Full Question & Answer Text (for Search Engines)
Question 1:
A 45-year-old male sustains a pelvic ring injury and requires surgical fixation via an anterior intrapelvic (modified Stoppa) approach. During dissection along the superior pubic ramus, brisk arterial bleeding is encountered. This bleeding is most likely originating from the 'corona mortis'. Which of the following describes the most common anatomical configuration of this vascular structure?
Options:
- An anastomosis between the internal pudendal artery and the inferior gluteal artery
- An anastomosis between the obturator vessels and the external iliac or inferior epigastric vessels
- An anastomosis between the superior gluteal artery and the iliolumbar artery
- A terminal branch of the internal iliac artery directly supplying the pubic symphysis
- An aberrant branch of the femoral artery traversing the inguinal canal
Correct Answer: An anastomosis between the obturator vessels and the external iliac or inferior epigastric vessels
Explanation:
The corona mortis ('crown of death') is a vascular anastomosis between the obturator system (internal iliac) and the external iliac or inferior epigastric system. It typically crosses the superior pubic ramus at an average distance of 5-6 cm from the pubic symphysis. Injury during ilioinguinal or Stoppa approaches can lead to significant, difficult-to-control hemorrhage.
Question 2:
A 32-year-old male sustains a high-energy Pauwels Type III femoral neck fracture. Biomechanically, which of the following internal fixation constructs provides the greatest stability and is most appropriate to counteract the predominant deforming forces in this specific fracture pattern?
Options:
- Three parallel cancellous screws placed in an inverted triangle configuration
- A fixed-angle construct such as a sliding hip screw (DHS) with an anti-rotation screw
- A cephalomedullary nail without a supplementary anti-rotation screw
- Two parallel cancellous screws placed superiorly and inferiorly
- A laterally based proximal femoral locking plate alone
Correct Answer: A fixed-angle construct such as a sliding hip screw (DHS) with an anti-rotation screw
Explanation:
Pauwels Type III fractures are characterized by a vertical fracture line (angle > 50 degrees), which subjects the fracture to high shear forces and varus instability. Multiple biomechanical and clinical studies have demonstrated that a fixed-angle construct (such as a sliding hip screw) with a supplementary anti-rotation screw provides superior resistance to shear and varus collapse compared to multiple cancellous screws, reducing the risk of nonunion and hardware failure in young patients.
Question 3:
A 28-year-old polytrauma patient is intubated in the ICU following a high-speed motorcycle collision. He has a comminuted closed tibia fracture. The nursing staff reports a tight, swollen calf. Which of the following intracompartmental pressure measurements is widely accepted as an absolute indication for emergent four-compartment fasciotomy?
Options:
- An absolute compartment pressure greater than 20 mmHg
- A delta pressure (Mean Arterial Pressure minus Compartment Pressure) less than 40 mmHg
- A delta pressure (Diastolic Blood Pressure minus Compartment Pressure) less than 30 mmHg
- A delta pressure (Systolic Blood Pressure minus Compartment Pressure) less than 50 mmHg
- An absolute compartment pressure greater than 25 mmHg
Correct Answer: A delta pressure (Diastolic Blood Pressure minus Compartment Pressure) less than 30 mmHg
Explanation:
The diagnosis of acute compartment syndrome in an obtunded or intubated patient relies on objective pressure measurements. The 'delta pressure' concept is standard, defined as Diastolic Blood Pressure (DBP) minus intracompartmental pressure. A delta pressure of less than 30 mmHg (meaning the compartment pressure is within 30 mmHg of the diastolic pressure) is the widely accepted threshold indicating inadequate tissue perfusion and the need for emergent fasciotomy.
Question 4:
A 40-year-old male presents with a Gustilo-Anderson Type IIIB open fracture of the tibia midshaft. After initial adequate surgical debridement and stabilization, plastic surgery is consulted for a free tissue transfer. According to classic and contemporary literature, what is the optimal timing for definitive soft tissue coverage to minimize deep infection rates?
Options:
- Within 24 hours of injury, immediately after the first debridement
- Between 3 and 5 days, allowing for a second-look debridement and prior to peak bacterial colonization
- Between 10 and 14 days, once the zone of injury has completely demarcated
- After 3 weeks, to allow for adequate granulation tissue formation
- Timing does not affect infection rates provided broad-spectrum antibiotics are continued
Correct Answer: Between 3 and 5 days, allowing for a second-look debridement and prior to peak bacterial colonization
Explanation:
Godina's classic paper advocated for coverage within 72 hours; however, modern multidisciplinary approaches (including the LEAP study) have shown that soft tissue coverage performed within 3 to 7 days (optimally before 5-7 days) provides the lowest risk of deep infection and flap failure. Delaying coverage beyond 7 days significantly increases the risk of deep infection, while immediate coverage (< 24h) is often impractical in polytrauma and may obscure evolving necrosis.
Question 5:
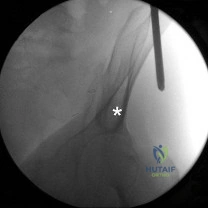
Review the clinical scenario associated with this image: A 25-year-old motorcyclist is brought to the trauma bay after being thrown into a tree. The right upper extremity is pulseless and flail. A chest radiograph demonstrates lateral displacement of the scapula with widening of the acromioclavicular and sternoclavicular joints. What is the most likely associated diagnosis?
Options:
- Isolated axillary artery intimal tear
- Scapulothoracic dissociation with massive brachial plexus and subclavian vessel avulsion
- Floating shoulder with an isolated musculocutaneous nerve injury
- Anterior shoulder dislocation with concomitant Bankart lesion
- Thoracic outlet syndrome secondary to clavicular malunion
Correct Answer: Scapulothoracic dissociation with massive brachial plexus and subclavian vessel avulsion
Explanation:
The clinical presentation (flail, pulseless arm) and radiographic finding of lateral displacement of the scapula with clavicular/sternoclavicular/acromioclavicular disruption is pathognomonic for scapulothoracic dissociation. This is essentially a 'closed forequarter amputation' and carries a devastating prognosis, almost universally associated with complete or partial brachial plexus avulsion and severe subclavian/axillary vascular injury.
Question 6:
On an anteroposterior (AP) radiograph of the pelvis in a patient with an acetabular fracture, a 'Spur sign' is identified. This radiographic finding is pathognomonic for which type of acetabular fracture according to the Judet-Letournel classification?
Options:
- T-type fracture
- Anterior column posterior hemitransverse
- Transverse with posterior wall
- Posterior column
- Both-column fracture
Correct Answer: Both-column fracture
Explanation:
The 'Spur sign' is seen on the obturator oblique view (or occasionally AP) and represents the intact portion of the ilium (the strut) that remains attached to the axial skeleton, while the entire articular surface is separated from it. This indicates a complete dissociation of the articular surface from the axial skeleton, which is the defining characteristic of a both-column acetabular fracture.
Question 7:
A 34-year-old female sustains a high-energy dorsiflexion injury to her foot. Radiographs reveal a Hawkins Type III fracture of the talar neck. Which of the following best describes the anatomical disruption in a Hawkins Type III fracture, and its associated risk of avascular necrosis (AVN)?
Options:
- Talar neck fracture with subtalar subluxation; ~50% risk of AVN
- Nondisplaced talar neck fracture; <10% risk of AVN
- Talar neck fracture with both subtalar and tibiotalar dislocation; nearly 100% risk of AVN without urgent reduction
- Talar neck fracture with subtalar, tibiotalar, and talonavicular dislocation; ~25% risk of AVN
- Fracture of the lateral process of the talus; 0% risk of AVN
Correct Answer: Talar neck fracture with both subtalar and tibiotalar dislocation; nearly 100% risk of AVN without urgent reduction
Explanation:
The Hawkins classification for talar neck fractures: Type I is nondisplaced (0-15% AVN). Type II is displaced with subtalar subluxation/dislocation (~50% AVN). Type III involves dislocation of both the subtalar and tibiotalar joints; the talar body is often extruded posteromedially. The risk of AVN in Type III approaches 80-100% due to disruption of the artery of the tarsal canal, deltoid branches, and intraosseous supply. Type IV (added by Canale) includes talonavicular subluxation/dislocation.
Question 8:
A 40-year-old male sustains a posterior knee dislocation during a football game. The dislocation is reduced in the emergency department, and distal pulses are palpable but weak. His Ankle-Brachial Index (ABI) is measured at 0.85. What is the most appropriate next step in management?
Options:
- Discharge with urgent outpatient orthopedic follow-up in 3 days
- Admit for serial clinical vascular examinations every 4 hours without further imaging
- Immediate CT angiography of the lower extremity
- Immediate transport to the operating room for prophylactic four-compartment fasciotomy
- Application of a hinged knee brace locked in 30 degrees of flexion and weight-bearing as tolerated
Correct Answer: Immediate CT angiography of the lower extremity
Explanation:
An Ankle-Brachial Index (ABI) or Arterial Pressure Index (API) less than 0.9 in the setting of a knee dislocation is highly sensitive for a significant arterial injury (popliteal artery). The standard of care mandates advanced vascular imaging (typically CT angiography) when the ABI is < 0.9, or emergent vascular surgery intervention if there are hard signs of ischemia (absent pulses, expanding hematoma, active bleeding).
Question 9:
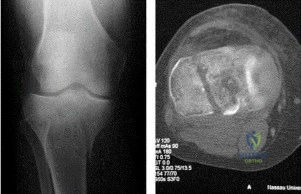
Based on the fracture pattern typically seen in the coronal plane of the distal femur (Hoffa fracture) as demonstrated in clinical practice: Which femoral condyle is most commonly involved, and what is the preferred trajectory of lag screw fixation?
Options:
- Medial condyle; anterior-to-posterior (AP) lag screws
- Lateral condyle; anterior-to-posterior (AP) lag screws
- Lateral condyle; posterior-to-anterior (PA) lag screws
- Medial condyle; posterior-to-anterior (PA) lag screws
- Both condyles equally; superior-to-inferior lag screws
Correct Answer: Lateral condyle; anterior-to-posterior (AP) lag screws
Explanation:
A Hoffa fracture (AO/OTA 33-B3) is a coronal shear fracture of the distal femur. It most commonly involves the lateral femoral condyle due to the physiologic valgus of the lower extremity and direction of ground reaction forces. Because the fracture is posterior, fixing it with anterior-to-posterior (AP) lag screws (often countersunk to avoid patellofemoral articulation) provides excellent biomechanical compression across the coronal fracture plane.
Question 10:
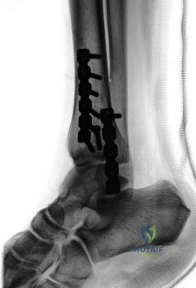
Review the following clinical indication for midfoot trauma: A 28-year-old athlete sustains a purely ligamentous Lisfranc injury. Plantar ecchymosis is present. According to prospective randomized trials comparing open reduction internal fixation (ORIF) to primary arthrodesis for purely ligamentous Lisfranc injuries, which of the following represents the primary advantage of primary arthrodesis?
Options:
- Decreased operative time and less soft tissue stripping
- Preservation of normal midfoot kinematics
- Lower rate of symptomatic hardware requiring removal and lower risk of subsequent secondary fusion
- Immediate return to weight-bearing in the postoperative period
- Higher union rates in the lateral column (4th and 5th TMT joints)
Correct Answer: Lower rate of symptomatic hardware requiring removal and lower risk of subsequent secondary fusion
Explanation:
Prospective randomized trials (e.g., Ly and Coetzee, Henning et al.) have demonstrated that for purely ligamentous Lisfranc injuries (involving the 1st, 2nd, and 3rd TMT joints), primary arthrodesis results in better functional outcomes and avoids the high rate of secondary procedures (e.g., hardware removal, late salvage arthrodesis for post-traumatic arthritis) associated with ORIF. Note: the lateral column (4th and 5th TMT) is highly mobile and should NOT be primarily fused.
Question 11:
A 50-year-old female presents with a 'Terrible Triad' injury of the elbow (coronoid fracture, radial head fracture, and elbow dislocation). During surgical reconstruction, what is the generally accepted optimal sequence of repair to restore elbow stability?
Options:
- Repair the lateral ulnar collateral ligament (LUCL), fix the radial head, fix the coronoid
- Fix the radial head, repair the medial collateral ligament (MCL), fix the coronoid
- Fix or replace the radial head, fix the coronoid, repair the LUCL
- Fix the coronoid, fix or replace the radial head, repair the LUCL
- Repair the MCL, repair the LUCL, fix the coronoid
Correct Answer: Fix the coronoid, fix or replace the radial head, repair the LUCL
Explanation:
The standard surgical algorithm for a Terrible Triad injury progresses from deep to superficial and typically from medial/anterior to lateral. The accepted sequence is: 1) Fix the coronoid (to restore the anterior buttress), 2) Fix or replace the radial head (to restore the lateral column/anterior buttress), 3) Repair the lateral collateral ligament complex (LUCL) to the lateral epicondyle. The MCL is only repaired if the elbow remains grossly unstable after these steps.
Question 12:
A 65-year-old female on long-term alendronate therapy for osteoporosis presents with atraumatic thigh pain. Radiographs demonstrate focal lateral cortical thickening of the subtrochanteric femur with a transverse radiolucent line. Which of the following is the primary pathophysiologic mechanism leading to this atypical femur fracture (AFF)?
Options:
- Excessive osteoblastic proliferation causing disorganized woven bone
- Severe suppression of targeted osteoclastic bone remodeling leading to accumulation of microdamage
- Depletion of uncarboxylated osteocalcin leading to brittle collagen cross-linking
- Spontaneous localized osteonecrosis of the lateral cortex
- Increased parathyroid hormone (PTH) activity secondary to bisphosphonate use
Correct Answer: Severe suppression of targeted osteoclastic bone remodeling leading to accumulation of microdamage
Explanation:
Bisphosphonates profoundly suppress osteoclast function and apoptosis. Prolonged use (typically > 5 years) severely impairs targeted bone remodeling. Normally, microcracks from daily stress are repaired by basic multicellular units (BMUs). Suppressed remodeling allows these microcracks to accumulate, particularly on the tensile side of the femur (lateral cortex), eventually coalescing into an atypical femur fracture.
Question 13:
When utilizing the extensile lateral approach for open reduction and internal fixation of a displaced intra-articular calcaneus fracture, full-thickness flap necrosis is a dreaded complication. The viability of this flap is primarily dependent on which of the following vascular structures?
Options:
- Medial calcaneal artery
- Dorsalis pedis artery
- Sural artery
- Lateral tarsal artery
- Lateral calcaneal artery
Correct Answer: Lateral calcaneal artery
Explanation:
The extensile lateral approach creates a full-thickness fasciocutaneous flap. Its blood supply is highly reliant on the lateral calcaneal artery, which is a terminal branch of the peroneal artery. Careful tissue handling, avoiding 'no-touch' retractor techniques (using K-wires into the talus and fibula instead), and making subperiosteal full-thickness cuts are critical to prevent corner necrosis.
Question 14:
A 22-year-old male presents after a diving accident. Cervical spine imaging reveals a traumatic spondylolisthesis of the axis (Hangman's fracture). The fracture demonstrates severe angulation but minimal translation, consistent with a Levine-Edwards Type IIA injury. Which of the following interventions is strictly CONTRAINDICATED in the acute management of this specific fracture pattern?
Options:
- Application of cervical traction
- Placement in a rigid cervical collar
- Application of a Halo vest with slight compression
- Surgical fixation using C2 pars screws
- Surgical fixation using a C2-C3 anterior cervical discectomy and fusion
Correct Answer: Application of cervical traction
Explanation:
The Levine-Edwards Type IIA Hangman's fracture is caused by flexion-distraction forces. It is characterized by severe angulation with minimal translation. Because the mechanism involves distraction and injury to the posterior longitudinal ligament and C2-C3 disc, the application of cervical traction is strictly contraindicated as it will exacerbate the deformity and over-distract the spine. Treatment is typically a Halo vest applied with slight extension and compression.
Question 15:
A 26-year-old male sustains a low-velocity civilian gunshot wound to the thigh, resulting in a comminuted midshaft femur fracture. The bullet passed cleanly through the thigh, leaving small entrance and exit wounds without gross contamination. Distal pulses are intact, and there is no expanding hematoma. What is the most appropriate initial management of the soft tissues and fracture?
Options:
- Immediate formal operative debridement of the entire bullet tract followed by external fixation
- Pulsatile lavage of the wounds in the emergency department and conservative management in a cast
- Emergent exploration of the femoral artery due to the high kinetic energy of the bullet
- Local wound care, intravenous antibiotics for 24-48 hours, and antegrade intramedullary nailing without formal tract debridement
- Surgical excision of the entrance and exit wounds with immediate primary closure and plating
Correct Answer: Local wound care, intravenous antibiotics for 24-48 hours, and antegrade intramedullary nailing without formal tract debridement
Explanation:
Low-velocity civilian gunshot wounds with associated long bone fractures behave similarly to Gustilo Type I open fractures. Unless there is gross contamination (e.g., shotgun wadding, bowel involvement), vascular injury, or intra-articular extension, formal operative debridement of the bullet tract is unnecessary. Standard care involves superficial local wound cleansing, short-course IV antibiotics (typically a first-generation cephalosporin), and definitive fixation (e.g., IM nailing).
Question 16:
A 45-year-old female sustains a 'floating shoulder' following a motor vehicle collision. Which of the following combinations of specific injury characteristics (Goss's criteria) most strongly indicates the need for operative fixation?
Options:
- Any displacement of the clavicle regardless of the scapular neck position
- A non-displaced clavicle fracture with 5 mm of scapular neck translation
- Medialization (translation) of the glenoid fragment > 10 mm or angulation > 40 degrees
- Concomitant fracture of the acromion without clavicular displacement
- An associated nondisplaced rib fracture
Correct Answer: Medialization (translation) of the glenoid fragment > 10 mm or angulation > 40 degrees
Explanation:
A 'floating shoulder' typically involves ipsilateral fractures of the clavicular shaft and the scapular neck. Nonoperative management is successful for minimally displaced injuries. However, surgical intervention (usually fixing the clavicle first, which often indirectly reduces the scapula) is indicated based on Goss's criteria/Bartoníček's criteria: scapular neck translation > 1 cm (10 mm) or angulation > 40 degrees, as these lead to altered glenohumeral mechanics and poor functional outcomes.
Question 17:
A 55-year-old female sustains a complex intra-articular fracture of the distal radius. Preoperative CT reveals a small, displaced volar ulnar corner (lunate facet) fragment. Why is fragment-specific fixation of this specific piece considered critical?
Options:
- Failure to fix it leads to attritional rupture of the flexor pollicis longus (FPL) tendon
- The fragment acts as an essential buttress; failure to fix it leads to volar subluxation of the radiocarpal joint (carpus)
- It is the primary attachment site of the triangular fibrocartilage complex (TFCC) foveal fibers
- Failure to fix it prevents pronation and supination due to distal radioulnar joint (DRUJ) block
- It contains the vascular supply to the lunate, risking Kienbock's disease if left displaced
Correct Answer: The fragment acts as an essential buttress; failure to fix it leads to volar subluxation of the radiocarpal joint (carpus)
Explanation:
The volar ulnar corner of the distal radius (volar lunate facet) contains the attachments of the stout volar radiocarpal ligaments (short radiolunate ligament). This fragment is often small and can easily 'escape' standard volar locking plates. If it is not anatomically reduced and stably fixed (e.g., with a fragment-specific hook plate or wire), the carpus will subluxate volarly with the fragment, leading to catastrophic joint failure and arthritis.
Question 18:
In the acute trauma bay: A hemodynamically unstable patient with an Anteroposterior Compression Type III (APC-III) pelvic ring injury is receiving a circumferential pelvic binder. To be maximally effective in reducing pelvic volume and controlling hemorrhage without causing paradoxical widening, where must the binder be centered?
Options:
- Over the greater trochanters
- Over the iliac crests
- At the level of the umbilicus
- Directly over the anterior superior iliac spines (ASIS)
- Mid-thigh bilaterally
Correct Answer: Over the greater trochanters
Explanation:
A common and potentially fatal error in trauma management is placing a pelvic binder too high. If placed over the iliac crests, it can cause the iliac wings to act as a fulcrum, paradoxically widening the true pelvis and exacerbating hemorrhage. The binder must be centered exactly over the greater trochanters of the femur to directly close the pubic symphysis and reduce the pelvic volume.
Question 19:
A 25-year-old male is brought to the trauma center after a high-speed MVC. He has bilateral femur fractures, blunt chest trauma, and a closed head injury. The decision between Early Total Care (ETC, immediate intramedullary nailing) and Damage Control Orthopedics (DCO, external fixation) is being made. Which of the following physiologic parameters is the best indicator that the patient is adequately resuscitated and may safely undergo ETC?
Options:
- Core body temperature of 34.5°C
- Platelet count of 75,000/mcL
- Arterial pH of 7.15
- Serum lactate < 2.5 mmol/L with a normalizing base deficit
- Systolic blood pressure transiently responding to 2 liters of crystalloid
Correct Answer: Serum lactate < 2.5 mmol/L with a normalizing base deficit
Explanation:
Damage Control Orthopedics (DCO) is indicated for patients who are hemodynamically unstable, in extremis, or 'borderline'. The lethal triad includes acidosis, hypothermia, and coagulopathy. Indicators of adequate resuscitation permitting Early Total Care (ETC) include a serum lactate < 2.5 mmol/L (often < 2.0 is preferred), a base deficit normalizing to > -2, normal coagulation parameters, and normothermia. Options A, B, and C reflect a severely deranged physiologic state mandating DCO.
Question 20:
A 45-year-old male sustains a high-energy Schatzker Type IV tibial plateau fracture (medial plateau involvement). A coronal CT scan demonstrates a large posteromedial fracture fragment. What is the optimal surgical approach and internal fixation strategy for this specific fragment?
Options:
- Anterolateral approach with a laterally based locking plate to 'raft' the medial side
- Posteromedial approach with an under-contoured anti-glide plate applied to the posteromedial cortex
- Direct medial approach utilizing multiple AP lag screws without a plate
- Midline anterior approach with a dual-plate construct applied over the tibial tubercle
- Arthroscopically-assisted percutaneous screw fixation from anterior to posterior
Correct Answer: Posteromedial approach with an under-contoured anti-glide plate applied to the posteromedial cortex
Explanation:
Schatzker IV fractures (medial plateau) frequently possess a significant posteromedial fragment with a vertical coronal split, driven by a varus/extension or axial load. This fragment tends to displace distally and posteriorly. Laterally based locking screws cannot effectively capture or buttress this fragment. The optimal biomechanical solution is a posteromedial approach with a buttress (or anti-glide) plate applied directly to the apex of the posteromedial fragment.
Question 21:
A 28-year-old male is brought to the trauma bay after a high-speed motorcycle collision. He has bilateral closed femoral shaft fractures, a pulmonary contusion, and a closed head injury. His blood pressure is 95/60 mmHg, heart rate is 115 bpm, and his initial serum lactate is 3.5 mmol/L. According to the Hannover/Pape criteria for Damage Control Orthopedics (DCO) versus Early Total Care (ETC), which of the following is the most appropriate initial management for his femoral fractures?
Options:
- Immediate bilateral reamed intramedullary nailing
- Immediate bilateral unreamed intramedullary nailing
- Bilateral spanning external fixation
- Open reduction and internal fixation with compression plating
- Skeletal traction until day 5, followed by intramedullary nailing
Correct Answer: Bilateral spanning external fixation
Explanation:
This patient fits the criteria for a 'borderline' or 'unstable' polytrauma patient. An initial lactate > 2.5 mmol/L, base excess < -4, concurrent severe chest trauma, and bilateral femur fractures place him at high risk for a "second hit" phenomenon (such as ARDS or multiorgan failure) if subjected to prolonged surgery like bilateral intramedullary nailing. Damage Control Orthopedics (DCO), which involves rapid stabilization with bilateral external fixation, is the gold standard here to minimize the systemic inflammatory response while waiting for physiologic stabilization.
Question 22:
During the anterior surgical approach (ilioinguinal or modified Stoppa) for an anterior column acetabulum fracture, massive hemorrhage is encountered when dissecting near the superior pubic ramus. Which of the following best describes the most likely source of this bleeding?
Options:
- Anastomosis between the external iliac artery and the obturator artery
- Anastomosis between the internal iliac artery and the superior gluteal artery
- Laceration of the deep circumflex iliac artery
- Avulsion of the internal pudendal artery
- Laceration of the inferior mesenteric artery
Correct Answer: Anastomosis between the external iliac artery and the obturator artery
Explanation:
The 'corona mortis' (crown of death) is a vascular anastomosis between the external iliac (or deep inferior epigastric) and the obturator vessels (which branch from the internal iliac system). It traverses over the superior pubic ramus and is highly susceptible to injury during anterior approaches to the pelvis and acetabulum (such as the ilioinguinal or Stoppa approaches), potentially causing massive, difficult-to-control hemorrhage.
Question 23:
A 45-year-old female presents with a complex bicondylar tibial plateau fracture after a fall from a height. The surgeon plans a dual-incision approach, utilizing a standard anterolateral approach and a posteromedial approach. When dissecting through the posteromedial interval to apply a buttress plate, which of the following structures is at the greatest risk of iatrogenic injury if the dissection strays too superficial and anterior?
Options:
- Common peroneal nerve
- Tibial nerve
- Saphenous nerve
- Popliteal artery
- Sural nerve
Correct Answer: Saphenous nerve
Explanation:
The posteromedial approach to the tibial plateau typically utilizes the interval between the medial head of the gastrocnemius (posterior) and the pes anserinus (anterior). The saphenous nerve and the greater saphenous vein run superficial to the pes anserinus and are at risk if the incision or superficial dissection is carried too far anteriorly or carelessly retracted. The common peroneal nerve is lateral, and the popliteal bundle/tibial nerve is central/posterior and protected by the gastrocnemius.
Question 24:
A 32-year-old female sustains a distal femur fracture. Radiographs show a coronal plane fracture of the lateral femoral condyle (Hoffa fracture). Which of the following anatomical structures primarily remains attached to this osteochondral fragment, leading to characteristic posterior and proximal displacement?
Options:
- Anterior cruciate ligament and lateral head of the gastrocnemius
- Popliteus tendon and lateral collateral ligament
- Medial collateral ligament and medial head of the gastrocnemius
- Biceps femoris and iliotibial band
- Posterior cruciate ligament and plantaris
Correct Answer: Popliteus tendon and lateral collateral ligament
Explanation:
A Hoffa fracture is a coronal shear fracture of the distal femoral condyle, most commonly involving the lateral condyle. The lateral condylar fragment typically displaces proximally and posteriorly due to the pull of the structures attached to it, primarily the lateral head of the gastrocnemius, the popliteus tendon, and the lateral collateral ligament (LCL).
Question 25:
Review the radiograph of a hemodynamically unstable trauma patient. The patient has an Anteroposterior Compression (APC) type injury to the pelvic ring. Disruption of which of the following structures differentiates a rotationally unstable but vertically stable APC II injury from a globally unstable APC III injury?
Options:
- Symphysis pubis
- Anterior sacroiliac ligaments
- Sacrospinous ligaments
- Posterior sacroiliac ligaments
- Iliolumbar ligaments
Correct Answer: Posterior sacroiliac ligaments
Explanation:
In the Young-Burgess classification, an APC II injury involves disruption of the symphysis pubis, the anterior sacroiliac (SI) ligaments, and the sacrotuberous/sacrospinous ligaments, leading to rotational instability but preserving vertical stability because the strong posterior SI ligaments are intact. An APC III injury implies complete disruption of both the anterior and posterior SI ligaments, leading to both rotational and vertical instability.
Question 26:
A 26-year-old male sustains a Hawkins Type III fracture of the talar neck. In this injury, the talar body extrudes from both the subtalar and tibiotalar joints. In which direction is the extruded talar body most commonly displaced, and which structure is primarily at risk of being tethered or injured?
Options:
- Anterolaterally; superficial peroneal nerve
- Anteromedially; anterior tibial artery
- Posteromedially; posterior tibial neurovascular bundle
- Posterolaterally; sural nerve
- Directly posteriorly; Achilles tendon
Correct Answer: Posteromedially; posterior tibial neurovascular bundle
Explanation:
In a Hawkins Type III talar neck fracture, the body of the talus dislocates from both the subtalar and the tibiotalar joints. It typically extrudes posteromedially, wrapping around the medial malleolus. This displacement places the posterior tibial neurovascular bundle at immense risk of stretching, tethering, or direct laceration, necessitating an urgent closed or open reduction.
Question 27:
According to the findings of the Lower Extremity Assessment Project (LEAP) study regarding severe lower extremity trauma (Gustilo IIIB/IIIC injuries), which of the following variables was found to be the most significant predictor of poor functional outcome at 2 years post-injury?
Options:
- Decision to amputate versus attempt limb salvage
- Presence of an insensate plantar surface at initial presentation
- Poor patient psychosocial and economic status
- Use of a free tissue transfer versus a rotational flap
- Initial wound size greater than 10 centimeters
Correct Answer: Poor patient psychosocial and economic status
Explanation:
The LEAP study was a landmark prospective trial comparing amputation versus limb salvage in severe lower extremity trauma. It concluded that at 2 years, there was no significant difference in functional outcomes between the two groups. The most significant predictors of poor functional outcomes were not injury-specific or treatment-specific variables, but rather patient-related socioeconomic and psychosocial factors (e.g., lack of insurance, low education level, smoking, lack of social support).
Question 28:
A 50-year-old male requires open reduction and internal fixation of a Sanders Type III calcaneus fracture via a standard extensile lateral approach. To minimize the risk of the most common complication associated with this surgical approach, the surgeon must ensure full-thickness flap elevation. Which artery provides the primary blood supply to the corner of this L-shaped flap?
Options:
- Anterior lateral malleolar artery
- Lateral calcaneal artery
- Medial calcaneal artery
- Dorsalis pedis artery
- Lateral plantar artery
Correct Answer: Lateral calcaneal artery
Explanation:
The standard extensile lateral approach to the calcaneus creates an L-shaped flap. Wound edge necrosis and dehiscence at the apex (corner) of this flap is the most common complication. The primary blood supply to this full-thickness flap, specifically the corner, is the lateral calcaneal artery, which is a terminal branch of the peroneal artery. The dissection must be strictly subperiosteal to preserve this vascular supply.
Question 29:
A 40-year-old intoxicated male is found down after an unknown period and is brought to the emergency department. He has severe swelling of his right lower leg, which is cold, pulseless, and completely insensate. Passive stretch elicits no pain, and there is no active motion. Compartment pressures measure 65 mmHg, and his diastolic blood pressure is 80 mmHg. The exact time of injury is unknown but is estimated to be over 48 hours ago. What is the most appropriate management?
Options:
- Immediate four-compartment fasciotomy
- Immediate single-incision fasciotomy
- Administration of IV mannitol and observation
- Nonoperative management, allowing the leg to contracture
- Hyperbaric oxygen therapy followed by delayed fasciotomy
Correct Answer: Nonoperative management, allowing the leg to contracture
Explanation:
This patient presents with a 'missed' or late-presenting compartment syndrome (>24-48 hours) where the muscle is already dead (indicated by pulseless, insensate limb with no stretch pain and lack of active motion). Performing a fasciotomy in this setting is contraindicated due to a highly prohibitive risk of introducing infection into necrotic tissue, which frequently leads to severe sepsis and death. The standard of care is nonoperative management, allowing the leg to fibrose and form a contracture, or an amputation if it becomes infected or for definitive functional management later.
Question 30:
In the treatment of a displaced, vertically oriented (Pauwels Type III) femoral neck fracture in a 25-year-old patient, a sliding hip screw (SHS) with a derotational screw is often preferred over three parallel cancellous lag screws. What is the primary biomechanical advantage of the SHS construct in this specific fracture pattern?
Options:
- Increased resistance to vertical shear forces
- Greater preservation of the lateral epiphyseal artery
- Prevention of femoral head avascular necrosis
- Enhanced compression along the axis of the femoral neck
- Reduced risk of intra-articular screw penetration
Correct Answer: Increased resistance to vertical shear forces
Explanation:
Pauwels Type III femoral neck fractures are characterized by a highly vertical fracture line (angle > 50 degrees to the horizontal). This vertical orientation subjects the fracture to immense vertical shear forces rather than compressive forces. A fixed-angle construct, such as a sliding hip screw (often supplemented with an anti-rotation screw), provides superior biomechanical resistance to these vertical shear forces compared to multiple parallel cancellous screws, reducing the risk of varus collapse and nonunion.
Question 31:
A 35-year-old right-hand-dominant male presents with a closed distal-third spiral fracture of the humeral shaft (Holstein-Lewis type) following an arm-wrestling match. On examination, he is unable to actively extend his wrist or digits, though his triceps function is intact. His pulses are palpable. What is the most appropriate initial management?
Options:
- Immediate surgical exploration of the radial nerve and ORIF
- Application of a coaptation splint and observation of the nerve palsy
- Electromyography (EMG) to determine the extent of nerve injury before treatment
- Immediate external fixation to stabilize the nerve environment
- Closed reduction with immediate intraoperative nerve exploration if reduction fails
Correct Answer: Application of a coaptation splint and observation of the nerve palsy
Explanation:
A primary radial nerve palsy associated with a closed humeral shaft fracture (even a Holstein-Lewis distal third fracture) is generally treated conservatively with a coaptation splint or functional brace and observation. Over 70-80% of these palsies represent neurapraxia and will recover spontaneously. Immediate exploration is indicated for open fractures, penetrating trauma, vascular compromise, or a secondary nerve palsy that develops *after* a closed reduction attempt.
Question 32:
A 45-year-old female sustains a volar Barton's fracture of the distal radius. During the injury, the carpus subluxates volarly in conjunction with the distal radius fracture fragment. Which of the following volar extrinsic radiocarpal ligaments is primarily responsible for pulling the carpus volarly with the fractured fragment?
Options:
- Radioscaphocapitate and short radiolunate ligaments
- Long radiolunate and radioscapholunate ligaments
- Ulnolunate and ulnotriquetral ligaments
- Volar radioulnar ligament
- Dorsal radiocarpal ligament
Correct Answer: Radioscaphocapitate and short radiolunate ligaments
Explanation:
A volar Barton's fracture is a fracture-dislocation where the volar rim of the distal radius shears off, and the carpus translates volarly with it. The carpus follows the volar rim fragment because the stout volar extrinsic ligaments—specifically the radioscaphocapitate (RSC) and the short radiolunate (SRL) ligaments—remain firmly attached to this volar bony fragment.
Question 33:
A 68-year-old female sustains a Dubberley Type 3B fracture of the capitellum (a coronal shear fracture involving the capitellum and trochlea with posterior condylar comminution). If the surgeon elects to perform an Open Reduction and Internal Fixation (ORIF) via an extensile lateral approach (Kocher interval), between which two muscles is the dissection carried out?
Options:
- Brachioradialis and Extensor Carpi Radialis Longus
- Extensor Carpi Radialis Brevis and Extensor Digitorum Communis
- Extensor Digitorum Communis and Extensor Carpi Ulnaris
- Anconeus and Extensor Carpi Ulnaris
- Triceps and Anconeus
Correct Answer: Anconeus and Extensor Carpi Ulnaris
Explanation:
The Kocher approach to the lateral elbow utilizes the internervous plane between the Extensor Carpi Ulnaris (ECU, innervated by the posterior interosseous nerve) and the Anconeus (innervated by the radial nerve). This provides excellent access to the capitellum and lateral joint space for addressing coronal shear fractures.
Question 34:
A 72-year-old female with a history of a cementless total hip arthroplasty presents with thigh pain after a ground-level fall. Radiographs show a periprosthetic femur fracture that occurs around the stem, extending just distal to its tip. The femoral stem is noted to be clinically loose, but the bone stock surrounding the proximal femur is robust and adequate. According to the Vancouver classification, what is the injury type and the most appropriate standard surgical treatment?
Options:
- Vancouver A; Nonoperative management with protected weight-bearing
- Vancouver B1; Open reduction and internal fixation with a locking plate
- Vancouver B2; Revision arthroplasty with a long-stem femoral component
- Vancouver B3; Revision arthroplasty with proximal femoral replacement
- Vancouver C; Open reduction and internal fixation with a locking plate
Correct Answer: Vancouver B2; Revision arthroplasty with a long-stem femoral component
Explanation:
This is a Vancouver B2 periprosthetic fracture. The fracture occurs around or just below the stem (Type B), the stem is loose (sub-type 2), but the proximal bone stock is adequate (differentiating it from B3, which has poor bone stock). The standard of care for a Vancouver B2 fracture is revision of the femoral component to a long-stem prosthesis (usually cementless, fully porous-coated, or fluted tapered) that bypasses the fracture by at least two cortical diameters.
Question 35:
A 22-year-old collegiate football player sustains a pure ligamentous Lisfranc injury. Weight-bearing radiographs demonstrate 4 mm of diastasis between the medial cuneiform and the base of the second metatarsal. Current orthopedic literature suggests which of the following treatments provides the lowest rate of hardware removal and highest long-term functional scores for this specific injury pattern?
Options:
- Closed reduction and percutaneous pinning
- Open reduction and internal fixation with transarticular screws
- Primary arthrodesis of the medial 1st, 2nd, and 3rd tarsometatarsal joints
- Primary arthrodesis of the 4th and 5th tarsometatarsal joints
- Non-weight bearing cast immobilization for 8 weeks
Correct Answer: Primary arthrodesis of the medial 1st, 2nd, and 3rd tarsometatarsal joints
Explanation:
For purely ligamentous Lisfranc injuries, multiple randomized controlled trials (e.g., Ly and Coetzee) have demonstrated that primary arthrodesis of the medial column (1st, 2nd, and 3rd TMT joints) yields better functional outcomes, less chronic pain, and lower reoperation rates compared to ORIF. ORIF is generally preferred for purely bony Lisfranc fractures where anatomic reduction of articular surfaces can heal predictably.
Question 36:
A 6-year-old boy falls off monkey bars and presents with a swollen, deformed forearm. Radiographs reveal a fracture of the proximal third of the ulna with an anterior dislocation of the radial head. According to the Bado classification, what type of Monteggia lesion is this, and what is the presumed mechanism of injury?
Options:
- Bado Type I; Forced pronation of the forearm
- Bado Type II; Axial loading with a flexed elbow
- Bado Type III; Varus stress to the elbow
- Bado Type IV; Direct blow to the radius
- Bado Type I; Forced supination of the forearm
Correct Answer: Bado Type I; Forced pronation of the forearm
Explanation:
A proximal ulna fracture with an anterior dislocation of the radial head is a Bado Type I Monteggia fracture. It is the most common type, particularly in children. The accepted mechanism of injury is a fall on an outstretched hand with forced pronation of the forearm, causing the radial head to dislocate anteriorly while the ulna fractures and apexes anteriorly.
Question 37:
A 28-year-old male is brought to the trauma bay after a high-velocity knee dislocation. His knee was reduced in the field. On physical examination, his dorsalis pedis and posterior tibial pulses are present but diminished compared to the contralateral leg. His Ankle-Brachial Index (ABI) is calculated to be 0.85. There is no expanding hematoma or pulsatile bleeding. What is the most appropriate next step in his vascular workup?
Options:
- Immediate surgical exploration of the popliteal artery
- Discharge with instructions to return if the foot becomes cold
- Computed Tomography (CT) Angiogram of the lower extremity
- Application of a spanning external fixator, ignoring the ABI
- Compartment pressure measurement
Correct Answer: Computed Tomography (CT) Angiogram of the lower extremity
Explanation:
In the setting of a knee dislocation, vascular injury (to the popliteal artery) is a major concern. 'Hard signs' of vascular injury (pulsatile bleeding, expanding hematoma, absent pulses, cold/ischemic limb) warrant immediate surgical exploration. 'Soft signs' or an asymmetric ABI < 0.9 (as seen in this patient with an ABI of 0.85 and diminished pulses) warrant further advanced imaging, with CT Angiography being the gold standard to evaluate for an intimal flap or non-occlusive injury.
Question 38:
A 40-year-old construction worker falls 15 feet, sustaining a severe, comminuted, high-energy tibial pilon fracture with massive soft tissue swelling. A staged protocol is chosen. A spanning external fixator is placed on day 1. Which of the following is the most reliable clinical indicator that the soft tissues are ready for definitive open reduction and internal fixation?
Options:
- Resolution of all ecchymosis
- Return of the ankle-brachial index to > 1.0
- Appearance of skin wrinkling around the ankle
- Normalization of C-reactive protein (CRP) levels
- A minimum of 21 days since the initial injury
Correct Answer: Appearance of skin wrinkling around the ankle
Explanation:
In the staged management of high-energy pilon fractures, definitive ORIF must be delayed until the soft tissue envelope has recovered sufficiently to allow safe surgical incisions and closure without necrosis or wound breakdown. The appearance of skin wrinkles (the 'wrinkle sign') over the anterior ankle and fracture site is the most reliable clinical indicator that the acute edema has subsided enough to proceed safely with ORIF.
Question 39:
Following open reduction and internal fixation of a rotational ankle fracture with syndesmotic instability, intraoperative fluoroscopy is used to assess the reduction of the distal tibiofibular joint. However, postoperative CT imaging frequently identifies malreduction even when radiographs appear acceptable. In which plane does syndesmotic malreduction most commonly occur?
Options:
- Coronal plane (proximal/distal translation)
- Sagittal plane (anterior/posterior translation)
- Axial plane (internal/external rotation of the tibia)
- Transverse plane (medial/lateral shift of the talus)
- Oblique plane (varus/valgus angulation)
Correct Answer: Sagittal plane (anterior/posterior translation)
Explanation:
Studies utilizing postoperative CT scans have shown that syndesmotic malreduction following clamp application and screw fixation occurs in up to 30-50% of cases when assessed only by plain radiography. The most common direction of malreduction is in the sagittal plane, specifically anterior or posterior translation of the fibula relative to the tibial incisura, often caused by the vectors of the reduction clamp.
Question 40:
A 19-year-old male suffers a gunshot wound to the right knee. Radiographs reveal a retained bullet lying entirely within the intra-articular space of the knee. The patient has no other systemic injuries, and the soft tissue wounds are small and clean. Which of the following is an absolute indication for the surgical retrieval of this bullet?
Options:
- Prevention of systemic lead toxicity and lead arthropathy
- Prevention of acute septic arthritis caused by the heat of the bullet
- High risk of migration into the popliteal artery
- Prevention of foreign-body induced osteosarcoma
- Improvement of the MRI compatibility of the limb
Correct Answer: Prevention of systemic lead toxicity and lead arthropathy
Explanation:
A retained bullet within an intra-articular space (especially synovial joints like the knee or hip) is an absolute indication for surgical removal. Synovial fluid breaks down the lead bullet, which can lead to rapid, destructive mechanical joint wear (lead arthropathy) and systemic lead absorption causing systemic lead toxicity (plumbism). Acute septic arthritis is less directly correlated with the heat (bullets are actually sterilized by heat to some degree but carry skin flora in). Migration and malignancy are not the primary driving reasons.