Orthopedic Shoulder & Elbow MCQs: Practice Questions & Exam Preparation
Key Takeaway
This interactive board review contains 100 randomly selected orthopedic surgery questions with clinical images, immediate feedback, and detailed references.
Orthopedic Shoulder & Elbow MCQs: Practice Questions & Exam Preparation
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 72-year-old female undergoes a reverse total shoulder arthroplasty (rTSA) for severe rotator cuff tear arthropathy. Compared to the native anatomic shoulder, which of the following best describes the biomechanical alteration of the center of rotation following a standard Grammont-style rTSA?
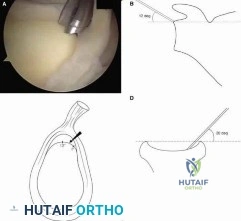
Explanation
Question 2
A 45-year-old male bodybuilder sustains an acute distal biceps tendon rupture and opts for surgical repair via a single-incision anterior approach. Postoperatively, he complains of sensory loss along the lateral aspect of his forearm. Which nerve is most commonly injured during this specific surgical approach?
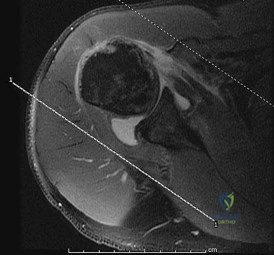
Explanation
Question 3
A 22-year-old football player presents with recurrent anterior shoulder instability. A 3D CT scan demonstrates a bipolar bone loss pattern with a Hill-Sachs lesion. Applying the 'glenoid track' concept, an 'off-track' lesion is defined by which of the following criteria?
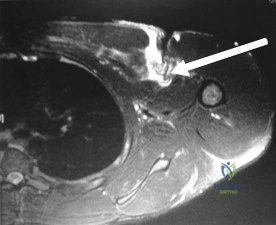
Explanation
Question 4
A 35-year-old male falls on an outstretched hand and sustains a 'terrible triad' injury of the elbow. What is the standard algorithmic sequence for surgical fixation of this injury pattern?
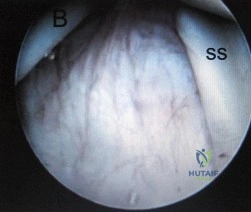
Explanation
Question 5
A 28-year-old female sustains an elbow injury following an axial load combined with a varus stress. Imaging reveals a specific fracture pattern pathognomonic for varus posteromedial rotatory instability (VPMRI). Which anatomic structure is characteristically fractured in this injury mechanism?
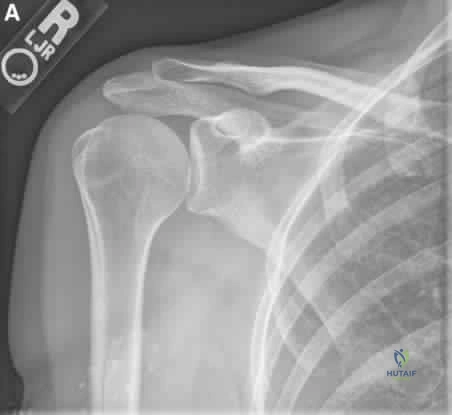
Explanation
Question 6
Historically, the arcuate branch of the anterior humeral circumflex artery was considered the primary blood supply to the humeral head. However, modern quantification studies (e.g., Hettrich et al.) have established that the predominant blood supply to the native humeral head is actually provided by which of the following vessels?
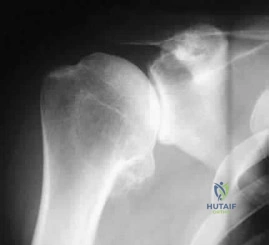
Explanation
Question 7
A 24-year-old male presents with right shoulder pain and weakness after a blunt trauma to his upper back. Physical examination reveals pronounced medial winging of the scapula that worsens when the patient is asked to perform a wall push-up. Which nerve and corresponding muscle are injured?

Explanation
Question 8
A 31-year-old volleyball player presents with deep posterior shoulder pain. MRI arthrogram reveals a posterior labral tear with an associated large paralabral cyst extending into the spinoglenoid notch. Clinically, this patient is most likely to exhibit which of the following isolated motor deficits?

Explanation
Question 9
A 30-year-old male weightlifter hears a 'pop' and experiences sudden sharp pain in his chest while bench pressing. Examination reveals a loss of the normal anterior axillary fold contour. Intraoperatively, the sternoclavicular head of the pectoralis major is found to be avulsed. What is the normal anatomic insertion of this specific head?
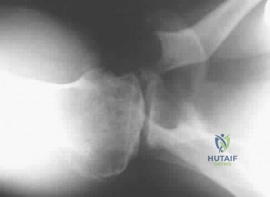
Explanation
Question 10
A 26-year-old cyclist sustains a Type V acromioclavicular (AC) joint separation requiring surgical reconstruction. The surgeon plans to drill tunnels mimicking the native coracoclavicular (CC) ligaments. Which of the following accurately describes the anatomic relationship of the CC ligaments?
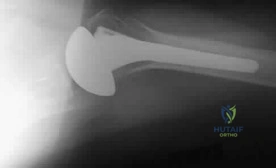
Explanation
Question 11
A 65-year-old male with a massive, retracted rotator cuff tear undergoes radiographic evaluation. According to the Hamada classification for rotator cuff tear arthropathy, what specific radiographic finding defines a Stage 3 arthropathy?
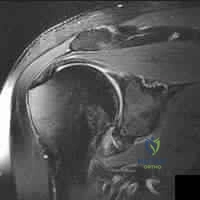
Explanation
Question 12
The anterior bundle of the ulnar collateral ligament (UCL) is the primary restraint to valgus stress at the elbow. It is subdivided into distinct bands. Which of the following accurately describes the tensioning pattern of these bands during elbow range of motion?
Explanation
Question 13
A 78-year-old female with severe, long-standing rheumatoid arthritis sustains a comminuted distal humerus fracture. A linked (semi-constrained) total elbow arthroplasty (TEA) is planned. What is the primary biomechanical advantage of utilizing a linked prosthesis over an unlinked prosthesis in this scenario?
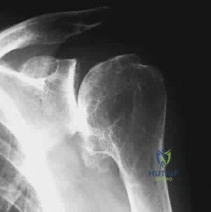
Explanation
Question 14
A 50-year-old diabetic female presents with an insidious onset of severe shoulder pain and progressive stiffness over the last 4 months. Which of the following physical examination findings is considered pathognomonic for idiopathic adhesive capsulitis?
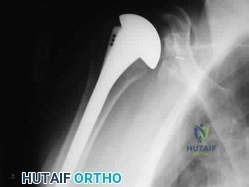
Explanation
Question 15
A 40-year-old male experiences a seizure and subsequently presents with a locked posterior shoulder dislocation. Imaging reveals a 30% anterior articular surface defect (reverse Hill-Sachs lesion). Which of the following surgical procedures is most appropriate to prevent recurrent engagement of this specific defect?
Explanation
Question 16
A 32-year-old male sustains a simple transverse fracture of the olecranon and undergoes tension band wiring. Which of the following biomechanical principles correctly describes how this construct facilitates fracture healing?
Explanation
Question 17
A 45-year-old female presents after a fall with a complex elbow fracture. Advanced imaging identifies a coronal shear fracture that involves the capitellum and extends medially to include most of the trochlea. According to the modified Bryan and Morrey classification (McKee modification), what type of fracture is this?
Explanation
Question 18
A 12-year-old elite baseball pitcher presents with medial elbow pain that worsens during the acceleration phase of throwing. Radiographs demonstrate widening of the medial epicondyle apophysis. Which muscle group is the primary deforming force contributing to this condition?
Explanation
Question 19
A 60-year-old male with severe cubital tunnel syndrome presents with noticeable intrinsic muscle wasting in his hand. When asked to firmly pinch a piece of paper between his thumb and index finger, his thumb interphalangeal joint strongly flexes. This compensatory finding (Froment's sign) is driven by which of the following muscles?
Explanation
Question 20
During a submuscular anterior transposition of the ulnar nerve, the surgeon must diligently release all potential sites of compression. One such structure is the Arcade of Struthers. Which of the following accurately describes the anatomical location of this structure?
Explanation
Question 21
A 42-year-old man presents with acute, severe, unrelenting right shoulder pain that began 3 weeks ago without any antecedent trauma. The pain lasted for 10 days and has since significantly improved, but he now notices profound weakness when trying to elevate his arm or externally rotate it. Physical examination reveals prominent atrophy of the supraspinatus and infraspinatus fossae. MRI of the shoulder reveals no rotator cuff tears, but shows diffuse T2 hyperintensity and edema within the supraspinatus and infraspinatus muscles. What is the most likely diagnosis?
Explanation
Question 22
Scapular notching is a well-recognized complication following Reverse Total Shoulder Arthroplasty (RTSA). Based on modern biomechanical principles and implant design modifications, which of the following component positioning strategies is most effective in minimizing the risk of inferior scapular notching?

Explanation
Question 23
A 28-year-old competitive weightlifter feels a sudden 'pop' and tearing sensation in his anterior chest wall while performing a heavy bench press. Examination reveals loss of the normal anterior axillary fold contour and weakness with internal rotation. In an acute pectoralis major rupture, which head is structurally most vulnerable and typically ruptures first?
Explanation
Question 24
A 35-year-old overhead athlete complains of chronic, vague posterior shoulder pain and numbness over the lateral deltoid. Physical examination demonstrates point tenderness at the posterior aspect of the shoulder, inferior to the teres minor and lateral to the long head of the triceps. Which neurovascular bundle is most likely entrapped in this anatomic space?
Explanation
Question 25
A 60-year-old active laborer presents with a massive, retracted, and irreparable posterosuperior rotator cuff tear. He has significant weakness in external rotation and a positive external rotation lag sign, but intact anterior elevation. He wishes to avoid arthroplasty. Which of the following tendon transfers is biomechanically superior for restoring active external rotation and closely replicates the force vector of the infraspinatus?
Explanation
Question 26
A 45-year-old man requires operative repair of a complete acute distal biceps tendon rupture. The surgeon must choose between a single-incision anterior approach and a two-incision approach. Compared to the single-incision technique, the two-incision approach has a historically higher risk of which of the following complications?

Explanation
Question 27
A 30-year-old patient presents with a 'terrible triad' injury of the elbow following a fall onto an outstretched hand. The injury involves an elbow dislocation, a radial head fracture, and a coronoid process fracture. According to standard surgical protocols, what is the most widely accepted sequence of structural repair to restore elbow stability?

Explanation
Question 28
A 40-year-old female presents with a 6-month history of aching pain in her proximal lateral forearm. Physical examination reveals no wrist or finger drop, but she has focal tenderness 4 cm distal to the lateral epicondyle. Pain is exacerbated by resisted extension of the middle finger with the elbow extended. In Radial Tunnel Syndrome, what is the most common anatomic site of nerve compression?
Explanation
Question 29
During elbow arthroscopy, establishing standard portals requires precise knowledge of regional neurovascular anatomy. When creating the standard anteromedial portal, which neural structure is at the greatest risk of injury due to its close proximity (often 1-2 mm) to the arthroscopic trocar?
Explanation
Question 30
A 24-year-old motorcyclist is involved in a high-speed collision and presents with massive soft tissue swelling around the shoulder girdle. AP chest radiograph shows severe lateral displacement of the scapula relative to the spinous processes and a widely displaced clavicle fracture. Examination shows a pulseless, flail upper extremity. In the setting of this suspected scapulothoracic dissociation, what is the most reliable prognostic indicator for long-term functional recovery of the limb?
Explanation
Question 31
An 18-year-old male presents to the emergency department after a football tackle complaining of severe pain at the base of his neck. He is experiencing mild stridor and a choking sensation. Clinical exam and CT imaging reveal a posterior displacement of the medial clavicle. Given the patient's age and clinical presentation, what is the most accurate anatomic description of this injury?
Explanation
Question 32
A 21-year-old collegiate baseball pitcher undergoes Medial Ulnar Collateral Ligament (MUCL) reconstruction (Tommy John surgery). The surgeon must anatomically restore the primary restraint to valgus stress at the elbow. Which bundle of the MUCL is being reconstructed, and what is its role in elbow kinematics?

Explanation
Question 33
A 48-year-old man presents with painful swelling at the posterior aspect of both elbows and inability to actively extend against resistance. He reports a sudden 'tearing' sensation bilaterally while attempting to break a fall. MRI confirms bilateral triceps tendon ruptures. Which of the following systemic medical conditions is classically most associated with bilateral spontaneous triceps tendon ruptures?
Explanation
Question 34
A 52-year-old female with poorly controlled type 1 diabetes presents with severe restriction of active and passive range of motion of her right shoulder, consistent with adhesive capsulitis (frozen shoulder). Pathophysiologically, the joint capsule in this condition demonstrates dense fibroblastic proliferation. Which of the following cytokines/growth factors is most heavily implicated in driving the fibrogenic cascade in adhesive capsulitis?
Explanation
Question 35
A 34-year-old female sustains a coronal shear fracture of the distal humerus. Imaging demonstrates that the fracture involves both the capitellum and the lateral half of the trochlea in a single contiguous articular fragment. According to the Dubberley classification, this represents a Type 3 injury. What specific radiographic feature differentiates a Dubberley Type 3B from a Type 3A injury?

Explanation
Question 36
A 28-year-old male describes a sensation of his elbow 'clicking and giving way' when he tries to push himself up from an armchair. Physical exam reveals apprehension and a clunk with a supination, valgus, and axial compression load applied to the elbow as it is moved from extension to flexion. What is the primary ligamentous restraint that is deficient, and what is its anatomic insertion on the ulna?
Explanation
Question 37
A 26-year-old man suffered a severe pan-brachial plexus avulsion injury 2 years ago and has no functional recovery of shoulder or elbow musculature, though he has undergone successful distal nerve transfers to restore rudimentary hand grip. He is scheduled for a shoulder arthrodesis to provide a stable proximal platform to aid in hand-to-mouth function. According to modern recommendations, what is the ideal position for glenohumeral fusion?
Explanation
Question 38
A 13-year-old elite Little League pitcher presents with progressive, activity-related right proximal humerus pain over the past 6 weeks. He denies any acute trauma. Plain radiographs reveal widening and irregularity of the proximal humeral physis compared to the contralateral side. What is the most appropriate initial management?
Explanation
Question 39
A 27-year-old professional volleyball attacker complains of subtle posterior shoulder pain and a subjective decrease in hitting power. Physical exam reveals normal active elevation, 5/5 strength in shoulder abduction, but notable weakness (3/5) in external rotation with the arm at the side. MRI of the shoulder is ordered. Based on the physical exam findings, where is the isolated neural compression most likely located, and what is the classic associated pathologic finding?
Explanation
Question 40
A 45-year-old man falls from a ladder and sustains a highly comminuted, unsalvageable radial head fracture (Mason III). During evaluation, he is also noted to have intense pain at the wrist and extreme instability of the distal radioulnar joint (DRUJ), indicative of an Essex-Lopresti injury. If the surgeon simply excises the radial head without replacing it, what is the most profound long-term biomechanical consequence?

Explanation
Question 41
A 45-year-old female falls on her outstretched hand. Radiographs confirm an elbow dislocation, a comminuted radial head fracture, and a Type II coronoid fracture.
According to standard surgical protocols for this 'terrible triad' injury, what is the most appropriate sequence of repair to restore elbow stability?

Explanation
Question 42
When performing a lateral ulnar collateral ligament (LUCL) reconstruction for posterolateral rotatory instability (PLRI) of the elbow, accurate graft placement is critical. Where is the precise isometric origin of the LUCL on the lateral epicondyle to ensure stability and uniform tension throughout the elbow's range of motion?
Explanation
Question 43
A 38-year-old bodybuilder sustains a distal biceps tendon rupture and undergoes a two-incision (Mayo) repair. Postoperatively, he presents with an inability to extend his fingers and thumb, though wrist extension is preserved but deviates radially. Sensation is intact. Which technical error most likely caused this complication?
Explanation
Question 44
A 29-year-old elite volleyball player presents with insidious onset of shoulder weakness. Physical examination reveals isolated atrophy of the infraspinatus fossa with normal bulk of the supraspinatus. Weakness is noted in external rotation. An MRI demonstrates a paralabral cyst. Where is the cyst most likely located, and what is the typical associated labral pathology?
Explanation
Question 45
A 22-year-old male is involved in a high-speed motorcycle collision. On examination, he has massive swelling over the shoulder girdle and a complete lack of motor and sensory function in his left upper extremity. Radiographs demonstrate marked lateral displacement of the scapula. Which radiographic parameter is most strongly predictive of a major vascular injury in this condition?
Explanation
Question 46
A 65-year-old female with severe rheumatoid arthritis undergoes a linked (semi-constrained) total elbow arthroplasty (TEA).
Three years later, she develops rapid early polyethylene wear and aseptic loosening of the components. What is the most common iatrogenic cause of early bushing wear and failure in a linked TEA?

Explanation
Question 47
A 45-year-old man receives a radial head replacement for a highly comminuted radial head fracture. Two years postoperatively, he complains of progressive lateral elbow pain and stiffness. Radiographs demonstrate widening of the lateral ulnohumeral joint space and erosive changes of the capitellum. What is the most likely cause of these findings?
Explanation
Question 48
A 32-year-old male weightlifter felt a sudden 'pop' and tearing sensation in his anterior axilla while performing a heavy bench press. Examination reveals loss of the anterior axillary fold contour. Operative repair is planned. Which of the following best describes the anatomic insertion of the most commonly ruptured segment of the pectoralis major tendon?
Explanation
Question 49
During a Latarjet procedure for recurrent anterior shoulder instability, the coracoid process is transferred to the anterior glenoid neck. Postoperatively, the patient is unable to actively flex his elbow and reports decreased sensation over the lateral forearm. Which of the following surgical steps posed the greatest risk to the injured structure?
Explanation
Question 50
A 22-year-old male with recurrent anterior shoulder dislocations undergoes arthroscopic stabilization. Imaging reveals 20% glenoid bone loss and an engaging Hill-Sachs lesion. The surgeon performs a Bankart repair and a Remplissage procedure. Which anatomic structure is tenodesed into the Hill-Sachs defect, and what clinical restriction is most commonly observed postoperatively?
Explanation
Question 51
A 28-year-old offensive lineman presents with vague posterior shoulder pain that worsens during blocking maneuvers. The surgeon performs a Kim test to evaluate for a posterior labral tear. Which of the following accurately describes the correct execution of the Kim test?
Explanation
Question 52
A 35-year-old female falls on an outstretched hand and sustains an isolated capitellar fracture.
According to the Dubberley classification of capitellum fractures, what finding distinguishes a Type 3 fracture from a Type 1 or 2, and what is its primary surgical implication?

Explanation
Question 53
A 45-year-old male loses his footing and falls directly onto a flexed elbow. He is unable to actively extend his elbow against gravity, and a palpable gap is felt posteriorly. During operative repair of this distal triceps tendon rupture, understanding the native footprint is crucial. Which of the following describes the normal anatomic insertion of the triceps tendon on the olecranon?
Explanation
Question 54
A 12-year-old competitive baseball pitcher presents with medial elbow pain that worsens during pitching. Radiographs show widening and irregularity of the medial epicondyle apophysis. What is the primary pathophysiologic mechanism causing 'Little League Elbow' in this patient population?
Explanation
Question 55
A 40-year-old female complains of a vague, aching pain in her proximal volar forearm. She reports numbness in the radial three and a half digits. Phalen's test and Tinel's sign at the carpal tunnel are negative. She experiences significant pain reproduction upon resisted pronation of the forearm while her elbow is held in full extension. Which structure is most likely causing the nerve compression?
Explanation
Question 56
A 6-year-old child presents after a fall from monkey bars. Radiographs reveal a fracture of the proximal third of the ulnar diaphysis with an anterior dislocation of the radial head.
According to the Bado classification, what type of Monteggia lesion is this, and what is the classically described mechanism of injury?

Explanation
Question 57
A 45-year-old male presents with sudden inability to make an 'OK' sign with his thumb and index finger following an episode of viral neuritis. He has normal sensation throughout the hand and forearm. Which of the following muscle groups is innervated by the specific nerve involved in this condition?
Explanation
Question 58
A 25-year-old female presents with severe, painful crepitus and snapping at the superomedial border of her scapula during active arm elevation. Extensive non-operative management has failed to provide relief. If an arthroscopic excision of the superomedial angle of the scapula is performed, which muscle's insertion must be carefully elevated and subsequently securely repaired?
Explanation
Question 59
A 30-year-old male with a devastating global brachial plexus injury (C5, C6, C7 root avulsions) is undergoing a shoulder arthrodesis to stabilize his shoulder and allow better positioning for his remaining hand/elbow function. According to current biomechanical and functional literature, what is the optimal position for glenohumeral arthrodesis?
Explanation
Question 60
A 35-year-old male sustains a closed, extra-articular fracture of the distal third of the humeral shaft (Holstein-Lewis fracture). On initial presentation in the emergency department, examination reveals a complete radial nerve palsy. According to current orthopaedic guidelines, what is the most appropriate initial management for the nerve palsy in this specific scenario?
Explanation
Question 61
A 12-year-old boy presents after falling onto an outstretched hand. He was found to have an elbow dislocation, which was closed reduced in the emergency department. Post-reduction, the elbow joint appears congruent, but the medial epicondyle is no longer visible in its anatomic position. A radiograph reveals a bone fragment within the joint space.
Which of the following is the most appropriate management for this patient?

Explanation
Question 62
During open reduction and internal fixation of a highly comminuted capitellum fracture, excessive posterior soft tissue stripping is performed. The patient subsequently develops avascular necrosis (AVN) of the capitellum. Which of the following best describes the anatomical basis for this complication?
Explanation
Question 63
A 35-year-old male presents with sudden-onset, severe right shoulder pain that awakened him from sleep. The acute severe pain lasted for 5 days and then gradually subsided, but was immediately followed by profound weakness in shoulder elevation and external rotation. An MRI of the cervical spine and shoulder is unremarkable.
What is the most likely diagnosis?

Explanation
Question 64
A professional baseball pitcher presents with vague posterior shoulder pain during the late cocking phase of throwing. Physical examination reveals an internal rotation deficit of 25 degrees compared to the non-dominant shoulder, while external rotation is increased by 10 degrees. Which of the following pathomechanical processes is most directly responsible for this glenohumeral internal rotation deficit (GIRD)?
Explanation
Question 65
A 68-year-old female with advanced rheumatoid arthritis undergoes a primary linked semi-constrained total elbow arthroplasty (TEA).
Following comprehensive postoperative rehabilitation, what specific lifelong functional limitation must she be advised to adhere to in order to minimize the risk of aseptic loosening?

Explanation
Question 66
A 28-year-old manual laborer complains of a painful grating sensation and audible popping at the superomedial border of his right scapula with overhead activities. Nonoperative management, including targeted periscapular strengthening and corticosteroid injections, has failed after 6 months. If surgical excision of the inflamed bursae is performed, which of the following bursae are specifically targeted in this region?
Explanation
Question 67
A 40-year-old female presents with a highly comminuted, un-reconstructable radial head fracture and distal radioulnar joint (DRUJ) instability after a high-energy fall.
What is the primary reason why simple radial head excision is strictly contraindicated in this specific injury pattern?

Explanation
Question 68
During the surgical management of a 'Terrible Triad' injury of the elbow, the lateral ulnar collateral ligament (LUCL) is repaired to the humerus using suture anchors.
To ensure isometric function of the LUCL throughout the arc of elbow flexion and extension, where must the humeral anchor be placed?

Explanation
Question 69
A 32-year-old elite volleyball player presents with progressive, isolated weakness in external rotation of the shoulder. He denies any acute trauma but reports deep posterior shoulder pain. Clinical examination reveals profound atrophy of the infraspinatus fossa but normal bulk and strength of the supraspinatus. Which of the following intra-articular pathologies is most commonly associated with this specific nerve entrapment syndrome?
Explanation
Question 70
A 13-year-old male baseball pitcher complains of right shoulder pain that worsens when throwing hard. He has localized tenderness over the lateral aspect of the proximal humerus. Radiographs reveal widening of the proximal humeral physis compared to the contralateral side.
What is the recommended initial management for this condition?

Explanation
Question 71
A 30-year-old male presents with severe chest wall bruising, loss of the anterior axillary fold, and weakness in internal rotation and adduction after feeling a "pop" while performing a heavy bench press.
During surgical repair of the ruptured pectoralis major tendon, the surgeon isolates the torn sternocostal head. Relative to the clavicular head footprint on the humerus, where is the anatomic footprint of the sternocostal head located?

Explanation
Question 72
A 22-year-old collegiate baseball pitcher is undergoing evaluation for medial elbow pain.
The examiner places the patient's shoulder in 90 degrees of abduction and external rotation, rapidly extends the elbow from full flexion to 30 degrees, and applies a valgus torque. The patient reports a sharp pain specifically between 120 and 70 degrees of elbow flexion. This clinical test (Moving Valgus Stress Test) evaluates the integrity of which specific structure?

Explanation
Question 73
A patient presents with poorly localized shoulder pain and paresthesias over the lateral deltoid that worsen when the arm is abducted and externally rotated. An MRI reveals fibrous bands compressing structures within the quadrilateral space. Which of the following correctly defines the anatomic borders of the quadrilateral space?
Explanation
Question 74
A 65-year-old sedentary male with a massive, irreparable rotator cuff tear and severe biceps tendinopathy is scheduled for surgery.
The surgeon discusses performing a biceps tenotomy versus a biceps tenodesis. According to highest-level current evidence (systematic reviews and meta-analyses), what is the primary expected difference in clinical outcome between these two procedures in this demographic?

Explanation
Question 75
A 45-year-old mechanic presents with an inability to actively extend his thumb and the fingers at the metacarpophalangeal (MCP) joints.
Wrist extension is preserved but distinctly deviates radially. Sensation in the hand and forearm is entirely normal. Which of the following structures is the most frequent site of compression causing this exact clinical picture?

Explanation
Question 76
A 6-year-old girl falls off monkey bars and presents with elbow swelling and forearm deformity. Radiographs demonstrate an anterior dislocation of the radial head and a fracture of the ulnar diaphysis with anterior apex angulation. Which of the following is the standard initial treatment principle for achieving and maintaining reduction of the radial head in this specific fracture-dislocation (Bado Type I)?
Explanation
Question 77
A 35-year-old male suffered a severe traumatic brain injury and an ipsilateral elbow fracture-dislocation 8 months ago.
He now presents with a rigid elbow contracture secondary to massive heterotopic ossification (HO). Before proceeding with surgical excision of the HO and capsular release, which of the following criteria is considered the most reliable indicator that the HO is "mature" enough to minimize the risk of massive postoperative recurrence?

Explanation
Question 78
A 45-year-old male weightlifter sustains an acute distal biceps tendon rupture. He undergoes operative repair via a single-incision anterior approach using cortical button fixation.
Postoperatively, he complains of an area of numbness and tingling extending down the radial (lateral) aspect of his forearm. Which nerve is most likely injured, and what specific surgical maneuver places it at highest risk?

Explanation
Question 79
A 24-year-old motorcyclist is brought to the trauma bay after a high-speed collision. He presents with massive swelling over the shoulder girdle and a pulseless, flail upper extremity. Radiographs show significant lateral displacement of the scapula relative to the thoracic spine and an intact clavicle. Which of the following associated injuries is the most critical determinant of the long-term functional salvageability of this limb?
Explanation
Question 80
A 21-year-old collegiate javelin thrower presents with chronic posterior shoulder pain.
His pain is highly localized to the late cocking phase of his throwing motion. Arthroscopic evaluation reveals fraying of the posterosuperior labrum and an articular-sided, partial-thickness tear of the posterior supraspinatus and anterior infraspinatus tendons. Which of the following best describes the exact mechanism of 'internal impingement' occurring in this athlete?

Explanation
Question 81
A 65-year-old female sustains a 4-part proximal humerus fracture. Which of the following radiographic findings is the strongest predictor of ensuing humeral head ischemia according to Hertel criteria?
Explanation
Question 82
A 35-year-old overhead athlete presents with painless weakness in external rotation of the shoulder. Examination reveals atrophy isolated to the infraspinatus fossa. MRI demonstrates a paralabral cyst. At which of the following anatomic locations is the nerve compression most likely occurring?
Explanation
Question 83
A 40-year-old male sustains a 'terrible triad' injury of the elbow. During surgical reconstruction, what is the generally recommended sequence of repair to restore elbow stability?
Explanation
Question 84
A 28-year-old mechanic complains of right shoulder pain and weakness 4 months after a radical neck dissection. Examination reveals lateral winging of the scapula, with the scapula translated laterally and rotated downward. Which muscle-nerve combination is deficient, and what is the preferred salvage tendon transfer?
Explanation
Question 85
During the surgical reconstruction of a chronic type V acromioclavicular (AC) joint separation, the surgeon reconstructs the coracoclavicular (CC) ligaments. The native conoid ligament inserts on the clavicle at what distance from the distal clavicle, and what is its primary biomechanical role?
Explanation
Question 86
A 24-year-old rugby player undergoes a Latarjet procedure for recurrent anterior shoulder instability with 25% glenoid bone loss. Postoperatively, he exhibits profound weakness in elbow flexion and decreased sensation over the lateral aspect of his forearm. Which nerve was most likely injured during coracoid retraction?
Explanation
Question 87
A 19-year-old collegiate baseball pitcher undergoes ulnar collateral ligament (UCL) reconstruction using a palmaris longus autograft. Which bundle of the native UCL is the primary restraint to valgus stress between 30 and 120 degrees of flexion, and where does it insert?
Explanation
Question 88
A 30-year-old weightlifter feels a pop in his anterior chest while performing a bench press. MRI confirms a complete rupture of the sternal head of the pectoralis major. Compared to the clavicular head, how does the sternal head normally insert onto the humerus?
Explanation
Question 89
In planning a reverse total shoulder arthroplasty (rTSA), the surgeon decides to use a lateralized glenosphere rather than a standard medialized Grammont design. What is the primary biomechanical advantage of lateralizing the center of rotation on the glenoid side?
Explanation
Question 90
A 35-year-old female falls on an outstretched hand and sustains a coronal shear fracture of the distal humerus involving the capitellum and extending medially to include the lateral ridge of the trochlea. According to the Bryan and Morrey classification, what type of fracture is this?
Explanation
Question 91
A 45-year-old male develops severe heterotopic ossification (HO) and elbow stiffness following a distal humerus fracture treated with ORIF 6 months ago. His ROM is currently 60 to 90 degrees. What is the optimal timing and prerequisite for surgical excision of the HO?
Explanation
Question 92
A 60-year-old male with a massive, irreparable posterosuperior rotator cuff tear and intact subscapularis undergoes a latissimus dorsi tendon transfer. During harvest, the primary neurovascular pedicle must be protected. What is the major arterial supply to the latissimus dorsi muscle?
Explanation
Question 93
A surgeon is performing a two-incision distal biceps repair (modified Boyd-Anderson approach). To minimize the risk of proximal radioulnar synostosis, which technical step is most critical during the procedure?
Explanation
Question 94
A 42-year-old man presents with anterior shoulder pain after a fall. On examination, the examiner places the patient's palm on his contralateral shoulder and attempts to lift the hand off the shoulder while the patient resists. Which specific portion of the rotator cuff is best isolated by this test?
Explanation
None
