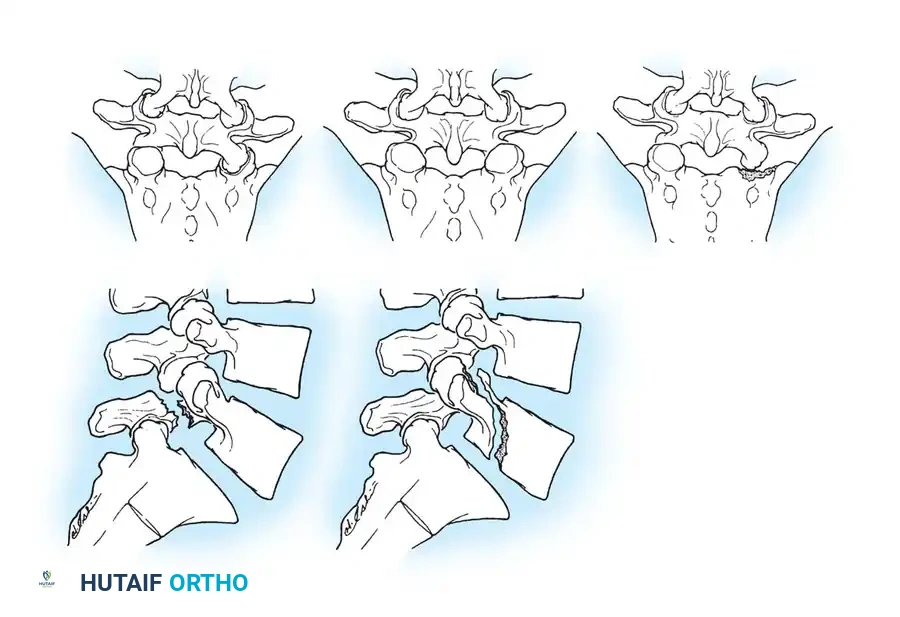
Operative Management of Pelvic Malunions and Nonunions
Key Takeaway
The operative management of pelvic malunions and nonunions presents a formidable challenge requiring meticulous preoperative planning and advanced surgical expertise. Indications for reconstruction include intractable pain, pelvic instability, sitting imbalance, and severe leg-length discrepancy. Successful correction often necessitates a complex, multi-stage surgical approach involving precise osteotomies, mobilization of fibrosed articulations, and rigid internal fixation to restore pelvic ring biomechanics and optimize patient outcomes.
Introduction to Pelvic Malunions and Nonunions
The management of pelvic malunions and nonunions represents one of the most formidable challenges in orthopedic traumatology. Historically, many pelvic ring disruptions were managed nonoperatively, leading to a high incidence of chronic deformity. Even with contemporary advancements in acute fracture fixation, malunions—particularly those involving the acetabulum with central dislocation of the femoral head—continue to occur. The pathoanatomy of these chronic lesions is characterized by complex, multiplanar deformities, severe soft-tissue contractures, and altered load-bearing biomechanics.
Late correction of a pelvic deformity is inherently more difficult, less successful, and associated with a significantly higher incidence of complications than the management of acute pelvic fractures. Therefore, the paramount principle in pelvic trauma remains adequate initial reduction and rigid stabilization to prevent the sequelae of malunion and nonunion. When chronic deformity does occur, operative intervention should be reserved for highly symptomatic patients and performed exclusively by surgeons with extensive experience in complex pelvic and acetabular reconstruction.
Clinical Evaluation and Indications for Surgery
Tile emphasized that a pelvic nonunion does not universally cause pain; however, severe malunions—most commonly those involving the sacroiliac (SI) complex—are frequently highly symptomatic. The decision to proceed with operative reconstruction must be based on a thorough clinical evaluation correlating the patient's symptoms with the radiographic deformity.
Primary Indications for Reconstruction
- Intractable Pain: Posterior pelvic pain is typically mechanical, arising from nonunion, chronic instability, or malreduction of the sacroiliac joint. Correction of these biomechanical faults provides reliable pain relief in the majority of patients. Conversely, posterior pelvic pain of uncertain etiology, or pain secondary to irreversible neurological injury, is unlikely to improve with structural reconstruction.
- Pelvic Instability: Gross clinical instability, often demonstrable on alternating single-leg stance, severely impairs gait and requires rigid stabilization.
- Sitting Imbalance: Cranial displacement of the hemipelvis (typically 1 cm or greater) leads to a profound sitting imbalance. The resulting asymmetrical ischial tuberosity prominence causes severe pain when sitting and a characteristic cosmetic deformity.
- Limb Shortening and Malrotation: Severe shortening combined with internal rotation of the hemipelvis alters the mechanical axis of the lower extremity. While isolated leg-length discrepancies can be managed with standard equalization techniques (e.g., shoe lifts or contralateral epiphysiodesis/shortening), complex rotational deformities often necessitate pelvic osteotomy.
- Visceral Impingement: A severely displaced superior pubic ramus can erode into the perineum or impinge upon the bladder, leading to urinary frequency, dyspareunia, or vaginal wall impingement.
Clinical Pearl: Always evaluate for concomitant lumbar spine pathology. Posterior pelvic pain may be referred from lumbar injuries, which must be ruled out or addressed concurrently to ensure optimal postoperative outcomes.
Patient Selection and Counseling
Patient selection is as critical as surgical execution. Patients must possess realistic expectations and fully comprehend the substantial risks involved, including massive blood loss, iatrogenic neurovascular injury, persistent nonunion, and loss of reduction. Furthermore, compliance is mandatory; patients must be capable of adhering to strict weight-bearing restrictions for 3 to 5 months postoperatively.
Radiographic and Advanced Imaging Assessment
A meticulous radiographic evaluation is required to define the extent of fracture union, the nature of the deformity, and the precise multiplanar geometry of the malunion.
Standard Radiographic Series
- Anteroposterior (AP) Pelvis: Evaluates overall ring symmetry and limb shortening. Limb shortening is quantified by comparing the cranial displacement of the acetabular roof relative to a line drawn perpendicular to the midline of the sacrum.
- Judet Views (45-degree Oblique): The obturator and iliac oblique views are essential for assessing the anterior and posterior columns of the acetabulum.
- Inlet and Outlet Views: The 40-degree caudad (inlet) view assesses posterior displacement and internal/external rotational deformities. The 40-degree cephalad (outlet) view evaluates cranial/caudal translation (vertical shear deformities).
- Single-Leg Stance Radiographs: Right and left alternating weight-bearing AP views are invaluable for detecting dynamic instability in nonunions.
Advanced Imaging
A high-resolution pelvic Computed Tomography (CT) scan is mandatory. Three-dimensional (3D) CT reconstructions provide an unparalleled spatial understanding of the deformity, allowing the surgeon to map proposed osteotomies and anticipate areas of severe bony impingement or defect.
Management of Acetabular Malunions
Malunions involving the acetabular articular surface rapidly precipitate post-traumatic osteoarthritis. Letournel’s landmark review of acetabular reconstructions established strict criteria for attempting joint-preserving surgery versus arthroplasty or arthrodesis.
Letournel’s Criteria for Acetabular Reconstruction
Before attempting a joint-preserving reconstruction of an acetabular malunion, the surgeon must evaluate:
1. The location and structural integrity of the different segments of the acetabular articular surface and their supporting bony columns.
2. The degree of mechanical wear and chondral damage on the femoral head.
3. The severity of established osteoarthritis.
4. The presence or absence of avascular necrosis (osteonecrosis) of the femoral head or acetabular fragments.
Treatment Algorithms
- Joint-Preserving Reconstruction: Indicated in younger patients with minimal femoral head wear and viable articular cartilage. Letournel reported excellent-to-fair results in 50% of highly selected patients.
- Arthrodesis: The treatment of choice for young, heavy laborers whose occupation requires prolonged standing or walking, provided they have severe unilateral post-traumatic arthritis and a normal contralateral hip, knee, and lumbar spine.
- Total Hip Arthroplasty (THA): Indicated for older patients, those with sedentary occupations, or those with advanced osteoarthritis/osteonecrosis. THA in the setting of pelvic malunion often requires complex acetabular reconstruction with structural bone grafting or custom triflange components to address bone loss and altered center of rotation.
The Three-Stage Reconstruction for Pelvic Ring Malunions
Matta, Dickson, and Markovich popularized the multi-stage approach for complex pelvic malunions. Because chronic deformities are tethered by robust, contracted fibrous tissue and healed bone, anatomical reduction is frequently impossible with a single approach. A three-stage procedure provides the maximal degree of mobilization and deformity correction.
Preoperative Setup and Positioning
Patients are placed on a radiolucent operating table to allow unimpeded fluoroscopic guidance for osteotomies, reduction, and hardware placement. A Judet traction table or a femoral distractor is highly advantageous for applying controlled, sustained traction to overcome chronic proximal migration of the hemipelvis.
Surgical Sequence
The procedure can be sequenced as Anterior-Posterior-Anterior or Posterior-Anterior-Posterior, depending on the primary site of deformity and the surgeon's preference. The classic sequence is as follows:
Stage 1: Anterior Mobilization (Supine)
- Approach: A Pfannenstiel or modified Stoppa approach is utilized to access the anterior ring.
- Osteotomy: The deformed anterior pelvic structures (symphysis or pubic rami) are osteotomized at the sites of the old injuries. Fibrous nonunions are aggressively debrided.
- Closure: The anterior wound is temporarily closed, and the patient is carefully repositioned.
Stage 2: Posterior Mobilization and Fixation (Prone)
- Approach: A posterior approach to the sacroiliac joint or sacrum is performed.
- Release and Osteotomy: Posterior pelvic deformities are osteotomized. To facilitate the correction of severe cranial displacement, the attachments of the sacrospinous and sacrotuberous ligaments to the sacrum must be divided.
- Reduction: Intraoperative external fixators, Schanz pins placed in the iliac wings, and femoral distractors are utilized as joysticks to manipulate the hemipelvis.
- Fixation: Once the posterior ring is reduced, it is rigidly stabilized using large-fragment reconstruction plates, transiliac-transsacral screws, or robust iliosacral screws. Old deformities are highly resistant to correction and exert massive deforming forces; therefore, fixation must be significantly stronger than that used for acute fractures.
- Closure: The posterior wound is definitively closed.
Stage 3: Anterior Reduction and Fixation (Supine)
- Repositioning: The patient is returned to the supine position, and the anterior wound is reopened.
- Final Reduction: With the posterior ring stabilized, the anterior reduction is finalized.
- Fixation: The symphysis or pubic rami are stabilized using multi-hole pelvic reconstruction plates.
Surgical Warning: Anatomical reduction of a chronic pelvic malunion is frequently impossible due to remodeling and soft-tissue contracture. The primary goals are the restoration of pelvic stability, correction of severe leg-length discrepancy, and normalization of sitting balance.
Management of Concurrent Proximal Femoral Malunions
High-energy pelvic trauma is occasionally accompanied by proximal femoral fractures. If mismanaged, these result in complex cervicotrochanteric or femoral head malunions that severely compromise hip biomechanics.
Cervicotrochanteric Malunions
In young adults, malunion of the femoral neck or intertrochanteric region often results in a severe varus and externally rotated deformity. While function can be improved with corrective osteotomy, complete restoration of the neck-shaft angle and limb length is rarely achieved.
Operative Technique for Trochanteric Osteotomy:
1. Exposure and Debridement: Due to external rotation, the fractured surface of the greater trochanter faces anteromedially, creating a wedge-shaped space filled with fibrous tissue. Excise this fibrous tissue down to bleeding bone.
2. Osteotomy: Divide the osseous union posteriorly with a sharp osteotome.
3. Mobilization: Tenotomize the adductors if necessary to obtain sufficient abduction of the distal fragment.
4. Reduction: Appose the bony surfaces. Correct the deformity by abducting and internally rotating the distal fragment while applying marked traction via a fracture table or femoral distractor.
5. Verification: Confirm the restoration of the neck-shaft angle using orthogonal image intensification.
6. Fixation: Stabilize the osteotomy with a dynamic hip screw (DHS) or proximal femoral locking plate.
* Pediatric Consideration: In children, a pediatric compression hip screw is preferred for easier insertion into the dense bone of the femoral neck, taking absolute care to avoid violating the capital femoral physis.
Femoral Head Malunions (Pipkin Fractures)
Femoral head fractures (e.g., Pipkin type I) treated nonoperatively can malunite, leading to mechanical blocks to motion and severe limping. Yoon et al. demonstrated that malunion should be highly suspected in patients with limited hip motion following closed management of posterior hip fracture-dislocations.
Management:
Surgical intervention involves a surgical dislocation of the hip (Ganz approach) or an anterior approach to access the joint. The protruding bony prominence of the malunited fragment is meticulously resected and debrided to restore the sphericity of the femoral head. Postoperatively, patients are allowed immediate full weight-bearing and aggressive range-of-motion exercises. Sontich and Cannada reported excellent outcomes with near-full, painless range of motion following this joint-preserving debridement.
Postoperative Protocol and Aftertreatment
The postoperative management of pelvic reconstructions is as critical as the surgery itself.
- Weight Bearing: Patients are restricted to toe-touch or non-weight-bearing status on the affected extremity for a minimum of 3 to 5 months, depending on the complexity of the osteotomies, the rigidity of the fixation, and radiographic evidence of union.
- Pediatric Considerations: If complete correction of a proximal femoral malunion is secured in a child, a spica cast should be applied and worn for at least 8 weeks. Even with meticulous fixation, a progressive decrease in the neck-shaft angle (varus collapse) is common as the bone remodels.
- Thromboprophylaxis: Given the extensive operative time (averaging 7 hours) and massive endothelial trauma, aggressive chemical and mechanical deep vein thrombosis (DVT) prophylaxis is mandatory unless contraindicated by active bleeding.
Complications and Outcomes
Operative correction of pelvic malunions carries a high complication profile. In Matta’s series of 37 patients, the overall complication rate was 19%, with an average blood loss approaching 2,000 mL (range 200 to 7,200 mL).
Specific Complications
- Neurological Injury (8.1%): The L5 nerve root is highly vulnerable during sacral osteotomies and iliosacral screw placement. Intraoperative neuromonitoring (SSEP and MEP) is highly recommended, though it does not completely eliminate the risk of postoperative footdrop. The superior gluteal nerve is also at risk during osteotomies extending into a deformed greater sciatic notch.
- Vascular Injury (2.7%): The external iliac vein and the corona mortis are at significant risk during anterior mobilization, particularly when dissecting through dense scar tissue. Immediate availability of a vascular surgeon is advised.
- Loss of Reduction (11%): Due to massive deforming forces, hardware failure or loss of reduction can occur, particularly in noncompliant patients who bear weight prematurely.
- Persistent Nonunion (5.4%): Requires revision bone grafting and augmented internal fixation.
Despite these risks, the functional payoff for carefully selected patients is substantial. Over 86% of patients report definitive improvement in pain, sitting balance, and gait, underscoring the value of this complex reconstructive endeavor when executed by experienced pelvic surgeons.
You Might Also Like