Complex Tibial Shaft Fracture: Plate Fixation for Plafond Extension
Key Takeaway
We review everything you need to understand about Complex Tibial Shaft Fracture: Plate Fixation for Plafond Extension. A **tibial shaft fracture** extending into the plafond is a complex injury characterized by a displaced, often multifragmentary break in the midshaft of the tibia that also involves the ankle joint's articular surface. These severe fractures commonly require immediate fasciotomy if compartment syndrome is present, followed by open reduction and internal fixation (ORIF) to restore anatomical alignment and joint function.
Comprehensive Introduction and Patho-Epidemiology
The management of complex tibial shaft fractures with extension into the distal articular surface (the tibial plafond or pilon) represents one of the most formidable challenges in orthopedic traumatology. These injuries typically result from high-energy mechanisms, such as a fall from a significant height or a motor vehicle collision, where axial loading forces are combined with severe rotational and shear vectors. The classic presentation, as highlighted in our index case of a 26-year-old male who fell 3 meters into a hole, involves not only catastrophic bony disruption but also devastating injury to the surrounding soft tissue envelope. The delicate nature of the soft tissues in the distal third of the leg, characterized by sparse muscular coverage and a precarious vascular supply, dictates the entire trajectory of clinical decision-making.
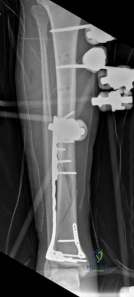
When a diaphyseal fracture propagates into the distal articular block, the injury transcends the typical treatment algorithms reserved for isolated tibial shaft fractures. Intramedullary nailing, the gold standard for diaphyseal fractures, becomes fraught with complications such as articular malreduction, propagation of intra-articular fracture lines, and inadequate distal fixation. Therefore, plate fixation—often utilizing minimally invasive percutaneous plate osteosynthesis (MIPPO) techniques—emerges as the primary definitive treatment modality. In the setting of an AO/OTA 43C3.3 fracture, where the articular surface is multifragmentary and completely dissociated from the diaphysis, the surgeon must meticulously reconstruct the joint surface before bridging the diaphyseal segment.
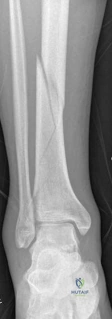
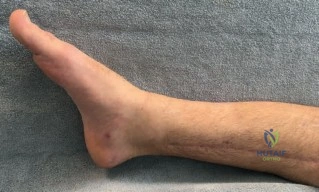
The patho-epidemiology of these injuries is inextricably linked to the incidence of acute compartment syndrome. High-energy axial loads result in rapid swelling, hemorrhage, and edema within the unyielding fascial compartments of the leg. As demonstrated in our reference case, clinical examination often reveals a tense, swollen limb necessitating an immediate four-compartment fasciotomy. The dual-incision technique remains the standard of care to decompress the anterior, lateral, superficial posterior, and deep posterior compartments. The presence of fasciotomy wounds further complicates the surgical approach for definitive internal fixation, requiring strict adherence to the principles of damage control orthopedics (DCO).
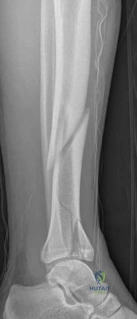
Initial management in these high-velocity scenarios mandates the application of a spanning external fixator to achieve skeletal traction, restore length, and allow the soft tissue envelope to recover. This temporary stabilization minimizes ongoing secondary soft tissue trauma from mobile fracture fragments. However, the application of external fixators is not without risk; meticulous pin placement is required. For instance, calcaneal transfixion pins must be placed with strict attention to the neurovascular bundle to avoid iatrogenic tibial nerve irritation, an issue that required revision in the early phase of our index patient's care.
Detailed Surgical Anatomy and Biomechanics
A profound understanding of the distal tibia's surgical anatomy and the biomechanical principles of fracture fixation is non-negotiable for the operating surgeon. The distal tibia expands from a triangular diaphyseal cross-section to a rectangular metaphyseal flare, culminating in the articular plafond. The plafond itself is anatomically divided into three primary columns or fragments: the medial malleolus, the anterolateral (Chaput) fragment, and the posterior (Volkmann) fragment. The syndesmotic ligamentous complex binds the distal tibia to the fibula, playing a critical role in ankle mortise stability. In high-energy axial load injuries, the talus acts as a hammer, driving upward into the plafond and causing central impaction and comminution that is often devoid of soft tissue attachments.

The vascular anatomy of the distal leg is notoriously unforgiving. The anterior tibial, posterior tibial, and peroneal arteries supply specific angiosomes. The anteromedial face of the tibia is subcutaneous, lacking muscular coverage, and relies entirely on a delicate periosteal and fascial blood supply. Surgical incisions must respect these angiosomes to prevent wound necrosis. The traditional extensile approaches have largely been abandoned in favor of targeted, tissue-sparing incisions. When planning plate fixation, the surgeon must decide between an anterolateral approach, which utilizes the muscular bed of the anterior compartment for coverage, or a medial approach, which carries a higher risk of wound dehiscence but provides excellent access to the medial column.
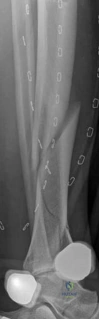
Biomechanically, the transition from the rigid diaphysis to the cancellous metaphysis creates a stress riser. When utilizing plate osteosynthesis for a fracture extending from the shaft into the plafond, the construct must fulfill two distinct biomechanical roles: absolute stability at the articular surface and relative stability along the multifragmentary diaphysis. Absolute stability of the articular block is achieved through anatomic reduction and interfragmentary compression using lag screws. This reconstructs the joint and provides a solid foundation.
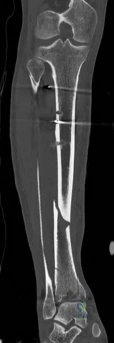
Once the articular block is reconstituted, the plate acts as a bridging construct across the zone of metaphyseal and diaphyseal comminution. Locking plate technology is paramount in this region. The locking screws provide angular stability, functioning as an internal fixator that does not rely on friction between the plate and the underlying periosteum. This preserves the extraosseous blood supply, which is vital for secondary bone healing via callus formation. The working length of the plate must be optimized to allow for micromotion at the fracture site, promoting robust enchondral ossification while preventing catastrophic hardware failure.
Exhaustive Indications and Contraindications
The decision-making process regarding the timing and modality of surgical intervention in complex tibial shaft fractures with plafond extension requires a nuanced appreciation of patient physiology, soft tissue status, and fracture morphology. The implementation of a staged protocol—initial spanning external fixation followed by delayed definitive internal fixation—has drastically reduced the historical rates of deep infection and wound sloughing.
| Category | Specific Criteria | Clinical Rationale |
|---|---|---|
| Indications for Spanning Ex-Fix | Gross soft tissue swelling, fracture blisters, open fractures (Tscherne II/III), acute compartment syndrome requiring fasciotomy. | Allows soft tissue resuscitation, restores length/alignment, and facilitates wound care and repeated debridements. |
| Indications for Definitive Plating | Resolution of soft tissue edema ("wrinkle sign" present), epithelialization of fracture blisters, clean and granulating fasciotomy beds. | Provides necessary biomechanical stability for articular reconstruction and diaphyseal bridging, enabling early ROM. |
| Absolute Contraindications | Active deep infection, profound peripheral vascular disease, non-reconstructable soft tissue envelope, medically unstable polytrauma patient. | High risk of amputation, hardware seeding, and systemic decompensation. Requires alternative salvage strategies. |
| Relative Contraindications | Severe osteopenia/osteoporosis, uncontrolled diabetes mellitus, heavy tobacco use, severe psychiatric non-compliance. | Increased risk of hardware pullout, delayed union, nonunion, and catastrophic postoperative wound complications. |
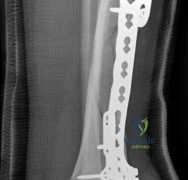
In the setting of acute compartment syndrome, the presence of fasciotomy wounds fundamentally alters the surgical timeline. The primary goal is the preservation of limb viability through immediate decompression. Once the external fixator is applied, the fasciotomy wounds are typically managed with negative pressure wound therapy (NPWT) or vessel loops (shoelace technique) to facilitate gradual closure. Definitive internal fixation must be delayed until the soft tissue envelope is deemed capable of withstanding further surgical insult, which often takes 10 to 21 days.
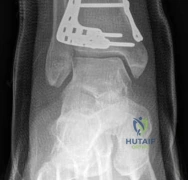
When evaluating the patient for definitive fixation, the surgeon must assess the "wrinkle sign"—the return of normal skin creasing indicating the resolution of interstitial edema. Proceeding with definitive plating through swollen, indurated tissues is a recipe for disaster, frequently leading to wound dehiscence and deep hardware infection. If the soft tissues fail to recover adequately, or if the patient is a poor candidate for extensive internal fixation, definitive management in a circular fine-wire frame (e.g., Ilizarov or Taylor Spatial Frame) may be indicated as a viable alternative to plating.
Pre-Operative Planning, Templating, and Patient Positioning
Pre-operative planning is the cornerstone of successful execution in complex pilon-variant tibial shaft fractures. The surgeon must transition from a conceptual understanding of the injury to a concrete, step-by-step surgical blueprint. This begins with high-quality orthogonal radiographs of the entire tibia, ankle, and knee. However, plain films drastically underestimate the degree of articular comminution and central impaction. A fine-cut computed tomography (CT) scan with 2D multiplanar reformats (coronal and sagittal) and 3D surface rendering is absolutely mandatory.
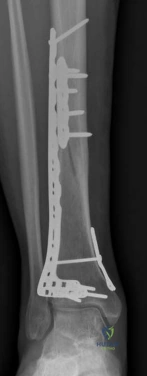
The CT scan allows the surgeon to map the fracture lines, identify the primary articular fragments (Chaput, Volkmann, medial malleolus), and quantify the degree of central die-punch impaction. In an AO/OTA 43C3.3 fracture, where no articular fragment is in continuity with the diaphysis, the surgeon must plan the sequence of reduction. Typically, the fibula is addressed first to restore lateral column length and rotation, provided the fibular fracture is not located at the level of the syndesmosis where fixation might interfere with the lateral surgical approach to the tibia.
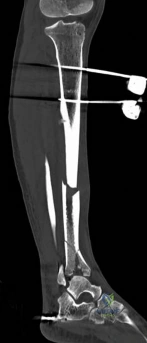
Digital templating is utilized to select the appropriate implant. For a fracture extending into the diaphysis, an extra-long anatomical distal tibia locking plate is required. The surgeon must determine whether an anterolateral or medial plate (or dual plating) will provide the optimal biomechanical construct based on the fracture morphology. The trajectory of the distal locking screws must be planned to provide a subchondral raft supporting the articular surface without penetrating the joint space. Furthermore, the availability of bone graft or orthobiologics must be confirmed, as elevating impacted articular segments will leave a metaphyseal void requiring structural support.
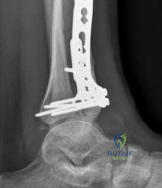
Patient positioning is critical for facilitating intra-operative imaging and surgical access. The patient is placed supine on a radiolucent Jackson or flat Jackson-type table. A bump is placed under the ipsilateral hip to correct the natural external rotation of the lower extremity, bringing the patella and ankle mortise into a neutral, upward-facing position. A sterile tourniquet is applied to the proximal thigh. The entire limb is prepped and draped free, allowing for unrestricted manipulation. The fluoroscopy unit (C-arm) is positioned on the contralateral side of the table, ensuring that perfect AP, lateral, and mortise views can be obtained effortlessly throughout the procedure.
Step-by-Step Surgical Approach and Fixation Technique
Soft Tissue Management and Approach Selection
The surgical approach must be carefully orchestrated, particularly in a patient with pre-existing fasciotomy incisions. If an anterolateral approach is selected, the incision is typically centered over the interval between the tibialis anterior and the extensor hallucis longus (EHL), or between the EHL and the extensor digitorum longus (EDL). The superficial peroneal nerve must be meticulously identified and protected, as it often crosses the surgical field in the distal third of the leg. The anterior tibial artery and deep peroneal nerve are retracted laterally with the EDL.
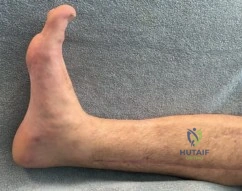
If a medial approach is utilized, the incision is made just medial to the tibial crest, avoiding the saphenous vein and nerve. The full-thickness fasciocutaneous flap is elevated off the periosteum to minimize devascularization. In cases where compartment syndrome fasciotomies have been performed, the surgeon must often incorporate the existing traumatic or surgical incisions into the definitive surgical approach to avoid creating narrow skin bridges that are prone to necrosis.
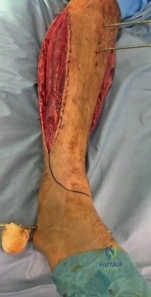
Articular Reconstruction
The first objective of the internal fixation phase is the anatomic reconstruction of the articular block. The joint capsule is incised to allow direct visualization of the plafond. A femoral distractor or a temporary external fixator spanning the joint can be utilized to gain joint space and visualize the central impacted fragments. Using a dental pick or a Freer elevator, the central die-punch fragments are carefully disimpacted and brought down flush with the talar dome.
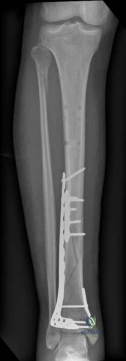
Once the articular surface is visually and fluoroscopically reduced, the resultant metaphyseal void is densely packed with cancellous allograft, autograft, or synthetic bone substitute to prevent late subsidence. The major articular fragments (Chaput, Volkmann, and medial malleolus) are then reduced around the central reconstructed block using pointed reduction forceps. Provisional fixation is achieved with multiple 1.6mm or 2.0mm Kirschner wires. Independent 3.5mm or 4.0mm lag screws can be placed outside the planned footprint of the definitive plate to secure the articular block.

Metaphyseal-Diaphyseal Fixation
With the articular surface reconstituted, the surgeon's focus shifts to bridging the complex metaphyseal-diaphyseal dissociation. A pre-contoured anatomical locking plate is slid submuscularly or subcutaneously along the diaphysis using a MIPPO technique. The plate is positioned on the anterolateral or medial surface, depending on the preoperative plan and soft tissue constraints.
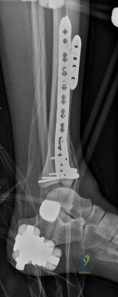
The distal portion of the plate is secured to the reconstructed articular block. It is imperative that the distal locking screws are placed parallel to the joint space, forming a rigid subchondral raft that supports the articular cartilage. Fluoroscopy is utilized extensively to ensure no screws have penetrated the joint. Once the distal block is secured to the plate, the diaphyseal segment is aligned. Length, alignment, and rotation are restored using manual traction or the femoral distractor. The proximal portion of the plate is then secured to the diaphysis using a combination of non-locking screws (to pull the bone to the plate) and locking screws (to create a fixed-angle construct). The working length of the plate is maximized by leaving several screw holes empty over the zone of comminution, promoting secondary bone healing.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique and adherence to staged protocols, complex tibial shaft fractures with plafond extension remain plagued by high complication rates. The combination of severe soft tissue trauma, tenuous vascularity, and complex intra-articular comminution creates a perfect storm for adverse outcomes.
| Complication | Estimated Incidence | Pathophysiology & Clinical Management |
|---|---|---|
| Deep Surgical Site Infection | 5% - 15% | Driven by soft tissue necrosis and compromised vascularity. Requires aggressive serial debridements, hardware removal if stability is lost, targeted IV antibiotics, and often soft tissue coverage (free flap). |
| Wound Dehiscence | 10% - 20% | Results from operating through edematous tissue or poor incision planning. Managed with NPWT, local wound care, and potential rotational or free tissue transfer. |
| Nonunion / Delayed Union | 10% - 25% | Caused by excessive periosteal stripping, rigid fixation of comminuted zones, or infection. Treated with autologous bone grafting, exchange plating, or conversion to a circular frame. |
| Post-Traumatic Osteoarthritis | 30% - 50% | Secondary to initial cartilage impact damage (chondrocyte apoptosis) and residual articular step-off. Managed conservatively initially; definitive salvage is ankle arthrodesis. |
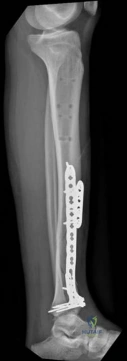
In cases involving acute compartment syndrome, the sequelae can be particularly devastating. Even with prompt fasciotomy, some degree of muscle necrosis may occur, leading to late fibrotic contractures, particularly of the deep posterior compartment (resulting in claw toes and equinus contracture). Neurologic deficits, such as foot drop from deep peroneal nerve ischemia, may be permanent, necessitating subsequent tendon transfers or ankle-foot orthoses (AFOs).
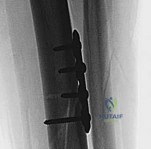
When joint-preserving procedures fail due to advanced post-traumatic osteoarthritis, severe avascular necrosis of the distal tibial block, or intractable deep infection, salvage management is required. Ankle arthrodesis remains the gold standard for painful, arthritic pilon nonunions. In cases of massive bone loss or recalcitrant infection, a tibiotalocalcaneal (TTC) fusion utilizing a retrograde intramedullary nail or a circular external fixator with bone transport may be necessary to salvage a functional, plantigrade limb. In the most extreme cases, where limb salvage has failed after multiple reconstructive attempts, a below-knee amputation (BKA) may provide the patient with the highest functional outcome and quality of life.
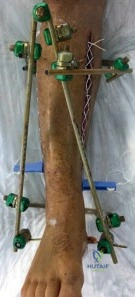

Phased Post-Operative Rehabilitation Protocols
The rehabilitation following plate fixation of a complex tibial shaft fracture with plafond extension is a marathon, not a sprint. The protocol must carefully balance the need for early joint mobilization to prevent stiffness and nourish articular cartilage with the absolute necessity of protecting the fragile osteosynthesis construct from premature mechanical failure.
Phase I: Immediate Post-Operative Period (Weeks 0-2)
The primary goals in the acute phase are wound healing, edema control, and pain management. The limb is placed in a bulky, well-padded posterior splint with the ankle in neutral dorsiflexion to prevent equinus contracture. The patient is strictly non-weight-bearing (NWB) on the operative extremity. Elevation above the level of the heart is mandatory to facilitate venous and lymphatic drainage. Deep vein thrombosis (DVT) prophylaxis is initiated per institutional protocols. At the two-week mark, sutures or staples are removed, provided the wounds (including fasciotomy sites) are adequately healed.
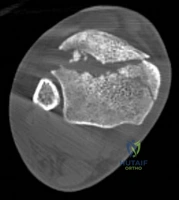
Phase II: Early Mobilization (Weeks 2-6)
Once the soft tissue envelope is secure, the patient is transitioned to a removable controlled ankle motion (CAM) boot. Strict NWB status is maintained. The patient is instructed to remove the boot multiple times a day to perform active and active-assisted range of motion (ROM) exercises of the ankle and subtalar joints. Early motion is critical for preventing capsular fibrosis and promoting the diffusion of synovial fluid, which provides nutrition to the healing articular cartilage. Strengthening of the proximal musculature (quadriceps, hamstrings, gluteals) is encouraged to prevent profound deconditioning.
Phase III: Progressive Weight-Bearing (Weeks 6-12)
At the 6-to-8-week mark, clinical and radiographic evaluations are performed to assess for early callus formation at the diaphyseal fracture site and maintenance of articular reduction. If signs of early clinical union are present, the patient may begin progressive partial weight-bearing (PWB), typically starting at 20-30 lbs and advancing by 10-15 lbs per week. Pool therapy or an anti-gravity treadmill can be highly beneficial during this transition. Physical therapy focuses on proprioception, intrinsic foot muscle strengthening, and aggressive ankle ROM.
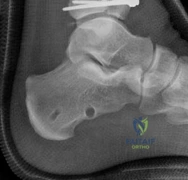
Phase IV: Advanced Rehabilitation and Return to Function (Weeks 12+)
Full weight-bearing (FWB) is generally permitted between 10 and 12 weeks, contingent upon radiographic evidence of bridging callus across three of four cortices. The focus of therapy shifts to gait normalization, closed-kinetic-chain strengthening, and functional specific activities. Patients must be counseled that maximal medical improvement (MMI) may not be reached for 12 to 18 months post-injury. Persistent swelling, aching pain after prolonged standing, and some degree of permanent stiffness are common and should be discussed early in the postoperative course to manage patient expectations.
Summary of Landmark Literature and Clinical Guidelines
The modern management of complex tibial plafond fractures is built upon decades of evolving surgical philosophy and landmark clinical studies. Understanding this literature is essential for the academic orthopedic surgeon.
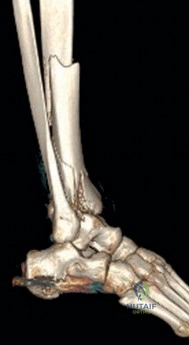
The foundational principles of articular reconstruction were established by Rüedi and Allgöwer in 1969. They outlined four classic steps: (1) restoration of fibular length, (2) reconstruction of the tibial articular surface, (3) use of cancellous bone graft to fill metaphyseal defects, and (4) rigid internal fixation with plates. While their initial results were excellent in low-energy skiing injuries, the application of these immediate, rigid plating techniques to high-energy trauma resulted in disastrous complication rates, including soft tissue sloughing and deep infection rates approaching 30-50%.
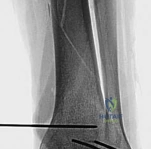
This unacceptably high complication profile led to a paradigm shift formalized by Sirkin et al. (1999) and Patterson and Krause (1999). These landmark papers introduced the staged protocol: immediate spanning external fixation for soft tissue resuscitation, followed by delayed definitive internal fixation at 10 to 21 days. This approach drastically reduced the incidence of deep infection and wound complications, cementing the staged protocol as the current gold standard for high-energy pilon and complex tibial shaft fractures.
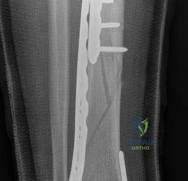
More recently, the literature has focused on the biomechanics and clinical outcomes of Minimally Invasive Percutaneous Plate Osteosynthesis (MIPPO). Studies by Borg et al. (2004) and Helfet et al. have demonstrated that preserving the extraosseous blood supply through submuscular plating techniques yields high union rates and minimizes soft tissue stripping. Current clinical guidelines strongly advocate for the integration of CT-based preoperative planning, staged management for high-energy injuries, and the use of anatomically contoured locking plates applied via MIPPO techniques to optimize both biological healing and mechanical stability in these devastating injuries.
