Arthroscopic Ankle Arthrodesis: Master the Procedure
Key Takeaway
We review everything you need to understand about Arthroscopic Ankle Arthrodesis: Master the Procedure. **Arthroscopic ankle arthrodesis** is a minimally invasive surgical technique for severe ankle arthritis, resulting from conditions like osteoarthritis, rheumatoid arthritis, or trauma, when conservative treatments have proven ineffective. This procedure fuses the tibiotalar and fibulotalar articulations, aiming to alleviate persistent pain, correct gait abnormalities, and restore diminished function, thereby improving stability and quality of life for patients with advanced ankle joint degeneration.
Introduction and Epidemiology
Arthritis of the ankle represents a uniquely challenging pathology within orthopedic surgery, diverging significantly from the epidemiological profiles of hip and knee osteoarthritis. While primary osteoarthritis dominates the hip and knee, ankle arthritis is overwhelmingly post-traumatic in etiology, accounting for approximately 70% to 80% of cases. Other etiologies include primary osteoarthritis, rheumatoid arthritis, seronegative spondyloarthropathies, infectious sequelae, and crystalline arthropathies such as gout and pseudogout.

As articular cartilage degradation progresses, patients present with escalating mechanical pain, antalgic gait abnormalities, and progressive loss of function. When conservative modalities—including nonsteroidal anti-inflammatory drugs (NSAIDs), targeted intra-articular corticosteroid or orthobiologic injections, ankle-foot orthoses (AFOs), and activity modification—are exhausted, surgical intervention becomes indicated.

Historically, open ankle arthrodesis (OAA) was the gold standard for end-stage tibiotalar arthritis. However, the advent and refinement of arthroscopic ankle arthrodesis (AAA) have revolutionized the surgical management of this condition. First described in the 1980s, AAA has demonstrated superior outcomes in appropriately selected patients, including decreased surgical morbidity, minimized blood loss, accelerated rates of osseous union, and shorter hospital stays compared to traditional open techniques. This guide provides an exhaustive, step-by-step academic review of the arthroscopic ankle arthrodesis procedure.
Surgical Anatomy and Biomechanics
A profound understanding of the osseous and neurovascular anatomy of the ankle is paramount for safe portal placement and effective joint preparation. The ankle joint is a highly congruent hinge joint composed of the tibiotalar and fibulotalar articulations. The talar dome is wider anteriorly than posteriorly, contributing to inherent stability in dorsiflexion. The fibula bears approximately 16% to 20% of the weight-bearing stress across the ankle joint, acting as a dynamic lateral buttress.

Neurovascular Structures at Risk
Arthroscopic access to the ankle joint relies on standard anterior portals, which place several critical neurovascular structures at risk:
* Superficial Peroneal Nerve (SPN): The terminal branches (medial and intermediate dorsal cutaneous nerves) cross the anterolateral aspect of the ankle. The anterolateral portal must be established strictly lateral to the peroneus tertius tendon, utilizing transillumination and blunt dissection to avoid SPN injury.
* Saphenous Nerve and Vein: Located anterior to the medial malleolus. The anteromedial portal is placed immediately medial to the tibialis anterior tendon to avoid these structures.
* Deep Peroneal Nerve and Anterior Tibial Artery: These run centrally between the extensor hallucis longus (EHL) and extensor digitorum longus (EDL). Central portals are generally avoided in routine AAA to prevent catastrophic injury to this neurovascular bundle.

Biomechanically, a successful tibiotalar arthrodesis eliminates motion at the ankle joint proper. Consequently, compensatory motion and increased mechanical stress are transferred to the adjacent subtalar and transverse tarsal (Chopart) joints. Optimal positioning of the fused ankle is critical to mitigate accelerated adjacent segment disease and ensure a functional gait pattern.

Indications and Contraindications
Patient selection is the primary determinant of success in arthroscopic ankle arthrodesis. The procedure is highly effective for end-stage arthritis but possesses strict limitations regarding deformity correction and bone stock.
Standing evaluation is critical in determining the feasibility of an arthroscopic technique versus an open approach. Minor degrees of malalignment may be corrected arthroscopically (typically up to 10 to 15 degrees). Varus deformity is the most critical element to reverse to neutral, as residual varus leads to rigid lateral column overload and rapid subtalar breakdown.

Severe malalignment (>15 degrees), significant avascular necrosis (AVN) of the talus with structural collapse, and massive bone loss requiring structural allograft or autograft are general contraindications to the arthroscopic approach, necessitating an open procedure.
| Clinical Scenario | Operative Management | Non-Operative Management |
|---|---|---|
| End-Stage Osteoarthritis | Indicated (AAA preferred if deformity <15°) | Exhausted prior to surgery (Bracing, NSAIDs, Injections) |
| Severe Coronal Deformity (>15°) | Indicated (Open Arthrodesis with osteotomy) | Custom AFO / Patellar Tendon Bearing Brace |
| Significant Talar Bone Loss / AVN | Indicated (Open Arthrodesis with structural graft) | Non-weight bearing / Charcot Restraint Orthotic Walker (CROW) |
| Active Joint Infection | Contraindicated (Requires I&D, explant, antibiotics) | Intravenous Antibiotic Therapy |
| Neuropathic (Charcot) Arthropathy | Relative Contraindication for AAA (Open preferred for rigid fixation) | Total Contact Casting / CROW boot |
| Adjacent Subtalar Arthritis | Indicated (Consider combined Tibiotalocalcaneal Arthrodesis) | Rigid AFO to block hindfoot motion |

Pre Operative Planning and Patient Positioning
Thorough preoperative planning ensures appropriate patient selection and dictates the fixation strategy. Optimization of host factors is non-negotiable; smoking cessation is mandatory, and glycemic control (HbA1c < 7.5%) must be achieved to minimize the risk of nonunion and surgical site infection.
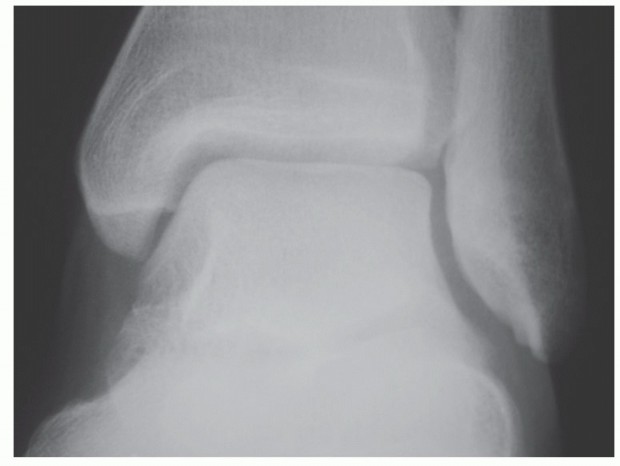
Imaging Modalities
Standard radiographic evaluation must include standing anteroposterior (AP), lateral, and mortise views. These images determine the extent of joint space narrowing, the presence of anterior or posterior osteophytes (which must be resected for access and correction), and the overall coronal and sagittal alignment.

Advanced imaging is frequently utilized. Computed tomography (CT) is highly recommended to evaluate subchondral cyst formation, bone stock, and hidden rotational deformities. Magnetic resonance imaging (MRI) is indicated if avascular necrosis of the talus is suspected, as compromised vascularity significantly alters the biological healing potential and may necessitate an open approach with bone grafting.

Patient Positioning and Setup
The patient is typically positioned supine on a radiolucent operating table. A bump is placed under the ipsilateral hip to internally rotate the lower extremity, bringing the foot into a neutral, upward-facing position (correcting for the natural external rotation of the hip).

A thigh tourniquet is applied but inflated only if visualization becomes compromised, as continuous fluid pump pressure (typically 40-50 mmHg) is often sufficient for hemostasis.

Joint distraction is critical for adequate visualization and instrument maneuverability. While invasive skeletal distraction (calcaneal and tibial pins) was historically popular, non-invasive strap distraction or manual gravity distraction is now preferred to avoid pin-site complications and tethering of the extensor tendons.

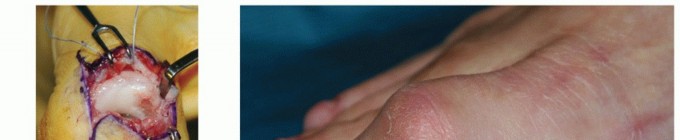
Detailed Surgical Approach and Technique
The arthroscopic ankle arthrodesis is a technically demanding procedure that requires meticulous attention to joint preparation and biomechanically sound fixation.
Portal Placement and Joint Access
Standard anteromedial and anterolateral portals are established. The anteromedial portal is created first, medial to the tibialis anterior tendon at the level of the joint line. A #11 blade is used for skin incision only, followed by blunt dissection with a mosquito hemostat to enter the joint capsule, protecting the saphenous nerve.

A 4.0-mm, 30-degree arthroscope is introduced. Under direct intra-articular visualization, the anterolateral portal is established lateral to the peroneus tertius using a spinal needle for precise localization. The skin is incised, and blunt dissection is utilized to bypass the superficial peroneal nerve branches.

Initial access is often impeded by significant synovial hypertrophy and large anterior tibial osteophytes. An aggressive synovectomy is performed using a 4.5-mm full-radius shaver. Anterior osteophytes are resected using a 4.0-mm or 5.5-mm motorized burr or arthroscopic osteotomes. This "gutter clearance" is mandatory to allow the talus to translate posteriorly during final positioning and to permit the arthroscope to advance into the posterior half of the joint.

Articular Preparation
The hallmark of a successful arthrodesis is the meticulous denudation of articular cartilage while preserving the structural integrity of the subchondral bone plate.

Using a combination of ring curettes, Cobb elevators, and motorized shavers, the remaining hyaline cartilage is stripped from the tibial plafond, the talar dome, and the medial and lateral gutters.

Once the cartilage is removed, the calcified cartilage layer must be addressed. A motorized high-speed burr is utilized to lightly decorticate the subchondral plate. The goal is to expose bleeding cancellous bone without destroying the subchondral architecture. Complete removal of the subchondral plate leads to structural collapse and loss of deformity correction.

The surgeon must observe the "punctate bleeding" or "paprika sign" across the entire surface of the tibia and talus. Continuous irrigation is vital during burring to prevent thermal necrosis of the bone, which can inhibit osteogenesis.

Microfracture awls or a 2.0-mm K-wire can be used to fenestrate the subchondral bone further, facilitating the migration of bone marrow elements and mesenchymal stem cells into the arthrodesis site.

Alignment and Fixation
Following thorough joint preparation, the distraction is released. The ankle is manually manipulated into the optimal position for fusion. The universally accepted parameters for ankle arthrodesis alignment are:
* Sagittal Plane: Neutral dorsiflexion (0 degrees). Avoid plantarflexion, which causes genu recurvatum, and avoid excessive dorsiflexion, which causes a peg-leg gait.
* Coronal Plane: 0 to 5 degrees of valgus. Varus positioning is strictly avoided.
* Axial Plane: 5 to 10 degrees of external rotation, matching the contralateral extremity.
* Translation: The talus should be translated slightly posterior to the mechanical axis of the tibia to improve the lever arm of the Achilles tendon.

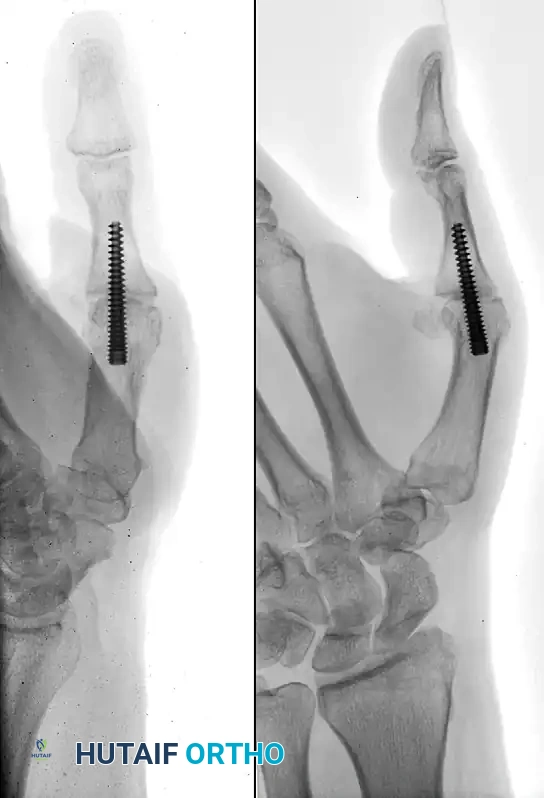
Once alignment is achieved and verified via multi-planar fluoroscopy, provisional fixation is obtained using large, threaded guide pins.

Definitive fixation typically consists of two or three large-diameter (6.5 mm to 7.3 mm) cannulated, partially threaded cancellous screws. The construct must provide rigid compression.

- The "Home Run" Screw: Placed from the posterior aspect of the distal tibia, directed anteriorly and inferiorly into the neck of the talus. This screw captures the densest bone and provides superior biomechanical stability.
- Medial Transmalleolar Screw: Directed from the medial malleolus into the lateral body of the talus.
- Lateral Transmalleolar Screw: Directed from the lateral malleolus into the medial body of the talus, crossing the medial screw superior to the joint line to avoid stress risers.

Screws are sequentially tightened to achieve uniform compression across the prepared joint surfaces. Fluoroscopy confirms screw length, trajectory, and the absence of joint penetration into the subtalar articulation.

Complications and Management
While arthroscopic ankle arthrodesis boasts a lower complication profile than open techniques, complications can still profoundly impact patient outcomes. Meticulous surgical technique and strict adherence to postoperative protocols are essential to mitigate these risks.

Nonunion (pseudoarthrosis) is the most significant complication. Risk factors include smoking, diabetes, inadequate joint preparation (failure to remove the calcified cartilage layer), thermal necrosis from aggressive burring without irrigation, and insufficient mechanical compression.

Nerve injury, particularly to the superficial peroneal nerve, is a known risk of anterior portal placement. Adjacent segment disease is an inevitable long-term consequence of ankle fusion, though its clinical manifestation can be delayed by achieving optimal neutral alignment during surgery.
| Complication | Estimated Incidence | Etiology / Risk Factors | Management / Salvage Strategy |
|---|---|---|---|
| Nonunion / Pseudoarthrosis | 3% - 10% | Smoking, AVN, poor compression, thermal necrosis | Revision open arthrodesis with autologous bone grafting (ICBG) and rigid plate fixation. |
| Superficial Peroneal Nerve Injury | 1% - 5% | Errant anterolateral portal placement | Observation for neuropraxia; surgical exploration and neurectomy if painful neuroma develops. |
| Infection (Superficial/Deep) | 1% - 3% | Diabetes, obesity, prolonged tourniquet time | Superficial: Oral antibiotics. Deep: Operative I&D, hardware removal if loose, IV antibiotics. |
| Malunion (Varus or Plantarflexion) | 2% - 5% | Inadequate intraoperative fluoroscopic assessment | Corrective closing wedge osteotomy and revision internal fixation. |
| Adjacent Segment Arthritis (Subtalar) | 50%+ at 10 years | Altered biomechanics, residual varus malalignment | Conservative management (bracing/injections); Subtalar arthrodesis if refractory. |
| Symptomatic Hardware | 10% - 15% | Prominent screw heads, lack of soft tissue coverage | Hardware removal after solid osseous union is confirmed via CT scan. |

Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol is designed to protect the fixation construct while biological healing occurs. Protocols may vary slightly based on surgeon preference and patient bone quality, but generally adhere to a strict phased timeline.
- Phase I (0 to 2 Weeks): The patient is placed in a sterile compressive dressing and a rigid posterior splint in the operating room. Strict non-weight-bearing (NWB) status is enforced. Elevation is critical to manage edema and prevent wound dehiscence.
- Phase II (2 to 6 Weeks): Sutures are removed at 2 weeks. The patient is transitioned to a short-leg cast or a locked controlled ankle motion (CAM) boot. Strict NWB status is maintained. Gentle active range of motion of the toes, knee, and hip is encouraged to prevent proximal atrophy.
- Phase III (6 to 12 Weeks): Radiographs are obtained at 6 weeks. If evidence of early trabecular bridging is present, the patient may begin progressive weight-bearing in a CAM boot, advancing from 25% to full weight-bearing over a 4-week period.
- Phase IV (12+ Weeks): Once solid osseous union is confirmed (often requiring a CT scan if radiographs are equivocal), the patient is transitioned to standard supportive footwear. Formal physical therapy is initiated, focusing on gait retraining, proprioception, and maximizing the range of motion in the adjacent transverse tarsal and subtalar joints.
Summary of Key Literature and Guidelines
The academic literature robustly supports the use of arthroscopic ankle arthrodesis over open techniques for appropriately selected patients.
Seminal studies by Ferkel et al. and O'Brien et al. established the early efficacy of the arthroscopic approach, demonstrating union rates exceeding 95%. More recent comparative cohorts and meta-analyses (e.g., Townshend et al., Gougoulias et al.) have consistently shown that AAA results in significantly shorter hospital stays, reduced postoperative pain, lower blood loss, and a faster time to clinical and radiographic union compared to OAA.
The primary caveat highlighted in the literature remains deformity. While highly experienced arthroscopists can manage coronal plane deformities up to 15 degrees, guidelines generally recommend open arthrodesis for deformities exceeding this threshold, or in cases of severe bone loss requiring structural grafting. Ultimately, arthroscopic ankle arthrodesis is a highly reliable, joint-salvaging procedure that restores function and alleviates pain in the setting of end-stage tibiotalar arthritis, provided meticulous surgical technique and rigid biomechanical principles are applied.
You Might Also Like