Thumb Metacarpal Extension Osteotomy
Introduction and Epidemiology
Thumb carpometacarpal (CMC) or trapeziometacarpal joint arthritis represents a ubiquitous and profoundly debilitating orthopaedic pathology, demonstrating a high prevalence among postmenopausal women and individuals with a history of repetitive manual labor. The natural history of basal joint arthritis often begins with ligamentous attenuation, specifically of the anterior oblique ligament complex. When this primary restraint at the thumb carpometacarpal joint is compromised, functional pinch and grip mechanics generate pathologic shear forces. This results in painful synovitis and dynamic hypermobility long before the manifestation of macroscopic cartilage wear and frank osteoarthritis.
This early clinical presentation, classically defined as Eaton-Littler Stage I disease, poses a unique therapeutic dilemma. At this juncture, the articular cartilage remains largely pristine, yet the joint is highly symptomatic due to dynamic instability and focal capsular overloading at the palmar aspect of the articulation. Historically, the management algorithm for early-stage trapeziometacarpal instability relied heavily on conservative modalities, eventually progressing to soft tissue stabilization procedures such as ligament reconstruction with tendon interposition (LRTI) or arthroscopic synovectomy with temporary pinning.
However, the thumb metacarpal extension osteotomy has emerged as a highly effective, joint-preserving, extra-articular alternative. By fundamentally altering the biomechanical force vectors across the trapeziometacarpal joint, a closing-wedge extension osteotomy at the base of the thumb metacarpal dynamically redirects compressive loads away from the vulnerable palmar compartment. This mechanical shift mitigates painful synovitis, stabilizes the joint via dorsal capsuloligamentous tensioning, and has been shown to potentially halt or significantly delay the progression of degenerative articular changes.
The epidemiological profile of trapeziometacarpal joint laxity and subsequent arthrosis demonstrates a strong predilection for the female demographic, with an incidence ratio of approximately six to one compared to their male counterparts. The onset of symptomatic hypermobility typically occurs in the fourth to fifth decades of life. This laxity is frequently exacerbated by occupational or recreational activities requiring repetitive forceful opposition or sustained lateral pinch. Recognizing this condition in its nascent stages is paramount; the clinical efficacy of an extra-articular extension osteotomy is strictly contingent upon the preservation of articular cartilage, particularly within the dorsal aspect of the trapeziometacarpal articulation.
Surgical Anatomy and Biomechanics
Osteology of the Trapeziometacarpal Joint
The trapeziometacarpal joint is a highly specialized, biconcave-convex saddle joint. This unique geometric configuration permits a wide, multi-planar range of motion encompassing flexion, extension, palmar and radial abduction, adduction, and the complex composite kinematic motion of opposition. However, this extensive mobility comes at the direct expense of intrinsic osseous stability. The joint relies minimally on bony constraints, making the surrounding ligamentous envelope critically important for maintaining congruence.
This is particularly relevant when considering the profound joint reaction forces transmitted across the articulation during functional pinch. Biomechanical models have consistently demonstrated a multiplier effect: a simple tip or key pinch can generate compressive loads at the trapeziometacarpal joint that are up to twelve times the applied force at the fingertips, subjecting the relatively small articular surface area to immense mechanical stress.
Ligamentous Anatomy and Stabilizers
In their comprehensive anatomical and biomechanical assessment of the trapeziometacarpal joint, Bettinger et al. described a complex network of sixteen distinct ligaments stabilizing the trapezium and the thumb metacarpal. Seven of these capsuloligamentous structures are responsible for directly stabilizing the trapeziometacarpal joint: the superficial anterior oblique ligament, the deep anterior oblique ligament, the dorsoradial ligament, the posterior oblique ligament, the ulnar collateral ligament, the intermetacarpal ligament, and the dorsal intermetacarpal ligament.
Eaton and Littler originally identified the anterior oblique ligament, frequently referred to as the "beak" ligament due to its robust insertion on the palmar beak of the thumb metacarpal base, as the primary stabilizer of the joint. With the advent of advanced micro-anatomical dissection and trapeziometacarpal joint arthroscopy, subsequent investigations have delineated the anterior oblique ligament into distinct superficial and deep components. The deep anterior oblique ligament is intracapsular and represents the true beak ligament. It plays an indispensable role in the kinematics of thumb opposition, acting as a pivotal fulcrum that becomes taut during pronation, opposition, and palmar abduction. Furthermore, it limits pronation in flexion and restricts both pronation and supination in extension.

The role of the dorsoradial ligament in joint stability was historically a subject of debate. However, contemporary biomechanical analyses have unequivocally established it as a critical primary stabilizer, arguably as important as the anterior oblique ligament. Covering a large percentage of the posterior aspect of the joint capsule, the dorsoradial ligament is a wide, thick, and robust structure originating on the dorsal tubercle of the trapezium and inserting onto the dorsum of the metacarpal base. This ligament tightens in response to dorsal translational forces in all positions except full extension. It also exhibits increased tension during supination and during pronation combined with joint flexion.
Pathomechanics of Basal Joint Arthritis
Functional incompetence of the basal joint's anterior oblique ligament results in pathologic laxity and abnormal dorsal translation of the metacarpal base upon the trapezium. This subluxation generates excessive shear forces between the incongruent joint surfaces, particularly within the palmar portion of the joint during grip and pinch activities. Histological and intraoperative studies have demonstrated that attritional changes in the anterior oblique ligament at its attachment to the palmar lip of the metacarpal consistently precede the macroscopic degeneration of articular cartilage.
Because the anterior oblique ligament is a primary stabilizer and its attenuation results in dorsal translation of the metacarpal, its anatomical reconstruction was traditionally recommended to restore thumb stability. However, Pellegrini et al. evaluated the biomechanical efficacy of an extra-articular extension osteotomy as a viable alternative. Their seminal work demonstrated that a closing-wedge extension osteotomy effectively unloads the palmar contact area, creating a concomitant shift in articular contact stresses toward the more dorsal aspect of the joint. This load-shifting mechanism is highly effective provided that arthrosis does not extend dorsally beyond the midpoint of the trapezium.
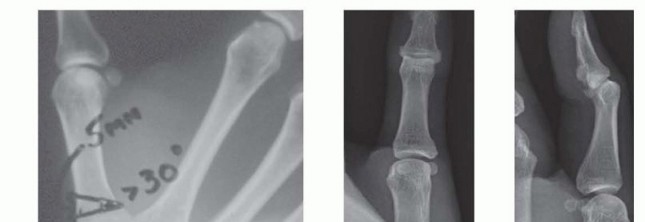
Shrivastava et al. further elucidated the biomechanical rationale by studying the effect of a simulated osteotomy on trapeziometacarpal joint laxity. By flexing the metacarpal base thirty degrees relative to the metacarpal shaft, the osteotomy places the joint in a spatial relationship that inherently tightens the dorsal capsule and the dorsoradial ligament. This provides a dynamic stabilization effect that effectively counteracts the palmar ligamentous incompetence without the need for intra-articular exploration or soft tissue grafting.
Indications and Contraindications
The clinical success of a thumb metacarpal extension osteotomy is highly dependent on rigorous, evidence-based patient selection. The procedure is primarily indicated for patients with Eaton-Littler Stage I disease and select, carefully vetted cases of early Eaton-Littler Stage II disease. The ideal surgical candidate presents with pain localized strictly to the trapeziometacarpal joint, demonstrable hypermobility, a positive grind test or traction-shift test, and radiographic evidence of a normal or near-normal joint space without significant osteophyte formation.
A critical, non-negotiable prerequisite for this joint-preserving procedure is the absence of advanced cartilage wear. If the articular cartilage in the dorsal compartment of the trapezium is degraded, shifting the mechanical load dorsally via an extension osteotomy will inevitably result in persistent or exacerbated pain. Therefore, Eaton-Littler Stage III and IV diseases are absolute contraindications. Furthermore, the presence of concomitant scaphotrapezial trapezoidal (STT) joint arthritis must be carefully evaluated; altering the biomechanics of the thumb ray via osteotomy may unmask or aggravate subclinical midcarpal pathology.
| Parameter | Operative Indications for Extension Osteotomy | Non Operative Indications and Contraindications |
|---|---|---|
| Clinical Presentation | Painful pinch, subjective weakness, positive grind test, symptomatic hypermobility | Mild intermittent pain, asymptomatic laxity, pain responsive to NSAIDs |
| Eaton Littler Stage | Stage I and early Stage II | Stage III and Stage IV |
| Radiographic Findings | Normal joint space, minimal to no osteophytes, dorsal subluxation < 1/3 of joint surface | Joint space narrowing, subchondral sclerosis, large osteophytes, cystic changes |
| Conservative Management | Failure of minimum 3 to 6 months of splinting, NSAIDs, and targeted hand therapy | Responsive to thumb spica splinting, activity modification, and corticosteroid injections |
| Concomitant Pathology | Isolated trapeziometacarpal joint involvement | Scaphotrapezial trapezoidal arthritis, active local or systemic infection, inflammatory arthropathy |
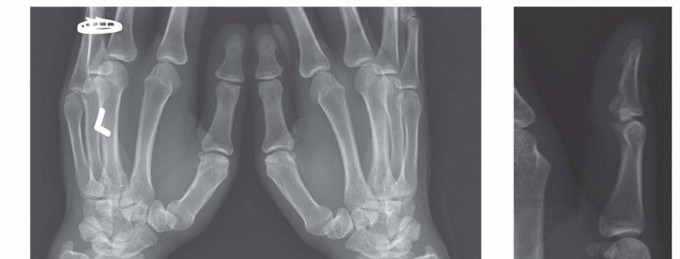
Patient Selection Criteria
When evaluating a patient for an extension osteotomy, the orthopaedic surgeon must perform a meticulous physical examination to differentiate trapeziometacarpal pathology from adjacent pain generators such as De Quervain tenosynovitis, trigger thumb (flexor pollicis longus tenosynovitis), or radioscaphoid arthritis. A local anesthetic injection (e.g., 1% lidocaine without epinephrine) directly into the trapeziometacarpal joint can serve as a highly specific diagnostic tool. Complete, albeit temporary, relief of pain following the intra-articular injection strongly correlates with the trapeziometacarpal joint as the primary pain generator and validates the rationale for surgical intervention.
Pre Operative Planning and Patient Positioning
Radiographic Evaluation
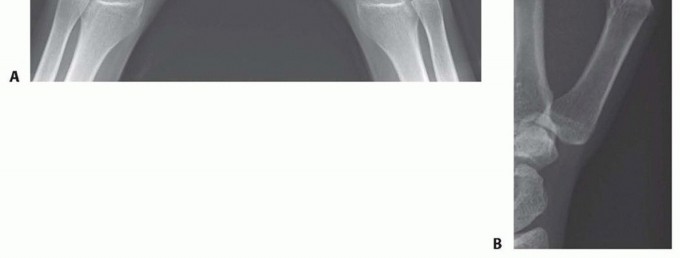
Comprehensive radiographic evaluation is mandatory for precise preoperative templating and staging. Standard imaging should include a posteroanterior (PA) view, a true lateral view of the thumb ray, and an anteroposterior (AP) view of the trapeziometacarpal joint, universally referred to as the Robert's view. The Robert's view is obtained by hyperpronating the forearm with the dorsum of the thumb resting flat against the radiographic cassette, providing an orthogonal projection of the trapeziometacarpal joint space unencumbered by overlapping carpal bones. Bett's view may also be utilized to assess the STT joint and the trapeziometacarpal articulation simultaneously.
Stress radiography may be utilized to quantify the degree of radial and dorsal subluxation. The surgeon must carefully scrutinize the dorsal aspect of the trapezium for any subtle signs of joint space narrowing or subchondral sclerosis, which would definitively preclude the use of an extension osteotomy.
Preoperative templating involves calculating the angle of the closing dorsal wedge. Biomechanical studies and extensive clinical series suggest that an extension angle of 20 to 30 degrees is optimal for unloading the palmar beak and tensioning the dorsal ligamentous complex. The osteotomy is typically planned approximately 10 to 15 millimeters distal to the trapeziometacarpal joint line to ensure adequate proximal bone stock for rigid internal fixation.
Surgical Set Up
The patient is positioned supine on the operating table with the operative extremity extended onto a radiolucent hand table. Regional anesthesia, typically an ultrasound-guided axillary or supraclavicular brachial plexus block, is highly preferred to provide excellent intraoperative anesthesia, skeletal muscle relaxation, and prolonged postoperative analgesia.
A well-padded pneumatic tourniquet is applied to the proximal upper arm and inflated to standard upper extremity pressures (typically 250 mmHg or 100 mmHg above systolic blood pressure) following exsanguination with an Esmarch bandage. Intraoperative fluoroscopy (mini C-arm) must be readily available and positioned parallel to the hand table to allow for seamless orthogonal imaging of the thumb ray without compromising the sterile surgical field.
Detailed Surgical Approach and Technique
Incision and Superficial Dissection
A dorsoradial incision (often a modification of the Wagner approach) is utilized to access the base of the thumb metacarpal. The incision begins approximately 1 centimeter proximal to the trapeziometacarpal joint and extends distally for 4 to 5 centimeters along the radial border of the first metacarpal shaft.
Superficial dissection requires meticulous, loupe-assisted technique to identify and protect the sensory branches of the superficial radial nerve (SRN) and the lateral antebrachial cutaneous nerve (LABCN). These neural structures are highly variable in their arborization over the anatomical snuffbox and the first dorsal compartment. Retraction of these nerve branches should be performed with vessel loops using minimal tension to prevent postoperative traction neuritis, which is a notoriously difficult and debilitating complication to manage.
Deep Dissection and Joint Exposure
The deep fascial incision is typically made between the extensor pollicis brevis (EPB) and the abductor pollicis longus (APL) tendons. Alternatively, the interval between the extensor pollicis longus (EPL) and the EPB can be utilized depending on the planned hardware placement and patient-specific anatomy. The radial artery, which courses obliquely across the anatomical snuffbox proximal to the trapeziometacarpal joint, must be identified and carefully protected during the proximal extent of the exposure.
The periosteum over the dorsal and radial aspects of the proximal first metacarpal is incised longitudinally and elevated. A limited dorsal capsulotomy may be performed if direct visualization of the articular surface is deemed necessary to confirm the absence of advanced chondral wear, though this is not strictly required if preoperative imaging is definitive. Subperiosteal dissection is carried circumferentially around the metacarpal base, utilizing curved, low-profile Hohmann retractors to protect the palmar soft tissues and the intrinsic thenar musculature.
Osteotomy Execution
The planned osteotomy site is marked 10 to 15 millimeters distal to the trapeziometacarpal joint line using a sterile marking pen or electrocautery. Using a microsagittal saw under continuous cold saline irrigation to prevent thermal necrosis of the bone, the distal cut of the wedge is made perpendicular to the longitudinal axis of the metacarpal shaft. The proximal cut is then made at an angle of 20 to 30 degrees relative to the first cut, creating a dorsally based wedge of bone.
It is absolutely critical to leave the palmar cortex intact to act as a stabilizing hinge. This intact palmar hinge provides inherent structural stability, facilitates accurate reduction, and promotes rapid endochondral bone healing. If the palmar cortex is inadvertently breached, the osteotomy becomes inherently unstable, necessitating more robust internal fixation and significantly increasing the risk of malunion, apex-dorsal angulation, or nonunion.
Reduction and Internal Fixation
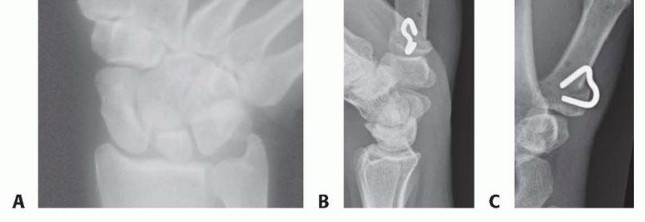
Once the dorsal wedge of bone is excised, the osteotomy is closed by extending the distal metacarpal shaft. This maneuver effectively flexes the metacarpal base relative to the shaft, achieving the desired biomechanical alteration. The reduction is provisionally held with a pointed reduction clamp or a longitudinally directed 0.045-inch Kirschner wire.
Stable internal fixation is paramount. While crossed Kirschner wires can be utilized and were common historically, rigid internal fixation with a low-profile titanium plate is generally preferred in modern practice to allow for early mobilization and predictable union. A 2.0-millimeter or 2.4-millimeter T-plate or straight locking plate is contoured to intimately fit the dorsal or dorsoradial aspect of the metacarpal.
The plate is applied with at least two locking or non-locking screws in the proximal fragment and two to three screws in the distal fragment. Careful fluoroscopic evaluation in both the true AP (Robert's) and true lateral planes is mandatory to confirm appropriate hardware placement, ensure that no proximal screws have penetrated the concave trapeziometacarpal joint surface, and verify the correct angle of the osteotomy.
Following definitive fixation, the tourniquet is deflated, and meticulous hemostasis is achieved with bipolar electrocautery. The periosteum and deep fascia are closed over the plate if possible to provide a smooth gliding surface for the overlying extensor tendons. The skin is closed with non-absorbable sutures (e.g., 4-0 or 5-0 nylon), and a bulky sterile dressing incorporating a rigid thumb spica splint is applied.
Complications and Management
While thumb metacarpal extension osteotomy is a highly effective, joint-preserving procedure, it is not without potential pitfalls. Complications can arise from technical errors during the execution of the osteotomy, improper patient selection, or postoperative issues related to hardware prominence and soft tissue healing.
Intraoperative Challenges
The most significant intraoperative challenge is the inadvertent completion of the osteotomy through the palmar cortex. Loss of the palmar hinge destabilizes the construct and makes controlling the apex-dorsal angulation exceedingly difficult. If this occurs, the surgeon must rely entirely on the rigid plate construct to maintain the 30-degree angular correction. This often requires the use of a longer, more robust plate or supplementary interfragmentary Kirschner wire fixation to prevent displacement and subsequent malunion.
Another critical intraoperative risk is the penetration of the proximal screws into the trapeziometacarpal joint. The proximal fragment is relatively small, and the concavity of the articular surface can be highly deceptive on standard fluoroscopic views. Utilizing a true Robert's view and dynamically rotating the thumb under live fluoroscopy is essential to ensure strictly extra-articular screw placement.
Postoperative Complications
Superficial radial nerve (SRN) neuritis is a well-documented complication following any surgical approach to the radial aspect of the wrist and hand. It typically presents as dysesthesia, hyperalgesia, or a positive Tinel's sign over the surgical scar. Management begins with conservative modalities, including gabapentinoids, aggressive desensitization therapy, and topical compounded analgesics. Refractory cases may require surgical exploration, neurolysis, or targeted muscle reinnervation (TMR) if a frank neuroma is identified.
Nonunion or delayed union of the osteotomy site is relatively rare, given the excellent blood supply to the metaphyseal bone of the metacarpal base and the compressive forces acting across the closing wedge. However, it can occur in patients with compromised healing capacity, such as active smokers or those with metabolic bone disease. Treatment of symptomatic nonunion typically requires revision open reduction and internal fixation (ORIF) combined with the application of autologous bone graft.
| Complication | Incidence Rate | Etiology and Risk Factors | Management and Salvage Strategies |
|---|---|---|---|
| Superficial Radial Nerve Neuritis | 5% to 10% | Iatrogenic traction, scar tissue entrapment, direct transection | Desensitization therapy, gabapentinoids, surgical neurolysis, neuroma excision and capping |
| Nonunion / Delayed Union | 1% to 3% | Smoking, thermal necrosis during saw cut, loss of palmar hinge, inadequate fixation | Smoking cessation, bone stimulator, revision open reduction internal fixation with bone grafting |
| Hardware Prominence | 10% to 15% | Use of bulky plates, inadequate soft tissue coverage over the dorsal metacarpal | Hardware removal after radiographic confirmation of complete osseous union (typically > 6 months) |
| Progression of Osteoarthritis | 10% to 20% (Long-term) | Inappropriate patient selection (unrecognized Stage III disease), failure to achieve adequate extension angle | Conversion to trapeziectomy with or without ligament reconstruction and tendon interposition (LRTI), or total joint arthroplasty |
| Malunion | 2% to 5% | Inaccurate preoperative templating, loss of fixation, asymmetric wedge resection | Corrective osteotomy if highly symptomatic, or salvage arthroplasty if secondary arthritis has developed |
Post Operative Rehabilitation Protocols
Early Immobilization Phase
The immediate postoperative goal is to protect the osteotomy site while aggressively managing edema and pain. The patient is placed in a rigid, custom-molded thermoplastic thumb spica splint or a fiberglass cast within the first week following surgery. The interphalangeal (IP) joint of the thumb is typically left free to allow for active flexion and extension, which helps prevent extensor pollicis longus adhesions and promotes venous return to minimize swelling.
During the first four weeks, the patient is instructed to maintain strict elevation of the operative extremity and perform active range of motion exercises for the digits, wrist (if not incorporated into the cast), elbow, and shoulder. Weight-bearing and forceful pinch activities are strictly prohibited during this initial phase of osseous consolidation.
Mobilization and Strengthening Phase
At approximately four to six weeks postoperatively, clinical and radiographic evaluations are performed. If orthogonal radiographs demonstrate early bridging callus formation and obliteration of the osteotomy line, the continuous rigid immobilization is discontinued. The patient is transitioned to a removable, custom-fitted thumb spica splint, which is worn primarily during sleep and high-risk activities.
Supervised hand therapy is initiated, focusing on active and active-assisted range of motion for the trapeziometacarpal joint. Techniques such as scar massage, silicone sheeting, and desensitization are employed to mitigate hypersensitivity over the dorsoradial incision.
By eight weeks postoperatively, assuming complete clinical and radiographic union, progressive strengthening exercises are introduced. These include isometric pinch exercises, grip strengthening, and dynamic stabilization drills for the thenar musculature (specifically the abductor pollicis brevis and opponens pollicis). Patients are typically cleared for a full return to unrestricted occupational and recreational activities between ten and twelve weeks, though maximal grip and pinch strength may continue to improve for up to six to twelve months following the procedure.
Summary of Key Literature and Guidelines
The evolution and validation of the thumb metacarpal extension osteotomy are deeply rooted in rigorous biomechanical research and long-term clinical outcome studies. The foundational work by Eaton and Littler established the critical role of the anterior oblique ligament in trapeziometacarpal stability, paving the way for targeted surgical interventions.
Pellegrini et al. provided the definitive biomechanical justification for the extension osteotomy. Their cadaveric studies elegantly demonstrated that an extension osteotomy effectively unloads the palmar compartment of the joint, which is the primary site of early chondral wear and synovitis. By shifting the contact stresses dorsally, the osteotomy protects the vulnerable palmar structures and normalizes joint kinematics.
Shrivastava et al. expanded on this foundation by defining the precise kinematic alterations induced by the osteotomy. They proved that flexing the metacarpal base thirty degrees relative to the shaft dynamically tensions the dorsal capsule and the dorsoradial ligament, thereby neutralizing the palmar instability caused by an incompetent anterior oblique ligament.
Clinical series by Tomaino, Wilson, and others have corroborated these biomechanical findings, reporting high rates of pain relief, significantly improved pinch strength, and a halt in radiographic disease progression in appropriately selected patients. Long-term follow-up studies indicate that survivorship of the native joint following an extension osteotomy exceeds 80% at ten years, provided the initial indication was strictly limited to Eaton-Littler Stage I or early Stage II disease.
In summary, the thumb metacarpal extension osteotomy represents a sophisticated, joint-preserving surgical technique. By leveraging a profound understanding of trapeziometacarpal kinematics, ligamentous anatomy, and load distribution, the orthopaedic surgeon can effectively alter the natural history of basal joint arthritis, providing durable symptom relief and preserving functional anatomy in the young, active, and high-demand patient.
You Might Also Like