Patient Presentation & History
A 72-year-old male presented to the emergency department following a ground-level fall at his home. He reported immediate, severe pain in his left thigh and an inability to bear weight. There was no direct impact to the thigh, and he described a twisting mechanism as he lost balance.
His past medical history is significant for Paget's disease of bone, diagnosed approximately 15 years prior, affecting the left femur, pelvis, and lumbar spine. He had been managed with intermittent oral bisphosphonate therapy (alendronate) for exacerbations of pain, with his last course completed 6 months prior. Other comorbidities include well-controlled hypertension, type 2 diabetes mellitus managed with oral hypoglycemics, and chronic stable angina. He is a non-smoker and reports occasional alcohol consumption. He has no prior history of major trauma or orthopedic surgery. His activity level was previously independent ambulation with a cane for longer distances, primarily limited by chronic low back pain and left hip stiffness attributed to his Paget's disease.
This mechanism, coupled with his known underlying bone pathology, raised immediate suspicion for a pathologic or fragility fracture in a Pagetically altered bone. The patient reported no prodromal pain worsening beyond his usual chronic discomfort prior to the fall, nor any constitutional symptoms.
Clinical Examination
Upon arrival, the patient was hemodynamically stable.
Inspection:
The left lower extremity was visibly shortened, externally rotated, and abducted. Significant swelling and ecchymosis were noted in the proximal thigh region. No open wounds or skin tenting were observed. There was a mild bowing deformity of the left tibia, consistent with his known Paget's disease. The patient’s skull appeared slightly enlarged, also a known Pagetic manifestation.
Palpation:
Marked tenderness was elicited over the proximal left femur, specifically around the subtrochanteric region. Crepitus was palpable with gentle manipulation. The skin over the left proximal thigh felt diffusely warm compared to the contralateral side, which is often associated with the hypervascularity of active Pagetic bone.
Range of Motion:
Both active and passive range of motion of the left hip were severely limited due to pain, with any attempt at movement causing exquisite discomfort.
Neurological Assessment:
Distal sensation was intact to light touch in all dermatomes of the left foot. Motor strength was graded 5/5 for ankle dorsiflexion, plantarflexion, and toe flexion/extension, although full assessment of hip and knee strength was limited by pain. The femoral and dorsalis pedis pulses were strong and equal bilaterally. Capillary refill was brisk in all digits. No signs of neurovascular compromise were identified.
General Systemic Assessment:
Cardiopulmonary examination was unremarkable. Abdominal examination revealed no masses or tenderness.
Imaging & Diagnostics
Initial Radiographs:
Anteroposterior (AP) and lateral radiographs of the left femur were obtained immediately. These images confirmed a displaced, comminuted subtrochanteric fracture of the left femur. The fracture pattern was oblique, extending from the lesser trochanter distally into the proximal diaphysis, with significant medial comminution.
The radiographs also demonstrated classic features of Paget's disease throughout the proximal femur:
*
Cortical thickening:
Particularly prominent along the medial and lateral cortices, with an indistinct endosteal border.
*
Trabecular coarsening:
A disorganized, thickened trabecular pattern, often described as a "cotton wool" or "woven bone" appearance in weight-bearing areas.
*
Bone enlargement:
The overall diameter of the proximal femoral shaft was increased compared to a normal femur, and also compared to the contralateral femur (though contralateral imaging wasn't initially performed for comparison).
*
Bowing:
A subtle anterior bowing of the femoral shaft was evident, a common deformity in Pagetic long bones.
* The fracture line itself appeared to propagate through this extensively altered bone structure, making it a true pathologic fracture in the context of Paget's disease.
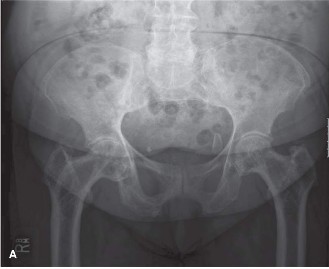
Initial AP radiograph demonstrating a subtrochanteric femoral fracture in a Pagetic bone. Note the marked cortical thickening, trabecular coarsening, and overall enlargement of the proximal femur, characteristic of Paget's disease.
Computed Tomography (CT) Scan:
Due to the complexity of the fracture, the underlying Pagetic bone, and the need for detailed pre-operative planning, a CT scan of the left femur with 3D reconstructions was performed. The CT confirmed the comminuted subtrochanteric fracture (AO/OTA 32-A3.3) and provided invaluable information regarding:
*
Fracture Morphology:
Precise location of fracture lines, degree of comminution, and fragment displacement. This detailed assessment was critical for anticipating reduction challenges.
*
Medullary Canal Anatomy:
The CT clearly demonstrated significant narrowing and sclerosis of the medullary canal of the proximal femur due to Paget's disease. The canal diameter was irregular and substantially reduced in various segments, posing a significant challenge for intramedullary nail insertion.
*
Cortical Quality:
While thickened, the cortex also showed areas of irregular density, suggesting a heterogeneous bone quality that could compromise screw purchase.
*
Exclusion of Sarcoma:
Although no overt soft tissue mass or aggressive periosteal reaction was seen, the CT provided a baseline for evaluating the bony lesion itself.
Magnetic Resonance Imaging (MRI): An MRI was considered but deferred initially due to the acute nature of the fracture requiring urgent stabilization. If there were suspicious features on plain films or CT suggestive of sarcomatous transformation (e.g., rapid growth, aggressive periosteal reaction, large soft tissue component), an MRI would be paramount to assess the extent of soft tissue involvement and guide biopsy. However, in this case, the fracture appeared primarily traumatic within the known Pagetic lesion, without overt signs of malignant transformation on initial imaging.
Bone Scan (Technetium-99m Scintigraphy): A bone scan was performed to assess the extent of active Paget's disease throughout the skeleton. It revealed intense, diffuse uptake in the left femur (consistent with the fracture and active Paget's), as well as increased uptake in the pelvis, lumbar vertebrae, and frontal skull, confirming polyostotic Paget's disease with active lesions beyond the fractured femur. This helped in understanding the systemic nature of his disease.
Laboratory Investigations:
*
Routine Pre-operative Panel:
Complete Blood Count (CBC) showed mild anemia (Hb 11.5 g/dL), likely chronic due to age and comorbidities. Electrolytes, renal function, and coagulation profile were within acceptable limits. Type and Crossmatch were performed for anticipated blood loss.
*
Paget's Specific Markers:
*
Serum Alkaline Phosphatase (ALP):
Significantly elevated at 580 U/L (reference range 40-129 U/L), indicating high osteoblastic activity associated with active Paget's disease.
*
Serum Calcium and Phosphate:
Both were within normal limits, ruling out concomitant hyperparathyroidism or other significant metabolic derangements.
*
Urinary N-telopeptide (NTX):
Elevated, further supporting high bone turnover.
These lab findings confirmed active Paget's disease, which has implications for bone quality and post-operative medical management.
Templating:
Extensive pre-operative templating was performed using the CT scan and contralateral femur radiographs. This was crucial given the altered morphology of the Pagetic femur. We specifically templated for:
*
Intramedullary (IM) Nail Length and Diameter:
The narrowed medullary canal necessitated careful consideration of nail diameter. Custom or smaller diameter nails were considered, or the possibility of needing a plate osteosynthesis if IM nailing proved impossible due to severe canal sclerosis.
*
Screw Lengths:
To ensure adequate purchase in the irregular Pagetic bone.
*
Entry Point:
Optimal entry point for IM nail to accommodate the femoral bowing and achieve central canal alignment distally.
Differential Diagnosis
The differential diagnosis for a pathologic fracture in an elderly patient, particularly with the radiographic features observed, must include several bone pathologies. A detailed comparison is essential for accurate diagnosis and management.
| Feature | Pagetic Fracture (Our Case) | Metastatic Carcinoma (e.g., Prostate, Breast) | Primary Bone Sarcoma (Paget's Sarcoma / Osteosarcoma) |
|---|---|---|---|
| Pathophysiology | Disordered bone remodeling with excessive bone resorption followed by disorganized bone formation (woven bone replacing lamellar bone). | Hematogenous spread of malignant cells from a distant primary tumor to bone, causing osteolysis and/or osteosclerosis. | Malignant transformation of osteoblasts; in Paget's sarcoma, malignant transformation of Pagetic osteoclasts/osteoblasts. |
| Typical Patient Profile | Elderly (>50-60s), male predilection, often polyostotic, family history common. | Elderly, known history of primary malignancy (prostate, breast, lung, kidney, thyroid most common). | Very rare, but increased incidence in patients with long-standing Paget's disease (>70s), radiation exposure. |
| Clinical Presentation | Often asymptomatic until fracture; bone pain, deformity (bowing), bone enlargement, warmth over lesions. | Bone pain (often worsening at night), pathologic fracture, constitutional symptoms (weight loss, fatigue), symptoms of primary cancer. | Rapid onset/progression of severe bone pain, rapidly enlarging palpable soft tissue mass, swelling, warmth, pathologic fracture. |
| Radiographic Features | Classic triad: Cortical thickening, trabecular coarsening ("cotton wool"), bone enlargement. Osteolytic wavefront ("V-shaped"). Femoral bowing. Usually well-defined margins. | Lytic: Punched-out lesions (myeloma, kidney, thyroid). Blastic: Increased density (prostate, breast). Mixed: Both lytic/blastic. Cortical destruction, often ill-defined margins. | Aggressive osteolysis with cortical destruction, periosteal reaction (sunburst, Codman's triangle), large soft tissue mass, ill-defined margins. |
| Bone Scan (Tc-99m) | Diffuse, intense, "flame-shaped" uptake in active Pagetic lesions. Multifocal if polyostotic. | Focal, often multiple, hot spots; may be less intense than Paget's. | Intense, focal uptake at the primary tumor site. |
| Laboratory Findings | Markedly elevated Serum Alkaline Phosphatase (ALP); normal Calcium, Phosphate; elevated bone turnover markers (NTX, CTX). | Varies with primary (e.g., PSA for prostate, ↑ Ca for lytic lesions). ALP may be ↑ if extensive blastic disease or liver mets. | ALP may be mildly elevated (non-specific). Non-specific inflammatory markers (ESR, CRP) may be elevated. Ca/Phos usually normal. |
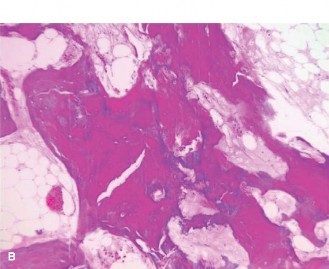
| Biopsy Findings | Characteristic mosaic pattern of woven and lamellar bone, increased osteoclast/osteoblast activity, irregular cement lines. | Malignant cells consistent with the primary tumor type. | Malignant spindle cells producing osteoid matrix (osteosarcoma), chondroid, or fibrous components; highly pleomorphic cells. |
| Management Implications | Medical management with bisphosphonates/denosumab to suppress bone turnover. Surgical fixation tailored to poor bone quality and altered anatomy. | Systemic anti-cancer therapy, radiation therapy, prophylactic fixation for impending fractures (Mirels' score), surgical stabilization for pathologic fractures. | Aggressive neoadjuvant chemotherapy, wide surgical resection, adjuvant chemotherapy, possibly radiation. |
In our patient's case, the long-standing history of Paget's disease, the characteristic radiographic features (cortical thickening, trabecular coarsening, bone enlargement, bowing), and the markedly elevated ALP strongly favored a Pagetic fracture. While a Paget's sarcoma is a serious concern in long-standing Paget's, the absence of an aggressive soft tissue mass or rapid clinical progression on initial assessment made it less likely as the primary diagnosis, though a biopsy during fixation would be prudent if any suspicious features were noted. Metastatic disease was less likely given the absence of a known primary malignancy, and the radiologic features were more characteristic of Paget's than typical metastases.
Surgical Decision Making & Classification
Operative vs. Non-operative Management:
Given the patient's displaced, comminuted subtrochanteric femur fracture, the decision was unequivocally for operative management. Non-operative management, typically involving prolonged traction followed by casting, is associated with high rates of malunion, nonunion, significant morbidity, and mortality, particularly in elderly patients with poor bone quality. The goal of surgery was anatomical reduction and stable internal fixation to allow early mobilization and weight-bearing, minimizing complications associated with prolonged recumbency.
Fracture Classification:
The fracture was classified using the
AO/OTA Fracture Classification System
as a
32-A3.3 fracture
.
*
32:
Denotes a fracture of the femur (3) in the proximal segment (2).
*
A3:
Indicates a subtrochanteric simple or multifragmentary fracture, involving the lesser trochanter.
*
.3:
Specifies a multifragmentary subtrochanteric fracture with significant comminution, particularly involving the medial cortex.
This classification highlighted the comminuted nature and the challenge of achieving stable fixation.
Considerations Specific to Paget's Disease:
The presence of Paget's disease introduced several critical factors influencing surgical decision-making:
1.
Bone Quality:
The abnormal woven bone of Paget's disease is mechanically inferior to normal lamellar bone. It is soft, brittle, and highly vascular. This compromises screw purchase and increases the risk of implant pull-out, iatrogenic fracture during reaming or screw insertion, and delayed union or nonunion.
2.
Medullary Canal Anatomy:
As identified on CT, the medullary canal was sclerotic, narrowed, and often irregular due to Pagetic remodeling. This significantly impacted the choice and size of intramedullary nails. Pre-operative templating was paramount.
3.
Hypervascularity:
Pagetic bone is highly vascular, posing a risk for increased intraoperative blood loss. This required careful anesthetic planning and the availability of blood products.
4.
Deformity:
Pre-existing bowing of the femur could affect nail trajectory and length.
5.
Sarcomatous Transformation:
The lifetime risk of sarcomatous transformation (Paget's sarcoma, usually osteosarcoma) in polyostotic Paget's is approximately 1%. While no overt signs were present, any atypical lesion or rapidly progressive component would necessitate biopsy.
Implant Choice:
Given the subtrochanteric location and comminution, an
intramedullary nail (IMN)
was considered the implant of choice for biomechanical superiority in load-sharing, compared to plating, which relies on load-bearing. However, the significantly narrowed and sclerotic medullary canal presented a major hurdle.
*
Standard Trochanteric Entry Nailing:
This was the primary plan. We anticipated requiring extensive reaming and potentially a smaller diameter nail or a specific nail designed for narrow canals.
*
Alternative: Extramedullary Plating:
If IM nailing proved impossible due to insurmountable canal obstruction or iatrogenic fracture during reaming, a long reconstructive locking plate (e.g., a Proximal Femoral Locking Plate or a Long Proximal Femur Plate) would be the fallback. This would require greater stripping and rely heavily on adequate screw purchase in compromised bone.
*
Augmentation:
The poor bone quality meant that supplementary augmentation, such as polymethylmethacrylate (PMMA) cement injection, might be necessary to enhance screw fixation or fill gaps, particularly for plating.
Pre-operative Optimization:
Although active Paget's disease with elevated ALP should ideally be treated with bisphosphonates (e.g., zoledronic acid) or denosumab to reduce bone turnover and improve bone quality, acute traumatic fractures typically cannot wait for several weeks of medical treatment to take effect. Therefore, the patient was scheduled for surgery expeditiously after medical optimization and discussion with the endocrinology team. The decision was made to proceed with surgery and initiate IV zoledronic acid post-operatively once stable.
Surgical Technique / Intervention
Pre-operative Preparation:
* Patient consent was obtained, detailing the risks including blood loss, nonunion, infection, nerve/vascular injury, and the possibility of implant failure due to Pagetic bone. The alternative of plating if IMN failed was also discussed.
* Appropriate intravenous access was established, and prophylactic antibiotics (cefazolin) were administered pre-incision.
* Two units of packed red blood cells were cross-matched and available in the operating room due to the anticipated hypervascularity of Pagetic bone and potential for significant blood loss.
Patient Positioning:
The patient was carefully positioned in the lateral decubitus position on a radiolucent fracture table. The left foot was secured in a boot, and appropriate padding was used to protect pressure points. The contralateral leg was draped free, allowing for dynamic assessment of leg length and rotation. Fluoroscopy was set up to allow for AP and lateral views without repositioning.
Surgical Approach:
A standard limited lateral approach was utilized for trochanteric entry of the intramedullary nail. A 5-7 cm incision was made, centered over the tip of the greater trochanter. The gluteus medius and minimus muscles were split in line with their fibers to expose the trochanteric fossa.
Reduction Techniques:
Achieving and maintaining reduction was a primary challenge due to the comminution and the altered bone quality.
1.
Closed Reduction via Traction and Rotation:
Gentle traction was applied via the fracture table to restore length. Internal rotation was applied to correct external rotation deformity. AP and lateral fluoroscopic views guided the reduction.
2.
Open Reduction:
Despite traction, the significant comminution and displacement of the lesser trochanter fragment prevented satisfactory closed reduction. Therefore, a small secondary incision was made on the medial aspect of the thigh to access the fracture site directly. Reduction clamps were used to reduce the main fragments. Care was taken to minimize soft tissue stripping to preserve vascularity. Provisional fixation with Kirschner wires (K-wires) was attempted but found to be difficult due to the friable bone. A temporary cerclage wire was considered but ultimately deferred to avoid further compromise to periosteal blood supply.
Intramedullary Nailing Technique:
1.
Entry Point:
The entry point for the IM nail was carefully chosen at the tip of the greater trochanter, slightly medial to the piriformis fossa, to ensure a central trajectory down the medullary canal. This was confirmed with fluoroscopy.
2.
Canal Preparation:
A flexible guide wire was cautiously advanced across the fracture site and down the femoral canal. This was extremely challenging due to the severe sclerosis and narrowing of the Pagetic canal. Multiple attempts with different guide wire angulations were required. Once the guide wire was positioned appropriately, sequential reaming commenced.
This step was particularly critical.
We started with very small reamers (8 mm) and slowly increased by 0.5 mm increments. Reaming was performed meticulously and slowly, often pausing to clear debris, to avoid iatrogenic fracture of the brittle, sclerotic Pagetic bone. Significant resistance was encountered, and the surgeon had to be prepared for the possibility of abandoning IMN if reaming proved impossible or led to a catastrophic iatrogenic fracture. The reamed canal was ultimately prepared to 1 mm larger than the chosen nail diameter.
3.
Nail Insertion:
A 13 mm diameter, 380 mm long trochanteric entry cephalomedullary nail was selected. The nail was carefully advanced down the reamed canal. Again, significant resistance was met, requiring firm but controlled mallet blows. Fluoroscopy confirmed proper nail trajectory and depth. The length was chosen to extend well into the distal diaphysis, bypassing any significant Pagetic lesions.
4.
Proximal Fixation:
The proximal screw for the femoral neck was inserted under fluoroscopic guidance, engaging the femoral head and providing stable angular support. An additional anti-rotation screw was placed to enhance stability in the comminuted trochanteric region.
5.
Distal Locking:
Two distal interlocking screws were placed via a targeting guide to ensure rotational stability and prevent shortening. This was performed using a minimally invasive technique.
Bone Grafting:
Given the comminution and the inherent poor healing potential of Pagetic bone, autogenous bone graft (from the greater trochanter) was harvested and packed around the fracture site, particularly in the medial comminution zone, to promote osteoinduction and osteoconduction.
Closure:
Following irrigation and hemostasis, the surgical wound was closed in layers. A drain was not routinely used but considered if excessive bleeding persisted. Skin was closed with staples.

Post-operative AP radiograph showing the well-reduced subtrochanteric fracture fixed with a cephalomedullary nail. Note the persistent Pagetic changes in the bone despite fixation.
Intraoperative Blood Loss: Total estimated blood loss was 1200 mL, necessitating the transfusion of two units of packed red blood cells. This confirmed the hypervascularity often associated with active Paget's disease.
Post-Operative Protocol & Rehabilitation
Immediate Post-Operative Period:
*
Pain Management:
A multimodal pain regimen was initiated, including opioid analgesics, NSAIDs (if not contraindicated), and acetaminophen to optimize comfort and facilitate early mobilization.
*
DVT Prophylaxis:
Low molecular weight heparin (enoxaparin) was started on post-operative day 1 and continued for 4-6 weeks to prevent deep vein thrombosis, a significant risk in trauma patients, especially with prolonged immobilization.
*
Antibiotics:
Post-operative antibiotics were continued for 24 hours.
*
Wound Care:
The surgical incision was inspected daily for signs of infection or hematoma. Staples were planned for removal at 2 weeks post-op.
*
Paget's Disease Management:
An intravenous infusion of zoledronic acid (5 mg over 30 minutes) was administered on post-operative day 3, prior to discharge. This potent bisphosphonate aimed to suppress the active Paget's disease, reduce bone turnover, decrease pain, and potentially improve bone quality in the long term, thereby reducing the risk of further Pagetic complications or fractures. Serum ALP and calcium levels were monitored.
*
Mobilization:
Physical therapy consultation was obtained on post-operative day 1. The patient was encouraged to begin active ankle pumps and gentle knee flexion/extension.
Rehabilitation Protocol:
The rehabilitation protocol was tailored to the specific challenges posed by Pagetic bone quality, balancing the need for early mobilization with protecting the fixation.
*
Phase 1: Initial Mobilization (Weeks 0-6):
*
Weight Bearing:
Touch-down weight bearing (TDWB) of 10-15 kg on the operative leg was permitted immediately with the assistance of a walker. This allowed for muscle activation and proprioception while minimizing stress on the healing fracture. Full weight-bearing was deferred due to concerns regarding slow healing and implant failure in Pagetic bone.
*
Range of Motion:
Gentle active-assisted and passive range of motion exercises for the hip and knee within a pain-free range.
*
Strengthening:
Isometric quadriceps and gluteal muscle strengthening. Upper extremity strengthening to assist with transfers and walker use.
*
Transfers:
Instruction on safe bed mobility and transfers to a chair.
*
Phase 2: Progressive Loading (Weeks 6-12):
*
Radiographic Assessment:
Follow-up radiographs at 6 weeks showed early signs of callus formation.
*
Weight Bearing:
Progression to partial weight-bearing (PWB) up to 50% of body weight, as tolerated, using a walker or crutches.
*
Range of Motion:
Continued progression of hip and knee ROM exercises.
*
Strengthening:
Introduction of light resistance exercises for hip abductors, adductors, flexors, extensors, and knee musculature.
*
Gait Training:
Focus on normalized gait pattern with appropriate assistive device.
*
Phase 3: Advanced Rehabilitation & Return to Function (Weeks 12+):
*
Radiographic Assessment:
Radiographs at 12 weeks demonstrated bridging callus and signs of consolidation. Clinical examination confirmed minimal pain and stable fixation.
*
Weight Bearing:
Progression to full weight-bearing (FWB) without an assistive device, as tolerated.
*
Functional Activities:
Advanced strengthening, balance, and proprioception exercises. Gait training on uneven surfaces, stair climbing.
*
Return to Activities:
Gradual return to activities of daily living. Low-impact activities encouraged. Avoidance of high-impact or contact sports indefinitely.
Long-Term Follow-up:
Regular follow-up appointments were scheduled at 6 weeks, 3 months, 6 months, and 1 year post-operatively, and annually thereafter. This included:
*
Clinical Assessment:
Evaluation of pain, function, gait, and limb length discrepancy.
*
Radiographic Assessment:
Monitoring fracture healing, implant integrity, and progression or quiescence of Paget's disease.
*
Biochemical Monitoring:
Periodic serum ALP and bone turnover markers to assess the efficacy of Paget's medical therapy and guide further treatment.
*
Complication Surveillance:
Monitoring for potential complications such as nonunion, malunion, implant failure, infection, or the rare but critical development of Paget's sarcoma. Any new or worsening pain, swelling, or radiographic changes would warrant further investigation, including biopsy.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- High Index of Suspicion for Paget's: In elderly patients presenting with fragility fractures, especially those with classic radiographic findings (cortical thickening, trabecular coarsening, bone enlargement, bowing), always consider Paget's disease. Confirm with serum Alkaline Phosphatase (ALP) and targeted imaging.
-
Pre-operative Optimization and Assessment:
- Medical Management: Ideally, acute active Paget's should be treated with bisphosphonates (e.g., zoledronic acid) or denosumab pre-operatively to suppress bone turnover and potentially improve bone quality. However, acute fracture fixation often cannot wait. Administer post-operatively if deferred.
- Imaging: CT scans with 3D reconstructions are invaluable for pre-operative planning, especially to characterize the medullary canal, which is often sclerotic and narrowed in Pagetic bone.
- Templating: Meticulous pre-operative templating for implant size, length, and entry point is essential due to altered bone geometry and canal morphology.
- Blood Loss: Be prepared for increased intraoperative blood loss due to the hypervascularity of active Pagetic bone. Cross-match sufficient blood products.
-
Surgical Strategy for Fragile Bone:
- Intramedullary Nailing (IMN): Generally preferred for subtrochanteric and diaphyseal fractures due to load-sharing properties. However, be acutely aware of the challenges posed by a sclerotic, narrowed, or bowed medullary canal.
- Careful Reaming: If IMN is chosen, ream slowly and sequentially, starting with small reamers, to prevent iatrogenic fracture of the brittle Pagetic bone.
- Alternative Fixation: Have a robust alternative plan, such as a long bridging locking plate, in case IMN is not feasible or fails intraoperatively.
- Augmentation: Consider cement augmentation (PMMA) for screws in plates or even around the IM nail if bone quality is severely compromised, particularly in fixation points. Bone grafting for comminuted areas is often beneficial.
- Biopsy: In any atypical lesion, or if suspicion of sarcomatous transformation exists, obtain a biopsy at the time of fixation.
-
Post-operative Management:
- Paget's-specific Therapy: Ensure continuation of medical therapy (bisphosphonates/denosumab) post-operatively to manage the underlying disease. Monitor ALP levels.
- Rehabilitation: Tailor weight-bearing protocols cautiously due to concerns about delayed healing and implant failure in Pagetic bone. Progressive weight-bearing based on radiographic healing and clinical comfort.
Pitfalls:
- Missing the Diagnosis of Paget's: Attributing a pathologic fracture in an elderly patient solely to osteoporosis without considering Paget's can lead to inadequate pre-operative planning and mismanagement of the underlying disease.
-
Underestimating Bone Fragility and Hypervascularity:
Failure to recognize the poor mechanical properties and hypervascularity of Pagetic bone can lead to:
- Iatrogenic Fractures: During reaming or implant insertion.
- Excessive Blood Loss: Resulting in hemodynamic instability.
- Implant Failure: Due to inadequate screw purchase or stress on the implant.
- Medullary Canal Mismatch: Forcing a standard IM nail into a sclerotic or bowed Pagetic canal without adequate reaming or appropriate implant selection can lead to iatrogenic fracture, malreduction, or nail jamming.
- Inadequate Fixation Construct: Using short implants or non-locking constructs in poor quality Pagetic bone significantly increases the risk of screw pull-out, nonunion, and implant failure.
- Failure to Biopsy Suspicious Lesions: Overlooking subtle signs of sarcomatous transformation (rapidly enlarging mass, aggressive lytic lesions, periosteal reaction) can delay diagnosis and significantly worsen prognosis for Paget's sarcoma.
- Neglecting Long-term Paget's Management: Discontinuing medical therapy for Paget's post-operatively can lead to disease progression, increased pain, and risk of further fractures or complications.
- Premature Aggressive Weight-Bearing: Allowing early full weight-bearing without sufficient radiographic healing and clinical stability in Pagetic bone increases the risk of implant failure or delayed union.
- Technical Difficulties with Reduction: The comminution and altered bone morphology can make achieving and maintaining reduction challenging, leading to malunion. Be prepared for open reduction if closed methods fail.
Clinical & Radiographic Imaging