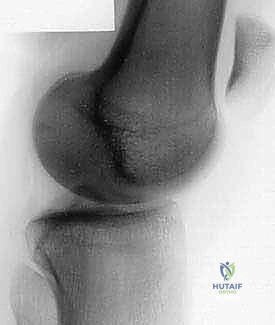
Anteromedial Tibial Tubercle Transfer: A Masterclass in Patellofemoral Rebalancing
Key Takeaway
This masterclass details anteromedial tibial tubercle transfer, a powerful procedure for patellofemoral instability and arthritis. We cover comprehensive anatomy, meticulous preoperative planning, and a granular, step-by-step intraoperative execution. Learn precise osteotomy, fixation, and critical techniques to unload the patellofemoral joint, ensuring long-term stability and pain relief. Pearls, pitfalls, and postoperative management are extensively discussed to optimize patient outcomes.
Alright, fellows, gather around. Today, we're operating on a complex case of patellofemoral instability and arthritis, and we're going to perform an anteromedial tibial tubercle transfer. This is a versatile and powerful procedure, often misunderstood but incredibly effective when indicated and executed precisely. It's not just about moving bone; it's about rebalancing the entire extensor mechanism and restoring the delicate biomechanics of the patellofemoral joint.
The core concept here is compensation. When multiple structural and alignment factors conspire to cause patellar instability or arthritis, a meticulously planned repositioning of the tibial tubercle can compensate for those underlying deficiencies. This provides lasting relief from pain and instability, often avoiding the need for more complex joint resurfacing down the line.
Understanding the Patellofemoral Joint: Comprehensive Surgical Anatomy
Let's begin by refreshing our understanding of the anterior knee. This is critical for every step we take.
Patellofemoral Articulation and Kinematics
The patella, our largest sesamoid bone, articulates within the femoral trochlea. Normally, as the knee begins to flex, the distal aspect of the patella enters the trochlea from a slightly lateralized position. This entry should be prompt, typically within the first 10 degrees of flexion. As flexion progresses, the contact point on the patella shifts proximally. In full flexion, the load is borne on the proximal aspect of the patella, with a gradual transfer of load along the patellar articular surface with each degree of flexion.
The trochlea itself deepens with increasing knee flexion, enhancing patellar containment. This means the point of greatest instability is often in early flexion, where the trochlea is at its shallowest.
The Extensor Mechanism and Retinacular Structures
The patella is enveloped by a complex soft tissue layer of tendon and retinacular structures.
- Patellar Tendon: Distally, connecting the patella to the tibial tubercle.
- Quadriceps Tendon: Proximally, a massive structure connecting the patella to the quadriceps muscle group, with a significant vastus lateralis tendon component on the proximal lateral aspect of the patella.
- Medial Patellofemoral Ligament (MPFL): This is a primary medial stabilizer, extending from the proximal half of the patella to the adductor tubercle region on the medial femoral epicondyle. It's often torn or elongated in cases of patellar dislocation.
- Lateral Retinaculum: Extends to the iliotibial band and has components attaching to the lateral femur (patellofemoral) and tibia (patellotibial).
- Vastus Lateralis Obliquus (VLO): Dynamically supports the superolateral corner of the patella, interdigitating with the lateral intermuscular septum.
Bony Landmarks and Malalignment Indices
We often refer to the tibial tuberosity to trochlear groove (TT-TG) index. This measurement, derived from superimposed tomographic images, quantifies the lateralization of the tibial tubercle relative to the central trochlear groove.

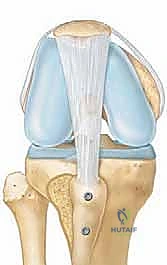
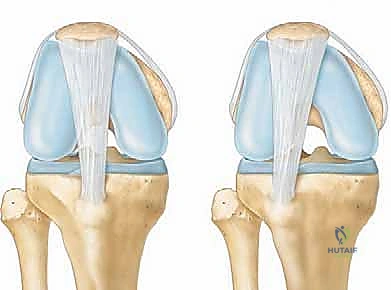
FIG 1 • The relation of the tibial tubercle (TT) to the central trochlear groove (TG)—the TT-TG relationship— pertains to patella instability. A. Normal TT-TG relationship, in which the tibial tubercle and trochlear groove are lined up. B. Lateralized tibial tubercle.
A high TT-TG index (typically >20 mm) is a strong indicator for surgical correction, as it signifies significant lateral malalignment. Similarly, a high Q-angle (usually >20 degrees) also points to an imbalance in the extensor mechanism.
Pathogenesis of Patellofemoral Disorders
Problems around the patellofemoral joint stem from a combination of anterior knee anatomy dysplasia, malalignment, and trauma. Chronic lateral tracking of the patella leads to overload and increased point loading, particularly on the patella itself. This can eventually cause articular cartilage breakdown, a condition Ficat termed "excessive lateral pressure syndrome."
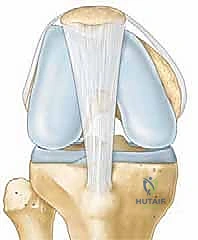
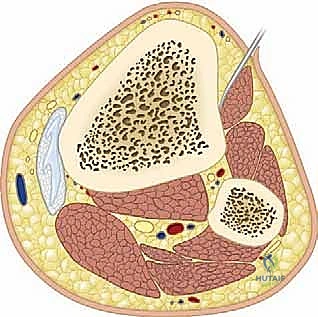
FIG 2 • A. Normal trochlear groove.
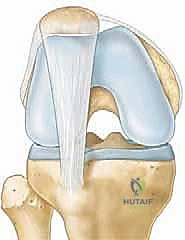
FIG 2 • B. With prolonged lateral patella tracking, the lateral trochlea becomes flattened, further aggravating lateral patella instability and stretching the medial patella support structure (including the medial patellofemoral ligament). , center of trochlea; spTG, sagittal plane of trochlear groove; spTT, sagittal plane of tibial tubercle; TT, tibial tubercle.*
A chronically lateralized extensor mechanism can lead to developmental flattening of the lateral trochlea and even the patella itself, perpetuating instability. Dislocation often tears the MPFL, which, even after healing, can remain elongated, further exacerbating lateral displacement. Blunt trauma to the flexed knee typically results in proximal patella injury, with pain originating from the injured subchondral bone, as cartilage itself is aneural.
Neurovascular Considerations
As we approach the tibial tubercle, we must be acutely aware of the neurovascular structures.
* Infrapatellar Branch of the Saphenous Nerve: This sensory nerve typically crosses the surgical field anteromedially, often 2-3 cm distal to the patella and medial to the patellar tendon. It's highly susceptible to injury during incision and dissection, leading to an annoying neuroma or chronic numbness. Meticulous dissection and careful retraction are paramount.
* Anterior Tibial Artery/Vein: While deeper and more central, awareness of its proximity is important, especially when drilling or placing hardware.
* Superficial Peroneal Nerve: While typically lateral, extreme lateral dissection should be avoided.
Preoperative Planning and Patient Positioning
Thorough preoperative planning is the bedrock of a successful outcome.
Patient Selection and Indications
We've established that this patient is a strong candidate for tibial tubercle transfer. This definitive surgery is indicated due to structural alignment imbalance and articular overload leading to instability and pain. Key indicators include:
* High TT-TG index (typically >20 mm).
* High Q-angle (usually >20 degrees).
* Dysplastic lateral trochlea, where soft tissue reconstruction alone is unlikely to succeed or would require excessive tension, leading to medial patellofemoral joint overload.
* Patellofemoral arthritis, especially with distal or lateral patella articular degeneration, where anteromedial transfer unloads these facets.
* Combined instability and arthritis.
Imaging and Diagnostic Studies
Our planning relies heavily on precise imaging.
* Standardized Office Radiographs:
* Lateral view (true lateral): Taken at 30 degrees of knee flexion, standing, with posterior femoral condyles overlapped. This view provides crucial information about trochlear depth and patella alta/baja.
* Axial view (Merchant view): Taken with the knee flexed exactly to 30 degrees. This is critical for assessing patellar tilt and subluxation. Many patients present with 90-degree flexion views, which are less useful for early flexion instability. We use a support frame to standardize our 30-degree flexion.
* 45-degree flexion view: Useful for screening patellar centralization.
* Computed Tomography (CT) Scan: This is indispensable for measuring the TT-TG index. It's ideally performed at 0, 15, 30, and 45 degrees of knee flexion, obtaining mid-patella transverse images to dynamically assess how the patella enters the trochlea. This must be done with the patient replicating normal standing alignment on the tomographic table.
* Magnetic Resonance Imaging (MRI): Less useful for bony alignment but excellent for evaluating articular cartilage integrity, soft tissue structures (MPFL, retinaculum), and subchondral bone reaction.
* Radionuclide Scan (SPECT): While not routinely used, it can be extremely helpful in determining subchondral bone reaction to overload, especially in trauma, unexplained pain, or chronic overload cases. It can accurately locate sources of subchondral bone overload, selectively guiding procedures like patella unloading.
Templating and Surgical Goals
Our goal today is an anteromedial tibial tubercle transfer. This accomplishes two critical objectives:
1. Medialization: To rebalance the patella into the central trochlea and unload the lateral facet, addressing chronic lateralization and instability.
2. Anteriorization: To unload the distal articular surface of the patella, which is often degenerated in patients with patellofemoral chondrosis or arthrosis. This shifts contact proximally on the patella.
We will template the desired amount of medialization and anteriorization based on our TT-TG measurements and patellar tracking assessment. We're aiming for a TT-TG of approximately 9-12 mm.
Nonoperative Management (Exhausted)
Remember, fellows, before we even consider surgery, every patient must exhaust nonoperative management. This includes comprehensive lower extremity core stability therapy, patellofemoral taping and bracing (I've found the Tru-Pull brace quite effective), and activity modification. Viscosupplementation can be helpful for arthritis, but often less so for patellofemoral issues specifically. This patient has failed all conservative measures.
Patient Positioning and Setup
Let's get our patient positioned.
- Supine Position: The patient is supine on the operating table.
- Tourniquet Application: A pneumatic tourniquet is applied high on the thigh.
- Leg Holder: We'll use a standard leg holder to allow for full knee flexion and extension intraoperatively, ensuring stability during the procedure. This will also allow us to drop the foot of the bed.
- Fluoroscopy Setup: The C-arm will be positioned to allow for both true lateral and axial patellofemoral views without repositioning the patient. We'll confirm its range of motion and sterility.
- Sterile Prep and Drape: Standard sterile prep from the mid-thigh to the foot, ensuring the entire knee joint and proximal tibia are accessible. We'll drape the leg free, allowing for full range of motion.
Step-by-Step Intraoperative Execution: The Surgeon's Viewpoint
Alright, team, let's scrub in.
1. Incision and Initial Dissection
"Scalpel, please. We're making a longitudinal anteromedial incision, approximately 8-10 cm in length, centered over the tibial tubercle. I prefer to start just distal to the patellar apex and extend distally past the tibial tubercle. This allows for excellent exposure and the ability to perform a thorough soft tissue release if needed."
- Skin Incision: Make a clean, precise incision through the skin and subcutaneous tissue.
-
Subcutaneous Dissection: "Now, let's carefully elevate the skin and subcutaneous flaps. Remember our anatomy: we're looking for the infrapatellar branch of the saphenous nerve here. It's variable, but often crosses our path. Use blunt dissection with Metzenbaum scissors to identify and protect it. We want to retract it gently, either medially or laterally, ensuring it's out of harm's way."
SURGICAL WARNING: Injury to the infrapatellar branch of the saphenous nerve can lead to a painful neuroma or persistent numbness, a significant source of patient dissatisfaction. Meticulous dissection is key.
-
Exposure of Patellar Tendon and Tibial Tubercle: "Continue dissecting down to the deep fascia. We'll incise the deep fascia longitudinally, just medial to the patellar tendon, to expose the patellar tendon and the underlying periosteum of the tibial tubercle. We need to define the borders of the tibial tubercle clearly."
2. Defining the Osteotomy and Preparing the Tubercle
"Now that we have excellent exposure, let's mark our osteotomy. We're aiming for an anteromedial transfer, so we need to plan both our medial shift and our anterior elevation."
-
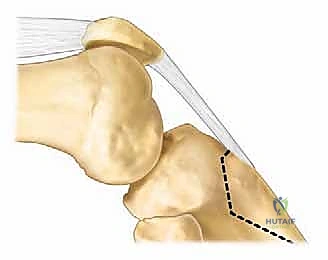
Marking the Osteotomy: "Using a marking pen, outline the bone block we intend to harvest. Typically, this block is about 1.5-2 cm wide and 4-6 cm long, ensuring it includes the entire patellar tendon insertion. We want to keep the distal periosteal attachment intact if possible, as this preserves blood supply and aids healing. This also allows us to hinge the tubercle distally."
- The medial cut will be parallel to the sagittal plane of the tibia.
- The lateral cut will be slightly convergent distally.
- The proximal cut will be just distal to the patellar tendon insertion.
- The distal cut will be oblique, allowing for a hinge, or if a complete osteotomy is needed, it will be made carefully.
-
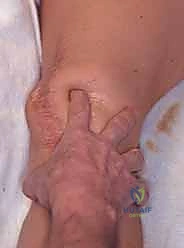
Subperiosteal Dissection: "Using a Cobb elevator, carefully elevate the periosteum and muscle attachments (primarily the tibialis anterior origin) from the medial and lateral aspects of the tibial tubercle, staying within our marked lines. This creates space for our saw blade and protects soft tissues."
Intraoperative view showing initial subperiosteal dissection around the tibial tubercle.
3. Performing the Osteotomy
"Time for the oscillating saw. Precision is paramount here."
- Medial and Lateral Cuts: "Using a small oscillating saw, make the medial and lateral osteotomy cuts. Maintain a slight oblique angle to create a trapezoidal shape, wider proximally, which helps prevent proximal fracture during fixation. Ensure these cuts are deep enough to completely penetrate the cortex but avoid plunging deep into the medullary canal initially."
- Distal Cut (if complete osteotomy): "If we're not hinging, make the distal cut next, angling it slightly proximally to create a wedge that can be advanced anteriorly. If we are hinging, we will preserve the distal periosteum."
- Proximal Cut: "Now, the proximal cut. This needs to be precise, just distal to the patellar tendon insertion. Again, avoid plunging."
-
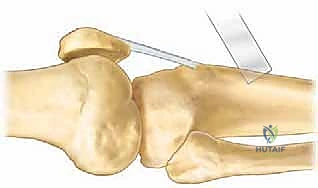
Completion with Osteotomes: "Once the saw cuts are complete, use thin osteotomes and a mallet to carefully complete the osteotomy. Start gently, tapping along the cut lines to separate the bone block. We want a clean, intact block."
Intraoperative view demonstrating the precise osteotomy cuts being made with an oscillating saw.
> **SURGICAL WARNING:** Excessive force with the osteotome can lead to an irregular fracture line or, worse, a comminuted fracture of the tubercle, making fixation challenging. Gentle, controlled taps are essential.
- Mobilization of the Tubercle: "Once the tubercle is free, or hinged distally, we can carefully mobilize it. Use a small periosteal elevator to ensure it's completely freed from its bed. We'll keep it temporarily retracted with a stay suture or a small clamp while we prepare the recipient site."
4. Preparing the Recipient Bed
"Now, we need to create the perfect home for our newly mobilized tubercle, ensuring we achieve both anteriorization and medialization."
- Medialization: "On the medial aspect of the tibia, identify the desired position for the tubercle. We're aiming for a medial shift that corrects the TT-TG index to our templated value, usually around 9-12 mm. Use a ruler and fluoroscopy to confirm the new medial position. Mark this new position."
-
Anteriorization: "To achieve anteriorization, we need to create a trough or a step-cut in the anterior tibia. Using a saw, create a shallow trough or remove a small amount of bone from the anterior tibia at the desired medialized position. The depth of this trough will determine the amount of anteriorization. We're looking for 10-15 mm of anteriorization to effectively unload the distal patella."
Intraoperative image showing the prepared recipient bed on the tibia, ready for tubercle transfer.
-
Fluoroscopic Guidance: "Let's bring in the C-arm. Obtain a true lateral view to confirm the depth of our trough and the potential for anteriorization. Then, an axial view to confirm our medialization target. We'll use these measurements to guide our bone removal."
SURGICAL WARNING: Over-resection of the tibial cortex can weaken the tibia, increasing the risk of stress fracture. Under-resection will limit our ability to achieve adequate anteriorization.
5. Transfer and Fixation of the Tibial Tubercle
"Now for the critical step: placing and fixing the tubercle."
- Placement of the Tubercle: "Carefully position the mobilized tibial tubercle into its new anteromedial recipient bed. Ensure good bony contact between the raw surfaces of the tubercle and the tibia. We want maximum surface area for healing."
- Initial Stabilization: "Use a K-wire or a small bone clamp to temporarily stabilize the tubercle in its desired position. This allows us to assess patellar tracking before definitive fixation."
-
Assessment of Patellar Tracking: "Nurse, can you flex and extend the knee gently? I'm palpating the patella. We're looking for smooth, centralized tracking throughout the range of motion, without excessive lateral deviation or medial tethering. The patella should enter the trochlea smoothly, and the 'J-sign' should be eliminated or significantly reduced. If the tracking isn't ideal, we can make minor adjustments to the tubercle's position now."
- Test for Medial Patella Subluxation: "Remember the test for medial patella subluxation? Hold the patella medially in extension and flex the knee abruptly to 30-40 degrees. If the patella enters the trochlea very suddenly and reproduces the patient's symptom, it might indicate a medial instability problem. While rare in this context, it's a good reminder to ensure we haven't over-medialized."
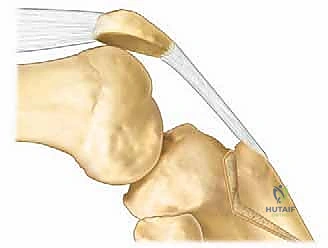
FIG 4 • Test for medial patella subluxation. The patella is held medial and knee is flexed abruptly. If patella relocation reproduces the patient’s symptom, pathologic medial subluxation probably is present.
<figure class="operative-step-slider my-4 text-center p-3 border rounded shadow-sm bg-light">
FIG 4 • Test for medial patella subluxation. The patella is held medial and knee is flexed abruptly. If patella relocation reproduces the patient’s symptom, pathologic medial subluxation probably is present.
-
Drilling for Fixation: "Once we're satisfied with the position and tracking, we'll proceed with definitive fixation. I typically use two 4.5 mm cannulated cortical screws for this. First, drill a pilot hole through the tibial tubercle and into the underlying tibia using a 3.2 mm drill bit. Ensure the drill trajectory is perpendicular to the tubercle's surface for optimal compression, and that the screws will achieve good purchase in the posterior tibial cortex."
Intraoperative image showing drilling of pilot holes for screw fixation of the transferred tibial tubercle.
> **SURGICAL WARNING:** Drill under constant fluoroscopic guidance to prevent over-penetration of the posterior cortex, which could irritate posterior neurovascular structures, or under-penetration, which would compromise fixation. Aim for bicortical purchase.
-
Screw Placement and Lag Technique: "Measure the screw length. We'll use a lag technique to compress the tubercle firmly against its new bed. Over-drill the near cortex (tibial tubercle) with a 4.5 mm drill bit, then tap the far cortex. Insert the two 4.5 mm cortical screws. Tighten them sequentially to achieve even compression."
Intraoperative image demonstrating the placement of screws for definitive fixation of the tibial tubercle.
<figure class="operative-step-slider my-4 text-center p-3 border rounded shadow-sm bg-light">
Intraoperative fluoroscopic image confirming appropriate screw length and position, ensuring bicortical purchase.
> **SURGICAL WARNING:** Overtightening screws can lead to stress risers and potential fracture of the tubercle. Ensure firm, but not excessive, compression.
- Final Fluoroscopy: "Let's get a final set of fluoroscopic images – lateral and axial – to confirm the tubercle's position, the amount of anteriorization and medialization, and the excellent placement of our screws. This is our final check."
6. Addressing Associated Pathology (If Indicated)
"In some cases, especially with chronic lateralization, we might need to address other issues."
- Lateral Retinacular Release: "If, after the tubercle transfer, there's still significant lateral tightness or tilt, a limited lateral retinacular release can be performed. However, with a well-executed anteromedial transfer, this is often unnecessary or can be done very sparingly, as the rebalancing itself reduces lateral pressure."
-
MPFL Reconstruction/Imbrication: "If the primary pathology was a significant MPFL deficiency without severe malalignment (e.g., low TT-TG, normal Q-angle), we might have considered MPFL reconstruction first. However, in this patient with a high TT-TG and arthritic changes, the tubercle transfer is the primary solution. We've already assessed the MPFL preoperatively for competency."
Another intraoperative view, possibly showing assessment of patellar tracking after initial fixation or a lateral release if performed.
7. Closure
"With the tubercle securely fixed and patellar tracking optimized, we can proceed with closure."
- Hemostasis: "Ensure meticulous hemostasis. We don't want any postoperative hematoma."
- Periosteal Closure: "Close the periosteum over the transferred tubercle and the recipient site with absorbable sutures. This helps to secure the bone graft and promote healing."
- Fascial Closure: "Close the deep fascia with interrupted absorbable sutures."
- Subcutaneous Closure: "Close the subcutaneous layer with absorbable sutures to obliterate dead space."
- Skin Closure: "Close the skin with staples or a running subcuticular suture, based on preference. Apply a sterile dressing."
Extensive Pearls and Pitfalls
Fellows, this procedure, while effective, comes with its own set of challenges. Anticipating and managing these is what makes a master surgeon.
Pearls for Success:
- Precise Preoperative Planning: Never underestimate the value of accurate CT measurements for TT-TG and meticulous templating. Know your target medialization and anteriorization before you incise.
- Protect the Infrapatellar Nerve: This is arguably the most common complication. Meticulous blunt dissection and gentle retraction are non-negotiable.
- Maintain Distal Periosteal Hinge (if possible): This preserves blood supply to the tubercle, promoting faster and more reliable healing. If a complete osteotomy is necessary, be extra cautious with handling the bone block.
- Adequate Bone Block Size: Ensure the tubercle block is large enough to incorporate the entire patellar tendon insertion and provide adequate surface area
REFERENCES
-
Amis AA, Firer P, Mountney J, et al. Anatomy and biomechanics of the medial patellofemoral ligament. Knee 2003;10:215–220.
-
Buuck DA, Fulkerson JP. Anteromedialization of the tibial tubercle: a 4to 12year follow-up. Oper Tech Sports Med 2000;8:131–137.
-
Cox JS. Evaluation of the Roux-Elmslie-Trillat procedure for knee extensor realignment. Am J Sports Med 1982;10:303–310.
-
Dejour H, Walch G, Nove-Josserand L, et al. Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 1994;2:19–26.
-
Dye SF, Chew MH. The use of scintigraphy to detect increased osseous metabolic activity about the knee. J Bone Joint Surg Am 1993; 75A:1388–1406.
-
Farr J. Anteromedialization of the tibial tubercle for treatment of patellofemoral malpositioning and concomitant isolated patellofemoral arthrosis. Tech Orthop 1997;12:151–164.
-
Ficat P. The syndrome of lateral hyperpressure of the patella (translated from French). Acta Orthopaedica Belgica 1978;44(1):65–76.
-
Fulkerson JP. Anteromedialization of the tibial tuberosity for patellofemoral malalignment. Clin Orthop Rel Res 1983;177: 176–181.
-
Fulkerson JP. Anterolateralization of the tibial tubercle. Tech Orthop 1997;12:165–169.
-
Fulkerson JP. A clinical test for medial patella tracking. Tech Orthop 1997;12:144.
You Might Also Like