Chevron-Type Medial Malleolar Osteotomy: An Intraoperative Masterclass for Talar Dome Lesion Exposure
Key Takeaway
Join us in the OR for a detailed masterclass on the chevron-type medial malleolar osteotomy. This technique provides unparalleled exposure for posteromedial talar dome lesions. We'll meticulously cover preoperative planning, patient positioning, intricate surgical anatomy, step-by-step execution, critical pearls to avoid pitfalls, and comprehensive postoperative care, ensuring optimal outcomes for complex ankle pathologies.
Comprehensive Introduction and Patho-Epidemiology
The management of complex talar dome pathology remains one of the most formidable challenges in orthopedic foot and ankle surgery. When addressing elusive, centrally or posteromedially located lesions of the talar dome, standard arthroscopic techniques and conventional arthrotomies frequently fall short, failing to provide the perpendicular access required for definitive cartilage restoration or fracture fixation. The chevron-type medial malleolar osteotomy has emerged as the gold-standard extensile approach, offering unparalleled, uncompromised visualization of the medial and central tibiotalar joint. This procedure is not undertaken lightly; it is a meticulously planned intervention reserved for pathologies that demand direct, wide exposure, such as comminuted talar body fractures, massive osteochondral lesions of the talus (OCLTs), and complex intra-articular reconstructive efforts.
The patho-epidemiology of talar dome lesions heavily dictates the necessity of this approach. Osteochondral lesions of the talus frequently occur secondary to traumatic ankle inversion or eversion injuries, leading to shear forces that disrupt the articular cartilage and underlying subchondral bone. While anterolateral lesions are typically shallow and more easily accessed via standard arthroscopy, posteromedial lesions tend to be deeper, more morphologically complex, and heavily obscured by the medial malleolus and the curvature of the tibial plafond. When these lesions progress to subchondral cyst formation or structural collapse, simple marrow stimulation techniques are inadequate. Advanced cartilage restoration techniques, such as osteochondral autograft transfer systems (OATS) or bulk structural allografts, require precise, perpendicular instrumentation—a geometric impossibility without mobilizing the medial malleolus.
The evolution of the medial malleolar osteotomy has seen various configurations, including transverse, oblique, and step-cut designs. However, the chevron-type osteotomy is biomechanically superior and is widely considered the optimal technique. The inverted "V" configuration of the chevron cut provides intrinsic multiplanar stability, effectively resisting anterior-posterior translation and rotational forces during the healing phase. Furthermore, the chevron geometry significantly increases the surface area of the osteotomy site compared to a simple transverse cut, thereby enhancing the biologic potential for rapid bony union. By mastering this specific osteotomy, the orthopedic surgeon gains a powerful, reproducible tool that maximizes intra-articular exposure while minimizing the risk of postoperative nonunion or malunion.
Despite its biomechanical advantages, the chevron medial malleolar osteotomy requires profound respect for the surrounding soft tissue envelope and articular congruity. The procedure introduces iatrogenic trauma to the joint space and necessitates a period of postoperative immobilization that must be carefully balanced against the need for early articular mobilization. Potential disadvantages include the risk of delayed union, degenerative ankle arthrosis due to malreduction, and the frequent necessity for subsequent hardware removal due to symptomatic prominence. Therefore, the execution of this procedure demands an intraoperative masterclass in precision, from the initial preoperative templating to the final compression of the osteotomy site.
Detailed Surgical Anatomy and Biomechanics
A profound understanding of the medial ankle's surgical anatomy is the absolute prerequisite for executing the chevron medial malleolar osteotomy safely and effectively. The medial malleolus serves as the distal-most extension of the tibia, providing critical medial restraint to the ankle mortise. Its medial surface is entirely subcutaneous, rendering it highly accessible but also susceptible to wound healing complications and hardware prominence. The lateral surface of the malleolus is covered in hyaline cartilage and articulates directly with the medial facet of the talus. The precise spatial relationship between the medial malleolus, the tibial plafond, and the talar dome must be conceptualized in three dimensions to plan an osteotomy that avoids iatrogenic damage to the primary weight-bearing articular surfaces.
Posterior to the medial malleolus lies the malleolar sulcus, a critical anatomical corridor housing the tendons of the deep posterior compartment of the leg. Immediately posterior to the malleolus is the posterior tibialis tendon, followed closely by the flexor digitorum longus (FDL) tendon. The flexor hallucis longus (FHL) tendon is located further posteriorly and deeper, resting in its own groove on the posterior aspect of the talus. During the osteotomy and subsequent retraction, the posterior tibialis tendon is at significant risk of iatrogenic laceration from the oscillating saw. Meticulous subperiosteal dissection and the placement of protective retractors within the tendon sheath are mandatory steps to safeguard these dynamic stabilizers of the foot and ankle.
The deltoid ligament complex is arguably the most critical soft-tissue structure involved in this procedure. It is divided into superficial and deep components. The superficial deltoid originates from the anterior colliculus of the medial malleolus and fans out to insert on the navicular, spring ligament, and calcaneus. The deep deltoid, which is the primary medial stabilizer of the ankle, originates from the posterior colliculus and intercollicular groove, inserting directly onto the medial surface of the talus. The fundamental principle of the medial malleolar osteotomy is to utilize the deep deltoid ligament as a robust, vascularized hinge. By leaving the distal attachments of the deltoid intact and carefully reflecting the osteotomized fragment inferiorly, the surgeon preserves the critical intraosseous and extraosseous blood supply to the malleolar fragment, drastically reducing the risk of avascular necrosis and nonunion.
Neurovascular considerations are equally paramount. The saphenous nerve and the great saphenous vein course along the anteromedial aspect of the ankle, often crossing directly over the planned incision site. The saphenous nerve is purely sensory, supplying the medial aspect of the foot and ankle. Iatrogenic transection or aggressive retraction can lead to devastating neuropathic pain, complex regional pain syndrome (CRPS), or symptomatic neuromas that overshadow the success of the intra-articular procedure. Posteriorly, the posterior tibial neurovascular bundle (comprising the posterior tibial artery, vein, and nerve) lies deep to the flexor retinaculum. While generally protected during a standard medial approach, over-penetration of the drill bit or oscillating saw during the posterior limb of the chevron cut can plunge into this neurovascular bundle, leading to catastrophic hemorrhagic or neurologic complications.
Exhaustive Indications and Contraindications
The decision to proceed with a chevron medial malleolar osteotomy must be based on a rigorous evaluation of the patient's pathology, functional demands, and overall medical optimization. This extensile approach is not a first-line intervention; it is a definitive surgical maneuver utilized when less invasive techniques have failed or are anatomically precluded. The primary indication is the presence of a large, deep, or morphologically complex osteochondral lesion of the talus (OCLT) located in the central or posteromedial aspect of the talar dome. Lesions exceeding 1.5 centimeters in diameter, those associated with massive subchondral cystic changes, or those that have failed prior arthroscopic marrow stimulation (microfracture) require structural grafting. Techniques such as osteochondral autograft transfer (OATS), fresh osteochondral allograft transplantation, or autologous chondrocyte implantation (ACI) necessitate strict perpendicular access to the talar dome to ensure flush graft seating and optimal integration, making the malleolar osteotomy indispensable.
Beyond cartilage restoration, the chevron medial malleolar osteotomy is frequently indicated in the realm of complex orthopedic trauma. Comminuted fractures of the talar body or complex talar neck fractures with posterior extension often defy adequate visualization through standard anteromedial or anterolateral arthrotomies. The osteotomy allows the surgeon to "open the book" of the ankle joint, providing a panoramic view of the talar articular surface. This exposure is critical for the meticulous debridement of intra-articular fracture fragments, the anatomic reduction of the articular surface, and the precise placement of interfragmentary fixation. Furthermore, in cases of chronic, neglected ankle fractures or malunions requiring intra-articular corrective osteotomies, the medial approach provides the necessary working space to execute complex reconstructive geometries.
Despite its utility, several strict contraindications exist that must preclude the use of this approach. Absolute contraindications include the presence of active, untreated localized or systemic infection, which would invariably seed the osteotomy site and the pristine intra-articular space. Severe peripheral vascular disease (PVD) is another absolute contraindication; the medial malleolar skin envelope is notoriously tenuous, and compromised vascularity will predictably lead to wound dehiscence, exposed hardware, and deep infection. Neuropathic arthropathy (Charcot joint), particularly in the setting of uncontrolled diabetes mellitus, represents a severe relative-to-absolute contraindication due to the profoundly compromised bone healing capacity and the high likelihood of catastrophic hardware failure and osteotomy nonunion.
Relative contraindications revolve around patient compliance and the presence of underlying degenerative joint disease. Patients who are unable or unwilling to adhere to a strict, prolonged non-weight-bearing postoperative protocol are at a high risk for early hardware failure and displacement of the osteotomy. Additionally, if preoperative imaging reveals advanced, widespread tibiotalar osteoarthritis (e.g., Kellgren-Lawrence grade 3 or 4), performing an extensile osteotomy to address a focal talar lesion is generally futile. In such end-stage scenarios, definitive salvage procedures, such as ankle arthrodesis or total ankle arthroplasty, should be considered instead of focal cartilage restoration via an osteotomy.
Indications and Contraindications Summary
| Category | Specific Conditions | Rationale / Clinical Context |
|---|---|---|
| Absolute Indications | Massive posteromedial OCLTs (>1.5cm) | Requires perpendicular access for OATS or bulk allograft. |
| Absolute Indications | Comminuted Talar Body Fractures | Necessitates panoramic visualization for anatomic articular reduction. |
| Relative Indications | Failed prior arthroscopic microfracture | Revision procedures require structural grafting and debridement. |
| Absolute Contraindications | Active localized soft tissue infection | High risk of seeding the joint space and osteotomy site. |
| Absolute Contraindications | Severe Peripheral Vascular Disease (PVD) | Predictable wound necrosis and failure of osteotomy healing. |
| Relative Contraindications | Uncontrolled Diabetes / Charcot Arthropathy | High risk of nonunion, hardware failure, and progressive collapse. |
Pre-Operative Planning, Templating, and Patient Positioning
Thorough preoperative planning is the cornerstone of a successful chevron medial malleolar osteotomy. This phase begins with a comprehensive suite of imaging modalities to precisely define the underlying pathology and map the surgical approach. Standard weight-bearing radiographs of the ankle (anteroposterior, lateral, and mortise views) are obtained to assess overall joint alignment, joint space narrowing, and the presence of osteophytes. However, standard radiography is insufficient for the three-dimensional planning required for this procedure. Magnetic Resonance Imaging (MRI) is mandatory for evaluating osteochondral lesions; specific sequences, particularly T2-weighted fat-suppressed and T1-weighted images, provide critical data regarding the surface area of the cartilage defect, the depth of subchondral bone involvement, and the presence of underlying bone marrow edema or cystic degeneration.
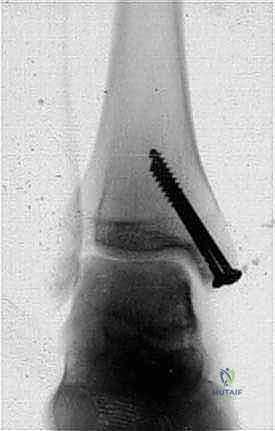
Computed Tomography (CT) scanning is arguably the most critical tool for the mechanical templating of the osteotomy. A fine-cut CT scan with multiplanar reconstructions and 3D rendering allows the surgeon to visualize the exact location of the talar lesion relative to the medial malleolus. During the templating phase, the surgeon must determine the precise apex of the chevron cut. The apex should be directed proximally and located at the junction of the medial malleolus and the tibial plafond, ensuring that the osteotomy exits into the "axilla" of the ankle mortise without violating the weight-bearing horizontal articular surface of the tibia. The limbs of the chevron are typically templated at an angle of 90 to 110 degrees relative to each other, optimizing both the surface area for healing and the intrinsic stability of the fragment.
Patient positioning and operating room setup must be meticulously orchestrated to facilitate seamless intraoperative workflow. The patient is placed in the supine position on a radiolucent operating table. A bump is placed under the ipsilateral hip to internally rotate the leg slightly, bringing the medial malleolus directly towards the ceiling and optimizing the surgeon's working trajectory. A well-padded thigh tourniquet is applied to ensure a completely bloodless surgical field, which is an absolute necessity for identifying delicate neurovascular structures and visualizing the subtle transition between cartilage and subchondral bone. The limb is prepped and draped in a standard sterile fashion, ensuring exposure from the proximal tibia down to the toes to allow for dynamic manipulation of the foot and ankle during the procedure.
Fluoroscopy positioning is a critical logistical component that must be finalized before the initial incision. The C-arm should be positioned on the contralateral side of the table, entering perpendicular to the operative field. The surgeon must verify that perfect anteroposterior, mortise, and lateral views of the ankle can be obtained effortlessly without compromising the sterile field or requiring awkward maneuvering of the leg. The monitor should be placed directly across from the primary surgeon for optimal ergonomics. Establishing this fluoroscopic workflow preoperatively prevents intraoperative delays and ensures that the critical predrilling and osteotomy steps are executed with absolute radiographic precision.
Step-by-Step Surgical Approach and Fixation Technique
Incision, Superficial Dissection, and Nerve Protection
The surgical approach begins with a meticulously planned longitudinal or slightly curvilinear incision centered over the medial malleolus. The incision typically starts 4 to 5 centimeters proximal to the tip of the malleolus and extends distally, curving gently toward the medial cuneiform or navicular tuberosity. As the skin is incised, the surgeon must immediately transition to blunt dissection utilizing hemostats or Metzenbaum scissors. The superficial fascia in this region is thin, and the great saphenous vein and saphenous nerve lie immediately beneath it, usually crossing the proximal third of the incision from anterior to posterior.

Identification and mobilization of the saphenous neurovascular bundle are mandatory before proceeding to deeper layers. Once identified, the vein and nerve are gently mobilized together and retracted anteriorly using a vessel loop. Aggressive traction must be avoided to prevent neuropraxia. Following the protection of these superficial structures, the deep fascia overlying the medial malleolus is incised longitudinally. A periosteal elevator is then utilized to create full-thickness anterior and posterior fascioperiosteal flaps. This subperiosteal dissection must expose the entire medial face of the malleolus, extending anteriorly to the joint capsule and posteriorly to the malleolar sulcus, providing a clear canvas for the planned osteotomy.
Deep Dissection and Tendon Management
With the medial malleolus exposed, attention must turn to the posterior structures, specifically the posterior tibialis tendon (PTT). The PTT lies in the malleolar sulcus directly posterior to the bone and is at extreme risk during the posterior limb of the chevron saw cut. The surgeon must carefully incise the flexor retinaculum and open the tendon sheath of the PTT. Using a blunt instrument, the tendon is mobilized from its groove. A small, smooth Hohmann retractor or a flexible malleable retractor is then placed carefully between the posterior aspect of the medial malleolus and the PTT.
This retractor serves a dual purpose: it physically displaces the tendon posteriorly, shielding it from the oscillating saw, and it provides a tactile backstop for the surgeon, indicating when the saw blade has breached the posterior cortex of the malleolus. It is imperative that the retractor is placed gently to avoid crushing the tendon or compressing the more posteriorly located posterior tibial neurovascular bundle. The anterior aspect of the joint capsule is also minimally elevated to expose the anterior joint line, allowing the surgeon to visually confirm the level of the tibial plafond, which is critical for determining the apex of the osteotomy.
The Critical Step: Predrilling for Fixation
Perhaps the most vital technical pearl of the entire procedure is the predrilling of the fixation hardware trajectories prior to executing the osteotomy. Attempting to drill and tap a mobile, osteotomized malleolar fragment anatomically is notoriously difficult and frequently leads to malreduction, articular step-off, and loss of compression. While the medial malleolus is still in its native, contiguous state, the surgeon uses fluoroscopic guidance to plan the placement of two lag screws. Typically, 4.0-mm partially threaded cancellous screws or 3.5-mm cortical screws utilized in a lag fashion are selected for fixation.
Under multiplanar fluoroscopy, a 2.5-mm drill bit is advanced from the distal tip of the medial malleolus, directed proximally and slightly laterally, aiming perpendicular to the planned limbs of the chevron cut. Two divergent drill holes are created, ensuring they cross the planned osteotomy site and achieve adequate purchase in the dense metaphyseal bone of the distal tibia. The depth of these holes is measured, and if non-cannulated, fully threaded screws are to be used, the near cortex (the malleolar fragment) is overdrilled to the core diameter of the screw (e.g., 3.5mm or 4.0mm) to ensure a true interfragmentary lag effect upon final fixation. This predrilling step guarantees that when the fragment is reduced later, the screws will follow their exact native tracks, forcing the fragment back into perfect anatomic alignment.
Executing the Chevron Osteotomy
With the soft tissues protected and the fixation tracks predrilled, the surgeon proceeds with the chevron osteotomy. The apex of the chevron is marked with a sterile pen or a shallow score line using a scalpel, typically located 1 to 2 centimeters proximal to the joint line, aiming directly into the axilla of the mortise. Using a fine-toothed microsagittal saw under continuous saline irrigation to prevent thermal necrosis, the surgeon creates the anterior and posterior limbs of the inverted "V". The saw blade must be kept strictly perpendicular to the medial cortex in the sagittal plane to prevent creating an oblique cut that could slide or displace upon compression.
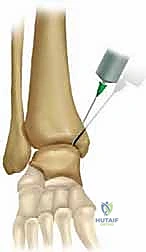
A critical biomechanical concept during this step is the avoidance of the "Kerf" effect. The saw blade has an inherent thickness (typically 1 to 1.5 mm). If the surgeon saws completely through the subchondral bone and articular cartilage, this 1.5 mm of bone is permanently lost. Upon reduction and compression, the loss of this bone stock will inevitably create an incongruous articular step-off, leading to rapid, focal joint degeneration. To prevent this, the surgeon must stop the saw cuts approximately 2 to 3 millimeters short of the articular cartilage.
Osteoclasis, Retraction, and Pathologic Intervention
Once the saw cuts are nearly complete, the surgeon switches to a fine, sharp osteotome. The osteotome is gently inserted into the apex of the chevron cut and tapped lightly with a mallet. By applying controlled leverage, the remaining subchondral bone bridge and the articular cartilage are fractured (osteoclasis). This creates a rough, interdigitating fracture line through the cartilage rather than a smooth saw cut. Because no bone is removed by the saw at the articular level, anatomic reduction will result in a perfectly congruous joint surface with zero step-off.
Following osteoclasis, a sharp bone hook or a towel clip is placed into the distal aspect of the medial malleolus. The fragment is gently reflected inferiorly, opening the ankle joint like a book. During this retraction, the surgeon must meticulously preserve the deep deltoid ligament attachments to the medial talus and the osteotomized fragment. This vascularized hinge is the lifeline of the bone flap. With the malleolus reflected, the surgeon now has uninhibited, perpendicular access to the central and posteromedial talar dome to execute the planned cartilage restoration (e.g., OATS, massive allografting) or fracture fixation.
Anatomic Reduction and Final Fixation
Following the definitive treatment of the intra-articular pathology, the joint is thoroughly irrigated to remove any cartilaginous debris, bone dust, or loose bodies. The medial malleolar fragment is then manually reduced back into its anatomic bed. Because of the rough, interdigitating nature of the osteoclasis at the articular surface, the fragment will typically "lock" into its native position. A large, pointed reduction forceps (Weber clamp) is applied, with one tine on the distal tip of the malleolus and the other on the proximal tibial metaphysis, to apply rigid compression across the osteotomy site.
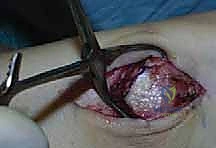
With the fragment held securely, the previously selected lag screws are inserted into the predrilled tracks. As the screws are tightened, the surgeon should visually and tactilely confirm interfragmentary compression at the osteotomy site. Fluoroscopy is utilized in the anteroposterior, lateral, and mortise planes to verify the anatomic reduction of the medial clear space, the perfect congruity of the tibial plafond, and the appropriate length and trajectory of the hardware. The periosteum, deep fascia, and superficial skin layers are then meticulously closed in a layered fashion over a closed suction drain to prevent hematoma formation.
Complications, Incidence Rates, and Salvage Management
While the chevron medial malleolar osteotomy provides unparalleled access, it is an inherently invasive procedure carrying a distinct profile of potential complications. The most dreaded complication is the nonunion or delayed union of the osteotomy site. Historically, transverse osteotomies carried nonunion rates approaching 10%. However, the chevron configuration, due to its increased surface area and intrinsic rotational stability, has reduced this incidence to approximately 2-5% in appropriately selected patients. Risk factors for nonunion include smoking, diabetes, aggressive stripping of the deltoid ligament (compromising the vascular hinge), and thermal necrosis from the oscillating saw. Management of a symptomatic nonunion typically requires revision surgery with hardware exchange, aggressive decortication of the nonunion site, and the application of autologous bone graft or orthobiologics.
Hardware prominence is the most frequent postoperative complaint, occurring in up to 30% of patients. The medial malleolus is entirely subcutaneous, and the heads of the fixation screws, even when countersunk, can cause significant irritation, particularly in patients wearing rigid footwear or athletic boots. Symptomatic hardware typically presents as localized pain, erythema, and palpable prominence directly over the screw heads, usually manifesting 6 to 12 months postoperatively after the surrounding edema has subsided. The management is straightforward: elective hardware removal once radiographic union is definitively confirmed, typically no earlier than 6 to 9 months post-index procedure.
Articular step-off and subsequent secondary osteoarthritis represent a technical failure of the procedure. If the surgeon fails to respect the "Kerf" effect and saws directly through the articular cartilage, or if the predrilled tracks are lost, malreduction of the malleolus will occur. Even a 1-millimeter step-off in the weight-bearing tibiotalar joint drastically alters contact mechanics, leading to accelerated wear of the talar dome. Salvage for early symptomatic malreduction may require a corrective intra-articular osteotomy, while late presentation with end-stage degenerative changes will necessitate an ankle arthrodesis or total ankle arthroplasty.
Neurologic complications, specifically saphenous neuritis or neuroma formation, occur in approximately 5-10% of cases. Iatrogenic injury during the initial incision or aggressive retraction of the superficial tissues can damage the saphenous nerve. Patients present with burning, neuropathic pain, hyperesthesia, or a positive Tinel's sign over the medial ankle. Initial management includes neuropathic pain modulators (e.g., gabapentin, pregabalin) and targeted corticosteroid injections. Refractory neuromas may require surgical exploration, neuroma excision, and burying of the proximal nerve stump deep into the muscular fascia to prevent recurrence.
Complications and Management Summary
| Complication | Estimated Incidence | Primary Etiology / Risk Factors | Salvage / Management Strategy |
|---|---|---|---|
| Hardware Prominence | 20 - 30% | Subcutaneous nature of medial malleolus; inadequate countersinking. | Elective hardware removal after definitive radiographic union (6-9 months). |
| Saphenous Neuritis | 5 - 10% | Iatrogenic traction or transection during superficial dissection. | Neuromodulators, targeted injections; surgical neuroma excision and burying. |
| Nonunion / Delayed Union | 2 - 5% | Smoking, thermal necrosis, disruption of deltoid vascular hinge. | Revision ORIF with autologous bone grafting and orthobiologic augmentation. |
| Articular Step-off / OA | < 5% | Failure to use osteoclasis (Kerf effect); loss of predrilled tracks. | Early: Corrective osteotomy. Late: Ankle arthrodesis or Arthroplasty. |
Phased Post-Operative Rehabilitation Protocols
The postoperative rehabilitation following a chevron medial malleolar osteotomy must be meticulously phased to balance two competing biological demands: the absolute necessity of rigid immobilization to allow the bone osteotomy to heal, and the critical need for early articular mobilization to nourish the newly treated cartilage lesion or allograft. The protocol is heavily dictated by the specific intra-articular procedure performed, but a standard framework applies to the osteotomy itself.
Phase I (Weeks 0 to 2) focuses on strict protection and soft tissue healing. The patient is placed in a well-padded, rigid short-leg splint or a bivalved cast in neutral dorsiflexion immediately postoperatively. The patient is made strictly non-weight-bearing (NWB) on the operative extremity, utilizing crutches, a walker, or a knee scooter. Strict elevation above the
