Patient Presentation & History
A 68-year-old male presented to the emergency department with a chief complaint of acute onset left thigh pain and inability to bear weight after a minor fall from standing height. He reported simply losing his balance and twisting his leg, followed by immediate, severe pain. The mechanism of injury was low-energy, inconsistent with the severity of the clinical findings in a healthy individual.
His past medical history was significant for hypertension, hyperlipidemia, and well-controlled type 2 diabetes mellitus. Of particular note, he had a history of prostate cancer diagnosed 8 years prior, treated with radical prostatectomy and adjuvant radiation therapy. He had been in remission with stable PSA levels until approximately 18 months ago, when his PSA began to slowly trend upwards, reaching 28 ng/mL at his last oncology visit three months prior. He also reported a 6-month history of dull, aching left hip and thigh pain, initially intermittent but progressively worsening, especially at night and with weight-bearing. He attributed this to "old age" and activity. There was no history of fever, chills, night sweats, or recent unintentional weight loss. He is a non-smoker and consumes alcohol occasionally. His family history is unremarkable.
This presentation, characterized by a pathological fracture in a patient with a known history of malignancy and antecedent pain, immediately raised suspicion for metastatic bone disease. The minor trauma served as a "last straw" for an already compromised bone.
Clinical Examination
Upon examination, the patient was alert and oriented, in moderate distress dueating to pain. He appeared somewhat frail but not overtly cachectic.
Local Examination (Left Lower Extremity):
*
Inspection:
Marked swelling and ecchymosis were noted over the lateral aspect of the left thigh, extending from the greater trochanter to the mid-diaphysis. A distinct external rotation and shortening deformity of the left lower limb was evident, consistent with a left subtrochanteric femoral fracture. The skin was intact, without evidence of open wounds or blistering.
*
Palpation:
Diffuse tenderness was elicited over the proximal and mid-shaft of the left femur. Gross instability and crepitus were palpable with gentle manipulation. The skin was warm to touch over the affected area, but no specific mass was appreciated separate from the fracture hematoma.
*
Range of Motion (ROM):
Active ROM of the left hip and knee was severely restricted and painful. Passive ROM was similarly limited and elicited significant pain. The patient was unable to bear any weight on the left lower extremity.
*
Neurological Assessment:
Distal sensation (light touch, pinprick) was intact in the distribution of the femoral, obturator, peroneal, and tibial nerves. Motor function was assessed as 5/5 in the right lower extremity, and grossly limited due to pain in the left, but he could weakly flex his hip and dorsiflex his ankle, indicating no gross neurological deficit.
*
Vascular Assessment:
Distal pulses (femoral, popliteal, dorsalis pedis, posterior tibial) were strong, symmetric, and easily palpable bilaterally. Capillary refill was brisk in all digits of the left foot.
*
Systemic Examination:
A brief systemic examination revealed no palpable lymphadenopathy, hepatosplenomegaly, or other overt signs of widespread malignancy. Respiratory and cardiovascular examinations were unremarkable.
The clinical presentation, particularly the deformity, gross instability, and patient history, strongly suggested a pathological subtrochanteric femoral fracture secondary to metastatic disease.
Imaging & Diagnostics
Immediate imaging studies were obtained in the emergency department.
1. Radiographs (X-rays):
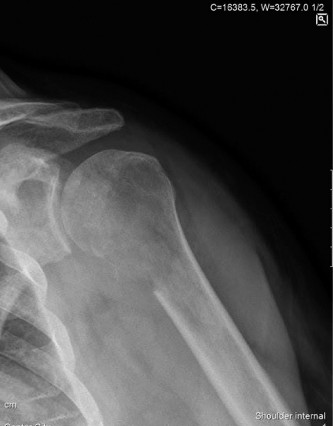
Anterior-posterior (AP) and lateral views of the left hip and femur confirmed a complete, displaced, comminuted subtrochanteric fracture of the left femur. The fracture line extended from below the lesser trochanter into the mid-diaphysis. Critically, the radiographs revealed a large, destructive, mixed lytic and blastic lesion involving the subtrochanteric region, with significant cortical destruction and endosteal scalloping, consistent with a pathological fracture. There was evidence of periosteal reaction adjacent to the lesion, indicating aggressive bone remodeling. The lesion measured approximately 8 cm in craniocaudal extent.
-
2. Computed Tomography (CT) Scan:
A CT scan of the left femur and pelvis was performed to further delineate the extent of bone destruction, soft tissue involvement, and fracture morphology. The CT confirmed the extensive lytic and sclerotic changes within the subtrochanteric region of the left femur, with complete cortical breach circumferentially. A large associated soft tissue mass, inseparable from the fracture hematoma, was noted, measuring approximately 9 x 6 x 7 cm. This soft tissue component raised concerns for tumor extension. The contralateral femur showed no obvious lesions on initial imaging. A CT chest, abdomen, and pelvis was subsequently performed for staging, revealing multiple bilateral pulmonary nodules, suspicious for metastatic lung disease, and retroperitoneal lymphadenopathy. No clear evidence of primary lung malignancy was seen, but the findings were highly suggestive of widespread metastatic disease.
3. Magnetic Resonance Imaging (MRI):
An MRI of the left femur was obtained for detailed assessment of marrow involvement, soft tissue extension, and proximity to neurovascular structures. T1-weighted sequences demonstrated diffuse low signal intensity throughout the subtrochanteric and proximal diaphyseal marrow, extending beyond the visible fracture, indicating widespread marrow infiltration. T2-weighted and STIR sequences showed high signal intensity within the lesion and surrounding soft tissue, consistent with edema, hemorrhage, and tumor burden. The femoral artery and nerve appeared to be intimately associated with the medial aspect of the soft tissue mass but not overtly compressed. MRI was also critical in identifying the exact proximal and distal extent of marrow involvement, guiding surgical margin planning for intramedullary nail placement.
4. Bone Scintigraphy (Technetium-99m Bone Scan):
A whole-body bone scan was performed to assess for other skeletal metastases. It revealed intense uptake in the left proximal femur, correlating with the known lesion. Additionally, abnormal increased uptake was noted in the T8 vertebral body, right iliac wing, and left humeral head, confirming multifocal skeletal metastatic disease. This provided a comprehensive overview of the metastatic burden.
5. Positron Emission Tomography – Computed Tomography (PET-CT):
A PET-CT scan was performed to identify the metabolic activity of the lesions and to search for the primary tumor, given the widespread metastatic pattern. It showed intensely fluorodeoxyglucose (FDG)-avid lesions in the left proximal femur, T8 vertebra, right iliac wing, left humeral head, and the previously noted pulmonary nodules and retroperitoneal lymphadenopathy. No definitive primary lung lesion was identified that was distinct from the metastatic nodules. The findings were most consistent with metastatic prostate adenocarcinoma, given the patient's history and the mixed lytic/blastic nature of the lesions, though definitive confirmation would require biopsy.
6. Biopsy:
Given the widespread disease and the need for histological confirmation, a CT-guided core needle biopsy of the left femoral lesion was performed by interventional radiology. Histopathological analysis confirmed metastatic adenocarcinoma, positive for PSA and androgen receptor (AR) immunohistochemical staining, consistent with prostate cancer origin. Gleason score could not be definitively assessed from the metastatic tissue, but the findings confirmed the diagnosis.
7. Laboratory Tests:
Initial blood work revealed normocytic anemia (Hemoglobin 10.2 g/dL), mild hypercalcemia (ionized calcium 1.40 mmol/L, normal range 1.15-1.35 mmol/L), and elevated alkaline phosphatase (180 U/L, normal range 40-120 U/L), indicating significant bone turnover. Prostate-specific antigen (PSA) was elevated at 32 ng/mL. Renal and liver function tests were within normal limits. Serum protein electrophoresis and urine protein electrophoresis were normal, effectively ruling out multiple myeloma.
8. Pre-operative Templating:
Based on the imaging, pre-operative templating was performed. A long cephalomedullary nail was deemed the most appropriate fixation strategy for this subtrochanteric fracture with significant diaphyseal extension. Measurements were taken from the contralateral femur and available images to determine appropriate nail length, diameter, and screw placement. The nail was planned to extend at least two cortical diameters beyond the distal extent of the tumor on MRI, and proximally to engage the femoral head adequately. The extent of the lesion mandated a nail that bypassed the entire fracture and tumor zone, ideally extending into the distal metaphysis to prevent distal fracture.
Differential Diagnosis
The clinical presentation and initial imaging in a patient with a known malignancy history strongly favored metastatic bone disease. However, it is imperative to consider other pathologies, particularly when the primary tumor status is unknown or the imaging is equivocal. Below is a detailed comparison of relevant differential diagnoses:
| Feature | Metastatic Bone Disease (e.g., Prostate, Breast) | Primary Bone Sarcoma (e.g., Osteosarcoma) | Primary Multiple Myeloma | Other considerations (e.g., Infection, Benign Tumors) |
|---|---|---|---|---|
| Age | Typically >50 years (median 60s-80s) | Bimodal: 10-20 years (peak), >60 years (secondary peak) | >50 years (median 69) | Any age, but specific benign lesions have typical age ranges (e.g., GCT 20-40) |
| Clinical History | Known primary malignancy, antecedent pain, weight loss, systemic symptoms | Localized pain, swelling, constitutional symptoms less common | Diffuse bone pain, fatigue, renal dysfunction, recurrent infections, hypercalcemia | Fever, chills, trauma history, specific syndrome (e.g., fibrous dysplasia, Paget's) |
| Lesion Type (X-ray) | Predominantly lytic (e.g., lung, renal, thyroid, breast), blastic (prostate, breast), or mixed. Often cortical destruction. | Mixed lytic/blastic, often aggressive. Can be purely lytic or blastic. | Purely lytic, "punched-out" lesions, diffuse osteopenia, pathological fractures. | Lytic (GCT, ABC), sclerotic (Paget's), mixed (FD). May have specific characteristics. |
| Cortical Integrity | Often breached, leading to pathological fracture. Endosteal scalloping. | Aggressive cortical destruction, often with an associated soft tissue mass. | Thinning of cortex, "punched-out" erosions without reactive sclerosis. | Variable. GCT causes cortical thinning, ABC expands cortex, Paget's has thickened cortex. |
| Periosteal Reaction | Minimal or absent, unless associated with pathological fracture or aggressive lesion. | Often prominent and aggressive: Codman's triangle, sunburst, lamellated ("onion peel"). | Absent or minimal. | Absent (most benign lesions), or less aggressive (e.g., solid periosteal reaction in chronic osteomyelitis). |
| Soft Tissue Mass | Common, especially with pathological fracture or aggressive lesions. | Very common and often large, infiltrating adjacent structures. | Less common, usually only with large plasmacytomas or extreme cortical destruction. | Variable. ABC can have soft tissue component, chronic osteomyelitis can have abscess. |
| Laboratory | Elevated Ca, Alk Phos (variable), specific tumor markers (PSA, CEA, CA 15-3). Anemia. | Elevated Alk Phos, LDH. | M-spike (SPEP/UPEP), Bence-Jones proteinuria, anemia, hypercalcemia, renal failure. | Elevated ESR/CRP/WBC (infection), elevated Alk Phos (Paget's), normal (most benign). |
| MRI Features | Marrow infiltration beyond visible bone destruction, often diffuse edema. | Heterogeneous signal, prominent soft tissue component, aggressive enhancement. | Diffuse marrow infiltration, multifocal lesions, absence of periosteal reaction. | Variable. Cystic components (ABC), fat suppression changes (infection). |
| Bone Scan | Multiple foci of increased uptake (hot spots) common, indicating widespread disease. | Focal, intensely increased uptake. May be multifocal in skip lesions. | Usually cold or mildly hot on Tc-99m scan (purely lytic without osteoblastic activity). PET-CT more sensitive. | Focal uptake (infection, Paget's), or variable (benign tumors). |
| Biopsy | Carcinoma cells (specific to primary tumor origin, e.g., adenocarcinoma). | Malignant cells (e.g., osteoblasts producing osteoid for osteosarcoma). | Plasma cells (often >10% marrow involvement). | Inflammatory cells (infection), specific benign tumor histology (GCT giant cells). |
| Treatment | Fixation/reconstruction, radiation, systemic therapy. | Neoadjuvant chemo, surgery, adjuvant chemo. | Systemic therapy (chemo, novel agents), radiation, supportive care, fixation. | Specific to diagnosis (antibiotics, curettage, observation, resection). |
In the presented case, the patient's age, known prostate cancer history, elevated PSA, mixed lytic/blastic lesion on X-ray, multifocal skeletal disease on bone scan/PET-CT, and definitive biopsy confirming metastatic adenocarcinoma all strongly pointed towards metastatic prostate cancer. While a primary bone sarcoma was a possibility given the aggressive appearance, the systemic spread and known primary cancer shifted the diagnosis away from a primary bone tumor. Multiple myeloma was less likely due to the mixed lytic/blastic nature of the lesion (myeloma is typically purely lytic with punched-out lesions) and normal SPEP/UPEP.
Surgical Decision Making & Classification
The primary goals in managing this patient's pathological subtrochanteric femoral fracture were:
1.
Pain relief:
The fracture was acutely painful and disabling.
2.
Restoration of function:
Allow the patient to mobilize and bear weight, improving quality of life.
3.
Local tumor control:
Stabilize the bone and prevent further fracture or progression.
4.
Facilitation of adjuvant therapy:
Provide a stable construct to allow for post-operative radiation and systemic therapies.
5.
Preservation of neurological/vascular integrity:
Prevent complications from fracture displacement or tumor expansion.
Operative vs. Non-operative:
Given the patient's acute, complete, displaced, and painful pathological fracture of a major weight-bearing bone, non-operative management was not a viable option. Non-operative treatment would involve prolonged bed rest, intractable pain, significant morbidity (DVT, decubitus ulcers, pneumonia), and permanent loss of ambulation. Surgical stabilization was imperative.
Classification and Prognostic Indicators:
1.
Mirels' Score:
This classification system is crucial for evaluating the risk of impending pathological fractures and guiding prophylactic fixation.
*
Site:
Proximal femur (weight-bearing) = 3 points
*
Pain:
Weight-bearing pain = 3 points
*
Lesion Type:
Mixed lytic/blastic = 2 points
*
Size:
>2/3 cortical involvement (approximately 8 cm lesion in a bone roughly 3 cm diameter) = 3 points
*
Total Mirels' Score = 3 + 3 + 2 + 3 = 11 points.
A score of 9 or greater strongly indicates the need for prophylactic fixation, and in this case, an actual fracture occurred, further emphasizing the need for intervention.
-
Tokuhashi Score and Katagiri Score:
These prognostic scoring systems are used to estimate patient survival in metastatic spinal disease, but the principles can be applied to inform the aggressiveness of treatment for appendicular skeletal metastases. While not directly used for fixation type, they guide the extent of surgery.
- Tokuhashi Score: Considers general condition, number of extraskeletal metastases, primary cancer type, paralysis, and metastasis to major organs. In this case, with prostate cancer (favorable prognosis among primaries), multiple extraskeletal metastases (lung, lymph nodes), and good general condition, the score would suggest a reasonable life expectancy (e.g., 6-12 months).
- Katagiri Score: Also considers age, general condition, number of bone metastases, number of visceral metastases, and primary tumor type. Similar to Tokuhashi, this patient's profile suggested a reasonable prognosis to warrant aggressive, durable fixation.
Surgical Choice:
For subtrochanteric and proximal diaphyseal femoral fractures in metastatic disease,
intramedullary (IM) nailing
is generally the preferred method of fixation for several reasons:
*
Load sharing:
IM nails share load with the bone, reducing stress shielding and the risk of hardware failure compared to plates.
*
Minimally invasive:
Less soft tissue dissection compared to extensive plating or prosthetic replacement, potentially reducing operative time, blood loss, and infection risk.
*
Durable fixation:
Provides robust stability, allowing early weight-bearing and facilitating adjuvant radiation.
*
Bypasses the entire lesion:
A long IM nail can extend well beyond the tumor margins, providing prophylactic fixation against potential skip lesions or future fractures.
*
Adjuvant cement:
Allows for percutaneous cement augmentation (PMMA) of the lesion after nailing, further enhancing stability and local tumor control through thermal necrosis.
While a proximal femoral endoprosthesis or total hip arthroplasty could be considered for very extensive destruction of the femoral head/neck or periacetabular region, in this case, the fracture was primarily subtrochanteric with diaphyseal extension, making IM nailing a more appropriate and less morbid choice for durable fixation, especially given the anticipated need for post-operative radiation.
Therefore, the decision was made for surgical stabilization with a long cephalomedullary nail.
Surgical Technique / Intervention
Pre-operative Preparation:
The patient was type and cross-matched for 2 units of packed red blood cells. Given his diabetes, perioperative glucose control was optimized. Prophylactic antibiotics (Cefazolin) were administered pre-incision. Deep vein thrombosis (DVT) prophylaxis (sequential compression devices) was initiated.
1. Patient Positioning and Anesthesia:
The patient was placed supine on a fracture table. The left foot was placed in a boot with appropriate traction to assist with reduction. The contralateral limb was abducted and flexed at the hip to provide clearance for the image intensifier. A general anesthetic was administered. Preparation and draping were performed to ensure a sterile field encompassing the entire left lower extremity from the ipsilateral iliac crest to the foot.
2. Surgical Approach:
A standard trochanteric entry point was utilized. A 5 cm longitudinal skin incision was made just proximal to the tip of the greater trochanter, slightly lateral to the midline. Dissection was carried down through the gluteus medius fibers to expose the greater trochanter.
3. Entry Point and Reaming:
A starting awl was used to create an entry portal at the tip of the greater trochanter, in line with the femoral shaft axis on both AP and lateral fluoroscopic views.
Initial reaming was performed using a flexible-shaft reamer, gradually increasing the reamer size. Due to the lytic nature of the tumor, reaming was performed gently and carefully to avoid further fracture propagation or uncontrolled tumor spread. Reaming bypassed the fracture site and the entire tumor burden, extending distally to approximately 1 cm larger than the intended nail diameter. The canal was reamed to 17mm. Careful fluoroscopic monitoring was essential throughout reaming to ensure centralization and avoid iatrogenic perforation.
4. Fracture Reduction:
Achieving and maintaining reduction of the comminuted subtrochanteric fracture was critical. Traction on the fracture table was adjusted, and external rotation was applied to reduce the external rotation deformity. Manipulative techniques, including direct pressure over the greater trochanter and manual alignment of the distal fragment, were utilized under fluoroscopic guidance. In this comminuted subtrochanteric fracture, an open reduction technique with limited exposure of the fracture site was required to gain anatomical alignment. A K-wire was used to provisionally hold the reduction.
Consideration was also given to injecting polymethylmethacrylate (PMMA) cement into the fracture gap and tumor defect prior to nail insertion to augment stability and fill the void left by the tumor. However, given the comminution and risk of cement extravasation, this was deferred to post-nailing augmentation.
5. Nail Insertion:
A 15mm diameter, 420mm long cephalomedullary nail (e.g., Trochanteric Fixation Nail - TFN) was selected, based on pre-operative templating. The nail was advanced carefully into the femoral canal. The cephalic component of the nail was seated appropriately in the femoral neck and head. Fluoroscopy was used to confirm proper nail position, ensuring it was centered in the canal and bypassed the entire tumor lesion distally, extending into the healthy bone of the distal metaphysis.
6. Proximal Locking:
Using the jig, two lag screws were inserted through the nail into the femoral head and neck, providing robust angular stability for the proximal fragment and resisting rotation. Screw length was confirmed with fluoroscopy.
7. Distal Locking:
After confirming the final rotational alignment of the femoral shaft and fracture reduction, two distal locking screws were inserted using a free-hand technique under fluoroscopic guidance. An image intensifier was positioned to obtain a perfect circle of the distal locking holes, and a drill guide was used for precise screw placement. The distal screws were placed bicortically to provide rotational and axial stability to the distal fragment.
8. Cement Augmentation (Adjuvant Therapy):
Following definitive fixation with the IM nail, the remaining lytic defect within the subtrochanteric region, which still contained tumor burden, was augmented with PMMA bone cement. Under fluoroscopic guidance, small incisions were made laterally over the tumor defect. Cannulated awls or trocars were used to create access points into the tumor bed. Low-viscosity PMMA cement was injected incrementally into the tumor cavity and fracture defect, filling the void and providing additional mechanical stability. The exothermic reaction of PMMA polymerization also provides a local thermal ablation effect on residual tumor cells. Care was taken to avoid extravasation of cement into the soft tissues or joint.
9. Wound Closure:
The surgical site was thoroughly irrigated. Hemostasis was achieved. A layered closure was performed, with closure of the gluteus medius fascia, subcutaneous tissue, and skin. A sterile dressing was applied.
Intraoperative Considerations and Pitfalls:
*
Blood Loss:
Pathological fractures, especially with large tumor burdens, can be associated with significant intraoperative bleeding. Blood loss was estimated at 1200 mL and managed with fluid resuscitation and one unit of packed red blood cells.
*
Tumor Seeding:
Careful handling of the tumor tissue during reaming and cement augmentation is crucial to minimize the risk of tumor cell dissemination.
*
Iatrogenic Fracture:
Fragile bone due to tumor makes the femur susceptible to iatrogenic fractures during reaming or nail insertion.
*
Inadequate Fixation:
Failure to extend the nail sufficiently beyond the tumor or poor locking screw placement can lead to early hardware failure or periprosthetic fracture.
*
Malreduction:
Incorrect rotational or angular alignment can lead to functional impairment.
Post-Operative Protocol & Rehabilitation
Immediate Post-Operative Period:
*
Pain Management:
A multimodal pain management strategy was initiated, including scheduled oral analgesics (acetaminophen, NSAIDs if not contraindicated) and patient-controlled analgesia (PCA) with opioids initially, transitioning to oral opioids as tolerated. Regional nerve blocks were considered pre-operatively but not utilized in this case due to the chosen anesthetic approach. Gabapentinoids were considered for neuropathic pain components.
*
DVT Prophylaxis:
Pharmacological DVT prophylaxis (e.g., low molecular weight heparin) was initiated within 12-24 hours post-operatively, once surgical bleeding risk was minimized, and continued for 4-6 weeks.
*
Weight Bearing:
The patient was encouraged to mobilize and bear weight as tolerated on the operated limb, leveraging the robust stability provided by the long cephalomedullary nail and PMMA augmentation. Physiotherapy commenced on post-operative Day 1.
Rehabilitation Phase:
*
Physical Therapy (PT):
*
Day 1-3:
Focus on pain control, bed mobility, transfers, and protected weight-bearing to tolerance with an assistive device (walker). Gentle active and passive range of motion exercises for the hip and knee were initiated. Quadriceps and gluteal isometric exercises were started.
*
Week 1-2:
Progressive ambulation with a walker, increasing distance and duration. Continued ROM and strengthening exercises, focusing on hip abductors, extensors, and knee flexors/extensors. Stair training initiated if appropriate.
*
Weeks 3-6:
Progression to a cane for ambulation. Advanced strengthening exercises, proprioceptive training, and balance activities. Emphasis on restoring functional independence.
*
Beyond 6 weeks:
Transition to outpatient physical therapy. Focus on advanced strengthening, endurance, and return to pre-morbid activities as tolerated, considering the patient's overall medical condition and oncologic prognosis.
*
Occupational Therapy (OT):
Assessment and training for activities of daily living (ADLs), home safety modifications, and use of adaptive equipment to promote independence.
Oncologic Management and Follow-up:
*
Adjuvant Radiation Therapy:
The patient was evaluated by radiation oncology within 1 week post-operatively. External beam radiation therapy (EBRT) to the operated site was initiated approximately 3-4 weeks post-surgery, once wound healing was sufficient. The goal of radiation was local tumor control, reduction of pain, and prevention of local recurrence.
*
Systemic Therapy:
The medical oncology team adjusted the patient's systemic therapy for prostate cancer, introducing new generation anti-androgen therapy and considering chemotherapy based on the widespread metastatic disease and PSA progression.
*
Regular Follow-up:
*
Orthopedic Trauma Clinic:
Follow-up at 2 weeks, 6 weeks, 3 months, 6 months, and annually thereafter, with interval radiographs to monitor implant stability, healing, and assess for any local recurrence or further skeletal events.
*
Medical Oncology:
Regular follow-up for monitoring of systemic disease, PSA levels, and management of systemic therapies.
*
Radiation Oncology:
Follow-up to monitor response to radiation and manage potential side effects.
Potential Complications and Monitoring:
*
Hardware failure:
Careful monitoring for implant loosening, breakage, or cutout, especially at the tumor-bone interface.
*
Local tumor recurrence:
Although debulked and irradiated, recurrence is possible. Vigilant clinical and radiological surveillance is required.
*
New skeletal metastases:
Ongoing risk in a patient with widespread disease. Regular bone scans or PET-CT scans are typically performed by oncology.
*
Non-union/Delayed union:
The healing potential of pathological fractures is compromised by tumor and radiation. PMMA augmentation helps mitigate this.
*
Infection:
Despite prophylactic antibiotics, the presence of tumor and hardware increases infection risk.
*
DVT/PE:
Continued vigilance and prophylaxis.
The comprehensive post-operative and rehabilitative care, coordinated with oncology, aims to optimize functional recovery and quality of life while effectively managing the underlying oncological disease.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- "Metastasis Until Proven Otherwise": In any older adult presenting with a painful, destructive bone lesion, especially a pathological fracture, the diagnosis is metastatic disease until unequivocally disproven. Maintain a high index of suspicion.
-
Thorough Systemic Workup is Mandatory:
A comprehensive oncologic workup is essential. This includes:
- Whole-body imaging: Bone scan (Tc-99m), PET-CT, or whole-body MRI to identify all skeletal lesions and guide treatment.
- Primary tumor search: CT chest/abdomen/pelvis (or PET-CT) to identify the primary tumor and assess visceral metastases.
- Laboratory markers: CBC, LFTs, renal function, Ca/Alk Phos, and specific tumor markers (PSA, CEA, CA 19-9, CA 125, etc.) as indicated. SPEP/UPEP to rule out myeloma.
- Mirels' Score is Your Guide: Utilize the Mirels' scoring system for impending pathological fractures. A score of 7 or greater warrants prophylactic internal fixation to prevent catastrophic fracture. Do not wait for a complete fracture in high-risk lesions.
- Biopsy is Essential for Diagnosis: Always obtain a tissue diagnosis (CT-guided core needle biopsy often preferred) before definitive surgical fixation, especially if the primary tumor is unknown or the lesion is atypical. This guides oncologic management. Ensure the biopsy tract is amenable to resection or is in the planned surgical approach.
- Definitive Fixation for Pathological Fractures: Pathological fractures of weight-bearing bones require robust, definitive internal fixation or prosthetic reconstruction. Anticipate poor healing potential due to tumor and radiation.
- Intramedullary Nails are Gold Standard for Long Bones: For diaphyseal and subtrochanteric/intertrochanteric femoral metastases, a long cephalomedullary nail is generally the implant of choice. It provides load-sharing stability, bypasses the entire lesion, and can extend prophylactically.
- PMMA Augmentation is Key: Adjuvant polymethylmethacrylate (PMMA) cement augmentation provides immediate mechanical stability, fills bone defects, and creates a thermal cytotoxic effect on residual tumor cells. It is particularly useful in lytic defects and enhances hardware longevity.
- Team Approach is Paramount: Close collaboration with medical oncologists, radiation oncologists, and palliative care specialists is crucial for optimizing patient care, timing adjuvant therapies, and managing overall prognosis.
- Early Mobilization: Encourage early weight-bearing and mobilization post-operatively to improve quality of life and prevent complications of immobility, leveraging the stable fixation.
Pitfalls:
- Misdiagnosis: Mistaking a metastatic lesion for a benign process, a primary bone tumor, or an infection without adequate workup. This can lead to inappropriate treatment.
- Inadequate Biopsy: Performing an open biopsy without careful planning, contaminating soft tissues, or obtaining non-diagnostic samples, thus delaying diagnosis and definitive treatment.
- Underestimation of Mechanical Demands: Using inadequate fixation (e.g., plating alone for significant bone loss in a weight-bearing long bone) without adjuvant cement or prosthetic replacement, leading to early hardware failure.
- Failure to Extend Fixation: Not extending the implant sufficiently proximally and distally beyond the tumor margins (at least two cortical diameters from the visible tumor on MRI) results in periprosthetic fractures.
- Ignoring Prognosis: Over-aggressive surgery in patients with very limited life expectancy may lead to unnecessary morbidity without significant improvement in quality of life. Conversely, under-treatment in patients with good prognoses can lead to early failure.
- Delaying Adjuvant Therapy: Unnecessary delays in initiating post-operative radiation therapy can compromise local tumor control and increase the risk of recurrence.
- Inadequate Pain Control: Failure to address cancer-related bone pain comprehensively can severely impact the patient's quality of life and rehabilitation potential.
- Neurological Complications: Aggressive reaming or misplaced screws can lead to iatrogenic nerve injury, especially in the setting of cortical destruction.
- Poor Communication: Lack of clear communication and coordinated care between orthopedic surgeons and oncology teams can lead to suboptimal outcomes.

