Pediatric Trigger Thumb (Stenosing Tenosynovitis): A Comprehensive Academic Guide

Key Takeaway
Pediatric trigger thumb is FPL stenosing tenosynovitis, where a Notta's nodule catches at the A1 pulley, causing locking or triggering. It's developmental, not congenital. Treatment ranges from observation in young children to surgical A1 pulley release for persistent locking or a fixed flexion deformity, preventing secondary joint changes.
Introduction and Epidemiology
Stenosing tenosynovitis of the flexor pollicis longus (FPL), colloquially known as pediatric trigger thumb, is a common acquired condition presenting in early childhood. While historically referred to as "congenital trigger thumb," its typical presentation months or years after birth suggests a developmental rather than truly congenital etiology. The condition is characterized by a mechanical obstruction to the smooth gliding of the FPL tendon within its fibro-osseous sheath at the level of the A1 pulley, leading to triggering, locking, or a fixed flexion deformity of the interphalangeal (IP) joint of the thumb.
Epidemiologically, pediatric trigger thumb has an estimated incidence ranging from 0.03% to 3.3% in children. Large prospective screening studies of newborns have consistently failed to identify the condition at birth, heavily supporting the acquired developmental theory. There is no clear gender predilection, and bilateral involvement is reported in 20-30% of cases. The most common age of presentation is between six months and three years.
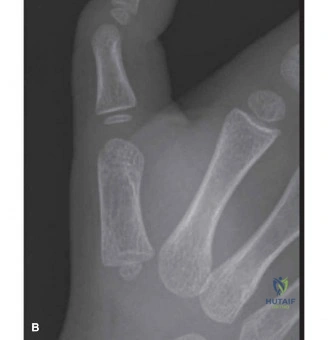
While the exact etiology remains debated, leading theories propose a disproportionate growth rate between the FPL tendon and its sheath, or a localized thickening of the A1 pulley and/or the tendon itself, forming a nodule (Notta's nodule) at the level of the metacarpophalangeal (MCP) joint. Histological studies of Notta's nodule reveal fibrocartilaginous metaplasia and myxoid degeneration within the tendon substance, suggesting a localized inflammatory or degenerative process rather than a purely congenital malformation. The surrounding A1 pulley exhibits parallel collagen fiber disorganization and chondroid metaplasia, indicative of chronic mechanical stress and friction. Familial cases are exceedingly rare, further supporting an acquired or developmental basis over a genetic one.
Differentiating pediatric trigger thumb from other pediatric hand anomalies is critical. The differential diagnosis includes congenital clasped thumb (characterized by extensor mechanism hypoplasia), arthrogryposis multiplex congenita, cerebral palsy (spastic thumb-in-palm deformity), and post-traumatic tendon tethering. Unlike these conditions, a classic pediatric trigger thumb presents in an otherwise neurologically and globally intact child, with a palpable nodule at the volar MCP flexion crease and an isolated inability to actively or passively extend the IP joint.
Surgical Anatomy and Biomechanics
A thorough understanding of the surgical anatomy of the thumb's flexor mechanism is paramount to safe and effective intervention for pediatric trigger thumb. The FPL tendon originates from the anterior surface of the radius and interosseous membrane, traversing distally through the carpal tunnel and then into the thumb. Its course is maintained by a series of annular and cruciform pulleys, which act as retinacular restraints, preventing bowstringing and optimizing mechanical advantage.
The critical structure implicated in pediatric trigger thumb is the A1 pulley. This first annular pulley originates from the volar plate and neck of the proximal phalanx, bridging the FPL tendon at the level of the MCP joint. In trigger thumb, the A1 pulley becomes thickened and constricted, impeding the smooth passage of the FPL tendon. A palpable nodule, termed Notta's nodule, typically forms on the FPL tendon just proximal to the A1 pulley. This nodule is essentially an eccentric thickening of the tendon, which then becomes ensnared within the narrowed A1 pulley as the child attempts to extend the thumb, causing the characteristic "triggering" or "locking" phenomenon. In severe cases, particularly with chronic locking, a fixed flexion contracture of the IP joint can develop due to adaptive shortening of the volar plate and collateral ligaments.
Neurovascular Structures of Concern
The median nerve innervates the FPL muscle in the forearm. Distally, the primary neurovascular structures at risk during A1 pulley release are the digital nerves and vessels of the thumb. The radial digital nerve of the thumb and the ulnar digital nerve of the thumb (branching from the median nerve) lie in close proximity to the A1 pulley incision site.
The radial digital nerve of the thumb typically courses along the radial side of the FPL sheath, superficial to the A1 pulley. Crucially, it often crosses obliquely from the ulnar side to the radial side over the proximal aspect of the FPL sheath near the MCP flexion crease. This superficial and variable course makes it highly susceptible to iatrogenic injury during skin incision and superficial dissection.
The ulnar digital nerve of the thumb (often splitting from the common digital nerve to the index finger) generally lies on the ulnar side of the FPL sheath and is less commonly injured, though it remains at risk with overly aggressive ulnar dissection. The precise anatomical variability of these nerves, particularly their superficial course within the subcutaneous tissue of the thenar crease, mandates careful dissection. The vascular supply to the thumb, primarily from the princeps pollicis artery, is also superficial in the area and must be protected.

The biomechanical consequence of a stenotic A1 pulley is the disruption of the normal excursion of the FPL tendon, creating a mechanical block to extension. The thumb flexor pulley system differs significantly from the triphalangeal digits. It consists of the A1 pulley, the variable annular pulley (Av), the oblique pulley, and the A2 pulley. The oblique pulley, originating from the proximal ulnar aspect of the proximal phalanx and inserting distally and radially, is the most critical biomechanical restraint against FPL bowstringing. During a surgical release of the A1 pulley, the surgeon must definitively identify and preserve the oblique pulley. Iatrogenic transection of the oblique pulley results in significant bowstringing of the FPL tendon, leading to a loss of IP joint flexion power, altered kinematics, and a secondary flexion contracture of the MCP joint.
Indications and Contraindications
The management of pediatric trigger thumb requires a nuanced approach, balancing the relatively high rate of spontaneous resolution in very young children against the risk of persistent fixed flexion contractures if left untreated. Natural history studies indicate that up to 60% of trigger thumbs presenting before the age of one year may resolve spontaneously or with conservative management (such as extension splinting and passive stretching). However, for children presenting after the age of two, or those with rigid, long-standing fixed flexion deformities, the rate of spontaneous resolution drops precipitously.
| Management Strategy | Indications | Contraindications |
|---|---|---|
| Observation and Stretching | Presentation under 12 months of age; intermittent triggering without fixed contracture; parental preference for non-operative initial approach. | Fixed, rigid flexion deformity; presentation in an older child (greater than 3 years) where spontaneous resolution is highly unlikely. |
| Extension Splinting | Children aged 1 to 2 years; flexible deformity; compliant parents capable of managing a rigid thermoplastic splint. | Non-compliant patient or family; skin breakdown or intolerance to splinting; fixed IP joint contracture unresponsive to passive stretching. |
| Surgical A1 Pulley Release | Persistent triggering or fixed flexion deformity after 1-2 years of age; failure of conservative management (splinting/stretching) after 3-6 months; presentation with a rigid deformity in a child over 2-3 years old. | Active local soft tissue infection; untreated systemic coagulopathy; alternative diagnoses such as spasticity (cerebral palsy) or congenital clasped thumb requiring different algorithmic approaches. |
Corticosteroid injections, while a mainstay of treatment for adult stenosing tenosynovitis, are generally contraindicated and rarely utilized in the pediatric population. The efficacy is poorly documented in children, the injection is highly distressing to the awake pediatric patient, and there is a theoretical risk of subcutaneous fat atrophy, depigmentation, and tendon rupture.
Pre Operative Planning and Patient Positioning
Preoperative evaluation is predominantly clinical. The diagnosis is confirmed by the presence of a palpable Notta's nodule at the volar MCP crease and a fixed or triggering flexion deformity of the IP joint. Advanced imaging, such as ultrasonography or magnetic resonance imaging (MRI), is rarely indicated for classic presentations. However, in atypical cases where a foreign body, anomalous tendon insertion, or mass (e.g., giant cell tumor of the tendon sheath) is suspected, ultrasound can be a cost-effective and non-invasive adjunct to evaluate the morphological characteristics of the FPL tendon and pulley system.
Surgical intervention in the pediatric population necessitates general anesthesia. The patient is positioned supine on the operating table with the affected upper extremity extended on a radiolucent hand table. A well-padded pediatric tourniquet is applied to the upper arm to provide a bloodless surgical field, which is absolutely critical for the safe identification of the delicate neurovascular structures.
The surgeon should utilize loupe magnification (typically 2.5x to 3.5x) to aid in the precise visualization of the digital nerves and the distinction between the A1 and oblique pulleys. Prior to inflation of the tourniquet, the limb is exsanguinated using an Esmarch bandage or by simple elevation, depending on the child's size. The hand and forearm are prepped and draped in a standard sterile orthopedic fashion.
Detailed Surgical Approach and Technique
The surgical release of the A1 pulley in a pediatric patient is a meticulous procedure that relies heavily on strict adherence to anatomical planes and blunt dissection techniques to avoid iatrogenic injury.
Incision and Superficial Dissection
The skin incision is typically planned at or just proximal to the prominent flexion crease of the thumb MCP joint. A transverse incision, measuring approximately 1.0 to 1.5 centimeters, is preferred by most pediatric hand surgeons as it heals with a cosmetically acceptable scar that blends into the natural skin creases. Alternatively, a longitudinal zigzag or Brunner-type incision can be utilized, though this is generally reserved for revision cases or when extensive exposure is anticipated.

Following the skin incision, dissection proceeds through the subcutaneous adipose tissue. This must be performed exclusively with blunt spreading techniques using fine tenotomy or mosquito scissors. The scissors should be oriented parallel to the longitudinal axis of the thumb to avoid inadvertent transection of the neurovascular bundles.
The most critical step in the superficial dissection is the definitive identification and protection of the radial digital nerve. As previously noted, this nerve frequently crosses the surgical field obliquely from ulnar to radial. Once identified, the nerve should be gently retracted radially using a small blunt retractor (such as a Senn or Ragnell retractor). The ulnar digital nerve should also be identified and protected ulnarly.
Pulley Release and Verification
With the neurovascular structures safely retracted, the underlying flexor tendon sheath is exposed. The surgeon must clear the areolar tissue overlying the sheath to accurately delineate the proximal edge of the A1 pulley and the distal extent where it transitions toward the oblique pulley.
The A1 pulley is then incised longitudinally along its midline. This is typically performed using a #15 scalpel blade or fine scissors. The release must begin proximally at the origin of the A1 pulley and extend distally. As the release progresses, the thickened Notta's nodule will become visible, often herniating through the retinacular defect.
The surgeon must exercise extreme caution at the distal aspect of the A1 pulley to avoid violating the oblique pulley. The oblique pulley can be identified by its fibers, which run at an angle relative to the transverse fibers of the A1 pulley. Preservation of the oblique pulley is non-negotiable to prevent FPL bowstringing.
Following the complete division of the A1 pulley, the adequacy of the release must be verified. The surgeon passively flexes and extends the IP joint of the thumb multiple times. The FPL tendon and Notta's nodule should glide smoothly without any residual catching, snapping, or triggering. Furthermore, the IP joint should achieve full passive extension. If full extension is not achieved, the surgeon must evaluate for an incomplete distal release of the A1 pulley or, in cases of chronic long-standing deformity, a secondary contracture of the volar plate. If the A1 pulley is fully released and a joint contracture persists, gentle passive manipulation is usually sufficient; aggressive volar plate release is rarely indicated in the primary setting.
Once the release is confirmed, the tourniquet is deflated, and meticulous hemostasis is achieved using bipolar electrocautery. The skin is closed using interrupted absorbable sutures (e.g., 5-0 or 6-0 plain gut or chromic gut) to eliminate the need for suture removal in an awake child. A soft, bulky, non-compressive dressing is applied.
Complications and Management
While A1 pulley release is generally a safe and highly successful procedure, complications can occur, primarily related to technical errors during dissection or incomplete release. Understanding these complications and their salvage strategies is essential for the operating surgeon.
| Complication | Estimated Incidence | Etiology and Clinical Presentation | Management and Salvage Strategies |
|---|---|---|---|
| Incomplete Release / Recurrence | 1% - 3% | Failure to completely divide the distal aspect of the A1 pulley. Presents as persistent triggering or recurrent locking post-operatively. | Revision surgery to complete the release. Careful assessment during the primary surgery to ensure smooth tendon glide is the best prevention. |
| Digital Nerve Injury | < 1% | Iatrogenic transection or traction neuropraxia of the radial digital nerve (most common) or ulnar digital nerve. Presents as sensory deficit along the affected border of the thumb. | Prevention via blunt longitudinal dissection. If transection is identified intraoperatively, immediate microsurgical epineurial repair is mandated. Neuropraxia generally resolves with observation. |
| FPL Bowstringing | < 1% | Iatrogenic transection of the oblique pulley. Presents as loss of IP joint flexion power, prominent tendon under the skin, and secondary MCP flexion contracture. | Pulley reconstruction using a free tendon graft (e.g., palmaris longus) or a slip of the extensor retinaculum. Requires advanced hand surgery techniques. |
| Wound Infection | 1% - 2% | Superficial surgical site infection. Presents with erythema, warmth, and purulent drainage. | Oral antibiotics covering common skin flora (Staphylococcus, Streptococcus). Local wound care. Deep infections requiring operative debridement are exceedingly rare. |
| Incisional Scar Contracture | Rare | Hypertrophic scarring or placement of a longitudinal incision directly across the flexion crease. | Scar massage and silicone gel sheeting. Severe contractures may require Z-plasty scar revision. |
Iatrogenic digital nerve injury represents the most devastating complication. The radial digital nerve's superficial and oblique course makes it particularly vulnerable. If a nerve injury is recognized intraoperatively, the tourniquet should be let down, and the nerve ends should be prepared for primary microsurgical repair using 8-0 or 9-0 nylon under microscopic magnification.
Post Operative Rehabilitation Protocols
The postoperative rehabilitation for a pediatric trigger thumb release is relatively straightforward, as children generally mobilize the digit intuitively once the mechanical block is removed and surgical pain subsides.
Immediately post-operatively, the thumb and hand are placed in a soft, bulky dressing. Rigid immobilization or splinting is not required and is generally discouraged, as early active motion helps prevent tendon adhesions. Parents are instructed to keep the dressing clean and dry.
The bulky dressing is typically removed at home by the parents or in the clinic at 5 to 7 days post-operatively. Once the dressing is removed, the child is encouraged to use the hand normally for age-appropriate play and activities. Formal physical therapy or occupational therapy is rarely indicated for primary trigger thumb releases.
In cases where a chronic, severe fixed flexion contracture was present preoperatively, the IP joint may not immediately achieve full active extension despite a complete A1 pulley release. This is due to adaptive shortening of the volar structures and weakness of the extensor pollicis longus (EPL) muscle from chronic disuse. In these specific scenarios, parents are instructed on gentle passive extension stretching exercises to be performed several times daily. If full active extension is not restored within 4 to 6 weeks, a nighttime extension splint and a brief course of targeted occupational therapy may be implemented.
Follow-up typically occurs at 2 weeks to assess wound healing and at 6 to 12 weeks to confirm the restoration of full active motion and the absence of triggering. Once normal kinematics are confirmed, the patient can be discharged from the surgical clinic.
Summary of Key Literature and Guidelines
The academic understanding and surgical management of pediatric trigger thumb have been shaped by several landmark studies that clarify its natural history, etiology, and optimal treatment algorithms.
Natural History and Observation:
Dinham and Meggitt's classic 1974 study in the Journal of Bone and Joint Surgery (British Volume) remains a foundational text. They observed that in children presenting before six months of age, up to 30% experienced spontaneous resolution without intervention. This established the paradigm of observation for infants. Subsequent studies have expanded this window, suggesting that observation up to 12-24 months is reasonable, provided the deformity is not rigidly fixed.
Etiology (Acquired vs. Congenital):
The debate regarding the congenital nature of the condition was largely settled by Baek et al. in their 2008 prospective study published in the Journal of Bone and Joint Surgery (American Volume). By screening over 2,000 newborns, they found zero cases of trigger thumb at birth, whereas the incidence rose significantly in the same cohort by age one. This robust epidemiological data firmly classifies the condition as an acquired developmental anomaly rather than a congenital defect.
Conservative Management:
The efficacy of extension splinting has been evaluated in numerous series. Lee et al. (2006) demonstrated that custom thermoplastic extension splinting of the IP joint, when applied in children under two years of age and worn consistently, could yield success rates approaching 70%. However, the compliance burden on parents is high, and failure rates increase significantly in older children or those with rigid contractures.
Surgical Outcomes:
Surgical release of the A1 pulley remains the gold standard for persistent or late-presenting cases. Large retrospective series consistently report success rates exceeding 95%, with minimal recurrence when the release is complete. The literature strongly emphasizes the anatomical variations of the radial digital nerve as the primary surgical pitfall. Current consensus guidelines recommend surgical intervention for children presenting with a locked trigger thumb after the age of 2 years, or for those who have failed a 3-to-6-month trial of conservative management.
