Terrible Triad Injury of the Elbow: A Detailed Clinical Case Study & Diagnostic Imaging Analysis
Key Takeaway
A terrible triad elbow injury involves posterior elbow dislocation, radial head fracture, and coronoid process fracture, typically from a FOOSH mechanism. Diagnosis relies on clinical examination revealing deformity and pain, confirmed by X-rays showing dislocation and fractures, followed by CT for detailed surgical planning and assessment of fracture morphology.
Patient Presentation and History
We present the case of a 44-year-old right-hand dominant male who sustained a high-energy injury following a fall from a height of approximately 3 meters while working on a ladder. He landed directly on his outstretched right upper extremity, sustaining significant force transmission through his hand and forearm to the elbow joint. He presented to the emergency department with acute, severe pain in his right elbow, obvious deformity, and complete inability to move the joint. There was no reported loss of consciousness.
His medical history was unremarkable, with no known chronic conditions, previous surgeries, or allergies. He denied tobacco or illicit drug use, and consumed alcohol socially. His primary occupation involves manual labor, underscoring the critical need for optimal functional recovery of his dominant limb. The mechanism of injury, a Fall On Outstretched Hand (FOOSH) with an axial load component, is highly characteristic for elbow dislocation and associated complex injuries. The severity of the fall suggested a potentially complex injury pattern involving both osseous and ligamentous structures.
To understand the pathogenesis of this specific injury, it is imperative to analyze the biomechanical cascade of elbow failure. The classic mechanism involves a combination of axial loading, supination of the forearm, and a valgus bending moment applied to the elbow as the body rotates over the fixed hand. According to the Horii circle of soft-tissue disruption described by O'Driscoll, the failure typically begins on the lateral side with the disruption of the lateral ulnar collateral ligament (LUCL), progressing anteriorly to involve the joint capsule, and finally reaching the medial collateral ligament (MCL) complex. In a high-energy scenario, the radial head and coronoid process act as osseous buttresses against this displacing force; when the force exceeds the ultimate tensile and compressive strengths of these structures, they fracture, resulting in the classic "Terrible Triad" pattern.
Given the height of the fall, the patient was initially evaluated according to Advanced Trauma Life Support (ATLS) protocols to rule out concomitant axial skeleton, head, or visceral injuries. Once cleared, the focus shifted entirely to the isolated, high-energy upper extremity trauma. The occupational demands of this patient cannot be overstated; manual laborers require not only a stable elbow but also a joint capable of withstanding repetitive axial and torsional loads. Consequently, the threshold for achieving near-anatomic restoration of the articular geometry and precise ligamentous tensioning is exceptionally high.
Clinical Examination Findings
Upon initial assessment in the emergency department, the patient was alert and in significant distress due to pain. The clinical examination of a suspected complex elbow dislocation requires a systematic approach, prioritizing the identification of limb-threatening neurovascular compromise while carefully assessing the integrity of the soft tissue envelope.
Inspection of the Soft Tissue Envelope
Gross deformity of the right elbow was immediately apparent. The olecranon was prominently displaced posteriorly, with the forearm appearing shortened relative to the humerus. Significant swelling was evident around the elbow joint, and early ecchymosis was noted, suggestive of substantial soft tissue disruption and capsular tearing. The soft tissue envelope was assessed using the Tscherne classification for closed fractures. The patient exhibited a Tscherne Grade 2 soft tissue injury, characterized by deep contaminated skin abrasions and localized skin or muscle contusion from direct trauma, alongside impending compartment swelling. No open wounds or skin tenting suggestive of an impending open fracture were observed, though the skin over the posterior olecranon was under significant tension, necessitating urgent reduction to prevent pressure necrosis.
Palpation and Bony Landmarks
Palpation revealed diffuse tenderness across the entire elbow joint. The bony landmarks, specifically the medial epicondyle, lateral epicondyle, and olecranon, were severely disrupted, making the classic equilateral triangular relationship (in flexion) and linear relationship (in extension) impossible to ascertain. The radial head could not be palpated in its normal anatomic position within the radiocapitellar articulation, suggesting either gross dislocation, comminuted fracture with displacement, or a combination thereof. There was no palpable crepitus, which could be attributed to significant soft tissue tension or displacement preventing bony apposition. Furthermore, the flexor-pronator mass and the extensor origin were tender to palpation, indicating potential avulsions or tears extending from the epicondylar origins.
Range of Motion and Stability Assessment
Active and passive range of motion of the elbow was severely limited and exquisitely painful. The joint was held in approximately 30-40 degrees of flexion, with any attempt at movement eliciting severe muscle guarding and pain. Forearm pronation and supination were completely restricted. In the acute, unreduced, and unanesthetized state, provocative stability testing (such as the pivot-shift test for posterolateral rotatory instability or valgus stress testing for MCL integrity) is strictly contraindicated due to the risk of exacerbating the injury, causing further articular cartilage damage, or inducing neurovascular traction injuries.
Neurological and Vascular Assessment
A thorough neurovascular examination was performed given the high potential for neurovascular compromise in posterior elbow dislocations. The brachial artery and the median and ulnar nerves are particularly vulnerable to traction or direct compression over the distal humerus during posterior displacement of the radius and ulna.
- Radial Nerve: Sensation to the dorsal first web space was intact. Wrist extension (extensor carpi radialis longus/brevis) and thumb extension (extensor pollicis longus) were strong (Medical Research Council grade 5/5).
- Median Nerve: Sensation to the volar tip of the index finger and thumb was intact. Thumb opposition and finger flexion (flexor digitorum profundus to the index finger, flexor pollicis longus) were strong (MRC grade 5/5). The anterior interosseous nerve (AIN) function was specifically confirmed to be intact.
- Ulnar Nerve: Sensation to the volar tip of the fifth finger and the ulnar aspect of the fourth finger was intact. Finger abduction and adduction (dorsal and palmar interossei) were strong (MRC grade 5/5). There was no evidence of ulnar nerve subluxation or acute cubital tunnel syndrome symptoms.
- Vascular Status: Radial and ulnar pulses were palpable and strong bilaterally. Capillary refill in the digits was brisk (less than 2 seconds). Doppler ultrasound was available but deemed unnecessary given the robust palpable pulses.
- Compartment Assessment: The forearm compartments were soft and compressible. However, given the high-energy nature of the injury and the significant antecubital swelling, serial examinations were instituted to monitor for the delayed onset of acute compartment syndrome.
Despite the intact neurovascular status, the profound deformity, severe pain, and compromised skin tension over the olecranon necessitated urgent closed reduction in the emergency department prior to advanced imaging.
Imaging and Diagnostics Protocol
Immediate radiographic evaluation was performed in the emergency department to delineate the injury pattern and guide the subsequent closed reduction maneuver.
Initial Radiographic Evaluation
Anteroposterior and lateral radiographs of the right elbow were obtained.
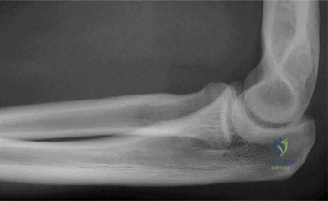
These initial views clearly demonstrated a posterior dislocation of the ulnohumeral joint. The olecranon was positioned posterior and proximal to the distal humerus.
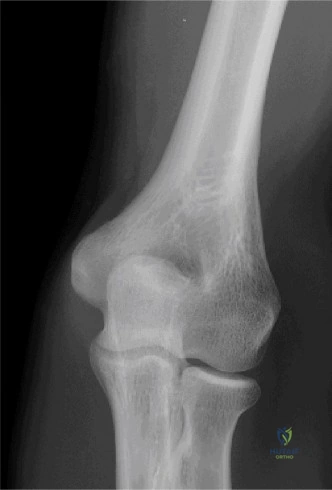
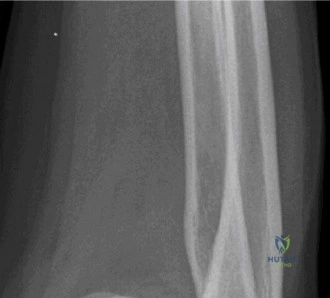
Crucially, the lateral radiograph revealed associated fractures of the radial head and the coronoid process, confirming the diagnosis of a Terrible Triad injury of the elbow. The radial head appeared significantly comminuted, with fragments displaced anteriorly and laterally. A small, seemingly transverse fracture fragment of the coronoid process was visible, though its exact size and involvement of the sublime tubercle were difficult to ascertain definitively on plain films due to bony overlap.
Following the initial imaging, a closed reduction was performed under procedural sedation using propofol and fentanyl. The reduction maneuver involved longitudinal traction with the elbow in slight flexion, accompanied by anterior translation of the olecranon and supination of the forearm to clear the coronoid under the trochlea. A palpable "clunk" was felt, and the elbow was provisionally immobilized in a posterior long-arm splint at 90 degrees of flexion and neutral forearm rotation. Post-reduction radiographs were immediately obtained.

The post-reduction radiographs confirmed concentric reduction of the ulnohumeral joint. However, the radiocapitellar line remained slightly disrupted due to the severe comminution and displacement of the radial head fracture. The "drop sign"—an increase in the ulnohumeral distance on the lateral view—was noted, indicating profound residual ligamentous instability despite the reduction.
Advanced Imaging and Computed Tomography
While plain radiographs are sufficient for the initial diagnosis and confirmation of reduction, they are notoriously inadequate for precisely defining the fracture morphology of the radial head and, more importantly, the coronoid process. Understanding the exact anatomy of the coronoid fracture is the linchpin of surgical planning in Terrible Triad injuries. Therefore, a non-contrast Computed Tomography (CT) scan of the right elbow with 3D reconstructions was ordered.
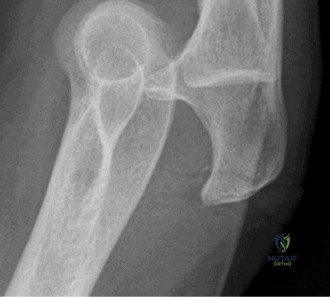
The CT scan provided critical insights that dictated the surgical approach:
1. Coronoid Process: The CT revealed an O'Driscoll Type 1, Subtype 2 fracture (involving the tip and extending slightly into the anteromedial facet). The fragment was approximately 4 millimeters in height but involved the capsular insertion. The sublime tubercle, the insertion site of the anterior bundle of the MCL, remained intact with the ulnar shaft.
2. Radial Head: The scan confirmed a highly comminuted Mason Type III fracture involving the entire radial head and extending into the radial neck. There were more than four distinct articular fragments, and the central articular depression was severe. The degree of comminution and the involvement of the radial neck strongly suggested that Open Reduction and Internal Fixation (ORIF) would be biomechanically inferior and technically unfeasible, pointing the surgical decision toward radial head arthroplasty.
3. Joint Congruency: Even in the splinted position, the CT axial cuts demonstrated subtle posterior subluxation of the ulna relative to the trochlea, reiterating the complete incompetence of the lateral collateral ligament complex and the anterior capsuloligamentous structures.
Preoperative Templating
Using the contralateral uninjured elbow as a reference (when necessary) and the 3D CT reconstructions, preoperative templating was performed to estimate the required size of the radial head prosthesis. Accurate sizing is critical; overstuffing the radiocapitellar joint can lead to capitellar erosion, early osteoarthritis, and persistent stiffness, while under-sizing can fail to restore the valgus and longitudinal stability of the forearm, exacerbating the inherent instability of the Terrible Triad.
Differential Diagnosis
When evaluating a complex elbow trauma with instability, several distinct patterns must be differentiated, as their surgical management and prognostic implications vary significantly. The "ring of stability" concept dictates that the elbow relies on primary stabilizers (ulnohumeral articulation, anterior bundle of the MCL, LUCL) and secondary stabilizers (radial head, common flexor/extensor origins, capsule). Disruption of different combinations of these structures leads to distinct clinical entities.
| Diagnostic Entity | Mechanism of Injury | Key Radiographic Findings | Clinical and Biomechanical Hallmarks |
|---|---|---|---|
| Terrible Triad Injury | High-energy FOOSH; Valgus stress, axial load, and supination. | Posterior ulnohumeral dislocation, Radial head fracture, Coronoid process fracture. | Profound multidirectional instability. Loss of both the anterior osseous buttress (coronoid) and the lateral osseous buttress (radial head), combined with LUCL disruption. |
| Posterolateral Rotatory Instability (PLRI) | FOOSH with supination and axial load; often lower energy than a Triad. | May show no fracture. Subtle posterior subluxation of the radial head. "Drop sign" on lateral radiograph. | Primary disruption of the LUCL. Positive pivot-shift test. The elbow subluxates in extension and supination, and reduces in flexion. |
| Transolecranon Fracture Dislocation | Direct blow to the posterior elbow or high-energy axial load. | Comminuted fracture of the olecranon with anterior dislocation of the radius and ulna relative to the humerus. | The radiocapitellar and ulnohumeral relationships are maintained distal to the fracture. The instability is osseous (the trochlear notch is disrupted), not primarily ligamentous. |
| Varus Posteromedial Rotatory Instability | Axial load combined with a varus stress. | Fracture of the anteromedial facet of the coronoid. Often associated with LCL avulsion. | Loss of the medial osseous buttress. The elbow subluxates posteriorly and medially. Requires specific attention to the anteromedial coronoid facet and LCL repair. |
In this case, the presence of both radial head and coronoid fractures alongside the posterior dislocation definitively ruled out isolated PLRI or a varus posteromedial rotatory instability pattern. The posterior direction of the dislocation ruled out a transolecranon fracture-dislocation, which typically presents with anterior displacement of the forearm unit.
Surgical Decision Making and Classification
The management of Terrible Triad injuries has evolved significantly over the past two decades. Historically, non-operative management or simple radial head excision led to dismal outcomes, characterized by chronic, debilitating instability, recurrent dislocations, and rapid onset of severe post-traumatic arthrosis. Today, the standard of care is aggressive, early surgical intervention aimed at restoring the osseous anatomy and repairing the ligamentous restraints to allow for early mobilization.
Fracture Classification and Implications
- Radial Head (Mason Classification): The patient presented with a Mason Type III fracture (comminuted, displaced, involving the entire head/neck). While modern osteosynthesis techniques have expanded the indications for ORIF in Mason II and some Mason III fractures, the extreme comminution and loss of structural integrity of the radial neck in this patient made ORIF highly prone to failure. The radial head is a critical secondary stabilizer to valgus stress and longitudinal forces; in the setting of an incompetent MCL (common in Triad injuries), the radial head becomes the primary valgus stabilizer. Therefore, a structurally sound radial head must be present. The decision was made to proceed with Radial Head Arthroplasty (RHA).
- Coronoid Process (Regan-Morrey and O'Driscoll Classifications): The fracture was a Regan-Morrey Type I (avulsion of the tip) but more accurately described by the O'Driscoll classification as a Type 1, Subtype 2 (involving the tip and capsular insertion). The coronoid acts as the primary anterior osseous buttress preventing posterior subluxation of the ulna. Even small fragments, if they involve the anterior capsular insertion, represent a significant loss of soft-tissue tensioning. The surgical plan mandated either rigid internal fixation of the fragment or robust reattachment of the anterior capsule to the remaining coronoid base to restore this anterior restraint.
Rationale for the Standard Surgical Protocol
The surgical strategy followed the systematic, stepwise protocol popularized by Pugh and colleagues, which addresses the pathology from deep to superficial and prioritizes the restoration of the stabilizing structures:
1. Restoration of the anterior osseous buttress (Coronoid fixation or capsular repair).
2. Restoration of the lateral osseous buttress (Radial head ORIF or Arthroplasty).
3. Restoration of the lateral tension band (LUCL repair).
4. Intraoperative assessment of stability.
5. Address the medial tension band (MCL repair) or apply a hinged external fixator only if the elbow remains unstable after steps 1-3.
Non-operative management was entirely precluded in this patient due to the persistent subluxation (drop sign) on post-reduction imaging and the high functional demands of his occupation.
Surgical Technique and Intervention
The patient was taken to the operating room on hospital day two, following optimization of the soft tissue envelope with elevation and strict ice therapy.
Patient Positioning and Anesthesia
Under general anesthesia supplemented with an ultrasound-guided supraclavicular regional nerve block for postoperative analgesia, the patient was positioned supine on the operating table. The right arm was draped free across the chest, supported by a sterile bolster. This position allows for excellent access to both the lateral and medial aspects of the elbow, facilitates intraoperative fluoroscopy, and permits the surgeon to utilize gravity to assist with reduction during the procedure. A non-sterile tourniquet was applied high on the brachium and inflated to 250 mmHg after exsanguination.
Surgical Approach
A universal posterior midline incision was utilized, curving slightly lateral to the tip of the olecranon to avoid placing the scar directly over the weight-bearing prominence. Full-thickness fasciocutaneous flaps were elevated medially and laterally. This extensile approach was chosen because it allows access to both the lateral and medial compartments through a single skin incision, should a medial approach be required for MCL repair or complex coronoid fixation.
The deep dissection began on the lateral side. The Kocher interval, between the extensor carpi ulnaris (ECU) and the anconeus, was identified and developed. This approach provides direct access to the radiocapitellar joint and the LUCL footprint. Upon entering the joint, a massive hematoma was evacuated. The LUCL was found to be completely avulsed from its isometric origin on the lateral epicondyle, confirming the preoperative suspicion.
Step 1: Management of the Coronoid Process
With the lateral capsule open and the comminuted radial head fragments removed, excellent visualization of the anterior compartment and the coronoid process was achieved through the empty radiocapitellar space. The coronoid fragment was identified; it was a small, transverse piece attached to the anterior capsule. Given its small size, screw fixation was deemed inappropriate due to the risk of fragmentation.
Instead, a "suture lasso" technique was employed. Two #2 high-strength non-absorbable sutures were passed through the anterior capsule just proximal to the bony fragment using a Mason-Allen configuration. Two parallel drill holes were then created from the posterior aspect of the proximal ulna, exiting precisely at the base of the coronoid fracture bed. The suture limbs were shuttled through these osseous tunnels using a suture passing wire. These sutures were left untied temporarily; they would be tied over the posterior ulnar cortex later in the procedure, simultaneously reducing the bony fragment and tensioning the anterior capsule to restore the anterior buttress.
Step 2: Radial Head Arthroplasty
Attention was turned to the radial head. The native radial head fragments were pieced together on the back table to estimate the native diameter and height. The radial neck was prepared using a broach. A modular, smooth-stemmed, metallic radial head prosthesis was selected. The rationale for a smooth, loose-fitting stem is to allow the implant to act as a spacer, tracking anatomically with the capitellum during forearm rotation, thereby reducing edge-loading and capitellar wear.
The trial prosthesis was inserted. Fluoroscopy and direct visualization were used to ensure the articular surface of the implant was perfectly flush with the lateral edge of the coronoid process, restoring the native radiocapitellar line. Care was taken to avoid "overstuffing" the joint, which is assessed by ensuring a symmetric ulnohumeral joint space on the AP fluoroscopic view and confirming smooth tracking without subluxation during flexion and extension. Once the correct size was confirmed, the definitive implant was assembled and impacted into place.

Step 3: Lateral Ulnar Collateral Ligament (LUCL) Repair
The critical step of restoring the lateral tension band was performed next. The isometric point of the LUCL origin on the lateral epicondyle was identified—typically located at the center of capitellar curvature. The cortical bone at this footprint was decorticated with a high-speed burr to promote healing.
Two double-loaded metallic suture anchors were placed precisely at the isometric point. The sutures were passed through the avulsed LUCL and the overlying extensor origin using a Krackow locking stitch technique.
Before tying the LUCL sutures, the previously placed coronoid/anterior capsule sutures were tied over the posterior ulnar cortex with the elbow held in 90 degrees of flexion. This secured the anterior buttress. Subsequently, the LUCL sutures were tied securely with the forearm in full pronation and the elbow at 90 degrees of flexion. Pronation closes the lateral joint space and removes tension from the lateral repair.
Step 4: Intraoperative Stability Assessment
Following the reconstruction of the coronoid, radial head, and LUCL, a rigorous intraoperative stability assessment was conducted. The "Hang Test" was performed: the elbow was extended with the forearm in neutral rotation, allowing gravity to apply a posterior subluxating force. Fluoroscopy confirmed that the ulnohumeral joint remained concentrically reduced from 0 to 130 degrees of flexion. There was no opening of the medial joint space under valgus stress, indicating that the radial head prosthesis and the intact dynamic stabilizers were sufficient to compensate for the likely injured MCL.
Because concentric stability was achieved through a full functional arc of motion, medial exploration for MCL repair and the application of a hinged external fixator were deemed unnecessary.
The wound was irrigated copiously. The extensor origin and the Kocher interval were meticulously closed over a suction drain. The subcutaneous tissues and skin were closed in a layered fashion. A sterile dressing was applied, and the arm was placed in a hinged elbow brace locked at 90 degrees of flexion with the forearm in neutral rotation.
The final postoperative lateral radiograph demonstrated a concentrically reduced ulnohumeral joint, optimal positioning of the radial head prosthesis, and restoration of the radiocapitellar alignment without evidence of overstuffing.
Post Operative Protocol and Rehabilitation
The primary goal of the postoperative rehabilitation protocol in Terrible Triad injuries is to navigate the precarious balance between protecting the surgical repair and preventing debilitating elbow stiffness. The elbow joint capsule is highly prone to contracture, and prolonged immobilization universally results in a poor functional outcome.
Phase 1: Acute Protection and Early Motion (Weeks 0-2)
The patient was admitted for 24 hours of intravenous antibiotics and pain control. The suction drain was removed on postoperative day one. The patient was instructed to keep the arm elevated above heart level to mitigate edema.
Crucially, early active-assisted range of motion was initiated on postoperative day two. The hinged elbow brace was unlocked to allow motion from 30 degrees of extension to 130 degrees of flexion. Full extension was initially blocked to protect the anterior capsule repair and the LUCL from extreme tension. Forearm pronation and supination were permitted only with the elbow flexed to 90 degrees. The patient was explicitly instructed to avoid any active shoulder abduction combined with internal rotation (e.g., reaching behind the back or pushing up from a chair), as this generates a significant varus torque that places the LUCL repair at high risk of failure.
Heterotopic Ossification (HO) prophylaxis was initiated consisting of Indomethacin 75mg sustained-release daily for three weeks, given the high-energy nature of the trauma, the central nervous system intactness, and the extensive surgical dissection.
Phase 2: Progression of Motion (Weeks 2-6)
At the two-week follow-up, the surgical incision demonstrated excellent healing, and sutures were removed. Radiographs confirmed maintenance of the concentric reduction.
The extension block on the hinged brace was gradually reduced by 10 degrees per week. The patient continued with physical therapy, focusing on active and active-assisted motion. Passive stretching by the therapist was strictly prohibited, as forceful passive manipulation causes microtrauma to the joint capsule, inciting an inflammatory response that paradoxically increases stiffness and drastically elevates the risk of heterotopic ossification.
Phase 3: Strengthening and Weaning (Weeks 6-12)
By week six, the hinged brace was discontinued for daily activities but worn at night or in crowded environments for protection. Radiographs at this stage showed no evidence of implant loosening or joint subluxation.
Isometric strengthening of the biceps, triceps, and forearm musculature was initiated. Isotonic strengthening was introduced gradually at week eight. The focus remained on achieving a functional arc of motion (defined by Morrey as 30 to 130 degrees of flexion, and 50 degrees of both pronation and supination).
Phase 4: Return to Function (Months 3+)
At three months postoperative, the patient had achieved a range of motion from 15 degrees of extension to 135 degrees of flexion, with full, symmetric pronation and supination. Grip strength was 80% of the contralateral dominant side. He was cleared to begin work conditioning and simulated occupational tasks. By month five, he successfully returned
