Complex Revision THA Case Title: Impaction Grafting Success

Key Takeaway
Learn more about Complex Revision THA Case Title: Impaction Grafting Success and how to manage it. "Case title revision" often describes complex procedures like Revision THA addressing aseptic loosening. This includes impaction bone grafting for severe Paprosky type 2B socket and 3A femoral bone loss, or re-revision for acetabular Paprosky 2A defects. These interventions, utilizing techniques like mesh and constrained liners, aim to restore stability and function, managing significant bone loss and component loosening.
Patient Presentation and History
Welcome to this Grand Rounds presentation. Today, we will critically examine a complex revision total hip arthroplasty (THA) case characterized by massive pelvic and femoral osteolysis, managed successfully with impaction bone grafting (IBG). The objective of this presentation is to delineate the clinical decision-making process, the biomechanical rationale for biological reconstruction of bone stock, and the rigorous surgical technique required to achieve durable survivorship in the setting of catastrophic bone loss.
The patient is a 68-year-old male who presented to our tertiary orthopedic oncology and reconstruction clinic with a 12-month history of progressive, debilitating right hip pain, an increasingly pronounced Trendelenburg limp, and a precipitous decline in his functional baseline. The pain was described as mechanical, insidious in onset, and localized primarily to the groin and lateral peritrochanteric region, with occasional radiation to the anterior thigh. The pain was particularly exacerbated by weight-bearing, the initiation of movement from a seated position, and prolonged ambulation. Conservative modalities, including non-steroidal anti-inflammatory drugs (NSAIDs), targeted physical therapy focusing on abductor strengthening, and assistive device utilization (cane in the contralateral hand), failed to provide clinically meaningful relief.
His surgical history is significant for a primary right total hip arthroplasty performed 15 years prior for end-stage degenerative osteoarthritis. Operative records from the index procedure indicated the utilization of an uncemented, proximally porous-coated titanium femoral stem and a hemispherical uncemented acetabular shell with a ceramic-on-polyethylene bearing surface. The specific polyethylene utilized predated the widespread adoption of highly cross-linked ultra-high-molecular-weight polyethylene (UHMWPE), predisposing the construct to accelerated volumetric wear and subsequent particulate debris generation.
Following the index arthroplasty, the patient experienced an uneventful postoperative recovery and maintained an excellent functional status (Harris Hip Score > 90) for approximately a decade. The current clinical deterioration began gradually, transitioning from intermittent discomfort to constant, activity-limiting pain. He reported increasing difficulty with activities of daily living (ADLs), noting specific limitations in stair negotiation, lower extremity dressing, and ambulation beyond household distances.
His past medical history is notable for essential hypertension, which is well-controlled on a calcium channel blocker, and Type 2 Diabetes Mellitus, managed with oral hypoglycemic agents (Metformin and an SGLT2 inhibitor). His most recent Hemoglobin A1c was 6.8%, indicating adequate glycemic control, a critical factor for mitigating postoperative infection risk and optimizing allograft incorporation. He has a remote history of tobacco use, having achieved smoking cessation a decade prior to presentation. His Body Mass Index (BMI) is 31 kg/m², placing him in the Class I obesity category, which alters the biomechanical load across the hip joint and accelerates wear mechanics.
Crucially, the patient denied any history of recent acute trauma, antecedent systemic infections, fevers, chills, night sweats, or unexplained weight loss. There were no symptoms suggestive of neurovascular compromise, such as radicular pain, paresthesias, or distal motor weakness.
Pathophysiology of Particle Disease
Before progressing to the clinical examination, it is imperative to contextualize the patient's presentation within the framework of aseptic loosening secondary to particle disease. The relatively early generation of the polyethylene liner utilized in the index procedure is highly susceptible to adhesive and abrasive wear. The generation of submicron polyethylene wear debris initiates a robust macrophage-mediated foreign body response.
Phagocytosis of these particles by local macrophages leads to the secretion of pro-inflammatory cytokines, predominantly Interleukin-1 (IL-1), Interleukin-6 (IL-6), and Tumor Necrosis Factor-alpha (TNF-alpha). These cytokines upregulate the expression of Receptor Activator of Nuclear Factor Kappa-B Ligand (RANKL) by osteoblasts and stromal cells. RANKL subsequently binds to the RANK receptor on osteoclast precursors, driving their differentiation, activation, and survival. The resultant uncoupling of the normal bone remodeling process leads to aggressive periprosthetic osteolysis, compromising the structural integrity of the host bone and ultimately resulting in catastrophic component loosening, as observed in this clinical scenario.
Clinical Examination Findings
A comprehensive musculoskeletal and neurovascular examination of the right lower extremity was performed. On initial static inspection, the patient exhibited a mild fixed external rotation deformity of the right lower extremity. Dynamic evaluation revealed a pronounced, uncompensated Trendelenburg gait, indicative of significant abductor mechanism dysfunction. This dysfunction is frequently multifactorial in the setting of severe osteolysis, resulting from superior migration of the greater trochanter (decreasing the abductor moment arm), direct abductor muscle damage from the index posterior approach, or pain-induced reflex inhibition.
Evaluation of limb length revealed no gross clinical discrepancy; however, apparent leg length measurements can be misleading in the presence of fixed pelvic obliquity or significant component subsidence. True leg length measurement (anterior superior iliac spine to medial malleolus) suggested a 1.5 cm shortening of the right lower extremity, consistent with the radiographic findings of femoral subsidence and superior acetabular migration.
Inspection of the integument revealed a well-healed, non-erythematous, and non-adherent posterolateral surgical scar from the index arthroplasty. There was no evidence of local swelling, calor, erythema, or fluctuance to suggest an acute infectious process or the presence of a superficial sinus tract.
Palpation elicited diffuse tenderness over the greater trochanter and the anterior joint capsule. However, there was an absence of focal point tenderness over the trochanteric bursa, making isolated greater trochanteric pain syndrome (GTPS) an unlikely primary etiology for his profound functional deficit.
Range of Motion and Provocative Testing
Active and passive range of motion (ROM) of the right hip were globally restricted and elicited significant mechanical pain, particularly at the extremes of motion.
- Flexion: 0-70 degrees (limited by anterior impingement and pain)
- Extension: 0 degrees (loss of terminal extension)
- Abduction: 0-10 degrees (severely restricted, indicating capsular contracture and abductor insufficiency)
- Adduction: 0-5 degrees
- Internal Rotation: 0-5 degrees
- External Rotation: 0-15 degrees
Passive ROM closely mirrored active ROM, confirming a true mechanical restriction rather than isolated muscle weakness. Provocative testing, including the Stinchfield test (resisted active straight leg raise), elicited severe groin pain, highly specific for intra-articular pathology and component loosening. While no frank mechanical apprehension or palpable subluxation was noted during ROM, the assessment of gross instability was limited by the patient's pain tolerance.
Neurovascular Assessment
A meticulous neurological examination of the right lower extremity demonstrated intact motor strength (Grade 5/5 on the Medical Research Council scale) in all major myotomes (L2-S1), including the iliopsoas, quadriceps, tibialis anterior, extensor hallucis longus, and gastrocnemius-soleus complex. Sensation was intact to light touch and pinprick across all corresponding dermatomes. Deep tendon reflexes (patellar and Achilles) were symmetric and graded 2+ bilaterally.
Vascular examination revealed palpable and symmetric femoral, popliteal, dorsalis pedis, and posterior tibial pulses. Capillary refill was brisk (< 2 seconds) in the distal digits. There was no clinical evidence of deep vein thrombosis (DVT) or chronic venous insufficiency.
Given the extensive osteolysis and the necessity of excluding periprosthetic joint infection (PJI) prior to any revision intervention, a comprehensive serological workup was initiated. The Erythrocyte Sedimentation Rate (ESR) and C-Reactive Protein (CRP) were within normal institutional limits (ESR: 12 mm/hr; CRP: 0.4 mg/dL). Despite the reassuring serology, the magnitude of the planned reconstruction mandated a preoperative fluoroscopically guided hip aspiration. The synovial fluid analysis revealed a nucleated cell count of 850 cells/µL with 45% polymorphonuclear leukocytes (PMNs), and cultures remained sterile at 14 days, effectively ruling out an indolent PJI and confirming the diagnosis of aseptic loosening.
Imaging and Diagnostics
The cornerstone of preoperative planning in complex revision arthroplasty is a rigorous, multi-modal imaging assessment to quantify bone loss, evaluate component stability, and identify potential occult pelvic discontinuities or periprosthetic fractures.
Radiographic Assessment
Initial radiographic evaluation consisted of standardized, weight-bearing anteroposterior (AP) and lateral views of the right hip, alongside a full-length AP pelvis radiograph to assess bilateral symmetry, pelvic obliquity, and offset.
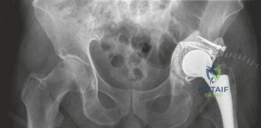
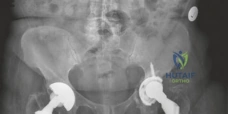
The AP Pelvis radiograph demonstrated catastrophic failure of the index arthroplasty. There was evidence of severe, expansile acetabular osteolysis, predominantly localizing to DeLee and Charnley zones 1 (superior) and 2 (medial). The uncemented acetabular shell exhibited significant superior and medial migration, with apparent protrusion of the medial wall into the true pelvis. A continuous, wide radiolucent line (>2 mm) was visible at the bone-prosthesis interface, confirming gross aseptic loosening. The teardrop was obliterated, and the Kohler's line (ilioischial line) appeared compromised, raising the clinical suspicion for an uncontained medial defect or impending pelvic discontinuity.
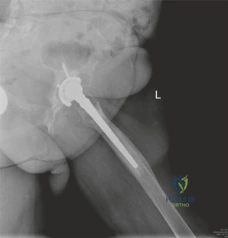
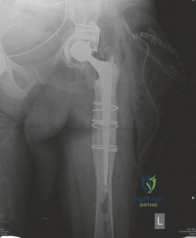
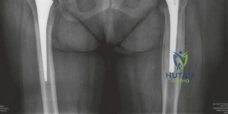
The lateral radiograph corroborated the AP findings, further delineating the extent of anterior and posterior column involvement. The femoral component also exhibited unequivocal signs of failure. Extensive radiolucency was evident at the bone-prosthesis interface spanning Gruen zones 1, 7, and 2, consistent with proximal osteolysis. Distally, in zones 3, 4, and 5, there was prominent cortical hypertrophy and pedestal formation at the tip of the stem. This radiographic pattern is pathognomonic for proximal stress shielding combined with distal point loading, indicating a loss of proximal fixation and subsequent micro-motion leading to distal toggle. Minor axial subsidence of the femoral stem (approximately 8 mm) was also noted when compared to immediate postoperative radiographs from 15 years prior.
Advanced Cross-Sectional Imaging
Given the severity of the cavitary and segmental bone loss observed on plain radiography, advanced cross-sectional imaging was mandated to facilitate three-dimensional spatial understanding and precise surgical templating. A high-resolution, multi-detector Computed Tomography (CT) scan of the pelvis and right femur was obtained using metal artifact reduction sequence (MARS) protocols.

The coronal CT reconstruction provided a stark visualization of the volumetric acetabular bone loss. The superior migration of the cup had created a massive cavitary defect in the ilium. The remaining superior dome was paper-thin, lacking the structural integrity necessary to support a standard hemispherical revision component without significant augmentation. The medial wall was critically thinned, with focal areas of complete dehiscence, confirming a contained medial defect that had progressed to an uncontained state in isolated regions.

The axial CT slices were crucial for evaluating the integrity of the anterior and posterior columns. While severe osteolysis had attenuated both columns, continuous bone was identified bridging the superior ilium to the inferior ischium and pubis. This finding was paramount, as it confirmed the absence of a complete pelvic discontinuity, thereby dictating a different reconstructive algorithm than would be required for a dissociated pelvis. The axial views also highlighted the extensive granulomatous tissue burden occupying the osteolytic cysts, which would require meticulous intraoperative debridement.
To further assist in preoperative templating and spatial orientation, a 3D reconstruction of the pelvis was generated. This modality allows the surgical team to virtually rotate the hemipelvis, assessing the size and morphology of the segmental defects. The 3D model clearly delineated a massive superior-medial cavitary defect with a compromised superolateral rim.
Based on the comprehensive imaging suite, the acetabular defect was classified as a Paprosky Type IIIB. This classification signifies severe superior migration (>3 cm), massive volumetric bone loss, an incompetent superior dome, and a teardrop that is frequently destroyed or significantly altered, yet with the maintenance of pelvic continuity. The femoral defect was classified as a Paprosky Type III, characterized by extensive metadiaphyseal bone loss with intact diaphyseal bone distal to the isthmus, capable of providing initial mechanical stability for a revision stem.
Differential Diagnosis
The presentation of a painful, failing total hip arthroplasty requires a systematic approach to rule out potentially limb-threatening or life-threatening etiologies before attributing the failure solely to mechanical wear. The differential diagnosis must be broad, encompassing infectious, mechanical, and biological failure modes.
| Differential Diagnosis | Clinical Presentation | Radiographic/Imaging Findings | Laboratory/Aspiration Findings |
|---|---|---|---|
| Aseptic Loosening (Particle Disease) | Insidious onset, mechanical pain (worse with weight-bearing), progressive functional decline. History of older generation polyethylene. | Expansile, scalloped osteolytic lesions. Radiolucent lines >2mm at the bone-prosthesis interface. Component migration or subsidence. No periosteal reaction. | Normal ESR/CRP. Synovial fluid WBC < 3000 cells/µL, PMN < 80%. Negative cultures. Macrophages containing wear debris on histology. |
| Periprosthetic Joint Infection (PJI) | Can be acute (fever, erythema, severe rest pain) or chronic (insidious pain, similar to aseptic loosening). History of delayed wound healing or systemic bacteremia. | May show rapid, aggressive bone resorption, periosteal reaction, or early component loosening. Often indistinguishable from aseptic loosening in chronic cases. | Elevated ESR/CRP. Synovial fluid WBC > 3000 cells/µL, PMN > 80%. Positive cultures (aerobic, anaerobic, fungal, AFB). Positive Alpha-defensin. |
| Adverse Local Tissue Reaction (ALTR) / Metallosis | Groin pain, palpable mass (pseudotumor), abductor weakness, unexplained instability. Associated with MoM bearings, trunnionosis, or modular neck failures. | Often normal initial radiographs. MRI (MARS) shows thick-walled cystic masses, fluid collections, and soft tissue destruction. | Normal ESR/CRP (usually). Elevated serum Cobalt and Chromium ion levels. Aspiration yields dark, metallic fluid. |
| Occult Periprosthetic Fracture | Sudden onset of severe pain, often following a minor traumatic event or rotational stress. Inability to bear weight. | Disruption of cortical continuity. May require CT scan to identify non-displaced spiral fractures or fractures obscured by the implant. | Normal inflammatory markers. |
In this clinical scenario, the chronicity of the symptoms, the classic radiographic appearance of expansile osteolysis with component migration, the normal inflammatory markers, and the negative preoperative aspiration definitively pointed toward Aseptic Loosening secondary to Particle Disease as the primary diagnosis.
Surgical Decision Making and Classification
The management of massive bone loss in revision THA presents a formidable reconstructive challenge. The primary goals of the intervention are the eradication of particulate debris, the restoration of anatomic hip mechanics (center of rotation, offset, and leg length), the achievement of rigid initial component stability, and the long-term reconstitution of host bone stock.
The acetabular defect, classified as Paprosky Type IIIB, implies that a standard hemispherical component will not achieve adequate stability (less than 50% host bone contact). The reconstructive options for such severe defects include:
- Jumbo Uncemented Cups: Often insufficient in Type IIIB defects due to the lack of a supportive superior rim and the risk of medializing the center of rotation excessively.
- Highly Porous Metal Augments (Trabecular Metal) with Revision Shells: Excellent for addressing specific segmental defects, but rely on remaining host bone for ingrowth and do not biologically restore the cavitary void.
- Custom Triflange Acetabular Components (CTAC) or Cup-Cage Constructs: Typically reserved for pelvic discontinuity or extreme cases where biological reconstruction is deemed impossible. These are expensive, require significant lead time, and offer no potential for host bone restoration.
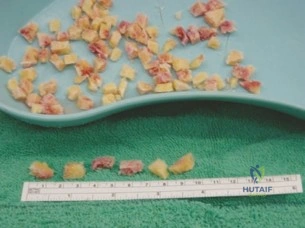
- Impaction Bone Grafting (IBG) with a Cemented Cup: The technique pioneered by Slooff and the Nijmegen group. This utilizes tightly impacted morselized cancellous allograft to fill cavitary defects and reconstruct segmental deficits (often in conjunction with metallic mesh), followed by the cementation of a polyethylene cup.
For the femoral side (Paprosky Type III), options include:
- Fully Porous-Coated Cylindrical Stems: Rely on diaphyseal scratch fit. Can be technically challenging to achieve correct version and leg length simultaneously.
- Modular Fluted Tapered Stems: The current workhorse for femoral revision. Provide excellent diaphyseal fixation and allow independent adjustment of version and offset. However, they do not address the proximal bone loss and can be associated with stress shielding or subsidence.
- Femoral Impaction Bone Grafting with a Taper-Slip Stem: The Exeter technique. Involves creating a neo-medullary canal with impacted allograft and cementing a highly polished, double-tapered stem.
Rationale for Impaction Bone Grafting
Given the patient's relatively young age (68 years) and the massive volumetric loss on both the acetabular and femoral sides, a purely mechanical reconstruction (e.g., augments and modular stems) would leave the patient with a severely depleted bone reservoir, complicating any potential future revisions.
We elected to proceed with Acetabular and Femoral Impaction Bone Grafting. The biological rationale for IBG is profound. The tightly packed morselized cancellous allograft provides immediate mechanical stability through the interlocking of the bone chips. Over time, this graft undergoes creeping substitution—a process of simultaneous osteoclastic resorption and osteoblastic bone formation—ultimately incorporating and remodeling into living host bone according to Wolff's Law.
On the femoral side, the biomechanics of the Exeter taper-slip stem are uniquely suited for IBG. The highly polished surface prevents bonding between the cement and the stem. Under axial load, the double-tapered geometry allows the stem to subside microscopically within the cement mantle. This subsidence generates radial compressive forces (hoop stresses) that are transmitted through the cement to the impacted graft, mechanically stimulating the graft and promoting consolidation and incorporation, rather than stress shielding.
Surgical Technique and Intervention
The patient was optimized medically and cleared for surgery. He was positioned in the lateral decubitus position on a radiolucent operating table, utilizing rigid pelvic positioners to ensure stability during the vigorous impaction process. Intravenous tranexamic acid (TXA) and prophylactic antibiotics (Cefazolin) were administered prior to incision.
Approach and Component Extraction
A standard posterolateral approach to the hip was utilized, incorporating the previous surgical incision. Meticulous dissection was performed to elevate the gluteus maximus fascia and identify the sciatic nerve, which was protected throughout the procedure. The short external rotators and posterior capsule were incised and tagged for later repair.
The hip was dislocated posteriorly with gentle internal rotation and flexion, taking extreme care to avoid inducing an intraoperative periprosthetic fracture in the severely osteoporotic proximal femur.

Component extraction is a critical phase where further bone loss must be minimized. The femoral head was removed. The femoral stem, exhibiting gross clinical loosening as predicted by the radiographs, was extracted utilizing a slap hammer threaded onto the trunnion. The extraction was straightforward, requiring minimal force, confirming the loss of proximal and distal biological fixation.
Attention was then turned to the acetabulum. The uncemented shell was visibly loose and surrounded by a thick layer of reactive granulomatous tissue. It was carefully levered out of the acetabular vault using curved gouges and explantation forceps, preserving the remaining fragile sclerotic rim.
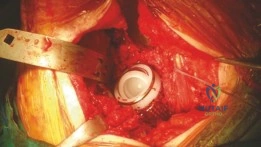
Acetabular Preparation and Reconstruction
Following component removal, the true magnitude of the defect was apparent. The acetabulum was filled with a massive volume of fibrous, metallotic granuloma.
Radical debridement was performed using a combination of curettes, rongeurs, and a high-speed burr. It is absolutely critical to remove all soft tissue and expose bleeding, punctate host bone to provide the vascular supply necessary for graft incorporation. The neocapsule was excised to mobilize the femur and provide unhindered access to the acetabular vault.
The defect was assessed. The medial wall was profoundly thinned, with a small uncontained central
Clinical & Radiographic Imaging