Tumors of the Hand and Wrist: Surgical Management
Key Takeaway
The management of hand and wrist tumors requires a meticulous understanding of complex anatomy, oncologic staging, and reconstructive principles. This guide details the evidence-based surgical approaches for benign lesions, malignant sarcomas, and tumorous conditions like ganglion cysts and Paget's disease. Emphasizing limb salvage and functional restoration, it provides orthopedic surgeons with critical insights into biopsy techniques, tumor resection margins, and advanced reconstructive protocols.
Introduction to Neoplasia of the Hand and Upper Extremity
The evaluation and management of tumors and tumor-like conditions in the hand and wrist present a unique challenge to the orthopedic surgeon. The dense concentration of critical neurovascular, tendinous, and articular structures within a confined anatomical space demands meticulous surgical planning. While the vast majority of hand masses are benign or represent pseudotumors (such as ganglion cysts), the potential for primary or metastatic malignancy must never be overlooked.
This comprehensive guide synthesizes the principles of musculoskeletal oncology—including the Enneking staging system—with advanced hand surgery techniques, detailing the operative management of benign, malignant, and tumorous conditions of the upper extremity.
Principles of Evaluation, Staging, and Biopsy
Clinical and Radiographic Evaluation
The diagnostic algorithm begins with a thorough history and physical examination, focusing on the rate of growth, presence of pain (especially rest pain or night pain), and neurologic symptoms. Standard orthogonal radiographs remain the cornerstone of initial imaging, characterizing the lesion's zone of transition, periosteal reaction, and matrix mineralization.
Magnetic Resonance Imaging (MRI) with and without gadolinium contrast is the gold standard for evaluating soft tissue masses and determining the intraosseous and extraosseous extent of bone tumors.
The Enneking Surgical Staging System
Surgical planning is dictated by the Enneking staging system for musculoskeletal tumors, which categorizes lesions based on histologic grade (G), local anatomic extent (T), and the presence of regional or distant metastasis (M).
* Stage 1 (Low Grade): Managed typically with wide local excision.
* Stage 2 (High Grade): Requires radical resection or amputation, often with neoadjuvant or adjuvant therapies.
* Stage 3 (Metastatic): Palliative or systemic management takes precedence.
Surgical Biopsy Principles
The biopsy is a critical operative step that can dictate the success or failure of subsequent limb salvage surgery.
Surgical Warning: A poorly planned biopsy can contaminate adjacent compartments, converting a salvageable limb into an obligate amputation. The biopsy tract must always be placed in line with the planned definitive surgical incision so it can be excised en bloc.
Key Biopsy Tenets:
1. Longitudinal Incisions: Always use longitudinal incisions in the extremities. Transverse incisions contaminate multiple neurovascular planes.
2. Tourniquet Use: Exsanguination by elevation is permitted, but never use an Esmarch bandage over a suspected tumor, as this can mechanically seed tumor cells into the systemic circulation.
3. Hemostasis: Meticulous hemostasis is mandatory before closure to prevent a post-biopsy hematoma, which acts as a vehicle for local tumor dissemination.
Benign Tumors of Bone and Soft Tissue
Enchondroma
Enchondromas are the most common primary bone tumors of the hand, typically presenting as asymptomatic swelling or a pathologic fracture in the proximal phalanx or metacarpal. Radiographically, they appear as well-circumscribed, centrally located lytic lesions with stippled chondroid calcification.
Surgical Technique: Intralesional Curettage and Grafting
1. Approach: A dorsal longitudinal incision is made over the affected phalanx or metacarpal, splitting the extensor mechanism longitudinally (or retracting it laterally) to expose the periosteum.
2. Cortical Window: A high-speed burr or osteotome is used to create an oval cortical window. The window must be large enough to access the entire medullary canal.
3. Curettage: Meticulous intralesional curettage is performed using angled curettes. The cavity must be scraped down to healthy, bleeding cortical bone.
4. Adjuvant Treatment: The cavity is treated with a chemical adjuvant (e.g., 88% phenol followed by alcohol neutralization, or hydrogen peroxide) to eliminate microscopic disease.
5. Defect Management: The void is packed with cancellous autograft, allograft, or bone cement (PMMA). PMMA provides immediate structural stability, allowing for early mobilization.
Giant Cell Tumor of Bone (GCT)
GCTs in the hand are rare but exhibit a more aggressive clinical course and a higher recurrence rate than their counterparts in the axial skeleton or long bones. They typically involve the epiphysis and metaphysis.
Surgical Management:
Due to the aggressive nature of GCTs in the hand, simple curettage is associated with unacceptably high recurrence rates.
* Extended Curettage: Aggressive curettage combined with high-speed burring and cryosurgery (liquid nitrogen) or phenol is required.
* Wide Resection: For lesions with extensive cortical destruction or joint involvement, wide en bloc resection with structural reconstruction (e.g., non-vascularized fibular autograft or vascularized bone transfer) is indicated.
Glomus Tumor
Glomus tumors are benign hamartomas of the neuromyoarterial glomus body, classically presenting with a triad of severe pain, cold intolerance, and point tenderness. They are most commonly subungual.
Surgical Technique: Transungual Excision
1. Nail Plate Removal: The nail plate is carefully elevated and removed.
2. Nail Bed Incision: A longitudinal incision is made directly through the sterile matrix over the bluish discoloration of the tumor.
3. Enucleation: The tumor is usually well-encapsulated and can be enucleated bluntly using tenotomy scissors or a Freer elevator.
4. Repair: The nail bed is meticulously repaired with 6-0 or 7-0 absorbable sutures to prevent postoperative nail deformity. The native nail plate (or a silicone substitute) is replaced as a stent.
Peripheral Nerve Tumors
Schwannoma (Neurilemmoma):
Schwannomas are the most common benign nerve tumors in the upper extremity. They grow eccentrically from the nerve fascicles and are encapsulated. Under loupe or microscopic magnification, the epineurium is incised longitudinally, and the tumor can typically be enucleated while preserving the functional nerve fascicles.
Lipofibromatous Hamartoma:
This rare, benign tumor predominantly affects the median nerve, presenting with fibrofatty infiltration between and within the nerve fascicles.
Clinical Pearl: Attempting to resect a lipofibromatous hamartoma will result in catastrophic neurologic deficit. Treatment is strictly palliative, consisting of prophylactic carpal tunnel release to decompress the enlarged nerve.
Malignant Tumors of the Hand
Primary malignancies of the hand are exceedingly rare. When they occur, the principles of oncologic margins take absolute precedence over functional preservation.
Chondrosarcoma
Chondrosarcoma is the most common primary malignant bone tumor of the hand. It often arises in the proximal phalanges or metacarpals, sometimes secondary to a pre-existing enchondroma. Patients typically present with a painful, enlarging mass. Radiographs show aggressive bone destruction, cortical breakthrough, and soft tissue extension.
Surgical Management:
* Ray Amputation: For lesions confined to a single digit or metacarpal, a radical ray amputation provides definitive wide margins.
* Limb Salvage: In select cases involving the carpus or distal radius, wide en bloc resection followed by complex reconstruction (e.g., wrist arthrodesis with vascularized fibular graft) may be attempted, provided negative margins can be achieved.
Soft Tissue Sarcomas (Epithelioid and Synovial Sarcoma)
Epithelioid sarcoma is notorious for presenting as a benign-appearing, painless subcutaneous nodule or chronic ulceration, leading to frequent misdiagnosis and delayed treatment. It has a high propensity for lymphatic spread.
Surgical Management:
* Wide Local Excision vs. Amputation: Radical resection with 2-3 cm margins is required. Given the lack of expendable soft tissue in the hand, this frequently necessitates digital or ray amputation.
* Lymph Node Evaluation: Due to the risk of regional metastasis, sentinel lymph node biopsy or regional lymphadenectomy is often indicated for epithelioid sarcoma.
* Adjuvant Therapy: Postoperative brachytherapy or external beam radiation is utilized for high-grade lesions or close margins.
Metastatic Disease (Acrometastases)
Metastatic lesions to the hand (acrometastases) are rare, accounting for less than 0.1% of all osseous metastases. The lung is the most common primary source, followed by the breast and kidney. They often present with severe pain, swelling, and erythema, mimicking an acute infection (osteomyelitis or felon). Treatment is generally palliative, involving localized radiation or simple ray amputation for pain control and rapid return to function.
Tumorous Conditions and Pseudotumors
Ganglion Cysts
Ganglion cysts are the most common soft tissue masses of the hand and wrist. They are mucin-filled pseudocysts arising from adjacent joint capsules or tendon sheaths.
Dorsal Wrist Ganglion:
Arising from the scapholunate (SL) ligament.
* Open Resection: A transverse incision is made over the mass. The cyst is traced down to its stalk at the SL interval. A small window of the dorsal capsule must be excised along with the stalk to minimize recurrence.
* Arthroscopic Resection: Utilizing the 3-4 and 4-5 or 6R portals, the dorsal capsule and ganglion stalk are debrided from within the joint using a shaver, offering excellent visualization of the SL ligament and potentially faster recovery.
Volar Wrist Ganglion:
Arising from the radiocarpal joint or scaphotrapezial joint, often intimately associated with the radial artery.
* Surgical Technique: A longitudinal or zigzag incision is used. The radial artery must be identified, mobilized, and protected. The stalk is traced to the volar capsule and excised. Arthroscopic resection is generally avoided for volar cysts due to the proximity of the radial artery and palmar cutaneous branch of the median nerve.
Paget's Disease of Bone
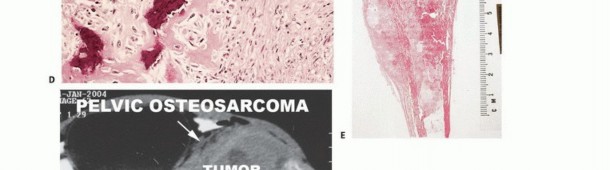
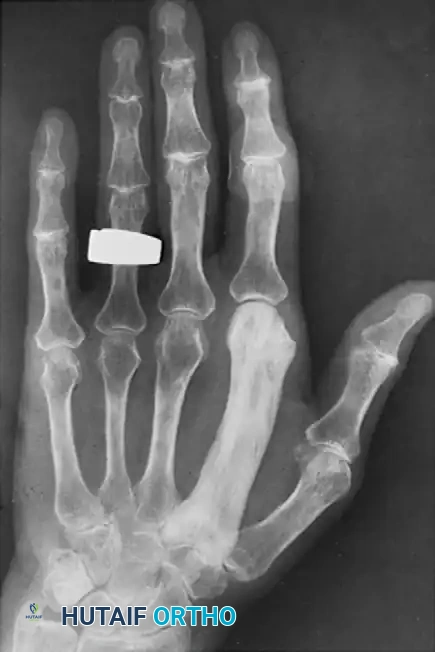
Paget's disease (osteitis deformans) is a disorder of abnormal bone remodeling characterized by excessive osteoclastic resorption followed by disorganized osteoblastic bone formation. While it commonly affects the pelvis, femur, and skull, involvement of the hand is exceptionally rare.
When the hand is involved, it may present as a monostotic or polyostotic process. Patients may experience localized pain, bony enlargement, and deformity. Radiographically, the affected bones demonstrate cortical thickening, trabecular coarsening, and osseous expansion.
Management:
Surgical intervention for Paget's disease in the hand is rarely indicated unless there is a pathologic fracture or severe deformity causing functional impairment. Medical management with bisphosphonates is the primary treatment modality to decrease bone turnover and alleviate pain. If surgery is required (e.g., corrective osteotomy or fracture fixation), the surgeon must be prepared for highly vascular bone and the potential for delayed union. Furthermore, any sudden increase in pain or rapid swelling in a Pagetic bone must raise the clinical suspicion for malignant transformation to secondary osteosarcoma, which carries a grave prognosis.
Postoperative Protocols and Rehabilitation
The postoperative management of hand tumors is highly variable and depends entirely on the extent of resection and the nature of the reconstruction.
- Benign Lesions (e.g., Ganglion Excision, Enchondroma Curettage):
- Immobilization in a bulky soft dressing or volar splint for 7-10 days to allow for wound healing.
- Early active range of motion (AROM) is initiated to prevent tendon adhesions and joint stiffness.
- If a large cortical window was created for an enchondroma, protective splinting during heavy lifting may be required for 4-6 weeks until bone graft incorporation is evident radiographically.
- Malignant Lesions (Limb Salvage/Amputation):
- Prolonged immobilization may be necessary if complex flap coverage or vascularized bone grafting was performed.
- Close coordination with hand therapy is essential for edema control, scar management, and adaptive functional training.
- Strict oncologic surveillance protocols (serial radiographs, chest CT, MRI) must be established based on the specific tumor histology and Enneking stage.
Conclusion
The surgical management of hand and wrist tumors requires a delicate balance between aggressive oncologic resection and the preservation of intricate hand function. A thorough understanding of tumor biology, strict adherence to biopsy principles, and mastery of complex reconstructive techniques are paramount. Whether performing a simple marginal excision of a ganglion cyst or a complex limb-salvage reconstruction for a primary sarcoma, the orthopedic surgeon must approach each lesion with meticulous planning and a deep respect for the anatomical complexities of the upper extremity.
You Might Also Like