Mastering SC Joint Dislocations: Diagnosis & Treatment Insights
Key Takeaway
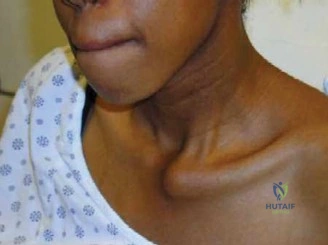
Your ultimate guide to Mastering SC Joint Dislocations: Diagnosis & Treatment Insights starts here. **SC joint dislocations** involve displacement of the sternoclavicular joint. Patients typically experience severe pain, often supporting the injured arm with a tilted head. Anterior dislocations may show a prominent medial clavicle. Posterior dislocations, though rarer, can cause venous congestion, numbness, and tingling, requiring careful evaluation due to associated risks.
Introduction and Epidemiology
Sternoclavicular joint dislocations, while rare, represent a distinct clinical challenge within orthopedic trauma. Constituting less than 3 percent of all shoulder girdle injuries and less than 1 percent of all dislocations, their infrequency belies their potential for significant morbidity. The mechanism of injury typically involves high-energy trauma, often from motor vehicle accidents or direct sports-related impact.
Dislocations are broadly classified based on the direction of clavicular displacement relative to the sternum. Anterior dislocations are the most common type, accounting for approximately 90 percent of sternoclavicular joint dislocations. The medial clavicle displaces anteriorly and superiorly. While generally considered less dangerous than posterior dislocations, they can cause chronic pain, instability, and cosmetic deformity. Posterior dislocations represent a critical injury, comprising approximately 10 percent of sternoclavicular joint dislocations. The medial clavicle displaces posteriorly into the superior mediastinum. Due to the proximity of vital structures, including the trachea, esophagus, subclavian vessels, brachial plexus, and pleura, posterior dislocations carry a substantial risk of life-threatening complications, including airway obstruction, vascular injury, and pneumothorax.
Further classifications include acute injuries presenting less than three weeks from injury, subacute injuries presenting between three weeks and three months, and chronic injuries greater than three months from injury. Injuries are also delineated as complete versus incomplete based on the degree of ligamentous disruption, and open versus closed. Open dislocations are surgical emergencies due to infection risk and potential for greater soft tissue damage.
A critical diagnostic nuance in the young adult population involves the medial clavicular epiphysis. The medial clavicle possesses the last physeal plate to close in the human body, typically fusing between 22 and 25 years of age. Consequently, injuries presenting as sternoclavicular dislocations in patients under 25 are frequently Salter-Harris type I or II fractures of the medial clavicle. Accurate diagnosis and timely intervention are paramount, particularly for posterior displacements, to mitigate severe complications and optimize long-term functional outcomes.
Surgical Anatomy and Biomechanics
The sternoclavicular joint is a diarthrodial saddle joint, unique for its ability to provide significant mobility while maintaining remarkable stability. It is the sole bony articulation between the upper extremity and the axial skeleton.
Articular Surfaces and Disc
The medial end of the clavicle articulates with the manubrium sterni and the first costal cartilage. These surfaces are incongruent, with the clavicular facet being larger than the sternal facet. A crucial biconcave fibrocartilaginous disc resides within the joint. It acts as a shock absorber, improves joint congruity, and divides the joint into two separate synovial cavities. The disc attaches superiorly to the posterosuperior aspect of the clavicle, inferiorly to the first costal cartilage, and anteriorly and posteriorly to the joint capsule.
Ligamentous Stabilizers
A robust fibrous capsule encloses the joint, reinforced by several primary stabilizing ligaments. The anterior sternoclavicular ligament consists of thick, broad fibers coursing from the anterosuperior clavicle to the anterior manubrium, resisting anterior and superior displacement. The posterior sternoclavicular ligament is thinner but stronger than the anterior ligament, extending from the posterosuperior clavicle to the posterior manubrium. It is the primary restraint against posterior displacement and thus critical in preventing mediastinal compromise.
The interclavicular ligament connects the superior aspects of the medial clavicles, crossing the superior aspect of the manubrial notch. It resists superior displacement of the clavicle and transmits forces between the two clavicles. Finally, the costoclavicular ligament, often referred to as the rhomboid ligament, is arguably the most important primary stabilizer of the sternoclavicular joint. It consists of anterior and posterior laminae, extending from the superior surface of the first rib and costal cartilage to the inferior surface of the medial clavicle. It restricts all clavicular movements except for inferior glide, acting as a central pivot point for shoulder girdle elevation and rotation.
Mediastinal Proximity and Danger Zone
The retrosternal anatomy dictates the high morbidity associated with posterior dislocations. The "danger zone" immediately posterior to the sternoclavicular joint contains the innominate artery and vein, the left common carotid artery, the left subclavian vein, the internal jugular vein, the vagus and phrenic nerves, the trachea, and the esophagus. The distance from the posterior aspect of the medial clavicle to these vital structures can be as little as five to ten millimeters. Consequently, posterior displacement requires immediate clinical attention and high suspicion for neurovascular or airway compromise.
Indications and Contraindications
The management of sternoclavicular joint dislocations is dictated by the direction of the dislocation, the acuity of the injury, the presence of mediastinal symptoms, and patient-specific functional demands.
Operative Indications
Posterior dislocations mandate urgent intervention. While closed reduction is the first-line treatment for acute posterior dislocations, operative management is indicated if closed reduction fails, if the joint remains highly unstable post-reduction, or if there is any evidence of neurovascular, tracheal, or esophageal compromise. Open reduction and internal reconstruction are also indicated for chronic posterior dislocations that are symptomatic, though these present significant surgical challenges.
For anterior dislocations, operative indications are much narrower. Acute anterior dislocations are almost universally managed non-operatively, as closed reductions are notoriously unstable, and the functional outcomes of unreduced anterior dislocations are generally excellent. Operative intervention for anterior dislocations is reserved for chronic, highly symptomatic instability in active patients, severe cosmetic deformity that the patient finds intolerable, or failure of conservative management.
Non Operative Indications
Non-operative management is the gold standard for acute and chronic anterior dislocations without significant pain or functional limitation. Acute posterior dislocations that are successfully reduced closed and demonstrate stability can also be managed non-operatively, provided the patient is monitored closely for delayed mediastinal complications.
Operative Versus Non Operative Management
| Injury Type | Non Operative Indications | Operative Indications |
|---|---|---|
| Acute Anterior Dislocation | Standard of care for nearly all cases; benign neglect | Open fracture; severe skin tenting threatening necrosis |
| Chronic Anterior Dislocation | Asymptomatic or minimally symptomatic patients | Intractable pain; severe functional limitation; overhead athletes |
| Acute Posterior Dislocation | Successful, stable closed reduction; absence of mediastinal symptoms | Failed closed reduction; neurovascular compromise; airway obstruction |
| Chronic Posterior Dislocation | Asymptomatic patients with incidental findings | Dysphagia; dyspnea; thoracic outlet syndrome symptoms; chronic pain |
| Medial Clavicle Physeal Fracture | Minimally displaced fractures; stable reductions | Severe displacement with mediastinal impingement; open fractures |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is critical, particularly for posterior dislocations, given the potential for catastrophic intraoperative complications.
Advanced Imaging Protocols
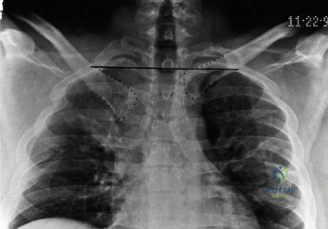
Standard radiography includes an anteroposterior view of the chest and a Serendipity view. The Serendipity view is obtained with the patient supine and the x-ray beam angled 40 degrees cephalad, centered on the manubrium. This view allows for comparison of the bilateral medial clavicles. In an anterior dislocation, the affected clavicle will appear superior to the uninjured side. In a posterior dislocation, the affected clavicle will appear inferior.
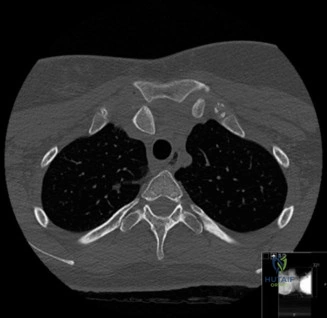
Despite the utility of the Serendipity view, computed tomography is the gold standard for evaluating sternoclavicular joint pathology. A CT scan of the chest with intravenous contrast should be obtained for all suspected posterior dislocations. Axial, coronal, and sagittal reconstructions clearly delineate the direction of displacement, the presence of physeal fractures in younger patients, and the relationship of the medial clavicle to the retrosternal vascular and aerodigestive structures. A CT angiogram is strongly recommended to rule out intimal tears, pseudoaneurysms, or direct compression of the great vessels.

Multidisciplinary Coordination
For posterior dislocations requiring open reduction, the presence or immediate availability of a cardiothoracic or vascular surgeon is mandatory. The surgical team must be prepared for emergent sternotomy or thoracotomy if a great vessel is lacerated during the reduction maneuver or dissection. Cross-matched blood should be available in the operating room.
Operating Room Setup and Positioning
The patient is placed in the supine position on a radiolucent operating table. A bump or rolled towel is placed between the scapulae to allow the shoulders to fall posteriorly, which aids in the reduction of anterior dislocations and facilitates surgical access. The operative arm must be prepped and draped free to allow for full range of motion, which is essential for intraoperative reduction maneuvers and assessing joint stability after reconstruction. The anterior chest is prepped from the chin to the costal margins, extending laterally past the bilateral acromioclavicular joints.
Detailed Surgical Approach and Technique
The surgical management of sternoclavicular joint dislocations has evolved significantly. The historical use of Kirschner wires or Steinman pins across the joint is now universally condemned due to the well-documented and potentially fatal complication of hardware migration into the heart, lungs, or great vessels. Current techniques rely on soft tissue reconstruction.
Closed Reduction Techniques
For acute anterior dislocations, closed reduction is rarely attempted, as the joint almost invariably re-dislocates. For acute posterior dislocations, closed reduction should be attempted in the operating room under general anesthesia with muscle relaxation.
The standard closed reduction maneuver is the abduction-traction technique. The patient is positioned supine with a bump between the scapulae. The arm is abducted to 90 degrees and extended. Inline traction is applied to the arm while an assistant provides counter-traction to the thorax. If the clavicle does not reduce, the surgeon can grasp the medial clavicle with a sterile towel clip percutaneously and apply direct anterior traction. A palpable clunk usually indicates successful reduction. The joint is then assessed for stability.
Open Surgical Approach
If open reduction is required, an anterior approach to the sternoclavicular joint is utilized. A transverse or lazy-S incision is made centered over the sternoclavicular joint, extending from the medial third of the clavicle to the midline of the manubrium. Subcutaneous tissues are dissected, and hemostasis is meticulously maintained.
The platysma is divided in line with the incision. The supraclavicular nerves should be identified and protected if possible, though sacrifice of medial branches may be necessary and results in a predictable patch of anterior chest numbness. The periosteum of the medial clavicle and the anterior capsule of the sternoclavicular joint are exposed.
For posterior dislocations, extreme care must be taken during the deep dissection. The anterior capsule is incised, and subperiosteal dissection is performed on the medial clavicle. A malleable retractor must be carefully placed posterior to the medial clavicle to protect the mediastinal structures before any drilling or extensive manipulation occurs.
Graft Reconstruction Techniques
The gold standard for stabilizing an unstable sternoclavicular joint is a figure-of-eight tendon graft reconstruction, as popularized by Spencer and Kuhn. This technique relies on reconstructing the anterior and posterior sternoclavicular ligaments using an autograft or allograft, typically the semitendinosus, gracilis, or palmaris longus.
Following open reduction of the joint, drill holes are created to accept the graft. Using a 4.0 millimeter or 4.5 millimeter drill bit, two holes are drilled in the medial clavicle and two holes are drilled in the manubrium. The holes in the clavicle are placed approximately 15 millimeters lateral to the articular margin, one superior and one inferior, directed from anterior to posterior. The holes in the manubrium are placed similarly, 15 millimeters medial to the articular margin.
A malleable retractor must be firmly held behind the bone during all drilling to prevent plunging into the mediastinum. The drill holes are then connected using a curette to create tunnels.
The tendon graft is passed through the drill holes in a figure-of-eight fashion. The graft is passed from anterior to posterior through the inferior manubrial hole, then posterior to anterior through the superior clavicular hole. It crosses the joint anteriorly, passes from anterior to posterior through the superior manubrial hole, and finally posterior to anterior through the inferior clavicular hole.
The joint is held in anatomic reduction while the graft is tensioned and sutured to itself using high-strength, non-absorbable sutures. Additional fixation can be achieved by suturing the graft to the native capsular remnants. The wound is irrigated, and the fascial layers and skin are closed in a standard fashion.
Complications and Management
Surgical intervention at the sternoclavicular joint carries a unique and potentially severe complication profile. Strict adherence to safe surgical principles is required to minimize morbidity.
Intraoperative Complications
The most feared intraoperative complication is iatrogenic injury to the retrosternal structures. Drilling or placing retractors too deeply can lacerate the innominate vein, subclavian artery, or pleura. Management requires immediate packing, control of hemorrhage, and emergent consultation with cardiothoracic or vascular surgery. Preventative measures include the meticulous use of malleable retractors, utilizing drill stops, and avoiding over-penetration of the posterior cortex.
Postoperative Complications
Hardware migration is a historical complication associated with smooth pin fixation. Pins have been documented migrating into the aorta, pulmonary artery, and spinal canal, leading to fatal outcomes. This complication is the primary reason that pin fixation is absolutely contraindicated in modern sternoclavicular joint surgery.
Recurrent instability can occur, particularly in patients with generalized ligamentous laxity or those who fail to comply with postoperative immobilization protocols. Management of recurrent instability after graft reconstruction is challenging and may require revision reconstruction with a larger graft or, in extreme cases, medial clavicle excision.
Infection is a risk with any open procedure. Superficial infections are managed with oral antibiotics, while deep space infections require urgent irrigation and debridement, potentially jeopardizing the tendon graft.
Complications Incidence and Salvage Strategies
| Complication | Estimated Incidence | Salvage Strategy |
|---|---|---|
| Recurrent Dislocation | 5 to 15 percent | Revision figure-of-eight reconstruction; medial clavicle resection arthroplasty |
| Great Vessel Injury | Less than 1 percent | Emergent sternotomy; primary vascular repair; endovascular stenting |
| Infection | 2 to 4 percent | Aggressive irrigation and debridement; intravenous antibiotics; possible graft removal |
| Post Traumatic Arthritis | 10 to 25 percent | Conservative management with NSAIDs and injections; medial clavicular resection |
| Hardware Migration | Historical (High with pins) | Emergent cardiothoracic surgical retrieval; absolute avoidance of pin usage |
Post Operative Rehabilitation Protocols
Rehabilitation following sternoclavicular joint reconstruction must balance the need to protect the healing graft with the goal of restoring functional shoulder range of motion. The protocol is generally divided into three distinct phases.
Early Protective Phase
The first zero to four weeks postoperatively constitute the early protective phase. The patient is placed in a standard shoulder sling or a figure-of-eight brace. The primary goal is to protect the graft reconstruction and allow for initial soft tissue healing. All active range of motion of the shoulder is strictly prohibited. Patients are instructed to perform active range of motion of the elbow, wrist, and hand to prevent distal stiffness. Pendulum exercises may be initiated at two weeks postoperatively at the surgeon's discretion, though elevation above 45 degrees is avoided.
Intermediate Mobilization Phase
From four to eight weeks, the intermediate mobilization phase begins. The sling is gradually weaned. Passive range of motion exercises are initiated, focusing on forward elevation and external rotation. Extension and cross-body adduction are introduced cautiously, as these motions place significant stress on the sternoclavicular joint. Scapular retraction exercises and isometric deltoid strengthening can commence. Active-assisted range of motion is allowed towards the end of this phase, provided the patient is pain-free.
Advanced Strengthening Phase
The advanced strengthening phase begins at eight weeks and continues through four to six months postoperatively. Active range of motion should be full and symmetrical before progressing to heavy resistance training. Progressive resistive exercises for the rotator cuff, deltoid, and periscapular musculature are implemented. For athletes, sport-specific training can begin at three months. Return to contact sports or heavy manual labor is typically restricted until at least four to six months postoperatively, contingent upon the demonstration of full strength, absence of pain, and dynamic stability of the shoulder girdle.
Summary of Key Literature and Guidelines
The management of sternoclavicular joint dislocations is guided by several landmark studies and evolving consensus guidelines within the orthopedic community.
Landmark Studies
The biomechanical importance of the sternoclavicular ligaments was definitively described by Bearn in 1967, establishing the costoclavicular ligament as the primary restraint to superior displacement and the posterior capsule as the primary restraint to posterior displacement.
Wirth and Rockwood provided the definitive classification and management algorithm for sternoclavicular joint injuries, delineating the critical differences in the natural history of anterior versus posterior dislocations. Their work solidified the concept of "benign neglect" for most anterior dislocations and aggressive management for posterior dislocations.
The modern surgical technique for sternoclavicular joint reconstruction was established by Spencer and Kuhn in 1997. Their biomechanical study demonstrated that a figure-of-eight reconstruction using a semitendinosus graft was biomechanically superior to intramedullary ligament reconstruction and subclavius tendon reconstruction, providing stability comparable to the intact native joint.
Current Consensus Guidelines
Current orthopedic consensus strongly dictates the avoidance of any transarticular pin or wire fixation due to the catastrophic risks of migration. The standard of care for symptomatic, unstable sternoclavicular joints requiring surgery is soft tissue reconstruction, utilizing either autograft or allograft tissue in a figure-of-eight configuration.
Furthermore, consensus guidelines emphasize the necessity of advanced imaging, specifically computed tomography with angiography, for any suspected posterior dislocation. The multidisciplinary approach, ensuring the availability of a cardiothoracic surgeon during the open reduction of posterior dislocations, is considered a mandatory safety standard in contemporary orthopedic trauma surgery.
