Operative Management of Hand Tumors and Ganglion Cysts
Key Takeaway
Ganglion cysts are the most common focal hand masses, typically arising from the scapholunate interosseous ligament. While conservative management includes aspiration, surgical excision remains the gold standard for definitive treatment. This guide details the step-by-step surgical technique for dorsal wrist ganglion excision, emphasizing capsular margin removal and preservation of the scapholunate ligament to minimize recurrence and optimize postoperative wrist biomechanics.
MALIGNANT TUMORS OF THE HAND
Primary malignant tumors of the hand are exceedingly rare, yet they demand a high index of suspicion, rigorous diagnostic workup, and aggressive multidisciplinary management. Unlike benign tumorous conditions, malignancies in the upper extremity carry a significant risk of morbidity, limb loss, and mortality.
Rhabdomyosarcoma
Rhabdomyosarcoma is a highly aggressive malignant mesenchymal tumor exhibiting skeletal muscle differentiation. While it is the most common soft tissue sarcoma in childhood, its presentation in the hand and upper extremity is exceptionally rare. Historically, most reported cases of rhabdomyosarcoma in the hand have been fatal, standing in stark contrast to the relatively better prognoses of other primary bone or soft tissue tumors in the upper extremity. The tumor typically presents as a rapidly enlarging, firm, and often painless mass. Early hematogenous spread to the lungs and lymphatic dissemination are common, necessitating aggressive neoadjuvant chemotherapy, wide oncologic surgical resection, and adjuvant radiation therapy.
Ewing Sarcoma
Ewing sarcoma of the hand is another rare but highly aggressive malignancy, typically affecting children and young adults. Radiographically, it is characterized by a permeative pattern of bone destruction accompanied by an aggressive periosteal reaction, often described as an "onion-skin" or "sunburst" appearance.
Clinical Pearl: Any permeative osteolytic lesion in the tubular bones of the hand in a young patient must be considered Ewing sarcoma until proven otherwise. A prompt incisional biopsy is mandatory.
In the past, the prognosis for Ewing sarcoma was dismal, with 5-year survival rates reported between 10% and 15%. However, the advent of modern multidisciplinary treatment protocols—combining multi-agent systemic chemotherapy (e.g., vincristine, doxorubicin, cyclophosphamide, alternating with ifosfamide and etoposide) with localized radiation therapy and wide surgical excision—has dramatically altered the natural history of the disease. Current 5-year survival rates have improved significantly, ranging from 50% to 75% for localized disease.
Subungual Squamous Cell Carcinoma
Squamous cell carcinoma (SCC) is the most common primary malignancy of the nail bed. It is frequently misdiagnosed as a chronic paronychia, verruca vulgaris, or pyogenic granuloma, leading to a dangerous delay in definitive treatment. Patients typically present with chronic ulceration, nail plate deformity, or a non-healing subungual mass.
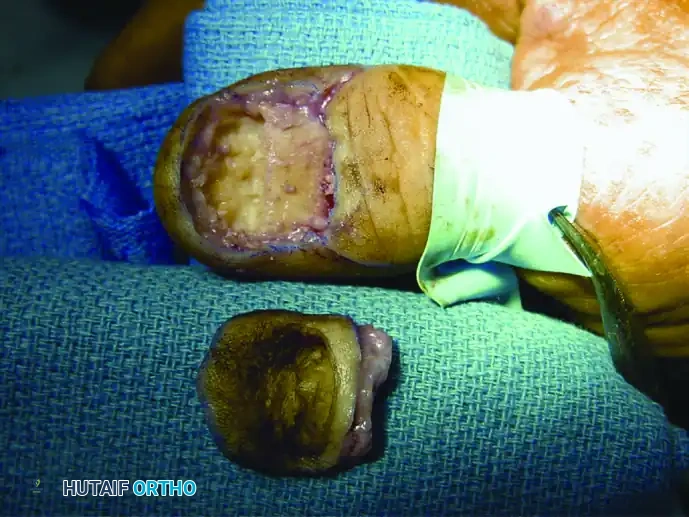
Figure 1: Clinical presentation of a subungual squamous cell carcinoma of the nail bed, demonstrating chronic ulceration and destruction of the nail plate.
Surgical management dictates wide local excision. Depending on the depth of invasion and bone involvement (assessed via preoperative radiographs or MRI), treatment ranges from wide local excision of the nail bed with full-thickness skin grafting to distal interphalangeal (DIP) joint amputation.
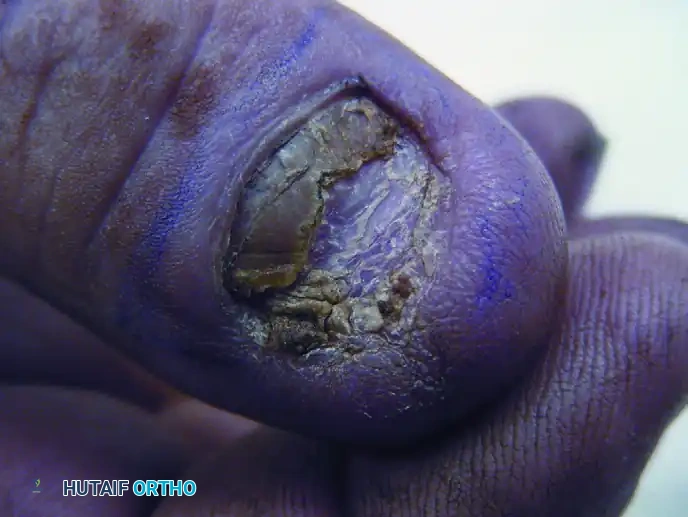
Figure 2: Wide surgical excision of the squamous cell carcinoma, including a portion of the underlying distal phalanx, to ensure negative oncologic margins while allowing for adequate soft tissue closure.
When bone is not grossly invaded but close margins are suspected, a partial ostectomy of the distal phalanx may be performed to ensure clear margins while preserving the length and tactile function of the digit.
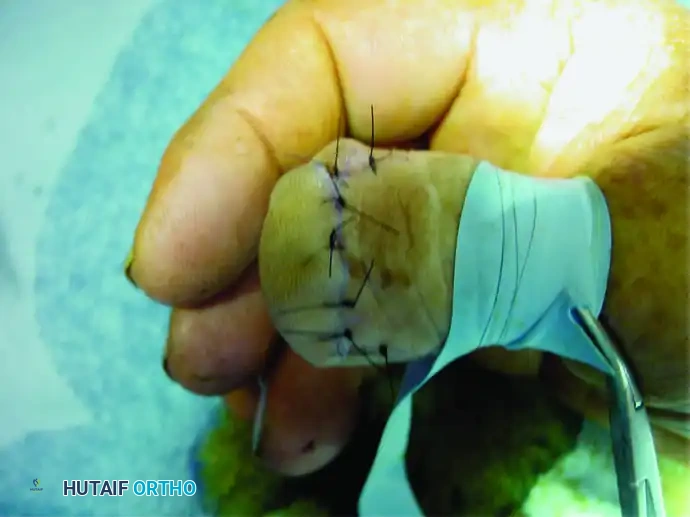
Figure 3: Final closure after wide excision. Meticulous soft tissue handling is required to provide a durable, sensate tip.
TUMOROUS CONDITIONS: GANGLION CYSTS
Pathogenesis and Epidemiology
Ganglions are the most common cause of focal hand masses, accounting for 50% to 70% of all soft tissue tumors of the hand and wrist. They characteristically arise from the synovium of joints, tendon sheaths, or directly from tendons. While the exact etiology remains debated, the prevailing theory suggests that a history of acute trauma or recurrent chronic microtrauma (often occupational) leads to mucoid degeneration of connective tissue and the formation of a one-way valve mechanism. This allows synovial fluid to escape the joint capsule but prevents its return, leading to the concentration of hyaluronic acid and the formation of a thick, highly viscous, mucin-filled cyst.
Clinical Presentation and Topography
Dorsal Wrist Ganglions
Dorsal wrist ganglia are the most common upper extremity ganglia (comprising 60% to 70% of cases). They almost exclusively originate from the distal dorsal portion of the scapholunate (SL) interosseous ligament. Clinically, they present as firm, smooth, fluctuant, and round masses, most frequently palpable between the second and fourth extensor tendon compartments.
Surgical Warning: The size of a dorsal ganglion is not proportional to the pain experienced by the patient. Occult, small, or imperceptible cysts hidden beneath the extensor retinaculum can cause incapacitating pain due to mass effect on the posterior interosseous nerve (PIN) during extreme wrist extension.
Volar Wrist Ganglions
The second most frequent site is the volar wrist, typically presenting just radial to the flexor carpi radialis (FCR) tendon. These cysts usually arise from the radioscaphocapitate (RSC) or radiolunate (RL) ligaments. Ganglions extending proximally along the extensor or flexor tendons are likely to be less firm, multilocular, and irregular, but they still contain the pathognomonic slightly yellow, gelatinous fluid.
Flexor Tendon Sheath Ganglions (Retinacular Cysts)
The most common site for a ganglion in the digits is the volar aspect of the metacarpophalangeal (MCP) joint flexion crease. Arising from the A1 or A2 pulley of the flexor tendon sheath, these masses are typically small (3-5 mm), round, hard, and exquisitely tender to firm pressure. They may cause snapping or trigger finger symptoms due to mechanical impingement.
Guyon Canal Ganglions
Ganglions seldom occur in the palm. When they do, their presence is often heralded not by an external palpable mass, but by secondary neurologic changes caused by compression. Cysts arising in or distal to the Guyon canal can compress the deep motor branch of the ulnar nerve, leading to profound, painless atrophy of the ulnar-innervated intrinsic muscles of the hand.
Evidence-Based Management Strategies
Ganglions occasionally resolve spontaneously, but they frequently recur when treated by simple rupture or aspiration. Historically, dorsal cysts were ruptured by striking them with a heavy book (the "Bible bump" treatment), a practice now universally condemned due to the risk of collateral carpal injury.
Current evidence dictates the following cure rates based on intervention:
* Needle Rupture/Aspiration with Corticosteroid: 65% cure rate. (Note: Volar wrist ganglions should never be ruptured by pressure or blindly aspirated due to the intimate association of the cyst with the radial artery).
* Surgical Excision (Local Anesthesia + Tourniquet): 84% cure rate.
* Surgical Excision (General Anesthesia / Regional Block): 94% cure rate.
Arthroscopic resection of dorsal wrist ganglions has gained popularity, offering a low complication rate and smaller incisions. However, comparative studies demonstrate that this technically demanding procedure has not substantially lowered the recurrence rate when compared to meticulous open excision.
For flexor tendon sheath ganglions, multiple punctures with an 18-gauge needle under local anesthesia can be curative, though open cyst excision with a small window of the retinacular pulley remains the definitive gold standard.
SURGICAL TECHNIQUE 77-1: DORSAL WRIST GANGLION EXCISION
The cornerstone of successful ganglion excision is the complete removal of the cyst along with a generous margin of the adjacent joint capsule at its base. Failure to excise the capsular root is the primary cause of recurrence.
Preoperative Preparation and Positioning
- Anesthesia: The procedure is optimally performed under a regional block (axillary or supraclavicular) or general anesthesia to ensure complete patient comfort and allow for a motionless surgical field.
- Tourniquet: Exsanguinate the limb and inflate an upper arm tourniquet to 250 mmHg to provide a bloodless field, which is critical for identifying the capsular stalk and protecting cutaneous nerves.
- Positioning: Place the patient supine with the operative arm extended on a radiolucent hand table. Pronate the forearm and slightly flex the wrist over a rolled towel to bring the dorsal cyst into prominence.
Step-by-Step Surgical Approach
1. Incision and Superficial Dissection
* Make a 2.0- to 3.0-cm transverse incision in one of the dorsal wrist creases, centered directly over the scapholunate interval.
* This incision will often be slightly proximal to the maximum prominence of the cyst, roughly along a line connecting the ulnar and radial styloids.
* Pitfall Avoidance: Do not extend the incision too far radially or ulnarly. Carry the incision through the dermis only. Spread the underlying subcutaneous tissues longitudinally to avoid transecting the superficial sensory branches of the radial nerve (SRN) or the dorsal ulnar sensory nerve (DUSN).
2. Nerve Protection and Retinacular Exposure
* Protect all cutaneous nerves by carefully elevating the soft tissues off the extensor retinaculum. The superficial sensory branch of the radial nerve is often visible and must be gently retracted radially with a vessel loop.
* Identify the extensor retinaculum and the borders of the third extensor compartment.
3. Deep Dissection and Tendon Retraction
* Open the ulnar border of the third extensor compartment (extensor pollicis longus - EPL) from the radiocarpal joint distally for several centimeters.
* Retract the EPL tendon and the underlying radial wrist extensor tendons (ECRL and ECRB) radially.
* Dissect out the extensor digitorum communis (EDC) to the index finger, and retract it along with the remaining EDC tendons ulnarly. This exposes the dorsal wrist capsule.
4. Cyst Isolation and Capsular Excision
* Identify the dorsal intercarpal and radiocarpal ligaments. Retract them distally and proximally, respectively.
* Using a combination of sharp and blunt dissection, isolate the ganglion in its entirety down to its stalk.
* Excise the cyst along with a 1 cm x 1 cm portion of its capsular origin at the dorsal scapholunate ligament.
* CRITICAL STEP: Do not injure the intrinsic scapholunate interosseous ligament. The cyst typically arises from the distal dorsal portion of this ligament. While the dorsal capsule must be excised, the deep interosseous and volar portions of the SL ligament are the primary stabilizers of the SL joint. Dissect the capsular tissue cleanly to expose, but not violate, the SL ligament.
* Remove any redundant or degenerative capsular tissue from the midcarpal and radiocarpal joints.
5. Posterior Interosseous Nerve (PIN) Neurectomy
* To reduce postoperative pain and decrease the risk of neuroma formation from capsular stretching, a PIN neurectomy is highly recommended.
* Identify the terminal branch of the posterior interosseous nerve on the radial floor of the fourth extensor compartment.
* Resect a 1.0-cm segment of the nerve and allow the proximal stump to retract deep into the muscle belly, proximal to the radiocarpal joint.
6. Hemostasis and Closure
* Deflate the tourniquet. Irrigate the wound copiously with sterile saline and meticulously cauterize all remaining bleeding points using bipolar electrocautery.
* Do not attempt to close the joint capsule. Leaving the capsular defect open prevents postoperative wrist stiffness and does not increase the risk of instability.
* Close the skin incision with a running, subcuticular 4-0 or 5-0 nylon or absorbable monofilament suture.
* Apply Steri-Strips over a liquid skin adhesive.
Postoperative Care and Rehabilitation
- Immediate Post-Op: Apply a soft, bulky compressive dressing with a volar orthoplast splint holding the wrist in slight extension (20 degrees) to support the wrist and control edema.
- Days 2 to 3: The patient is instructed to remove the bulky dressing at home and immediately initiate an active range-of-motion (ROM) program for the fingers and wrist. Early mobilization is paramount to prevent capsular scarring and extensor tendon adhesions.
- Week 2: The first formal postoperative clinical appointment occurs at 10 to 14 days. Sutures are removed, and a more aggressive, therapist-directed hand therapy program is encouraged to restore terminal flexion and extension.
- Return to Activity: Heavy lifting and extreme weight-bearing across the wrist are restricted for 4 to 6 weeks to allow the dorsal capsular defect to heal via secondary intention. Full recovery and resolution of deep aching pain may take up to 3 months.
You Might Also Like
