attachments until complete vascularization through the arteriovenous pedicle to the great toe is ensured, and until the hand dissection team has confirmed that the recipient site is fully prepared. Premature amputation of the toe unnecessarily prolongs the critical ischemia time.
Neural Dissection
- Deep Peroneal Nerve: Follow the dorsal artery to the extensor hallucis brevis muscle. Divide and elevate the muscle to expose the deep peroneal nerve, which lies lateral to the dorsalis pedis artery. Preserve a generous length of this nerve for coaptation to a recipient nerve (e.g., superficial radial nerve branches) in the thumb area to restore dorsal sensibility.
- Plantar Digital Nerves: In the first web space, identify the plantar digital nerve on the lateral side of the great toe. Carefully separate it from the digital nerve to the second toe by performing an intraneural dissection proximally into the common digital nerve. Similarly, dissect the plantar digital nerve on the medial side of the great toe, mobilizing it as far proximally as possible. Both digital nerves must be preserved for coaptation to the digital nerves of the thumb.
Tendon and Bone Harvest
- Tendons: Isolate and transect the extensor hallucis longus (EHL) and flexor hallucis longus (FHL) tendons as proximally as required to bridge the defect in the hand.
- Osteotomy: Perform the osteotomy at the planned level (usually the proximal phalanx or the metatarsophalangeal joint). Ensure the first metatarsal head is preserved and its articular cartilage is contoured or covered to prevent painful neuromas or bursitis.
Recipient Hand Preparation and Anastomosis
- Osteosynthesis: Transfer the toe to the hand. Rigid skeletal fixation is achieved first, utilizing crossed Kirschner wires, intraosseous wiring, or miniature titanium plates and screws. Proper pronation and palmar abduction of the transferred digit are critical for functional opposition.
- Tendon Repair: Repair the extensor and flexor tendons using standard core suture techniques. Adjust tension to match the resting cascade of the hand.
- Microvascular Anastomosis: Under the operating microscope, perform the arterial anastomosis (typically end-to-end to the radial artery or a major branch) and the venous anastomoses (to the cephalic vein or dorsal venous system). Ensure there is no tension or kinking of the pedicle.
- Nerve Coaptation: Perform epineurial repairs of the plantar digital nerves to the proper digital nerves of the thumb, and the deep peroneal nerve to the dorsal sensory branches of the radial nerve.
Donor Site Closure
Meticulous closure of the foot is vital to minimize morbidity. The capsule of the first metatarsophalangeal joint should be closed if possible. Local advancement flaps or full-thickness skin grafts may be required. A split-thickness skin graft should only be used over healthy muscle beds, never over bare bone or tendon. Apply a bulky, non-compressive dressing and a posterior splint to maintain the foot in a neutral position.
POSTOPERATIVE MANAGEMENT AND REHABILITATION
The postoperative phase is as critical as the surgical execution.
Flap Monitoring
The patient is monitored in a specialized microsurgical unit. The transferred digit is assessed hourly for the first 48 hours, evaluating color, capillary refill, tissue turgor, and temperature. An implantable venous Doppler or surface Doppler is utilized to confirm pedicle patency. The ambient room temperature must be kept warm to prevent vasospasm.
Anticoagulation and Medications
Protocols vary by institution, but most regimens include intravenous hydration, aspirin, and prophylactic low-molecular-weight heparin. Dextran or continuous heparin infusions are reserved for cases with intraoperative thrombotic complications or poor flow.
Rehabilitation Protocol
- Weeks 0-3: The hand is immobilized in a bulky protective splint. The foot is kept strictly elevated and non-weight-bearing to promote graft take and wound healing.
- Weeks 3-6: Gentle, controlled active range of motion (AROM) of the reconstructed thumb is initiated under the guidance of a specialized hand therapist. Partial weight-bearing on the heel of the donor foot may begin, utilizing a rigid postoperative shoe.
- Weeks 6-12: Passive range of motion (PROM) and progressive strengthening are introduced once radiographic evidence of bony union is confirmed. Full weight-bearing is gradually resumed. Sensory re-education begins once advancing Tinel's signs reach the fingertip.
COMPLICATIONS AND PITFALLS
- Vascular Thrombosis: The most devastating complication is arterial or venous thrombosis, typically occurring within the first 72 hours. Immediate return to the operating room for exploration, thrombectomy, and potential vein grafting is mandatory to salvage the transfer.
- Donor Site Morbidity: Delayed wound healing on the foot is common, particularly if skin grafts are placed over avascular beds. Hypertrophic scarring can cause discomfort with footwear. Strict adherence to offloading and the use of custom orthotics can mitigate these issues.
- Cold Intolerance: As with many replantations and free flaps, patients frequently experience cold intolerance in the reconstructed digit, which may persist for years but generally improves over time.
- Nonunion/Malunion: Failure of osteosynthesis requires revision bone grafting and rigid internal fixation. Precise initial bone cuts and robust fixation are the best prevention.
By adhering to strict microsurgical principles, comprehensive preoperative planning, and rigorous postoperative care, the single-stage great toe transfer remains the gold standard for restoring form and function to the severely mutilated hand.
You Might Also Like