Proximal Hamstring Avulsion Repair: An Intraoperative Masterclass
Key Takeaway
This masterclass provides an exhaustive guide to proximal hamstring avulsion repair. We cover crucial surgical anatomy, meticulous preoperative planning, and a granular, step-by-step intraoperative execution from incision to closure. Fellows will learn precise instrument use, critical pearls and pitfalls, and comprehensive postoperative rehabilitation protocols to optimize patient outcomes. Master this complex procedure with expert guidance.
Introduction and Epidemiology
Proximal hamstring injuries encompass a broad continuum of pathology, ranging from mild stretch-induced strains at the musculotendinous junction to complete avulsions of the hamstring muscle complex from the ischial tuberosity. These injuries are highly prevalent among athletes participating in sports that require explosive acceleration, rapid deceleration, or extreme ranges of hip flexion combined with knee extension. The incidence of hamstring injuries is particularly high in track and field, rugby, soccer, and water skiing.
Understanding the natural history of these injuries is critical for appropriate clinical decision-making. The clinical trajectory varies considerably based on the anatomic location and severity of the structural damage. More proximal injuries, particularly those involving the tendinous origin at the ischium, result in a significantly longer time for recovery to pre-injury status compared to distal or mid-substance myofascial injuries. Furthermore, complete avulsions carry a high likelihood of requiring surgical intervention due to the persistent and significant disability associated with loss of the posterior thigh kinetic chain.
Partial or complete hamstring avulsions must be strictly differentiated from strains at the musculotendinous junction. While musculotendinous strains are generally self-limiting and respond well to structured physical therapy, avulsions can be profoundly disabling. Patients with untreated avulsions frequently report intractable weakness, loss of eccentric muscle control during fast-paced running, and deep gluteal pain, particularly when sitting.
Fortunately, the majority of proximal hamstring injuries are strains at the musculotendinous junction that are best managed non-operatively. Strains most often occur in the biceps femoris, and the most common location is near the proximal muscle-tendon junction. Recovery time correlates directly with the percentage of muscle involved. This can be quantified by measuring the cross-sectional area or the longitudinal length of abnormal muscle signal on T2-weighted magnetic resonance imaging. Injuries involving over 50 percent of the cross-sectional area typically necessitate a recovery period exceeding six weeks, whereas those with minimal or normal imaging findings may resolve in approximately one week.
The greatest risk factor for injury to the hamstring muscle complex is a history of previous injury to the ipsilateral extremity. Literature reports recurrence rates for hamstring injuries ranging from 12 to 31 percent. Whether this high rate of reinjury is attributable to insufficient rehabilitation, premature return to sport, or the persistence of pre-existing biomechanical deficits, the treating orthopedic surgeon must possess the ability to accurately assess the degree of injury, a comprehensive knowledge of the reparative process of healing muscle, and a thorough understanding of both operative and non-operative management strategies.
Surgical Anatomy and Biomechanics
The hamstring muscle group consists of three distinct muscles residing in the posterior compartment of the thigh: the biceps femoris, the semitendinosus, and the semimembranosus. With the exception of the short head of the biceps femoris, all of these muscles originate from the ischial tuberosity of the pelvis. The hamstrings function as biarticular muscles, bridging both the hip and the knee joints, thereby playing a crucial role in simultaneous hip extension and knee flexion.

Osseous Origin and Tendinous Footprint
The anatomy of the ischial tuberosity footprint is highly specific and critical for anatomic surgical repair. The tuberosity is divided by a transverse ridge into an upper and lower portion. The upper portion is further divided by an oblique ridge into an inferomedial and a superolateral facet.
The biceps femoris long head and the semitendinosus share a common origin, forming the conjoint tendon. This conjoint tendon originates from the inferomedial facet of the upper portion of the ischial tuberosity. The semimembranosus has a distinct, independent origin located on the superolateral facet, positioned anterolateral and slightly deep to the conjoint tendon. Understanding this spatial relationship is vital during surgical reconstruction to ensure each tendon is restored to its native footprint.
The proximal tendons of the hamstrings are remarkably long and extend significantly into their respective muscle bellies. Anatomical studies have demonstrated that the proximal tendon of the biceps femoris extends for approximately 62 percent of the muscle belly length, while the semimembranosus tendon extends for about 73 percent of its muscle belly. This extensive musculotendinous architecture is designed to dissipate high tensile loads but also creates a long transition zone susceptible to strain.

Neurovascular Relationships
The most critical anatomical landmark during proximal hamstring surgery is the sciatic nerve. The sciatic nerve exits the greater sciatic foramen deep to the piriformis muscle and descends through the gluteal region. At the level of the ischial tuberosity, the sciatic nerve lies immediately lateral to the hamstring origin. On average, the nerve is located 1.2 to 1.5 centimeters lateral to the most lateral aspect of the ischial tuberosity.
In the setting of an acute avulsion, the resulting hematoma can compress or irritate the sciatic nerve, leading to radicular symptoms. In chronic avulsions, the retracted hamstring tendons frequently form dense fibrotic adhesions directly to the sciatic nerve. Consequently, meticulous neurolysis is an obligatory step in the surgical management of chronic proximal hamstring ruptures.
The arterial supply to the proximal hamstrings is derived primarily from the inferior gluteal artery and the perforating branches of the profunda femoris artery. Innervation to the long head of the biceps femoris, semitendinosus, and semimembranosus is provided by the tibial division of the sciatic nerve, whereas the short head of the biceps femoris is innervated by the common peroneal division.
Pathogenesis and Biomechanical Mechanisms
The principal mechanism of proximal hamstring injury involves eccentric activation while the muscle-tendon unit is under extreme stretch. This biomechanical scenario is classically observed during the terminal swing phase of high-speed running. At this moment, the hip is acutely flexed, and the knee is extending; the hamstrings must contract eccentrically to decelerate the forward momentum of the tibia prior to heel strike. The massive tensile forces generated during this eccentric contraction frequently exceed the physiological limits of the tendon or the musculotendinous junction, resulting in mechanical failure.
An alternative, though less common, mechanism involves extreme passive stretch with an uncertain or variable amount of active muscle contraction. This typically occurs in scenarios such as water skiing, martial arts, or gymnastics, where the knee is fully extended and the hip is suddenly forced into hyperflexion. This mechanism is more frequently associated with complete tendinous avulsions from the ischial tuberosity rather than mid-substance strains.
Indications and Contraindications
The decision to proceed with surgical intervention versus conservative management depends heavily on the acuity of the injury, the number of tendons involved, the degree of tendon retraction, and the functional demands of the patient.
Acute injuries are generally defined as those presenting within four weeks of the index trauma. Chronic injuries present after four weeks and are characterized by significant tendon retraction, muscle atrophy, fatty infiltration, and the formation of dense scar tissue. Surgical outcomes are universally superior when repair is performed in the acute setting, as the tissues are more mobile, the anatomy is less distorted by fibrosis, and the sciatic nerve is easier to identify and protect.
| Clinical Scenario | Operative Indications | Non Operative Indications |
|---|---|---|
| Tendon Involvement | Complete 3-tendon avulsion; 2-tendon avulsion with >2 cm retraction | Isolated single tendon avulsion; MTJ strains |
| Patient Demographics | High-demand athletes; active individuals with high functional expectations | Elderly patients; low-demand individuals; high surgical risk |
| Symptomatology | Intractable deep gluteal pain; sciatic radiculopathy; profound weakness | Minimal pain; well-compensated gait; resolving symptoms |
| Chronicity | Acute repairs (<4 weeks) highly favored; chronic repairs for refractory symptoms | Chronic asymptomatic nonunions; acute partial tears |
| Imaging Findings | >2 cm retraction on MRI; sciatic nerve tethering/compression | <2 cm retraction; intact semimembranosus with isolated conjoint tear |
Contraindications to surgical repair include isolated musculotendinous strains, single-tendon avulsions with minimal retraction in non-elite athletes, and patients with significant medical comorbidities that preclude safe prone positioning or anesthesia. Additionally, chronic avulsions with severe, irreversible fatty infiltration of the muscle bellies (Goutallier stage 3 or 4) may represent a relative contraindication, as the muscle may lack the contractile capacity to justify the risks of surgical reconstruction.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning relies heavily on high-quality magnetic resonance imaging. MRI is the gold standard for evaluating proximal hamstring injuries. T2-weighted fat-suppressed sequences in both the axial and coronal planes are essential for determining the number of tendons avulsed, the exact distance of tendon retraction, the presence of an organizing hematoma, and the proximity of the retracted tendon stump to the sciatic nerve.

Clinical Evaluation
The patient history and physical findings are highly indicative of the underlying pathology. A proximal hamstring avulsion typically results in a sudden, sharp onset of pain in the posterior proximal thigh during athletic competition or training. Patients often report an audible pop or the sensation of being struck in the back of the leg.
Severe injuries present with visible deformity, massive ecchymosis tracking down the posterior thigh, and a palpable defect immediately distal to the ischial tuberosity. With the patient lying prone and the hamstrings actively engaged against resistance, palpation of the proximal hamstring origin is undertaken. A palpable defect or the absence of the normal taut tendinous cords implies a proximal avulsion. Provocative testing, including resisted knee flexion and resisted hip extension, will elicit significant weakness and focal pain.
Operating Room Setup and Positioning
Surgical repair is performed under general anesthesia. The patient is positioned prone on a Jackson radiolucent table or a standard operating table equipped with chest and pelvic rolls to allow the abdomen to hang free, thereby reducing venous pressure and intraoperative bleeding.

The affected lower extremity is prepped and draped free to allow for full intraoperative manipulation of the hip and knee. A sterile padded bump or a Mayo stand is placed under the operative leg to maintain the knee in approximately 60 to 90 degrees of flexion. Flexing the knee and slightly extending the hip reduces tension on the hamstring muscle complex, facilitating mobilization of the retracted tendons and allowing for tension-free fixation to the ischial tuberosity. Fluoroscopy should be available and positioned to allow for orthogonal views of the ischial tuberosity to confirm anchor placement and trajectory.
Detailed Surgical Approach and Technique
The surgical approach to the proximal hamstring requires meticulous dissection and a thorough understanding of the posterior thigh anatomy to avoid iatrogenic neurovascular injury.
Incision and Superficial Dissection
A transverse incision within the gluteal crease is cosmetically appealing and provides excellent access for acute injuries with minimal retraction. However, for chronic injuries or acute injuries with retraction exceeding 3 to 4 centimeters, a longitudinal incision centered over the ischial tuberosity and extending distally along the posterior thigh is strongly recommended. This extensile approach allows for adequate visualization of the retracted tendon stump and the sciatic nerve.

The subcutaneous tissues are divided in line with the incision. The fascia lata is identified and incised longitudinally. The inferior border of the gluteus maximus is identified and retracted superiorly. In some cases, a small portion of the gluteus maximus insertion on the linea aspera may need to be released to improve visualization of the ischial footprint.
Deep Dissection and Sciatic Nerve Identification
The most critical step in the deep dissection is the definitive identification and protection of the sciatic nerve. The nerve must be identified proximal to the zone of injury, where the anatomy remains relatively undisturbed. The nerve is located deep to the gluteus maximus and lateral to the ischial tuberosity.
Once identified, the sciatic nerve is carefully traced distally into the zone of injury. In acute cases, the nerve is often enveloped in a large hematoma. The hematoma should be evacuated, and the nerve gently retracted laterally using a vessel loop. In chronic cases, dense scar tissue will tether the retracted hamstring tendons to the sciatic nerve. A meticulous neurolysis using surgical loupes and micro-dissection instruments is required to separate the nerve from the fibrotic tendon stump. The nerve must be freed circumferentially to prevent postoperative tethering and radiculopathy.
Tendon Mobilization and Footprint Preparation
Following neurolysis, the retracted hamstring tendon complex is identified. The conjoint tendon and the semimembranosus tendon are often retracted as a single unit, though they may be torn independently. Heavy non-absorbable traction sutures (e.g., #2 or #5 FiberWire) are placed into the distal tendon stump using a locked Krackow configuration. This provides control of the tendon and aids in distal mobilization.

If the tendon is chronically retracted, circumferential release of fascial adhesions to the surrounding musculature is necessary. The knee is flexed to 90 degrees to assist in pulling the tendon proximally towards the ischial tuberosity.
Attention is then directed to the ischial tuberosity. The native footprint is cleared of remaining soft tissue and hematoma using an electrocautery and a periosteal elevator. The cortical surface of the ischial tuberosity is decorticated using a high-speed burr or a curette to expose bleeding cancellous bone. This creates an optimal biological environment for tendon-to-bone healing.
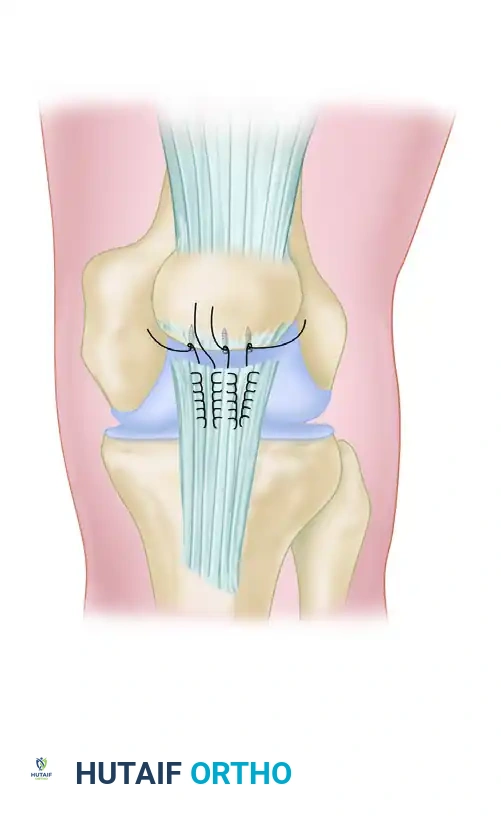
Anchor Placement and Tendon Fixation
Fixation is typically achieved using multiple suture anchors. Depending on the size of the patient and the footprint, two to four anchors are utilized. Double-loaded or triple-loaded metallic or PEEK (polyetheretherketone) anchors (typically 5.0 mm to 5.5 mm in diameter) are inserted into the decorticated ischial footprint.
The anchors should be placed systematically, typically starting with the most proximal and medial anchors to recreate the native anatomy. Care must be taken to angle the drill and anchors appropriately to avoid penetrating the inner table of the pelvis or violating the hip joint.
The suture limbs from the anchors are then passed through the mobilized hamstring tendon stump. A combination of horizontal mattress and simple stitches can be used. For a more robust biomechanical construct, a double-row equivalent technique can be employed, utilizing medial row anchors passed through the tendon and lateral row knotless anchors to compress the tendon against the bone.
The sutures are tied systematically while an assistant maintains the knee in 90 degrees of flexion and the hip in neutral extension to minimize tension on the repair. Following fixation, the repair is directly visualized and palpated to ensure a secure, gap-free approximation of the tendon to the ischial footprint. The wound is irrigated copiously, and the fascia, subcutaneous tissue, and skin are closed in a layered fashion.
Complications and Management
Surgical repair of proximal hamstring avulsions is a major procedure associated with a distinct set of potential complications. Thorough preoperative counseling and meticulous surgical technique are essential to mitigate these risks.
| Complication | Estimated Incidence | Etiology and Risk Factors | Management and Salvage Strategies |
|---|---|---|---|
| Sciatic Nerve Palsy / Irritation | 2% - 15% (Higher in chronic) | Iatrogenic traction; aggressive neurolysis; postoperative hematoma; scar tethering | Observation for neuropraxia; gabapentinoids; surgical exploration and neurolysis for refractory cases |
| Re Rupture / Failure of Fixation | 2% - 6% | Non-compliance with rehab; premature weight-bearing; poor tissue quality | Revision surgery with allograft augmentation (Achilles or hamstring allograft); conservative management if low demand |
| Deep Surgical Site Infection | 1% - 3% | Proximity to perianal region; large hematoma; prolonged operative time | Intravenous antibiotics; surgical irrigation and debridement; retention of hardware if stable |
| Venous Thromboembolism (DVT/PE) | < 1% | Prone positioning; postoperative immobilization | Chemical prophylaxis based on risk stratification; therapeutic anticoagulation if DVT confirmed |
| Ischial Apophysitis / Hardware Pain | 5% - 10% | Prominent suture knots; anchor pullout; heterotopic ossification | Corticosteroid injections; extracorporeal shockwave therapy; hardware removal after complete healing |
Sciatic nerve complications are the most feared morbidity associated with this procedure. Neuropraxia may occur due to excessive traction during surgery or compression from a postoperative hematoma. In chronic cases requiring extensive neurolysis, transient dysesthesias are relatively common and typically resolve over several weeks to months. If a patient presents with a dense, progressive motor deficit postoperatively, an expanding hematoma must be suspected, and emergent surgical decompression may be warranted.

Re-rupture is a devastating complication that often requires complex revision surgery. Revision techniques frequently necessitate the use of allograft tissue, such as an Achilles tendon with a bone block or a semitendinosus allograft, to bridge the gap between the retracted native tendon and the ischial tuberosity. To minimize the risk of re-rupture, strict adherence to postoperative rehabilitation protocols is paramount.
Post Operative Rehabilitation Protocols
Rehabilitation following proximal hamstring repair is a lengthy and highly structured process, typically requiring six to nine months before a full return to competitive sports is permitted. The protocol is divided into distinct phases designed to protect the surgical repair while progressively restoring range of motion, strength, and neuromuscular control.
Phase 1 Protection Phase Weeks 0 to 6
The primary goal of the initial phase is to protect the tendon-to-bone healing interface. The patient is placed in a hinged knee brace locked in 60 to 90 degrees of flexion. Weight-bearing is strictly limited; the patient is typically non-weight-bearing or toe-touch weight-bearing with the use of bilateral crutches. Active knee flexion and active hip extension are strictly prohibited to avoid concentric and eccentric loading of the repair. Passive range of motion is initiated carefully, avoiding simultaneous hip flexion and knee extension.
Phase 2 Intermediate Phase Weeks 6 to 12
At six weeks, the hinged knee brace is progressively unlocked to allow increasing degrees of knee extension. The patient is transitioned to partial weight-bearing and eventually full weight-bearing as tolerated. The brace is typically discontinued by week eight. Gentle active range of motion is initiated. Isometric hamstring strengthening begins in a protected position (e.g., prone with the knee flexed). Core stabilization and gluteal strengthening exercises are incorporated to address kinetic chain deficits.
Phase 3 Advanced Strengthening Phase Months 3 to 6
Once full, pain-free range of motion is achieved and normal gait mechanics are restored, the focus shifts to progressive resistance training. Isotonic hamstring curls are introduced, gradually increasing the resistance. Around the four-month mark, eccentric hamstring strengthening is initiated. Eccentric strength is critical for preventing reinjury, as it mimics the deceleration forces experienced during the terminal swing phase of running. Modalities such as Nordic hamstring exercises are introduced cautiously.
Phase 4 Return to Sport Phase Months 6+
The final phase involves sport-specific dynamic training. Agility drills, plyometrics, and sprinting mechanics are progressively integrated. Return to sport criteria are stringent and typically require the patient to demonstrate:
1. Full, symmetrical range of motion of the hip and knee.
2. Isokinetic hamstring strength testing demonstrating at least 90 percent strength compared to the uninjured contralateral limb.
3. Successful completion of sport-specific functional testing without pain or apprehension.
4. Psychological readiness to return to high-level competition.
Summary of Key Literature and Guidelines
The academic literature regarding proximal hamstring injuries has expanded significantly, providing robust evidence to guide clinical practice.
Landmark biomechanical studies have elucidated the complex strain patterns experienced by the hamstring complex. Research demonstrates that the biceps femoris is subjected to the highest degree of stretch during the terminal swing phase of sprinting, which correlates with the high incidence of biceps femoris musculotendinous strains.
Regarding surgical outcomes, systematic reviews consistently demonstrate that surgical repair of acute proximal hamstring avulsions yields superior subjective and objective outcomes compared to non-operative management in athletic populations. Acute repairs are associated with higher rates of return to pre-injury levels of sport, greater isokinetic strength recovery, and lower rates of persistent gluteal pain.
The literature also emphasizes the critical distinction between acute and chronic repairs. Chronic repairs are technically more demanding, have higher estimated blood loss, longer operative times, and a significantly higher incidence of postoperative sciatic nerve complications. Despite these challenges, surgical reconstruction of chronic symptomatic avulsions remains a viable and effective procedure for alleviating pain and improving function, though patients must be counseled that strength may never fully return to baseline.
Advancements in endoscopic techniques have also been reported in recent literature. Endoscopic repair of proximal hamstring avulsions is an emerging technique that aims to minimize soft tissue morbidity and reduce the risk of wound complications. While early outcomes are promising, this technique requires advanced arthroscopic skills and is generally reserved for partial avulsions or acute complete avulsions with minimal retraction. Open repair remains the gold standard for multi-tendon avulsions with significant retraction.
Clinical & Radiographic Imaging







You Might Also Like