Orthopedic Oncology Cases: Avoid Misdiagnosis of Tumor Mimickers
Patient Presentation & History
A 28-year-old male, a recreational athlete with no significant past medical history, presented to the Orthopedic Trauma clinic complaining of persistent and progressive pain and swelling in his left anterior thigh. Approximately three months prior, he sustained a direct contusion to the vastus intermedius region during a sporting event, which was initially managed conservatively with rest, ice, compression, and elevation (RICE). Over the subsequent weeks, the initial ecchymosis and tenderness resolved. However, about 6 weeks post-injury, he noticed a new, palpable mass developing within the muscle belly, which gradually increased in size and became increasingly painful, particularly with knee flexion and quadriceps activation. The pain was described as deep, aching, and non-radiating, exacerbated by activity and partially relieved by rest. He denied any constitutional symptoms such as fever, night sweats, or unexplained weight loss. He reported no history of previous orthopedic trauma, neurological conditions, or connective tissue disorders.
Clinical Examination
Inspection
On inspection of the left thigh, a subtle fullness was noted in the anteromedial aspect, approximately 10 cm proximal to the superior pole of the patella. No overlying skin erythema, warmth, or signs of infection were observed. The skin integrity was intact. Muscle bulk appeared symmetrical bilaterally, with no evidence of atrophy or fasciculations.
Palpation
Palpation revealed a firm, well-circumscribed, non-mobile mass measuring approximately 6 x 4 cm, deeply situated within the vastus intermedius muscle. The mass was tender to direct palpation but did not exhibit crepitus. It felt fixed to the surrounding muscle tissue but appeared separate from the underlying femur. There was no fluctuance. Minimal warmth was present over the mass.
Range of Motion
Active and passive range of motion of the left knee was assessed. Knee flexion was restricted to 90 degrees (compared to 140 degrees on the contralateral side) with associated pain and a firm end-feel. Knee extension was full, but pain was elicited with resisted quadriceps contraction. Hip range of motion was full and pain-free.
Neurological & Vascular Assessment
Distal neurological examination revealed intact sensation to light touch and pinprick in the L2-S1 dermatomes. Motor strength of the quadriceps (L3-L4), hamstrings (L5-S1), and ankle dorsi/plantar flexors was 5/5, though resisted knee extension caused significant pain. Peripheral pulses (femoral, popliteal, dorsalis pedis, posterior tibial) were all palpable and symmetrical bilaterally. Capillary refill was brisk (<2 seconds). No signs of acute compartment syndrome were present.
Imaging & Diagnostics
Initial X-ray Findings
Initial radiographs of the left femur and knee (AP and lateral views) taken shortly after the original contusion were unremarkable, demonstrating no acute osseous injury or significant soft tissue calcification. Follow-up radiographs performed at 6 weeks post-injury, coinciding with the development of the palpable mass, showed subtle, amorphous, ill-defined calcifications within the soft tissues of the anterior thigh. At the 12-week mark, repeat radiographs revealed a more organized pattern of ossification with a distinct, mature peripheral rim and a less dense, more radiolucent center, characteristic of the "zone phenomenon" associated with myositis ossificans. Notably, there was no evidence of cortical destruction or periosteal reaction involving the adjacent femur.
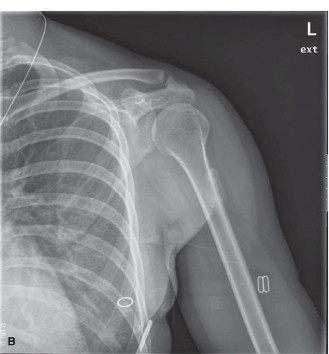
Figure 1: Initial radiograph demonstrating early, ill-defined soft tissue calcification within the quadriceps muscle, approximately 6 weeks post-trauma.
Advanced Imaging
Computed Tomography (CT) Scan: A CT scan of the left thigh was subsequently obtained to better characterize the lesion. The CT scan confirmed the presence of a well-circumscribed soft tissue mass in the vastus intermedius muscle, measuring 6.2 x 4.5 x 4.0 cm. Critically, it demonstrated the classic "zone phenomenon," with a dense, mature cortical rim of bone surrounding a less dense, trabeculated, and more radiolucent central core. The lesion appeared distinct from the femoral cortex, though in close proximity. No evidence of cortical erosion, frank bone invasion, or significant periosteal reaction was noted. The CT provided superior detail regarding the osseous maturation and confirmed the benign appearance of the lesion based on its distinct peripheral ossification pattern.
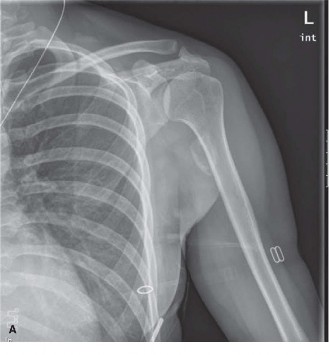
Figure 2: Coronal CT reformat showing a well-defined, peripherally ossified mass with a lucent center, consistent with a mature myositis ossificans lesion. The 'zone phenomenon' is clearly visible.
Magnetic Resonance Imaging (MRI): An MRI of the left thigh was performed to further assess the soft tissue characteristics and rule out a malignant process. The MRI revealed a heterogeneous mass with a peripheral low signal intensity rim on both T1- and T2-weighted sequences, corresponding to mature ossification. The central portion of the lesion demonstrated intermediate to high signal intensity on T2-weighted images and intermediate signal on T1-weighted images, indicative of immature fibrous tissue, edema, and fatty marrow. Post-contrast images showed heterogeneous enhancement, primarily within the central and intermediate zones, with less enhancement in the mature peripheral rim. Extensive surrounding muscle edema was not prominent at this stage, suggesting a maturing lesion. While features were suggestive of myositis ossificans, the infiltrative nature seen in early lesions or the heterogeneous enhancement can sometimes make differentiation from a low-grade sarcoma challenging without clinical-radiological-pathological correlation.
Biopsy Considerations
Given the increasing suspicion for myositis ossificans based on the imaging progression and the classic "zone phenomenon," a percutaneous core needle biopsy was considered. However, due to the high risk of misdiagnosis of an immature myositis ossificans lesion as an osteosarcoma or other high-grade sarcoma, especially if the biopsy had been performed earlier in the course of the lesion, the decision was made to initially manage conservatively and observe further maturation. The patient was educated on the natural history of the condition. If symptoms had persisted or worsened despite conservative management, or if the imaging had shown atypical features, a biopsy would have been performed, ideally targeting the central, more cellular portion while ensuring the pathologist was fully aware of the clinical and radiological findings to avoid misinterpretation of atypical cellularity and immature osteoid. In this specific case, the classical imaging features were sufficiently convincing to defer an immediate biopsy.
Differential Diagnosis
The clinical presentation of a rapidly growing, painful, calcified soft tissue mass following trauma necessitates a broad differential diagnosis, with a critical distinction between benign tumor mimickers and true malignant neoplasms. The following table outlines key differentials:
| Feature | Myositis Ossificans (MO) | Extraskeletal Osteosarcoma (EOS) | Calcified Hematoma / Traumatic Myositis |
|---|---|---|---|
| Etiology | Post-traumatic (single or repetitive), neurogenic, genetic syndromes | De novo, often unknown; rarely post-radiation, chronic inflammation | Direct trauma with hemorrhage; often resolves spontaneously |
| Age Group | Any, typically young adults/adolescents | Older adults (50-70s), but can occur at any age | Any, common in active individuals |
| Growth Pattern | Rapid initial growth (weeks-months), then stabilizes/regresses | Rapid, aggressive, relentless, infiltrative | Initial rapid swelling (hematoma), then slow resolution/calcification |
| Pain | Initially significant, often decreases with maturation | Persistent, often progressive, severe, unrelieved by rest | Initial severe pain from trauma, typically improves as hematoma resolves |
| Location | Large muscle groups (quadriceps, brachialis, gluteals) | Deep soft tissues, often thigh, retroperitoneum, abdominal wall | Any site of direct trauma |
| Imaging (X-ray/CT) | "Zone Phenomenon": Mature peripheral ossification, lucent center | Ill-defined, patchy, amorphous, central mineralization, lacks distinct rim | Irregular, amorphous, often diffuse calcification within soft tissue mass |
| Imaging (MRI) | Heterogeneous, T2 hyperintense center, T1/T2 hypointense rim; variable enhancement | Heterogeneous T1/T2, significant enhancement, infiltrative margins, adjacent bone/neurovascular involvement | Heterogeneous signal (blood products), often fluid levels, rim enhancement possible, no organized bone formation |
| Biopsy (Histology Early) | Zonation: immature cellular center with osteoid, maturing peripherally to lamellar bone. No significant atypia. | Atypical spindle cells, pleomorphism, malignant osteoid, atypical mitoses. Lacks zonation. | Hemosiderin-laden macrophages, fibrin, necrotic debris, inflammatory cells. No true bone formation or atypia. |
| Biopsy (Histology Late) | Mature lamellar bone at periphery, fibrous/immature bone centrally, zonation maintained. | Same as early, often more extensive malignant osteoid and cellularity. | Dense fibrous tissue, dystrophic calcification, chronic inflammatory cells. |
| Prognosis | Excellent, benign, self-limiting | Poor, high metastatic potential, requires aggressive multimodal therapy | Excellent, usually resolves completely |
| Management | Conservative (rest, NSAIDs) initially. Excision for symptomatic, mature lesions. | Wide en bloc resection, adjuvant chemotherapy/radiotherapy. | Observation, physical therapy. Rarely aspiration or excision for cosmesis. |
Surgical Decision Making & Classification
The primary surgical decision-making revolves around the initial diagnostic accuracy and the timing of intervention for myositis ossificans, contrasting sharply with the immediate and aggressive approach required for malignant sarcomas.
For Myositis Ossificans (MO):
1.
Non-Operative Management:
The initial management for a suspected MO lesion is almost always conservative. This involves:
*
Rest and activity modification:
Avoiding strenuous activity that irritates the lesion.
*
NSAIDs:
To help with pain and inflammation, and some studies suggest a role in preventing recurrence after excision, though less evidence for primary prevention.
*
Physical Therapy:
Gentle range of motion exercises, avoiding aggressive stretching or massage which can potentially exacerbate or induce recurrence.
*
Observation:
Regular clinical and radiographic follow-up to monitor lesion maturation.
2.
Surgical Intervention Indications:
Surgery is typically reserved for mature, symptomatic lesions that fail conservative management. Indications include:
*
Persistent pain:
Unrelieved by conservative measures.
*
Functional impairment:
Restriction of joint range of motion (as seen in this patient with knee flexion deficit), gait disturbance, or muscle weakness.
*
Neurological compression:
If the mass impinges on a peripheral nerve, though less common in the vastus intermedius.
*
Cosmetic deformity:
Rarely, for very large or superficial lesions.
3.
Timing of Surgery:
This is paramount. Excision should
only
be performed after the lesion has fully matured. Maturation is typically assessed clinically (pain reduction, stabilization of size) and radiographically (stable "zone phenomenon" on X-ray/CT, usually 6-12 months post-onset). Early excision of an immature lesion carries a significantly higher risk of recurrence (up to 30%).
4.
Classification:
While MO does not have a formal surgical classification system like fractures, its progression can be understood in phases:
*
Early (inflammatory/proliferative phase, <4-6 weeks):
Highly cellular, edematous, difficult to differentiate from sarcoma histologically. High recurrence if excised.
*
Intermediate (early ossification phase, 6-12 weeks):
Peripheral calcification begins, zone phenomenon becomes visible. Still cellular centrally.
*
Mature (late ossification phase, >3 months):
Well-defined peripheral cortex, less cellular center. Optimal for excision if indicated.
For Suspected Sarcoma (e.g., Extraskeletal Osteosarcoma):
In contrast, if the imaging and clinical picture had been ambiguous or overtly suggestive of a sarcoma (e.g., central calcification, infiltrative margins, cortical erosion, lack of zone phenomenon), the decision-making process would have been entirely different:
1.
Urgent Biopsy:
Image-guided core needle biopsy would be performed promptly. The biopsy must be planned carefully to avoid contaminating future surgical fields.
2.
Multidisciplinary Tumor Board:
Presentation to a musculoskeletal oncology tumor board is mandatory to formulate a comprehensive treatment plan, involving orthopedic oncology, medical oncology, radiation oncology, and pathology.
3.
Staging:
Extensive staging workup (CT chest/abdomen/pelvis, bone scan, PET-CT) would be initiated to rule out metastatic disease.
4.
Neoadjuvant Therapy:
Often indicated for high-grade sarcomas (chemotherapy, +/- radiation).
5.
Aggressive Surgical Resection:
Wide en bloc resection with clear surgical margins, potentially requiring complex reconstruction.
In this patient's case, the evolving imaging, particularly the development of the distinct "zone phenomenon" on CT, strongly favored a diagnosis of myositis ossificans. Coupled with the patient's improving pain profile and absence of constitutional symptoms, the decision was made to continue conservative management for further maturation. However, due to persistent, albeit reduced, pain and the limitation in knee flexion, surgical excision of the mature lesion was eventually planned.
Surgical Technique / Intervention
The surgical intervention for this patient involved the planned excision of the mature myositis ossificans lesion from the left quadriceps.
Pre-operative Planning
- Imaging Review: Detailed review of all plain radiographs, CT, and MRI scans to precisely localize the lesion, its relationship to critical neurovascular structures (femoral artery, vein, nerve, saphenous nerve), and adjacent bone.
- Patient Education: Comprehensive discussion with the patient regarding the benign nature of MO, the goals of surgery (symptom relief, improved ROM), potential risks (recurrence, infection, bleeding, nerve injury), and the post-operative rehabilitation protocol.
- Anesthesia: General endotracheal anesthesia.
Patient Positioning
The patient was positioned supine on the operating table. The entire left lower extremity, from the iliac crest to the foot, was prepped and draped in a sterile fashion, allowing for full range of motion of the hip and knee during the procedure. A tourniquet was applied to the proximal thigh but not inflated initially, allowing for assessment of vascularity and identification of small perforators.
Surgical Approach
A longitudinal incision was made directly over the palpable mass in the anterior thigh, approximately 12 cm in length, centered over the vastus intermedius. The incision was carried through the skin and subcutaneous tissue. Subcutaneous fat was carefully dissected, and saphenous vein tributaries were identified and ligated or coagulated. The deep fascia (fascia lata) overlying the quadriceps muscle was incised longitudinally.
Exposure and Excision
The vastus medialis and vastus lateralis muscles were carefully retracted. The lesion was found encapsulated within the vastus intermedius muscle, beneath the rectus femoris. The muscle fibers surrounding the well-circumscribed, firm, bony mass were gently separated using blunt and sharp dissection. The capsule of the myositis ossificans was robust and distinct. Care was taken to identify and protect any small nerves or vessels encountered within the muscle planes.
The goal was an en bloc excision of the entire mature lesion. The lesion was carefully dissected from its surrounding muscular attachments. Its posterior aspect was found to be adherent to the anterior cortex of the femur but not invading it. Using a combination of osteotomes and electrocautery, the lesion was meticulously separated from the femoral cortex without damaging the periosteum or articular cartilage. The dissection was performed circumferentially, ensuring complete removal of the ossified mass. The excised specimen measured approximately 6.5 x 4.8 x 4.2 cm.
Hemostasis and Closure
Meticulous hemostasis was achieved using electrocautery. The surgical bed was irrigated with sterile saline. A thorough final inspection confirmed complete removal of the mass and integrity of the femoral cortex and surrounding musculature. No drain was deemed necessary. The deep fascia was loosely approximated with absorbable sutures to avoid compartment issues. Subcutaneous layers were closed with absorbable sutures, and the skin was closed with non-absorbable staples. A sterile dressing was applied, followed by a compressive bandage.
Post-Operative Protocol & Rehabilitation
The post-operative protocol for excised myositis ossificans is designed to minimize the risk of recurrence while restoring function.
Immediate Post-Operative (Day 0-7)
- Pain Management: Multimodal analgesia (NSAIDs, acetaminophen, opioids as needed).
- Weight Bearing: Full weight-bearing as tolerated.
- Mobility: Gentle active and passive range of motion (ROM) exercises for the knee and hip, initiated within 24-48 hours. Emphasis on pain-free movement, avoiding aggressive stretching or forced ROM.
- Elevation & Compression: Continued elevation of the limb and use of a compressive bandage to minimize swelling and hematoma formation.
- Cryotherapy: Regular application of ice packs.
- Wound Care: Daily dressing changes; staple removal at 10-14 days.
Early Rehabilitation (Week 2-6)
- Progressive ROM: Gradually increase active and passive ROM for the knee. The goal is to regain full knee flexion and extension without pain. Manual therapy techniques, such as joint mobilizations, may be introduced cautiously.
- Gentle Strengthening: Initiate isometric quadriceps and hamstring exercises. Progress to light resistance exercises as tolerated, focusing on endurance rather than maximal strength initially.
- Scar Management: Begin scar massage once the wound is well-healed to prevent adhesions.
- Gait Training: Focus on normal gait mechanics.
Intermediate Rehabilitation (Week 6-12)
- Advanced Strengthening: Progress to isotonic and isokinetic strengthening exercises for the entire lower extremity. Incorporate functional exercises such as lunges, squats, and step-ups.
- Proprioception and Balance: Begin balance exercises (e.g., single-leg stance, wobble board).
- Cardiovascular Conditioning: Introduce low-impact aerobic activities (e.g., stationary bike, swimming).
- Return to Activity Preparation: Begin sport-specific drills if applicable, gradually increasing intensity and duration. Avoid activities that involve direct impact or aggressive stretching of the surgical site.
Late Rehabilitation (Month 3-6+)
- Full Return to Activity: Gradual return to full recreational or athletic activities, guided by pain, strength, and ROM. This phase can take several months.
- Monitoring for Recurrence: Clinical monitoring for recurrence (new pain, swelling, mass) and follow-up radiographs if symptoms arise, though routine imaging for asymptomatic patients is generally not necessary.
- Prophylaxis (Rare): In cases of recurrent myositis ossificans, or for patients with a known history of aggressive MO, some practitioners may consider short-course post-operative NSAIDs or low-dose radiation therapy, although the evidence for routine use is not strong. For a primary, well-excised MO, this is typically not required.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Clinical Suspicion is Key: Always consider myositis ossificans in the differential for a painful, enlarging soft tissue mass following trauma, especially in large muscle groups. A clear history of antecedent trauma is a strong indicator.
- Radiological Hallmark: The "zone phenomenon" on plain radiographs or CT scan is pathognomonic for myositis ossificans. This describes mature peripheral ossification with a less dense, often lucent, central core. This feature is critical in differentiating MO from soft tissue sarcomas (which typically show central or diffuse, unorganized calcification).
- Timing of Imaging Matters: Early imaging may be non-diagnostic. Serial imaging (X-rays, CT) over weeks to months is invaluable to demonstrate the progressive maturation and the development of the zone phenomenon.
- Multidisciplinary Approach: For any ambiguous soft tissue mass, particularly if malignancy cannot be definitively excluded, a multidisciplinary tumor board discussion is paramount. Clinical findings, imaging characteristics, and potential biopsy results must be correlated.
- Biopsy Timing and Communication: If a biopsy is deemed necessary, it should ideally be performed after radiographic maturation (typically >6-8 weeks). Crucially, the pathologist must be provided with detailed clinical history and imaging findings, as early biopsy of MO can be easily misinterpreted as osteosarcoma due to cellularity, atypical fibroblasts, and immature osteoid formation, especially if the central, immature portion is sampled.
- Conservative Management First: Most MO lesions resolve or become asymptomatic with conservative management. Surgery is reserved for mature, symptomatic lesions causing functional impairment.
- Surgical Excision for Mature Lesions: When surgical excision is indicated, it should be performed only after the lesion is radiographically mature (usually 3-6 months post-injury). Early excision significantly increases the risk of recurrence. The goal is en bloc removal.
- Gentle Post-operative Rehabilitation: Aggressive stretching or vigorous physiotherapy in the early post-operative period should be avoided, as it can contribute to recurrence.
Pitfalls
- Misdiagnosis as Sarcoma: This is the most catastrophic pitfall. Incorrectly diagnosing MO as an extraskeletal osteosarcoma can lead to unnecessary aggressive interventions, including extensive resections, chemotherapy, and radiation, with significant morbidity and mortality. Conversely, mistaking a sarcoma for MO and delaying treatment is equally disastrous.
- Early Biopsy Leading to Misinterpretation: Biopsy of an immature MO lesion can show reactive cellularity, immature osteoid, and atypical features that closely mimic a high-grade sarcoma. Without knowledge of the patient's history and imaging progression, pathologists may render an erroneous diagnosis.
- Aggressive Early Surgical Intervention: Excising an immature MO lesion before it has fully matured is a common pitfall that significantly increases the risk of local recurrence. Patience is key.
- Inadequate Excision: If surgical excision is indicated, failure to remove the entire, well-defined mass can lead to recurrence. While MO is benign, it is locally aggressive if not completely excised.
- Confusing MO with Simple Calcified Hematoma or Dystrophic Calcification: While both are benign, calcified hematomas typically lack the organized "zone phenomenon" and internal architecture of MO. Misidentifying them rarely has severe consequences but can lead to unnecessary anxiety.
- Ignoring Clinical Context: Over-reliance on a single imaging modality or biopsy result without correlating it with the patient's history and clinical course is a dangerous pitfall. The clinical-radiological-pathological triad is fundamental.
