Psychoflexed and Psychoextended Hands: Diagnosis and Management
Key Takeaway
Psychoflexed and psychoextended hands represent complex psychogenic deformities requiring astute clinical differentiation from organic pathology. The psychoflexed hand typically involves severe, unyielding flexion of the ulnar three digits, often leading to palmar maceration. Conversely, the psychoextended hand presents with rigid proximal interphalangeal joint hyperextension. Recognizing paradoxical stiffness and avoiding unwarranted surgical intervention—such as Kirschner wire fixation or tendon releases—is paramount. Management relies primarily on multidisciplinary psychiatric care, specialized hand therapy, and behavioral modification techniques.
INTRODUCTION TO DYSFUNCTIONAL POSTURES OF THE HAND
The human hand is not only an organ of complex biomechanical function but also a profound instrument of psychological expression. In the realm of orthopedic surgery, encountering a patient with a severe, unyielding hand deformity in the absence of an identifiable organic etiology presents a formidable diagnostic and therapeutic challenge. These conditions, broadly categorized under psychogenic hand disorders, factitious disorders, or conversion disorders, manifest as dysfunctional postures that defy standard anatomical and neurological principles.
The most frequently encountered dysfunctional postures in clinical practice are the psychoflexed hand, the clenched fist syndrome, and the psychoextended hand. These conditions are characterized by rigid, non-anatomic posturing that often leads to secondary dermatological and infectious complications. For the practicing orthopedic surgeon, the primary objective is to accurately differentiate these psychogenic postures from true organic pathology (such as spasticity, ischemic contracture, or fibromatosis) and, crucially, to avoid the catastrophic pitfall of unwarranted surgical intervention.
Clinical Pearl: The hallmark of a psychogenic hand deformity is the presence of "paradoxical stiffness" and the complete resolution of the contracture under general anesthesia or regional block. Surgical intervention in these patients is strictly contraindicated and inevitably leads to recurrence, exacerbation of the deformity, or the development of new factitious symptoms.
THE PSYCHOFLEXED HAND
Clinical Presentation and Pathoanatomy
The psychoflexed hand, as classically described by Frykman, Wood, and Miller, is a profound dysfunctional posture characterized by severe, unyielding flexion contractures predominantly affecting the ulnar three digits (long, ring, and small fingers). The index finger and thumb are frequently spared, allowing the patient to maintain a rudimentary pinch mechanism for basic activities of daily living.
Unlike organic contractures, the psychoflexed posture is maintained by continuous, subconscious, or conscious active contraction of the flexor digitorum profundus (FDP) and flexor digitorum superficialis (FDS) muscles. Over time, this relentless posturing leads to severe secondary complications. The tightly clenched digits create a closed, moist environment in the palm, leading to profound palmar maceration.

The hygiene of the hand becomes severely compromised, often resulting in an offensive odor. Furthermore, the continuous pressure of the fingernails against the palmar skin can cause pressure necrosis, ulceration, and secondary bacterial or fungal infections. Notably, epidemiological data suggests there is no predilection for the minor or dominant hand, and the condition can present bilaterally.
Differential Diagnosis
An experienced hand surgeon must systematically rule out organic causes of digital flexion contractures before diagnosing a psychoflexed hand. The differential diagnosis includes:
- Dupuytren Contracture: Characterized by palpable palmar fascial cords and nodules. The contracture is fixed and does not resolve under anesthesia.
- Arthrogryposis Multiplex Congenita: A congenital condition presenting with multiple joint contractures, lacking the acute or subacute onset seen in psychogenic disorders.
- Spastic Hand Deformities: Secondary to upper motor neuron lesions (e.g., stroke, cerebral palsy, traumatic brain injury). Spasticity exhibits a "velocity-dependent catch" (clasp-knife phenomenon) and is often accompanied by hyperreflexia and other upper motor neuron signs.
- Volkmann Ischemic Contracture: Results from an untreated compartment syndrome, leading to muscle infarction and fibrotic replacement of the flexor pronator mass. It is associated with a history of trauma, ischemia, and a positive tenodesis effect.
THE CLENCHED FIST SYNDROME
Biomechanics and Paradoxical Stiffness
A variant of the psychoflexed hand is the clenched fist syndrome, extensively documented by Simmons and Vasile. In this presentation, the entire fist is tightly clenched, although the ulnar three digits often remain the most predominantly involved.
The diagnostic cornerstone for clenched fist syndrome is the demonstration of paradoxical stiffness. In a normal, organically intact upper extremity, the tenodesis effect dictates that passive flexion of the wrist causes passive extension of the digits due to tension on the extensor digitorum communis (EDC). Conversely, passive extension of the wrist causes digital flexion.
In clenched fist syndrome, this normal biomechanical relationship is abolished. When the examiner passively flexes the patient's wrist, the fingers remain rigidly flexed into the palm. This indicates that the patient is actively firing the flexor musculature to overpower the passive pull of the extensors—a physiological impossibility in a purely organic joint or tendon contracture.

Surgical Warning: The absence of the normal tenodesis effect during physical examination is highly sensitive for a psychogenic etiology. Do not proceed with tendon lengthening or joint capsulotomies in the presence of paradoxical stiffness.
Non-Operative Management Strategies
The management of clenched fist syndrome requires a delicate, multidisciplinary approach. Confronting the patient directly about the psychiatric nature of their deformity often leads to defensiveness, alienation, and a breakdown of the physician-patient relationship.
Spiegel and Chase reported successful outcomes using a combination of specialized hand therapy, exercises, and self-hypnosis. The core philosophy of this approach is to empower the patient. By emphasizing and enhancing the patient’s internal control over their disability—rather than aggressively questioning or challenging the underlying psychological cause—the patient is provided a "face-saving" avenue to relinquish the dysfunctional posture.
THE PSYCHOEXTENDED HAND
Clinical Presentation
The second major dysfunctional posture is the psychoextended hand. While less common than its flexed counterpart, it presents an equally perplexing clinical picture. The posture is characterized by rigid hyperextension at the proximal interphalangeal (PIP) joints and flexion at the metacarpophalangeal (MCP) joints, predominantly affecting the ulnar three digits.
This posture mimics an intrinsic-plus or severe swan-neck deformity but lacks the underlying structural pathology (such as volar plate laxity or intrinsic tightness) that typically causes these conditions.
Functional Implications and Biomechanics
Interestingly, the psychoextended hand often permits a partially functioning extremity. The pinch mechanism between the thumb and the index finger is usually preserved. The index finger MCP joint is held in flexion, but active flexion and extension are preserved at the PIP joint, allowing the index pulp to oppose the thumb. This selective sparing strongly points toward a psychogenic origin, as the patient subconsciously maintains enough function to perform basic tasks while sustaining the "sick role."
During examination, the surgeon may find that the patient permits passive extension at the MCP joint and passive flexion at the PIP joint. However, the moment the examiner releases the digits, the rigid psychoextended posture instantly recurs. Over time, persistent active stretching by the patient's own musculature can lead to profound, permanent hyperextension instability at the PIP joints.
The Futility of Surgical Intervention
A fascinating and challenging aspect of patients with psychoextended hands is their psychological affect. These patients are rarely distressed by their severe deformities (a phenomenon akin to la belle indifférence seen in conversion disorders) and rarely demand treatment to correct the posture.
However, if offered, they may readily permit surgery to be performed. The surgeon must exercise extreme restraint. The literature is replete with case reports of failed surgical interventions in these patients.
* Casting: Ineffective; the posture recurs immediately upon cast removal.
* Kirschner Wire Fixation: Pinning the joints in a functional position often leads to the patient actively bending or breaking the K-wires, or manipulating the pins to induce pin-tract infections and osteomyelitis.
* Amputation: Amputation of the fingertips or digits does not resolve the underlying psychiatric drive; the patient will simply adopt a new dysfunctional posture with the remaining digits or transfer the pathology to the contralateral limb.
Psychiatric management, cognitive behavioral therapy (CBT), and psychotropic medication (if an underlying mood or anxiety disorder is identified) must be the initial and primary treatments.
FACTITIOUS LESIONS AND SELF-MUTILATION
Beyond dysfunctional postures, orthopedic surgeons must be vigilant in recognizing factitious lesions of the hand. These are self-inflicted injuries driven by a psychological need to assume the sick role (Factitious Disorder/Munchausen Syndrome) or for secondary gain (Malingering).
Clinical Characteristics
Patients often present with chronic, non-healing wounds, unexplained edema (Secretan’s syndrome, caused by repetitive self-inflicted blunt trauma to the dorsum of the hand), or bizarre lesions that do not conform to typical dermatomal or traumatic patterns. The history provided is often vague, inconsistent, or attributed to "trivial trauma" that fails to explain the severity of the presentation.
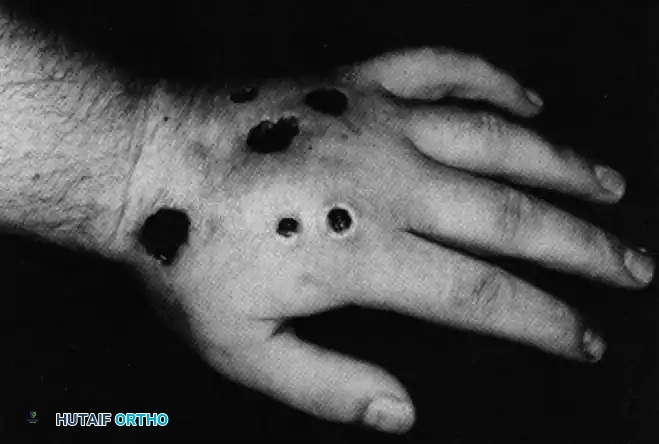
The "Cast Test" as a Diagnostic and Therapeutic Tool
A highly effective diagnostic and therapeutic modality for suspected factitious lesions is the application of a rigid, well-padded fiberglass cast that completely covers the lesions, preventing the patient from accessing them.
As demonstrated in the classic case reported by Louis DS (Fig. 67-16), lesions that are self-inflicted (such as cigarette burns or mechanically excoriated ulcers) will rapidly regress and heal under cast immobilization. However, upon removal of the cast, the lesions mysteriously reappear within days or weeks. This cycle of healing under protection and recurring upon exposure is pathognomonic for factitious trauma.
Clinical Pearl: When applying a diagnostic cast for suspected factitious lesions, ensure the cast extends sufficiently proximal and distal to prevent the patient from inserting objects (e.g., coat hangers, rulers) under the cast to continue the self-harm.
PROTOCOLS FOR CLINICAL EVALUATION AND MANAGEMENT
1. The Diagnostic Workup
When a psychogenic hand disorder is suspected, the diagnostic workup must be thorough to definitively exclude organic pathology, thereby protecting both the patient and the surgeon.
* Detailed History: Look for inconsistencies, a history of multiple unexplained medical issues, or recent severe psychosocial stressors.
* Electromyography and Nerve Conduction Studies (EMG/NCS): Typically normal in psychogenic postures, ruling out severe neuropathies or radiculopathies.
* The Anesthesia Examination: The gold standard for diagnosis. Under intravenous sedation (MAC) or general anesthesia, a psychogenic contracture will completely melt away, revealing full, unrestricted passive range of motion.
2. The Multidisciplinary Treatment Paradigm
Once the diagnosis is established, the orthopedic surgeon must transition from a surgical role to a coordinating role.
* Avoid Confrontation: Do not accuse the patient of "faking." Acknowledge their disability and validate that their hand is not functioning properly.
* Psychiatric Referral: Frame the referral carefully. Explain that the brain-nerve-muscle connection is "misfiring" due to stress, and that a specialist in this mind-body connection (a psychiatrist or psychologist) is required.
* Hand Therapy: Prescribe a regimen of gentle, active-assisted range of motion. The therapist should focus on positive reinforcement and biofeedback. Splinting can be attempted but is often sabotaged by the patient.
* Strict Surgical Avoidance: Document clearly in the medical record that the deformity is non-organic and that surgical intervention (releases, fusions, amputations) is absolutely contraindicated, as it carries a near 100% failure rate and high risk of iatrogenic harm.
CONCLUSION
Psychoflexed hands, psychoextended hands, and clenched fist syndromes are profound manifestations of psychological distress expressed through the musculoskeletal system. The orthopedic surgeon's role is paramount in recognizing the subtle biomechanical inconsistencies—such as paradoxical stiffness and the preservation of selective pinch mechanisms—that differentiate these conditions from organic disease. By employing diagnostic tools like the cast test and the anesthesia examination, and by strictly adhering to a non-operative, multidisciplinary management strategy, the surgeon can protect the patient from the devastating consequences of unwarranted surgical intervention while guiding them toward appropriate psychiatric and rehabilitative care.
You Might Also Like

