Mastering Excision and Reconstruction of Hand Malignancies: SCC & Melanoma
Key Takeaway
Join us in the OR for a masterclass on excising squamous cell carcinoma and melanoma of the hand. We'll meticulously cover preoperative planning, precise surgical anatomy, and granular intraoperative techniques for wide local excision, sentinel node biopsy, and advanced flap reconstruction. Learn critical pearls, pitfalls, and postoperative management strategies to optimize oncologic outcomes and preserve hand function.
Comprehensive Introduction and Patho-Epidemiology
The management of malignant neoplasms of the hand and upper extremity represents a profound challenge at the intersection of surgical oncology and reconstructive microsurgery. Squamous cell carcinoma (SCC) and melanoma are the most formidable of these cutaneous and subungual malignancies, demanding an uncompromising adherence to oncologic principles coupled with sophisticated reconstructive foresight. The hand is not merely a functional appendage; it is a highly visible, anatomically dense structure where millimeter-level decisions dictate both patient survival and lifelong functional utility. Our primary, non-negotiable objective is absolute tumor extirpation. Only once negative margins are definitively secured can we pivot to the secondary objective: meticulous anatomical reconstruction to preserve form, sensibility, and biomechanical function.
Squamous Cell Carcinoma of the Hand
Squamous cell carcinoma is the most common primary malignancy of the hand, originating from the epidermal keratinocyte cell layers. Its pathogenesis in the upper extremity is multifactorial, most frequently associated with cumulative ultraviolet (UV) radiation exposure, particularly in fair-skinned individuals. However, the hand surgeon must be acutely aware of alternative etiologies. SCC can arise aggressively within areas of chronic inflammation, thermal burn scars, or chronic non-healing wounds—a phenomenon classically described as a Marjolin’s ulcer. Furthermore, immunosuppression dramatically increases the incidence and aggressiveness of SCC; solid organ transplant recipients and those with HIV/AIDS present with a markedly higher risk of multiple, rapidly progressive lesions. Subungual SCC, a distinct clinical entity, is increasingly associated with high-risk human papillomavirus (HPV) strains, notably HPV 16 and 18, and often mimics benign paronychia or verruca vulgaris, leading to perilous delays in diagnosis.
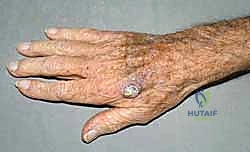
Clinically, a typical cutaneous SCC on the dorsum of the hand presents as a firm, hyperkeratotic, erythematous papule or nodule that exhibits rapid growth. It frequently progresses to central ulceration with indurated, raised, and inflamed borders. Unlike basal cell carcinoma, SCC lacks a pearly, telangiectatic perimeter. The histologic grading of SCC ranges from well-differentiated (Grade 1) to poorly differentiated (Grade 4), determined by the proportion of differentiating cells, nuclear atypia, and the depth of dermal or subcutaneous invasion. This grading is paramount, as poorly differentiated tumors, tumors exceeding 2 centimeters in diameter, and those exhibiting perineural or lymphovascular invasion carry a significantly higher risk of regional nodal metastasis and mandate a more aggressive surgical posture.
Cutaneous and Subungual Melanoma
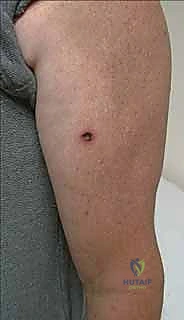
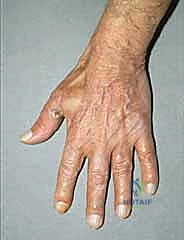
Melanoma, while less common than SCC, accounts for the vast majority of skin cancer-related mortality. These neoplasms arise from dendritic melanocytes derived from the neural crest, which migrate to the basal layer of the epidermis, the nail matrix, and various mucosal surfaces. In the upper extremity, melanomas exhibit a diverse array of clinicopathologic subtypes. Superficial spreading melanoma is the most prevalent, typically presenting as an asymmetric, variably pigmented macule or plaque. Nodular melanoma, characterized by rapid vertical growth, is inherently more aggressive and often presents as a deeply pigmented, ulcerated nodule. Acral lentiginous melanoma is of particular concern to the hand surgeon; it occurs on the palmar surfaces and subungual regions, disproportionately affecting patients of darker skin phenotypes, and is notorious for late presentation and poor prognosis.
The microstaging of melanoma remains the absolute cornerstone of prognostic determination and surgical planning. Breslow thickness—the vertical measurement in millimeters from the granular layer of the epidermis to the deepest point of tumor invasion—is the most reproducible and critical prognostic indicator. The Clark level, which categorizes the anatomic level of local invasion from the epidermis (Level I) into the subcutaneous fat (Level V), provides supplemental prognostic data but has largely been superseded by Breslow thickness and ulceration status in the modern American Joint Committee on Cancer (AJCC) staging system. It is imperative to remember that amelanotic melanomas occur and can be deceptively benign in appearance, masquerading as pyogenic granulomas or chronic paronychia.
Natural History and Metastatic Potential
The natural history of both SCC and melanoma involves local tissue destruction, regional lymphatic dissemination, and eventual distant hematogenous metastasis. The dense fascial planes and minimal subcutaneous tissue of the hand facilitate rapid deep extension of neglected tumors into paratenon, periosteum, and neurovascular bundles. Lymphatic spread follows predictable anatomical pathways, which must be thoroughly understood for accurate clinical staging and sentinel lymph node mapping. Melanoma, in particular, exhibits an unpredictable propensity for both in-transit metastases (cutaneous or subcutaneous deposits between the primary tumor and the regional nodal basin) and distant visceral spread. A profound understanding of these metastatic pathways is essential, as it dictates the necessity for advanced systemic imaging, sentinel lymph node biopsy, and the potential integration of adjuvant targeted therapies or immunotherapies (e.g., BRAF/MEK inhibitors, PD-1/CTLA-4 blockade) in the comprehensive management paradigm.
Detailed Surgical Anatomy and Biomechanics
A masterful oncologic resection in the hand requires an encyclopedic knowledge of its regional anatomy. The hand is an unforgiving anatomic territory; the proximity of the integument to critical neurovascular and musculotendinous structures means that achieving adequate oncologic margins frequently necessitates the sacrifice of functional components. Preoperative anticipation of these anatomical deficits is the foundation of reconstructive planning.
Integumentary and Fascial Architecture
The skin of the upper extremity exhibits profound regional variations that directly impact both tumor behavior and surgical reconstruction. The dorsal skin of the hand is exceedingly thin, highly pliable, and loosely attached to the underlying extensor paratenon and deep fascia via a lax areolar tissue layer. This mobility accommodates the extreme flexion of the digits and wrist. However, this thinness means that dorsal malignancies rapidly invade the underlying extensor apparatus. Conversely, the palmar skin is thick, glabrous, heavily keratinized, and firmly anchored to the palmar aponeurosis by robust vertical fibrous septa. This architecture provides a stable surface for grip but also acts as a dense barrier; palmar tumors may spread laterally along these fibrous septa before manifesting significant vertical growth, potentially underestimating the true extent of the lesion.
The lymphatic drainage of the hand is critically important for staging. The palmar lymphatic vessels course dorsally to join the dorsal lymphatic network. The lymphatic drainage of the ulnar three digits (small, ring, and ulnar aspect of the middle finger) typically ascends to the epitrochlear lymph nodes before progressing to the axillary basin. In contrast, the radial two digits (thumb, index, and radial aspect of the middle finger) generally drain directly into the axillary lymph nodes, bypassing the epitrochlear nodes. This anatomical divergence is crucial when performing clinical examinations and planning sentinel lymph node biopsies.
Neurovascular Topography
The vascular supply to the hand is derived from the radial and ulnar arteries, which form the superficial and deep palmar arches. From these arches, the common digital arteries arise, subsequently bifurcating into the proper digital arteries. Each digit is supplied by two neurovascular bundles running volar to the mid-axial line. These bundles contain the proper digital artery and the proper digital nerve, enveloped in Cleland's and Grayson's ligaments. During wide local excision of digital malignancies, particularly those on the lateral aspects of the digits or within the web spaces, these structures are at extreme risk. Inadvertent injury or necessary oncologic sacrifice of a digital nerve results in devastating sensory loss, while arterial sacrifice threatens digital viability.
The major peripheral nerves—median, ulnar, and radial—provide critical motor and sensory innervation. Tumors demonstrating perineural invasion (a poor prognostic indicator, especially in SCC) have a propensity to track proximally along these nerve sheaths. When perineural invasion is identified or suspected, the surgeon must be prepared to trace the nerve proximally, potentially requiring extensive nerve resection and subsequent intercalary nerve grafting to restore function. The proximity of tumors to the cubital tunnel or Guyon's canal demands meticulous dissection to protect the ulnar nerve while ensuring complete tumor extirpation.
The Subungual Apparatus and Osteotendinous Relationships
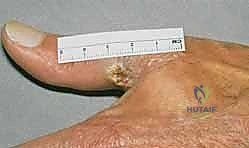
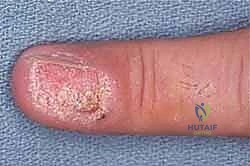
The subungual apparatus is a highly specialized anatomical region that lacks the physiologic barriers of the epidermis and dermis found in intact skin. It comprises the nail matrix (the germinal epithelium responsible for nail plate production), the nail bed (sterile matrix), the eponychium (proximal nail fold), and the hyponychium. Malignancies arising here, such as subungual melanoma or SCC, are in intimate proximity to the periosteum of the distal phalanx and the insertion of the extensor terminal tendon.
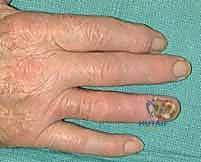
Because of this lack of anatomical barriers, subungual tumors can rapidly invade the underlying bone. The presence of Hutchinson's sign—the extension of brown-black melanin pigment from the nail bed, matrix, and nail plate onto the adjacent cuticle and proximal or lateral nail folds—is a classic, highly specific indicator of subungual melanoma. However, its absence does not preclude the diagnosis, particularly in amelanotic variants. Radiographic evaluation of the distal phalanx is mandatory for all subungual lesions to assess for cortical erosion or osseous invasion, which definitively shifts the surgical plan from wide local excision to amputation.

Exhaustive Indications and Contraindications
The decision-making process for extirpating hand malignancies is governed by strict oncologic protocols. The primary indication for surgery is the biopsy-proven presence of a malignant neoplasm. However, the extent of the surgery is dictated by tumor histology, depth of invasion, anatomical location, and patient-specific factors.
Establishing Surgical Candidacy
The absolute prerequisite for definitive surgical management is a high-quality tissue biopsy. The diagnosis and microstaging must be confirmed by rigorous histopathologic evaluation. For suspicious pigmented lesions or suspected SCC, full-thickness incisional biopsies (such as a punch biopsy through the thickest portion of the tumor) or complete excisional biopsies (for small lesions where the biopsy serves as the initial excision) are required. It is a cardinal rule of surgical oncology that suspicious lesions, particularly potential melanomas, are NEVER shaved, cauterized, or vaporized. Shave biopsies transect the tumor, rendering accurate assessment of Breslow thickness impossible, thereby destroying the most critical piece of prognostic and staging information. If the initial pathologic diagnosis is equivocal, the slides must be reviewed by a specialized dermatopathologist prior to definitive surgical intervention.
Indications for Wide Local Excision and Amputation
The indications for specific surgical procedures are directly tied to the tumor's characteristics. Wide local excision (WLE) is indicated for cutaneous SCC and melanoma where adequate margins can be achieved while preserving a functional hand. For cutaneous SCC, a 3 to 10 mm margin of clinically normal tissue is indicated, depending on the tumor's size, histologic grade, and depth. For cutaneous melanoma, the margins are dictated by Breslow thickness: a 1 cm margin is standard for lesions less than 1.5 mm thick, while a 2 cm margin is required for lesions thicker than 1.5 mm.
Amputation (ray resection or digital amputation) is indicated when a wide local excision would result in a functionally useless appendage, or when the tumor has directly invaded vital structures that cannot be reconstructed. For invasive nail matrix SCC or melanoma, amputation at the distal interphalangeal (DIP) joint for fingers, or the interphalangeal (IP) joint for the thumb, is the standard of care. Proximal digital melanoma with confirmed bone or joint involvement, or extensive perineural invasion, necessitates complete ray amputation to ensure local control.
Contraindications to Immediate Reconstruction
Contraindications to surgical excision are rare and generally limited to patients with profound medical comorbidities who cannot tolerate anesthesia, or those with widely disseminated metastatic disease where local control will not alter the clinical trajectory or improve quality of life. However, there are strict contraindications to immediate reconstruction. Immediate complex reconstruction (e.g., local flaps, free tissue transfer) is absolutely contraindicated if there is any ambiguity regarding margin status. If frozen sections are unavailable or unreliable, the wound must be managed with temporizing measures (such as a biologic dressing or negative pressure wound therapy) until permanent pathologic clearance is confirmed. Reconstructing over a positive margin is an oncologic disaster that buries residual disease and complicates subsequent re-excision.
| Parameter | Indications | Contraindications |
|---|---|---|
| Wide Local Excision (WLE) | Cutaneous SCC/Melanoma without deep structural invasion; margins achievable. | Deep bone/joint invasion; WLE leaves a non-functional digit. |
| Digital/Ray Amputation | Invasive subungual melanoma; bone/joint involvement; massive soft tissue destruction. | Superficial in situ lesions amenable to Mohs or WLE. |
| Sentinel Lymph Node Biopsy | Melanoma >0.8mm thick, or <0.8mm with ulceration/high mitotic rate; High-risk SCC. | Clinically palpable nodes (requires therapeutic lymph node dissection instead). |
| Immediate Flap Coverage | Confirmed negative margins (frozen or permanent); exposed vital structures. | Positive or pending margins; active local infection; severe patient instability. |
Pre-Operative Planning, Templating, and Patient Positioning
Flawless execution in the operating theater is the direct result of obsessive preoperative planning. The surgeon must synthesize clinical data, imaging, and pathologic staging to formulate a primary surgical plan and multiple reconstructive contingencies.
Clinical Staging and Imaging Modalities
Comprehensive staging begins with a meticulous physical examination, focusing not only on the primary lesion but also on the regional lymphatic basins. Palpation of the epitrochlear and axillary nodes is mandatory. Any palpable adenopathy necessitates a fine-needle aspiration (FNA) or core biopsy to rule out macroscopic nodal disease.
Imaging is tailored to the specific presentation. Plain radiographs of the affected hand in multiple orthogonal planes are standard to evaluate for cortical erosion or periosteal reaction, particularly for subungual lesions or large, fixed cutaneous tumors. For advanced local disease, Magnetic Resonance Imaging (MRI) with and without intravenous contrast is the gold standard for delineating soft tissue extent, neurovascular involvement, and intramedullary osseous extension. Systemic staging for high-risk SCC or melanoma includes a comprehensive metabolic panel, complete blood count, and cross-sectional imaging (CT of the chest, abdomen, and pelvis, or a whole-body PET/CT) to evaluate for distant metastasis.
Margin Determination and Reconstructive Ladder
The surgical strategy is predicated on the oncologic principle of tumor clearance first, reconstruction second. Margin determination is mapped preoperatively based on established guidelines. For a melanoma with a Breslow thickness of 2.5 mm on the dorsum of the hand, a 2 cm radial margin is marked. The deep margin must extend to the next un-involved anatomic barrier, which on the dorsum of the hand is typically the deep fascia or extensor paratenon.
Once the extirpative defect is templated, the reconstructive ladder is engaged. Small defects may be amenable to primary closure if the surrounding tissue is sufficiently lax. However, given the stringent margin requirements, most resections will require skin grafting or flap coverage. Full-thickness skin grafts (FTSG), harvested from the groin or hypothenar eminence, are preferred over split-thickness grafts for the palmar surface due to their durability and resistance to secondary contraction. For defects exposing bare bone, tendon without paratenon, or neurovascular structures, local or regional flaps are required. Contingency plans must include options such as V-Y advancement flaps, cross-finger flaps, reverse dorsal metacarpal artery flaps, or even pedicled radial forearm flaps for massive defects.
Anesthesia, Positioning, and Hemostasis
Optimal surgical conditions require meticulous patient positioning and anesthesia management. General anesthesia is typically employed, often supplemented with a regional block (e.g., an ultrasound-guided axillary or supraclavicular brachial plexus block). The regional block provides profound intraoperative muscle relaxation, excellent postoperative analgesia, and sympathectomy-induced vasodilation, which is highly beneficial for flap perfusion.
The patient is positioned supine with the affected upper extremity extended onto a radiolucent hand table. The arm is abducted and externally rotated to allow simultaneous access to the primary lesion and the axillary/epitrochlear nodal basins if a sentinel lymph node biopsy is planned. A pneumatic tourniquet is applied to the proximal brachium over soft padding. To ensure a completely bloodless field—an absolute necessity for precise micro-dissection and accurate margin assessment—the limb is exsanguinated with an Esmarch bandage, and the tourniquet is inflated to 250-280 mmHg, or precisely 100 mmHg above the patient's systolic blood pressure. Ischemia time is rigorously monitored, with a strict limit of 120 minutes before reperfusion is required.
Step-by-Step Surgical Approach and Fixation Technique
The intraoperative phase is an exercise in controlled, methodical precision. The surgical team must operate with a heightened awareness of oncologic boundaries, utilizing "no-touch" techniques to prevent tumor seeding.
Tumor Extirpation and Margin Control
Following the formal surgical time-out and sterile draping, the planned excision margins are meticulously drawn using a sterile surgical marker. The incision is initiated with a fresh #15 scalpel blade. The surgeon must ensure that the scalpel remains perfectly perpendicular to the skin surface throughout the initial incision. Beveling the incision inward is a common error that artificially narrows the deep margin, potentially leaving residual tumor at the base of the resection bed.
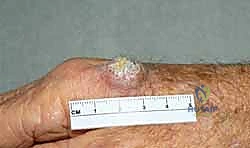
Deep dissection proceeds through the subcutaneous fat down to the predetermined fascial plane. Tissue handling is minimized; the tumor specimen is grasped only with fine-toothed forceps at its extreme periphery, or preferably, traction sutures are placed in the normal marginal tissue to manipulate the specimen without directly contacting the tumor. Hemostasis is achieved using bipolar electrocautery on a low setting to avoid thermal necrosis of the remaining tissue, which can confound subsequent pathologic evaluation.
Once the specimen is completely excised, it is critical to orient it for the pathologist. A standard marking system is employed (e.g., a short silk suture placed superiorly, a long silk suture placed laterally). This allows the pathologist to precisely localize any close or positive margins, directing the surgeon exactly where to take additional tissue if necessary.
Sentinel Lymph Node Biopsy (SLNB)
For melanomas of intermediate thickness (typically > 0.8 mm Breslow thickness, or thinner lesions with ulceration or high mitotic rate) and for high-risk SCCs, a Sentinel Lymph Node Biopsy is performed concurrently. This procedure relies on the principle that lymphatic metastasis occurs sequentially, first draining to a specific "sentinel" node before disseminating throughout the regional basin.
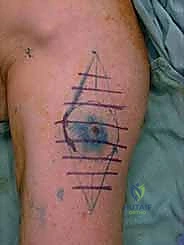
Preoperatively, a radiocolloid (Technetium-99m sulfur colloid) is injected intradermally around the primary tumor site, and lymphoscintigraphy is performed to map the lymphatic drainage. Intraoperatively, immediately prior to the primary tumor excision, Isosulfan blue or methylene blue dye is injected intradermally at the tumor periphery. The surgeon then utilizes a handheld gamma probe to trace the radiotracer to the axillary or epitrochlear basin. An incision is made over the area of maximum radioactivity, and careful dissection is performed to identify the sentinel node, which is typically stained blue and highly radioactive. The node is excised, and the bed is checked with the gamma probe to ensure the background radiation has dropped to less than 10% of the excised node's activity, confirming complete removal of all sentinel nodes.
Subungual Excision and Ray Amputation
For invasive subungual malignancies, amputation is frequently required. The level of amputation is dictated by the proximal extent of the tumor. For lesions confined to the distal phalanx, a disarticulation at the DIP joint is performed. The incision is designed with a volar V-Y or volar advancement flap to provide robust soft tissue coverage over the distal bone stump.
The extensor and flexor tendons are sharply transected under tension so they retract proximally into the wound bed. The collateral ligaments are released, and the distal phalanx is disarticulated. The articular cartilage of the middle phalanx head is often resected with a rongeur or oscillating saw to promote soft tissue adherence and prevent a bulbous, painful stump. The digital nerves are identified, drawn distally under gentle traction, and sharply transected, allowing them to retract deep into the soft tissue bed, well away from the surgical scar, to minimize the risk of a symptomatic terminal neuroma.
Soft Tissue Reconstruction and Coverage
Once negative margins are confirmed—either via intraoperative frozen section for SCC or expedited permanent section for melanoma—reconstruction commences. If a Full-Thickness Skin Graft (FTSG) is selected, it is harvested to exactly match the dimensions of the defect. The graft is meticulously defatted using tenotomy scissors to ensure optimal inosculation and revascularization from the recipient bed. The graft is inset using fine non-absorbable sutures, and a bolster dressing (tie-over dressing) is applied to provide uniform pressure, prevent hematoma formation, and immobilize the graft against the recipient bed.
For defects requiring flap coverage, local random-pattern flaps (e.g., Z-plasty, rhomboid flaps) or axial-pattern flaps (e.g., cross-finger flap for volar digital defects) are elevated and inset. Flap inset must be tension-free to prevent distal marginal necrosis. Meticulous hemostasis prior to flap inset is critical, as a sub-flap hematoma will rapidly lead to venous congestion and flap failure.
Complications, Incidence Rates, and Salvage Management
Surgical intervention for hand malignancies carries a significant risk profile, encompassing both oncologic failures and reconstructive complications. The surgeon must be adept at recognizing and managing these adverse events promptly.
Oncologic Failure and Recurrence
Local recurrence is the most dreaded oncologic complication, indicating inadequate primary resection or the presence of aggressive, unrecognized satellite micro-metastases. The incidence of local recurrence for cutaneous SCC of the hand ranges from 2% to 9%, while melanoma recurrence rates are highly variable and dependent on initial Breslow thickness and biologic tumor behavior. Recurrence demands a comprehensive restaging workup, including a repeat biopsy and advanced cross-sectional imaging. Salvage management typically involves a radically wider re-excision, frequently necessitating amputation of the involved digit or ray, followed by consideration of adjuvant radiation therapy or systemic immunotherapy.
Regional nodal recurrence or distant metastasis represents a systemic failure. In-transit metastases in melanoma are particularly challenging and may be managed with isolated limb perfusion/infusion (ILP/ILI) using chemotherapeutic agents like melphalan, or systemic targeted therapies. The prognosis drops precipitously once distant visceral metastases are identified.
Reconstructive and Functional Complications
Reconstructive complications are common given the delicate nature of hand surgery. Skin graft failure, occurring in approximately 5-10% of cases, is usually secondary to hematoma formation, shear forces disrupting neovascularization, or underlying infection. Partial graft loss can often be managed with conservative local wound care, while complete loss requires debridement and re-grafting. Flap necrosis is a more severe complication, resulting from excessive tension, venous congestion, or arterial insufficiency. Salvage requires urgent return to the operating room for release of tension, evacuation of hematoma, or, in the case of complete flap failure, debridement and coverage with a larger regional flap or free tissue transfer.
Functional complications include severe joint stiffness, tendon adhesions, and symptomatic neuromas. Prolonged immobilization to protect grafts or flaps invariably leads to capsular contracture and tendon adherence. Terminal neuromas occur when a transected nerve stump becomes entrapped in scar tissue, causing exquisite pain and hyperesthesia. Neuroma management involves surgical exploration, resection of the neuroma, and burying the nerve stump deep into adjacent muscle or bone to isolate it from mechanical stimulation. Lymphedema of the upper extremity is a significant long-term complication following axillary lymph node dissection (ALND), occurring in up to 20% of patients, and requires lifelong management with compression garments and specialized physical therapy.
| Complication | Estimated Incidence | Prevention & Salvage Management |
|---|---|---|
| Local Tumor Recurrence | 2% - 15% (varies by histology) | Prevention: Strict adherence to margin guidelines; frozen sections. Salvage: Radical re-excision; amputation; adjuvant radiation. |
| Skin Graft Failure | 5% - 10% | Prevention: Meticulous hemostasis; tie-over bolster dressing; strict immobilization. Salvage: Debridement and re-grafting. |
| Flap Necrosis | 2% - 5% | Prevention: Tension-free inset; preservation of pedicle geometry. Salvage: Suture release; leech therapy (venous congestion); re-flap. |
| Symptomatic Neuroma | 5% - 15% (post-amputation) | Prevention: Sharp nerve transection under tension; burying stump in muscle/bone. Salvage: Excision and relocation of nerve stump. |
| Upper Extremity Lymphedema | 5% - 20% (post-ALND) | Prevention: SLNB instead of routine ALND when possible. Salvage: Complex decongestive therapy; compression garments; lymphovenous bypass. |
Phased Post-Operative Rehabilitation Protocols
The ultimate functional outcome of any hand reconstruction is heavily dependent on a rigorously structured, phased postoperative rehabilitation program. The hand surgeon and the certified hand therapist (CHT) must work in lockstep to balance the competing demands of tissue healing and functional mobilization.
Phase I: Immobilization and Graft/Flap Protection
The initial postoperative phase (Days 1 to 10-14) is dedicated entirely to protecting the surgical site and ensuring the viability of the reconstruction. The hand is immobilized in a bulky, non-compressive dressing, reinforced with a custom-molded orthoplastic splint. The wrist is typically positioned in slight extension (20-30 degrees), the metacarpophalangeal (MCP) joints in 70-90 degrees of flexion, and the interphalangeal (IP) joints in full extension—the
