Distal Chevron Osteotomy: Essential Techniques for Success
Key Takeaway
For anyone wondering about Distal Chevron Osteotomy: Essential Techniques for Success, A distal chevron osteotomy is a surgical procedure primarily indicated for symptomatic hallux valgus deformity with moderate severity, typically when the intermetatarsal angle is less than 15 degrees. This V-shaped osteotomy near the metatarsal head corrects bone alignment and an abnormal distal metatarsal articular angle. Crucially, the plantar vascular supply must be preserved to minimize avascular necrosis risk.
As an Academic Orthopedic Surgeon and Medical Educator, I am pleased to present this comprehensive review of the distal chevron osteotomy, a cornerstone procedure in the surgical management of hallux valgus deformity. This document is intended as a high-yield reference for orthopedic surgeons, residents, and medical students, focusing strictly on scientific objectivity and best practices.
Introduction and Epidemiology
Hallux valgus, a complex deformity characterized by lateral deviation of the great toe and medial deviation of the first metatarsal, represents one of the most common forefoot pathologies encountered in orthopedic practice. Its prevalence is estimated to affect approximately 23% of adults aged 18-65, rising to 35% in those over 65 years, with a notable predilection for females. While often asymptomatic in its early stages, progressive deformity can lead to significant pain, functional impairment, difficulty with footwear, and secondary deformities such as hammertoes and metatarsalgia.
The distal chevron osteotomy, first described by Austin and Leventen in 1975, revolutionized the surgical approach to mild-to-moderate hallux valgus. Its introduction provided a reliable, reproducible technique for correcting intermetatarsal angle (IMA), hallux valgus angle (HVA), and distal metatarsal articular angle (DMAA) with a low incidence of complications, particularly avascular necrosis, which was a significant concern with earlier distal osteotomies. The procedure's enduring popularity stems from its biomechanical stability, robust fixation potential, and favorable long-term outcomes, making it a fundamental technique in the orthopedic surgeon's armamentarium for forefoot reconstruction.
Surgical Anatomy and Biomechanics
A thorough understanding of the intricate anatomy and biomechanics of the first metatarsophalangeal (MTP) joint is paramount for successful distal chevron osteotomy. The first MTP joint is a condyloid synovial joint, highly adapted for weight-bearing and propulsion.
Osseous Anatomy
The first metatarsal articulates proximally with the medial cuneiform and distally with the proximal phalanx of the great toe. Key anatomical landmarks include the metatarsal head, neck, and shaft. The articular surface of the metatarsal head is convex, with medial and lateral condyles separated by a sagittal sulcus, which accommodates the crista of the proximal phalanx. The presence of a prominent medial eminence is a hallmark of hallux valgus. The sesamoid bones (tibial and fibular) are embedded within the plantar plate and provide a mechanical advantage for the flexor hallucis brevis. Their position relative to the sagittal sulcus of the metatarsal head is a critical indicator of deformity severity and stability.
Ligamentous Structures
The first MTP joint capsule is reinforced by several critical ligaments. The medial collateral ligament (MCL) and lateral collateral ligament (LCL) provide mediolateral stability. The plantar plate, a fibrocartilaginous structure, reinforces the plantar aspect of the joint and is continuous with the flexor hallucis brevis tendons and sesamoids. In hallux valgus, the MCL is typically attenuated, while the LCL and adductor hallucis tendon become contracted, contributing to the hallux valgus deformity.
Musculature and Tendons
The intrinsic muscles of the foot play a vital role in stabilizing the first MTP joint. The abductor hallucis muscle and its tendon originate from the medial tuberosity of the calcaneus and insert on the medial base of the proximal phalanx and medial sesamoid. In hallux valgus, the abductor hallucis often displaces plantar-medially. The adductor hallucis muscle, comprising oblique and transverse heads, inserts on the lateral base of the proximal phalanx and lateral sesamoid. Its contracture contributes significantly to the lateral deviation of the hallux. The flexor hallucis brevis inserts via two heads onto the sesamoids and the base of the proximal phalanx. The extensor hallucis longus (EHL) and flexor hallucis longus (FHL) are extrinsic muscles that provide dynamic control.
Neurovascular Structures
The dorsal medial cutaneous nerve (DMCN), a branch of the superficial fibular nerve, courses along the dorsomedial aspect of the first metatarsal and is susceptible to iatrogenic injury during a medial approach. The plantar neurovascular bundle, supplying the great toe, lies deep and plantar to the first metatarsal head, underscoring the necessity for careful dissection during plantar osteotomy arm creation and deep soft tissue release.
Biomechanical Principles of Deformity
Hallux valgus is characterized by a multiplanar deformity involving first metatarsal adduction, internal rotation, and hallux abduction with a valgus rotation. The distal chevron osteotomy primarily corrects the first metatarsal adduction and the associated increase in IMA by laterally translating the metatarsal head. Rotational correction can also be achieved by altering the orientation of the osteotomy or the translation maneuver. Correction of DMAA is crucial to ensure a congruent joint post-translation and is typically achieved by rotating the capital fragment. The procedure aims to re-establish the normal mechanical axis of the first ray and realign the sesamoid apparatus beneath the metatarsal head.
Indications and Contraindications
The distal chevron osteotomy is indicated for symptomatic hallux valgus deformities, predominantly in the mild to moderate range. Careful patient selection is critical for achieving optimal outcomes.
Indications
The primary indication for a chevron osteotomy is symptomatic hallux valgus deformity with a moderate deformity, typically characterized by an intermetatarsal angle (IMA) of less than 15 degrees and a hallux valgus angle (HVA) of less than 30 degrees. The first metatarsocuneiform (MCJ) joint should be stable, as instability at this joint may necessitate a more proximal osteotomy or fusion. The osteotomy is highly effective in correcting an abnormal distal metatarsal articular angle (DMAA), either through intrinsic rotation of the capital fragment or by varying the osteotomy cut. It is used as a sole procedure in those presenting with minimal transfer symptoms and where the primary deformity is at the first MTP joint.
The procedure is also indicated for:
* Pain and difficulty with shoe wear
* Flexible hallux valgus deformity
* Congruent or reducible incongruent MTP joints
* Juvenile hallux valgus (with open physes, though modifications may be required)
Contraindications
Absolute contraindications include:
* Severe hallux valgus deformity (IMA > 18 degrees, HVA > 40 degrees) where the correction afforded by a chevron is insufficient.
* Advanced first MTP joint arthritis (Grade 3 or 4 Kellgren-Lawrence) which may necessitate an arthrodesis or arthroplasty.
* Significant first metatarsocuneiform joint instability or degenerative changes, which would compromise the stability of the first ray after distal osteotomy.
* Active infection.
* Peripheral vascular disease compromising healing.
* Neuropathic arthropathy.
* Non-compliance with postoperative rehabilitation.
* Unrealistic patient expectations.
Relative contraindications include:
* Older patients with osteopenia, where fixation may be challenging.
* Revision surgery for failed hallux valgus correction, depending on the prior procedure and residual deformity.
* Significant shortening of the first metatarsal, as translation can exacerbate this.
Operative vs. Non-Operative Indications
| Indication Type | Description | Considerations |
|---|---|---|
| Operative | Symptomatic hallux valgus (pain, difficulty with shoe wear) | Failure of conservative management |
| IMA 10-15 degrees | Primary indication for distal chevron | |
| HVA 20-30 degrees | Good correction achievable | |
| Abnormal DMAA | Correctable with rotational manipulation of capital fragment | |
| Flexible or reducible MTP joint | Allows for anatomical realignment | |
| Stable first TMT joint | Essential for durable correction | |
| Non-Operative | Asymptomatic hallux valgus | Surgical intervention not indicated for cosmetic reasons alone |
| Mild pain relieved by conservative measures | Wide toe-box shoes, orthotics, activity modification | |
| Severe deformity (IMA > 18, HVA > 35-40) | Chevron alone often insufficient; consider proximal osteotomy or fusion | |
| Advanced MTP arthritis (Grade 3-4) | Arthrodesis or arthroplasty more appropriate | |
| Unstable or arthritic first TMT joint | Requires different surgical strategy (e.g., Lapidus) | |
| Systemic comorbidities (e.g., severe PVD, neuropathy, immunocompromised) | Increased risk of complications |
Pre Operative Planning and Patient Positioning
Meticulous preoperative planning is critical to the success of a distal chevron osteotomy, encompassing detailed radiographic analysis, clinical evaluation, and precise patient positioning.
Preoperative Planning
Clinical Evaluation: A thorough history should elicit the patient's primary symptoms, their duration, and the impact on daily activities. Physical examination includes assessing the flexibility of the first MTP joint (reducible vs. fixed deformity), range of motion, presence of hypermobility at the first metatarsocuneiform joint, and evaluation for associated deformities (e.g., hammertoes, lesser metatarsalgia, tailor's bunion). Neurovascular status of the foot should be documented.
Radiographic Evaluation: Standard weight-bearing radiographs are indispensable. These include an anteroposterior (AP), lateral, and oblique view of the foot.
* AP View: Essential for evaluating:
* Intermetatarsal Angle (IMA): Angle between the first and second metatarsals. Normal is <9 degrees. Chevron is indicated for IMA 10-15 degrees.
* Hallux Valgus Angle (HVA): Angle between the first metatarsal and proximal phalanx. Normal is <15 degrees. Chevron for HVA 20-30 degrees.
* Distal Metatarsal Articular Angle (DMAA): Angle between the metatarsal articular surface and the longitudinal axis of the first metatarsal. A lateral deviation of this angle signifies an abnormal articular orientation (pes valgus/pronatus deformity) and requires rotational correction during the osteotomy.
* Sesamoid Position: Classified by Hardy and Clapham (I-VII) relative to the sagittal sulcus. Lateral subluxation (positions IV-VII) indicates soft tissue contracture and lateral deviation of the sesamoid apparatus.
* Congruity of the First MTP Joint: Assess for signs of arthritis, joint space narrowing, and osteophyte formation.
* Medial Eminence Size: Quantify the extent of the medial bunion.
* Metatarsal Length: While chevron typically does not significantly alter length, excessive shortening should be considered in planning.
* Lateral View: Evaluates metatarsal declination, plantarflexion/dorsiflexion of the first ray, and associated deformities.
* Oblique View: Useful for assessing the cuneiform-metatarsal joint for stability and arthritis.
For cases that may require a proximal phalangeal osteotomy (Akin osteotomy) to obtain complete correction, the interphalangeal angle (IPA) is assessed. If the hallux valgus interphalangeus angle is greater than 10 degrees, an Akin osteotomy should be considered.
Patient Positioning
Surgery is typically performed on an outpatient basis under regional anesthesia (ankle block) with or without conscious sedation, or general anesthesia.
* Prophylactic antibiotics covering skin flora (e.g., Cefazolin) are administered intravenously approximately 30-60 minutes prior to incision.
* A thigh tourniquet is applied to facilitate a bloodless field, which is crucial for precise soft tissue dissection and osteotomy execution. The tourniquet is inflated to 250-300 mmHg or 100 mmHg above systolic blood pressure.
* The patient is positioned supine on the operating table. A sandbag or small pillow is placed under the ipsilateral buttock to internally rotate the hip, ensuring the great toe points directly to the ceiling. This provides optimal access to the medial aspect of the foot and allows for accurate alignment during surgical maneuvers.
* The limb is prepped and draped in a sterile fashion from the knee to the toes, allowing ample space for instrumentation and visualization.
Detailed Surgical Approach and Technique
The distal chevron osteotomy involves a meticulous, step-by-step approach to ensure adequate deformity correction, stable fixation, and optimal soft tissue balance.
Surgical Incision and Exposure
The approach to the first metatarsal is through a medial longitudinal incision. This incision extends from a point approximately 1 cm proximal to the medial eminence distally to the medial flare of the proximal phalanx. The incision can be extended further distally if an Akin osteotomy of the proximal phalanx is anticipated.
Careful subcutaneous dissection is performed, and the dorsal medial cutaneous nerve (DMCN), a branch of the superficial fibular nerve, must be identified and protected. This nerve typically courses dorsomedially. Retraction should be gentle and precise to avoid neurapraxia.
The medial capsule of the first MTP joint is then sharply incised in a single longitudinal direction, typically along the mid-axis of the metatarsal shaft. This capsulotomy allows for full visualization of the medial eminence and the articular surface.

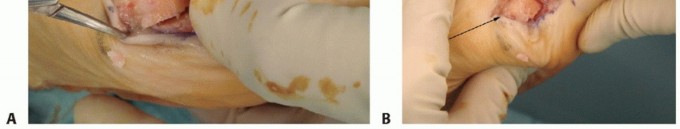
TECH FIG 1A illustrates the longitudinal medial capsular incision, revealing the underlying joint structures.
Medial Eminence Resection
Once the joint is exposed, the medial eminence, or "bunion," is resected. This is performed carefully, typically 1-2 mm medial to the sagittal sulcus of the metatarsal head, flush with the medial cortex. It is crucial to avoid over-resection, which can compromise the integrity of the medial collateral ligament attachment and lead to instability, or under-resection, which can result in residual prominence and recurrence of symptoms. An oscillating saw is generally used for this cut, ensuring a smooth surface.

TECH FIG 1B depicts the precise resection of the medial eminence, just medial to the sagittal sulcus.
Distal Soft Tissue Release (DSTR)
The extent of the DSTR depends on the reducibility of the deformity. For most chevron osteotomies, a lateral release is necessary to allow for adequate correction of the hallux valgus and realignment of the sesamoids. This is typically performed through the medial incision, accessing the lateral structures indirectly, or directly through a small first web space incision.
* Through the Medial Incision: The surgeon can identify the lateral collateral ligament and the adductor hallucis tendon insertion on the lateral base of the proximal phalanx. The release involves sequential division of:
1. The lateral sesamoid-phalangeal ligament.
2. The lateral head of the flexor hallucis brevis tendon sheath, to mobilize the fibular sesamoid.
3. The adductor hallucis tendon insertion from the lateral base of the proximal phalanx.
4. The lateral collateral ligament and a portion of the lateral joint capsule.
Care must be taken to avoid excessive stripping of the lateral metatarsal head soft tissues, which can jeopardize the blood supply to the capital fragment.
* Through a First Web Space Incision: A separate, small incision in the first web space allows for direct visualization and release of the adductor hallucis tendon and the lateral capsule. This approach can provide better exposure but adds another incision.
The most important part of the exposure, and particularly when performing a DSTR, is the identification and careful protection of the plantar neurovascular bundle to the hallux, which lies immediately deep and plantar to the metatarsal head.
Chevron Osteotomy Cuts
The chevron osteotomy involves making two osteotomy cuts that converge dorsally to form a 'V' shape.
1. Dorsal Arm: The first cut is typically made from dorsal-distal to plantar-proximal, entering the metatarsal head at the level of the dorsal articular cartilage and extending proximally for approximately 1-1.5 cm. The angle of this cut is usually around 60 degrees to the long axis of the metatarsal.
2. Plantar Arm: The second cut originates from the dorsal-proximal point of the first cut and extends plantar-distally, exiting the metatarsal head at a point just proximal to the plantar articular cartilage. The length of the plantar arm should be sufficient to allow for translation but not so long as to compromise stability or the plantar blood supply. The goal is to create a V-shaped osteotomy with an apex in the metatarsal shaft and arms exiting distally.

The saw blade should be kept perpendicular to the metatarsal shaft in the coronal plane to ensure accurate cuts. The dorsal apex of the osteotomy should be carefully identified to ensure proper bone purchase for fixation.

Image shows the osteotomy completed.
Translation and Rotational Correction
Once the osteotomy is complete, the distal capital fragment is translated laterally. The amount of lateral translation is critical for correcting the IMA. Typically, the fragment can be translated up to 50% of the width of the metatarsal shaft without compromising bone contact and stability. Excessive translation risks creating an unstable fragment and potentially disrupting the blood supply.

TECH FIG 1C (imagined) would illustrate the precise translation of the distal capital fragment laterally.
Rotational Correction for DMAA: If an abnormal DMAA is present, the capital fragment can be rotated around its dorsal apex prior to fixation. This involves slightly rotating the translated fragment such that the articular surface is more perpendicular to the long axis of the metatarsal, thereby improving joint congruity. The goal is to achieve a congruent first MTP joint with corrected IMA, HVA, and DMAA.
Fixation
Stable fixation of the osteotomy is paramount for early weight-bearing and predictable healing. Various methods are employed:
* K-wires: Traditionally used, particularly for smaller fragments or in situations where minimal compression is desired. Often two K-wires are inserted, typically from dorsal to plantar or oblique across the osteotomy.
* Cortical Screws: Small cortical screws (e.g., 2.0 mm or 2.7 mm) provide robust compression and stability. One or two screws can be placed. Common configurations include a single screw inserted from dorsal-proximal to plantar-distal across the osteotomy, or two screws placed obliquely.
* Headless Compression Screws: These screws offer excellent compression and typically sit flush or below the bone surface, reducing soft tissue irritation. They are often placed perpendicular to the osteotomy plane or from dorsal-proximal to plantar-distal.

This image likely depicts the insertion of a headless compression screw for fixation.

This image shows the distal capital fragment secured with two headless compression screws. The trajectory and position are critical for stable fixation.
The choice of fixation often depends on surgeon preference, bone quality, and the desired level of compression and stability. Intraoperative fluoroscopy can be used to confirm satisfactory alignment and hardware placement.
Capsular Repair and Closure
After satisfactory bone fixation, the medial capsule is imbricated (tightened) and repaired with absorbable sutures. This helps to maintain the correction, especially for the HVA, and reinforce the medial aspect of the joint. If a lateral release was performed, the lateral capsule is left open or loosely repaired to allow the new alignment to persist. The skin incision is then closed in layers, paying attention to aesthetics and avoiding tension.
Adjunctive Procedures
- Akin Osteotomy: If a significant hallux valgus interphalangeus (HVIP) exists (IPA > 10 degrees), an Akin osteotomy of the proximal phalanx is performed. This involves a medial closing wedge osteotomy at the base of the proximal phalanx, fixed with a staple or K-wire.
- Cheilectomy: If there is evidence of dorsal impingement or early dorsal osteophytes, a cheilectomy (excision of dorsal osteophytes) can be performed to improve joint motion.
- Sesamoidectomy: Rarely performed, only in cases of severe sesamoiditis or irreversible lateral subluxation that cannot be corrected with DSTR and metatarsal head repositioning.
- Gastrocnemius Recession: May be considered in cases of concurrent equinus deformity or limited ankle dorsiflexion, though less commonly associated with chevron.
Complications and Management
While the distal chevron osteotomy is generally considered safe and effective, like any surgical procedure, it is associated with potential complications. Awareness of these risks and strategies for management is crucial.
Common Complications
| Complication | Incidence | Description | Salvage / Management Strategy |
|---|---|---|---|
| Recurrence of Hallux Valgus | 5-15% | Return of hallux valgus deformity, often due to inadequate initial correction, insufficient DSTR, unstable fixation, or patient non-compliance. | Revision surgery (e.g., repeat chevron, Scarf osteotomy, Lapidus arthrodesis for proximal instability, or MTP fusion for severe recurrence/arthritis), re-evaluate underlying causes (e.g., TMT hypermobility). |
| Metatarsalgia (Transfer) | 5-10% | Pain under the lesser metatarsal heads, typically the second or third, due to excessive shortening or elevation of the first metatarsal, leading to increased pressure transfer. | Orthotics with metatarsal pads, shoe modifications. If severe and persistent, lesser metatarsal osteotomies (e.g., Weil osteotomy) or first metatarsal lengthening osteotomy (rare) if shortening is significant. |
| Avascular Necrosis (AVN) | <1-3% | Ischemic necrosis of the metatarsal head, primarily due to disruption of the blood supply during dissection (e.g., stripping the lateral soft tissues) or aggressive osteotomy. Presents as pain, stiffness, and radiographic collapse. | Conservative management (rest, protected weight-bearing) for mild cases. If severe collapse, debridement and grafting, or MTP fusion. |
| Nonunion / Delayed Union | <1-2% | Failure of the osteotomy to heal within 6 months. Risk factors include poor bone quality, unstable fixation, infection, or excessive translation. | Protected weight-bearing, bone stimulators. If persistent, revision surgery with decortication, bone grafting, and rigid internal fixation. |
| Malunion | 2-5% | Healing of the osteotomy in an incorrect position (e.g., dorsal malunion causing metatarsalgia, inadequate correction, or excessive shortening/lengthening). | Revision osteotomy to correct the deformity, potentially with bone grafting if bone loss has occurred. |
| Stiffness / Limited ROM | 5-10% | Restricted range of motion at the first MTP joint, often due to capsular scarring, inadequate early mobilization, or joint incongruity. | Early physical therapy, gentle manipulation. If persistent, MTP arthrolysis or cheilectomy. |
| Hardware-Related Issues | 5-10% | Screw prominence, irritation, or breakage. Can cause pain, inflammation, or soft tissue impingement. | Hardware removal once osteotomy is healed. Revision fixation if osteotomy has not healed and hardware fails. |
| Nerve Injury | 2-5% | Injury to the dorsal medial cutaneous nerve (DMCN), leading to numbness, paresthesia, or painful neuroma. Less commonly, superficial fibular or saphenous nerve injury. | Conservative management for neurapraxia. If persistent or painful neuroma, local injection, surgical neurolysis, or neurectomy. |
| Infection | <1% | Superficial or deep surgical site infection. Risk factors include poor wound healing, immunosuppression, or prolonged surgery. | Superficial: Oral antibiotics, local wound care. Deep: Surgical debridement, intravenous antibiotics, possible hardware removal and reimplantation if infection persists after initial treatment. |
| Overcorrection (Hallux Varus) | <1% | Rare but debilitating, where the hallux deviates medially. Often due to excessive lateral soft tissue release and/or over-correction of the metatarsal. | Early detection and bracing. If severe and symptomatic, revision surgery with medial capsular release, lateral capsular imbrication, or reverse Akin osteotomy. In severe cases, MTP fusion. |
General Management Principles
- Early Recognition: Prompt identification of complications is crucial for effective management.
- Conservative Measures First: For many complications (e.g., mild metatarsalgia, early stiffness, mild nerve symptoms), non-surgical interventions are the initial approach.
- Revision Surgery: When conservative measures fail, or for severe complications like nonunion or significant recurrence, revision surgery tailored to the specific pathology is indicated.
- Patient Education: Thoroughly educating patients preoperatively about potential complications and realistic outcomes can manage expectations and improve compliance with postoperative protocols.
Post Operative Rehabilitation Protocols
A structured and progressive rehabilitation protocol is integral to achieving a successful outcome following a distal chevron osteotomy. The goal is to minimize pain and swelling, protect the osteotomy, restore range of motion, and gradually return to full activity.
Immediate Postoperative Period (Weeks 0-2)
- Weight-Bearing: Immediate partial weight-bearing (PWB) is often initiated in a rigid postoperative shoe or walking boot, flat-soled. The primary goal is to protect the osteotomy site.
- Dressings: A bulky dressing with cotton padding between the toes (e.g., 'buddy taping' the great toe to the second toe in a corrected position) is applied to maintain the hallux position and reduce swelling. This dressing is typically changed at the first follow-up.
- Elevation and Ice: Strict elevation of the foot above heart level for the first 48-72 hours, along with intermittent icing, is crucial to minimize swelling and pain.
- Pain Management: Oral analgesics (NSAIDs, acetaminophen, opioids if necessary) are prescribed.
- Mobility: Non-weight-bearing exercises for the ankle and knee are encouraged. Wiggle toes of the lesser digits. Gentle passive range of motion (PROM) for the first MTP joint may be initiated, depending on surgeon preference and fixation stability, usually after the first week.
Early Rehabilitation Phase (Weeks 2-6)
- Weight-Bearing: Progressive weight-bearing in the rigid sole shoe or walking boot.
- Dressing Changes: Continue with toe spacers or buddy taping.
- Physical Therapy (PT): May begin around week 2-3.
- Range of Motion: Focus on active and passive range of motion (AROM/PROM) for the first MTP joint, emphasizing dorsiflexion and plantarflexion. Avoid aggressive inversion/eversion.
- Swelling Management: Continue elevation, icing, and consider compression stockings.
- Soft Tissue Mobilization: Gentle massage around the incision once healed.
- Activity: Avoid high-impact activities, prolonged standing, or strenuous exercise.
Intermediate Rehabilitation Phase (Weeks 6-12)
- Weight-Bearing: Transition out of the surgical shoe/boot into wide, comfortable, supportive athletic shoes.
- PT Progression:
- Strengthening: Initiate gentle strengthening exercises for the intrinsic and extrinsic foot muscles (e.g., toe curls, towel scrunches, marble pick-ups, calf raises).
- Balance and Proprioception: Incorporate balance exercises (e.g., single-leg stance, wobble board).
- Gait Training: Focus on restoring a normal heel-to-toe gait pattern.
- Activity: Gradually increase walking distance and duration. Low-impact activities like swimming or cycling may be introduced.
Advanced Rehabilitation and Return to Activity (Weeks 12 onwards)
- Footwear: Patients can generally return to more varied footwear, emphasizing good arch support and adequate toe box width. High heels should be introduced cautiously and are generally discouraged long-term.
- PT Progression:
- Functional Training: Progress to sport-specific drills or activities relevant to the patient's lifestyle.
- Advanced Strengthening: Plyometric exercises if appropriate.
- Return to Sport: Gradual return to sports and high-impact activities usually begins at 3-6 months, depending on healing, pain levels, and functional recovery. Full return may take 6 months to a year.
- Long-Term Considerations: Continue with supportive footwear. Regular follow-up for radiographic assessment of healing and alignment.
The specific timeline and intensity of rehabilitation may be adjusted based on the individual patient's healing capacity, bone quality, stability of fixation, and presence of any complications. Close communication between the surgeon and physical therapist is essential for optimizing recovery.
Summary of Key Literature and Guidelines
The distal chevron osteotomy has been extensively studied since its inception, establishing its role as a reliable and effective procedure for mild-to-moderate hallux valgus deformity.
Efficacy and Outcomes
Numerous studies have consistently demonstrated good-to-excellent clinical and radiographic outcomes following distal chevron osteotomy. A meta-analysis by Politi et al. (2014) reported an average HVA correction of 15-20 degrees and IMA correction of 5-8 degrees, with high patient satisfaction rates (typically >85%) and low complication rates. Long-term follow-up studies (e.g., by Kitaoka et al., 2001) have confirmed the durability of the correction, although some degree of recurrence or loss of correction can occur over decades.
Comparison with Other Osteotomies
- Scarf Osteotomy: For moderate-to-severe deformities, the Scarf osteotomy often provides greater correctional power and allows for simultaneous metatarsal shortening, lengthening, and multiplanar correction. While technically more demanding, studies comparing Scarf and chevron for similar deformities show comparable clinical outcomes, with the Scarf potentially offering greater flexibility in correction.
- Proximal Metatarsal Osteotomies (e.g., Ludloff, Crescentic): These are generally reserved for more severe deformities or cases with TMT joint instability, where correction needs to be achieved more proximally. They carry a higher risk of nonunion or delayed union due to larger osteotomy surfaces and often require more rigid fixation and prolonged protected weight-bearing.
- Lapidus Arthrodesis: Indicated for severe hallux valgus, particularly with first TMT joint hypermobility or arthritis. It provides powerful, stable, and durable correction but involves a fusion, leading to a longer non-weight-bearing period.
Current guidelines generally advocate for the distal chevron osteotomy as the first-line surgical option for flexible, mild-to-moderate hallux valgus without significant first TMT joint pathology. Its advantages include good stability, low risk of AVN, predictable correction, and enabling early weight-bearing.
Technical Considerations and Refinements
Literature highlights several key technical considerations:
* DMAA Correction: Recognition and correction of an elevated DMAA, often through appropriate rotation of the capital fragment, are crucial for achieving a congruent joint and preventing recurrence.
* Distal Soft Tissue Release: The importance of an adequate, but not excessive, lateral soft tissue release to allow for complete correction of the hallux valgus deformity and sesamoid repositioning is consistently emphasized. Over-release can lead to hallux varus.
* Fixation: While K-wires remain an option, the trend towards rigid internal fixation (e.g., headless compression screws) is supported by studies demonstrating improved stability, earlier weight-bearing, and reduced incidence of loss of correction.
* Combined Procedures: The frequent need for adjunctive procedures, particularly an Akin osteotomy, to address concomitant hallux valgus interphalangeus is well-documented.
In conclusion, the distal chevron osteotomy remains a highly effective and well-established procedure for the correction of mild-to-moderate hallux valgus. Its success hinges on meticulous preoperative planning, precise surgical technique, appropriate soft tissue balancing, and adherence to a structured postoperative rehabilitation protocol. Continued advancements in imaging, instrumentation, and understanding of forefoot biomechanics further refine its application and enhance patient outcomes.
Clinical & Radiographic Imaging


You Might Also Like


