Smith and Colles Fractures: Understand Their Crucial Distinctions
Key Takeaway
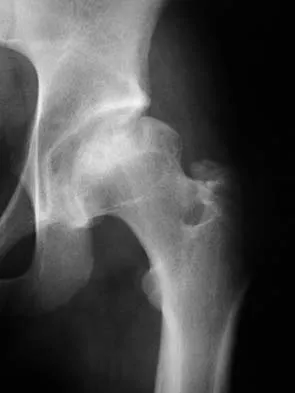
Here are the crucial details you must know about Smith and Colles Fractures: Understand Their Crucial Distinctions. Smith and Colles fractures are two distinct wrist breaks involving the distal radius bone. A Smith fracture occurs when the broken bone moves towards the palm, often due to forceful wrist flexion. Conversely, a Colles fracture involves the bone displacing towards the back of the hand, typically from forceful wrist extension. Both require medical treatment for proper healing.
Introduction and Epidemiology
Distal radius fractures represent one of the most frequently encountered injuries in orthopedic traumatology, accounting for approximately one sixth of all fractures treated in emergency departments. Among these, the Colles and Smith fractures represent two distinct pathological entities with opposing mechanisms of injury, displacement patterns, and biomechanical considerations. Understanding the crucial distinctions between these fracture patterns is paramount for orthopedic surgeons to execute appropriate reduction maneuvers, select optimal fixation constructs, and mitigate long term functional deficits.
The Colles fracture, first described by Abraham Colles in 1814, is defined as an extra-articular fracture of the distal radius characterized by dorsal comminution, dorsal angulation, dorsal displacement, and radial shortening. It is the most common distal radius fracture pattern. Epidemiologically, it presents with a bimodal distribution. In the elderly population, predominantly postmenopausal females, it occurs following low energy trauma such as a fall on an outstretched hand. In younger cohorts, it is typically the result of high energy trauma, including motor vehicle collisions or sports related injuries.
Conversely, the Smith fracture, described by Robert William Smith in 1847, is often referred to as a reverse Colles fracture. It is an extra-articular fracture of the distal radius characterized by volar angulation and volar displacement of the distal fragment. Smith fractures are significantly less common, comprising less than five percent of all distal radius fractures. The mechanism of injury typically involves a fall onto a flexed wrist or a direct blow to the dorsum of the hand. While it shares the bimodal age distribution of the Colles fracture, the inherent instability of the volar displacement often necessitates a higher index of suspicion for operative intervention.
Surgical Anatomy and Biomechanics
Osteology of the Distal Radius
The distal radius is structurally complex, transitioning from the dense diaphyseal cortical bone to the metaphyseal cancellous bone, which is highly susceptible to compressive failure. Normal radiographic parameters of the distal radius are critical benchmarks for anatomical reduction. The radial inclination averages 22 degrees, radial height averages 11 to 12 millimeters, and volar tilt averages 11 degrees.
The articular surface features two distinct fossae separated by an interfossal ridge. The scaphoid fossa is triangular and lateral, while the lunate fossa is quadrilateral and medial. The sigmoid notch articulates with the distal ulna to form the distal radioulnar joint. The three column theory of Rikli and Regazzoni divides the distal forearm into the radial column (radial styloid and scaphoid fossa), the intermediate column (lunate fossa and sigmoid notch), and the ulnar column (distal ulna and triangular fibrocartilage complex). Colles and Smith fractures primarily disrupt the radial and intermediate columns, though ulnar styloid avulsions frequently compromise the ulnar column.
Ligamentous and Soft Tissue Anatomy
The distal radius is stabilized by a robust network of extrinsic and intrinsic ligaments. The volar radiocarpal ligaments, including the radioscaphocapitate, long radiolunate, and short radiolunate ligaments, are thick and provide primary stability to the carpus. The dorsal radiocarpal ligaments are comparatively thinner.
The watershed line is a critical surgical landmark on the volar aspect of the distal radius. It is a transverse ridge marking the distal margin of the pronator quadratus fossa and the origin of the volar radiocarpal ligaments. Hardware placed distal to this line significantly increases the risk of flexor tendon irritation and subsequent rupture, particularly the flexor pollicis longus.
Biomechanics of Injury
The biomechanical forces dictating the fracture pattern depend on the position of the wrist at the time of impact. In a Colles fracture, the wrist is typically extended between 40 and 90 degrees during a fall on an outstretched hand. The force transmission results in tension failure of the volar cortex and compression failure of the dorsal cortex, leading to the characteristic dorsal comminution and loss of volar tilt.
In a Smith fracture, the wrist is flexed, or a direct dorsal impact occurs. This creates tension along the dorsal cortex and compression along the volar cortex. The resulting volar comminution and volar displacement create a highly unstable configuration. The deforming forces of the forearm musculature further exacerbate displacement. The brachioradialis exerts a proximal and radial translation force on the radial styloid, while the pronator quadratus pulls the distal fragment toward the ulna and into pronation.
Indications and Contraindications
The decision to pursue operative versus non-operative management hinges on patient specific factors, functional demands, and the radiographic stability of the fracture. The Lafontaine criteria are frequently utilized to predict instability following closed reduction. These include initial dorsal angulation greater than 20 degrees, dorsal comminution, intra-articular extension, associated ulnar fracture, and patient age over 60 years.
While Colles fractures in low demand, elderly patients may often be managed non-operatively even with imperfect radiographic parameters, Smith fractures are inherently more unstable due to the volar shear forces and the trajectory of the flexor tendons. Volar displacement is notoriously difficult to maintain in a cast, making operative fixation the standard of care for the majority of Smith fractures.
| Parameter | Non-Operative Criteria | Operative Criteria |
|---|---|---|
| Radial Shortening | Less than 3 millimeters | Greater than 3 to 5 millimeters |
| Dorsal Tilt (Colles) | Less than 10 degrees dorsal tilt | Greater than 10 degrees dorsal tilt |
| Volar Tilt (Smith) | Restored to neutral or anatomic | Uncorrectable volar angulation |
| Intra-articular Step-off | Less than 2 millimeters | Greater than 2 millimeters |
| Fracture Stability | Stable post closed reduction | Loss of reduction in cast |
| Patient Profile | Low functional demand or high surgical risk | High functional demand and medically optimized |
| Associated Injuries | Isolated injury | Concomitant carpal or neurovascular injury |
Absolute contraindications to operative intervention include active local infection, critically compromised soft tissue envelopes precluding safe incision, and patients who are medically unstable for anesthesia. Relative contraindications include severe baseline dementia precluding postoperative compliance, or advanced osteoporosis where hardware purchase is deemed impossible, though modern locked plating has significantly expanded the indications in osteoporotic bone.
Pre Operative Planning and Patient Positioning
Radiographic Evaluation and Templating
Comprehensive preoperative imaging is mandatory. Standard orthogonal views must include a posteroanterior, true lateral, and oblique radiograph of the wrist. The true lateral view is critical for assessing volar tilt, dorsal comminution, and the sagittal alignment of the carpus. A teardrop angle measurement can aid in evaluating the lunate facet.
Computed tomography is highly recommended for any fracture exhibiting intra-articular extension to assess articular step-off, gap formation, and the presence of a die punch fragment. While classic Colles and Smith fractures are extra-articular, complex variants often involve the radiocarpal joint. Digital templating is utilized to determine plate length, width, and the trajectory of distal locking screws to ensure they support the subchondral bone without penetrating the joint.
Patient Positioning and Anesthesia
Surgical management is typically performed under regional anesthesia, such as an axillary or supraclavicular brachial plexus block, often supplemented with intravenous sedation or general anesthesia depending on patient preference and comorbidities.
The patient is positioned supine on the operating table with the operative extremity extended onto a radiolucent hand table. A pneumatic tourniquet is applied to the proximal arm. The limb is prepped and draped in a standard sterile fashion. Fluoroscopy is positioned either parallel or perpendicular to the hand table, ensuring unimpeded access for orthogonal intraoperative imaging.
Detailed Surgical Approach and Technique
The Modified Henry Volar Approach
The advent of anatomically contoured volar locking plates has made the volar approach the gold standard for both Smith and Colles fractures. The modified Henry approach provides excellent exposure of the distal radius while utilizing a safe internervous plane.
An 8 to 10 centimeter longitudinal incision is made over the flexor carpi radialis tendon, extending distally to the wrist crease. Subcutaneous tissue is bluntly dissected to protect the palmar cutaneous branch of the median nerve, which lies ulnar to the flexor carpi radialis. The flexor carpi radialis tendon sheath is incised longitudinally, and the tendon is retracted ulnarly. The deep posterior sheath is then incised, exposing the underlying flexor pollicis longus and the pronator quadratus.
The internervous plane lies between the median nerve innervated structures medially and the radial nerve innervated brachioradialis laterally. The radial artery is identified laterally and carefully protected or retracted radially. The pronator quadratus is identified and released from its radial border in an L-shaped fashion, leaving a small cuff of tissue for later repair if possible. The muscle is elevated ulnarly to expose the volar cortex of the distal radius.
Fracture Reduction Techniques
Reduction maneuvers differ significantly between Colles and Smith fractures due to their opposing displacement patterns.
For a Colles fracture, the distal fragment is displaced dorsally. Reduction involves longitudinal traction to restore radial height, followed by volar translation and flexion of the distal fragment to restore volar tilt. The brachioradialis insertion on the radial styloid often acts as a deforming force and may require fractional lengthening or complete release to facilitate reduction. Intrafocal Kapandji pinning or the use of a Freer elevator as a joystick can assist in manipulating the distal fragment.
For a Smith fracture, the distal fragment is displaced volarly. Reduction requires longitudinal traction, dorsal translation, and extension of the distal fragment. Because the volar cortex is often comminuted, the fracture is intrinsically unstable when approached from the volar side. The volar plate itself is frequently used as a reduction tool. By securing the plate to the distal fragment first, the surgeon can use the plate as a lever to restore alignment to the radial shaft.
Internal Fixation Strategies
Volar locking plate osteosynthesis is the preferred fixation method. The plate must be positioned proximal to the watershed line to prevent flexor tendon attrition.
In Colles fractures, the volar locking plate acts as a load bearing device to support the dorsal comminution. The distal locking screws are directed dorsally and proximally to capture the dorsal cortex and support the subchondral bone of the radiocarpal joint. It is imperative to avoid dorsal screw prominence, which can lead to extensor tendon rupture, particularly the extensor pollicis longus.
In Smith fractures, the volar plate functions primarily as a buttress plate to counteract the volar shear forces. The plate must be perfectly contoured to the volar anatomy. Distal fixation is achieved with locking screws or pegs, ensuring purchase in the dense subchondral bone of the distal fragment.
Once provisional fixation is achieved with Kirschner wires or a single non-locking cortical screw in the oblong slotted hole of the plate, fluoroscopy is utilized to confirm anatomic reduction, restoration of radial parameters, and appropriate hardware placement. The distal locking screws are inserted, followed by the remaining proximal shaft screws. Thorough irrigation is performed, and the pronator quadratus is loosely reapproximated over the plate if feasible, though its functional significance remains debated in the literature.
Complications and Management
Surgical management of distal radius fractures carries inherent risks. Anticipation, early recognition, and aggressive management of these complications are essential for optimizing patient outcomes.
| Complication | Incidence Rate | Etiology and Salvage Strategy |
|---|---|---|
| Extensor Pollicis Longus Rupture | 1 to 5 percent | Caused by dorsal screw prominence or fracture hematoma in non-operative Colles. Managed via Extensor Indicis Proprius to Extensor Pollicis Longus tendon transfer. |
| Flexor Tendon Irritation or Rupture | 2 to 10 percent | Caused by plate placement distal to the watershed line. Managed by prompt hardware removal and tendon repair or reconstruction. |
| Median Nerve Neuropathy | 5 to 15 percent | Caused by fracture displacement, hematoma, or iatrogenic traction. Managed by acute carpal tunnel release if progressive, or observation if transient. |
| Complex Regional Pain Syndrome | 2 to 25 percent | Abnormal autonomic response to trauma or surgery. Managed by early recognition, aggressive multimodal pain management, stellate ganglion blocks, and intensive physical therapy. |
| Intra-articular Hardware Penetration | 1 to 3 percent | Unrecognized screw penetration into the radiocarpal or distal radioulnar joint. Prevented by meticulous fluoroscopic skyline views. Managed by immediate hardware revision. |
| Malunion | Highly variable | Failure to achieve or maintain reduction. Results in altered carpal kinematics and radiocarpal arthrosis. Managed by corrective osteotomy if symptomatic. |
| Nonunion | Less than 1 percent | Rare due to robust metaphyseal blood supply. Managed by rigid internal fixation and autologous bone grafting. |
Hardware related complications represent a significant portion of postoperative morbidity. The use of volar locking plates has decreased the incidence of dorsal tendon irritation compared to dorsal plating, but has introduced the risk of flexor tendon rupture if the watershed line is violated. Intraoperative fluoroscopic evaluation using the dorsal skyline view is mandatory to confirm that dorsal screws do not protrude past the dorsal cortex.
Post Operative Rehabilitation Protocols
Early Mobilization Phase
Modern rigid internal fixation allows for accelerated rehabilitation protocols, which have been shown to improve early functional outcomes and decrease the incidence of stiffness and Complex Regional Pain Syndrome.
Immediately postoperatively, the patient is placed in a bulky soft dressing and a removable volar splint. Active range of motion of the digits, elbow, and shoulder is initiated on postoperative day one to minimize edema and prevent tendon adhesions.
At the one to two week follow up, sutures are removed, and radiographic evaluation is performed to confirm maintenance of reduction. The patient is transitioned to a custom molded orthoplast splint to be worn between exercise sessions. Active and active assisted range of motion of the wrist and forearm (flexion, extension, pronation, and supination) is initiated under the guidance of a certified hand therapist.
Strengthening Phase
At six weeks postoperatively, clinical and radiographic assessments are performed to evaluate bony healing. Once bridging callus is visualized and the fracture is clinically stable, the protective splint is discontinued.
Progressive strengthening exercises are introduced, focusing on grip strength, intrinsic hand muscle strengthening, and dynamic stabilization of the wrist. Weight bearing and heavy lifting are typically restricted until eight to twelve weeks postoperatively, depending on the severity of the initial fracture and the radiographic evidence of consolidation. Maximum medical improvement is generally achieved between six and twelve months, though patients may continue to experience mild improvements in grip strength and range of motion for up to two years.
Summary of Key Literature and Guidelines
The management of distal radius fractures has evolved significantly, driven by advancements in implant technology and rigorous clinical research. The American Academy of Orthopaedic Surgeons Clinical Practice Guidelines provide evidence based recommendations for the treatment of these injuries.
A paradigm shift occurred with the popularization of the volar locking plate by Orbay and Fernandez in the early 2000s. Their seminal work demonstrated that fixed angle volar plating could effectively maintain reduction in unstable, dorsally comminuted Colles fractures without the need for dorsal plates or external fixation, significantly reducing the complication rates associated with those earlier modalities.
The DRAFFT (Distal Radius Acute Fracture Fixation Trial) by Costa et al. provided critical insight into the management of dorsally displaced fractures. While the trial found no clinically significant difference in patient reported outcomes at one year between volar locking plates and Kirschner wire fixation for fractures that could be closed reduced, subsequent subgroup analyses and clinical consensus maintain that volar plating provides superior early functional recovery and is biomechanically necessary for fractures with severe comminution or those that cannot be adequately reduced closed.
For Smith fractures, the literature is unequivocal regarding the necessity of a volar buttress. Jupiter and colleagues have extensively documented the biomechanical failure of dorsal fixation or cast immobilization in managing volar shear injuries. The volar locking plate acts as a definitive buttress, neutralizing the deforming forces of the flexor tendons and the pronator quadratus.
Furthermore, the management of elderly patients with Colles fractures remains a topic of active investigation. Studies by Arora et al. have demonstrated that in patients over the age of 65 with low functional demands, non-operative management with cast immobilization yields functional outcomes comparable to operative fixation, despite inferior radiographic alignment. This highlights the critical importance of tailoring the treatment strategy to the physiological age and functional requirements of the patient, rather than treating the radiograph in isolation.
In conclusion, distinguishing between Smith and Colles fractures is not merely an academic exercise but a fundamental requirement for executing appropriate surgical management. While both involve the distal radius, their opposing mechanisms, displacement patterns, and biomechanical demands dictate distinct reduction techniques and fixation strategies. Mastery of the volar approach, meticulous attention to anatomical landmarks such as the watershed line, and adherence to evidence based rehabilitation protocols are essential for optimizing functional recovery and minimizing surgical morbidity.
