Orthopaedic Management of Epidermolysis Bullosa and Associated Hand Lesions
Key Takeaway
Epidermolysis bullosa (EB) presents profound challenges in hand surgery, primarily due to recurrent blistering, pseudosyndactyly, and flexion contractures. Surgical intervention focuses on repetitive degloving and contracture release to maintain functional prehension. Due to the high risk of recurrence and chronic infection, operative management must be meticulously timed, often delayed until subperiosteal bone maturation, and followed by rigorous, prolonged postoperative splinting to maximize functional longevity.
Introduction to Epidermolysis Bullosa in Orthopaedics
Epidermolysis bullosa (EB) encompasses a group of rare, inherited mechanobullous disorders characterized by extreme skin and mucosal fragility. The severe dystrophic form of epidermolysis bullosa (Recessive Dystrophic Epidermolysis Bullosa, or RDEB) is a profound hereditary disorder occurring in approximately one of every 300,000 births. It is caused by mutations in the COL7A1 gene, leading to a defect in type VII collagen, the primary component of anchoring fibrils at the dermoepidermal junction.
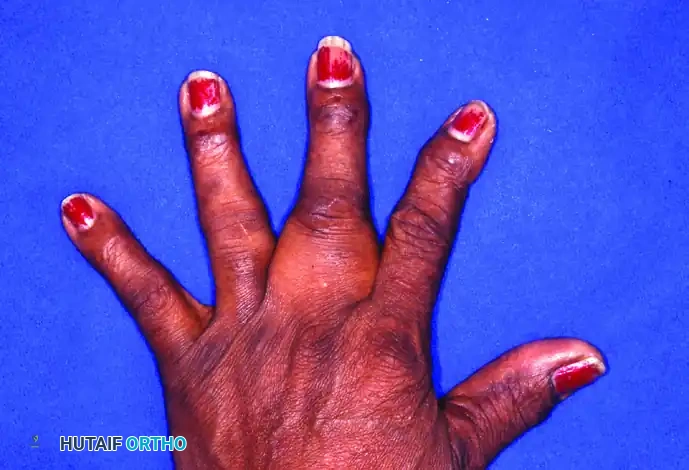
For the orthopaedic hand surgeon, EB presents a formidable reconstructive challenge. The disease process affects the entire dermis and frequently involves the mucous membranes. At birth or shortly thereafter, minor mechanical trauma induces the formation of widespread bullae over the extremities. The ultimate, devastating course of the disease in the upper extremity is characterized by chronic infection of these bullae, relentless scarring, and the continuing formation of a cocoon-like epidermis over all the fingers of each hand, resulting in severe pseudosyndactyly (the "mitten hand" deformity) and profound flexion contractures.
Clinical Pearl: Patients with severe dystrophic EB are exceptionally poor surgical risks. Chronic infection, severe malnutrition, anemia, and a reported mortality rate of up to 25% during childhood or adolescence (often due to debilitation, sepsis, or aggressive squamous cell carcinoma) mandate a highly cautious, multidisciplinary approach to surgical intervention.
Pathomechanics and Associated Lesions
The orthopaedic manifestations of EB extend beyond soft-tissue syndactyly, profoundly affecting the osseous and tendinous structures of the hand.
Subperiosteal Hemorrhage and Turret Exostosis
The extreme fragility of the tissues means that even minor trauma can cause subperiosteal hemorrhage. Over time, this hemorrhage eventually ossifies. Clinically, this presents as a firm, palpable mass developing on the dorsum of the phalanx.
This heterotopic ossification, often referred to as a turret exostosis, acts as a mechanical block. It severely limits the excursion of the extensor apparatus, directly limiting the flexion of the interphalangeal (IP) joints distal to the lesion. The extensor mechanism becomes tethered to the underlying new bone, destroying the delicate balance of the digital sweep and contributing to fixed contractures.

FIGURE 77-35 Turret exostosis. Note the dome-shaped osseous prominence on the dorsal aspect of the phalanx, which mechanically impedes the extensor hood.
Calcinosis Circumscripta
In addition to subperiosteal ossification, patients with chronic blistering disorders may develop calcinosis circumscripta—localized deposits of calcium salts within the dermal and subcutaneous tissues. In the hand, these deposits frequently occur around the fingertips and the thumb, exacerbating pain, limiting mobility, and serving as a nidus for recurrent ulceration and chronic infection.
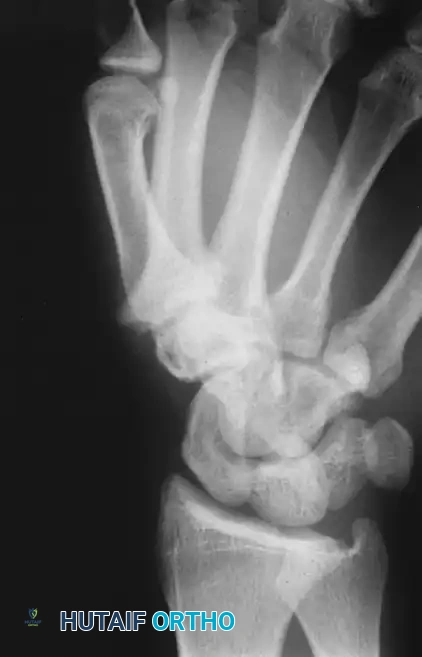
FIGURE 77-34 Calcinosis circumscripta of thumb. (Courtesy of E.C. Wieckesser, MD.)
Radiographic Evaluation
Early radiographic evaluation of the EB hand can be deceptive. Radiographs taken during the first few weeks after an acute injury or blistering episode typically reveal negative results regarding osseous changes.
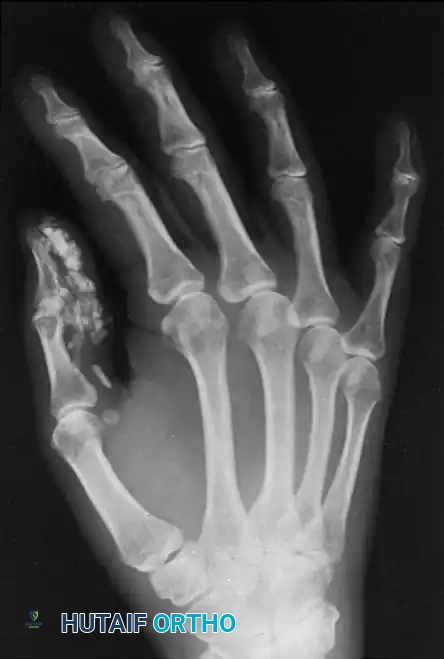
However, serial imaging later reveals subperiosteal new bone located on the dorsum of the phalanx, confirming the ossification of the preceding subperiosteal hemorrhage. Advanced imaging may also demonstrate severe osteopenia (due to disuse and nutritional deficits), joint subluxations, and the presence of calcific deposits or carpometacarpal bossing.
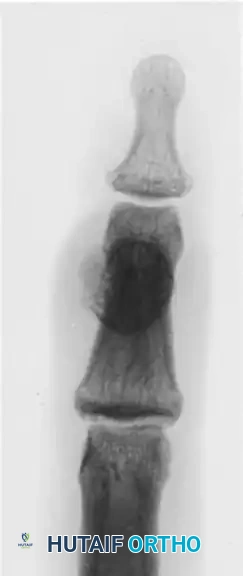
Radiographic demonstration of advanced osseous changes and joint contractures typical in severe mechanobullous disorders.
Indications and Timing for Surgery
Conservative treatment for the osseous and severe contracture manifestations of EB has historically not been beneficial. However, surgical intervention must be meticulously timed.
Timing of Osseous Resection:
Any indicated surgery to address a turret exostosis or subperiosteal ossification must be delayed until the subperiosteal bone becomes fully mature. This maturation process usually takes 4 to 6 months after the initial injury or hemorrhagic event. Operating prematurely on immature heterotopic bone carries an unacceptably high risk of explosive recurrence. Once the bone is mature, recurrence is significantly less likely.
Indications for Soft Tissue Release:
Surgical release of the cocooned digits is indicated when the patient loses functional prehension (the ability to grasp objects or feed themselves). However, surgeons must counsel patients and families that surgical release of these digits is often discouraging because the recurrence of the webbing and flexion contractures of the fingers is rapid and inevitable. Surgical procedures in EB are fundamentally repetitious degloving procedures designed to provide limited hand function over a limited time.
Surgical Warning: The goal of surgery in EB is not the restoration of normal anatomy, but rather the temporary restoration of functional prehension. Over-aggressive correction of joint contractures can lead to neurovascular compromise or catastrophic skin loss.
Preoperative Optimization
Operating on an EB patient requires a highly specialized, multidisciplinary approach:
* Anesthesia: Endotracheal intubation is hazardous due to mucosal fragility; bullae can form in the oropharynx and trachea, leading to life-threatening airway obstruction. Regional anesthesia (axillary or supraclavicular block) is strongly preferred.
* Skin Protection: Absolutely no adhesive tape can be used anywhere on the patient's body. Blood pressure cuffs and tourniquets must be heavily padded with soft cotton (Webril) to prevent shearing forces.
* Infection Control: Chronic colonization with Staphylococcus aureus and Pseudomonas aeruginosa is ubiquitous. Preoperative cultures of open wounds and targeted prophylactic intravenous antibiotics are mandatory.
Surgical Technique: Degloving Release and Pseudosyndactyly Reconstruction
The primary surgical intervention for the "mitten hand" is a radical degloving and release of the pseudosyndactyly.
1. Positioning and Preparation
The patient is placed supine with the arm extended on a hand table. A pneumatic tourniquet is applied over multiple layers of soft cast padding. Skin preparation is performed with gentle pouring or dabbing of chlorhexidine or povidone-iodine; aggressive scrubbing is strictly contraindicated.
2. Incision and Degloving
- A longitudinal incision is made along the fused dorsal and volar aspects of the pseudosyndactyly.
- The cocoon-like epidermis is carefully incised. Because this is a pseudosyndactyly (fusion of the skin, not the underlying native web spaces), blunt dissection with a blunt-tipped scissors or a mosquito hemostat can often separate the digits along the avascular scar planes.
- The dissection must remain superficial to the neurovascular bundles, which are typically displaced volarly by the severe flexion contractures.
3. Contracture Release
- Once the digits are separated, the severe proximal interphalangeal (PIP) and distal interphalangeal (DIP) joint flexion contractures must be addressed.
- Release of the volar skin is often insufficient. Stepwise release of the volar plate and, if necessary, excision of the accessory collateral ligaments may be required.
- Caution: Do not attempt to force the joints into full extension if there is resistance, as this will stretch and potentially rupture the contracted neurovascular bundles.
4. Skeletal Stabilization
- Because the soft tissues have a relentless tendency to contract, the digits must be stabilized in maximum safe extension.
- Longitudinal Kirschner wires (K-wires) (typically 0.035 or 0.045 inch) are driven retrograde through the distal phalanx, across the DIP and PIP joints, and into the metacarpal to maintain extension.
5. Soft Tissue Coverage
- Free skin grafts (split-thickness or full-thickness) and distant flaps have been used historically, but as the literature notes, they offer only limited advantage. The donor sites for grafts often become new sites of chronic blistering and scarring.
- Many modern centers prefer to allow the surgically created web spaces and volar defects to heal by secondary intention, utilizing advanced biologic dressings, cultured epidermal autografts, or acellular dermal matrices.
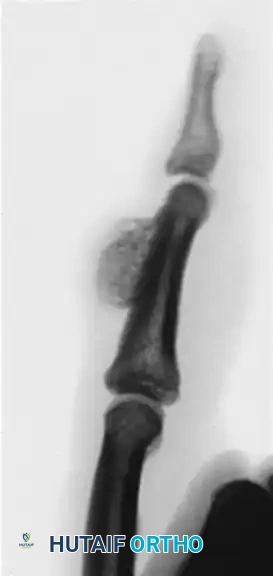
Surgical planning and radiographic assessment are critical prior to undertaking complex degloving and osseous resections in the EB hand.
Surgical Technique: Excision of Turret Exostosis
When a mature subperiosteal ossification (turret exostosis) is mechanically blocking extensor excursion, surgical excision is indicated.
- Approach: A dorsal longitudinal or gently curved incision is made over the affected phalanx, taking extreme care with the fragile skin.
- Extensor Mechanism Mobilization: The extensor tendon is frequently adherent to the exostosis. A meticulous tenolysis is performed to elevate the extensor hood off the bony mass.
- Excision: The mature exostosis is excised flush with the native cortex of the phalanx using a sharp osteotome or a high-speed burr under continuous saline irrigation.
- Barrier Interposition: To prevent readherence of the extensor tendon to the raw bony bed, a small flap of local adipose tissue or a synthetic barrier membrane may be interposed.
- Closure: The skin is closed with fine, non-absorbable sutures (e.g., 5-0 or 6-0 nylon) using a tension-free technique.
Postoperative Protocol and Rehabilitation
The postoperative management of the EB hand is arguably more critical than the surgery itself. The less severe types of the disease may not need extensive surgical treatment, but splinting after any degloving or minor release is universally required.
Immediate Postoperative Care
- Dressings: Wounds are covered with non-adherent, silicone-based contact layers (e.g., Mepitel). Petroleum-impregnated gauze can also be used. The hand is wrapped in bulky, soft dressings to absorb exudate and protect against shear.
- Immobilization: The hand is immobilized in a bulky dressing with a volar resting splint. The K-wires remain in place for 3 to 4 weeks to allow the soft tissues to heal in an extended position.
Long-Term Rehabilitation
- Splinting: Once the K-wires are removed, the patient must be transitioned to custom-fabricated, well-padded thermoplastic splints. Night splinting is mandatory and indefinite. Failure to maintain a rigorous night splinting regimen will result in rapid recurrence of the pseudosyndactyly and flexion contractures.
- Web Space Maintenance: Silicone web spacers or specialized gloves are utilized during the day to delay the proximal migration of the web spaces.
- Wound Care: Ongoing, meticulous wound care is required to manage chronic ulcerations and prevent secondary bacterial infections.
Complications and Prognosis
The orthopaedic surgeon must approach Epidermolysis Bullosa with a clear understanding of the disease's grim prognosis and high complication rates.
- Recurrence: Recurrence of the pseudosyndactyly is the rule, not the exception. Surgery is a palliative measure to buy time and function. Repetitious degloving procedures will be necessary throughout the patient's life.
- Infection: Chronic open wounds make these patients highly susceptible to osteomyelitis and systemic sepsis.
- Malignant Transformation: Chronic, non-healing wounds in EB patients have a remarkably high rate of malignant transformation into aggressive Squamous Cell Carcinoma (Marjolin's ulcer). Any suspicious, hypergranulating, or rapidly changing lesion must be biopsied immediately. Amputation is frequently required for definitive oncologic control in these cases.
- Mortality: As noted, the systemic burden of severe RDEB carries a death rate of up to 25% during childhood or adolescence due to profound debilitation, malnutrition, and sepsis.
In conclusion, the orthopaedic management of Epidermolysis Bullosa requires a delicate balance between aggressive surgical release to maintain hand function and meticulous, tissue-sparing techniques to prevent catastrophic complications. Success is measured not by permanent anatomical correction, but by the maximization of the patient's functional independence and quality of life over time.
You Might Also Like