Comprehensive Surgical Management of Upper Extremity Nonunions: Humeral Condyle and Forearm Reconstruction
Key Takeaway
The surgical management of upper extremity nonunions requires meticulous preoperative planning, rigid internal fixation, and biological augmentation. This guide details the operative techniques for humeral condyle and forearm nonunions, emphasizing the restoration of the radial bow, the management of segmental bone defects using autogenous grafting, and the critical "fish-scaling" technique to stimulate osteogenesis while preventing iatrogenic radioulnar synostosis.
INTRODUCTION TO UPPER EXTREMITY NONUNIONS
The treatment of nonunions in the upper extremity presents a formidable challenge to the orthopedic surgeon. Unlike the lower extremity, where weight-bearing forces can be harnessed to promote osteogenesis through dynamization, the upper extremity relies heavily on complex, multi-planar motion—particularly pronation and supination of the forearm and the hinge-pivot mechanics of the elbow. Successful management dictates a dual approach: the restoration of absolute mechanical stability and the optimization of the biological environment.
This comprehensive guide delineates the advanced surgical protocols for managing nonunions of the humeral condyle, the diaphyseal radius and ulna, and periarticular fractures of the distal radius and proximal ulna.
OPEN REDUCTION INTERNAL FIXATION WITH BONE GRAFTING OF THE HUMERAL CONDYLE
Nonunions of the humeral condyle (lateral or medial) severely compromise elbow kinematics, leading to progressive valgus or varus instability, tardy ulnar nerve palsy, and debilitating pain. Surgical intervention is indicated to restore the articular congruity, re-establish the anatomic mechanical axis, and provide a stable fulcrum for elbow motion.
Preoperative Planning and Positioning
Patients should be evaluated with orthogonal radiographs and a fine-cut computed tomography (CT) scan to assess the size of the condylar fragment, the extent of articular cartilage loss, and the degree of metaphyseal bone resorption.
* Positioning: The patient is placed in the lateral decubitus or supine position with the arm draped over a radiolucent arm board. A sterile tourniquet is applied high on the brachium.
Surgical Approach and Technique
- Incision and Dissection: Begin the incision laterally over the distal third of the humerus. Extend it approximately 10 cm distally, terminating just proximal to the radial head. This utilizes the internervous plane between the triceps (radial nerve) and the brachialis (musculocutaneous nerve) proximally, and the anconeus (radial nerve) and extensor carpi ulnaris (posterior interosseous nerve) distally.
- Exposure of the Nonunion: Employ meticulous subperiosteal dissection to expose the anterior and posterior aspects of the nonunion site.
> Surgical Pearl: Free all surrounding adhesions and fibrotic soft tissues to mobilize the joint, but strictly preserve the muscular and ligamentous attachments to the lateral epicondyle (specifically the lateral collateral ligament complex and the common extensor origin) to prevent avascular necrosis of the condylar fragment. - Preparation of the Fragment: Remodel the large condylar fragment. Excise all intervening fibrous tissue and sclerotic bone until punctate bleeding (the "paprika sign") is observed, indicating a viable osteogenic bed.
- Reduction and Fixation: Freshen and anatomically appose the fracture surfaces. Provisionally hold the reduction with Kirschner wires. Fix the fragment to the distal humerus using two interfragmentary lag screws (typically 3.5 mm or 4.0 mm partially threaded cancellous screws). In cases of significant metaphyseal comminution, a contoured lateral column locking plate may be required to neutralize shear forces.
- Biological Augmentation: The debridement of sclerotic bone inevitably leaves a metaphyseal void. Fill the space proximal to the restored condyle with densely packed autologous cancellous bone graft harvested from the iliac crest.
- Ulnar Nerve Management: Evaluate the ulnar nerve. If the patient presents with preoperative persistent ulnar neuritis, or if the hardware placement/deformity correction places the nerve under tension, perform an anterior subcutaneous or submuscular transposition of the ulnar nerve through a separate medial incision.
Postoperative Protocol
The elbow is immobilized in a posterior plaster splint or a custom-molded abduction humeral splint at 90 degrees of flexion. To prevent debilitating elbow stiffness, passive and active-assisted range of motion (ROM) exercises are initiated at 6 weeks, contingent upon radiographic evidence of early bridging callus.
MANAGEMENT OF DIAPHYSEAL FOREARM NONUNIONS
The forearm must be conceptualized as a complex, articulated ring structure, analogous to the pelvis. The radius and ulna articulate at the proximal and distal radioulnar joints (PRUJ and DRUJ), tethered by the interosseous membrane. Any alteration in length, alignment, or the critical "radial bow" will exponentially restrict pronation and supination.
Biomechanical Imperatives
Re-creation of the radial bow is essential for a good functional outcome. A loss of the radial bow or an angular deformity exceeding 15 degrees will cause impingement of the radius against the ulna during rotation. Furthermore, length discrepancies between the two bones will alter the kinematics of the DRUJ, leading to ulnar impaction syndrome or DRUJ subluxation.
Surgical Warning: When using bone graft in the forearm, meticulous care must be taken to graft away from the opposing forearm bone and the interosseous membrane. Extravasation of bone graft into the interosseous space is a primary catalyst for iatrogenic radioulnar synostosis, a devastating complication that abolishes forearm rotation.
Nonunions Involving Both the Radius and Ulna
When bony defects are present in both bones, the surgical strategy depends on the size of the defect after thorough debridement of all sclerotic, devascularized bone. Best outcomes for malunions and nonunions are achieved when the corrective procedure is performed within 1 year of the index injury.
- Symmetrical Shortening: If the lengths of the bones can be equalized by resecting the sclerotic ends without causing excessive overall shortening of the forearm (typically < 2-3 cm), the fragments can be apposed directly. Rigid fixation with 3.5 mm dynamic compression plates (LC-DCP or LCP) combined with autogenous cancellous bone grafting is usually sufficient.
- Asymmetrical or Large Defects: When direct apposition would shorten the arm excessively, each bone must be treated independently.
- Segmental Defects: If one bone can be apposed but the other has a large gap, or if both have large gaps, structural bridging is required.
- Graft Options: The cancellous insert graft of Nicoll (utilizing blocks of iliac crest) is excellent for defects up to 4-5 cm. For massive segmental defects (>6 cm), free vascularized fibular grafts yield superior results.
- Infection History: If the nonunion is complicated by a history of osteomyelitis in one bone, the uninfected bone should be grafted and stabilized first. Grafting of the previously infected bone should be delayed for at least several weeks to ensure eradication of the pathogen.
Nonunions of the Radius or Ulna Alone
When one bone fails to unite and the other unites in an unsatisfactory position (malunion), enough bone is resected from the malunited segment to equalize the length of the bones, followed by standard plating and grafting.
However, if one bone is intact (either unfractured or united in perfect alignment) and the other has a nonunion with a defect, the intact bone must not be shortened to close the defect. Shortening a normal bone risks creating a second nonunion and alters DRUJ/PRUJ mechanics.
* Bridging the Defect: The defect in the nonunited bone must be bridged. Short defects can be managed with a bridge plate construct and packed with iliac crest cancellous bone. Larger defects require a structural Nicoll graft or a non-vascularized fibular strut graft.
* Intramedullary Fixation: While locked intramedullary forearm nails combined with Nicoll grafts have been described, debate continues regarding their rotational stability compared to dual-plate constructs, especially in the recalcitrant nonunion setting. Plating remains the gold standard.
Defect in One Bone with Overriding Fragments in the Other
In cases where one bone has a defect and the other has united with overriding fragments (shortening), the maximal length that can be restored is determined by the soft tissue envelope and neurovascular tension.
- Osteotomy and Traction: The united, overriding fragments are separated with an osteotome. Gentle, sustained longitudinal traction is applied.
- Equalization: The ends of the overriding fragments are cut to permit end-to-end apposition. The resected fragment can sometimes be utilized as an autograft if it is of sufficient length and biological quality to fit the defect in the opposite bone.
- Preparation of the Nonunion Bed: This is the most critical biological step. All sclerotic and devascularized tissue must be aggressively resected. The medullary canals, which are typically sealed with dense sclerotic caps, must be recannulated with a drill to restore endosteal blood flow.
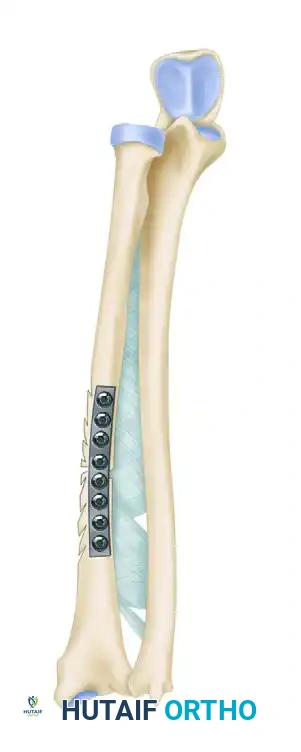
The "Fish-Scaling" Technique
To maximize the osteogenic potential of the host bone, the cortices adjacent to the fracture site are decorticated. This technique, known as "fish-scaling," involves using a sharp osteotome to raise small, overlapping osteoperiosteal flaps.

Clinical Pearl: As illustrated above, the cortices must be fish-scaled strictly on the side opposite the interosseous membrane. This exposes osteoprogenitor cells and creates a rich, bleeding bed for the applied bone graft, while deliberately avoiding osteogenic stimulation in the interosseous space, thereby mitigating the risk of synostosis.
MANAGEMENT OF PERIARTICULAR NONUNIONS
Nonunited Colles Fracture (Distal Radius)
Nonunions of the distal radius are relatively rare due to the rich metaphyseal blood supply, but when they occur, they are highly debilitating.
* Substantial Distal Fragment: If the distal fragment is large and possesses good bone stock, it can be managed similarly to a malunion: corrective osteotomy, structural bone grafting (to restore volar tilt and radial inclination), and rigid internal fixation with a volar locking plate.
* Osteoporotic/Small Distal Fragment: In elderly patients or those with severe osteopenia where the distal fragment is too small to accept screws, bone grafting combined with dorsal spanning plates or customized pin fixation is indicated. In cases of profound articular destruction or unsalvageable bone loss, a radiocarpal arthrodesis serves as a reliable salvage procedure to restore a painless, stable wrist.
Proximal End of the Ulna (Olecranon)
The treatment of olecranon nonunions depends on the location of the nonunion relative to the trochlear notch and the functional demands of the patient.
* Conservative Management: In middle-aged or elderly patients with a strong fibrous union and minimal pain, the functional disability may be slight, and surgical intervention may not be justified.
* Excision and Advancement: If the ununited proximal fragment constitutes less than 50% of the articular surface of the olecranon, it can be simply excised. The distal expansion of the triceps tendon is then advanced and securely reattached to the intact proximal ulna using heavy non-absorbable sutures through bone tunnels or suture anchors.
* ORIF: For fragments larger than 50%, or in high-demand patients, contoured posterior plating (using a pre-contoured olecranon locking plate) combined with autogenous bone grafting provides static compression and allows for early, aggressive elbow range of motion.
Distal End of the Ulna
Nonunions of the distal 3.5 cm of the ulna often result in DRUJ instability and ulnar-sided wrist pain.
* Fixation: They can be treated with a dedicated 3.5-mm or 2.7-mm distal ulna compression plate supplemented with cancellous bone grafting.
* Resection (Darrach Procedure): Alternatively, if the nonunion is highly comminuted or associated with severe DRUJ arthrosis, resection of the distal ulna (Darrach procedure) or a Suave-Kapandji procedure may be performed. Occasionally, a stable, asymptomatic nonunion of the distal third of the ulna results in insufficient disability to warrant any surgical intervention.
MASSIVE DEFECTS AND SALVAGE PROCEDURES
Defects in the radial head, radial neck, or the distal 5 cm of the ulna can often be treated by simple excision, as these fragments are relatively dispensable compared to the morbidity of complex grafting. However, excision of the radial head in the presence of interosseous membrane disruption (Essex-Lopresti lesion) is strictly contraindicated. In such instances, prosthetic radial head replacement is mandatory to restore radiocapitellar contact, eliminate the nonunion, and provide resistance against proximal migration of the radius.
The One-Bone Forearm
For massive, unsalvageable defects of the radial or ulnar shaft where segmental grafting has failed or is impossible, the creation of a one-bone forearm is a recognized salvage operation.
* Technique: Typically, the defect is in the ulna. The radius is osteotomized, and the distal end of the proximal ulnar fragment is internally fixed to the proximal end of the distal radial fragment.
* Outcome: While this operation completely abolishes pronation and supination, it restores longitudinal stability, improves the cosmetic appearance of the extremity, and provides a strong, stable lever arm for hand function.
Indications for Amputation
The decision to amputate an upper extremity is profound and must be made collaboratively with the patient, considering economic hardships, length of hospitalization, and psychological impact. The surgeon is likely to recommend amputation under the following strict circumstances:
1. When multiple exhaustive reconstructive efforts have definitively failed.
2. When a proposed plan of reconstruction is highly likely to result in a stiff, insensate, and painful limb that offers less satisfactory function than an amputation combined with a properly fitted modern prosthesis.
3. When the physiological danger of major, prolonged reconstructive operations to the life of the patient (e.g., severe systemic comorbidities, sepsis) outweighs the anticipated functional benefit.
4. When the damaged part (such as a severely contracted, insensate finger) cannot be restored and actively interferes with the function of the extremity as a whole.
5. When local tissue destruction is so absolute that reconstruction is anatomically impossible.
Following any amputation, it is imperative that the operating surgeon—or a specialized physiatrist—directly supervises the rehabilitation protocol and the fitting of the prosthesis to ensure optimal functional integration.
You Might Also Like