
Orthopedic MCQS Trauma 0018
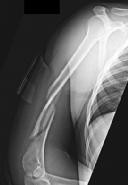
left shoulder in a motor vehicle collision. He underwent uncomplicated ORIF (see Figure 2), but at his first post-operative visit he had persistent pain and deformity (see Figure 3). What is the primary factor contributing to this complication?
---
---
---
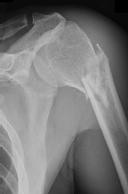
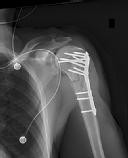
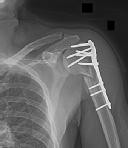
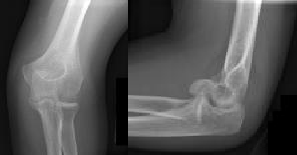
Figures 1 and 2 are the radiographs of a 35-year-old man who has elbow pain after falling from a ladder onto an outstretched hand. Examination reveals elbow pain, swelling, limited motion, and normal neurologic function.
A pathognomonic radiographic feature of this injury is a
---
---
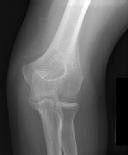
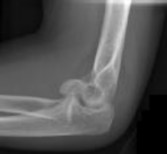
Figures 1 and 2 are the radiographs of a 35-year-old man who has elbow pain after falling from a ladder onto an outstretched hand. Examination reveals elbow pain, swelling, limited motion, and normal neurologic function.
What is the typical intra-operative patient position for treatment of this injury?
---
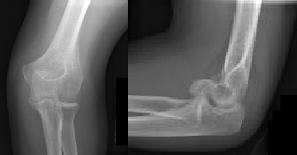
Figures 1 and 2 are the radiographs of a 35-year-old man who has elbow pain after falling from a ladder onto an outstretched hand. Examination reveals elbow pain, swelling, limited motion, and normal neurologic function.
The surgical exposure that provides optimal visualization to treat this injury is
---
---
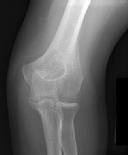
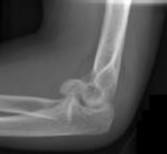
Figures 1 and 2 are the radiographs of a 35-year-old man who has elbow pain after falling from a ladder onto an outstretched hand. Examination reveals elbow pain, swelling, limited motion, and normal neurologic function.
What type of screws should be available for stabilization of this injury?
---
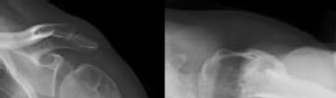
limited range of motion two years after a proximal humerus fracture, which was treated non-operatively. He has forward elevation to 100 degrees with pain at the terminal arc of motion. A subsequent MRI reveals no soft tissue abnormality. After a failed course of non-operative treatment, what is the most appropriate surgical treatment?
---
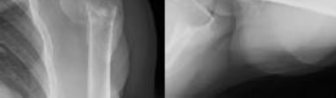
emergency department after a fall from a ladder with pain and a closed injury to his left shoulder. He undergoes open reduction internal fixation (ORIF) of his left proximal humerus fracture. A postoperative radiograph is shown in Figure


Figures 1 and 2 are the radiographs of a 19-year-old man with a closed right humeral shaft fracture as well as a right femoral shaft fracture and a left ankle fracture-dislocation after a motor vehicle collision. On initial examination, he is noted to have a complete radial nerve palsy of his right upper extremity.
What represents the best indication for surgical management of the humeral shaft fracture in this patient?
---
---
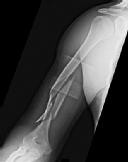
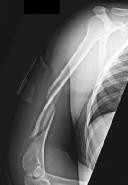
Figures 1 and 2 are the radiographs of a 19-year-old man with a closed right humeral shaft fracture as well as a right femoral shaft fracture and a left ankle fracture-dislocation after a motor vehicle collision. On initial examination, he is noted to have a complete radial nerve palsy of his right upper extremity.
After a discussion with the patient, surgery is chosen for the right humerus. A posterior triceps-reflecting approach is selected. What structure marks the most proximal extent of the humerus that can be exposed through this approach?
---
---
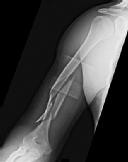
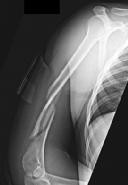
Figures 1 and 2 are the radiographs of a 19-year-old man with a closed right humeral shaft fracture as well as a right femoral shaft fracture and a left ankle fracture-dislocation after a motor vehicle collision. On initial examination, he is noted to have a complete radial nerve palsy of his right upper extremity.
Postoperative radiographs are shown in Figures 3 and
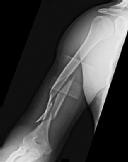
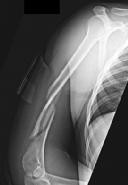
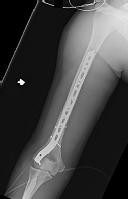
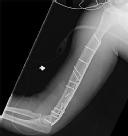
Figures 1 and 2 are the radiographs of a 19-year-old man with a closed right humeral shaft fracture as well as a right femoral shaft fracture and a left ankle fracture-dislocation after a motor vehicle collision. On initial examination, he is noted to have a complete radial nerve palsy of his right upper extremity.
The working length of the plate is best described as the length
---
---
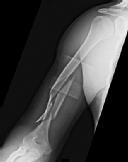
low-demand patient population?
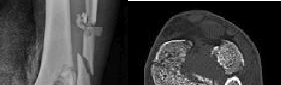
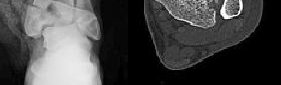
Figure 1 is the radiograph and Figure 2 is the CT image of a 45-year-old woman who fell about 20 feet off her balcony. These images show an isolated, open injury with a 3-cm open medial wound.
Three years following surgery, which parameter will most likely predict a poor clinical outcome and failure to return to work?
---
---
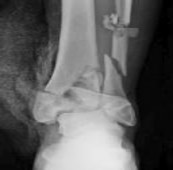
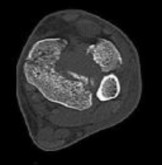
Figures 1 and 2 are the radiographs of a 68-year-old woman who comes to the emergency department after stepping into a hole and twisting her ankle. She is complaining of isolated ankle pain and is unable to bear weight.
After closed manipulative reduction and splint placement, she is scheduled for operative treatment. The stability of the syndesmosis should be evaluated after
---
---
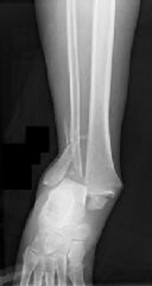
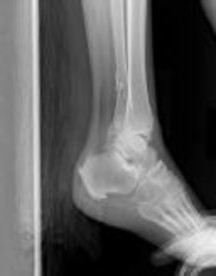
Figures 1 and 2 are the radiographs of a 68-year-old woman who comes to the emergency department after stepping into a hole and twisting her ankle. She is complaining of isolated ankle pain and is unable to bear weight.
How is syndesmotic instability best assessed intra-operatively?
---
---
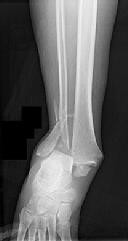
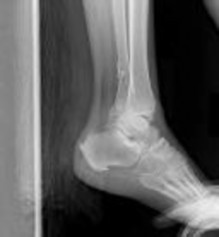
Figures 1 and 2 are the radiographs of a 68-year-old woman who comes to the emergency department after stepping into a hole and twisting her ankle. She is complaining of isolated ankle pain and is unable to bear weight.
How is syndesmotic reduction best assessed intra-operatively?
---


Figures 1 and 2 are the radiographs of a 68-year-old woman who comes to the emergency department after stepping into a hole and twisting her ankle. She is complaining of isolated ankle pain and is unable to bear weight.
Our understanding of malreduction of the syndesmosis has changed over the years based on changes in technique and imaging. Our current understanding is that malreduction of the syndesmosis
---

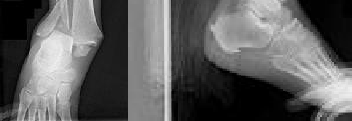
Figures 1 and 2 are the radiographs of a 68-year-old woman who comes to the emergency department after stepping into a hole and twisting her ankle. She is complaining of isolated ankle pain and is unable to bear weight.
Anatomic reduction and stabilization of the posterior malleolus fracture component
---

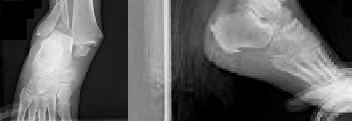
Figures 1 and 2 are the radiographs of a 68-year-old woman who comes to the emergency department after stepping into a hole and twisting her ankle. She is complaining of isolated ankle pain and is unable to bear weight.
What is the morphology of the posterior malleolar fracture component?
---
---
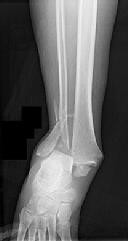
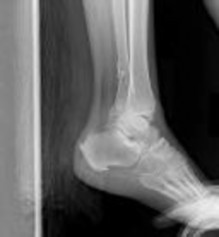
Figures 1 and 2 are the radiographs of a 35-year-old man who is brought into the emergency department after a motor vehicle collision. He is complaining of isolated knee pain. Examination reveals swelling, blood filled blisters, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
This knee injury is best described as a
---
---
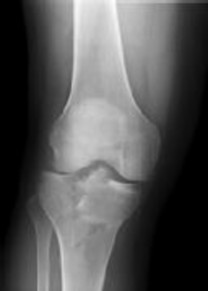
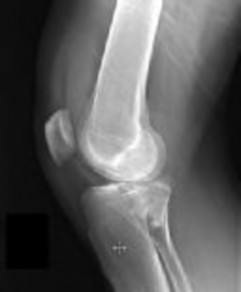
Figures 1 and 2 are the radiographs of a 35-year-old man who is brought into the emergency department after a motor vehicle collision. He is complaining of isolated knee pain. Examination reveals swelling, blood filled blisters, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
Initial surgical management should consist of
---
---
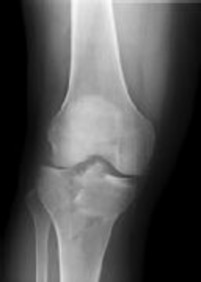
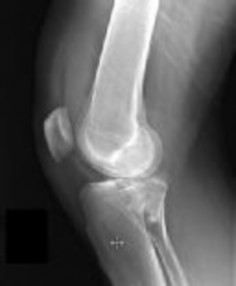
Figures 1 and 2 are the radiographs of a 35-year-old man who is brought into the emergency department after a motor vehicle collision. He is complaining of isolated knee pain. Examination reveals swelling, blood filled blisters, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
Figures 3 through 8 are the axial and sagittal CT scan sections of the injury. Intra-operative patient positioning for definitive fixation should be
---
---
---
---
---
---
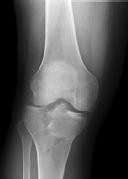


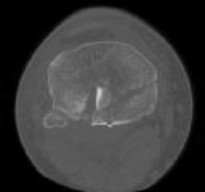
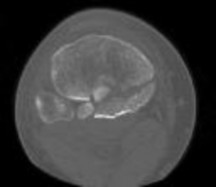




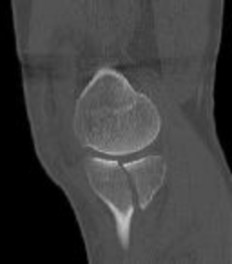
Figures 1 and 2 are the radiographs of a 35-year-old man who is brought into the emergency department after a motor vehicle collision. He is complaining of isolated knee pain. Examination reveals swelling, blood filled blisters, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
The surgical approach for definitive reduction and stabilization of this pattern is
---
---
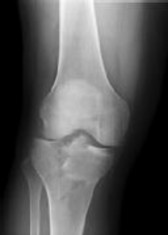
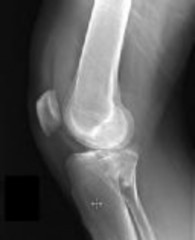
Figures 1 through 3 are the radiographs of a 25-year-old man who is brought to the emergency department after a motorcycle collision. He is complaining of isolated knee pain. Examination reveals swelling, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
This knee injury is best described as a
---
---
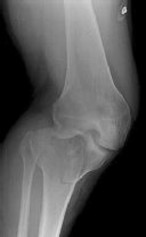
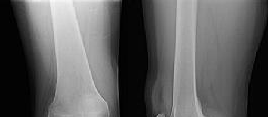
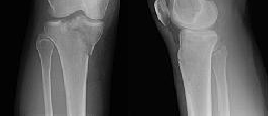
Figures 1 through 3 are the radiographs of a 25-year-old man who is brought to the emergency department after a motorcycle collision. He is complaining of isolated knee pain. Examination reveals swelling, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
Initial surgical management should consist of
---
---
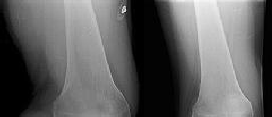
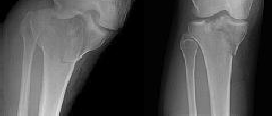
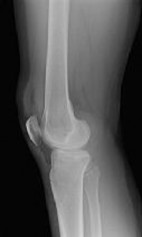
Figures 1 through 3 are the radiographs of a 25-year-old man who is brought to the emergency department after a motorcycle collision. He is complaining of isolated knee pain. Examination reveals swelling, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
Figures 4 through 8 are the axial and coronal CT scan sections of the injury. Intra-operative patient positioning for definitive fixation should be
---
---
---
---
---
---
---
---
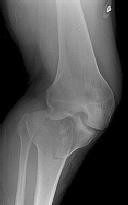
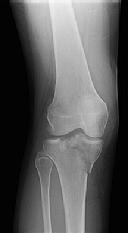
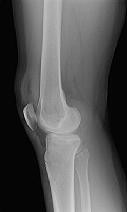
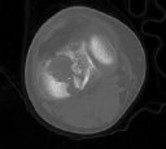
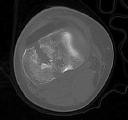
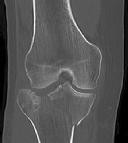
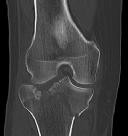
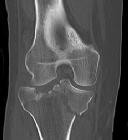
Figures 1 through 3 are the radiographs of a 25-year-old man who is brought to the emergency department after a motorcycle collision. He is complaining of isolated knee pain. Examination reveals swelling, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
The surgical approach for definitive reduction and stabilization of this pattern is
---
---
---
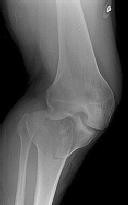
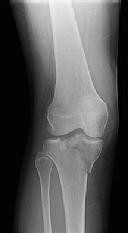
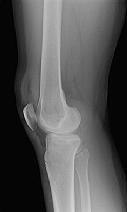
Figure 1 is the radiograph taken 6 weeks ago of a 41-year-old woman with persistent pain in her right leg after sustaining a tibia fracture 12 months ago in a motor vehicle collision. On examination, she has well-healed scars and a well-healed flap on the medial aspect at the level of the fracture. She reports having an infection after the initial surgery, which resulted in debridement of the soft tissue and need for the local rotational flap. There are no changes at the fracture site as shown in the most recent radiograph (Figure 2). She is healthy and has no comorbidities.
What is the best next step in the patient’s evaluation?
---




Figure 1 is the radiograph taken 6 weeks ago of a 41-year-old woman with persistent pain in her right leg after sustaining a tibia fracture 12 months ago in a motor vehicle collision. On examination, she has well-healed scars and a well-healed flap on the medial aspect at the level of the fracture. She reports having an infection after the initial surgery, which resulted in debridement of the soft tissue and need for the local rotational flap. There are no changes at the fracture site as shown in the most recent radiograph (Figure 2). She is healthy and has no comorbidities.
Based on the radiographs shown in Figures 1 and 2, her tibia is a
---
---
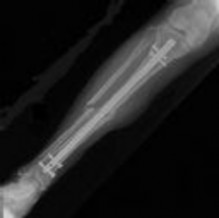
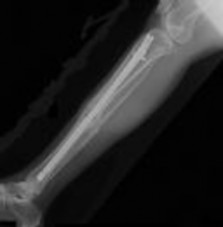
infrapatellar nailing is associated with
Figure 1 is the radiograph taken 6 weeks ago of a 41-year-old woman with persistent pain in her right leg after sustaining a tibia fracture 12 months ago in a motor vehicle collision. On examination, she has well-healed scars and a well-healed flap on the medial aspect at the level of the fracture. She reports having an infection after the initial surgery, which resulted in debridement of the soft tissue and need for the local rotational flap. There are no changes at the fracture site as shown in the most recent radiograph (Figure 2). She is healthy and has no comorbidities.
Assuming her workup is negative for any other causes, what is the best treatment option?
---


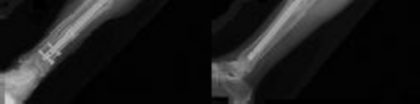
---

show
Commented [1]:
an external fixator. Deep cultures are most likely to pathogens found in
---
---
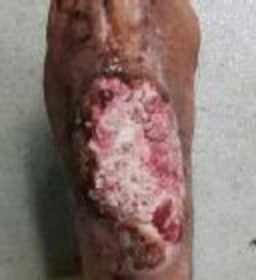


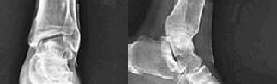
Figure 1 is the radiograph of a 67-year-old woman who is involved in a motor vehicle collision and sustains an isolated injury to her left hip. She is a community ambulatory who does not use any assistive devices.
She undergoes a closed reduction in the emergency department. Figures 2 through 5 are post-reduction CT images. What is the ideal surgical approach to address this fracture?
---
---
---
---
---
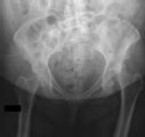
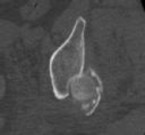
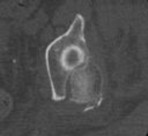
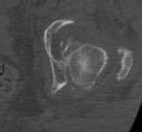
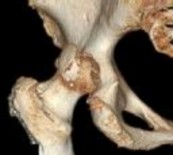
Figure 1 is the radiograph of a 67-year-old woman who is involved in a motor vehicle collision and sustains an isolated injury to her left hip. She is a community ambulatory who does not use any assistive devices.
Which factors will lead a surgeon to pursue fracture fixation and acute total hip arthroplasty instead of fixation alone?
---
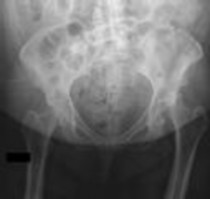
Figure 1 is the radiograph of a 67-year-old woman who is involved in a motor vehicle collision and sustains an isolated injury to her left hip. She is a community ambulatory who does not use any assistive devices.
In this patient, what other potential injury can be associated with this fracture pattern and is commonly overlooked?
---
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding orthopedic-mcqs-trauma-0018
