MPFL Repair & Reconstruction: A Masterclass in Patellar Instability Surgery
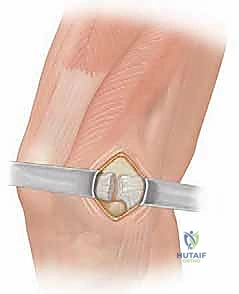
Key Takeaway
This masterclass guides fellows through medial patellofemoral ligament (MPFL) repair and reconstruction for patellar instability. We'll cover comprehensive surgical anatomy, meticulous preoperative planning, and granular intraoperative execution from a surgeon's perspective. Expect detailed steps on incision, dissection, hardware application, and critical decision-making. We'll also delve into pearls, pitfalls, and holistic postoperative rehabilitation strategies for optimal patient outcomes.
Alright, fellows, welcome to the operating theater. Today, we're tackling a common yet challenging problem: patellar instability. This isn't just about a "kneecap popping out"; it's a complex interplay of anatomy, biomechanics, and patient factors. Our goal is to restore stability and function, and we'll do that by either repairing or reconstructing the Medial Patellofemoral Ligament (MPFL). Let's scrub in.
Understanding Patellar Instability: The Foundation
Before we make any incisions, let's refresh our understanding of this condition. Patellar instability typically manifests as episodes of complete dislocation or subluxation of the patella from the trochlear groove, almost exclusively in the lateral direction. This is a significant event, often causing pain and considerable apprehension.
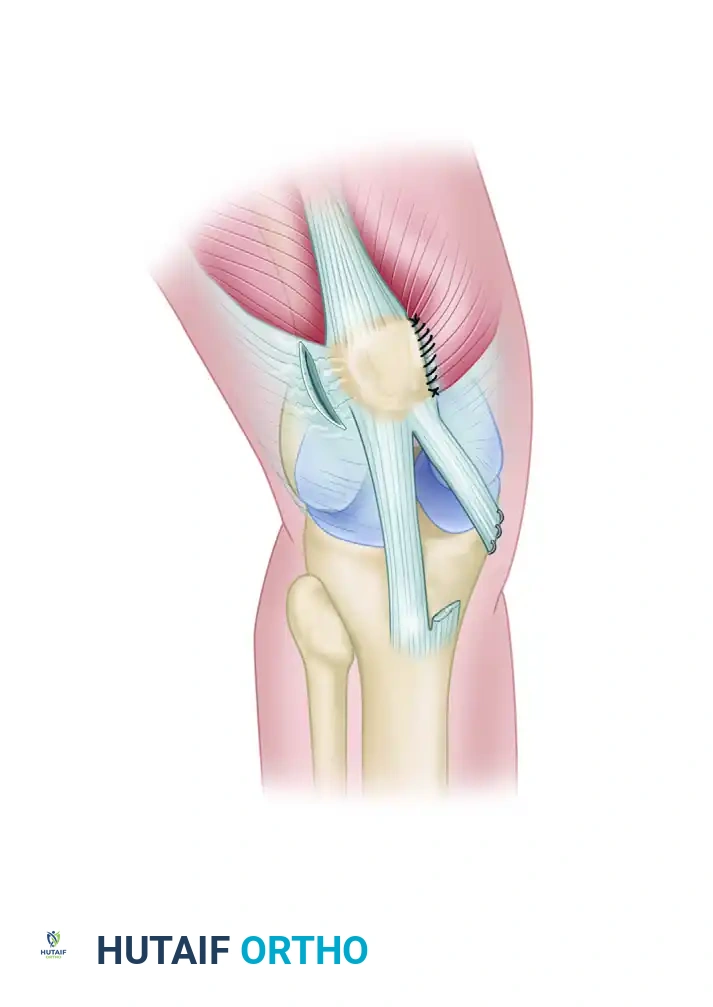
The Critical Role of the MPFL
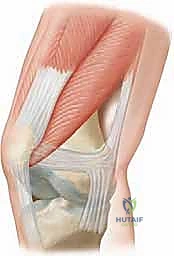
The MPFL is the primary static restraint against lateral patellar displacement, contributing 50% to 80% of the restraining force. It's a flat, fibrous band intimately associated with the medial retinaculum, extending from the medial patella to the medial femoral condyle.
- Patellar Attachment: It inserts broadly into the superior two-thirds of the medial border of the patella. This broad attachment is crucial for distributing stress.
- Femoral Attachment: This is a critical anatomical landmark for our surgery. The MPFL attaches to the femur just distal to the adductor tubercle and just superoposterior to the medial epicondyle. In skeletally immature patients, it attaches between the growth plate and the medial epicondyle, a detail we must respect to avoid iatrogenic growth arrest.
Types of Patellar Dislocation
We generally categorize patellar dislocations into two types:
- Traumatic Dislocation: This usually involves a distinct injury mechanism, often non-contact where the lower extremity internally rotates with knee valgus on a planted foot – very similar to an ACL injury mechanism. Less commonly, it's a direct blow pushing the kneecap laterally. These often spontaneously reduce in the field.
- Atraumatic Dislocation/Subluxation: This is secondary to generalized ligamentous laxity or underlying anatomical predisposition without a specific traumatic event.
Associated Injuries: What Else to Look For
A primary traumatic patellar dislocation is rarely an isolated injury. We must be vigilant for concomitant damage:
* Osteochondral Fractures: These are common and can be serious.
* Medial Patellar Facet: A serious fracture of the medial patellar facet can occur.
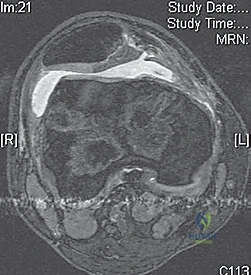
* Lateral Femoral Condyle: An osteochondral fracture of the lateral femoral condyle, often at the sulcus terminalis, is a signature injury. This suggests dislocation usually occurs at 70-80 degrees of flexion.
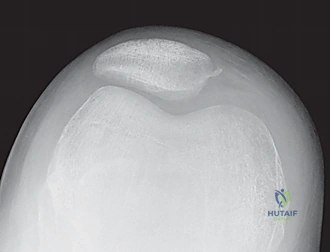
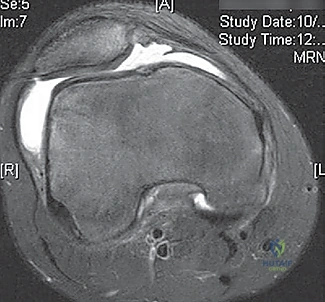
* Bone Bruises: MRI often reveals increased signal on the medial patella and the midportion of the lateral femoral condyle. This distinct pattern helps differentiate it from ACL tears.
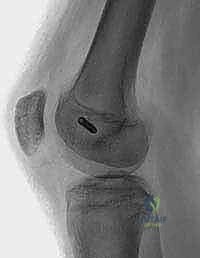
* Nonarticular Avulsion Fracture: A less serious avulsion fracture of the MPFL off the medial patella is pathognomonic. This can appear immediately or be delayed as an ossific lesion.
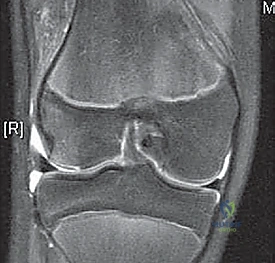
Predisposing Factors
Several anatomical and biomechanical factors increase the risk of patellar dislocation:
- Patella Alta: This is a proven risk factor.
- Trochlear Dysplasia: A shallow trochlear groove.
- Lateralized Tibial Tubercle: Increased TT-TG distance.
- Hypoplastic Tibial Tubercle
- Valgus Knee Alignment
- Increased Q Angle
- Femoral Intorsion, Tibial Extorsion, Foot Pronation
- Ligamentous Laxity, Family History, Young Age
Preoperative Planning: The Blueprint for Success
Our success starts long before the first incision. Careful preoperative planning is paramount.
Patient History and Physical Examination
- History: Most patients present with a history of a noncontact or contact injury, often not recognizing it as a patellar dislocation due to spontaneous reduction. Pain is usually acute, not chronic patellofemoral pain.
- Physical Exam:
- Effusion: Usually present after traumatic dislocation, rarely atraumatic.
- Patella Apprehension Sign: The most reliable test. With the knee flexed 25-30 degrees over a bolster, gently translate the patella laterally. A positive test elicits patient apprehension or guarding.
- Patella Glide Test: Lateral translation of more than two quadrants of the patella with the knee flexed 25-30 degrees indicates instability.
- J Sign: Patella pulls laterally as the knee reaches full extension, forming an upside-down J, indicating proximal alignment issues.
- Overall Knee Stability: Rule out other ligamentous injuries (ACL, MCL, LCL, PCL) and meniscal tears.
Imaging and Diagnostic Studies
- Plain Radiographs:
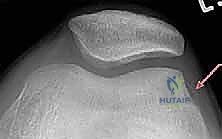
- AP, Lateral, Sunrise/Merchant Views: Essential. The sunrise view, requiring 30-45 degrees of flexion, might be delayed due to acute pain but is crucial for assessing trochlear morphology and patellar tilt.
- Limitations: Plain films can miss up to 40% of arthroscopically documented chondral or osteochondral lesions. Subtle slivers of bone can be easily overlooked.
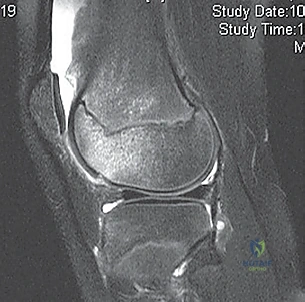
- MRI Scan: Highly recommended for all patients with a large traumatic effusion due to the high rate of occult articular or osteoarticular injury.
* Osteochondral Lesions: Crucial for determining size, location, and potential for repair versus removal.
* Bone Bruise Pattern: Confirms patellar dislocation (medial patella and lateral femoral condyle).
* Anatomical Risk Factors: Assesses patella alta, trochlear dysplasia, tibial tubercle-trochlear groove (TT-TG) distance.
Indications for Surgical Management
While routine operative stabilization of primary dislocations doesn't always improve natural history, specific scenarios warrant intervention:
- Failure of Nonoperative Management: Recurrent traumatic or atraumatic dislocations despite bracing and physical therapy.
- Osteochondral Damage: Lesions larger than 1 cm with bone attached to the chondral fragment necessitating repair, or removal of a loose body.
- Attenuated MPFL: Noted intraoperatively in cases of recurrent instability.
- First-time Dislocation with Failed Concentric Reduction.
Surgical Contraindications for MPFL Reconstruction:
- Malalignment that is the primary driver of instability (may require other procedures like tibial tubercle osteotomy, but not in skeletally immature patients).
- Isolated patellofemoral pain.
- Arthrosis.
Tibial Tubercle Realignment Procedures: Avoid these in skeletally immature patients with open growth plates due to the risk of iatrogenic genu recurvatum from growth arrest.
Patient Positioning and Setup
"Alright team, let's get our patient positioned."
- Supine Position: Our patient is supine on the operating table.
- Imaging Compatibility: Ensure the table allows for easy C-arm access for intraoperative fluoroscopy (AP, lateral, and axial views). We want minimal repositioning of the patient once draped.
- Knee Flexion Bolster: We'll tape an intravenous fluid bag or use a specialized bolster beneath the knee. This allows us to maintain the knee at approximately 30 to 60 degrees of flexion during MPFL repair or reconstruction tensioning. This specific range is critical for assessing patellar tracking and preventing over- or under-correction.
- Tourniquet: A high thigh tourniquet is applied to ensure a bloodless field, which is essential for identifying delicate structures and precise dissection.
- Contralateral Leg: The contralateral leg will be placed in a well-padded leg holder or allowed to rest naturally, ensuring no undue pressure on neurovascular structures.
- Sterile Prep and Drape: Standard sterile preparation from the mid-thigh to the ankle. We'll use a stockinette and impervious drapes to isolate the operative field, allowing for full range of motion of the knee intraoperatively.
Intraoperative Masterclass: Step-by-Step Execution
Now, let's get down to business. We'll walk through the MPFL repair first, then the reconstruction.
Medial Patellofemoral Ligament (MPFL) Repair
This approach is typically reserved for acute, first-time dislocations with a clearly identifiable avulsion of the MPFL, often off the patella, and without significant attenuation.
1. Incision and Initial Dissection
"Scalpel, please. We'll make a precise incision, fellows."
- Skin Incision: A 3 to 5 cm longitudinal incision is made, centered directly over the medial border of the patella. This provides adequate exposure while minimizing soft tissue disruption.
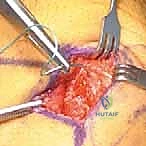
* Subcutaneous Dissection: Use blunt and sharp dissection to carry the incision down through the subcutaneous fat, identifying the deep fascia.
* Fascial Incision: Incise the deep fascia longitudinally, just medial to the patella.
2. Elevating Periosteum and Developing Tissue Planes
"Now, let's carefully elevate the soft tissues. Precision is key here to preserve the integrity of the retinaculum."
- Subperiosteal Incision: Make a vertical subperiosteal incision down to bone, approximately 1 to 1.5 cm lateral to the medial patellar border. This defines our working area on the patella.
- Periosteal Elevation: Using a small Cobb elevator or a Freer elevator, meticulously elevate the periosteum and all overlying soft tissues off the medial patella.
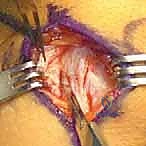
* Developing the Fatty Plane: With Metzenbaum or curved tenotomy scissors, carefully develop a tissue plane in the fatty layer between the retinaculum and the synovial joint capsule. This is a crucial step: we want to stay extra-articular.
> Surgical Warning: Avoid entering the joint space. This is an extra-articular procedure. Entering the joint increases the risk of arthrofibrosis and other complications.
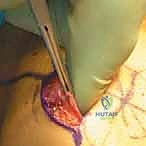
3. MPFL Identification and Assessment
"Now, let's identify the MPFL itself. We need to assess its quality and suitability for repair."
- Digital Palpation: Place a finger into the extrasynovial tunnel you've just created. This tunnel lies just outside the synovium of the knee joint but is deep to the MPFL.
- Traction and Palpation: Apply gentle traction on the patellar end of the MPFL (if it's avulsed from the patella) with a Kocher clamp. Digitally palpate the MPFL on its inner surface, tracing it down to the medial epicondyle.
* Assessment: The MPFL should feel like a stout band of tissue originating from the medial epicondyle. If it's attenuated, frayed, or severely damaged, repair may not be sufficient, and reconstruction should be considered.
4. Patellar Preparation for Repair
"We need a good bed for healing on the patella."
- Decortication: Using a rongeur or a high-speed burr, perform superficial decortication of the exposed anterior medial patella. This creates a bleeding bony bed, optimizing healing of the advanced MPFL.
5. Creating Suture Tunnels or Anchors
"Now for our fixation points on the patella."
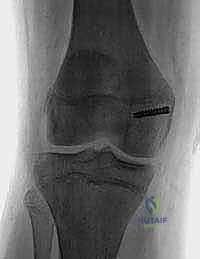
- Transosseous Tunnels: Create multiple extra-articular drill holes (three or four) in the patella to form transosseous suture tunnels for imbrication. Use a small drill bit (e.g., 2.0 mm) and ensure the tunnels are placed strategically to capture the MPFL effectively.
> Surgical Warning: Ensure drill holes are truly extra-articular to prevent damage to the articular cartilage of the patella.
* Suture Anchors: As an alternative, suture anchors can be used for fixation to the patella. Insert these carefully into the decorticated bone, ensuring good purchase.
6. Suturing the MPFL
"Let's secure this ligament back where it belongs."
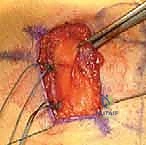
- Suture Placement: Pass No. 2 or stronger nonabsorbable sutures through the patella tunnels (or suture anchor eyelets). Then, meticulously weave these sutures through the advanced MPFL tissue.
* Attachment Point: Critically, the MPFL should be sutured to the anteromedial surface of the patella, not the posteromedial surface. This ensures the correct vector of pull and avoids medial patellar tilt.
7. Tensioning the Repair
"This is arguably the most critical step for functional outcomes."
- Knee Flexion: Position the knee at 45 to 60 degrees of flexion. This is the sweet spot for tensioning.
- Tensioning: With the knee in this position, carefully tie down the sutures, applying appropriate tension.
> Surgical Warning: Over-tensioning can lead to medial patellar pain, chondral overload, and restricted flexion. Under-tensioning will result in persistent instability. The goal is to allow for smooth patellar tracking without excessive lateral excursion, but also without undue medial restriction.
8. Assessing the Repair and Closure
"Let's test our work."
- Range of Motion: Put the knee through a full range of motion, from full extension to deep flexion. Observe the patellar tracking. The patella should track smoothly in the trochlea without subluxation or excessive lateral pull, and without undue resistance to flexion. Perform a patellar apprehension test again.
- Final Soft Tissue Closure: The remaining free lateral edge of the MPFL tissue (retinaculum) is sewn down to the patellar soft tissue with a running 2-0 absorbable suture. This reinforces the repair and closes the soft tissue layers.
- Wound Closure: Irrigate the wound thoroughly. Close the subcutaneous layers with absorbable sutures and the skin with staples or non-absorbable sutures.
Medial Patellofemoral Ligament (MPFL) Reconstruction
This procedure is indicated for recurrent instability, significant MPFL attenuation, or in patients where primary repair is deemed inadequate. We'll use a hamstring autograft.
1. Incision and Initial Dissection (Patellar Side)
"For reconstruction, our initial patellar approach is similar, but we'll be preparing for graft passage."
- Skin Incision: A 3 to 5 cm longitudinal medial patellar skin incision is made, identical to the repair approach.
- Deep Dissection: Carry dissection down to the medial patella.
- Periosteal Flap Elevation: Elevate a thick periosteal flap off the medial 1 to 1.5 cm of the patella. This flap is then carried distally down to the medial fibrofatty layer, just outside the knee synovium. This creates a robust bed for our graft.
- Extrasynovial Tunnel: Create an extrasynovial tunnel extending inferiorly from the patellar exposure down towards the medial epicondyle. This will be our path for the graft.
2. Graft Harvest: Semitendinosus Tendon
"Now, let's harvest our graft material. The semitendinosus is a reliable choice."
- Incision: Make a standard proximal medial tibial approach incision, typically 2-3 cm long, slightly obliquely over the pes anserinus.
- Semitendinosus Identification: Identify the sartorius fascia and incise it. Locate the semitendinosus tendon, which is typically found posterior and slightly inferior to the gracilis.
- Tendon Stripper: Use a tendon stripper to harvest a single semitendinosus tendon. Carefully strip the tendon proximally, ensuring a good length.
<a href="/media/hutaif_opertive/hutaif-ch20
Additional Intraoperative Imaging & Surgical Steps
.
Overtightening of medial soft tissue can result in medial dislocation. This is especially possible if a medial repair is tensioned in full extension or is combined with an extensive lateral release.
Care must be taken to avoid patella articular cartilage penetration when drilling patella holes, especially with the Galeazzi procedure.
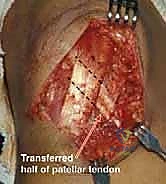
With the Roux-Goldthwaite procedure, there are reports of patellar tendon rupture of the untransferred tendon.