Factitious Hand Syndromes: Comprehensive Diagnosis and Management
Key Takeaway
Factitious hand syndromes present a complex diagnostic challenge for orthopedic surgeons. Characterized by self-inflicted injuries, prolonged edema, or unexplained deformities, these conditions require a high index of suspicion. Management relies on ruling out organic pathology, utilizing diagnostic casting to confirm self-mutilation, and integrating psychiatric care. This guide details the clinical evaluation, Grunert’s classification, and the strategic use of immobilization to differentiate factitious disorders from true organic disease.
INTRODUCTION TO FACTITIOUS HAND SYNDROMES
Factitious hand syndromes encompass a broad and perplexing spectrum of self-induced upper extremity pathologies. These conditions—ranging from factitious lymphedema and Secretan syndrome to self-mutilation, subcutaneous emphysema, and pachydermodactyly—are encountered by physicians across all specialties but are frequently referred to the orthopedic hand surgeon due to their complex, non-healing, or structurally destructive presentations.
Unlike malingering, where the patient is motivated by secondary gain (e.g., financial compensation, avoidance of work), patients with factitious disorders are driven by a primary psychological need to assume the "sick role." This distinction is critical, as the management paradigm shifts from purely structural orthopedic reconstruction to a delicate balance of diagnostic exclusion, complication management, and psychiatric integration.
The orthopedic surgeon must maintain a high index of suspicion. A careful, exhaustive history and physical examination are paramount to recognizing the warning signs of a patient who may be actively causing or perpetuating their presenting illness. Failure to identify a factitious etiology often leads to a cascade of unnecessary, invasive, and potentially iatrogenic diagnostic procedures and surgeries.
Clinical Pearl: Self-induced injury should be highly suspected when there is a history of prolonged, intractable edema, a profound lack of wound healing despite optimal care, or a bizarre deformity without a plausible biomechanical or organic explanation.
PATHOPHYSIOLOGY AND PSYCHOLOGICAL CLASSIFICATION
Understanding the psychological underpinnings of factitious hand syndromes is essential for the orthopedic surgeon, as it directly dictates the success or failure of any physical intervention.
The Grunert Classification
Grunert et al. provided a foundational framework by identifying three distinct types of factitious hand syndromes based on their physical presentation:
- Self-Mutilation and Wound Manipulation: Patients actively destroy tissue, often reopening surgical incisions, injecting foreign substances (e.g., feces, saliva, air), or inflicting thermal/chemical burns.
- Edema: Patients induce swelling, typically through the covert application of proximal tourniquets (e.g., rubber bands, tight strings) that obstruct venous and lymphatic return while preserving arterial inflow.
- Finger and Hand Deformities: Patients present with rigid contractures, clenched fist syndromes, or bizarre posturing that does not conform to known anatomical nerve distributions or musculotendinous pathology.
Psychological Profiles and Prognosis
These physical presentations are typically rooted in two distinct psychological diagnoses: factitious disorder with physical symptoms and conversion disorder.
Utilizing the Minnesota Multiphasic Personality Inventory (MMPI), researchers have identified two primary personality profiles that directly correlate with treatment outcomes:
* The Emotionally Dependent Group: These patients often present with edema or conversion-type deformities. They generally exhibit a more favorable response to behavioral treatment, non-confrontational counseling, and multidisciplinary rehabilitation.
* The Angry, Hostile, and Self-Mutilating Group: These patients frequently present with severe wound manipulation or amputations. They possess the poorest prognosis, are highly resistant to psychiatric intervention, and are at the highest risk for severe iatrogenic complications if the surgeon attempts complex reconstructive procedures.
CLINICAL PHENOTYPES AND PRESENTATIONS
Secretan Syndrome and Factitious Lymphedema
Originally described by Secretan in 1901 as "hard edema" of the dorsum of the hand, this condition is now widely recognized in many cases as a factitious disorder. It is characterized by peritendinous fibrosis and brawny edema over the dorsal metacarpals, typically induced by repetitive, self-inflicted blunt trauma or the covert use of a proximal tourniquet. The edema is often non-pitting and fails to resolve with standard elevation or compression therapy.
Factitious Ulcerations and Wound Manipulation
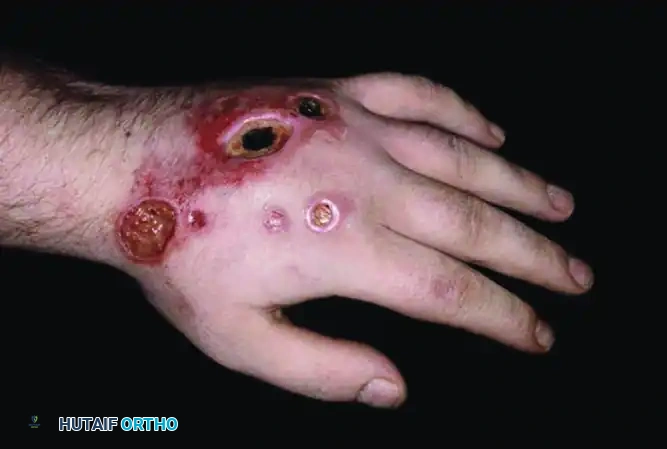
Patients may present with chronic, non-healing ulcers that possess geometric, unnatural borders. These lesions are often the result of chemical applications, repetitive excoriation, or thermal injuries (such as cigarette burns).

FIGURE 70-16 A: A 22-year-old man who developed severe, geometrically distinct lesions that would not heal after trivial trauma at work. The unnatural, punched-out appearance of these wounds is highly suspicious for self-inflicted thermal injury (presumed cigarette burns).
Pachydermodactyly
This is a rare, benign, superficial fibromatosis characterized by asymptomatic soft tissue swelling of the lateral aspects of the proximal interphalangeal (PIP) joints. It is predominantly seen in young males and is caused by repetitive, obsessive-compulsive rubbing or interlacing of the fingers.
Subcutaneous Emphysema
A sudden onset of swelling with palpable crepitus in the absence of a penetrating trauma or necrotizing infection should raise suspicion for factitious subcutaneous emphysema. This is typically achieved by the patient injecting air into the subcutaneous tissues using a hypodermic needle.
DIAGNOSTIC EVALUATION AND RED FLAGS
The diagnosis of a factitious hand syndrome is primarily one of exclusion, but it must be considered early in the differential to prevent unnecessary surgical morbidity.
History and Physical Examination
Further suspicion should be aroused when the patient provides a history of having seen several competent physicians who were unable to establish an organic diagnosis despite multiple diagnostic procedures (the "wandering patient" or Munchausen syndrome).
Key Red Flags Include:
* Wounds that heal normally under unremovable dressings but break down immediately upon exposure.
* Anesthesia or paralysis that does not follow dermatomal or peripheral nerve distributions.
* "La belle indifférence"—a paradoxical lack of concern regarding the severity of their condition.
* Symptoms that exclusively occur when the patient is unobserved.
* A history of extensive medical knowledge or a background in healthcare.
Surgical Warning: Never proceed with complex reconstructive surgery (e.g., free tissue transfer, tendon grafting) in a patient with a suspected factitious disorder. The patient will likely sabotage the reconstruction, leading to catastrophic flap failure or deep space infection.
THE DIAGNOSTIC CASTING PROTOCOL
When a factitious etiology is suspected—particularly in cases of prolonged edema, non-healing wounds, or unexplained contractures—diagnostic casting is the gold standard orthopedic intervention.
Casting the edematous part or wound serves a dual purpose: it acts as a rigid barrier preventing the patient from manipulating the tissues, and it provides a controlled environment to observe the natural physiological healing process.
Indications for Diagnostic Casting
- Unexplained, chronic dorsal hand edema (suspected Secretan syndrome or tourniquet application).
- Non-healing ulcers or wounds with negative cultures and normal vascular studies.
- Suspected clenched-fist syndrome or conversion disorder deformities.
Step-by-Step Casting Technique
- Wound Preparation: If open lesions are present, perform a gentle bedside debridement of necrotic tissue. Apply a non-adherent, antimicrobial dressing (e.g., Xeroform or silver-impregnated gauze).
- Positioning: The hand should be placed in the intrinsic-plus (safe) position to prevent collateral ligament contracture. The wrist is extended 20-30 degrees, metacarpophalangeal (MCP) joints flexed 70-90 degrees, and interphalangeal (IP) joints fully extended.
- Padding: Apply generous cast padding, particularly over bony prominences (ulnar styloid, radial styloid, metacarpal heads) to prevent iatrogenic pressure sores, as these patients may intentionally apply pressure to the cast to create new wounds.
- Application of Rigid Material: Fiberglass is preferred over plaster due to its durability and resistance to patient manipulation. The cast must extend proximal to the elbow (long-arm cast) if a covert tourniquet is suspected, ensuring the patient cannot apply a constricting band proximal to the cast.
- Tamper-Evident Measures: This is a critical step. The surgeon should draw a continuous line across the cast with a permanent marker, or apply a specific, unique tape pattern. If the patient bivalves or removes the cast and attempts to replace it, the lines will not align, confirming manipulation.
Interpretation of Results
The cast must be worn long enough for a wound to heal or for edema to resolve (typically 2 to 3 weeks).
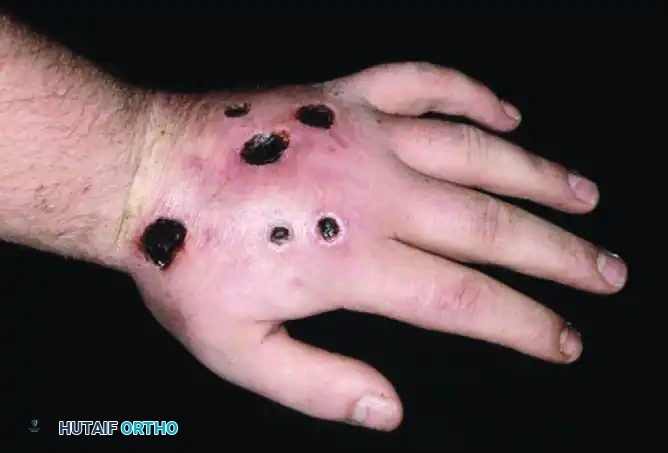
FIGURE 70-16 B: The same 22-year-old man from Figure A. The lesions demonstrated significant regression and healing under strict cast immobilization. However, the wounds reappeared shortly after cast removal, confirming the diagnosis of a factitious disorder.
If the edema resolves or the wound heals completely within the cast, but reappears shortly after cast removal, the diagnosis of a factitious disorder is definitively established.
SURGICAL MANAGEMENT OF COMPLICATIONS
While the primary treatment for factitious disorders is psychiatric, the orthopedic surgeon is frequently required to manage the severe, organic complications that arise from self-mutilation. Patients may inject toxic substances (e.g., paint thinner, feces, saliva) into the tendon sheaths or joint spaces, necessitating emergent surgical intervention.
Indications for Operative Intervention
- Septic Arthritis or Purulent Tenosynovitis: Secondary to self-injection.
- Compartment Syndrome: Secondary to massive fluid injection or severe, prolonged tourniquet application.
- Necrotizing Soft Tissue Infections: Requiring radical debridement.
Surgical Approach and Debridement
- Incision and Drainage: Utilize standard, extensile surgical approaches (e.g., Brunner incisions for volar digits, dorsal longitudinal incisions for metacarpals).
- Radical Debridement: All necrotic skin, subcutaneous tissue, and devitalized fascia must be excised. In cases of foreign substance injection, copious pulsatile lavage is required.
- Tissue Cultures: Obtain deep tissue cultures for aerobic, anaerobic, fungal, and mycobacterial organisms. Factitious infections often yield polymicrobial or atypical organisms (e.g., Eikenella corrodens from human saliva, enteric flora from feces).
- Wound Management: Leave the wound open. Utilize negative pressure wound therapy (NPWT) if the patient can be monitored to ensure they do not tamper with the device. Otherwise, apply a bulky, rigid, tamper-proof dressing.
- Definitive Coverage: Avoid complex flaps. Opt for healing by secondary intention or simple split-thickness skin grafting once the wound bed is clean and the patient is under strict psychiatric observation.
Pitfall: Attempting a pedicled groin flap or free tissue transfer in a patient with an active, unmanaged factitious disorder will almost certainly result in the patient avulsing the flap or injecting the pedicle, leading to catastrophic failure and further loss of limb function.
POSTOPERATIVE PROTOCOL AND MULTIDISCIPLINARY CARE
The management of factitious hand syndromes extends far beyond the operating room. A coordinated, multidisciplinary approach involving orthopedic surgery, psychiatry, psychology, and specialized hand therapy is mandatory.
The Confrontation Dilemma
Once the diagnosis is confirmed (e.g., via diagnostic casting), the medical team must decide how to address the patient.
* Direct Confrontation: Historically, directly accusing the patient of self-harm leads to anger, denial, and the patient abruptly leaving against medical advice (AMA) to seek care from another unsuspecting surgeon.
* Non-Confrontational Approach: The currently favored, evidence-based approach involves presenting the diagnosis as a "stress-related condition." The surgeon might say, "The cast proved that your body has the remarkable ability to heal when protected. However, it seems that stress or subconscious habits are causing the wounds to return when the cast is off. We are going to involve a stress-management specialist (psychiatrist) to help your body continue to heal."
Rehabilitation and Hand Therapy
Hand therapy must be carefully prescribed. Therapists should focus on objective, measurable goals (e.g., passive range of motion, grip strength via Jamar dynamometer). Therapists serve as the "eyes and ears" of the surgical team, often being the first to notice inconsistencies in the patient's presentation or signs of recurrent self-mutilation.
Long-Term Outcomes
The prognosis for factitious hand syndromes remains guarded. While the emotionally dependent cohort may achieve remission with intensive psychotherapy and behavioral modification, the hostile/self-mutilating cohort frequently progresses to severe, irreversible disability, including self-induced amputations. The orthopedic surgeon's primary goal is to "do no harm"—avoiding iatrogenic injury, managing acute infectious complications, and gently guiding the patient toward the psychiatric care they fundamentally require.
You Might Also Like