INTRODUCTION TO ORTHOPAEDIC SOFT TISSUE RECONSTRUCTION
In the realm of operative orthopaedics and trauma surgery, the management of soft tissue defects is as critical as the stabilization of the underlying osseous structures. When a severe injury or surgical extirpation results in a skin defect that leaves deep, avascular structures exposed, the reconstructive surgeon must ascend the "reconstructive ladder."
A split-thickness skin graft (STSG) or full-thickness skin graft (FTSG) is fundamentally insufficient for the coverage of exposed nerves, tendons devoid of paratenon, and bare cortical bone devoid of periosteum. These deep structures do not possess the requisite capillary beds to readily support the physiological phases of graft take (plasmatic imbibition, inosculation, and angiogenesis). Consequently, a skin flap becomes an absolute necessity. Flaps provide not only the essential subcutaneous tissue bulk required for mechanical protection and gliding surfaces but also bring an intrinsic, robust vascularity that ensures tissue survival over avascular beds.
Clinical Pearl: The modern orthopaedic surgeon must view soft tissue and bone as a single, integrated functional unit. The survival of a complex intra-articular fracture fixation or a tendon repair is entirely dependent on the viability of the overlying soft tissue envelope.
CLASSIFICATION AND NOMENCLATURE OF SKIN FLAPS
The nomenclature of skin flaps is highly systematic, categorized primarily by their anatomical location, intrinsic blood supply, tissue composition, and the specific technique of transfer. Mastery of this classification is essential for preoperative planning and intraoperative decision-making.
Classification by Location
- Local Flaps: Harvested from tissue immediately adjacent to the primary defect. These include advancement, rotation, and transposition flaps. They offer the advantage of matching skin color, texture, and thickness.
- Regional Flaps: Harvested from the same anatomical region or limb but not immediately adjacent to the defect (e.g., a cross-finger flap or a reverse radial forearm flap).
- Distant Flaps: Harvested from a remote anatomical site. These can be pedicled (e.g., a groin flap attached to the hand) or transferred as free tissue.
Classification by Blood Supply
The vascular architecture of a flap dictates its design limits, specifically its length-to-width ratio, and its ultimate reliability.
* Random Pattern Flaps: These flaps receive their circulation exclusively through the unnamed, diffuse subdermal or subcutaneous plexus of vessels. Because they lack a primary axial vessel, their length-to-width ratio is strictly limited (traditionally 1:1 or 2:1 in the lower extremity, up to 3:1 in the highly vascularized face) to prevent distal tip necrosis.
* Axial Pattern Flaps: These flaps are supplied by a recognized, named anatomically consistent artery and its accompanying venae comitantes. The inclusion of this direct vascular axis allows for the design of much longer flaps, independent of traditional length-to-width ratios, provided the territory of the vessel (the angiosome) is respected.
Classification by Tissue Composition
Axial flaps are further subdivided based on the primary tissues incorporated into the transfer:
* Cutaneous Flaps: Consisting of skin and subcutaneous fat.
* Fasciocutaneous Flaps: Incorporating the deep fascia, which contains a rich prefascial and subfascial vascular plexus, significantly enhancing flap reliability.
* Musculocutaneous Flaps: Incorporating a muscle belly and its overlying skin, supplied by musculocutaneous perforators. These are ideal for obliterating deep dead spaces and providing robust coverage over infected bone (e.g., in chronic osteomyelitis).
Classification by Technique of Transfer
- Pedicled Flaps: The flap remains attached to its donor site vascular base (the pedicle) while the distal end is transposed to the defect. This often requires a two-stage procedure, with pedicle division occurring 2 to 3 weeks later once neovascularization from the recipient bed is established.
- Free Flaps: The flap is completely detached from the donor site, and its vascular pedicle is anastomosed to recipient vessels at the defect site using microsurgical techniques. This allows for single-stage reconstruction of massive defects.
COVERAGE OF SPECIFIC AREAS: THE DIGITS AND HAND
The hand presents unique reconstructive challenges due to its dense concentration of critical structures, lack of redundant soft tissue, and the paramount importance of preserving motion and sensation.
Fingertip Injuries and Amputations
Fingertip injuries are among the most common hand traumas encountered in the emergency department. The treatment algorithm is dictated by the size of the defect, the presence of exposed bone, and the geometry of the amputation (transverse, volar oblique, or dorsal oblique).
Defects with isolated skin loss measuring less than 1 cm² can usually be treated satisfactorily with conservative management, allowing healing by secondary intention. This approach often yields excellent functional results with minimal joint stiffness. If the defect is larger but lacks exposed bone, a full-thickness skin graft (FTSG) provides superior coverage compared to an STSG, offering less secondary contracture and a higher potential for the return of protective sensation.
The Purse-String Suture Technique (Hassanpour et al.)
For transverse or slightly oblique fingertip amputations with exposed bone, conventional local flaps (such as V-Y advancement flaps) are standard. However, Hassanpour et al. described an elegant and highly effective modification: the use of a purse-string suture in conjunction with flap coverage. This technique is designed to restore the natural contour of the fingertip, centralize the soft tissue pulp, and improve both aesthetic and functional outcomes.
Surgical Steps for the Purse-String Technique:
-
Preparation and Design: The amputated stump is meticulously debrided. A V-shaped volar advancement flap (Atasoy-Kleinert type) is designed.

(Figure A: The transverse amputation defect is assessed, and the V-shaped flap is designed over the volar pulp, ensuring the apex does not cross the distal interphalangeal joint crease.) -
Dissection and Advancement: The flap is incised through the dermis. Crucially, the fibrous septa connecting the skin to the distal phalanx are carefully divided to allow the flap to advance distally without tension, while preserving the neurovascular bundles entering the base of the flap.

(Figure B: The flap is mobilized and advanced distally to cover the exposed distal phalanx. Tension-free advancement is critical to prevent vascular compromise.) -
Purse-String Closure: Instead of standard interrupted sutures, a continuous purse-string suture (often using a monofilament non-absorbable suture like 4-0 or 5-0 Prolene) is woven through the dermal edges of the advanced flap and the surrounding native skin of the amputation stump.
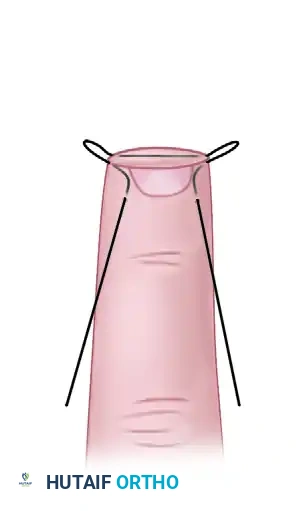
(Figure C: The two ends of the continuous purse-string suture are gently pulled. This action cinches the tissue centrally, creating a rounded, natural curve to the new fingertip and minimizing the dog-ear deformities typical of standard V-Y closures.)
Surgical Warning: When applying the purse-string tension, the surgeon must carefully assess capillary refill. Over-tightening the purse-string can strangulate the microcirculation of the advanced flap, leading to marginal or complete necrosis.
In their series of 41 fingertip amputations, Hassanpour et al. reported excellent or good cosmetic results in 100% of female patients and 81% of male patients, with only one poor functional result, highlighting the efficacy of this complementary technique.
Dorsal Digital Defects
A large skin defect on the dorsum of a finger that exposes the extensor mechanism devoid of paratenon represents an absolute indication for flap coverage. Skin grafts placed directly on bare tendon will fail, leading to tendon desiccation, necrosis, and rupture.
- Double Local Flaps: For moderate dorsal defects, a double local flap technique can be highly effective. This involves constructing two transposition flaps: a proximally based local flap rotated from one side of the defect, and a distally based local flap rotated from the contralateral side. Together, they meet over the exposed tendon. The resulting secondary donor defects, which now possess a vascularized bed of subcutaneous tissue and paratenon, are subsequently covered with split-thickness skin grafts.
- Reverse Cross-Finger Flap: For more proximal dorsal injuries where local rotational flaps from the same digit are insufficient, a reverse cross-finger flap is indicated. Unlike a standard cross-finger flap (which transfers volar skin to a volar defect), the reverse technique harvests the subcutaneous tissue and fascia from the dorsum of an adjacent, healthy finger. The skin of the donor finger is elevated as a thin, full-thickness door; the underlying vascularized subcutaneous tissue is flipped over like a page in a book to cover the defect on the injured finger; and finally, an STSG is placed over the transferred subcutaneous tissue. The donor site skin is then sutured back into place.
Proximal Palmar and Dorsal Digital Defects
For larger defects at the base of the digits or the proximal web spaces, an axial pattern flap is preferred. The "Flag" flap is a classic example. This is a fasciocutaneous axial flap based on the dorsal metacarpal arteries (usually the first or second DMA). The flap is designed on the dorsum of the proximal phalanx or metacarpal, elevated with its vascular pedicle, and rotated (like a flag on a pole) to cover proximal palmar or dorsal digital defects. Its axial blood supply makes it highly reliable.
Extensive Hand and Multiple Digit Trauma
When multiple fingers are involved, or a massive soft tissue avulsion occurs (e.g., a degloving injury or "roller-press" injury), local and regional hand flaps are entirely inadequate. Distant pedicled flaps or free tissue transfers are required.
- Subpectoral and Groin Flaps: Historically, the pedicled groin flap (based on the superficial circumflex iliac artery) or subpectoral flaps were the workhorses for massive hand coverage. The injured hand is surgically attached to the abdomen or chest wall, and the flap is divided 3 weeks later.
- The "Fat" Pitfall: A major limitation of distant pedicled flaps from the trunk is the thickness of the subcutaneous fat. Thick subcutaneous fat, particularly from the lower abdomen, is highly undesirable on the hand. It creates a bulky, insensate, "boxing glove" deformity that severely restricts joint mobilization and tendon gliding. Extensive, staged defatting procedures are almost always required postoperatively. Today, thin fasciocutaneous free flaps (e.g., anterolateral thigh flap in thin patients, or lateral arm flap) are generally preferred over pedicled trunk flaps to minimize this bulk.
PRINCIPLES OF SKIN GRAFTING IN ORTHOPAEDICS
While flaps are required for exposed deep structures, skin grafts remain a cornerstone of orthopaedic soft tissue management for appropriately vascularized beds (e.g., muscle, fascia, paratenon, periosteum, or healthy granulation tissue).
Preoperative Wound Bed Preparation
A skin graft cannot survive in the presence of gross infection or necrotic tissue. Prior to grafting, the wound must be meticulously debrided.
* Sepsis Identification: The bacterial bioburden must be controlled. Sepsis can be identified via surface swabs for culture, but a tissue biopsy for a quantitative colony count is the gold standard. A wound bed with greater than $10^5$ colony-forming units (CFU) per gram of tissue, or the presence of any beta-hemolytic Streptococcus, is an absolute contraindication to skin grafting.
Physiology of Graft Survival
For a graft to survive, it must rapidly reestablish its nutrition before ischemic necrosis of its entire thickness occurs. This occurs in three distinct phases:
1. Plasmatic Imbibition (Days 0-2): The graft passively absorbs serum and nutrients from the recipient bed via capillary action. The graft becomes edematous and increases in weight.
2. Inosculation (Days 2-4): Capillary buds from the recipient bed align and fuse with the severed capillary networks within the graft dermis.
3. Angiogenesis/Neovascularization (Days 4+): New blood vessels actively grow into the graft, establishing definitive circulation.
Causes of Graft Failure
Great care is required in both operative technique and postoperative aftercare to ensure the graft remains undisturbed and in direct, continuous contact with the recipient bed.
* Hematoma/Seroma: The most common cause of graft failure. A hematoma acts as a physical barrier, preventing plasmatic imbibition and inosculation. Meticulous hemostasis, meshing of the graft (to allow fluid egress), and the use of bolster dressings or negative pressure wound therapy (NPWT) are critical preventative measures.
* Shear Forces: Movement between the graft and the bed tears the fragile neovascular connections during the inosculation phase. Immobilization is paramount, which requires careful planning, especially in pediatric populations where compliance is challenging.
Graft Selection in the Hand
- Split-Thickness Skin Grafts (STSG): For primary coverage of acute wounds with vascularized beds, thin or medium-thickness STSGs are standard. They have lower metabolic demands than FTSGs and thus have a higher "take" rate. However, they contract significantly during healing and offer poor durability over pressure points.
- Full-Thickness Skin Grafts (FTSG): FTSGs contain the entire epidermis and dermis. They are used infrequently in acute hand trauma due to their higher metabolic demand and uncertain survival. However, they are the graft of choice for the palmar surface of the hand in elective reconstruction (e.g., syndactyly release or Dupuytren's contracture release). The palm requires elastic tissue to accommodate extension, and FTSGs contract far less than STSGs. Furthermore, in growing children, FTSGs tend to accommodate skeletal growth better than STSGs.
Pitfall: Never place a skin graft over bare cortical bone, bare tendon, or bare cartilage. The lack of a vascularized bed guarantees graft necrosis. If periosteum or paratenon has been stripped, a flap is mandatory.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The postoperative management of skin flaps and grafts is as critical as the surgical execution.
Flap Monitoring
For axial and free flaps, intensive monitoring is required for the first 72 hours. Clinical assessment of color, capillary refill, tissue turgor, and temperature is paramount. Venous congestion (flap appears blue, swollen, with brisk capillary refill) is more common than arterial insufficiency (flap appears pale, cool, with absent capillary refill) and requires immediate surgical re-exploration if identified.
Immobilization and Mobilization
- Skin Grafts: The grafted area must be strictly immobilized for 5 to 7 days to prevent shear forces. Splinting should place the hand in the intrinsic-plus position (safe position) to prevent collateral ligament contracture, unless the specific location of the graft dictates otherwise.
- Flaps: While the pedicle or anastomosis must be protected from tension and compression, early protected mobilization of the underlying tendons and joints is initiated as soon as the flap is deemed viable (often within 3 to 5 days). This prevents debilitating adhesions between the flap and the underlying repaired structures.
Long-Term Care
Once healed, both flaps and grafts lack normal sebaceous and sweat gland function initially. Patients must be educated on daily lubrication with non-perfumed emollients and strict sun protection to prevent hyperpigmentation and desiccation. Sensory re-education programs are instituted for neurosensory flaps or FTSGs to maximize functional recovery.
