Unstable Intertrochanteric Femur Fracture: Case Study, Diagnosis & Clinical Management
Key Takeaway
An unstable intertrochanteric femur fracture is diagnosed by severe hip pain and limb deformity after a fall. Radiographs confirm comminution, displacement, and specific patterns like AO/OTA 31-A2.2. Clinical examination, detailed imaging, and lab results are crucial for accurate classification and guiding the complex surgical management of this common geriatric orthopedic injury.
Patient Presentation and History
A 78-year-old male presented to the emergency department following a ground-level fall at home. He reported immediate onset of severe left hip pain and an inability to bear weight on the affected limb. He was found lying on the floor by his spouse approximately one hour after the fall. The mechanism described was a simple slip on a rug, resulting in a direct lateral impact to the left greater trochanteric region.
His medical history is highly relevant to his perioperative risk stratification and includes several systemic comorbidities. He has a long-standing history of Hypertension, currently managed with Amlodipine 5mg once daily. He also has Type 2 Diabetes Mellitus, managed with Metformin 1000mg twice daily, with a recent HbA1c of 7.1%, indicating reasonable glycemic control.
Crucially, the patient has a history of non-valvular Atrial Fibrillation and is currently anticoagulated with Apixaban 5mg twice daily. This presents a significant perioperative challenge regarding the timing of surgical intervention versus the risk of intraoperative hemorrhage. His renal function is impaired, classified as Chronic Kidney Disease Stage 3a, with an estimated glomerular filtration rate (eGFR) of 52 mL/min/1.73m². This degree of renal impairment directly affects the clearance kinetics of Apixaban and must be factored into the decision matrix for surgical timing.
Furthermore, he carries a diagnosis of Osteoporosis, established three years prior via dual-energy X-ray absorptiometry (DEXA), but is notably not on any specific anti-resorptive or anabolic therapy. This untreated osteoporotic state significantly compromises local bone quality, directly impacting implant purchase and increasing the risk of hardware failure, such as lag screw cut-out. His surgical history is notable for a previous right total knee arthroplasty performed five years ago without complication.
Prior to the injury, the patient lived independently with his wife and was community ambulatory, utilizing a single-point cane for longer distances. His social history indicates he is a retired school teacher, a lifelong non-smoker, and consumes alcohol occasionally. A thorough systems review upon admission denied any prodromal symptoms such as syncope, vertigo, palpitations, or chest pain prior to the fall, suggesting a purely mechanical etiology for the trauma rather than a secondary fall from a primary medical event.
Perioperative Medical Optimization
The presence of a direct oral anticoagulant (DOAC) in a geriatric hip fracture patient requires immediate multidisciplinary coordination. Current orthopedic trauma guidelines emphasize the importance of surgical intervention within 48 hours of admission to mitigate mortality, decrease the incidence of decubitus ulcers, and reduce rates of nosocomial pneumonia and deep vein thrombosis. However, operating on a fully anticoagulated patient risks catastrophic blood loss.
Given the patient's eGFR of 52 mL/min/1.73m², the half-life of Apixaban is approximately 12 to 15 hours. The standard protocol dictates withholding the DOAC and trending anti-Xa levels if available, or waiting a minimum of 48 hours from the last dose before proceeding with neuraxial anesthesia or major surgery. Reversal agents such as Andexanet alfa or 4-factor Prothrombin Complex Concentrate (PCC) are generally reserved for life-threatening hemorrhage and are rarely indicated for expediting semi-elective hip fracture surgery due to their profound prothrombotic risks. Therefore, the clinical pathway for this patient involves admission to the orthopedic trauma service with medical co-management, aggressive hydration to protect renal function, and scheduling for surgical fixation approximately 48 hours after his last Apixaban dose, provided his clinical status remains stable.
Clinical Examination Findings
Upon initial evaluation in the trauma bay, the patient was conscious, alert, and oriented, though in acute distress secondary to localized pain. The primary survey (Airway, Breathing, Circulation, Disability, Exposure) was intact and unremarkable.
Inspection and Palpation
Inspection of the left lower extremity revealed the classic pathognomonic posture of a proximal femur fracture. The limb was noticeably shortened by approximately 3 centimeters and held in a position of fixed external rotation. This deformity is biomechanically driven by the unopposed pull of the iliopsoas muscle on the lesser trochanter (contributing to external rotation and flexion) and the proximal pull of the gluteal musculature and adductor complex (driving the shortening).
Significant ecchymosis was already developing over the greater trochanter and lateral thigh, accompanied by diffuse, tense swelling encompassing the entire left hip joint and proximal thigh. A meticulous skin survey confirmed the absence of open wounds, abrasions, or impending skin tenting that would necessitate emergent intervention.
Palpation elicited exquisite point tenderness directly over the greater trochanter and the anterior groin crease. Palpable crepitus was noted with micro-motion of the limb. Extensive manipulation was strictly avoided to prevent further soft tissue trauma, neurovascular compromise, and exacerbation of the patient's pain.
Range of Motion and Neurovascular Assessment
Active range of motion of the left hip was completely abrogated due to pain inhibition. Passive range of motion was attempted with extreme caution; it revealed a marked mechanical block to internal rotation, adduction, and flexion. Any capsular stretch or movement of the fracture fragments resulted in severe pain escalation. The ipsilateral knee and ankle joints demonstrated full, painless arcs of motion, ruling out concomitant distal injuries.
A rigorous neurovascular examination is paramount in high-energy or highly displaced proximal femur fractures. Peripheral pulses, including the femoral, popliteal, dorsalis pedis, and posterior tibial arteries, were palpable, bounding, and symmetrical bilaterally. Capillary refill was brisk (less than 2 seconds) in all digits of the left foot.
Neurological assessment confirmed that light touch and pinprick sensation were intact and symmetric across all dermatomes of the left lower extremity (L1 through S1). While formal motor strength grading (Medical Research Council scale) of the hip and knee musculature was precluded by pain, gross distal motor function was intact. The patient demonstrated strong, symmetrical ankle dorsiflexion (deep peroneal nerve), ankle plantarflexion (tibial nerve), and extensor hallucis longus function. Patellar and Achilles deep tendon reflexes were graded as 2+ and symmetric.
Analgesic Management via Regional Blockade
To facilitate further evaluation, imaging, and patient comfort while awaiting surgical clearance, a fascia iliaca compartment block (FICB) was administered under ultrasound guidance in the emergency department. Utilizing 30 mL of 0.25% Bupivacaine, the block successfully anesthetized the femoral nerve and lateral femoral cutaneous nerve, providing profound analgesia without the systemic respiratory or cognitive side effects associated with high-dose intravenous opioids. This regional technique is an essential component of the modern geriatric fracture care pathway.
Imaging and Diagnostics
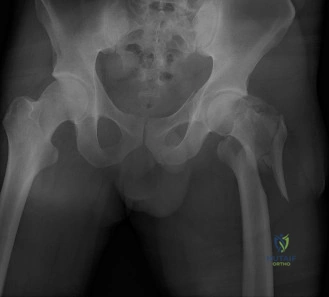
Initial radiographic evaluation in the emergency department consisted of a standard anteroposterior (AP) view of the pelvis, an AP view of the left hip, and a cross-table lateral view of the left proximal femur.
Radiographic Analysis
The AP pelvis radiograph demonstrated a complex, comminuted fracture involving the intertrochanteric region of the left femur. The primary fracture line propagated from the tip of the greater trochanter, extending inferiorly and medially to exit below the lesser trochanter.

There was pronounced comminution of the posteromedial cortex. The lesser trochanter was completely detached and displaced proximally and anteriorly due to the pull of the iliopsoas tendon. This posteromedial void is a critical determinant of fracture instability, as it eliminates the primary calcar strut necessary to resist compressive forces. Furthermore, there was significant proximal migration of the femoral shaft relative to the head-neck segment, resulting in varus collapse and the clinically observed limb shortening.
The cross-table lateral view provided essential three-dimensional context, confirming the posterior comminution and highlighting the degree of apex-anterior angulation at the fracture site. Crucially, the lateral radiograph allowed for the assessment of the anterior cortex, which is often the only remaining intact cortical hinge in severe intertrochanteric fractures.
Assessment of the Lateral Wall
A pivotal component of the radiographic analysis is the evaluation of the lateral femoral wall. The lateral wall is defined as the cortical bone extending from the vastus ridge to the tip of the greater trochanter. Its integrity is the primary anatomical factor dictating the choice of fixation implant. In this patient, while the lateral wall was not entirely blown out, its thickness was measured at approximately 18 millimeters on the AP radiograph. Biomechanical studies and clinical literature demonstrate that a lateral wall thickness of less than 20.5 millimeters is a strong predictor of postoperative lateral wall fracture and subsequent fixation failure if a sliding hip screw (extramedullary device) is utilized. This finding strongly mandates the use of an intramedullary device.
Advanced Imaging Indications
In this specific presentation, the plain radiographs provided sufficient detail to classify the fracture, determine instability, and formulate a definitive operative plan. Therefore, a computed tomography (CT) scan was not strictly indicated. However, CT imaging with 3D reconstruction is frequently utilized in modern orthopedic trauma for specific scenarios:
1. Evaluating occult extension of the fracture into the subtrochanteric region.
2. Assessing for a coronal shear component of the greater trochanter, which can complicate the entry point for cephalomedullary nailing.
3. Determining the exact morphology of the lesser trochanteric fragment and the extent of the posteromedial void.
Preoperative Templating
Digital preoperative templating was performed using the contralateral, uninjured right proximal femur as a reference to restore native biomechanics. Key parameters measured included:
* Neck-Shaft Angle: Templated at 130 degrees to restore native offset and abductor tension.
* Canal Diameter: Measured at the narrowest point of the isthmus to determine the appropriate nail diameter (templating suggested an 11.5mm nail to allow for 1-1.5mm of over-reaming).
* Lag Screw Length: Estimated to achieve a Tip-Apex Distance (TAD) of less than 25 millimeters, ensuring central-central or inferior-central placement within the femoral head.
Differential Diagnosis
While the clinical presentation of a shortened, externally rotated limb in an elderly patient following a fall is highly indicative of a proximal femur fracture, the exact anatomical location and fracture pattern must be differentiated, as this dictates the surgical approach and implant selection.
| Differential Diagnosis | Clinical Presentation | Radiographic Hallmarks | Biomechanical Implications |
|---|---|---|---|
| Intertrochanteric Femur Fracture | Severe groin pain, shortened and externally rotated limb. Swelling over the greater trochanter. | Fracture line between greater and lesser trochanters. Extracapsular. Often involves comminution of posteromedial cortex. | Extracapsular location means excellent blood supply and high union rates. Fixation must resist massive varus and rotational forces. |
| Femoral Neck Fracture | Groin pain, shortened and externally rotated limb (often less pronounced than intertrochanteric). | Fracture line proximal to the intertrochanteric line. Intracapsular. Disruption of medial calcar. | Intracapsular location disrupts the medial epiphyseal vessels, leading to high rates of avascular necrosis (AVN) and non-union. Often requires arthroplasty in the elderly. |
| Subtrochanteric Femur Fracture | Thigh pain, shortened limb. Proximal fragment flexed, abducted, and externally rotated. | Fracture centered within 5 cm distal to the lesser trochanter. | High cortical bone stress area. Deforming muscle forces make reduction extremely difficult. Requires intramedullary nailing with meticulous reduction techniques. |
| Acetabular Fracture (Anterior Column/Wall) | Groin pain, inability to bear weight. Limb may be externally rotated but shortening is less common unless central dislocation occurs. | Disruption of the iliopectineal line or anterior lip of the acetabulum on AP pelvis or Judet views. | Intra-articular injury. Requires precise anatomical reduction to prevent post-traumatic osteoarthritis. Often requires extensive pelvic approaches. |
Surgical Decision Making and Classification
The decision-making process for proximal femur fractures hinges on fracture stability, anatomical location, and patient-specific physiological reserves.
Fracture Classification
Based on the radiographic findings, this fracture is classified under the AO/OTA alphanumeric system as a 31-A2.2 fracture.
* 31: Femur, proximal segment.
* A: Extracapsular, trochanteric area.
* 2: Multifragmentary (comminuted) fracture.
* .2: Intermediate comminution, specifically involving the lesser trochanter and the posteromedial cortex, but with an intact (though thin) lateral wall.
Historically, the Evans-Jensen classification is also utilized, classifying this as a Type III fracture (unstable due to loss of posteromedial support).
Rationale for Operative Intervention
Non-operative management of intertrochanteric fractures in the ambulatory elderly population is associated with unacceptably high mortality rates (approaching 50-60% at one year), primarily due to complications of prolonged immobility, including deep vein thrombosis, pulmonary embolism, decubitus ulcers, pneumonia, and rapid physiological deconditioning. Operative fixation is therefore the absolute standard of care, serving as a resuscitative measure to allow for immediate weight-bearing and mobilization.
Implant Selection
The fundamental biomechanical goal in fixing an intertrochanteric fracture is to achieve a stable construct that allows for controlled impaction along the axis of the femoral neck while preventing varus collapse and excessive shortening. The two primary implant categories are extramedullary devices (Sliding Hip Screw - SHS) and intramedullary devices (Cephalomedullary Nail - CMN).
For stable fracture patterns (AO/OTA 31-A1) with an intact posteromedial cortex and a thick lateral wall, the SHS remains a highly effective, low-cost option. However, for unstable patterns like the 31-A2.2 presented in this case, the cephalomedullary nail is the implant of choice.
The rationale for utilizing a short cephalomedullary nail in this patient includes:
1. Shorter Lever Arm: The intramedullary location of the nail shifts the weight-bearing axis medially, closer to the mechanical axis of the limb, significantly reducing the bending moment on the implant compared to a lateral plate.
2. Lateral Wall Protection: The proximal aperture of the nail acts as an internal buttress. In fractures with a thin lateral wall (<20.5mm), an SHS requires a large lateral cortical window for the barrel, which often causes iatrogenic blowout of the lateral wall, converting the fracture to a highly unstable reverse-obliquity equivalent. The nail bypasses this risk.
3. Load Sharing: The CMN acts as a load-sharing device, transmitting forces directly into the femoral diaphysis, which is critical in the presence of severe posteromedial comminution where the native bone cannot share the compressive load.
4. Minimally Invasive Approach: Nailing can be performed through smaller incisions, reducing soft tissue stripping, blood loss, and operative time—crucial factors in a medically complex patient with CKD and recent DOAC use.
Surgical Technique and Intervention
The patient was taken to the operating room 48 hours after his last dose of Apixaban. Preoperative laboratory values confirmed a stable hemoglobin and normal coagulation parameters.
Patient Positioning and Setup
Following the induction of general endotracheal anesthesia (chosen over spinal anesthesia due to the recent DOAC use and the risk of epidural hematoma), the patient was transferred to a radiolucent fracture table. The patient was positioned supine with the bilateral upper extremities secured across the chest to allow unrestricted access for the C-arm fluoroscopy unit.
The perineal post was carefully padded to prevent pudendal nerve neurapraxia. The uninjured right leg was placed in a well-leg holder, flexed, and abducted to allow the C-arm to swing freely for cross-table lateral imaging of the operative hip. The injured left leg was secured in the traction boot.
Closed Reduction Maneuvers
Achieving an anatomical or slightly valgus reduction prior to draping is the most critical step in cephalomedullary nailing. The reduction maneuver proceeded as follows:
1. Longitudinal Traction: Gross traction was applied to restore limb length, utilizing the AP fluoroscopic view to compare the level of the lesser trochanter with the contralateral side.
2. Internal Rotation: The limb, which was resting in external rotation, was internally rotated approximately 10 to 15 degrees to antevert the femoral neck, bringing it parallel to the floor. This is essential for obtaining a true lateral fluoroscopic image.
3. Fluoroscopic Assessment: AP and lateral views were obtained. The AP view demonstrated restoration of the neck-shaft angle (aiming for 130-135 degrees) and correction of varus. The lateral view confirmed the reduction of the anterior cortical hinge, eliminating any apex-anterior sag.
The reduction was deemed acceptable, demonstrating cortical contact anteriorly and slight valgus impaction on the AP view. The surgical field was then prepped with Chlorhexidine-Alcohol and draped in a standard sterile fashion.
Surgical Approach and Entry Point
A 4-centimeter longitudinal incision was made approximately 2 to 3 centimeters proximal to the tip of the greater trochanter, in line with the femoral shaft. The fascia lata was incised in line with the skin incision, and the gluteus medius muscle fibers were bluntly split to access the trochanteric tip.
Establishing the correct starting point is paramount to avoid iatrogenic varus malalignment. Under biplanar fluoroscopy, a threaded guide pin was advanced. On the AP view, the entry point was targeted exactly at the tip of the greater trochanter (or slightly medial to it, depending on the specific nail design). On the lateral view, the pin was centered in the anterior-posterior plane of the greater trochanter, in line with the medullary canal.
Once the guide pin position was confirmed, an opening reamer was advanced over the pin to breach the proximal cortex, taking care to protect the soft tissues with a tissue protector.
Canal Preparation and Nail Insertion
A ball-tipped guide wire was passed down the femoral shaft to the level of the distal metaphysis. The canal was sequentially reamed over the guide wire in 0.5-millimeter increments up to 11.5 millimeters. Reaming was performed to generate autologous bone graft at the fracture site and to ensure smooth passage of the implant.
A 10-millimeter by 200-millimeter short cephalomedullary nail (130-degree neck angle) was assembled on the insertion jig. The nail was advanced over the guide wire by hand, utilizing gentle twisting motions. Mallet strikes were strictly avoided to prevent iatrogenic fracture of the femoral shaft. The nail depth was adjusted under fluoroscopy so that the projected trajectory of the cephalic lag screw was positioned in the inferior half of the femoral neck on the AP view and perfectly central on the lateral view.
Cephalic Fixation and the Tip-Apex Distance
Through the targeting jig, a lateral stab incision was made, and the guide pin sleeve was advanced to the lateral cortex. A guide pin was drilled into the femoral neck and head.
The placement of this pin dictates the success of the operation. The goal was to achieve a Tip-Apex Distance (TAD) of less than 25 millimeters. The TAD, described by Baumgaertner, is the sum of the distance from the tip of the lag screw to the apex of the femoral head on both the AP and lateral radiographs, after correcting for magnification. A TAD > 25mm is the single most significant predictor of lag screw cut-out.
Fluoroscopy confirmed the guide pin was placed inferiorly on the AP view (resting on the dense calcar bone) and centrally on the lateral view. The pin was measured, and the lateral cortex was opened. A lag screw was advanced over the pin to within 5 millimeters of the subchondral bone. The traction was temporarily released, and the compression mechanism of the nail was utilized to actively compress the intertrochanteric fracture site, closing the gap and stabilizing the construct.
Distal Interlocking and Closure
To control rotation and provide axial stability, a single distal interlocking screw was placed through the targeting jig via a stab incision. The screw was placed in a dynamic slot to allow for further micro-motion and secondary bone healing.
Final fluoroscopic images were saved, confirming excellent fracture reduction, optimal hardware placement, a TAD of 18 millimeters, and no evidence of iatrogenic fracture. The wounds were irrigated with sterile saline. The fascia lata was closed with interrupted #1 Vicryl sutures, the subcutaneous tissue with 2-0 Vicryl, and the skin with surgical staples. A sterile dressing was applied.
Post Operative Protocol and Rehabilitation
The immediate postoperative focus shifted to medical stabilization, pain management, and early mobilization.
Medical Management
- VTE Prophylaxis: Given the patient's preoperative Apixaban use, postoperative chemical prophylaxis requires careful timing. Standard protocol dictates restarting the DOAC 24 to 48 hours postoperatively, assuming complete hemostasis at the surgical site and stable hemoglobin levels. Mechanical prophylaxis (sequential compression devices) was initiated immediately in the recovery room.
- Pain Management: A multimodal analgesic regimen was employed to minimize opioid consumption and reduce the risk of postoperative delirium. This included scheduled intravenous Acetaminophen, oral Gabapentin, and PRN low-dose short-acting opioids. The preoperative fascia iliaca block provided significant residual pain control for the first 12-18 hours.
- Delirium Precautions: Geriatric protocols were initiated, including strict sleep-wake cycles, early removal of the indwelling urinary catheter, and avoidance of anticholinergic medications.
- Fluid and Renal Management: Intravenous fluids were titrated to maintain adequate urine output, carefully monitoring the patient's CKD Stage 3a status to prevent acute-on-chronic kidney injury.
Rehabilitation and Weight Bearing
The patient was cleared for Weight Bearing As Tolerated (WBAT) on the operative extremity immediately postoperatively. The biomechanical strength of the cephalomedullary construct in this fracture pattern allows for full weight loading, which is essential for fracture impaction and healing.
Physical therapy evaluated the patient on postoperative day one. Initial goals included bed mobility, transfers from bed to chair, and ambulation with a standard walker. The patient successfully ambulated 15 feet on postoperative day two. Occupational therapy focused on activities of daily living and adaptive equipment training.
Bone Health Optimization
A critical, often overlooked component of geriatric fracture care is secondary fracture prevention. This patient sustained a fragility fracture and has a known history of untreated osteoporosis. During the admission, an endocrinology consult was obtained. Baseline laboratory workup including Calcium, Vitamin D (25-OH), intact PTH, and comprehensive metabolic panel was drawn.
The plan was formulated to initiate an intravenous bisphosphonate (e.g., Zoledronic acid) prior to discharge, or alternatively, to refer the patient to a bone health clinic for initiation of anabolic therapy (e.g., Teriparatide or Romosozumab) given the severity of the fracture, pending optimization of his Vitamin D levels and evaluation of his renal function compatibility with these agents.
Clinical Pearls and Pitfalls
The management of unstable intertrochanteric fractures is fraught with potential complications. Adherence to strict biomechanical principles is required to achieve optimal outcomes.
- Pitfall: Varus Malreduction. Accepting a varus reduction increases the bending moment on the cephalic implant exponentially. This is the primary driver of hardware failure and cut-out. The fracture must be reduced anatomically or in slight valgus prior to draping. If closed reduction fails, percutaneous joysticks or a mini-open reduction using a bone hook must be employed.
- Pearl: The Anterior Cortical Hinge. On the lateral radiograph, the anterior cortex must be perfectly aligned. An apex-anterior sag indicates malreduction and will lead to eccentric reaming of the anterior cortex, potentially causing an iatrogenic anterior blowout during nail insertion.
- Pitfall: Ignoring the Lateral Wall. Failing to recognize a thin or compromised lateral wall and proceeding with a sliding hip screw will likely result in lateral wall catastrophic failure during dynamic impaction. Always utilize a cephalomedullary nail when the lateral wall is < 20.5mm or overtly fractured.
- Pearl: Calcar Referenced Pin Placement. When placing the cephalic guide pin, aiming for the inferior quadrant of the femoral head on the AP view allows the lag screw to rest on the dense primary compressive trabeculae (the calcar femorale). This provides the highest pull-out strength in osteoporotic bone.
- Pitfall: The Z-Effect and Reverse Z-Effect. In dual-screw cephalomedullary nails, differential migration of the screws can occur. The Z-effect involves lateral migration of the inferior screw and medial migration of the superior screw. The reverse Z-effect is the opposite. Utilizing a single, large-diameter helical blade or lag screw with a robust anti-rotation mechanism minimizes this risk in highly comminuted patterns.
- Pearl: Meticulous Starting Point. An entry point that is too lateral on the greater trochanter will force the nail into a varus trajectory, malreducing the fracture upon insertion. The entry must be exactly at the tip or slightly medial, directly in line with the medullary canal.
