Comprehensive Introduction and Patho-Epidemiology
Welcome, colleagues and fellows, to the operating theater and this advanced masterclass. Today, we are undertaking a comprehensive analysis of a challenging, technically demanding, yet incredibly rewarding procedure: Posterior Cruciate Ligament (PCL) reconstruction. This intervention transcends the mere replacement of a ruptured ligament; it represents the meticulous restoration of complex knee biomechanics and the critical prevention of long-term, debilitating degenerative changes. The nuances of PCL surgery dictate that precision is not merely an option, but an absolute necessity for clinical success.
Historically, the PCL has been termed the "forgotten cruciate," largely due to the higher incidence and dramatic presentation of Anterior Cruciate Ligament (ACL) injuries. However, epidemiological data indicates that PCL tears account for up to 20% of all knee ligament injuries, particularly in the context of high-energy trauma such as motor vehicle collisions or contact sports. Unlike the ACL, PCL injuries frequently do not present with a dramatic, audible "pop" or immediate, profound instability. This insidious clinical presentation often leads to delayed diagnosis, chronic functional impairment, and a progressive deterioration of joint health.
The pathogenesis of PCL deficiency is rooted in altered articular kinematics. The PCL is the primary static restraint to posterior translation of the tibia relative to the femur. In its absence, the tibia subluxates posteriorly, fundamentally altering the resting position of the joint. This posterior sag disrupts the normal rolling and gliding mechanics of the knee, leading to a dramatic increase in contact pressures within the medial and patellofemoral compartments. Untreated Grade III isolated injuries, or combined multiligamentous knee injuries (MLKI), invariably precipitate significant, accelerated chondral degeneration. Therefore, surgical intervention is not merely a stabilizing procedure, but a joint-preserving imperative.
Detailed Surgical Anatomy and Biomechanics
A profound, three-dimensional understanding of the posterior knee anatomy is the bedrock of successful PCL reconstruction. The PCL is a robust, intra-articular but extra-synovial structure, serving as the central pivot of the knee. It originates broadly in a semicircular pattern on the intercondylar surface of the medial femoral condyle. This origin is located anterior to the articular cartilage, roughly at the 1:00 position in a right knee (or 11:00 in a left knee) when viewed arthroscopically from the anterolateral portal. Its broad attachment ensures a wide functional footprint, which is critical to replicate during anatomic reconstruction.
The tibial insertion is equally complex. The PCL inserts on the posterior aspect of the tibia, within a distinct anatomic depression known as the PCL facet, situated between the medial and lateral tibial plateaus. This insertion point extends significantly distal to the joint line, typically 1.0 to 1.5 cm below the articular surface. Understanding this precise location is paramount for accurate tibial tunnel placement, particularly when utilizing a transtibial arthroscopic technique, as improper placement can lead to the dreaded "killer turn" effect on the graft. On average, the native PCL is approximately 13 mm wide and 38 mm in length, dimensions that speak to its substantial role in dynamic knee stability.
Fascicular Anatomy and Co-Dominant Biomechanics
The PCL is not a simple, uniform band of tissue; it is a complex, fasciculated structure comprising two main functional bundles: the Anterolateral (AL) bundle and the Posteromedial (PM) bundle. The AL bundle is the larger and biomechanically dominant of the two. Its femoral origin is more anterior on the intercondylar surface, and its tibial insertion is more lateral relative to the PM bundle. Biomechanically, the AL bundle becomes maximally taut in knee flexion (particularly beyond 70 degrees), providing essential stability during activities of daily living such as squatting, descending stairs, or decelerating.
Conversely, the Posteromedial (PM) bundle is smaller and exhibits reciprocal tensioning, becoming taut in knee extension and early flexion. Its femoral origin is more posterior, and its tibial insertion is more medial. Understanding this reciprocal tensioning of the AL and PM bundles is crucial for surgeons contemplating double-bundle reconstruction techniques, which aim to meticulously mimic native knee kinematics across the entire arc of motion. Furthermore, the meniscofemoral ligaments of Humphry (anterior to the PCL) and Wrisberg (posterior to the PCL) arise from the posterior horn of the lateral meniscus and insert onto the medial femoral condyle. These structures contribute up to 30% of posterior stability in a PCL-deficient knee and must be carefully evaluated and preserved when possible during posterior dissection.
Neurovascular Topography: The Popliteal Fossa
The most critical anatomical consideration during PCL reconstruction lies immediately posterior to the surgical field. Within the popliteal fossa, separated from the posterior capsule by mere millimeters of fat and connective tissue, lie the popliteal artery, the popliteal vein, and the tibial nerve. The popliteal artery is tethered proximally at the adductor hiatus and distally at the soleus arch, making it relatively immobile and highly vulnerable during posterior tibial tunnel drilling.
This vulnerability is exacerbated when utilizing an outside-in transtibial technique if the drill guide is not meticulously positioned and the guidewire is not directly visualized and protected. The middle geniculate artery, a direct branch of the popliteal, pierces the posterior capsule to supply the cruciate ligaments and is routinely encountered and ablated during posterior capsular preparation. Extreme caution, mandatory utilization of a posteromedial safety portal, and direct, uncompromised visualization are non-negotiable tenets when operating in the posterior compartment to prevent catastrophic vascular injury.
Exhaustive Indications and Contraindications
The decision-making algorithm for PCL reconstruction requires a nuanced synthesis of the patient's chronicity, injury severity, concomitant pathology, and functional demands. Unlike ACL tears, where surgical reconstruction is frequently the default pathway for active individuals, the management of PCL injuries is highly stratified. Isolated Grade I and II PCL injuries (0-10 mm of posterior translation) possess an intrinsic capacity for healing and are almost universally managed non-operatively with a structured rehabilitation program emphasizing quadriceps strengthening and dynamic bracing.
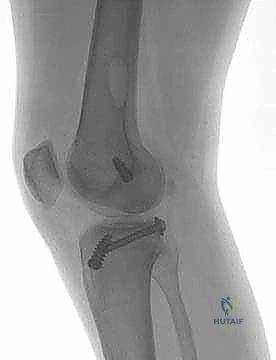
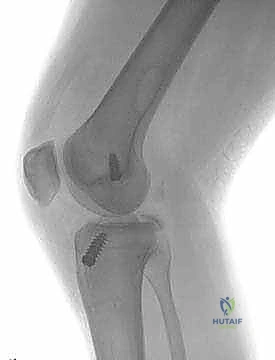
Surgical intervention becomes imperative in specific clinical scenarios. Acute, displaced bony avulsions of the PCL tibial insertion mandate prompt surgical repair, often achievable with primary screw or suture anchor fixation, yielding excellent clinical outcomes. Acute Grade III PCL injuries (>10 mm posterior translation) that occur in conjunction with other ligamentous disruptions—most notably the Posterolateral Corner (PLC), Medial Collateral Ligament (MCL), or ACL—necessitate surgical reconstruction to restore global knee stability. In chronic scenarios, patients presenting with symptomatic Grade II or III PCL deficiency characterized by recurrent instability, pain, or progressive medial/patellofemoral compartment deterioration despite exhaustive conservative management are prime candidates for reconstruction.
Graft Selection Principles
The selection of an appropriate graft is a critical variable in pre-operative planning, with each option presenting distinct biomechanical profiles and potential morbidities. Autologous tissue remains a viable option, particularly in younger, high-demand athletes. Bone-Patellar Tendon-Bone (BPTB) autograft offers robust initial fixation due to bone-to-bone healing within the tunnels; however, it carries a significant risk of anterior knee pain and donor-site morbidity, which is particularly detrimental in a PCL-reconstructed knee that relies heavily on quadriceps function. Hamstring autografts (semitendinosus and gracilis) offer reduced donor-site morbidity but may lack the requisite volume for a robust PCL reconstruction unless quadrupled or combined with allograft tissue.
In contemporary academic practice, allograft tissue has become the gold standard for PCL reconstruction, particularly in the setting of multiligamentous injuries where autograft harvest would induce unacceptable morbidity. Achilles tendon allograft with a bone block allows for excellent fixation in the femoral tunnel and robust soft-tissue fixation on the tibia. Alternatively, robust soft-tissue allografts such as the Tibialis Anterior or full-thickness Quadriceps tendon provide exceptional length and ultimate tensile strength. Our institutional preference strongly leans toward fresh-frozen Tibialis Anterior allograft for single-bundle reconstructions due to its superior cross-sectional area, ease of passage, and minimal host morbidity.
Absolute and Relative Contraindications
It is equally vital to recognize when PCL reconstruction is contraindicated to avoid exacerbating patient morbidity. Absolute contraindications include active local or systemic infection, severe peripheral vascular disease that compromises healing or increases the risk of ischemic complications during surgery, and profound medical comorbidities precluding safe anesthesia. A non-compliant patient who is unable or unwilling to adhere to the rigorous, protracted post-operative rehabilitation protocol is also an absolute contraindication, as premature weight-bearing or aggressive hamstring activation will inevitably lead to graft failure.
Relative contraindications require careful surgical judgment. Advanced, unicompartmental osteoarthritis in the medial or patellofemoral compartments may not be alleviated by soft-tissue reconstruction alone. In such cases, a concurrent high tibial osteotomy (HTO) to correct varus malalignment and unload the compromised compartment may be necessary alongside, or staged prior to, the PCL reconstruction. Furthermore, fixed posterior tibial subluxation that cannot be manually reduced under anesthesia precludes standard reconstructive techniques and may require extensive capsular releases or alternative salvage procedures.
| Category | Indications for Surgery | Contraindications for Surgery |
|---|---|---|
| Acute Injuries | Bony avulsion fractures; Grade III injuries with MLKI (PLC, ACL, MCL involvement); High-level athletes with isolated Grade III tears. | Active joint infection; Severe polytrauma precluding prolonged surgery; Medically unstable patient. |
| Chronic Injuries | Symptomatic Grade II/III instability; Progressive medial/patellofemoral OA secondary to posterior sag; Failure of exhaustive non-operative management. | Advanced tricompartmental OA; Fixed, irreducible posterior tibial subluxation; Severe, uncorrected varus/valgus malalignment. |
| Patient Factors | High functional demands; Commitment to rigorous, 6-9 month rehabilitation protocol. | Non-compliance; Inability to participate in physical therapy; Severe peripheral vascular disease. |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous pre-operative planning is the crucible in which surgical success is forged. The clinical examination must be exhaustive. The Posterior Drawer Test remains the most accurate clinical tool; performed at 90 degrees of flexion, the surgeon assesses the step-off between the medial femoral condyle and the anteromedial tibia. A normal knee exhibits a 1 cm anterior step-off. Loss of this step-off indicates a Grade II injury, while the tibia resting posterior to the condyles signifies a Grade III injury. The Godfrey Sag test, Quadriceps Active test, and the Dial Test (at 30 and 90 degrees) are mandatory to rule in or out concomitant posterolateral corner (PLC) pathology, which, if missed, is the leading cause of PCL graft failure.
Imaging protocols must be rigorous. Standard weight-bearing radiographs, including bilateral Rosenberg views and a merchant view, assess joint space narrowing. Stress radiographs (kneeling or Telos device) are invaluable for quantifying dynamic posterior tibial translation; a side-to-side difference of >8 mm strongly correlates with a complete PCL tear. High-resolution, 3-Tesla MRI is the definitive modality for evaluating the soft-tissue envelope, confirming the tear location (mid-substance vs. avulsion), and assessing the integrity of the menisci and chondral surfaces. Pre-operative templating on these images allows the surgeon to anticipate tunnel lengths and select the appropriate graft dimensions.
Anesthesia and Patient Setup
Once the patient is transferred to the operating theater, a multidisciplinary approach ensures optimal safety and exposure. Regional anesthesia, typically a combination of a femoral nerve block and a sciatic nerve block, is highly recommended for post-operative pain control, though these are often placed after the immediate post-operative neurological examination to ensure no intra-operative nerve traction injuries have occurred. General anesthesia is standard to ensure complete muscle relaxation, which is critical for joint manipulation and accurate tensioning of the graft.
Patient positioning is a critical, highly choreographed step. The patient is positioned supine on a standard operating table. We strongly advocate against the routine use of a pneumatic tourniquet. Operating without a tourniquet allows for continuous assessment of tissue perfusion, immediate identification and hemostasis of bleeding vessels (particularly the middle geniculate artery), and theoretically reduces the risk of deep vein thrombosis in these lengthy procedures. A Foley catheter is routinely placed due to the anticipated duration of the surgery and the fluid shifts associated with continuous arthroscopic irrigation.
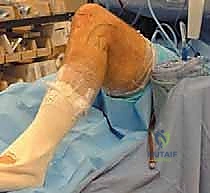
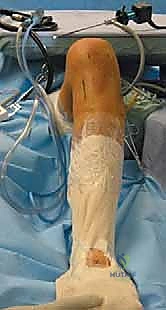
The 90-Degree Flexion Posture
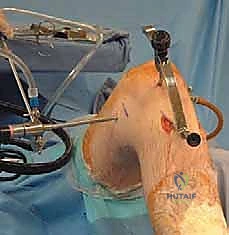
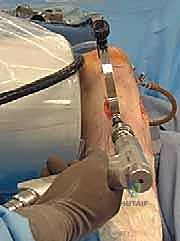
The operative leg is prepped and draped in a standard sterile fashion. The key to PCL reconstruction positioning is maintaining the knee in exactly 90 degrees of flexion during tunnel preparation. We utilize a generously padded, sterile bump taped securely to the table beneath the foot, combined with a lateral thigh post positioned just proximal to the lateral epicondyle. This setup allows the knee to rest comfortably at 90 degrees, providing optimal, unimpeded access to the posterior joint compartments.
Crucially, this 90-degree position prevents the inherent posterior sag of the tibia that occurs in a PCL-deficient knee. If the tibia is allowed to sag posteriorly during tibial tunnel drilling, the anatomical landmarks are distorted, and the risk of the guidewire penetrating the posterior capsule and injuring the neurovascular bundle increases exponentially. An intra-operative fluoroscopy unit (C-arm) is brought in from the contralateral side, draped sterilely, and positioned to provide perfect lateral views of the knee. The C-arm is an indispensable tool for verifying guidewire placement prior to reaming.

Step-by-Step Surgical Approach and Fixation Technique
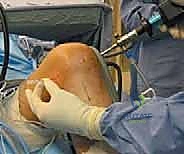
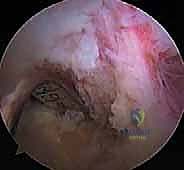
The surgical execution of a PCL reconstruction is an exercise in extreme anatomical precision and spatial awareness. The procedure begins with a standard diagnostic arthroscopy utilizing high anterolateral and anteromedial portals. High portal placement is critical; it allows the arthroscope and instruments to clear the anterior fat pad and the ACL, providing an unobstructed trajectory into the intercondylar notch and the posterior compartments. Any concomitant meniscal or chondral pathology is addressed at this stage before proceeding to the ligamentous reconstruction.
The intercondylar notch is meticulously debrided. The remnants of the native PCL are identified and carefully resected using a combination of motorized shavers and radiofrequency wands. It is paramount to preserve the ACL and the meniscofemoral ligaments (Humphry and Wrisberg) if they are intact. The femoral footprint of the PCL on the medial femoral condyle is decorticated to bleeding bone to promote graft incorporation, carefully delineating the margins of the articular cartilage to avoid iatrogenic damage.
Establishing the Posteromedial Safety Portal
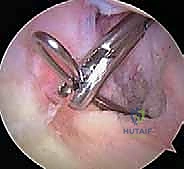
The hallmark of safe PCL surgery is the establishment of a posteromedial (PM) working portal. This is not optional; it is a mandatory safety measure. With the arthroscope passed through the intercondylar notch (the "Gillquist maneuver") into the posteromedial compartment, the area is transilluminated. A spinal needle is localized externally, ensuring the trajectory is superior to the medial meniscus and anterior to the medial head of the gastrocnemius.
Once the spinal needle is visualized intra-articularly, a vertical skin incision is made, and a blunt trocar is used to enter the capsule. This PM portal provides a direct, orthogonal view of the posterior tibial facet. A motorized shaver is introduced through the PM portal to elevate the posterior capsule off the posterior aspect of the tibia. This dissection must be meticulous, creating a clear space between the capsule (and the neurovascular structures behind it) and the bony tibial insertion of the PCL. This is often referred to as clearing the "killer curve."
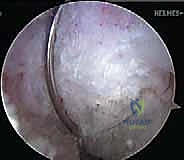
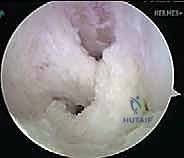
Tibial Tunnel Genesis and the "Killer Turn"
Tibial tunnel preparation is the most technically demanding and hazardous step of the procedure. We utilize an outside-in transtibial technique. A PCL tibial drill guide is introduced through the anteromedial portal and hooked meticulously over the posterior facet of the tibia, approximately 10-15 mm distal to the articular joint line. The external sleeve is positioned on the anteromedial tibia, midway between the tibial crest and the posteromedial border, roughly 4-5 cm distal to the joint line.
A specialized, calibrated guidewire is drilled from anterior to posterior. Crucially, the advancement of this wire is monitored simultaneously via direct arthroscopic visualization through the PM portal and via lateral fluoroscopy. The wire must emerge exactly at the center of the PCL footprint. Once confirmed, the tibial tunnel is reamed to the diameter of the prepared graft. To mitigate the "killer turn"—the acute angle the graft must navigate as it exits the tibial tunnel and turns superiorly toward the femur—we use a specialized rasp to meticulously chamfer and smooth the posterior intra-articular aperture of the tibial tunnel. Failure to chamfer this edge will lead to premature graft abrasion and failure.
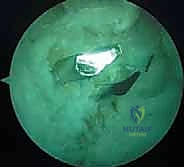
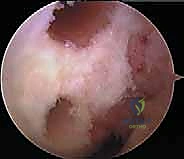
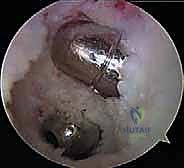
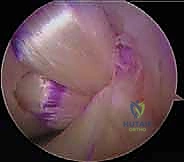
Femoral Tunnel Genesis and Graft Fixation
Femoral tunnel preparation is typically performed using an inside-out technique for single-bundle reconstructions. A femoral aiming guide is introduced through the anterolateral portal and positioned on the medial femoral condyle. For an anatomic single-bundle reconstruction (recreating the AL bundle), the guide pin is placed at the 1:00 position (right knee), approximately 7-8 mm proximal to the articular margin of the medial femoral condyle. The guidewire is drilled out through the anteromedial cortex of the femur, followed by an appropriately sized reamer.
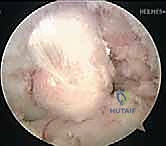
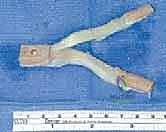
Graft passage requires patience and specialized instrumentation. A passing suture is shuttled from the femoral tunnel, through the joint space, and down the tibial tunnel. The graft is then pulled smoothly into position. We advocate for a "femur-first" fixation strategy. The graft is secured in the femoral tunnel using a cortical suspensory button or an interference screw, depending on the graft type.
Tibial fixation is performed with the knee flexed to exactly 90 degrees. An assistant applies a strong anterior drawer force to the proximal tibia to restore the normal anatomic step-off and eliminate any posterior sag. The graft is pre-tensioned manually to remove creep, and then secured in the tibial tunnel using a robust biocomposite interference screw, often backed up with a cortical screw and washer or a suture anchor for dual fixation, given the high biomechanical forces the PCL must withstand.
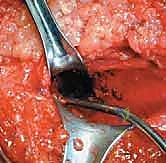
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, PCL reconstruction carries a distinct profile of intra-operative and post-operative complications. The most feared, albeit rare, complication is iatrogenic injury to the popliteal artery. The incidence of this catastrophic event is reported to be less than 0.1%, but its consequences—including compartment syndrome, limb ischemia, and potential amputation—are devastating. Prevention through the use of a posteromedial safety portal, fluoroscopy, and a posterior capsular elevator is absolute. If a vascular injury is suspected intra-operatively (e.g., pulsatile bleeding from the tibial tunnel), the procedure must be immediately aborted, a vascular surgeon consulted stat, and an on-table angiogram performed.
The most common long-term complication is residual posterior laxity, occurring in 10% to 20% of cases. This is rarely due to traumatic re-rupture; rather, it is typically the result of graft elongation (creep) over time, failure to address concurrent posterolateral corner injuries, or the "killer turn" effect causing mechanical abrasion of the graft at the posterior tibial aperture. While some residual laxity (Grade I) is often clinically well-tolerated, symptomatic Grade II or III recurrent laxity requires a thorough reassessment. Revision surgery is complex, often requiring bone grafting of widened tunnels, staging the reconstruction, and utilizing alternative graft sources (e.g., transitioning from allograft to autograft).
Arthrofibrosis and loss of flexion are also significant risks, particularly if surgery is performed during the acute inflammatory phase or if post-operative rehabilitation is delayed. The incidence of clinically significant stiffness ranges from 5% to 10%. Management begins with aggressive physical therapy and dynamic splinting. If conservative measures fail, arthroscopic lysis of adhesions and manipulation under anesthesia (MUA) may be required, typically performed 3 to 6 months post-operatively.
| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage / Management Protocol |
|---|---|---|---|
| Popliteal Artery Injury | < 0.1% | Over-penetration of tibial guidewire/reamer; Failure to use PM safety portal. | Immediate vascular surgery consult; On-table angiography; Open vascular repair. |
| Residual Posterior Laxity | 10% - 20% | Unrecognized PLC injury; Graft creep; "Killer turn" abrasion; Poor tibial fixation. | Assess for concurrent MLKI; Revision reconstruction with tunnel bone grafting; Osteotomy for malalignment. |
| Arthrofibrosis | 5% - 10% | Surgery during acute inflammatory phase; Prolonged immobilization; Poor pain control. | Aggressive PT; Dynamic bracing; Arthroscopic lysis of adhesions and MUA. |
| Graft Abrasion / Failure | 2% - 5% | Inadequate chamfering of posterior tibial tunnel aperture. | Revision surgery; Consider tibial inlay technique to bypass the killer turn entirely. |