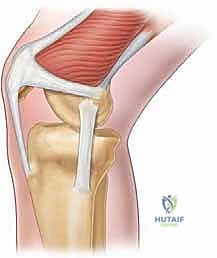
Proximal Metatarsal Opening Wedge Osteotomy: A Masterclass in Hallux Valgus Correction
Key Takeaway
Join us in the OR for a detailed masterclass on Proximal Metatarsal Opening Wedge Osteotomy. We'll explore intricate surgical anatomy, meticulous preoperative planning, and granular intraoperative steps for precise hallux valgus correction. Learn critical pearls, pitfalls, and comprehensive postoperative management to ensure optimal patient outcomes in this challenging foot deformity.
Alright, team, gather around. Today, we're tackling a common yet complex deformity: the symptomatic hallux valgus, or bunion. This isn't just a cosmetic issue; it's a painful, progressive condition characterized by lateral deviation (valgus) of the great toe's proximal phalanx and a compensatory medial (varus) deviation of the first metatarsal. Our goal with the Proximal Metatarsal Opening Wedge Osteotomy (PMOW) is to restore proper alignment, alleviate pain, and prevent further progression. This procedure, often combined with a distal soft tissue release and medial capsular placation, is particularly effective for moderate to severe deformities, those with a short first ray, an intermetatarsal angle (IMA) greater than 12 degrees, or recurrent hallux valgus.
Surgical Anatomy: Navigating the First Ray
Before we make any incisions, let's meticulously review the intricate anatomy of the first ray. Understanding these relationships is paramount to a successful outcome and avoiding complications.
Osteology of the First Ray
The first metatarsal is the stoutest of the metatarsals, articulating proximally with the medial cuneiform at the first metatarsal-cuneiform (MTC) joint and distally with the proximal phalanx at the metatarsophalangeal (MTP) joint. The MTP joint is unique due to its bipartite sesamoid complex embedded within the flexor hallucis brevis (FHB) tendon, acting as a fulcrum for the great toe's powerful flexors. We'll be working at the proximal metatarsal, roughly 1.5 cm distal to the first MTC joint. Remember, an intermetatarsal facet can occasionally be present between the first and second metatarsal bases, which can create a rigid metatarsus primus varus and impede correction of the 1-2 IMA.
Ligamentous & Tendinous Structures
The great toe MTP joint is stabilized by a robust complex of tendons and ligaments. The flexor hallucis brevis, abductor hallucis, and adductor hallucis tendons, along with the plantar aponeurosis and joint capsule, coalesce to form the plantar plate. This structure encases and stabilizes the first metatarsal head, crucial for weight-bearing and propulsion. The sesamoid ligaments mesh intimately with the collateral ligaments both medially and laterally, forming a critical meshwork. In hallux valgus, we typically find medial capsular laxity and lateral capsular contracture. The abductor hallucis, normally a medial stabilizer, can become functionally ineffective, sliding plantar to the metatarsal head, leading to pronation of the phalanx. The adductor hallucis tendon, inserting into the lateral aspect of the proximal phalanx and fibular sesamoid, becomes a deforming force, pulling the toe laterally.
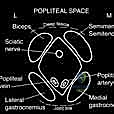
Neurovascular Considerations
This is where precision is non-negotiable.
* Nerves:
* Superficial Peroneal Nerve: A critical branch of this nerve supplies the dorsum of the foot, including the hallux. Its medial dorsal cutaneous branch crosses the surgical field dorsomedially. We must meticulously identify and protect it during our dorsomedial approach to the proximal metatarsal.
* Deep Peroneal Nerve: While deeper, it innervates the extensor hallucis brevis and the first dorsal interosseous muscle, and its terminal branch provides sensation to the first web space.
* Medial Plantar Nerve: Provides sensation to the medial plantar aspect of the hallux.
* Common Digital Nerves: Specifically, the first common digital nerve running in the first web space, which can be irritated by adductor contracture.
* Vessels:
* The first metatarsal receives its primary arterial supply from the lateral midshaft, with flow predominantly distal. Key sources include the first dorsal and plantar metatarsal arteries, and the superficial branch of the medial plantar artery. Intraosseous flow is variable. Meticulous hemostasis and careful dissection are essential to preserve this delicate blood supply, especially to the metatarsal head, to prevent avascular necrosis.
* Tendons:
* Extensor Hallucis Longus (EHL): This tendon runs dorsally over the first MTP joint. It must be identified and protected throughout the procedure, particularly during the dorsomedial incision and exposure of the metatarsal.
Surgical Warning: Always identify the superficial peroneal nerve branches and the EHL tendon immediately upon deep dissection. Retract them gently, never forcefully, to prevent iatrogenic injury. Nerve injury can lead to debilitating paresthesia or even an anesthetic toe.
Patient Evaluation & Preoperative Planning
Our journey begins long before the patient enters the operating room. Thorough assessment and meticulous planning are the cornerstones of success.
Clinical Assessment
We'll start with a detailed history, noting the chief complaint (often a painful, reddened prominence over the medial MTP joint), duration, and aggravating factors like constrictive footwear. On inspection, we look for the swollen, reddened medial eminence, lateral deviation of the toe, and often pronation in severe cases. Palpation reveals tenderness over the medial eminence, crepitus, warmth, and bursitis. We'll assess the range of motion (ROM) of the MTP joint, which is often surprisingly well-preserved even in severe deformities, though chronic deformities or congruent joints with increased distal metatarsal articular angle (DMAA) may show less dorsiflexion. We also check ROM while gently reducing the deformity. Don't forget to palpate the first MTC joint for prominence, swelling, or pain with cantilever stress, which might indicate instability. Assess gastrocnemius tightness and the mobility of the first MTC joint. Finally, a gait analysis, focusing on the stance phase and hindfoot position, is crucial. Any concomitant pes planovalgus deformity may need addressing. Neurological and vascular status (pulses, sensation, skin integrity) are also critical, as neuropathy or poor circulation can contraindicate surgery.
Radiographic Analysis
Weight-bearing anteroposterior (AP) and lateral radiographs are indispensable. We're looking for specific angles:
* Hallux Valgus Angle (HVA): The angle between the long axis of the proximal phalanx and the long axis of the first metatarsal. Normal is typically no greater than 15 degrees.
* 1-2 Intermetatarsal Angle (IMA): The angle between the long axis of the first and second metatarsals. Normal is usually no more than 9 degrees. Our PMOW procedure primarily targets this angle.
* Distal Metatarsal Articular Angle (DMAA): This measures the relationship between the metatarsal long axis and the lateral inclination of the distal metatarsal articular surface. An increased DMAA (greater than 15 degrees) indicates a valgus inclination of the articular surface and is often associated with congruent joint hallux valgus, especially in juvenile cases.
* Interphalangeal (IP) Angle (HVI): Measured by a line bisecting the base of the proximal phalanx and the long axis of the phalanx. An increased HVI (greater than 10 degrees) suggests a deformity within the phalanx itself, which typically requires a separate phalangeal osteotomy (Akin osteotomy) and is not corrected by proximal metatarsal or distal soft tissue procedures.
* Sesamoid Subluxation: Noted on the AP radiograph and sesamoid view, indicating the degree of MTP joint subluxation.
* First MTC Joint Stability: Look for a first MTC angle greater than 10 degrees, excess joint obliquity on the AP view, plantar gapping of more than 2 mm on the lateral view, or an intermetatarsal os. Frank instability or hypermobility may warrant a first MTC arthrodesis instead of a proximal metatarsal osteotomy.
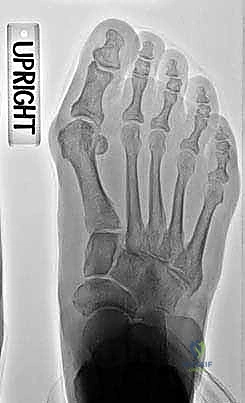
Preoperative weight-bearing AP radiograph shows a severe hallux valgus deformity.
Indications & Contraindications
Indications for PMOW:
* Moderate to severe hallux valgus with an IMA > 12 degrees.
* Hallux valgus associated with a short first ray.
* Recurrent hallux valgus after a distal procedure alone.
* As an adjunct to a distal procedure if subtotal correction is achieved.
* Congruent joint hallux valgus with an increased DMAA, especially when combined with a biplanar chevron.
Contraindications:
* Advanced arthrosis of the first MTP joint (arthrodesis is preferred).
* Active infection.
* Severe peripheral vascular disease or neuropathy (loss of protective sensation).
* Unrealistic patient expectations.
* Inability to comply with postoperative rehabilitation protocols.
* Significant first MTC joint instability, which may necessitate an MTC arthrodesis.
Surgical Goals
Our primary goals are to:
1. Correct the 1-2 IMA and restore the anatomical alignment of the first metatarsal.
2. Maintain or restore MTP joint congruity.
3. Decompress the medial eminence and resolve bursitis.
4. Balance the soft tissues around the MTP joint.
5. Allow for stable fixation and early weight-bearing.
Operating Room Setup & Patient Positioning
Team, let's get the room ready.
Fluoroscopy & Equipment
We'll need our C-arm positioned to allow for immediate AP, lateral, and oblique views of the foot. Ensure the C-arm can be brought in and out smoothly without contaminating the sterile field. We'll have the specialized PMOW plate fixation system (Arthrex, Inc.) ready, including the low-profile plates, various size osteotomes, a mini lamina spreader, and measuring wedges. A high-speed burr for the bunionectomy, appropriate retractors (Hohmann, Senn), and standard foot and ankle instrumentation will also be needed.
Patient Positioning
The patient will be in a supine position on the operating table. The affected leg will be prepped and draped in a sterile fashion, typically from the mid-calf to the toes. We'll use a thigh tourniquet for hemostasis, inflated to appropriate pressure after exsanguination with an Esmarch bandage. Ensure the foot is free to move for intraoperative fluoroscopy. A small bump under the ipsilateral hip can help internally rotate the leg slightly, bringing the foot into a more neutral position for the surgeon.
Intraoperative Execution: The Proximal Metatarsal Opening Wedge Osteotomy
Alright, everyone, let's begin. Tourniquet up.
Preparation & Incision Planning
We'll start by marking our incisions with a surgical pen. For most cases, we'll use two incisions, sometimes three if a first web space release is deemed necessary.
- Medial Bunionectomy Incision: Our first longitudinal incision will be centered over the medial eminence, extending proximally and distally enough to allow for adequate exposure. This will be our primary access for the bunionectomy and medial capsular work.
- Proximal Metatarsal Osteotomy Incision: Our second incision for the PMOW itself will be dorsomedially, beginning just distal to the first MTC joint. This incision needs to be long enough to accommodate the plate and screws, usually around 3-4 cm.
Surgical Warning: Prior to making the dorsomedial incision, palpate the course of the superficial peroneal nerve branches and the EHL tendon. Plan your incision to run parallel and slightly medial to the EHL, carefully avoiding any crossing nerve branches.
Medial Bunionectomy & Capsulotomy
Through our medial incision, we'll deepen our dissection, carefully identifying the medial dorsal cutaneous nerve branches and retracting them. We'll then perform a routine bunionectomy.
- Capsulotomy: We'll make an inverted L-shaped capsulotomy on the medial side of the MTP joint. The horizontal limb runs along the plantar aspect of the joint, and the vertical limb extends proximally along the medial aspect of the metatarsal. This allows for excellent exposure of the medial eminence and facilitates later capsular placation.
- Medial Eminence Resection: Using an oscillating saw or a high-speed burr, we'll resect the prominent medial eminence. Take care to remove only the exostosis, preserving the articular cartilage.
- Autograft Harvest: Crucially, we will save the bone resected from the medial eminence to use as autograft for our opening wedge osteotomy. This provides excellent osteoinductive and osteoconductive properties. Place it in a sterile basin with saline.
Proximal Metatarsal Osteotomy: Exposure & Creation
Now, let's move to the dorsomedial incision for the osteotomy.
- Deep Dissection: Deepen the dorsomedial incision through subcutaneous tissues. Identify the EHL tendon and retract it laterally. Carefully identify and protect the medial dorsal cutaneous nerve branches, retracting them medially or laterally as needed. We want minimal periosteal stripping to preserve the blood supply.
- Osteotomy Site Identification: We'll expose the proximal first metatarsal shaft. The osteotomy is initiated approximately 1.5 cm distal to the first MTC joint on the medial aspect of the metatarsal.
- Osteotomy Creation: Using a small, sharp oscillating saw blade, we will perform the osteotomy. The cut should be slightly oblique, about 20-30 degrees, directed from medial to lateral, aiming towards the lateral aspect of the first metatarsal base. The critical point here is to avoid violating the lateral cortex. We want to create a stable lateral hinge. Using a small osteotome or a Kirschner wire as a depth gauge can help prevent over-penetration.
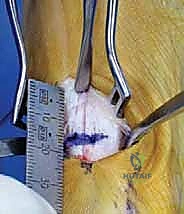
Site and position of first metatarsal opening wedge osteotomy. The osteotomy is initiated about 1.5 cm distal medial to the first MTC joint.
Surgical Warning: Maintain constant irrigation during saw cuts to prevent thermal necrosis. Be absolutely certain not to violate the lateral cortex; this hinge is crucial for stability and controlled opening. If the lateral cortex is breached prematurely, the construct can become unstable, requiring alternative fixation or additional stabilization.
Opening the Osteotomy & Achieving Correction
With the osteotomy complete, it's time to open our wedge.
- Controlled Opening: We'll use the specialized osteotomes from the PMOW set. Start with the smallest, then progress to successively larger blades. "Stacking" osteotomes – inserting one, then another next to it – is a key technique here. This allows for a gradual, controlled opening of the osteotomy, significantly diminishing the risk of breaking the lateral cortex compared to levering with a single osteotome.
- Correction Assessment: As we open the wedge, we'll apply manual pressure over the medial eminence and use a mini lamina spreader (supplied in the set) to gently distract the osteotomy and achieve the desired correction.
- Fluoroscopic Verification: At this stage, we'll bring in the C-arm. Obtain AP and oblique fluoroscopic views to verify the correction of the 1-2 IMA. We are aiming for an IMA of no more than 9 degrees.
- Wedge Sizing: Alternatively, a measuring wedge from the set can be inserted into the osteotomy to precisely determine the size of the opening required. Remember our planning rule: approximately 3 degrees of correction per millimeter of opening wedge.
- Graft Impaction: Once the desired correction is achieved and verified, we'll impact the autograft harvested from the medial eminence into the opening wedge. This provides structural support and promotes healing. If insufficient autograft is available, cancellous graft can be harvested from the lateral calcaneus through a small 1-2 cm lateral heel incision.
Surgical Warning: If the lateral cortical hinge should fail during opening, do not panic. The mini lamina spreader becomes even more useful to maintain the correction. Additional stabilization, such as an oblique screw placed outside the plate or a longer plate, may be required. In our experience, about 5% of cases result in lateral cortex fracture, but this rarely delays healing or modifies the postoperative protocol when managed appropriately.
Plate Application & Stabilization
With the osteotomy opened and grafted, we'll apply our low-profile opening wedge plate.
- Plate Positioning: The osteotomy site is held open, and the plate is positioned. The plate is designed to sit flush on the dorsomedial aspect of the metatarsal.
- First Screw Placement: The first screw is placed in the distal hole closest to the osteotomy. This effectively "sets" the plate and helps maintain the achieved correction. Drill a pilot hole, measure depth, tap if necessary, and insert the screw.
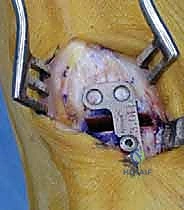
The plate has been set into position by insertion of the first screw.
3. Second Screw Placement: The next screw is placed in one of the proximal holes. We prefer to place both of these initial screws obliquely across the apex of the osteotomy. This provides excellent compression and stability across the osteotomy site.
4. Additional Stability: If there is any concern about stability, an additional oblique screw can be placed outside the plate, crossing the osteotomy to enhance the construct. To gain further support to the lateral cortex, one of the proximal screws may be placed not only through the plate but also across the osteotomy to capture the distal lateral cortex.
5. Final Screw Placement: The remaining screws are then placed distally and proximally to complete the fixation. Ensure all screws are appropriately seated and provide rigid fixation.
6. Final Fluoroscopic Check: With the plate securely fixed, we'll perform a final fluoroscopic check with the foot flat on the table. We'll verify a congruent MTP joint and ensure the IMA and DMAA are within acceptable limits. If the joint was congruent preoperatively with an increased DMAA, we confirm that the DMAA has been adequately addressed.
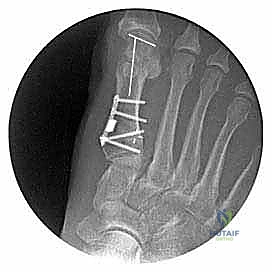
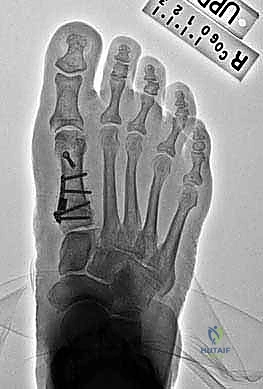
Six week postoperative weight-bearing AP radiograph shows good alignment post-PMOW first metatarsal and distal biplanar chevron bunionectomy.
Addressing Ancillary Deformities
Depending on the initial assessment, we may need to address other components of the deformity.
- Lateral Capsular Release: For subluxated deformities, the PMOW is typically combined with a modified McBride bunionectomy, which includes a lateral capsular release. This involves releasing the adductor hallucis tendon insertion, the lateral collateral ligament, and the fibular sesamoid ligament through a small incision in the first web space (our third incision, if used). However, with the powerful correction of the PMOW, an aggressive lateral release is often not required.
- Medial Capsular Plication: Through our medial incision, we'll perform a medial capsular placation. The capsule is repaired either through a drill hole at the metadiaphyseal junction or with a mattress suture technique proximally, provided the tissue quality is satisfactory. This tightens the medial capsule and helps maintain the corrected alignment
REFERENCES
-
Coughlin MJ. Juvenile hallux valgus. In: Coughlin MJ, Mann RA, eds. Surgery of the Foot and Ankle, ed
-
St. Louis, MO: CV Mosby, 1999:270–319.
-
Coughlin MJ, Carlson RE. Treatment of hallux valgus with an increased distal metatarsal articular angle: Evaluation of double and triple first ray osteotomies. Foot Ankle Int 1999;20:762–770.
-
Coughlin MJ, Shurnas PS. Hallux rigidus: Demographics, etiology, and radiographic assessment. Foot Ankle Int 2003;24:731–743.
-
Cooper MT, Berlet GC, Shurnas PS, et al. Proximal opening-wedge osteotomy of the first metatarsal for correction of hallux valgus. Surg Technol Int 2007;16:215–219.
-
Hardy RH, Clapham JCR. Observations on hallux valgus. J Bone Joint Surg 1951;33:376.
-
Mann RA, Coughlin MJ. Adult hallux valgus. In: Coughlin MJ, Mann RA, eds. Surgery of the Foot and Ankle, ed
-
St. Louis, MO: CV Mosby, 1999:150–269.
-
Sargas NP. Proximal opening wedge osteotomy of the first metatarsal for hallux valgus using a low profile plate. Foot Ankle Int 2009; 30:976–980.
-
Shereff MJ, Yang QM, Kummer FJ. Extraosseous and intraosseous arterial supply to the first metatarsal and metatarsophalangeal joint. Foot Ankle Int 1987;8:81–93.
-
Shurnas PS. Proximal opening wedge osteotomy of the 1st metatarsal: biomechanical and clinical evaluation. Proceedings of the AAOS Annual Meeting, Chicago, March 22–26, 2006.
-
Shurnas PS, Watson TS, Crislip TW. Proximal first metatarsal opening wedge osteotomy with a low profile plate. Foot Ankle Int 2009; 30:865–872.
-
Wukich DK, Roussel AJ, Dial D. Opening wedge osteotomy of the first metatarsal base: A technique for correction of metatarsus primus varus using a new titanium opening wedge plate. Oper Tech Orthop 2006;16:76–81.
-
Sargas 7 reported greater than 90% good and excellent results in a retrospective review of patients treated by proximal opening wedge osteotomy of the first metatarsal and distal procedure with a low incidence of complications and plate and screw removal.
-
The opposite side plate was used with excellent correction and minimal or no need for removal.
-
Shurnas 9 reported cadaveric biomechanical results comparing proximal chevron osteotomy and PMOW, finding no difference in load to failure, ultimate strength, or stiffness.
-
Shurnas 9 also reported the initial experience on 50 patients: 25 with at least 1 year of follow-up and 25 with 6 months to 1 year of follow-up.
-
The author reported about 3 degrees correction of 1–2 IMA per mm of opening wedge using an oblique osteotomy.
-
The mean postoperative IMA and HVA were 3 degrees and 11 degrees, respectively, with a mean change in IMA and HVA of 12 degrees and 20 degrees, respectively.
-
Mean time to radiographic and clinical healing was 5.8 weeks, with no instances of nonunion, malunion, or delayed union.
-
All patients were satisfied with their outcome, and mean range of motion was not significantly different comparing preoperative and postoperative values.
-
There was an insignificant increase in the mean first metatarsal protrusion distance of 1.9 mm but no instances of shortening, elevatus, or hardware failure.

You Might Also Like