Introduction and Epidemiology
Periprosthetic femoral fractures following total hip arthroplasty represent a complex and increasingly prevalent challenge in orthopedic traumatology. As the population ages and the volume of primary and revision arthroplasty procedures grows, the incidence of these fractures has seen a parallel, exponential rise. These injuries are associated with significant morbidity, substantial healthcare costs, and a mortality rate that approaches that of native proximal femur fractures in the elderly population.
The clinical vignette provided illustrates a classic presentation. A 78-year-old female with a history of bilateral total hip arthroplasty and osteoporosis presents following a low-energy torsional injury. The resulting comminuted, spiral fracture of the right femoral shaft, extending from the distal aspect of a cemented stem, highlights the typical fracture morphology seen in osteoporotic bone subjected to the stress risers created by an intramedullary implant.
The Vancouver Classification system remains the gold standard for categorizing these fractures, guiding both prognosis and surgical strategy. It is predicated on three critical factors: the location of the fracture relative to the prosthesis, the stability of the implant, and the quality of the surrounding bone stock.
- Vancouver Type A fractures involve the trochanteric region (AG for greater trochanter, AL for lesser trochanter).
- Vancouver Type B fractures occur around the stem or just distal to it. This is further subdivided based on implant stability and bone stock. Type B1 indicates a stable, well-fixed stem. Type B2 indicates a loose stem with adequate bone stock. Type B3 indicates a loose stem with poor bone stock.
- Vancouver Type C fractures occur well distal to the tip of the prosthesis, typically managed similarly to native femoral shaft fractures, albeit with consideration for the proximal hardware.
Based on the initial radiographic assessment in the presented case—a fracture spiraling around the distal tip of the stem with an apparently intact cement mantle and no gross subsidence—this injury is provisionally classified as a Vancouver Type B1. However, definitive classification often requires advanced imaging and intraoperative assessment, as plain radiographs have a known sensitivity deficit for detecting micro-motion and subtle loosening at the prosthesis-bone interface.
Surgical Anatomy and Biomechanics
A profound understanding of femoral anatomy and the altered biomechanics introduced by a total hip arthroplasty is essential for successful surgical planning and execution.
Vascular Anatomy and Fracture Healing
The femur relies heavily on its periosteal and endosteal blood supply. The endosteal supply is inevitably compromised, if not entirely obliterated, by the insertion of an intramedullary stem and the surrounding cement mantle. Consequently, the healing of a periprosthetic fracture is almost exclusively dependent on the periosteal blood supply. The primary vascular contributors are the perforating branches of the profunda femoris artery, which pierce the linea aspera posteriorly. Surgical approaches must strictly respect these posterior structures. Excessive periosteal stripping during exposure or plate application directly devascularizes the fracture fragments, drastically increasing the risk of atrophic nonunion.
Biomechanical Alterations and Stress Risers
The introduction of a rigid metallic stem into the viscoelastic femoral canal fundamentally alters load transmission. Normal physiological loading involves stress transfer through the proximal trabecular bone. An intramedullary stem bypasses this proximal region, transferring loads distally. This phenomenon, known as stress shielding, leads to proximal osteopenia over time, further weakening the bone.
Furthermore, the transition zone between the rigid prosthetic stem and the more elastic native diaphyseal bone acts as a massive stress riser. This mismatch in the modulus of elasticity concentrates torsional and bending forces exactly at the tip of the prosthesis. In the presented case, the torsional force from the patient twisting her body concentrated at the distal cement mantle, initiating the spiral fracture.
Principles of Fixation Construct Biomechanics
When designing a fixation construct for a Vancouver B1 fracture, the surgeon must adhere to the principles of relative stability. Absolute stability (anatomic reduction and absolute rigid fixation) is rarely achievable or desirable in comminuted osteoporotic periprosthetic fractures. Instead, the goal is secondary bone healing via callus formation.
The fixation construct must span the entire zone of injury and overlap the existing prosthesis by a minimum of two femoral cortical diameters to prevent creating a new stress riser at the end of the plate. The construct acts as a load-sharing device. The use of broad, heavy-duty locking compression plates is standard. In the proximal segment, where the intramedullary canal is occupied by the stem and cement, fixation relies on cerclage cables, wires, or specific unicortical locking screws designed to purchase the lateral cortex without impinging on the prosthesis.
Indications and Contraindications
The management of periprosthetic hip fractures is predominantly surgical. Non-operative management is fraught with complications, including prolonged immobility, decubitus ulcers, deep vein thrombosis, pneumonia, and a high rate of mortality. Therefore, non-operative management is strictly reserved for a very narrow subset of patients.
Operative and Non Operative Parameters
| Parameter | Operative Management | Non-Operative Management |
|---|---|---|
| Fracture Type | Vancouver B1, B2, B3, C; Displaced Vancouver A | Truly undisplaced Vancouver A (AG or AL) |
| Implant Status | Loose stem (requires revision); Stable stem (requires fixation) | Stable stem with undisplaced trochanteric fracture |
| Patient Status | Medically optimized, ambulatory prior to injury | Moribund, non-ambulatory baseline, unacceptable anesthetic risk |
| Bone Quality | Adequate to poor (dictates fixation vs revision type) | Severe osteopenia precluding any hardware purchase (rarely an absolute contraindication, often requires strut grafts) |
| Goals of Care | Early mobilization, restoration of length/alignment | Palliative care, pain control only |
The patient in the vignette is an independent ambulator with medically optimized comorbidities (controlled T2DM, HTN, CAD post-PCI). Despite her age and osteoporosis, surgical intervention is definitively indicated to restore her mobility and minimize the catastrophic risks of prolonged bed rest.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is the cornerstone of successful periprosthetic fracture management. The initial assessment must be augmented with advanced imaging to finalize the surgical strategy.
Advanced Imaging and Templating
Completing the diagnostic workup initiated in the clinical vignette: A CT scan of the right lower extremity with metal artifact reduction sequence (MARS) was obtained to definitively evaluate the cement mantle, assess for subtle stem subsidence, and map the complex fracture morphology.
CT imaging is critical because up to 20% of fractures classified as Vancouver B1 on plain radiographs are found to have loose stems intraoperatively, necessitating a shift from simple internal fixation to a complex revision arthroplasty (Vancouver B2 management). The CT scan allows for precise measurement of cortical thickness, evaluation of osteolysis, and planning for screw trajectories around the cemented stem.

Figure 1: Representative radiograph demonstrating a periprosthetic femoral fracture with significant comminution around a previously implanted femoral stem.
Digital templating must be performed on calibrated orthogonal radiographs. The surgeon must template the length of the required locking plate, ensuring it extends adequately distal to the fracture and proximal to the stem tip. Furthermore, the operating room must be equipped with a comprehensive armamentarium. Even if preoperative imaging suggests a stable stem (B1), the surgeon must have revision arthroplasty equipment available in the room. This includes long-stem revision implants, cement removal tools, extended trochanteric osteotomy (ETO) instrumentation, cortical allograft struts, and a variety of cerclage cable systems.
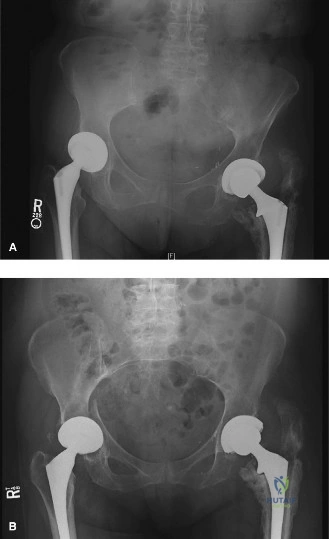
Figure 2: Advanced imaging and templating are essential for determining the precise relationship between the fracture lines, the cement mantle, and the native cortical bone.
Patient Positioning and Operating Room Setup
The choice of patient positioning depends heavily on the anticipated procedure.
For a presumed Vancouver B1 or C fracture where isolated open reduction and internal fixation (ORIF) is planned, the patient is typically placed supine on a radiolucent Jackson table or a flat trauma table. A bump is placed under the ipsilateral hip to achieve neutral rotation. This position facilitates easier assessment of limb length and alignment, and allows for unimpeded fluoroscopic imaging in both AP and lateral planes along the entire length of the femur.
If there is a high index of suspicion for a loose stem (Vancouver B2 or B3) requiring revision arthroplasty, the patient should be placed in the lateral decubitus position using rigid pelvic positioners. While this position makes assessing overall limb alignment more challenging during plating, it provides the necessary access to the hip joint for stem extraction, canal reaming, and insertion of a revision prosthesis.
Given the vignette's presentation of a B1 fracture, the supine position on a radiolucent table is optimal, provided the surgeon is prepared to adapt if intraoperative testing reveals implant instability.
Detailed Surgical Approach and Technique
The surgical execution for a Vancouver B1 periprosthetic fracture requires meticulous soft tissue handling, biological fixation principles, and robust biomechanical constructs.
Surgical Exposure and the Extensile Lateral Approach
An extensile direct lateral approach to the femur is utilized. The incision incorporates the previous lateral THA scar, extending distally along the axis of the femur as dictated by the templated plate length.
The subcutaneous tissues are divided in line with the incision. The fascia lata is incised longitudinally. The vastus lateralis is identified. Rather than splitting the muscle belly—which can denervate the anterior portion and cause significant bleeding—a subvastus or vastus-splitting approach at the posterior border is preferred. The vastus lateralis is elevated anteriorly off the lateral intermuscular septum. Perforating vessels from the profunda femoris will be encountered piercing the septum; these must be carefully identified, ligated, or cauterized to prevent postoperative hematoma, while strictly avoiding dissection posterior to the septum to preserve the primary periosteal blood supply.
Intraoperative Assessment of Implant Stability
Once the fracture site is exposed, the most critical step of the operation occurs: the intraoperative assessment of stem stability. The surgeon must perform a manual "push-pull" test. By placing an instrument on the collar or trunnion of the prosthesis (if exposed) or by manipulating the proximal fragment, the surgeon assesses for any gross or micromotion between the stem, the cement mantle, and the proximal bone. If any motion is detected, the diagnosis changes immediately to a Vancouver B2 fracture, and the surgical plan must pivot to stem extraction and revision using a long diaphyseal-engaging stem. Assuming the stem in this vignette remains rigidly fixed, the procedure proceeds with internal fixation.
Fracture Reduction Techniques
Direct exposure of the fracture fragments is minimized to preserve the fracture hematoma and periosteal attachments. Indirect reduction techniques are paramount. Traction is applied manually or via a femoral distractor. Pointed reduction forceps can be applied percutaneously or through the primary incision to manipulate major fragments. The goal is the restoration of length, alignment, and rotation, rather than anatomic cortical apposition of every comminuted fragment.
Plate Application and Fixation Strategy
A broad, heavy-duty locking compression plate (e.g., 4.5/5.0 mm LCP) is selected. The plate is slid submuscularly along the lateral aspect of the femur.
Proximal Fixation: In the region of the indwelling stem, bicortical screw purchase is impossible without damaging the implant or the cement mantle, which could precipitate late loosening. Fixation here relies on cerclage cables or wires passed circumferentially around the bone and plate. Specialized cable-ready plates or cable buttons are utilized. Care must be taken using cable passers to stay strictly on the bone to avoid neurovascular injury medially. Alternatively, specialized unicortical locking screws with blunt tips can be used to engage the lateral cortex without penetrating the cement mantle. A minimum of three, but preferably four or five, robust points of fixation are required in the proximal segment.
Distal Fixation: Distal to the stem tip, standard bicortical locking and non-locking screws are utilized. The plate must extend sufficiently distal to allow for at least four bicortical screws (eight cortices) spread over a long segment to maximize the working length of the construct.
Construct Optimization: To prevent a stress riser at the proximal end of the plate, the plate must overlap the proximal stem by at least two femoral diameters. If the bone is severely osteoporotic, the surgeon may augment the construct with a cortical allograft strut placed anteriorly or medially, secured with the same cerclage cables used for the plate. This creates a highly stable orthogonal construct.
Closure and Hemostasis
Following copious irrigation and fluoroscopic confirmation of alignment and hardware placement, the vastus lateralis is allowed to fall back into anatomical position. The fascia lata is closed meticulously with heavy absorbable sutures. Subcutaneous tissues and skin are closed in a standard layered fashion. Given the extensive dead space and potential for bleeding, a closed suction drain is frequently employed.
Complications and Management
Periprosthetic femur fractures carry a high rate of complications, driven by the advanced age of the typical patient demographic, the compromised local biology, and the mechanical challenges of fixation.
Common Complications and Salvage Strategies
| Complication | Estimated Incidence | Etiology and Risk Factors | Salvage and Management Strategies |
|---|---|---|---|
| Aseptic Nonunion | 5% - 12% | Excessive periosteal stripping, rigid short-segment fixation, poor bone biology | Revision ORIF with bone grafting (autograft/rhBMP-2), addition of cortical strut allografts, exchange to revision arthroplasty if stem loosens. |
| Hardware Failure | 3% - 8% | Plate fracture due to nonunion (fatigue failure), screw pullout in osteoporotic bone | Revision fixation utilizing dual plating (lateral and anterior), longer constructs, optimization of metabolic bone health. |
| Periprosthetic Joint Infection | 2% - 5% | Extensive soft tissue dissection, hematoma formation, prolonged operative time | Aggressive surgical debridement, implant retention (DAIR) if acute; two-stage revision with antibiotic spacer if chronic or involving loose hardware. |
| Stem Loosening (Late) | 5% - 10% | Unrecognized intraoperative instability, damage to cement mantle during drilling | Revision total hip arthroplasty utilizing long diaphyseal-engaging fluted tapered stems. |
| Venous Thromboembolism | 2% - 6% | Endothelial injury, venous stasis, hypercoagulability post-trauma | Chemical prophylaxis (LMWH or DOACs), mechanical compression, prompt mobilization. |
The management of nonunion is particularly challenging. If a patient presents with progressive pain and radiographic evidence of hardware failure or lack of callus formation at six months, intervention is required. If the stem remains well-fixed, revision plating with decortication, autologous bone grafting (e.g., from the iliac crest or using the Reamer-Irrigator-Aspirator system), and potentially dual-plate constructs are indicated.
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol must balance the mechanical limitations of the fixation construct with the absolute necessity of early mobilization in the geriatric population.
Weight Bearing and Mobilization
Historically, patients with periprosthetic fracture fixation were kept non-weight bearing for extended periods. However, modern locking plate technology and robust cerclage constructs allow for more aggressive rehabilitation.
For a securely fixed Vancouver B1 fracture utilizing a long locking plate and adequate proximal/distal purchase, patients are typically allowed touch-down or flat-foot weight bearing (approximately 10-15% of body weight) immediately postoperatively. This aids in proprioception and balance while protecting the hardware from catastrophic failure. Progression to partial and full weight bearing is strictly guided by radiographic evidence of bridging callus, typically assessed at the 6-week and 12-week postoperative marks.
Physical therapy focuses on early range of motion of the hip and knee to prevent arthrofibrosis. Hip abductor strengthening is initiated cautiously, as aggressive active abduction can place significant stress on the proximal fixation.
Medical Management and Optimization
The patient in the vignette has a history of osteoporosis and discontinued alendronate therapy. A critical component of the postoperative protocol is the reinstitution of metabolic bone management. Following the acute healing phase, an endocrinology or metabolic bone specialist consultation is mandatory to optimize calcium/Vitamin D levels and initiate appropriate anabolic or antiresorptive pharmacological therapy (e.g., Teriparatide or Denosumab, depending on specific indications and contraindications).
Furthermore, given her history of coronary artery disease and current aspirin use, deep vein thrombosis prophylaxis must be carefully managed. While aspirin 81mg provides some baseline protection, the massive thrombogenic stimulus of a femur fracture and subsequent surgery usually necessitates bridging to a low-molecular-weight heparin (LMWH) or a direct oral anticoagulant (DOAC) for 28 to 35 days postoperatively, in consultation with her cardiologist.
Summary of Key Literature and Guidelines
The management of periprosthetic fractures is heavily guided by established classification systems and evolving biomechanical research.
The seminal work by Duncan and Masri detailing the Vancouver Classification remains the foundational text for these injuries. Their classification elegantly dictates that the status of the implant is the primary driver of surgical decision-making.
Recent literature has focused heavily on the biomechanics of fixation for Vancouver B1 fractures. Studies by Ricci et al. and others have demonstrated that locking plates alone, while standard, may have unacceptably high failure rates in severely osteoporotic bone. This has led to the increasing adoption of supplementary fixation techniques. The use of cortical allograft struts, applied orthogonally to the lateral plate, has been shown in biomechanical models to significantly increase the load to failure and torsional rigidity of the construct.
Furthermore, the American Academy of Orthopaedic Surgeons (AAOS) guidelines emphasize the necessity of an interdisciplinary approach. The orthogeriatric co-management model—where orthopedic surgeons and geriatricians collaboratively manage the patient from admission through discharge—has been definitively shown to reduce time to surgery, decrease length of hospital stay, and lower the one-year mortality rate in elderly patients with periprosthetic fractures.
In conclusion, the successful management of a periprosthetic hip fracture requires a meticulous synthesis of accurate classification, advanced preoperative templating, precise execution of biological fixation principles, and comprehensive postoperative medical and rehabilitative care.
