Oncology Cases Osteosarcoma: Essential Orthopedic Insights
Patient Presentation & History
A 14-year-old male, otherwise healthy and active in school sports, presented with a 5-month history of progressive, insidious onset pain in his left knee. Initially, the pain was intermittent and activity-related, localized to the distal thigh and knee joint. Over the last 2 months, the pain became constant, worsened significantly at night, and was refractory to over-the-counter analgesics. He also reported noticing a slowly enlarging, firm mass above his left knee, which had become more prominent in the past 4-6 weeks. There was no history of acute trauma, fever, weight loss, night sweats, or other systemic symptoms. His past medical history was unremarkable, and he was not taking any regular medications. He denied any family history of malignancies. The parents reported a slight decrease in his athletic performance and a reluctance to participate in sports due to persistent discomfort.
Clinical Examination
General Inspection: The patient ambulated with an antalgic gait, demonstrating a shortened stance phase on the left lower extremity. He appeared comfortable at rest but demonstrated guarding when the left lower limb was manipulated. There was no obvious cachexia or pallor.
Local Inspection (Left Lower Extremity):
* A visible fusiform swelling was noted over the distal third of the left thigh, immediately proximal to the knee joint, measuring approximately 8x6 cm.
* The skin overlying the mass appeared taut and slightly erythematous, with subtle venous prominence.
* There were no open wounds, sinuses, or areas of ulceration.
* No muscle atrophy was immediately apparent in the thigh or calf.
Palpation (Left Lower Extremity):
* The mass was firm, fixed to the underlying bone, and elicited moderate tenderness upon palpation. It felt distinctly non-compressible and had ill-defined margins superiorly but was more discrete distally.
* The skin over the mass was warmer than the surrounding areas.
* A small to moderate knee effusion was palpable, and patellar tap was positive.
* No regional lymphadenopathy was identified in the inguinal or popliteal regions.
* Peripheral pulses (femoral, popliteal, dorsalis pedis, posterior tibial) were all robust and bilaterally symmetrical.
Range of Motion (Left Knee):
* Active and passive range of motion was significantly restricted and painful.
* Flexion was limited to 0-80 degrees (compared to 0-140 degrees on the contralateral side).
* Extension was limited to -5 degrees (extension lag), with pain at terminal extension.
* Pain was exacerbated with axial loading and rotational stresses on the knee joint.
Neurological Assessment (Left Lower Extremity):
* Sensation to light touch and pinprick was intact in all dermatomes (L2-S1).
* Motor strength was 5/5 in all muscle groups (hip flexion, extension, abduction, adduction; knee flexion, extension; ankle dorsiflexion, plantarflexion) although anti-gravity movements around the knee were painful and guarded.
* Deep tendon reflexes (patellar, Achilles) were 2+ bilaterally and symmetrical.
* No signs of nerve impingement or direct neurovascular compromise were noted, despite the mass's proximity to the neurovascular bundle.
Imaging & Diagnostics
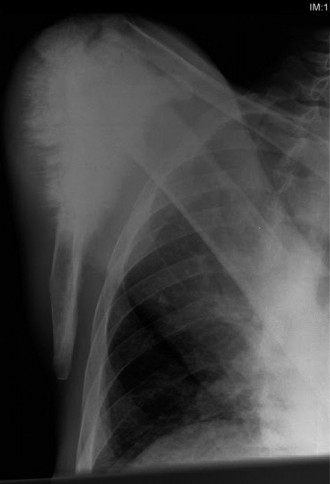
Initial Radiographs (Left Knee - Anteroposterior and Lateral Views):
* Demonstrated an aggressive, mixed lytic and blastic lesion centered in the distal femoral metaphysis, extending into the diaphysis.
* Evidence of cortical destruction and breach was observed, particularly on the anterior and lateral cortices.
* A characteristic "sunburst" periosteal reaction was prominent, indicative of rapid bone formation by the tumor.
* Codman's triangle was present along the posteromedial cortex, representing elevation of the periosteum by the expanding tumor.
* A large associated soft tissue mass was clearly visible, extending anteriorly and laterally from the distal femur, conforming to the palpable mass on examination.
* The joint space appeared preserved, but the tumor was in close proximity to the epiphyseal growth plate, though not definitively crossing it on plain films.
Magnetic Resonance Imaging (MRI) of the Left Femur (with and without contrast):
* MRI was performed for detailed local staging and surgical planning.
* Revealed a large, heterogeneously enhancing mass centered in the distal femoral metaphysis, measuring approximately 10 x 7 x 6 cm.
* The mass showed significant intramedullary extension, spanning approximately 12 cm proximally from the distal femoral articular surface.
* There was clear evidence of cortical breach and extensive extra-osseous soft tissue involvement, conforming to the radiographic findings.
* Crucially, the tumor was found to abut the popliteal neurovascular bundle posteromedially but did not appear to circumferentially encase it. The distal femoral epiphysis and articular cartilage were involved focally posteromedially, suggesting intra-articular extension in this region.
* Marrow edema was noted extensively both proximal and distal to the main tumor, but no definite skip lesions were identified within the femur or tibia.
* The biopsy tract was clearly visible extending from the lateral aspect of the thigh into the tumor.
Computed Tomography (CT) Chest, Abdomen, and Pelvis (with contrast):
* Performed to assess for distant metastatic disease.
* CT chest revealed multiple bilateral pulmonary nodules, the largest measuring 1.5 cm in the right lower lobe, highly suspicious for metastatic disease. No hilar or mediastinal lymphadenopathy was noted.
* CT abdomen/pelvis was unremarkable for metastatic disease or other primary lesions.
Technetium-99m Bone Scintigraphy:
* Demonstrated intense uptake in the distal left femur, correlating with the primary tumor site.
* No other areas of abnormal uptake suggestive of osseous metastases (skip lesions or distant bone metastases) were identified beyond the primary lesion.
Biopsy:
* An image-guided (CT-guided) core needle biopsy was performed by the orthopedic oncology team, ensuring the biopsy tract was planned in the axis of the definitive surgical incision to allow for en-bloc excision of the tract.
* Histopathological analysis revealed malignant spindle cells producing osteoid and immature woven bone, consistent with high-grade conventional osteosarcoma.
* Immunohistochemistry was not specifically required for this classic presentation but could be used to differentiate from other entities if morphology was ambiguous.
Templating:
* Detailed pre-operative templating was performed using MRI and CT scans. The required length of femoral resection to achieve wide oncologic margins (aiming for 2-3 cm of healthy bone proximal to the tumor, as assessed on MRI) was determined to be approximately 15 cm.
* This necessitated a reconstruction involving a distal femoral endoprosthesis, incorporating the knee joint. Different modular systems were considered based on patient size, bone quality, and available inventory. The potential for custom prosthesis or allograft-prosthesis composite was also discussed, but a standard modular system was deemed suitable given the estimated resection length and patient age. Considerations included attachment of the patellar tendon and collateral ligaments to the prosthesis.
Differential Diagnosis
The presentation of a painful, rapidly growing bone mass in an adolescent necessitates a broad differential diagnosis.
| Feature | Osteosarcoma (High-Grade Conventional) | Ewing Sarcoma | Acute Hematogenous Osteomyelitis (AHO) | Chondrosarcoma (Primary) |
|---|---|---|---|---|
| Typical Age | Bimodal: 10-25 years, >60 years (primary) | 5-25 years | Any age, most common in children (<10 years) | >40 years, rare in adolescents |
| Common Location | Metaphysis of long bones (distal femur, prox tibia, prox humerus) | Diaphysis/metaphysis of long bones, flat bones (pelvis, ribs) | Metaphysis of long bones (e.g., distal femur) | Flat bones (pelvis, scapula), prox femur/humerus (secondary) |
| Pain Character | Deep, aching, nocturnal, progressive; can be localized | Localized, intense, rapidly progressive; often with systemic symptoms | Acute onset, severe, localized pain; fever, chills, systemic illness | Insidious, dull ache; may become worse at night |
| Palpable Mass | Firm, fixed, tender; rapidly growing | Tender, rapidly growing; soft tissue component often larger | Tender, warm, erythematous, edematous; less distinct mass | Firm, lobulated, often slow-growing; less tenderness |
| Systemic Symptoms | Rare at presentation (unless metastatic), good general health | Common: Fever, weight loss, elevated ESR/CRP, anemia, malaise | Prominent: Fever (>38.5°C), chills, malaise, elevated ESR/CRP, leukocytosis | Generally absent unless advanced or large |
| X-ray Findings | Mixed lytic/blastic, aggressive periostitis (sunburst, Codman's triangle), cortical destruction, large soft tissue mass | Permeative lytic lesion, "onion-skin" (lamellated) periostitis, large soft tissue mass | Early: subtle soft tissue swelling, periosteal elevation. Later: focal lucency, cortical erosion, involucrum, sequestrum | Punctate/flocculent calcifications (popcorn calcification), endosteal scalloping, cortical thickening, soft tissue mass |
| MRI Findings | Heterogeneous T1/T2, intra/extra-osseous component, skip lesions, neurovascular involvement | Large soft tissue mass, intramedullary component, marrow edema, periosteal reaction; can mimic AHO | Marrow edema, subperiosteal/intracortical abscesses, sinus tracts, reactive bone formation; may enhance | Lobulated masses with high signal on T2 (cartilaginous matrix), characteristic enhancement pattern |
| Lab Markers | Elevated ALP (in 50-70% of cases), LDH; WCC, CRP usually normal | Elevated ESR/CRP, leukocytosis, anemia; LDH may be elevated | Markedly elevated ESR/CRP, leukocytosis, positive blood cultures (in 50%) | Usually normal. ALP may be mildly elevated if bone remodeling. |
| Histopathology | Malignant osteoid production by pleomorphic stromal cells; direct bone formation by tumor cells | Small round blue cell tumor; immunohistochemistry positive for CD99 (MIC2) | Inflammatory cells, necrosis, bacterial colonies; no malignant cells | Malignant cartilage production by atypical chondrocytes; no malignant osteoid |
Surgical Decision Making & Classification
The definitive diagnosis of high-grade osteosarcoma mandates a multidisciplinary approach involving pediatric oncology, radiation oncology, diagnostic and interventional radiology, pathology, and orthopedic oncology. Given the patient's age, the tumor's size and location, and the presence of lung metastases, the treatment strategy was complex.
Neoadjuvant Chemotherapy:
The initial step involved neoadjuvant (pre-operative) multi-agent chemotherapy. This strategy aims to:
1.
Downstage the tumor:
Reduce tumor size, potentially making surgical resection easier and improving local control.
2.
Treat micrometastatic disease:
Address any subclinical spread, thereby improving overall survival.
3.
Assess tumor response:
Evaluate the tumor's sensitivity to chemotherapy, which is a prognostic indicator (good response >90% necrosis correlated with improved survival).
The patient underwent 10 weeks of chemotherapy following standard protocols (e.g., using Methotrexate, Doxorubicin, Cisplatin). Post-chemotherapy imaging (MRI) showed a reduction in tumor size and signal characteristics, indicating a partial response, making limb salvage surgically feasible.
Surgical Decision: Limb Salvage vs. Amputation:
Despite the presence of lung metastases (Enneking Stage IIB with M1), limb salvage was deemed appropriate for this patient due to:
*
Achievable Wide Margins:
Post-chemotherapy imaging confirmed that a wide surgical margin (at least 2-3 cm of healthy tissue beyond the tumor extent) could be achieved, especially around the neurovascular bundle, which was not encased.
*
Absence of Irreparable Neurovascular Damage:
The neurovascular bundle was merely abutted, not invaded, meaning it could be safely dissected and preserved.
*
Preservation of Function:
Limb salvage offered the potential for a functional limb, critical for a young, active patient.
*
Patient and Family Preference:
After extensive counseling regarding the risks and benefits of both options, the family opted for limb salvage, understanding the potential for future complications and the necessity of further treatment for metastatic disease.
Amputation would have been considered if:
* Inability to obtain adequate oncologic margins (e.g., tumor extension into critical neurovascular structures that cannot be resected and reconstructed without major functional deficit).
* Pathologic fracture rendering stable reconstruction impossible or increasing local recurrence risk.
* Intra-articular contamination not amenable to complete resection.
* Severe infection or significant soft tissue loss.
* Failed response to neoadjuvant chemotherapy leading to extensive tumor progression.
Classification (Enneking Staging System for Musculoskeletal Sarcomas):
*
Grade (G):
G2 (High-grade). This was confirmed by biopsy.
*
Site (T):
T2 (Extracompartmental). The tumor breached the cortex and had an extensive extra-osseous component.
*
Metastasis (M):
M1 (Distant metastasis). Presence of bilateral lung nodules.
Therefore, the patient's osteosarcoma was staged as IIB (G2, T2, M0) prior to lung metastasis detection, then Stage III (G2, T2, M1) after detection. This systemic staging is crucial for prognosis and overall treatment planning. The immediate surgical goal remained local tumor control with wide margins, regardless of metastatic status, as this impacts local recurrence rates and long-term functional outcomes.
Surgical Technique / Intervention
Procedure: Wide en-bloc resection of the distal left femur with knee joint, followed by reconstruction with a modular distal femoral endoprosthesis.
Patient Positioning:
* The patient was positioned supine on the operating table.
* A deflated pneumatic tourniquet was applied high on the ipsilateral thigh (though often not inflated in oncologic resections to prevent potential tumor cell dissemination, or only inflated for short periods for specific tasks).
* A bolster was placed under the ipsilateral hip to allow for internal rotation of the limb and optimal exposure.
* The entire limb, from hip to toes, was prepped and draped in a sterile fashion, allowing for free manipulation of the limb and access for potential proximal femoral extension or venous access for harvesting if required. The previous biopsy incision was incorporated into the planned skin incision.
Surgical Approach:
* A long, straight anterior midline incision was made over the distal femur, extending from the mid-thigh, laterally curving around the patella, and ending distally over the anterior tibia. This incision directly incorporated the previous biopsy tract, ensuring its complete excision en-bloc with the tumor specimen.
* The skin and subcutaneous tissues were elevated carefully. The vastus medialis and lateralis were identified. The quadriceps muscle was sharply dissected off the anterior aspect of the femur.
* The plan involved a subvastus approach on the medial side and a lateral approach to isolate the femur.
Dissection and Tumor Resection (En-bloc Principles):
*
Deep Dissection:
The dissection proceeded carefully to identify critical structures while maintaining wide oncologic margins. The vastus muscles were mobilized.
*
Neurovascular Bundle Protection:
Meticulous dissection was performed posteriorly to identify and protect the popliteal artery, vein, and tibial nerve. The posterior capsule of the knee joint was carefully dissected from the tumor without violating the tumor pseudocapsule, especially given the focal intra-articular extension. The vascular pedicle (femoral artery and vein) was identified proximally and traced distally.
*
Soft Tissue Margins:
Soft tissue attachments to the tumor were resected widely. The medial and lateral collateral ligaments were sharply divided from their femoral attachments along with the resected bone. The anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) were divided at their femoral origins.
*
Proximal Osteotomy:
Based on pre-operative templating and intraoperative assessment (confirmed by frozen section of the resected marrow for clear margins), the proximal femoral osteotomy was performed approximately 15 cm proximal to the joint line, through healthy bone. A reciprocating saw was used to make a clean, perpendicular cut.
*
Distal Disarticulation/Osteotomy:
The distal resection included the entire distal femur, epicondyles, and the knee joint. The joint capsule was incised circumferentially. The patellar tendon was detached from the patella (or a patellar button of bone with the tendon attached was used if the patella was involved or for specific endoprosthesis designs). The specimen, comprising the distal femur, knee joint, and surrounding soft tissues (including the biopsy tract), was removed en-bloc.
(Image depicting a distal femoral endoprosthesis reconstruction following tumor resection)
Reconstruction with Modular Distal Femoral Endoprosthesis:
*
Femoral Preparation:
The intramedullary canal of the remaining proximal femur was reamed to accept the stem of the endoprosthesis.
*
Prosthesis Assembly:
A modular distal femoral replacement system was used. This consisted of:
* A femoral stem (cemented into the proximal femur for secure fixation, although uncemented options exist).
* A modular articulating hinge knee component, designed to replace the distal femur and articulate with the native tibia.
* A polyethylene bearing and a metal tibial tray, which would articulate with the femoral component.
*
Trial Reduction:
Trial components were inserted to assess alignment, limb length, and soft tissue tension. Adjustments were made as necessary.
*
Definitive Implantation:
The final components were assembled and implanted. The femoral stem was cemented into the proximal femur. The distal femoral component was secured to the stem. The tibial tray was cemented onto the prepared proximal tibia, ensuring correct rotational alignment.
*
Soft Tissue Reattachment:
This is a critical step for knee stability and function.
* The patellar tendon was reattached to the designated eyelets or specialized sleeve on the prosthesis using strong non-absorbable sutures (e.g., Krackow technique).
* The medial and lateral collateral ligaments, or their remnants, were reattached to soft tissue sleeves or anchor points on the prosthesis or reconstructed using synthetic grafts (e.g., Dacron) if necessary, providing mediolateral stability.
* The vastus medialis and lateralis were advanced and sutured to the quadriceps tendon and surrounding soft tissues to aid in patellar tracking and provide muscle bulk.
* Periosteal flaps and remaining muscle bellies were meticulously reapproximated to cover the prosthesis and provide soft tissue coverage, minimizing dead space and reducing infection risk.
Closure:
* A layered closure was performed, paying meticulous attention to hemostasis.
* Deep drains were placed to prevent hematoma formation.
* The fascia, subcutaneous layers, and skin were closed with appropriate sutures. A sterile dressing was applied.
Post-Operative Protocol & Rehabilitation
Immediate Post-Operative Period (Day 0-7):
*
Pain Management:
Aggressive multimodal analgesia (IV patient-controlled analgesia, regional nerve blocks, oral opioids/non-opioids).
*
DVT Prophylaxis:
Pharmacological (low molecular weight heparin) and mechanical (intermittent pneumatic compression devices) prophylaxis.
*
Wound Care:
Strict sterile dressing changes, monitoring for signs of infection or hematoma. Drains typically removed when output is minimal (<30-50 mL/24h).
*
Positioning:
Limb elevated, knee splinted in full extension to protect soft tissue repairs, particularly the patellar tendon reattachment.
*
Weight-Bearing:
Strict non-weight-bearing (NWB) on the operative limb, typically for 6-8 weeks to allow for soft tissue healing and bony integration (if uncemented) or cement setting.
*
Early Motion:
Passive range of motion (PROM) for the knee using a continuous passive motion (CPM) machine, usually initiated cautiously (e.g., 0-30 degrees) on POD 1-3, gradually increasing as tolerated to prevent arthrofibrosis. Hip and ankle active range of motion (AROM) encouraged.
Acute Rehabilitation Phase (Weeks 2-12):
*
Physical Therapy (PT):
Intensified PT focusing on:
*
Gradual Increase in ROM:
Progressing knee flexion and extension within protected limits, aiming for functional range (0-90 degrees initially).
*
Isometric Strengthening:
Quadriceps, hamstrings, gluteals, and calf muscles.
*
Gait Training:
Progression from NWB to toe-touch weight-bearing (TTWB) or partial weight-bearing (PWB) with crutches or a walker, as per surgeon's discretion based on stability of reconstruction and soft tissue healing.
*
Scar Management:
Massage and desensitization.
*
Adjuvant Chemotherapy:
Commenced once surgical wound healing was adequate (typically 3-4 weeks post-op) to treat residual microscopic disease and control lung metastases. The specific regimen and duration would be determined by the oncology team.
Intermediate to Long-Term Rehabilitation (Months 3-12+):
*
Progressive Weight-Bearing:
Gradually advance to full weight-bearing (FWB) over several weeks, with discontinuation of assistive devices as strength and balance improve.
*
Strengthening:
Progressive resistance exercises, focusing on regaining full strength and endurance of the entire lower extremity.
*
Proprioceptive Training:
Balance exercises, gait training on various surfaces.
*
Functional Training:
Return to activities of daily living (ADLs), and eventually modified recreational activities. High-impact sports are generally discouraged due to the risk of prosthesis loosening or failure.
*
Psychosocial Support:
Ongoing support for the patient and family is critical, addressing body image, emotional well-being, and adaptation to life with a prosthesis.
Oncologic Surveillance:
*
Local Recurrence:
Regular clinical exams and imaging (X-rays, MRI of the operative limb) every 3-6 months for the first 2-3 years, then annually.
*
Distant Metastasis:
CT chest every 3-4 months for the first 2-3 years, then less frequently. Bone scans periodically.
*
Lifelong Follow-up:
Essential due to the potential for late local recurrence, prosthesis complications, or secondary malignancies.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
-
Biopsy Protocol:
The single most critical diagnostic step.
- Done by Definitive Surgeon: The biopsy should be performed by, or in close consultation with, the orthopedic oncologist who will perform the definitive resection.
- Longitudinal Incision: Biopsy incision must be longitudinal and placed such that it can be entirely excised en-bloc with the tumor during definitive surgery.
- Avoid Contamination: Care must be taken to minimize hematoma and soft tissue contamination along the biopsy tract.
- Histological Confirmation: Never proceed with definitive surgery without a confirmed histological diagnosis from a reputable pathology service.
- Multidisciplinary Tumor Board: Essential for optimal patient management. Discussion with oncology, radiology, pathology, and surgery optimizes staging, treatment sequencing (neoadjuvant/adjuvant chemotherapy), and surgical planning.
-
Pre-operative Staging:
Thorough imaging is paramount.
- MRI: Gold standard for local staging (intramedullary extent, soft tissue involvement, neurovascular proximity, skip lesions, intra-articular extension).
- CT Chest: Mandatory for lung metastases (most common site).
- Bone Scan: Assess for other osseous metastases or skip lesions.
- Oncologic Margins: The primary goal of surgery is en-bloc resection with wide, tumor-free margins. This dictates the extent of resection, even if it means sacrificing more tissue or structures. Frozen sections of bone margins intraoperatively are crucial.
- Limb Salvage Considerations: While often preferred, it must not compromise oncologic safety. Criteria include ability to achieve wide margins, adequate soft tissue coverage, and a reconstructive option offering good long-term function.
- Chemotherapy Integration: Osteosarcoma is a chemosensitive tumor. Neoadjuvant and adjuvant chemotherapy are integral components of treatment and significantly improve survival rates.
- Reconstruction Planning: Detailed pre-operative templating is essential for choosing the appropriate endoprosthesis, determining the length of resection, and anticipating challenges in soft tissue reattachment and stability.
- Rehabilitation: Aggressive but cautious rehabilitation is vital for optimizing functional outcomes post-reconstruction. Understanding the limitations of the prosthesis is crucial for patient education.
Pitfalls:
-
Inadequate Biopsy:
- Transverse Incision: Makes en-bloc excision of the tract challenging and increases local recurrence risk.
- Hematoma/Infection: Poor biopsy technique can lead to hematoma formation, making subsequent dissection difficult, or infection, complicating limb salvage.
- Incorrect Site: Biopsy of reactive bone or necrotic tissue can lead to a misdiagnosis.
- "Seeding": Tumor cell dissemination along a poorly performed biopsy tract.
- Insufficient Staging: Proceeding to surgery without a complete workup (e.g., missing lung metastases) can lead to inappropriate treatment.
- Compromised Surgical Margins: Attempting to "save" tissue or vital structures at the expense of oncologic margins significantly increases the risk of local recurrence, often necessitating further, more aggressive surgery (e.g., amputation).
- Neurovascular Injury: Aggressive dissection in the vicinity of critical structures without clear identification and protection.
- Failure to Reconstruct Soft Tissues: Inadequate reattachment of patellar tendon, collateral ligaments, or muscle coverage can lead to extensor lag, instability, dislocation, or infection.
- Infection: Endoprosthetic reconstructions are highly susceptible to infection, which can be devastating and often requires implant removal. Meticulous surgical technique, perioperative antibiotics, and adequate soft tissue coverage are key.
- Prosthetic Complications: Aseptic loosening, mechanical failure (fracture of implant), periprosthetic fracture, joint instability, or pain can necessitate revision surgery.
- Delay in Diagnosis: Prolonged symptoms without appropriate investigation can lead to larger tumors, increased risk of metastasis, and more complex treatment.
- Ignoring Metastatic Disease: While limb salvage for the primary tumor is important, osteosarcoma has a high propensity for pulmonary metastasis. A comprehensive oncologic treatment plan addressing systemic disease is essential.

